- Open access
- Published: 26 November 2021

Women’s Perceptions and Experiences of Breastfeeding: a scoping review of the literature
- Bridget Beggs 1 ,
- Liza Koshy 1 &
- Elena Neiterman 1
BMC Public Health volume 21 , Article number: 2169 ( 2021 ) Cite this article
14k Accesses
30 Citations
4 Altmetric
Metrics details
Despite public health efforts to promote breastfeeding, global rates of breastfeeding continue to trail behind the goals identified by the World Health Organization. While the literature exploring breastfeeding beliefs and practices is growing, it offers various and sometimes conflicting explanations regarding women’s attitudes towards and experiences of breastfeeding. This research explores existing empirical literature regarding women’s perceptions about and experiences with breastfeeding. The overall goal of this research is to identify what barriers mothers face when attempting to breastfeed and what supports they need to guide their breastfeeding choices.
This paper uses a scoping review methodology developed by Arksey and O’Malley. PubMed, CINAHL, Sociological Abstracts, and PsychInfo databases were searched utilizing a predetermined string of keywords. After removing duplicates, papers published in 2010–2020 in English were screened for eligibility. A literature extraction tool and thematic analysis were used to code and analyze the data.
In total, 59 papers were included in the review. Thematic analysis showed that mothers tend to assume that breastfeeding will be easy and find it difficult to cope with breastfeeding challenges. A lack of partner support and social networks, as well as advice from health care professionals, play critical roles in women’s decision to breastfeed.
While breastfeeding mothers are generally aware of the benefits of breastfeeding, they experience barriers at individual, interpersonal, and organizational levels. It is important to acknowledge that breastfeeding is associated with challenges and provide adequate supports for mothers so that their experiences can be improved, and breastfeeding rates can reach those identified by the World Health Organization.
Peer Review reports
Public health efforts to educate parents about the importance of breastfeeding can be dated back to the early twentieth century [ 1 ]. The World Health Organization is aiming to have at least half of all the mothers worldwide exclusively breastfeeding their infants in the first 6 months of life by the year 2025 [ 2 ], but it is unlikely that this goal will be achieved. Only 38% of the global infant population is exclusively breastfed between 0 and 6 months of life [ 2 ], even though breastfeeding initiation rates have shown steady growth globally [ 3 ]. The literature suggests that while many mothers intend to breastfeed and even make an attempt at initiation, they do not always maintain exclusive breastfeeding for the first 6 months of life [ 4 , 5 ]. The literature identifies various barriers, including return to paid employment [ 6 , 7 ], lack of support from health care providers and significant others [ 8 , 9 ], and physical challenges [ 9 ] as potential factors that can explain premature cessation of breastfeeding.
From a public health perspective, the health benefits of breastfeeding are paramount for both mother and infant [ 10 , 11 ]. Globally, new mothers following breastfeeding recommendations could prevent 974,956 cases of childhood obesity, 27,069 cases of mortality from breast cancer, and 13,644 deaths from ovarian cancer per year [ 11 ]. Global economic loss due to cognitive deficiencies resulting from cessation of breastfeeding has been calculated to be approximately USD $285.39 billion dollars annually [ 11 ]. Evidently, increasing exclusive breastfeeding rates is an important task for improving population health outcomes. While public health campaigns targeting pregnant women and new mothers have been successful in promoting breastfeeding, they also have been perceived as too aggressive [ 12 ] and failing to consider various structural and personal barriers that may impact women’s ability to breastfeed [ 1 ]. In some cases, public health messaging itself has been identified as a barrier due to its rigid nature and its lack of flexibility in guidelines [ 13 ]. Hence, while the literature on women’s perceptions regarding breastfeeding and their experiences with breastfeeding has been growing [ 14 , 15 , 16 ], it offers various, and sometimes contradictory, explanations on how and why women initiate and maintain breastfeeding and what role public health messaging plays in women’s decision to breastfeed.
The complex array of the barriers shaping women’s experiences of breastfeeding can be broadly categorized utilizing the socioecological model, which suggests that individuals’ health is a result of the interplay between micro (individual), meso (institutional), and macro (social) factors [ 17 ]. Although previous studies have explored barriers and supports to breastfeeding, the majority of articles focus on specific geographic areas (e.g. United States or United Kingdom), workplaces, or communities. In addition, very few articles focus on the analysis of the interplay between various micro, meso, and macro-level factors in shaping women’s experiences of breastfeeding. Synthesizing the growing literature on the experiences of breastfeeding and the factors shaping these experiences, offers researchers and public health professionals an opportunity to examine how various personal and institutional factors shape mothers’ breastfeeding decision-making. This knowledge is needed to identify what can be done to improve breastfeeding rates and make breastfeeding a more positive and meaningful experience for new mothers.
The aim of this scoping review is to synthesize evidence gathered from empirical literature on women’s perceptions about and experiences of breastfeeding. Specifically, the following questions are examined:
What does empirical literature report on women’s perceptions on breastfeeding?
What barriers do women face when they attempt to initiate or maintain breastfeeding?
What supports do women need in order to initiate and/or maintain breastfeeding?
Focusing on women’s experiences, this paper aims to contribute to our understanding of women’s decision-making and behaviours pertaining to breastfeeding. The overarching aim of this review is to translate these findings into actionable strategies that can streamline public health messaging and improve breastfeeding education and supports offered by health care providers working with new mothers.
This research utilized Arksey & O’Malley’s [ 18 ] framework to guide the scoping review process. The scoping review methodology was chosen to explore a breadth of literature on women’s perceptions about and experiences of breastfeeding. A broad research question, “What does empirical literature tell us about women’s experiences of breastfeeding?” was set to guide the literature search process.
Search methods
The review was undertaken in five steps: (1) identifying the research question, (2) identifying relevant literature, (3) iterative selection of data, (4) charting data, and (5) collating, summarizing, and reporting results. The inclusion criteria were set to empirical articles published between 2010 and 2020 in peer-reviewed journals with a specific focus on women’s self-reported experiences of breastfeeding, as well as how others see women’s experiences of breastfeeding. The focus on women’s perceptions of breastfeeding was used to capture the papers that specifically addressed their experiences and the barriers that they may encounter while breastfeeding. Only articles written in English were included in the review. The keywords utilized in the search strategy were developed in collaboration with a librarian (Table 1 ). PubMed, CINAHL, Sociological Abstracts, and PsychInfo databases were searched for the empirical literature, yielding a total of 2885 results.
Search outcome
The articles deemed to fit the inclusion criteria ( n = 213) were imported into RefWorks, an online reference manager tool and further screened for eligibility (Fig. 1 ). After the removal of 61 duplicates and title/abstract screening, 152 articles were kept for full-text review. Two independent reviewers assessed the papers to evaluate if they met the inclusion criteria of having an explicit analytic focus on women’s experiences of breastfeeding.
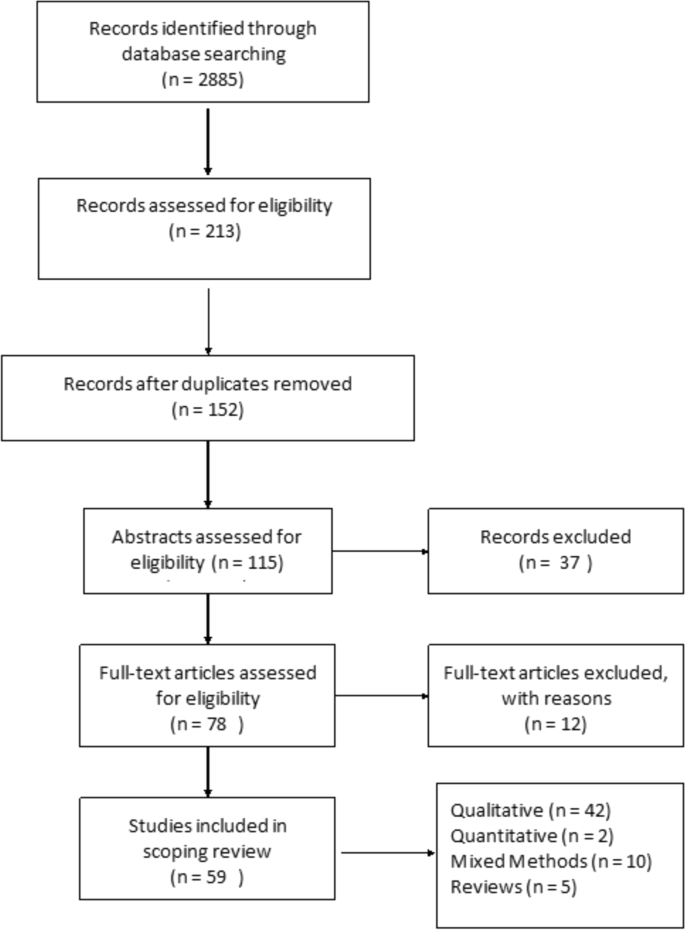
Prisma Flow Diagram
Quality appraisal
Consistent with scoping review methodology [ 18 ], the quality of the papers included in the review was not assessed.
Data abstraction
A literature extraction tool was created in MS Excel 2016. The data extracted from each paper included: (a) authors names, (b) title of the paper, (c) year of publication, (d) study objectives, (e) method used, (f) participant demographics, (g) country where the study was conducted, and (h) key findings from the paper.
Thematic analysis was utilized to identify key topics covered by the literature. Two reviewers independently read five papers to inductively generate key themes. This process was repeated until the two reviewers reached a consensus on the coding scheme, which was subsequently applied to the remainder of the articles. Key themes were added to the literature extraction tool and each paper was assigned a key theme and sub-themes, if relevant. The themes derived from the analysis were reviewed once again by all three authors when all the papers were coded. In the results section below, the synthesized literature is summarized alongside the key themes identified during the analysis.
In total, 59 peer-reviewed articles were included in the review. Since the review focused on women’s experiences of breastfeeding, as would be expected based on the search criteria, the majority of articles ( n = 42) included in the sample were qualitative studies, with ten utilizing a mixed method approach (Fig. 2 ). Figure 3 summarizes the distribution of articles by year of publication and Fig. 4 summarizes the geographic location of the study.
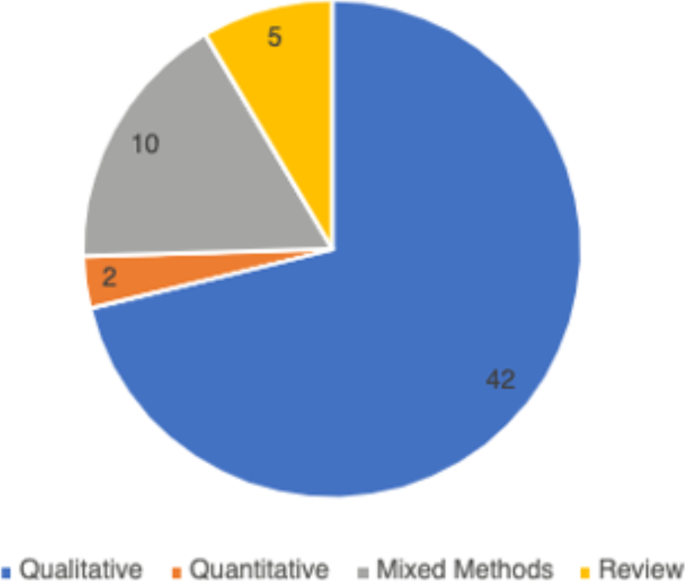
Types of Articles
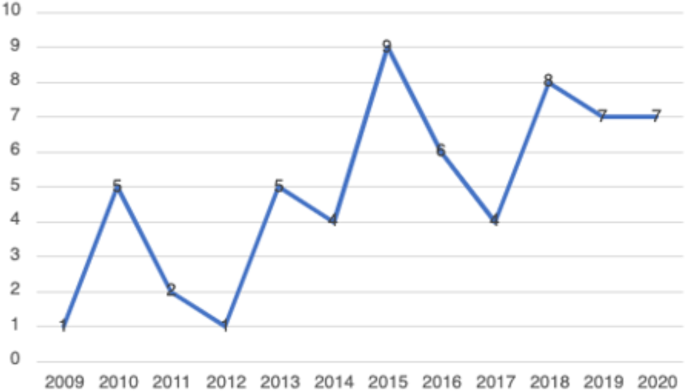
Years of Publication
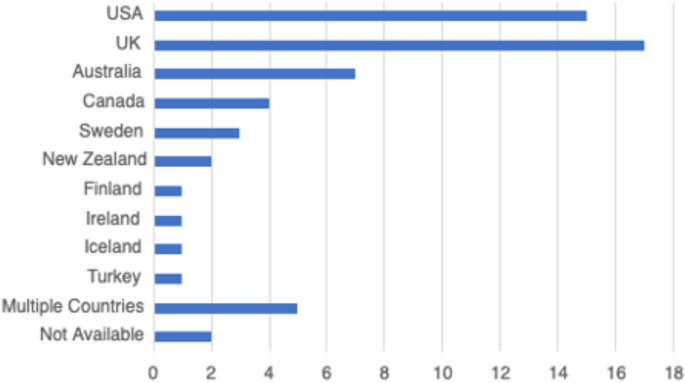
Countries of Focus Examined in Literature Review
Perceptions about breastfeeding
Women’s perceptions about breastfeeding were covered in 83% ( n = 49) of the papers. Most articles ( n = 31) suggested that women perceived breastfeeding as a positive experience and believed that breastfeeding had many benefits [ 19 , 20 ]. The phrases “breast is best” and “breastmilk is best” were repeatedly used by the participants of studies included in the reviewed literature [ 21 ]. Breastfeeding was seen as improving the emotional bond between the mother and the child [ 20 , 22 , 23 ], strengthening the child’s immune system [ 24 , 25 ], and providing a booster to the mother’s sense of self [ 1 , 26 ]. Convenience of breastfeeding (e.g., its availability and low cost) [ 19 , 27 ] and the role of breastfeeding in weight loss during the postpartum period were mentioned in the literature as other factors that positively shape mothers’ perceptions about breastfeeding [ 28 , 29 ].
The literature suggested that women’s perceptions of breastfeeding and feeding choices were also shaped by the advice of healthcare providers [ 30 , 31 ]. Paradoxically, messages about the importance and relative simplicity of breastfeeding may also contribute to misalignment between women’s expectations and the actual experiences of breastfeeding [ 32 ]. For instance, studies published in Canada and Sweden reported that women expected breastfeeding to occur “naturally”, to be easy and enjoyable [ 23 ]. Consequently, some women felt unprepared for the challenges associated with initiation or maintenance of breastfeeding [ 31 , 33 ]. The literature pointed out that mothers may feel overwhelmed by the frequency of infant feedings [ 26 ] and the amount as well as intensity of physical difficulties associated with breastfeeding initiation [ 33 ]. Researchers suggested that since many women see breastfeeding as a sign of being a “good” mother, their inability to breastfeed may trigger feelings of personal failure [ 22 , 34 ].
Women’s personal experiences with and perceptions about breastfeeding were also influenced by the cultural pressure to breastfeed. Welsh mothers interviewed in the UK, for instance, revealed that they were faced with judgement and disapproval when people around them discovered they opted out of breastfeeding [ 35 ]. Women recalled the experiences of being questioned by others, including strangers, when they were bottle feeding their infants [ 9 , 35 , 36 ].
Barriers to breastfeeding
The vast majority ( n = 50) of the reviewed literature identified various barriers for successful breastfeeding. A sizeable proportion of literature (41%, n = 24) explored women’s experiences with the physical aspects of breastfeeding [ 23 , 33 ]. In particular, problems with latching and the pain associated with breastfeeding were commonly cited as barriers for women to initiate breastfeeding [ 23 , 28 , 37 ]. Inadequate milk supply, both actual and perceived, was mentioned as another barrier for initiation and maintenance of breastfeeding [ 33 , 37 ]. Breastfeeding mothers were sometimes unable to determine how much milk their infants consumed (as opposed to seeing how much milk the infant had when bottle feeding), which caused them to feel anxious and uncertain about scheduling infant feedings [ 28 , 37 ]. Women’s inability to overcome these barriers was linked by some researchers to low self-efficacy among mothers, as well as feeling overwhelmed or suffering from postpartum depression [ 38 , 39 ].
In addition to personal and physical challenges experienced by mothers who were planning to breastfeed, the literature also highlighted the importance of social environment as a potential barrier to breastfeeding. Mothers’ personal networks were identified as a key factor in shaping their breastfeeding behaviours in 43 (73%) articles included in this review. In a study published in the UK, lack of role models – mothers, other female relatives, and friends who breastfeed – was cited as one of the potential barriers for breastfeeding [ 36 ]. Some family members and friends also actively discouraged breastfeeding, while openly questioning the benefits of this practice over bottle feeding [ 1 , 17 , 40 ]. Breastfeeding during family gatherings or in the presence of others was also reported as a challenge for some women from ethnic minority groups in the United Kingdom and for Black women in the United States [ 41 , 42 ].
The literature reported occasional instances where breastfeeding-related decisions created conflict in women’s relationships with significant others [ 26 ]. Some women noted they were pressured by their loved one to cease breastfeeding [ 22 ], especially when women continued to breastfeed 6 months postpartum [ 43 ]. Overall, the literature suggested that partners play a central role in women’s breastfeeding practices [ 8 ], although there was no consistency in the reviewed papers regarding the partners’ expressed level of support for breastfeeding.
Knowledge, especially practical knowledge about breastfeeding, was mentioned as a barrier in 17% ( n = 10) of the papers included in this review. While health care providers were perceived as a primary source of information on breastfeeding, some studies reported that mothers felt the information provided was not useful and occasionally contained conflicting advice [ 1 , 17 ]. This finding was reported across various jurisdictions, including the United States, Sweden, the United Kingdom and Netherlands, where mothers reported they had no support at all from their health care providers which made it challenging to address breastfeeding problems [ 26 , 38 , 44 ].
Breastfeeding in public emerged as a key barrier from the reviewed literature and was cited in 56% ( n = 33) of the papers. Examining the experiences of breastfeeding mothers in the United States, Spencer, Wambach, & Domain [ 45 ] suggested that some participants reported feeling “erased” from conversations while breastfeeding in public, rendering their bodies symbolically invisible. Lack of designated public spaces for breastfeeding forced many women to alter their feeding in public and to retreat to a private or a more secluded space, such as one’s personal car [ 25 ]. The oversexualization of women’s breasts was repeatedly noted as a core reason for the United States women’s negative experiences and feelings of self-consciousness about breastfeeding in front of others [ 45 ]. Studies reported women’s accounts of feeling the disapproval or disgust of others when breastfeeding in public [ 46 , 47 ], and some reported that women opted out of breastfeeding in public because they did not want to make those around them feel uncomfortable [ 25 , 40 , 48 ].
Finally, return to paid employment was noted in the literature as a significant challenge for continuation of breastfeeding [ 48 ]. Lack of supportive workplace environments [ 39 ] or inability to express milk were cited by women as barriers for continuing breastfeeding in the United States and New Zealand [ 39 , 49 ].
Supports needed to maintain breastfeeding
Due to the central role family members played in women’s experiences of breastfeeding, support from partners as well as female relatives was cited in the literature as key factors shaping women’s breastfeeding decisions [ 1 , 9 , 48 ]. In the articles published in Canada, Australia, and the United Kingdom, supportive family members allowed women to share the responsibility of feeding and other childcare activities, which reduced the pressures associated with being a new mother [ 19 , 20 ]. Similarly, encouragement, breastfeeding advice, and validation from healthcare professionals were identified as positively impacting women’s experiences with breastfeeding [ 1 , 22 , 28 ].
Community resources, such as peer support groups, helplines, and in-home breastfeeding support provided mothers with the opportunity to access help when they need it, and hence were reported to be facilitators for breastfeeding [ 19 , 22 , 33 , 44 ]. An increase in the usage of social media platforms, such as Facebook, among breastfeeding mothers for peer support were reported in some studies [ 47 ]. Public health breastfeeding clinics, lactation specialists, antenatal and prenatal classes, as well as education groups for mothers were identified as central support structures for the initiation and maintenance of breastfeeding [ 23 , 24 , 28 , 33 , 39 , 50 ]. Based on the analysis of the reviewed literature, however, access to these services varied greatly geographically and by socio-economic status [ 33 , 51 ]. It is also important to note that local and cultural context played a significant role in shaping women’s perceptions of breastfeeding. For example, a study that explored women’s breastfeeding experiences in Iceland highlighted the importance of breastfeeding in Icelandic society [ 52 ]. Women are expected to breastfeed and the decision to forgo breastfeeding is met with disproval [ 52 ]. Cultural beliefs regarding breastfeeding were also deemed important in the study of Szafrankska and Gallagher (2016), who noted that Polish women living in Ireland had a much higher rate of initiating breastfeeding compared to Irish women [ 53 ]. They attributed these differences to familial and societal expectations regarding breastfeeding in Poland [ 53 ].
Overall, the reviewed literature suggested that women faced socio-cultural pressure to breastfeed their infants [ 36 , 40 , 54 ]. Women reported initiating breastfeeding due to recognition of the many benefits it brings to the health of the child, even when they were reluctant to do it for personal reasons [ 8 ]. This hints at the success of public health education campaigns on the benefits of breastfeeding, which situates breastfeeding as a new cultural norm [ 24 ].
This scoping review examined the existing empirical literature on women’s perceptions about and experiences of breastfeeding to identify how public health messaging can be tailored to improve breastfeeding rates. The literature suggests that, overall, mothers are aware of the positive impacts of breastfeeding and have strong motivation to breastfeed [ 37 ]. However, women who chose to breastfeed also experience many barriers related to their social interactions with significant others and their unique socio-cultural contexts [ 25 ]. These different factors, summarized in Fig. 5 , should be considered in developing public health activities that promote breastfeeding. Breastfeeding experiences for women were very similar across the United Kingdom, United States, Canada, and Australia based on the studies included in this review. Likewise, barriers and supports to breastfeeding identified by women across the countries situated in the global north were quite similar. However, local policy context also impacted women’s experiences of breastfeeding. For example, maintaining breastfeeding while returning to paid employment has been identified as a challenge for mothers in the United States [ 39 , 45 ], a country with relatively short paid parental leave. Still, challenges with balancing breastfeeding while returning to paid employment were also noticed among women in New Zealand, despite a more generous maternity leave [ 49 ]. This suggests that while local and institutional policies might shape women’s experiences of breastfeeding, interpersonal and personal factors can also play a central role in how long they breastfeed their infants. Evidently, the importance of significant others, such as family members or friends, in providing support to breastfeeding mothers was cited as a key facilitator for breastfeeding across multiple geographic locations [ 29 , 34 , 48 ]. In addition, cultural beliefs and practices were also cited as an important component in either promoting breastfeeding or deterring women’s desire to initiate or maintain breastfeeding [ 15 , 29 , 37 ]. Societal support for breastfeeding and cultural practices can therefore partly explain the variation in breastfeeding rates across different countries [ 15 , 21 ]. Figure 5 summarizes the key barriers identified in the literature that inhibit women’s ability to breastfeed.
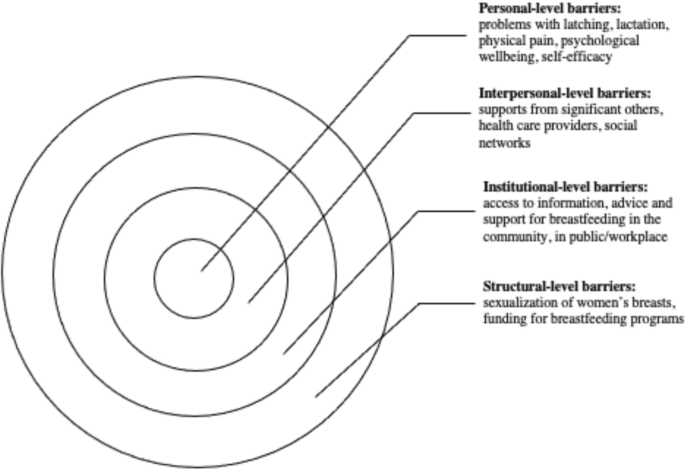
Barriers to Breastfeeding
At the individual level, women might experience challenges with breastfeeding stemming from various physiological and psychological problems, such as issues with latching, perceived or actual lack of breastmilk, and physical pain associated with breastfeeding. The onset of postpartum depression or other psychological problems may also impact women’s ability to breastfeed [ 54 ]. Given that many women assume that breastfeeding will happen “naturally” [ 15 , 40 ] these challenges can deter women from initiating or continuing breastfeeding. In light of these personal challenges, it is important to consider the potential challenges associated with breastfeeding that are conveyed to new mothers through the simplified message “breast is best” [ 21 ]. While breastfeeding may come easy to some women, most papers included in this review pointed to various challenges associated with initiating or maintaining breastfeeding [ 19 , 33 ]. By modifying public health messaging regarding breastfeeding to acknowledge that breastfeeding may pose a challenge and offering supports to new mothers, it might be possible to alleviate some of the guilt mothers experience when they are unable to breastfeed.
Barriers that can be experienced at the interpersonal level concern women’s communication with others regarding their breastfeeding choices and practices. The reviewed literature shows a strong impact of women’s social networks on their decision to breastfeed [ 24 , 33 ]. In particular, significant others – partners, mothers, siblings and close friends – seem to have a considerable influence over mothers’ decision to breastfeed [ 42 , 53 , 55 ]. Hence, public health messaging should target not only mothers, but also their significant others in developing breastfeeding campaigns. Social media may also be a potential medium for sharing supports and information regarding breastfeeding with new mothers and their significant others.
There is also a strong need for breastfeeding supports at the institutional and community levels. Access to lactation consultants, sound and practical advice from health care providers, and availability of physical spaces in the community and (for women who return to paid employment) in the workplace can provide more opportunities for mothers who want to breastfeed [ 18 , 33 , 44 ]. The findings from this review show, however, that access to these supports and resources vary greatly, and often the women who need them the most lack access to them [ 56 ].
While women make decisions about breastfeeding in light of their own personal circumstances, it is important to note that these circumstances are shaped by larger structural, social, and cultural factors. For instance, mothers may feel reluctant to breastfeed in public, which may stem from their familiarity with dominant cultural perspectives that label breasts as objects for sexualized pleasure [ 48 ]. The reviewed literature also showed that, despite the initial support, mothers who continue to breastfeed past the first year may be judged and scrutinized by others [ 47 ]. Tailoring public health care messaging to local communities with their own unique breastfeeding-related beliefs might help to create a larger social change in sociocultural norms regarding breastfeeding practices.
The literature included in this scoping review identified the importance of support from community services and health care providers in facilitating women’s breastfeeding behaviours [ 22 , 24 ]. Unfortunately, some mothers felt that the support and information they received was inadequate, impractical, or infused with conflicting messaging [ 28 , 44 ]. To make breastfeeding support more accessible to women across different social positions and geographic locations, it is important to acknowledge the need for the development of formal infrastructure that promotes breastfeeding. This includes training health care providers to help women struggling with breastfeeding and allocating sufficient funding for such initiatives.
Overall, this scoping review revealed the need for healthcare professionals to provide practical breastfeeding advice and realistic solutions to women encountering difficulties with breastfeeding. Public health messaging surrounding breastfeeding must re-invent breastfeeding as a “family practice” that requires collaboration between the breastfeeding mother, their partner, as well as extended family to ensure that women are supported as they breastfeed [ 8 ]. The literature also highlighted the issue of healthcare professionals easily giving up on women who encounter problems with breastfeeding and automatically recommending the initiation of formula use without further consideration towards solutions for breastfeeding difficulties [ 19 ]. While some challenges associated with breastfeeding are informed by local culture or health care policies, most of the barriers experienced by breastfeeding women are remarkably universal. Women often struggle with initiation of breastfeeding, lack of support from their significant others, and lack of appropriate places and spaces to breastfeed [ 25 , 26 , 33 , 39 ]. A change in public health messaging to a more flexible messaging that recognizes the challenges of breastfeeding is needed to help women overcome negative feelings associated with failure to breastfeed. Offering more personalized advice and support to breastfeeding mothers can improve women’s experiences and increase the rates of breastfeeding while also boosting mothers’ sense of self-efficacy.
Limitations
This scoping review has several limitations. First, the focus on “women’s experiences” rendered broad search criteria but may have resulted in the over or underrepresentation of specific findings in this review. Also, the exclusion of empirical work published in languages other than English rendered this review reliant on the papers published predominantly in English-speaking countries. Finally, consistent with Arksey and O’Malley’s [ 18 ] scoping review methodology, we did not appraise the quality of the reviewed literature. Notwithstanding these limitations, this review provides important insights into women’s experiences of breastfeeding and offers practical strategies for improving dominant public health messaging on the importance of breastfeeding.
Women who breastfeed encounter many difficulties when they initiate breastfeeding, and most women are unsuccessful in adhering to current public health breastfeeding guidelines. This scoping review highlighted the need for reconfiguring public health messaging to acknowledge the challenges many women experience with breastfeeding and include women’s social networks as a target audience for such messaging. This review also shows that breastfeeding supports and counselling are needed by all women, but there is also a need to tailor public health messaging to local social norms and culture. The role social institutions and cultural discourses have on women’s experiences of breastfeeding must also be acknowledged and leveraged by health care professionals promoting breastfeeding.
Availability of data and materials
All data generated or analysed during this study are included in this published article [and its supplementary information files].
Wolf JH. Low breastfeeding rates and public health in the United States. Am J Public Health. 2003;93(12):2000–2010. [cited 2021 Apr 21] Available from: http://ajph.aphapublications.org/doi/ https://doi.org/10.2105/AJPH.93.12.2000
World Health Organization, UNICEF. Global nutrition targets 2015: Breastfeeding policy brief 2014.
United Nations International Children’s Emergency Fund (UNICEF). Breastfeeding in the UK. 2019 [cited 2021 Apr 21]. Available from: https://www.unicef.org.uk/babyfriendly/about/breastfeeding-in-the-uk/
Semenic S, Loiselle C, Gottlieb L. Predictors of the duration of exclusive breastfeeding among first-time mothers. Res Nurs Health. 2008;31(5):428–441. [cited 2021 Apr 21] Available from: http://doi.wiley.com/ https://doi.org/10.1002/nur.20275
Hauck YL, Bradfield Z, Kuliukas L. Women’s experiences with breastfeeding in public: an integrative review. Women Birth. 2020;34:e217–27.
Hendaus MA, Alhammadi AH, Khan S, Osman S, Hamad A. Breastfeeding rates and barriers: a report from the state of Qatar. Int. J Women's Health. 2018;10:467–75 [cited 2021 Apr 20] Available from: /pmc/articles/PMC6110662/.
Google Scholar
Ogbo FA, Ezeh OK, Khanlari S, Naz S, Senanayake P, Ahmed KY, et al. Determinants of exclusive breastfeeding cessation in the early postnatal period among culturally and linguistically diverse (CALD) Australian mothers. Nutrients. 2019;11(7):1611 [cited 2021 Apr 21] Available from: https://www.mdpi.com/2072-6643/11/7/1611 .
Article Google Scholar
Ayton JE, Tesch L, Hansen E. Women’s experiences of ceasing to breastfeed: Australian qualitative study. BMJ Open. 2019;9(5):26234 [cited 2021 Apr 20] Available from: http://bmjopen.bmj.com/ .
Brown CRL, Dodds L, Legge A, Bryanton J, Semenic S. Factors influencing the reasons why mothers stop breastfeeding. Can J Public Heal. 2014;105(3):e179–e185. [cited 2021 Apr 20] Available from: https://link.springer.com/article/ https://doi.org/10.17269/cjph.105.4244
Sharma AJ, Dee DL, Harden SM. Adherence to breastfeeding guidelines and maternal weight 6 years after delivery. Pediatrics. 2014;134(Supplement 1):S42–S49. [cited 2021 Apr 21] Available from: www.pediatrics.org/cgi/doi/ https://doi.org/10.1542/peds.2014-0646H
Walters DD, Phan LTH, Mathisen R. The cost of not breastfeeding: Global results from a new tool. Health Policy Plan. 2019;34(6):407–17 [cited 2021 Apr 21] Available from: https://academic.oup.com/heapol/article/34/6/407/5522499 .
Friedman M. For whom is breast best? Thoughts on breastfeeding, feminism and ambivalence. J Mother Initiat Res Community Involv. 2009;11(1):26–35 [cited 2021 Apr 20] Available from: https://jarm.journals.yorku.ca/index.php/jarm/article/viewFile/22506/20986 .
Blixt I, Johansson M, Hildingsson I, Papoutsi Z, Rubertsson C. Women’s advice to healthcare professionals regarding breastfeeding: “offer sensitive individualized breastfeeding support” - an interview study. Int Breastfeed J 2019;14(1):51. [cited 2021 Apr 20] Available from: https://internationalbreastfeedingjournal.biomedcentral.com/articles/10.1186/s13006-019-0247-4
Obeng C, Dickinson S, Golzarri-Arroyo L. Women’s perceptions about breastfeeding: a preliminary study. Children. 2020;7(6):61 [cited 2021 Apr 21] Available from: https://www.mdpi.com/2227-9067/7/6/61 .
Choudhry K, Wallace LM. ‘Breast is not always best’: South Asian women’s experiences of infant feeding in the UK within an acculturation framework. Matern Child Nutr. 2012;8(1):72–87. [cited 2021 Apr 20] Available from: http://doi.wiley.com/ https://doi.org/10.1111/j.1740-8709.2010.00253.x
Da Silva TD, Bick D, Chang YS. Breastfeeding experiences and perspectives among women with postnatal depression: a qualitative evidence synthesis. Women Birth. 2020;33(3):231–9.
Kilanowski JF. Breadth of the socio-ecological model. J Agromedicine. 2017;22(4):295–7 [cited 2021 Apr 20] Available from: https://www.tandfonline.com/action/journalInformation?journalCode=wagr20 .
Arksey H, O’Malley L. Scoping studies: Towards a methodological framework. Int J Soc Res Methodol Theory Pract. 2005;8(1):19–32 [cited 2021 Apr 20] Available from: https://www.tandfonline.com/action/journalInformation?journalCode=tsrm20 .
Brown A, Lee M. An exploration of the attitudes and experiences of mothers in the United Kingdom who chose to breastfeed exclusively for 6 months postpartum. Breastfeed Med. 2011;6(4):197–204. [cited 2021 Apr 20] Available from: http://www.liebertpub.com/doi/ https://doi.org/10.1089/bfm.2010.0097
Morns MA, Steel AE, Burns E, McIntyre E. Women who experience feelings of aversion while breastfeeding: a meta-ethnographic review. Women Birth. 2021;34:128–35.
Jackson KT, Mantler T, O’Keefe-McCarthy S. Women’s experiences of breastfeeding-related pain. MCN Am J Matern Nurs. 2019;44(2):66–72 [cited 2021 Apr 20] Available from: https://journals.lww.com/00005721-201903000-00002 .
Burns E, Schmied V, Sheehan A, Fenwick J. A meta-ethnographic synthesis of women’s experience of breastfeeding. Matern Child Nutr. 2009;6(3):201–219. [cited 2021 Apr 20] Available from: http://doi.wiley.com/ https://doi.org/10.1111/j.1740-8709.2009.00209.x
Claesson IM, Larsson L, Steen L, Alehagen S. “You just need to leave the room when you breastfeed” Breastfeeding experiences among obese women in Sweden - A qualitative study. BMC Pregnancy Childbirth. 2018;18(1):1–10. [cited 2021 Apr 20] Available from: https://link.springer.com/articles/ https://doi.org/10.1186/s12884-017-1656-2
Asiodu IV, Waters CM, Dailey DE, Lyndon • Audrey. Infant feeding decision-making and the influences of social support persons among first-time African American mothers. Matern Child Health J. 2017;21:863–72.
Forster DA, McLachlan HL. Women’s views and experiences of breast feeding: positive, negative or just good for the baby? Midwifery. 2010;26(1):116–25.
Demirci J, Caplan E, Murray N, Cohen S. “I just want to do everything right:” Primiparous Women’s accounts of early breastfeeding via an app-based diary. J Pediatr Heal Care. 2018;32(2):163–72.
Furman LM, Banks EC, North AB. Breastfeeding among high-risk Inner-City African-American mothers: a risky choice? Breastfeed Med. 2013;8(1):58–67. [cited 2021 Apr 20]Available from: http://www.liebertpub.com/doi/ https://doi.org/10.1089/bfm.2012.0012
Cottrell BH, Detman LA. Breastfeeding concerns and experiences of african american mothers. MCN Am J Matern Nurs. 2013;38(5):297–304 [cited 2021 Apr 20] Available from: https://journals.lww.com/00005721-201309000-00009 .
Wambach K, Domian EW, Page-Goertz S, Wurtz H, Hoffman K. Exclusive breastfeeding experiences among mexican american women. J Hum Lact. 2016;32(1):103–111. [cited 2021 Apr 21] Available from: http://journals.sagepub.com/doi/ https://doi.org/10.1177/0890334415599400
Regan P, Ball E. Breastfeeding mothers’ experiences: The ghost in the machine. Qual Health Res. 2013;23(5):679–688. [cited 2021 Apr 21] Available from: http://journals.sagepub.com/doi/ https://doi.org/10.1177/1049732313481641
Hinsliff-Smith K, Spencer R, Walsh D. Realities, difficulties, and outcomes for mothers choosing to breastfeed: Primigravid mothers experiences in the early postpartum period (6-8 weeks). Midwifery. 2014;30(1):e14–9.
Palmér L. Previous breastfeeding difficulties: an existential breastfeeding trauma with two intertwined pathways for future breastfeeding—fear and longing. Int J Qual Stud Health Well-being. 2019;14(1) [cited 2021 Apr 21] Available from: https://www.tandfonline.com/action/journalInformation?journalCode=zqhw20 .
Francis J, Mildon A, Stewart S, Underhill B, Tarasuk V, Di Ruggiero E, et al. Vulnerable mothers’ experiences breastfeeding with an enhanced community lactation support program. Matern Child Nutr 2020;16(3):16. [cited 2021 Apr 20] Available from: https://onlinelibrary.wiley.com/doi/abs/ https://doi.org/10.1111/mcn.12957
Palmér L, Carlsson G, Mollberg M, Nyström M. Breastfeeding: An existential challenge - Women’s lived experiences of initiating breastfeeding within the context of early home discharge in Sweden. Int J Qual Stud Health Well-being 2010;5(3). [cited 2021 Apr 21] Available from: https://www.tandfonline.com/action/journalInformation?journalCode=zqhw20https://doi.org/ https://doi.org/10.3402/qhw.v5i3.5397
Grant A, Mannay D, Marzella R. ‘People try and police your behaviour’: the impact of surveillance on mothers and grandmothers’ perceptions and experiences of infant feeding. Fam Relationships Soc. 2018;7(3):431–47.
Thomson G, Ebisch-Burton K, Flacking R. Shame if you do - shame if you don’t: women’s experiences of infant feeding. Matern Child Nutr. 2015;11(1):33–46. [cited 2021 Apr 21] Available from: http://doi.wiley.com/ https://doi.org/10.1111/mcn.12148
Dietrich Leurer M, Misskey E. The psychosocial and emotional experience of breastfeeding: reflections of mothers. Glob Qual. Nurs Res. 2015;2:2333393615611654 [cited 2021 Apr 20] Available from: http://www.ncbi.nlm.nih.gov/pubmed/28462320 .
Fahlquist JN. Experience of non-breastfeeding mothers: Norms and ethically responsible risk communication. Nurs Ethics. 2016;23(2):231–241. [cited 2021 Apr 20] Available from: http://journals.sagepub.com/doi/ https://doi.org/10.1177/0969733014561913
Gross TT, Davis M, Anderson AK, Hall J, Hilyard K. Long-term breastfeeding in African American mothers: a positive deviance inquiry of WIC participants. J Hum Lact. 2017;33(1):128–139. [cited 2021 Apr 20] Available from: http://journals.sagepub.com/doi/ https://doi.org/10.1177/0890334416680180
Spencer RL, Greatrex-White S, Fraser DM. ‘I thought it would keep them all quiet’. Women’s experiences of breastfeeding as illusions of compliance: an interpretive phenomenological study. J Adv Nurs. 2015;71(5):1076–1086. [cited 2021 Apr 21] Available from: http://doi.wiley.com/ https://doi.org/10.1111/jan.12592
Twamley K, Puthussery S, Harding S, Baron M, Macfarlane A. UK-born ethnic minority women and their experiences of feeding their newborn infant. Midwifery. 2011;27(5):595–602.
PubMed Google Scholar
Lutenbacher M, Karp SM, Moore ER. Reflections of Black women who choose to breastfeed: influences, challenges, and supports. Matern Child Health J. 2016;20(2):231–9.
Dowling S, Brown A. An exploration of the experiences of mothers who breastfeed long-term: what are the issues and why does it matter? Breastfeed Med. 2013;8(1):45–52. [cited 2021 Apr 20] Available from: http://www.liebertpub.com/doi/ https://doi.org/10.1089/bfm.2012.0057
Fox R, McMullen S, Newburn M. UK women’s experiences of breastfeeding and additional breastfeeding support: a qualitative study of baby Café services. BMC Pregnancy Childbirth 2015;15(1):147. [cited 2021 Apr 20] Available from: http://bmcpregnancychildbirth.biomedcentral.com/articles/ https://doi.org/10.1186/s12884-015-0581-5
Spencer B, Wambach K, Domain EW. African American women’s breastfeeding experiences: cultural, personal, and political voices. Qual Health Res. 2015;25(7):974–987. [cited 2021 Apr 21] Available from: http://journals.sagepub.com/doi/ https://doi.org/10.1177/1049732314554097
McBride-Henry K. The influence of the They: An interpretation of breastfeeding culture in New Zealand. Qual Health Res. 2010;20(6):768–777. [cited 2021 Apr 21] Available from: http://journals.sagepub.com/doi/ https://doi.org/10.1177/1049732310364220
Newman KL, Williamson IR. Why aren’t you stopping now?!’ Exploring accounts of white women breastfeeding beyond six months in the east of England. Appetite. 2018 Oct;1(129):228–35.
Dowling S, Pontin D. Using liminality to understand mothers’ experiences of long-term breastfeeding: ‘Betwixt and between’, and ‘matter out of place.’ Heal (United Kingdom). 2017;21(1):57–75. [cited 2021 Apr 20] Available from: http://journals.sagepub.com/doi/ https://doi.org/10.1177/1363459315595846
Payne D, Nicholls DA. Managing breastfeeding and work: a Foucauldian secondary analysis. J Adv Nurs. 2010;66(8):1810–1818. [cited 2021 Apr 21] Available from: http://doi.wiley.com/ https://doi.org/10.1111/j.1365-2648.2009.05156.x
Keely A, Lawton J, Swanson V, Denison FC. Barriers to breast-feeding in obese women: a qualitative exploration. Midwifery. 2015;31(5):532–9.
Afoakwah G, Smyth R, Lavender DT. Women’s experiences of breastfeeding: A narrative review of qualitative studies. Afr J Midwifery Womens Health. 2013 ;7(2):71–77. [cited 2021 Apr 21] Available from: https://www.magonlinelibrary.com/doi/abs/ https://doi.org/10.12968/ajmw.2013.7.2.71
Símonardóttir S. Getting the green light: experiences of Icelandic mothers struggling with breastfeeding. Sociol Res Online. 2016;21(4):1.
Szafranska M, Gallagher DL. Polish women’s experiences of breastfeeding in Ireland. Pract Midwife. 2016;19(1):30–2 [cited 2021 Apr 21] Available from: https://europepmc.org/article/med/26975131 .
Pratt BA, Longo J, Gordon SC, Jones NA. Perceptions of breastfeeding for women with perinatal depression: a descriptive phenomenological study. Issues Ment Health Nurs. 2020;41(7):637–644. [cited 2021 Apr 21] Available from: https://www.tandfonline.com/doi/abs/ https://doi.org/10.1080/01612840.2019.1691690
Durmazoğlu G, Yenal K, Okumuş H. Maternal emotions and experiences of mothers who had breastfeeding problems: a qualitative study. Res Theory Nurs Pract. 2020;34(1):3–20. [cited 2021 Apr 20] Available from: http://connect.springerpub.com/lookup/doi/ https://doi.org/10.1891/1541-6577.34.1.3
Burns E, Triandafilidis Z. Taking the path of least resistance: a qualitative analysis of return to work or study while breastfeeding. Int Breastfeed J. 2019;14(1):1–13.
Download references
Acknowledgements
The authors would like to acknowledge the assistance of Jackie Stapleton, the University of Waterloo librarian, for her assistance with developing the search strategy used in this review.
Not applicable.
Author information
Authors and affiliations.
School of Public Health Sciences, University of Waterloo, 200 University Ave West, Waterloo, ON, N2L 3G1, Canada
Bridget Beggs, Liza Koshy & Elena Neiterman
You can also search for this author in PubMed Google Scholar
Contributions
BB was responsible for the formal analysis and organization of the review. LK was responsible for data curation, visualization and writing the original draft. EN was responsible for initial conceptualization and writing the original draft. BB and LK were responsible for reviewing and editing the manuscript. All authors read and approved the final manuscript.
Authors’ information
BB is completing her Bachelor of Science (BSc) degree at the School of Public Health Sciences at the University of Waterloo.
LK is completing her Bachelor of Public Health (BPH) degree at the School of Public Health Sciences at the University of Waterloo.
EN (PhD), is a continuing lecturer at the School of Public Health Sciences at the University of Waterloo. Her areas of expertise are in women’s reproductive health and sociology of health, illness, and healthcare.
Corresponding author
Correspondence to Bridget Beggs .
Ethics declarations
Ethics approval and consent to participate, consent for publication, competing interests.
The authors declare that they have no competing interests.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/ . The Creative Commons Public Domain Dedication waiver ( http://creativecommons.org/publicdomain/zero/1.0/ ) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
Reprints and permissions
About this article
Cite this article.
Beggs, B., Koshy, L. & Neiterman, E. Women’s Perceptions and Experiences of Breastfeeding: a scoping review of the literature. BMC Public Health 21 , 2169 (2021). https://doi.org/10.1186/s12889-021-12216-3
Download citation
Received : 23 June 2021
Accepted : 10 November 2021
Published : 26 November 2021
DOI : https://doi.org/10.1186/s12889-021-12216-3
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Breastfeeding
- Experiences
- Public health
BMC Public Health
ISSN: 1471-2458
- General enquiries: [email protected]
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
Preview improvements coming to the PMC website in October 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- Front Public Health
Interventions for promoting and optimizing breastfeeding practices: An overview of systematic review
Mahalaqua nazli khatib.
1 Global Evidence Synthesis Initiative, Division of Evidence Synthesis, Jawaharlal Nehru Medical College, Datta Meghe Institute of Higher Education and Research, Wardha, Maharashtra, India
Abhay Gaidhane
2 Centre of One Health, School of Epidemiology and Public Health, Jawaharlal Nehru Medical College, Datta Meghe Institute of Higher Education and Research, Wardha, Maharashtra, India
Shilpa Upadhyay
3 Department of Research and Development, Datta Meghe Institute of Higher Education and Research, Wardha, Maharashtra, India
Shital Telrandhe
Deepak saxena.
4 i Health Consortium, Department of Epidemiology, Indian Institute of Public Health, Gandhinagar, Gujarat, India
Padam Prasad Simkhada
5 Global Consortium of Public Health Research, School of Human and Health Sciences, University of Huddersfield, Huddersfield, United Kingdom
Shailendra Sawleshwarkar
6 Postgraduate Coursework Programs, Faculty of Medicine and Health, Sydney Medical School, The University of Sydney Institute for Infectious Diseases (Sydney ID), University of Sydney, Camperdown, NSW, Australia
Syed Zahiruddin Quazi
7 South Asia Infant Feeding Research Network (SAIFRN), Jawaharlal Nehru Medical College, Datta Meghe Institute of Higher Education and Research, Wardha, Maharashtra, India
Associated Data
The original contributions presented in the study are included in the article/supplementary material, further inquiries can be directed to the corresponding author.
Optimal breastfeeding (BF) practices are essential for child survival and proper growth and development. The purpose of this overview is to evaluate the effectiveness of different interventions for promoting and optimizing breastfeeding.
We included systematic reviews (SRs) [including trials from Low-Income (LICs) and Low Middle-Income countries (LMICs)] that have evaluated the effect of various interventions for promoting and optimizing breastfeeding and excluded non-systematic reviews, and SRs based on observational studies. We searched various electronic databases. We followed the standard methodology as suggested by the Cochrane Handbook for Systematic Reviews of Interventions. Two sets of reviewers undertook screening followed by data extraction and assessment of the methodological quality of included SRs.
We identified and screened 1,002 Cochrane SRs and included six SRs in this overview. Included SRs reported only two of the primary outcomes, early initiation of breastfeeding (EIBF) and/or exclusive breastfeeding (EBF). None of the included SR reported continued BF up to 2 years of age. The results were evaluated using two major comparisons groups: BF intervention against routine care and one type of BF intervention vs. other types of BF intervention. Overall results from included SRs showed that there were improvements in the rates of EIBF and EBF among women who received BF intervention such as BF education sessions and support compared to those women who received only standard care. However, BF intervention via mobile devices showed no improvements. In Target Client Communication (TCC) via mobile devices intervention group, no significant improvements were reported in BF practices, and also the reported evidence was of very low certainty.
Community Based Intervention Packages (CBIP) delivered to pregnant and reproductive-age women during their Antenatal care (ANC) and/or Postnatal care (PNC) periods by Ancillary Nurse-Midwives reported the highest improvement in EIBF compared to women who received standard care. However, insufficient evidence was reported to suggest that BF intervention showed improvements in EBF in both the comparison groups. This overview highlighted the gaps in primary research regarding the uncertainty about the settings such as LICs or LMICs, lack of evidence from LMICs, and also identified gaps in the availability of reliable up-to-date SRs on the effects of several BF interventions to promote and optimize practices.
Systematic review registration
https://www.crd.york.ac.uk/prospero/display_record.php?ID=CRD42020174998 , PROSPERO [CRD42020174998].
Description of the condition
Optimal breastfeeding practices which include early initiation of breastfeeding (EIBF) within 1 h of birth, exclusive breastfeeding (EBF) for the first 6 months of age, and continued breastfeeding (CBF) for 2 years of age or beyond with complementary foods are vital for child survival and proper growth and development.
Globally, due to under-nutrition, more than 50% of child mortality has been ascribed to insufficient breastfeeding and/or complementary feeding ( 1 ). Children with inappropriate breastfeeding are more prone to develop infections such as respiratory infections ( 2 , 3 ), gastroenteritis ( 2 – 4 ), and otitis media ( 3 , 5 ), leading to increased hospitalization ( 6 ), morbidity, and mortality ( 7 – 10 ). Inadequately breastfed children are at elevated risk of juvenile diabetes and obesity ( 11 ) and have compromised intelligence ( 11 – 14 ), educational ( 15 ), behavioral ( 16 ), and neurodevelopmental outcomes ( 8 ). Evidence also indicates that women who inappropriate breastfeed their babies are more prone to develop breast cancer, ovarian cancer, osteoporosis, and diabetes ( 3 , 17 – 19 ).
Breastfeeding provides an economic advantage to society in addition to short- and long-term maternal and child health benefits ( 1 , 20 , 21 ). If 90% of US families abide by exclusively breastfeeding for 6 months, the United States would save 13 billion USD per year and avert surplus 911 mostly infants deaths ( 22 ). Investing in interventions to promote EIBF, EBF and longer BF durations may be cost-effective ( 22 ).
In the year 2003, the World Health Organization (WHO) recommended that babies should be exclusively breastfed throughout the initial 6 months of age and continued for at least 2 years of age ( 23 ). According to the CDC's 2018 Breastfeeding Report Card, fewer than half of newborns in the United States were exclusively breastfed for 3 months, and around a quarter were exclusively breastfed for 6 months ( 24 ). In many other high-income countries, initiation rates continued to be slightly low, particularly in low-income groups ( 24 ). A survey data from the South-Asian countries showed that EIBF and EBF escalated in India, Nepal, and Bangladesh from 1990 to 2016 ( 25 ). CBF remained fairly constant across South Asia ( 25 ). Improvement in optimal breastfeeding practices is of particular concern in Pakistan and Afghanistan ( 25 ). This data indicates that mothers may not be receiving the needed breastfeeding support from family members, health care providers, and employers.
Description of the interventions
There is currently a range of different interventions for supporting breastfeeding that may target pregnant women, their spouses, family members, the health service, or wider communities.
Telephone-based peer support intervention comprises health education imparted through mobile or telephones to women in ante-natal or post-natal periods. It is effective in initiating and maintaining breastfeeding and improving satisfaction with feeding ( 26 , 27 ). Interventions aimed to a woman alone or her family members comprise health education imparted through skills training, mother-baby contact, and peer support and that may be offered to one-on-one or groups, in formal or informal settings and be delivered by maternity support workers, health professionals, peers, or social media ( 28 ). Peer support interventions that support and promote breastfeeding entails communication between a pregnant woman and a woman with breastfeeding experience from the same background ( 29 ). This form of mother-to-mother assistance has been found to boost initiation, exclusivity, and/or continuation rates of BF ( 27 , 30 , 31 ). Peer supporters can undertake training, can be paid or unpaid can be separated or incorporated into the healthcare team ( 32 ). Mass or social media campaigns are initiatives directed at the general public that, when combined with other interventions, show some success in encouraging breastfeeding ( 33 ).
WHO/United Nations International Children's Emergency Fund (UNICEF), Baby-Friendly Hospital Initiative (BFHI) also referred to as the Baby-Friendly Initiative (BFI) has been proven to be the most effective health care intervention for promoting breastfeeding initiation. The BFHI/BFI is a comprehensive, systematic program that includes organizational change ( 34 , 35 ). It includes execution of the Ten Steps to effective breastfeeding which involve staff training policies, breastfeeding promotion, and support, infant formula, restricting the use of teats and pacifiers, and keeping mothers and infants together ( 36 ). The WHO/UNICEF Baby-friendly Hospital Initiative has been shown to improve breastfeeding rates ( 37 – 39 ) however ambiguity remains regarding effective approaches to improve BF in community health care services ( 40 , 41 ). According to reviews, interventions such as counseling and health education offered by healthcare and non-healthcare professionals as well as peer support have escalated the percentage of women who early initiate BF, exclusively breastfeed, and continue to breastfeed for a longer duration ( 26 , 32 , 33 , 35 , 42 , 43 ).
How the interventions might work
Breast milk is regarded as the best and only source of nutrition for all newborns from the time of birth to the age of 6 months. The nutritional benefits are due to potent immune boosters and a specialized composition that meets babies' proper growth and development requirements ( 13 ). Breast milk includes growth factors, hormones, cytokines, cells, etc., and offers several benefits over cow's milk or soy protein infant formulae ( 19 ). In the health setting, peer support is a “created” social interaction that aims to improve health care delivery ( 26 ). Peer volunteers are trained to offer “emotional, informational, and appraisal” support to improve breastfeeding outcomes by boosting wellbeing and social connectivity. By using their experiential expertise and training, the peers may provide a number of solutions and guidance on parenting and feeding challenges confronting new mothers ( 27 ). Volunteer training emphasizes the importance of assisting the mother in making her own decisions and referring the mother to professional help when necessary ( 27 ).
Why it is important to do this overview
The key step to meet WHO recommendations for breastfeeding is the escalating rates of early initiation of breastfeeding and realizing the probable role of breastfeeding in health improvement, minimizing the economic burden of illness, and minimizing health disparities. A variety of individual studies and systematic reviews have assessed a comprehensive range of support interventions for breastfeeding. However, we still need to learn more about what works best to support breastfeeding. There is a need to evaluate all potentially associated BF interventions for systematically promoting breastfeeding practices.
To the best of our knowledge, no published overview has assembled and summarized the evidence from systematic reviews on breastfeeding interventions, to aid health professionals, consumers, researchers, funding bodies, policymakers/guideline developers in decision-making and evidence translation. The aim of this overview is to assess interventions for promoting women to breastfeed, to assess their efficacy in terms of changes in the percentage of women who early initiate breastfeeding, who breastfeed exclusively, and who continue to breastfeed their children up to 2 years of age. We will identify existing knowledge gaps and can provide clear suggestions and recommendations for future systematic reviews and clinical research.
Primary objective
The objective of this overview is to summarize the evidence from systematic reviews on the impact of different interventions designed to promote and optimize early initiation of breastfeeding (EIBF), exclusive breastfeeding (EBF) for the first 6 months of life and continued breastfeeding up to 2 years of age and to assess the effects of these interventions on associated outcomes, including infant mortality.
Secondary objectives
- To describe different types of breastfeeding support (evaluated in systematic reviews) in terms of the timing and intensity of interventions and the settings (differential impact on different subgroups of the population) in which they have been used.
- To assess whether interventions delivered in both antenatal (ANC) and postnatal periods (PNC) are more effective than those delivered only in the postnatal period.
- To compare the efficiency of different care providers (who had given interventions).
- To explore appropriate strategy for supporting women who desire early initiation of breastfeeding, exclusive breastfeeding for the first 6 months of life, and continued breastfeeding up to 2 years of age.
Criteria for considering reviews for inclusion
Types of studies.
We included only Cochrane systematic reviews (that had included randomized clinical trials including cluster or quasi-randomized trials) evaluating the effect of various interventions for promoting and optimizing EIBF, EBF for the first 6 months of life, and continued breastfeeding up to 2 years of age. We excluded non-Cochrane SRs, non-systematic reviews, and SRs based on observational studies. We included the updated SRs. There were no restrictions on the language or publication status of systematic reviews.
Types of participants
Participants included were pregnant women, women who were breastfeeding their babies, and women who are willing to breastfeed in the future. We included SRs including trials from LICs and LMICs as defined by World Bank (based on Atlas Gross national per capita estimates). We excluded SRs based on trials from HIC and UMICs. However, we included SRs that had participants irrespective of countries as defined by the World Bank (LICs, LMICs, HICs, UMICs), but reported separate data for LICs and LMICs as subgroup analysis. We imposed no restriction on race/ethnicity, and the type of settings from where the participants were recruited. SRs focussed specifically on women and children with additional care needs or a specific health problem, e.g., mothers with diabetes, HIV/AIDS or infants with cleft palate, or premature babies, were excluded from this overview.
Types of interventions
“Support” interventions eligible for this overview may range from m-health, Behaviour Change Communication (BCC), health education, health systems and policy interventions like Health Sector Initiatives (HIS), Infant Young Childhood Feeding (IYCF), specialized clinics, workplace interventions, positive parenting interventions, and/or combination of interventions. We included SRs in which the intervention occurred only in the postnatal period (PNC) or in conjunction with an antenatal (ANC) component. Intervention could be offered by health professionals laypeople, or peers, in either hospital or community settings in LICs and LMICs.
Types of comparisons
We included SRs that have compared breastfeeding support intervention vs. routine care or one form of intervention vs. the other.
Types of outcomes
1. Primary outcomes
- Early initiation of breastfeeding.
- Exclusive breastfeeding for the first 6 months of life.
- Continued breastfeeding up to 2 years of age.
2. Secondary outcomes
- Acceptability: Any measure of acceptability.
- Satisfaction: Any measure of satisfaction.
Search methods for identification of reviews
We searched the Cochrane Database for Systematic Reviews (CDSR) for identifying Cochrane reviews and additional databases like PubMed, DARE, CINAHL, PsychINFO, Google Scholar for non-Cochrane Reviews if deemed necessary. We searched the Cochrane Pregnancy and Childbirth Editorial Base and Cochrane Child Health Editorial Base to seek any relevant reviews or review updates in progress, and The International Prospective Register of Systematic Reviews (PROSPERO) for SR protocols at https://www.crd.york.ac.uk/prospero/ . We contacted the Protocol authors for a pre-publication version of SRs. Additionally; we searched the reference lists of retrieved studies. We used medical subject heading and text word terms and tailor the search to individual databases. We used keywords and synonyms to sensitize the search. We searched all databases from their creation to the present and we did not restrict the language of publication status.
The protocol of this overview of systematic review was registered in PROSPERO (International prospective registration of systematic reviews) https://www.crd.york.ac.uk/prospero/display_record.php?ID=CRD42020174998 .
The registration number of the proposed protocol is CRD42020174998. We conducted our search on April 28, 2021 and update it on November 13, 2021, to include newly added SRs.
The search strategy for CENTRAL was as:
Search Strategy for CENTRAL via Cochrane library
#1 “breast feed * ”
#2 “breast fed”
#3 “breastfeed * ”
#4 “breast-fed”
#5 MeSH descriptor: [Breast Feeding] explode all trees
#6 #1 Or #2 OR #3 OR #4 OR #5.
Data collection and analysis
We followed the standard methodology as suggested by Part 1: Chapter V of Cochrane Handbook for Systematic Reviews of Interventions ( 44 ).
Selection of reviews
Two reviewers initially screened the titles and abstracts of all the included SRs using the “Rayyan” software ( 45 ) and all seemingly eligible SRs were moved for the next step screening on full texts. A PRISMA diagram ( 46 ) was prepared to keep track of the search process. Disagreements amongst the primary reviewers were resolved by discussion or consultation with a third reviewer. We presented a reason for exclusion where relevant.
Data extraction and management
One reviewer had extracted data from included systematic reviews into a Microsoft Excel file using a pre-designed data extraction form, which was pilot-tested for its suitability and usability. A second reviewer had checked the data extraction. The discrepancies were resolved through discussion or consultation with a third reviewer. We had created “Characteristics of Reviews” tables for both included and excluded reviews including the following information:
- Basic review information (review title, author, last assessed as up-to-date).
- Study information (number of included trials, the sample size in range).
- Population (settings, age, demographics, specific definitions of population, inclusion criteria, and other important participant characteristics).
- Interventions (type, frequency, intensity, duration, personnel delivering the intervention).
- Comparison.
- Outcome measures for which data are reported (for each prespecified outcome: Outcomes reported, the definition of the outcome, number of trials and participants for each outcome; time of measurement of outcome, and the reported effect estimate).
Wherever possible, we contacted review authors to clarify data included in systematic reviews or to inquire about missing data. We had attempted to include only one review per intervention to avoid the duplication of evidence and resultant double-counting of trial data, by including only the most current and inclusive systematic review on a given intervention. All the included SRs varied in interventions.
We made decisions transparent in the main text as well as in tables for the overview. Data extraction had driven by well-defined review questions and not by the individual review data. We extracted additional data from original trials for enhancing the quality of the overview. Where the data was not presented in the required format, we re-extracted the data from original SRs by using Review Manager (RevMan).
Assessment of methodological quality of included reviews
Quality of included reviews.
One reviewer assessed the methodological quality of included SRs with the Revised Assessment of Multiple Systematic Reviews (R-AMSTAR) tool ( 47 ), and a second reviewer checked these assessments for accuracy. Any disagreements amongst the primary reviewers were resolved by discussion or consultation with a third reviewer.
The R-AMSTAR tool consisted of the following questions to be answered with either “yes,” “no,” or “unclear.” One point was awarded for every question answered “yes” for the highest possible score of 11. High-quality reviews score 8 or higher; moderate-quality score 4–7; low-quality systematic reviews score 3 or fewer “yes” answers.
- Was an “a priori” design provided?
- Was there duplicate study selection and data extraction?
- Was a comprehensive literature search performed?
- Was the status of publication (i.e., gray literature) used as an inclusion criterion?
- Was a list of studies (included and excluded) provided?
- Were the characteristics of the included studies provided?
- Was the scientific quality of the included studies assessed and documented?
- Was the scientific quality of the included studies used appropriately in formulating conclusions?
- Were the methods used to combine the findings of studies appropriate?
- Was the likelihood of publication bias assessed?
- Was the conflict of interest stated?
We excluded systematic reviews that did not meet the minimum quality standards of a rating of at least 4. We recorded the R-AMSTAR assessments as a tables to the overview.
Quality of included studies within reviews
We reported and not reassessed the “Risk of bias” of included trials in systematic reviews as given by authors of SRs.
Quality of evidence in included reviews
We reported the quality of evidence of relevant outcomes (GRADE assessments) as presented in the “Summary of findings” tables of the included SRs; if provided. We did not exclude evidence of “low” or “very low” quality.
Data synthesis
We organized the evidence in texts and tables according to each of our pre-specified outcomes, rather than by intervention. We concentrated primarily on describing and classifying the intervention and its efficacy. We created a data synthesis table for each review that included the following outcomes: characteristics of included systematic reviews, summary effect estimates, and the GRADE assessments. Toward the end of data extraction, we further chalked out the process of structure, categorization, and analysis of tables. One reviewer had created data synthesis tables and another overview author checked the tables for accuracy. We had resolved the discrepancies by discussion and consultation with another reviewer. We compared the pooled estimates of effectiveness for each intervention to the comparator in SRs that contained meta-analyses. We presented the data by the outcome and not by intervention in texts and tables. If data permits, we had chosen to use a fixed-effects model when the data was not heterogeneous or use the random effects model in presence of heterogeneity. We tried to present the data as risk ratio for dichotomous outcomes and Mean Difference (MD) for continuous outcomes. Where the data was not presented in the required format, we re-extracted the data from original SRs by using Review Manager (RevMan). Where the systematic reviews did not include meta-analyses; we incorporated brief narrative assessments.
“Effectiveness statement”, We combined the GRADE assessment with the R-AMSTAR rating in order to summarize all intervention decisions in a single, concise judgement ( 48 ).
Analysis of subgroups or subsets
Based on the availability of data, we made appropriate categorizations of results in terms of the region (rural/urban), population subgroup, and type of intervention.
Summarizing the results
We summarized the results based on the outcome, type of interventions, and quality of evidence.
Search results
We identified and screened a total of 1,002 records from the Cochrane Database of Systematic Reviews (CDSR), written in the English language on interventions for pregnant women or women of reproductive age to promote and optimize breastfeeding practices. We excluded 980 systematic reviews (SRs) after the screening of title and abstract and screened 22 SRs full-texts for eligibility. Then, after excluding 16 SRs, we included six SRs that matched our inclusion criterion. Three of the six included SRs ( 43 , 49 , 50 ) were the updates of earlier reviews ( 51 – 53 ). We documented the selection process in the form of a PRISMA Flow diagram ( Figure 1 ).

PRISMA flow diagram.

Description of included studies
Details of included systematic reviews.
We examined six SRs ( 42 , 43 , 49 , 50 , 54 , 55 ) from the Cochrane database. Included SRs were aimed to promote BF practices such as EIBF, EBF, and continued BF for up to 2 years, etc. All the included SRs followed randomized controlled trials (RCTs), cluster-randomized trials, or quasi-randomized trials as their research design. Except for one SR ( 49 ), all five SRs were published on and after 2015, Two of the six SRs ( 50 , 54 ) included participants exclusively from LMIC or LIC, whereas the other three SRs ( 42 , 43 , 55 ) included participants from a range of low to high-income countries, although we extracted the data solely from LIC/LMIC. Of the six included SRs, one SR ( 49 ) addressed interventions delivered in the workplace to encourage BF practices although there was no study reported related to interventions delivered at the workplace to support BF. We have presented a comparison of the characteristics of the included studies in Table 1 .
Characteristics of included studies.
| Lumbiganon et al. ( ) | 1st March 2016 | No. of trials: 24 (two studies from LMIC) Total: 390 IG: 196 CG: 194 | Cluster RCT | Women attending monthly microcredit meetings | : Monthly BF education + weekly cell phone messages : Multiple methods of BF education (weekly cell phone BF messages and monthly face-to-face BF information) | Standard care | 1. EIBF 2. EBF at 3 and 6 months | Insufficient evidence to support that any type of BF education session vs. SC improved EIBF. |
| Lassi et al. ( ) | 2nd May 2017 | No. of trials: 33 : 1,26,375 | 1. Community-based-RCT 2. Cluster-RCT 3. Quasi-RCT | Pregnant women, mothers of neonates, women of reproductive age, caregivers | : Any combination of CHEI and any ANC : HCP or CHW : CHEI includes 1. Promotion of routine ANC 2. Maternal health education 3. Promotion of EIBF and EBF 4. KMC 5. Newborn resuscitation 6. Management of neonatal infections 1. One-to-one counseling 2. Group counseling 3. Mass media | Usual health services | 1. EIBF | Any combination of CHEI during any period (ANC/PNC) given to mothers or family members or both were found to improve BF practices. |
| Palmer et al. ( ) | July 2019 | No. of trials: 11 (four from LMICs and 1 from LIC) 5,497 (from LMICs and LIC) | RCTs | Pregnant and postpartum mother's and caregivers | : TCC mobile devices HCW : Delivered TCC mobile devices to improve maternal, new-born or child health or a combination of both | 1.Standard care 2. TCC non-digital communication 3. Digital non-targeted communication | 1. EBF | No improvement was reported in BF practices as 100% of women were involved in exclusive breastfeeding |
| Balogun et al. ( ) | 29th February 2016 | No. of trials: 28 (three from LMICs and 1 from LIC) : Nicaragua: unclear Malawi: 55,931 Nigeria: 461 Ghana: NR | RCTs, Cluster-RCTs | Pregnant and reproductive age group ( , – ) group women from LIC (Malawi) and LMIC (Nicaragua, Nigeria, and Ghana) | : BF education and support and Early mother-infant contact Non-HCPs (women's group, peer counselors) : Education and support on BF education. | Standard care | 1. EIBF | In LIC, BF interventions provided by non-HCPs had reported improvements in EIBF rates |
| Lassi and Bhutta ( ) | 25 May 2014 | No. of trials: 26 : Total: 72.464 IG: 37,813 CG: 34,651 | Community-based RCT, cluster RCT, quasi-RCT | Pregnant and reproductive age group women from developing countries | : CBIP : ANMs : CBIP including additional training of LHW/visitor, community midwives, CHW/VHW, facilitators, or TBAs in maternal care. | Usual maternal and newborn care services | 1. EIBF within 1 h of birth | CBIP were found to improve BF practices |
| Abdulwadud and Snow ( ) | 2 August 2012 | No included studies and no participants were recruited | RCTs, Cluster or quasi RCTs | Women in full-time or part-time employment in both private and public sectors return to paid work after giving birth. | : interventions to support BF at the workplace : Any type of workplace strategy, to encourage, assist and support BF practices for women returning to work after giving birth. | No intervention or two or more workplace interventions against each other. | No outcomes reported | No conclusion can be drawn |
LMIC, low middle income country; LIC, low income country; IG, intervention group; CG, control group; RCTs, randomized controlled trials; ANC, antenatal care; PNC, postnatal care; LC, lactation consultation; SC, standard care; BF, breastfeeding; EIBF, early initiation of breastfeeding; EBF, exclusive breastfeeding; CHEI, community health educational intervention; HCP, health care professionals; CHW, community health workers; VHW, village health workers; KMC, kangaroo mother care; HCW, health care workers; TCC, targeted client communication; HBC, health behavior change; CBIP, community based intervention packages; ANM, ancillary nurse-midwives; LHW, lady health workers; TBA, traditional birth attendants; NR, not reported.
Details of participants in included SRs
Six of the included SRs contributed data for analysis and reported interventions to promote breastfeeding practices. Lumbiganon et al. ( 43 ), conducted an SR on women attending monthly microcredit meetings. Pregnant women, mothers of neonates, women in their reproductive age, mothers in their postpartum period, partners/spouses, or family members exclusively or mostly from LMICs or LICs were all the recipients of the BF interventions in four included SRs ( 42 , 50 , 54 , 55 ). In addition, Abdulwadud et al. ( 49 ) performed an SR that targeted women in their full-time or part-time employment in both the commercial and public sectors who were returning to paid work following maternity break. Two of the six SRs ( 50 , 54 ) included participants mainly from LMIC or LIC, the other three SRs ( 42 , 43 , 55 ) included participants from a range of low to high-income countries although we retrieved the data solely from LIC/LMIC. Whereas, one of the SR ( 49 ) did not include any study. The number of participants included in the SRs ranged from 390 to 1,26,375. In the included SRs, participants were recruited from antenatal and/or postnatal phases. Four of the included SRs acknowledged the duration of the intervention ( 42 , 50 , 54 , 55 ). The other two SRs, on the other hand, did not specify the duration ( 49 , 51 ).
Details of interventions in included SRs
All SRs included in this overview had interventions aimed at optimizing and promoting BF practices, five SRs ( 42 , 43 , 50 , 54 , 55 ) evaluated the effect of educational interventions, and one SR ( 49 ) addressed support interventions for BF practices (including physical facilities, lactation breaks, creches, and nurseries). BF Interventions in the included SRs were delivered by personnel from government, non-governmental, and private organizations ( 54 ), health system or health workers ( 55 ), non-healthcare professionals (women's group peer counselors) ( 42 ), and female ancillary nurse midwives (ANMs) ( 50 ). Two of the included SRs ( 43 , 49 ) did not provide any information regarding the personnel who delivered the BF interventions.
Lumbiganon et al. ( 43 ) conducted a review on BF interventions which included weekly cell phone BF text and voice messages to cell phone and monthly face-to-face BF information delivered to women attending monthly microcredit meetings ( 43 ). Another review conducted by Lassi et al. ( 54 ), focussed on Community Health Education Interventions (CHEI) based on maternal and child health such as group counseling, one-to-one counseling, mass media (television, radio, cellular messages, brochures, newspaper, banners, etc.) or any combination of the above methods delivered to mothers or family members by the government, non-governmental organizations, and private providers. Palmer et al. ( 55 ) conducted an SR in both HICs and LICs settings and addressed Targeted Client Communication (TCC) via mobile devices delivered to pregnant women and parents of young children by the health system or health workers. An SR conducted by Balogun et al. ( 42 ) addressed any intervention such as BF education and support that promotes BF practices such as EIBF and EBF, delivered to pregnant women and reproductive age group women by women's group peer counselors. Lassi and Bhutta ( 50 ) promoted additional training (including lectures supervised hands-on training) of community midwives, lady health workers or visitors, community or village health workers, traditional birth attendants (TBAs), or facilitators in maternal care during pregnancy, delivery, and the postpartum period offered to pregnant and women of reproductive age by Auxillary nurse midwives (ANMs) from local government and non-government organizations. According to Abdulwadud and Snow ( 49 ), any form of workplace approach to promote, support, and assist BF practices for women returning to work after maternity leave is considered as workplace intervention. This SR, on the other hand, found no studies on workplace interventions to support BF.
Four of the six included SRs ( 42 , 43 , 50 , 54 ) included comparison groups that were either standard or routine care whereas one SR ( 55 ) had comparison groups both as standard care and another type of intervention which includes TCC with non-digital communication (face-to-face communication, pamphlets, letters). And one SR ( 49 ) had two or more workplace interventions compared against each other or no intervention.
Details of outcomes in included SRs
All six included SRs evaluated the impact of BF interventions on BF practices such as EIBF, EBF, and continued BF up to 2 years of age. Included SRs reported only two of the primary outcomes, EIBF and/or EBF in this overview. The third primary outcome i.e., continued BF up to 2 years of age as well as secondary outcomes such as acceptability and satisfaction were not assessed in any of the included SRs. The results were evaluated using two major comparisons groups: BF intervention against routine care and one type of BF intervention vs. other types of BF intervention. Four SRs ( 42 , 43 , 50 , 54 ) assessed the effect of interventions on EIBF whereas two SRs ( 43 , 55 ) evaluated the effect of interventions on EBF in BF intervention vs. routine care comparison group. Only one SR ( 55 ) reported EBF in another group i.e., one BF intervention vs. another form of BF intervention comparison group.
We retrieved relevant outcomes (reported as events and population size as well as RR) and categorized them for analysis based on the results mentioned below in Tables 2 , ,3 3 .
Findings of included studies.
| EIBF (early Initiation of breastfeeding) | ( ) | : 1 cluster-randomized trial (LMIC) : 390 | RR = 1.44 (95% CI = 1.06, 1.97) = 23.3% | High | NR | Insufficient evidence to suggest that any antenatal BF education was found to be more effective than standard care for improving EIBF |
| ( ) | : 11 RCTs : 72,464 | RR = 1.93 (95% CI = 1.55–2.39) = 98% | NR | NR | CBIP were found to be significantly effective in improving maternal and neonatal health | |
| ( ) | : 19 RCTs : 1,26,375 | : 100%RR = 1.56, (95% CI =1.37–1.77) = 99% | NR | NR | CHEI was found to be significantly effective for improving BF practices when given to mothers and other family members | |
| ( ) | : 3 RCTs : Total: 2,066 IG: 1,064 CG: 1,002 | RR = 1.7 (95% CI = 0.98–2.95) = 78% | Low | NR | BF interventions provided by non-healthcare professionals reported improvements in EIBF rates but the result was not statistically significant | |
| EBF (exclusive breast feeding) | ( ) | : 1 cluster-randomized trial (LMIC) : 390 | RR = 1.21 (95% CI = 0.91–1.61) RR = 1.47 (95% CI = 1.06, 2.05) | Moderate | NR | Insufficient evidence to suggest that any antenatal BF education was found to be more effective than standard care for improving EBF at 3 or 6 months |
| ( ) | : 1 RCT : 40 | RR = 0.92 (95% CI = 0.79–1.08) | Low | All women in the control group exclusively breastfed their babies | The intervention provided no significant improvement in BF practices as 100% of women reported EBF to their babies. | |
| Continue BF for 2 years | None of the SRs reported this outcome. | NR | NR | NR | NR | None of the SRs had assessed these parameters. Therefore, SR needs to be conducted considering these parameters. |
| Acceptability | None of the SRs reported this outcome. | NR | NR | NR | None of the SRs had assessed these parameters. Therefore, SR needs to be conducted considering these parameters. | |
| Satisfaction | None of the SRs reported this outcome. | NR | NR | NR | None of the SRs had assessed these parameters. Therefore, SR needs to be conducted considering these parameters. |
Comparison 1: BF intervention vs. routine care. NR, not reported.
| EIBF | None of the SRs reported this outcome. | NR | NR | NR | None of the SRs had assessed these parameters. Therefore, SR needs to be conducted considering these parameters. |
| EBF | ( ) | 1 RCT 42 participants | RR = 0.92 (95% CI = 0.79–1.07) | Low | Insignificant improvements were reported in BF practices in the TCC mobile devices group compared to non-digital TCC as 100% of women exclusively breastfed their babies. |
| Continue BF for 2 years | None of the SRs reported this outcome. | NR | NR | NR | None of the SRs had assessed these parameters. Therefore, SR needs to be conducted considering these parameters. |
| Accepatability | None of the SRs reported this outcome. | NR | NR | NR | None of the SRs had assessed these parameters. Therefore, SR needs to be conducted considering these parameters. |
| Satisfaction | None of the SRs reported this outcome. | NR | NR | NR | None of the SRs had assessed these parameters. Therefore, SR needs to be conducted considering these parameters. |
Comparison 2: One BF intervention vs. other intervention. NR, not reported.
Excluded systematic reviews
We excluded 16 SRs ( 56 – 71 ) from this overview following the screening of full texts articles. The most common reasons for exclusion were unrelated interventions and population. Of the 16 excluded SRs, seven SRs ( 56 – 62 ) did not focus on the interventions intended to promote BF practices, six SRs ( 63 – 68 ) did not target the population of interest, two SRs ( 69 , 70 ) did not specify the population and one SR had no subgroup analysis for LMICs/LICs population ( 71 ). We presented the list of excluded studies in Table 4 .
List of excluded studies with reasons.
| Kramer and Kakuma ( ) | Optimal duration of exclusive breastfeeding | Low birth weight babies Interventions not related to BF |
| Ndikom et al. ( ) | Extra fluids for breastfeeding mothers for increasing milk production | Interventions not related to BF |
| Bryanton et al. ( ) | Postnatal parental education for optimizing infant general health and parental infant relationships | Population from HIC |
| Fair et al. ( ) | Interventions for supporting the initiation and continuation of breastfeeding among women who are overweight or obese | Population from HIC |
| McFadden et al. ( ) | Support for healthy breastfeeding mothers with healthy term babies | No segregated data from HIC and LIC |
| Lewin et al. ( ) | Lay health workers in primary and community health care for maternal and child health and the management of infectious diseases | Interventions not related to BF |
| Gagnon and Sandall ( ) | Individual or group antenatal education for childbirth or parenthood, or both | Population from HIC |
| Sandall et al. ( ) | Midwife-led continuity models vs. other models of care for childbearing women | Population from HIC |
| Barlow et al. ( ) | Individual and group based parenting programmes for improving psychosocial outcomes for teenage parents and their children | Population from HIC |
| Becker et al. ( ) | Methods of milk expression for lactating women | Interventions not related to BF |
| Opiyo and English ( ) | In-service training for health professionals to improve care of seriously ill newborns and children in low-income countries | Interventions not related to BF |
| Pantoja et al. ( ) | Implementation strategies for health systems in low-income countries: an overview of systematic reviews | Intervention not related to BF |
| Ciapponi et al. ( ) | Delivery arrangements for health systems in low-income countries: an overview of systematic reviews | Intervention not related to BF |
| Jaafar et al. ( ) | Effect of restricted pacifier use in breastfeeding term infants for increasing duration of breastfeeding | Population from HIC |
| Jaafar et al. ( ) | Rooming-in for new mother and infant vs. separate care for increasing the duration of breastfeeding | Population not specified |
| Lee and Thomas ( ) | Antenatal breast examination for promoting breastfeeding | Population not specified |
Methodological quality of included reviews
The R-AMSTAR grading system was developed to evaluate the procedures employed in Cochrane reviews. All Cochrane reviews followed a general protocol outlining procedures, five of the six included reviews had a high score, while one included SR ( 49 ) had a low score. R-AMSTAR ratings for each Cochrane systematic review—Breastfeeding (BF) interventions—( Table 5 ).
Methodological quality of included studies.
| ) | ) | ) | ) | ) | ) | ||
|---|---|---|---|---|---|---|---|
| 1. | Was an “a priori” design provided? | 4 | 4 | 4 | 4 | 4 | 4 |
| 2. | Was there duplicate study selection and data extraction? | 4 | 4 | 4 (one author extract and other cross-checked) | 4 | 4 | 4 |
| 3. | Was a comprehensive literature search performed? | 4 | 4 | 4 | 4 | 4 | 4 |
| 4. | Was the status of publication (i.e., gray literature) used as an inclusion criterion? | 4 | 4 | 4 | 4 | 4 | 4 |
| 5. | Was a list of studies (included and excluded) provided? | 4 | 4 | 4 | 4 | 4 | 1 (no included studies) |
| 6. | Were the characteristics of the included studies provided? | 3 | 4 | 4 | 3 (data is not complete and accurate) | 4 | 1 (no included studies) |
| 7. | Was the scientific quality of the included studies assessed and documented? | 4 | 4 | 4 | 4 | 3 | 1 (no included studies) |
| 8. | Was the scientific quality of the included studies used appropriately in formulating conclusions? | 2 | 2 | 4 | 3 | 4 | 1 (no included studies) |
| 9. | Were the methods used to combine the findings of studies appropriate? | 4 | 4 | 4 | 3 | 4 | 1 (no included studies) |
| 10. | Was the likelihood of publication bias assessed? | 3 | 3 | 3 | 3 | 3 | 1 (no included studies) |
| 11. | Was the conflict of interest included? | 3 | 4 | 3 | 3 | 3 | 3 |
| 39 | 41 | 42 | 39 | 41 | 25 |
All six SRs ( 42 , 43 , 49 , 50 , 54 , 55 ) had provided a “a priori” design, and data was retrieved by two authors who independently searched and selected studies. All SRs had mentioned the type of publication (published, unpublished, gray literature). Only one SR ( 49 ) did not meet the criteria since there were no included studies. Five of the six included SRs provided the list of included and excluded studies. In presenting characteristics of included studies, three SRs ( 50 , 54 , 55 ) scored four ratings, two SRs ( 42 , 43 ) scored three ratings and one ( 49 ) scored one rating (since this SR did not include any study). Five of the included SRs also evaluated the scientific quality of included studies and described statistical methods used to combine findings of included studies. There were no publication biases and conflicts of interest reported in any of the six SRs. All included SRs scored high ratings except for one ( 49 ) as this SR did not include any study. All included five SRs ( 42 , 43 , 50 , 54 , 55 ) were of high quality.
Effect of interventions
We summarized the key findings of all six included SRs in Tables 2 , ,3 3 .
These findings provided a summary of the reported effects as well as the degree of certainty of the evidence for each intervention. We have presented the outcomes for all interventions for which independent data were available in two primary comparison groups
- Breastfeeding support Intervention vs. standard/routine care
- One form of intervention vs. other types of intervention
None of the included SRs reported the results for both types of comparisons. Included SRs compared the intervention with standard/routine care or with other interventions.
We organized the overall number of studies and a total number of participants randomized for each included SR. We also presented the number of studies and numbers of women randomized to each comparison group.
Findings of included SRs
Comparison 1: bf intervention vs. routine care, primary outcome.
Four included SRs ( 42 , 43 , 50 , 54 ) reported findings on EIBF ( Figure 2 ; Table 2 ). All the included SRs in this overview agreed that the BF interventions improved EIBF as compared to routine care. The overall improvement in EIBF reported in included SRs varied from 44% (RR = 1.44, 95% CI = 1.06–1.97; one study; 390 participants) ( 43 ) to 93% (RR = 1.93, 95% CI = 1.55–2.39; 11 studies; 72,464 participants) ( 50 ). Community-Based Intervention Packages delivered to pregnant and reproductive-age women during their ANC and/or PNC period by Ancillary Nurse-Midwives reported the highest improvement in EIBF by 93% (RR = 1.93, 95% CI = 1.55–2.39; 11 studies; 72,464 participants ; QoE = NR ) ( 50 ), followed by BF education and support and early mother-infant contact administered to pregnant and reproductive age group women during the antenatal period by women's group peer counselor by 70% (RR = 1.7, 95% CI = 0.98–2.95; three studies; 2,066 participants; QoE = low ) ( 42 ). Community Health Educational Intervention (CHEI) delivered to pregnant women and mothers throughout both the antenatal and postnatal period by health care workers improved EIBF by 56% (RR = 1.56, 95% CI = 1.37–1.77; 19 studies; 1,26,375 participants; QoE = NR ) ( 54 ). Another included SR addressed BF intervention which includes monthly BF education sessions and weekly cell phone messages delivered to women attending monthly microcredit meetings and reported an improvement in EIBF by 44% (RR = 1.44, 95% CI = 1.06–1.97; one study; 390 participants; QoE = high ) ( 43 ). However, three SRs ( 42 , 50 , 54 ) had reported significant heterogeneity ( I 2 between 78 and 98%).

Comparison 1: BF intervention vs. routine care. EIBF, early initiation of breastfeeding.
Two included SRs ( 43 , 55 ) reported EBF findings and concluded that monthly BF education sessions and weekly cell phone messages ( 43 ) reported the highest improvements in EBF at 6 months compared to TCC via mobile devices ( 55 ) ( Figure 3 ; Table 2 ). An SR conducted by Lumbiganon et al. ( 43 ) assessed EBF at 3 and 6 months. Palmer et al. ( 55 ) evaluated EBF for up to 3 months in a low-risk setting (Kenya) where all women in the control group exclusively breastfeed. Therefore, the intervention did not have any impact on improving EBF as 100% of the women reported EBF.

Comparison 1: BF intervention vs. routine care. EBF, exclusive breastfeeding.
Monthly BF education sessions and weekly cell phone messages delivered to women attending monthly microcredit meetings reported an improvement in EBF at 3 months by 21% (RR = 1.21, 95% CI = 0.91–1.61; one study; 390 participants; QoE = moderate) and at 6 months by 47% (RR = 1.47, 95% CI = 1.06–2.05; one study; 390 participants ; QoE = moderate) ( 43 ). In another included SR, Targeted Client Communication via mobile devices delivered to pregnant and postpartum women and caregivers during the antenatal and postnatal period by health care workers reported a little improvement in EBF up to 3 months by only 8% (RR = 0.92, 95% CI = 0.79–1.08; one study; 40 participants; QoE = low) in low-risk setting ( 55 ). Significant heterogeneity, on the other hand, was not applicable.
Secondary outcome
No secondary outcomes such as Acceptability and Satisfaction were reported in this comparison group by any of the included SR.
Comparison 2: One BF intervention vs. other intervention
Only one included SR ( 55 ) reported EBF findings (9 months postpartum) in this comparison group ( Figure 4 ; Table 3 ). Palmer et al. ( 55 ) assessed that Targeted client communication (TCC) via mobile devices compared to non-digital TCC (pamphlets) had less or no effect on the improvement of EBF. TCC via mobile devices delivered to pregnant and postpartum women and caregivers during both antenatal and postnatal periods by health care workers showed an improvement of only 8% (RR = 0.92, 95% CI = 0.79–1.07; one study; 42 participants; QoE = low) ( 55 ).

Comparison 2: One BF intervention vs. other intervention. EBF, exclusive breastfeeding.
Discussion and recommendations for research and clinical practice
We aimed to identify specific interventions with the potential to promote and optimize breastfeeding practices. Our discussion had focussed on where we have found high-quality evidence of important effects. We listed key Cochrane reviews in need of an update. Finally, we had made recommendations for future systematic reviews and clinical research.
We had foreseen that there can be variations in the population, interventions, and outcomes of interest that can lead to heterogeneity. We also anticipated that there would be different approaches across SRs, across different author teams.
To reduce bias in the overview process, we followed standard review methods such as methods regarding duplication of effort, discussion-based resolution, and exclusion of overview authors from assessing their systematic reviews or trials. The inclusion of subject experts, public health experts, methodological experts, and information specialists strengthens the overview.
We intended to look into the evidence generated in LICs and LMICs and hence generalizability of the findings was restricted to LICs and LMICs. We evaluated six SRs that assessed the effects of different BF interventions to promote and optimize BF practices such as EIBF, EBF, and continued BF up to 2 years. The highest number of SRs addressed only two categories of primary outcome: EIBF and EBF. None of the SRs reported other outcomes of this overview such as continued BF up to 2 years, acceptability, and satisfaction.
In this overview, we used the R-AMSTAR tool for assessing methodological quality. Overall, the methodological quality of all the included SRs was high except for one ( 49 ) as it did not meet the R-AMSTAR tool criteria. The quality of evidence (QoE) reported in the included SRs varied from high to low.
The overview identified extensive evidence based on the type of interventions: educational intervention or support intervention, who delivered the interventions: digital or non-digital devices, personals from government, non-governmental, and private organizations, health system or health workers, non-healthcare professionals (women's group, peer counselors), and female ancillary nurse midwives (ANMs), recipients of the intervention: pregnant women, mothers of neonates, women in their reproductive age, mothers in their postpartum period, partners/spouses, or family members and the duration of the intervention: antenatal or postnatal phase.
Only two studies from LMICs (Nigeria and Iran) were included by Lumbiganon et al. ( 43 ). However, since there was no subgroup analysis for any of the listed outcomes, we did not extract the data from Iran and only retrieved the data from Nigeria. In another included SR, conducted by Palmer et al. ( 55 ), BF intervention did not show any significant improvements in BF practices since 100% of women in the control group reported EBF, and also the reported evidence was of very low certainty. Balogun et al. ( 42 ) included three studies from LMICs (Ghana, Nicaragua, and Nigeria) and one from LIC (Malawi). The study from Malawi, Nigeria, and Ghana addressed the impact of non-healthcare professional-led BF education on EIBF. However, a study from Nicaragua evaluated the impact of early mother-infant contact. In addition, the number of participants from Ghana was not available. Therefore, only two studies (Malawi and Nigeria) reported the data on EIBF.
In summary, all forms of included BF interventions were found to be effective in improving BF practices in many low-middle-income countries except for TCC via mobile devices which favors standard care and non-digital TCC since all of the women in the comparison group were exclusively breastfed their babies ( 55 ). The results were evaluated using two major comparisons groups: BF intervention against routine care and one BF intervention vs. other intervention comparison groups. Four SRs ( 42 , 43 , 50 , 54 ) assessed the effect of interventions on EIBF whereas two SRs ( 43 , 55 ) evaluated the effect of interventions on EBF in BF intervention vs. routine care comparison group. Only one included SR ( 55 ) reported EBF in another group i.e., one BF intervention vs. other intervention comparison group. However, no significant improvement was reported since the evidence was of very low certainty.
In the BF intervention vs. routine care comparison group, Community Based Intervention Packages (CBIP) delivered to pregnant and reproductive-age women during their ANC and/or PNC periods by Ancillary Nurse-Midwives reported the highest improvement in EIBF. However, insufficient evidence was reported to suggest that BF intervention showed improvements in EBF in both the comparison groups.
Possible limitations, strength, and generalizability of the overview
Limitations of the review.
This overview examined the available evidence concerning the interventions addressed to improve BF practices with no restrictions on the type of interventions. We did, however, limit our search to Cochrane reviews alone. We found limited reviews on the proposed topic. We acknowledge that not all SRs included in this overview came from LMICs or LICs only. We discovered that some of the SRs included participants ranging from low to high-income countries. We excluded some of the SRs that lacked participant subgroup analysis, even though they were designed to promote BF practices.
Strength of the review
The possible bias in the overview is estimated to be low. We followed the methods described in the Cochrane handbook ( 72 ). The search was as comprehensive as possible. Two authors independently screened studies, extracted data, and evaluated the methodological quality of reviews. We intended to investigate the evidence generated in LICs and LMICs and hence generalizability of the findings was limited to LICs and LMICs.
After an extensive literature search, we did not come across any overview of SRs that has addressed this area. Although, we found few SRs on interventions to promote BF practices while searching in Pubmed ( 32 , 36 , 73 – 77 ).
Author's conclusion
Implications for practice.
BF interventions mentioned in this overview such as BF education sessions and support interventions, Community Based Intervention Packages, Community Health Educational Intervention delivered by health and non-healthcare professionals reported some improvements in the initiation of breastfeeding whereas insufficient evidence was reported for the improvement of EBF in LICs and LMICs. Among the different types of BF interventions, Community Based Intervention Packages (CBIP) was found to be most effective in improving BF initiation rates whereas BF intervention using multimedia such as TCC via mobile devices was found to be the least effective in promoting BF practices particularly in low and low-middle income countries.
This overview can assist personnel from government, non-governmental, and private organizations as well as a health system or health workers in raising awareness and encouraging pregnant women, mothers of neonates, women in their reproductive age, mothers in their postpartum period, partners/ spouses, or family members to improve BF practices.
Implications of research
Based on the data extracted from included SRs, this overview highlights the gaps in primary research regarding the uncertainty about the settings such as LICs or LMICs, lack of evidence from LMICs, and also identified gaps in the availability of reliable up-to-date SRs on the effects of several BF interventions to promote and optimize BF practices. None of the included SR reported one of the primary outcomes i.e., continued BF up to 2 years of age and the duration of BF practices ( Tables 2 , ,3). 3 ). In addition, the included SRs did not evaluate any of the secondary outcomes such as acceptability and satisfaction ( Tables 2 , ,3 3 ).
These identified gaps open up a new area of research and can be done on a priority basis. With an improved understanding of the significance of BF and the escalating risk of neonatal mortality and malnutrition due to inappropriate BF practices, there is an urgent need to perform good quality primary research on the mentioned interventions, especially in low-income (LIC) and low-middle-income countries (LMICs).
Data availability statement
Author contributions.
AG proposed the concept of the review. MK developed and implemented the search strategies. AG and MK developed the protocol. SU and SQ screened the title and abstract. SS and PS screened full texts articles. Through conversation, AG resolved discrepancies for screening among primary reviewers. SU extracted data. AG and DS evaluated the methodological quality of included SRs. MK and SU drafted the manuscript with inputs from ST, AG, and SQ. All authors made significant contributions to this overview in reading, writing, and revision of the manuscript. All authors contributed to the article and approved the submitted version.
Acknowledgments
We gratefully acknowledge the work of ST, Datta Meghe Institute of Medical Sciences for her administrative support.
Funding Statement
This overview was funded by the Indian Council of Medical Research (ICMR), New Delhi, India.
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
- My Bibliography
- Collections
- Citation manager
Save citation to file
Email citation, add to collections.
- Create a new collection
- Add to an existing collection
Add to My Bibliography
Your saved search, create a file for external citation management software, your rss feed.
- Search in PubMed
- Search in NLM Catalog
- Add to Search
Breastfeeding initiation and support: A literature review of what women value and the impact of early discharge
Affiliations.
- 1 School of Nursing and Midwifery, Flinders University, Australia.
- 2 School of Nursing and Midwifery, Flinders University, Australia. Electronic address: [email protected].
- PMID: 27773608
- DOI: 10.1016/j.wombi.2016.09.013
Problem: Early discharge following birth has become an emerging phenomenon in many countries. It is likely early discharge has an impact on the establishment of breastfeeding.
Objective: To critically appraise the evidence on what women value in relation to breastfeeding initiation and support, and investigate the impact early discharge can have on these values.
Method: A literature search was conducted for publications since 2005 using the following databases: Cumulative Index of Nursing and Allied Health Literature (CINAHL), Medline, Scopus and PsycINFO; 21 primary articles were selected and included in the review.
Findings: There is no standard definition for 'early discharge' worldwide. Due to inconsistent definitions worldwide and minimal literature using a 24h definition, research defining early discharge as up to 72h postpartum is included. Seven key factors in relation to breastfeeding initiation and support following early discharge were identified, namely trust and security, consistent advice, practical breastfeeding support, breastfeeding education, comfortable environment, positive attitudes and emotional support, and individualised care.
Conclusion: The findings suggest individualised postnatal lengths of stay may be beneficial for the initiation of breastfeeding. Five values were not impacted by early discharge, but rather individual midwives' practice. There is consensus in the literature that early discharge promoted a comfortable environment to support breastfeeding initiation. Wide variations in the definition of early postnatal discharge made it difficult to draw influential conclusions. Therefore, further research is required.
Keywords: Breastfeeding; Early discharge; Initiation or establish; Length of stay; Postnatal care.
Copyright © 2016 Australian College of Midwives. Published by Elsevier Ltd. All rights reserved.
PubMed Disclaimer
Similar articles
- Does postpartum length of stay affect breastfeeding duration? A population-based study. Heck KE, Schoendorf KC, Chávez GF, Braveman P. Heck KE, et al. Birth. 2003 Sep;30(3):153-9. doi: 10.1046/j.1523-536x.2003.00239.x. Birth. 2003. PMID: 12911797
- Adolescent mothers' breastfeeding social support needs. Grassley JS. Grassley JS. J Obstet Gynecol Neonatal Nurs. 2010 Nov-Dec;39(6):713-22. doi: 10.1111/j.1552-6909.2010.01181.x. Epub 2010 Sep 28. J Obstet Gynecol Neonatal Nurs. 2010. PMID: 20880051 Review.
- UK women's experiences of breastfeeding and additional breastfeeding support: a qualitative study of Baby Café services. Fox R, McMullen S, Newburn M. Fox R, et al. BMC Pregnancy Childbirth. 2015 Jul 7;15:147. doi: 10.1186/s12884-015-0581-5. BMC Pregnancy Childbirth. 2015. PMID: 26148545 Free PMC article.
- Home versus hospital breastfeeding support for newborns: a randomized controlled trial. McKeever P, Stevens B, Miller KL, MacDonell JW, Gibbins S, Guerriere D, Dunn MS, Coyte PC. McKeever P, et al. Birth. 2002 Dec;29(4):258-65. doi: 10.1046/j.1523-536x.2002.00200.x. Birth. 2002. PMID: 12431265 Clinical Trial.
- [Post-partum: Guidelines for clinical practice--Short text]. Sénat MV, Sentilhes L, Battut A, Benhamou D, Bydlowski S, Chantry A, Deffieux X, Diers F, Doret M, Ducroux-Schouwey C, Fuchs F, Gascoin G, Lebot C, Marcellin L, Plu-Bureau G, Raccah-Tebeka B, Simon E, Bréart G, Marpeau L. Sénat MV, et al. J Gynecol Obstet Biol Reprod (Paris). 2015 Dec;44(10):1157-66. doi: 10.1016/j.jgyn.2015.09.017. Epub 2015 Oct 31. J Gynecol Obstet Biol Reprod (Paris). 2015. PMID: 26527017 Review. French.
- Breastfeeding among parous women offered home-visit by a midwife after early discharge following planned cesarean section: Secondary analysis of a randomized controlled trial. Kruse AR, Lauszus FF, Forman A, Kesmodel US, Rugaard MB, Knud-En RK, Persson EK, Sundtoft IB, Uldbjerg N. Kruse AR, et al. Eur J Midwifery. 2023 Dec 7;7:38. doi: 10.18332/ejm/173089. eCollection 2023. Eur J Midwifery. 2023. PMID: 38075381 Free PMC article.
- Academy of Breastfeeding Medicine Clinical Protocol #2: Guidelines for Birth Hospitalization Discharge of Breastfeeding Dyads, Revised 2022. Hoyt-Austin AE, Kair LR, Larson IA, Stehel EK; Academy of Breastfeeding Medicine. Hoyt-Austin AE, et al. Breastfeed Med. 2022 Mar;17(3):197-206. doi: 10.1089/bfm.2022.29203.aeh. Breastfeed Med. 2022. PMID: 35302875 Free PMC article.
- Parental experiences and breastfeeding outcomes of early support to new parents from family health care centres-a mixed method study. Saade S, Flacking R, Ericson J. Saade S, et al. BMC Pregnancy Childbirth. 2022 Feb 23;22(1):150. doi: 10.1186/s12884-022-04469-6. BMC Pregnancy Childbirth. 2022. PMID: 35197015 Free PMC article.
- Early discharge of first-time parents and their newborn: A scoping review. Lindblad V, Gaardsted PS, Melgaard D. Lindblad V, et al. Eur J Midwifery. 2021 Oct 11;5:46. doi: 10.18332/ejm/140792. eCollection 2021. Eur J Midwifery. 2021. PMID: 34708193 Free PMC article. Review.
- Self-efficacy, support and sustainability - a qualitative study of the experience of establishing breastfeeding for first-time Australian mothers following early discharge. James L, Sweet L, Donnellan-Fernandez R. James L, et al. Int Breastfeed J. 2020 Nov 23;15(1):98. doi: 10.1186/s13006-020-00337-1. Int Breastfeed J. 2020. PMID: 33225944 Free PMC article.
Publication types
- Search in MeSH
Related information
- Cited in Books
LinkOut - more resources
Full text sources.
- Elsevier Science
Other Literature Sources
- scite Smart Citations
- MedlinePlus Consumer Health Information
- MedlinePlus Health Information
- Citation Manager
NCBI Literature Resources
MeSH PMC Bookshelf Disclaimer
The PubMed wordmark and PubMed logo are registered trademarks of the U.S. Department of Health and Human Services (HHS). Unauthorized use of these marks is strictly prohibited.
- Open access
- Published: 14 September 2020
Breastfeeding during the COVID-19 pandemic – a literature review for clinical practice
- Welma Lubbe ORCID: orcid.org/0000-0002-2468-5687 1 na1 ,
- Elina Botha 2 na1 ,
- Hannakaisa Niela-Vilen 3 na1 &
- Penny Reimers 4 na1
International Breastfeeding Journal volume 15 , Article number: 82 ( 2020 ) Cite this article
38k Accesses
68 Citations
40 Altmetric
Metrics details
The COVID-19 pandemic is disrupting normal life globally, every area of life is touched. The pandemic demands quick action and as new information emerges, reliable synthesises and guidelines for care are urgently needed. Breastfeeding protects mother and child; its health benefits are undisputed and based on evidence. To plan and support breastfeeding within the current pandemic, two areas need to be understood: 1) the clinical characteristics of COVID-19 as it applies to breastfeeding and 2) the protective properties of breastfeeding, including the practice of skin-to-skin care. This review aims to summarise how to manage breastfeeding during COVID-19. The summary was used to create guidelines for healthcare professionals and mothers.
Current publications on breastfeeding during the COVID-19 pandemic were reviewed to inform guidelines for clinical practice.
Current evidence states that the Coronavirus is not transmitted via breastmilk. Breastfeeding benefits outweigh possible risks during the COVID-19 pandemic and may even protect the infant and mother. General infection control measures should be in place and adhered to very strictly.
Conclusions
Breastfeeding should be encouraged, mothers and infant dyads should be cared for together, and skin-to-skin contact ensured throughout the COVID-19 pandemic. If mothers are too ill to breastfeed, they should still be supported to express their milk, and the infant should be fed by a healthy individual. Guidelines, based on this current evidence, were produced and can be distributed to health care facilities where accessible information is needed.
The COVID-19 pandemic is creating global disruption, causing markets to plummet and generating many questions in every area of life. Since it affects health in multiple ways, including sexual and reproductive health, publishing in all these areas has increased lately. Not all knowledge is based on scientific evidence, resulting in consequences which could be detrimental rather than providing the needed protection. One area, that needs to be based on scientific evidence, is breastfeeding. Although limited clinical research is available, we can build on what we know about breastfeeding and previous similar infection outbreaks to plan and manage the crisis. This review is intended for healthcare professionals involved with breastfeeding populations, both in an acute care and community health setting. It should not replace clinical judgement or specialist consultation, but rather strengthen clinical management, provide up-to-date evidence and optimize health in infants who may or may not have been exposed to COVID-19. This review has been compiled from information that is currently known about COVID-19 and since new information about the disease is becoming rapidly available, suggestions may be subject to change as additional information is shared.
The novel corona virus (SARS-CoV-2) originated in Wuhan, in Central China in December of 2019 and spread rapidly across China [ 1 , 2 , 3 ]. Forty-nine percent of patients who presented with pneumonia were exposed to the Huanan Seafood Wholesale Market [ 2 , 3 ]. On 5 February 2020, the virus also spread to other countries including Japan, Thailand, Singapore, Republic of Korea, the United States of America and Australia [ 1 ]. Currently, every continent across the globe has been affected [ 3 ] and the World Health Organization (WHO) declared the outbreak of the disease as an international public health emergency [ 4 ].
Although most of the infections occur in adults older than 60 years [ 3 ], some pregnant women have also been infected, causing concerns for the management of the perinatal period. A few studies have explored the infection of neonates with SARS-CoV-2 and none showed breastfeeding as method of the transmission of the virus [ 1 , 5 , 6 , 7 ]. Various research studies reporting primary data have been published on SARS-CoV-2 transmission in the perinatal period. Chen et al. published a retrospective review of medical records of nine infected pregnant woman [ 5 ], while Rasmussen et al. published their article on COVID-19 and Pregnancy: What obstetricians need to know [ 8 ]. Zhu and colleagues published a clinical analysis of 10 neonates born to mothers with 2019-nCoV pneumonia [ 1 ], while Zeng et al. performed a retrospective analysis of 33 neonates born from COVID-19 positive mothers [ 6 ]. Schwartz published an analysis of 38 pregnant women with COVID-19 and found no evidence supporting intrauterine or transplacental transmission from infected pregnant women to their foetuses [ 9 ]. Aligned with these publications, authoritative bodies released statements regarding COVID-19: the incidence, mortality, prevention and treatment thereof.
Within this valuable, but limited scientific information, in addition to an overload of public information, the question remained: How do we manage breastfeeding in the wake of COVID-19? The authors aim to provide a synthesis on what is currently known about COVID-19, with specific reference to breastfeeding in infants born to healthy, exposed or infected mothers. In addition, the authors aim to provide guidelines for the management of breastfeeding at home and within health facilities, including in the high risk and neonatal intensive care units. To plan and support breastfeeding within the current pandemic, two areas need to be understood: 1) the clinical characteristics of COVID-19 as it applies to breastfeeding and 2) the protective properties of breastfeeding, including the practice of skin-to-skin care. Taking these aspects into account it was possible to compile a clinical guide for both healthcare professionals and breastfeeding mothers.
The current (15 June 2020) publications on COVID-19 with specific reference to breastfeeding were reviewed to provide evidence-based information for healthcare professionals as well as mothers. Official documents available in English were included due to language abilities of the authors. These included published and in-press clinical research articles, as well as interim guides, expert reviews or guidelines/official statement documents from international associations, including the clinical management interim guides released by the World Health Organization in 2020 and the International Confederation of Midwives’ (ICM) Official Statements of Novel Coronavirus (SARS-CoV-2) and Pregnancy, as well as the Academy of Breastfeeding Medicine (ABM). In addition, articles discussing the characteristics of COVID-19 were included with specific interest in vertical transmission potential in the perinatal period. Articles explaining how breastfeeding could protect against the virus were also included.
The following exclusion criteria were used: Webpages which provide the public with questions and answers, media releases and practice advisories were excluded, since it was based on, and mostly included a repetition of official statements and documents and articles. Country-based webpages were read to compare available data, but not included in the review summary, since it was mostly based on the global recommendations of the WHO and if any discrepancies in management were found, the WHO recommendations were regarded as superior to country recommendations.
Data analysis
The publications have been reviewed for the characteristics of COVID-19 in the perinatal period, the potential of transmission from infected mother to her breastfeeding infant and proposed management of healthy, exposed and infected mother-infant dyads. The findings were synthesised and a clinical guide with rationale for each suggestion provided (see Table 1 ) and algorithms for both healthcare providers (Additional file 1 ) and mothers (Additional file 2 ) were designed.
Since the Coronavirus is a novel virus, we have little research to work with and must explore the data that is available, as well as build on knowledge and experience of similar past viral outbreaks, including SARS-CoV-1 and Middle Eastern Respiratory Syndrome (MERS). Furthermore, there is considerable knowledge on the properties of breastmilk which can inform researchers and clinicians of the most suitable route of action, within the limited knowledge on the COVID-19 disease. We will first discuss what is known about COVID-19 specifically within the context of breastfeeding [ 10 ] and then look at how breastmilk can be utilized as an intervention to protect infants. Laboratory research on breastfeeding and COVID-19 seems to have been initiated, as evident from social media, however no research on this topic is currently available.
COVID-19: the disease epidemiology and the breastfeeding population
SARS-CoV-2 is a beta coronavirus, which cause the COVID-19 disease [ 11 ]. Currently the mode of transport of SARS-CoV-2 suggests person-to-person transmission which occurs when in close contact with an infected person. The virus is transferred via respiratory droplets produced when coughing and sneezing. Droplets can either land on a healthy individual close to a cavity in the facial area or be inhaled into the lungs of persons in close proximity. It is important to note that the airborne transmission over long distances is unlikely.
In a recent study published in The Lancet, it was stated that all the information available on pneumonia caused by the 2019 novel coronavirus disease was based on information from the general population [ 2 ]. The conclusion drawn by Qiao was that the SARS-CoV-2 may have similar pathogenesis to the SARS-CoV1 and therefore we can draw on the management of these previous epidemics to inform current practice guidelines [ 12 ].
Vertical transmission refers to the passage of a pathogen from mother to infant during the period before and after birth, including via placental blood during pregnancy, via the birth canal during labour, delivery and during postpartum feeding [ 1 ]. In their study Zhu et al. found no evidence of such vertical transmission [ 1 ]. In addition, in a retrospective review of clinical records of nine pregnant women by Chen, Guo et al., the authors found limited data available to support the transmission potential of SARS-CoV-2 from mother to child via breastmilk. They assessed the evidence of intrauterine vertical transmission by testing for the presence of the virus in amniotic fluid, cord blood, neonatal throat swab samples and breastmilk samples collected and tested from patients after the first lactation [ 5 ]. Although some case studies of infants infected with COVID-19 have been reported, it can be noted that these studies did not test for the presence of the virus in amniotic fluid, cord blood, neonatal throat swabs or breastmilk [ 7 , 13 , 14 , 15 ] and included only three infants in total, indicating further investigation is needed. A few case studies were published from Spain [ 16 ], Vietnam [ 13 ], China [ 15 ] and USA [ 17 ], and none of these reported transmissions of the SARS-CoV-2 via breastmilk. A systematic review by Duran et al. and a study by Lu and Shi also reported that breastmilk does not appear to be a method of transmission of the virus [ 18 , 19 ]. Samples of breastmilk from 18 women infected with SARS-CoV-2 were evaluated and although SARS-CoV-2 RNA was detected in one sample of milk, the follow-up culture of the same sample was negative. It is likely that the SARS-CoV-2 RNA that was found does not contain replication-competent virus and so is unlikely to infect an infant [ 20 ]. Findings from this group of cases suggest that there is currently no evidence to show that respiratory viruses can be transmitted through breast milk.
Breastfeeding and breastmilk properties
Breastfeeding protects neonates, infants and children against morbidity and death [ 21 , 22 ]. The protective effect is particularly strong against infectious diseases, due to the direct transfer of antibodies as well as anti-infective factors and long-lasting transfer of immunological competence and memory [ 23 ].
Breastfeeding has both short and long-term benefits for the mother and her infant. To benefit from the protective factors in breast milk, every effort should be made to support and enable early and immediate initiation of breastfeeding. Not only does the early initiation decrease neonatal deaths, but together with frequent breastfeeding, ensures that the breastfeeding dyad are not separated. Early initiation of breastfeeding significantly increases the breastfeeding rates in healthy term infants at one to 4 month’s age by stimulating hormones and facilitating bonding [ 24 , 25 , 26 ]. The Lancet Breastfeeding Series (2016) reported that scaling up breastfeeding could prevent around 823,000 child deaths annually [ 21 ]. Breastfeeding reduces 64% of morbidity and mortality in diarrhoea, 74% in the severity of RSV and its hospitalization with 72% [ 22 ]. This demonstrates the protective benefits of breastfeeding, which pertain to COVID-19 pandemic.
The neonate has an immature immune system and colostrum, a powerful immune booster, protects infants from infections by means of bioactive factors and secretory IgA antibodies. Breast milk with its abundant source of immunoglobulins, lactoferrin, lysozyme and cytokines play an important role in absorbing and engulfing harmful micro-organisms and targeting specific bacteria and providing protection by regulating the immune response [ 27 ]. Human milk oligosaccharides, abundant in human milk, shape the microbiome, provide probiotics and modulate the developing immune system also displaying anti-adhesive effects for bacterial antigens [ 28 , 29 , 30 ]. All the above are compelling reasons for every infant to receive only breast milk and preferably their own mothers’ milk.
The best way to promote successful breastfeeding, is to ensure that the mother-infant dyad is kept together, and skin-to-skin contact is supported and encouraged [ 31 ]. Skin-to-skin is the safest and best transition for mothers and their infants to a new life together. Ensuring it happens immediately after birth, the infant’s microbiome can develop from the mother’s flora, so beneficial during a pandemic [ 32 ]. Skin-to-skin also increases blood glucose levels 75–90 min after birth, improves cardiorespiratory stability [ 26 ] and significantly reduces stress levels in the infant and mother [ 33 ]. Keeping mother and infant together can reduce birth stress and even prevent neurodevelopmental disorders in the infant. The smell, touch and voice of the mother naturally calms the infant [ 34 ].
Suggested practice guidelines
It should be noted that the WHO interim guidance documents on the management of COVID-19 has been informed by evidence-based guidelines also published by the WHO, such as the Infection prevention and control of epidemic- and pandemic-prone acute respiratory diseases in health care [ 35 ], as well as current information on COVID-19. General infection prevention measures should therefore always be taken, in all circumstances, with special attention to droplet protection. Guidance about the need for exposed and infected breastfeeding mothers to practice hand and respiratory hygiene has been given by many organisations internationally and experts in the field [ 36 , 37 , 38 , 39 ]. Additional suggestions are provided based on the current knowledge of COVID-19. Based on this information, and her right to choose, the mother can make an informed choice regarding breastfeeding during the pandemic [ 40 ]. Measures for expressing breastmilk should also be applied as in normal situations, however, no equipment should be shared between mothers. All equipment used to express milk, should be rinsed with cold water and secondly washed with warm water and soap and thirdly, sterilized. In case of an epidemic it may be advisable to sterilise equipment after each use, instead of once in 24 h [ 27 ]. Another additional measure is that if a mother is potentially exposed or tested positive for COVID-19, she should use a dedicated breast pump and not share one with other mothers. She should also express in the area in which she has been isolated. A practical suggestion may be that the mother express in her container in isolation and then decant the expressed milk into a clean container held by a healthy person with appropriate protective clothing, including masks and gloves, to prevent the virus from spreading via the surface of the container. In this manner a clean container can then also be stored/milk frozen for later use without the risk of contaminating other containers with milk [ 41 ]. There has been much debate on ways to reduce the risk of the external contamination of expressed human milk containers. Marinelli and Lawrence, advise bottles to be wiped down with a viricidal agent or a dilution of 1:10 diluted bleach (sodium hypochlorite [NaOCl]) and bottles stored in separate bins for each infant in refrigerators [ 37 ]. However, concerns were expressed about the necessity to do this as no proof of contamination of bottle surfaces exists [ 42 ].
Table 1 provide a synthesis of the evidence supported recommendations for breastfeeding amidst COVID-19, based on the latest evidence as available on 15 June 2020. Information about SARS-CoV-2 transmission is emerging daily, and the latest information should always be considered in clinical decision making.
Based on the evidence presented in Table 1 , a visual presentation for quick clinical reference is presented as an algorithm for healthcare professionals (Additional file 1 ) and mothers (Additional file 2 ) to support in decision-making regarding breastfeeding practices in the wake of COVID-19.
Global measures to control the spread of the coronavirus should be applied in everyday situations to prevent and stop the spread of pathogens. These measures include personal hygiene and social distancing, which should be applied to all infants, to prevent them from contracting the illness (refer to Table 1 ). This review aimed to map the current evidence-based literature about breastfeeding and COVID-19.
Continued breastfeeding and zero-separation of the mother-infant dyad appears to be the best practice in this situation. Considering the current evidence, it is not common for respiratory viruses to be transmitted via breast milk and transmission such as this has not been demonstrated in infants who contracted COVID-19 or were born to mothers who tested positive for the virus [ 16 , 53 ]. In addition, the properties in breast milk can protect the infant [ 10 , 43 ].
In their Practice Advisory on the Novel Coronavirus 2019 (SARS-CoV-2), the American College of Obstetricians and Gynecologists (ACOG), state that infants born to mothers with confirmed COVID-19, should be considered persons under investigation (PUI), and as such should be isolated according to the Infection Prevention and Control Guidance for PUIs [ 54 , 55 ]. They further state that confirmed or PUI mothers should be separated from their infants, in separate rooms until the maternal transmission-based precautions are discontinued. The National Health Commission of China in their notice: strengthening maternal disease treatment and safe midwifery during the prevention and control of new coronavirus pneumonia, in February 2020 [ 56 ], also followed this recommendation of separation for at least 14 days and not breastfeeding. However, in the next section of the ACOG advisory on breastfeeding it is stated that breastfeeding should be initiated and continued, since currently it seems that this respiratory virus cannot be transmitted through breastmilk [ 54 ]. American Academy of Pediatrics (AAP), 2020 and the Centers for Disease Control and Prevention (CDC), also suggest that infected mothers and their infants be temporarily separated and once home should maintain a distance of at least 6 feet (2 m) between them, with mothers expressing to provide breastmilk for their infants [ 57 , 58 ].
The ICM [ 4 ] concur with UNICEF, the ABM and RCOG in that currently there is no evidence that respiratory viruses can be transmitted via breast milk. Therefore, breastfeeding should be continued while general infection control measures are applied in symptomatic mothers and when mothers are too ill to breastfeed. Mothers who are too ill to breastfeed could express milk, and a healthy individual could then cup, or spoon feed the infant.
The authors agree that breastfeeding should be continued, since the protective benefits of breastmilk far outweigh the risk of potential pathogen transmission. In addition, we want to highlight that mother and infant separation has negative effects on the mental and physical health of both mothers and infants [ 34 , 59 ] and should therefore be limited to extreme situations and supported by good evidence or clinical reasoning (see Table 1 ).
Breastfeeding is the best protective measure available for healthy and at-risk infants and their mothers during the COVID-19 pandemic. Therefore, breastfeeding should not be interrupted, mothers and infants should not be separated, and skin-to-skin contact should not be discontinued. While ensuring normality as far as possible, general infection control measures should be in place and adhered to very strictly. In exposed or infected mother’s additional droplet protection should be taken by mother by wearing a (see-through), surgical face mask when handling and feeding her infant. When mothers are too ill to breastfeed, they should still be supported to express their milk, and the infant should be fed by a healthy individual. Breastfed infants have an advantage receiving additional protection against SARS-CoV-2. Based on the current evidence, it seems that the virus is not transmitted via breastmilk. For this reason, the benefits of breastmilk outweigh the risk of breastfeeding cessation and of a potential transmission of the coronavirus [ 38 ].
Availability of data and materials
Not applicable
Abbreviations
Severe acute respiratory syndrome coronavirus 2
Middle Eastern Respiratory Syndrome
Coronavirus disease 2019
2019 Novel Coronavirus
Respiratory Syncytial Virus
World Health Organization
Zhu H, Wang L, Fang C, Peng S, Zhang L, Chang G, et al. Clinical analysis of 10 neonates born to mothers with 2019-nCoV pneumonia. Transl Pediatr. 2020;9(1):51–60.
Article PubMed PubMed Central Google Scholar
Chen N, Zhou M, Dong X, Qu J, Gong F, Han Y, et al. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study. Lancet. 2020;395(10223):507.
Article CAS PubMed PubMed Central Google Scholar
Li Q, Guan X, Wu P, Wang X, Zhou L, Tong Y, et al. Early transmission dynamics in Wuhan, China, of novel coronavirus-infected pneumonia. N Engl J Med. 2020;382:1199–207.
CAS PubMed PubMed Central Google Scholar
International Confederation of Midwives, (ICM). Official statements on novel coronavirus (COVID-19) and pregnancy. Available at: https://www.internationalmidwives.org/icm-news/unfpa-statement-on-novel-coronavirus-(covid-19)-and-pregnancy.html . Issued 7 Mar 2020. Accessed 20 Mar 2020.
Chen H, Guo J, Wang C, Luo F, Yu X, Zhang W, et al. Clinical characteristics and intrauterine vertical transmission potential of COVID-19 infection in nine pregnant women: a retrospective review of medical records. Lancet. 2020;395(10226):809.
Zeng L, Xia S, Yuan W, Yan K, Xiao F, Shao J, et al. Neonatal early-onset infection with SARS-CoV-2 in 33 neonates born to mothers with COVID-19 in Wuhan, China. JAMA Pediatr. 2020;174(7):722–5.
Dong L, Tian J, He S, Zhu C, Wang J, Liu C, et al. Possible vertical transmission of SARS-CoV-2 from an infected mother to her newborn. JAMA. 2020;323(18):1846–8.
Rasmussen SA, Smulian JC, Lednicky JA, Wen TS, Jamieson DJ. Coronavirus disease 2019 (COVID-19) and pregnancy: what obstetricians need to know. Am J Obstet Gynecol. 2020;222(5):415–26.
Schwartz DA. An analysis of 38 pregnant women with COVID-19, their newborn infants, and maternal-fetal transmission of SARS-CoV-2: maternal coronavirus infections and pregnancy outcomes. Arch Pathol Lab Med. 2020;144(7):799–805.
Article PubMed Google Scholar
Centers for Disease Control and Prevention, (CDC). Interim infection prevention and control recommendations for patients with suspected or confirmed coronavirus disease 2019 (COVID-19) in healthcare settings. Available at: https://www.cdc.gov/coronavirus/2019-ncov/infection-control/control-recommendations.html . Updated 18 May 2020. Accessed 15 June 2020.
Hong H, Wang Y, Chung HT, Chen CJ. Clinical characteristics of novel coronavirus disease 2019 (COVID-19) in newborns, infants and children. Pediatr Neonatol. 2020;61(2):131–2.
Qiao J. What are the risks of COVID-19 infection in pregnant women? Lancet. 2020;395(10226):760–2.
Le TH, Nguyen VL, Tran MD, Do TH, Tran TH, Le TY, et al. The first infant case of COVID-19 acquired from a secondary transmission in Vietnam. Lancet Child Adolesc Health. 2020;4(5):405–6.
Zeng H, Xu C, Fan J, Tang Y, Deng Q, Zhang W, et al. Antibodies in infants born to mothers with COVID-19 pneumonia. JAMA. 2020;323(18):1848–9.
Fan C, Lei D, Fang C, Li C, Wang M, Liu Y, et al. Perinatal transmission of COVID-19 associated SARS-CoV-2: should we worry? Clin Infect Dis. 2020. https://doi.org/10.1093/cid/ciaa226 .
Díaz AC, Maestro LM, Pumarega MT, Antón FB, Alonso PCR. First case of neonatal infection due to SARS-CoV-2 in Spain. An Pediatr. 2020;92(4):237–8.
Article Google Scholar
Dumpa V, Kamity R, Vinci AN, Noyola E, Noor A. Neonatal coronavirus 2019 (COVID-19) infection: a case report and review of literature. Cureus. 2020;12(5):e8165.
PubMed PubMed Central Google Scholar
Duran P, Berman S, Niermeyer S, Jaenisch T, Forster T, Gomez Ponce de Leon R, et al. COVID-19 and newborn health: systematic review. Rev Panam Salud Publica. 2020;44:e54.
Lu Q, Shi Y. Coronavirus disease (COVID-19) and neonate: what neonatologist need to know. J Med Virol. 2020;92(6):564–7.
Article CAS PubMed Google Scholar
Chambers CD, Krogstad P, Bertrand K, Contreras D, Bode L, Tobin N, et al. Evaluation of SARS-CoV-2 in breastmilk from 18 infected women. medRxiv. 2020. https://doi.org/10.1101/2020.06.12.20127944 .
Victora CG, Bahl R, Barros AJD, França GVA, Horton S, Krasevec J, et al. Breastfeeding in the 21st century: epidemiology, mechanisms, and lifelong effect. Lancet. 2016;387(10017):475–90.
American Academy of Pediatrics, (AAP). Breastfeeding and the use of human milk. Pediatrics. 2012;129(3):e827.
Hanson LA. Breastfeeding provides passive and likely long-lasting active immunity [published correction appears in Annals of Allergy, Asthma & Immunology. 1999 May;82(5):478]. Ann Allergy Asthma Immunol. 1998;81(6):523–37.
Khan J, Vesel L, Bahl R, Martines J. Timing of breastfeeding initiation and exclusivity of breastfeeding during the first month of life: effects on neonatal mortality and morbidity—a systematic review and meta-analysis. Matern Child Health J. 2015;19(3):468–79.
Jaafar SH, Ho JJ, Lee KS. Rooming-in for new mother and infant versus separate care for increasing the duration of breastfeeding. Cochrane Database Syst Rev. 2016;8:CD006641.
Google Scholar
Moore ER, Anderson GC, Bergman N, Dowswell T. Early skin-to-skin contact for mothers and their healthy newborn infants. Cochrane Database Syst Rev. 2016;11:CD003519.
PubMed Google Scholar
Hamosh M. Bioactive factors in human milk. Pediatr Clin N Am. 2001;48(1):69–86.
Article CAS Google Scholar
Coppa VG, Gabrielli VO, Zampini VL, Galeazzi VT, Ficcadenti VA, Padella VL, et al. Oligosaccharides in 4 different milk groups, Bifidobacteria, and Ruminococcus Obeum. J Pediatr Gastroenterol Nutr. 2011;53(1):80–7.
Morrow AL, Ruiz-Palacios G, Altaye M, Jiang X, Lourdes Guerrero M, Meinzen-Derr J, et al. Human milk oligosaccharides are associated with protection against diarrhea in breast-fed infants. J Pediatr. 2004;145(3):297–303.
Williams JE, Price WJ, Shafii B, Yahvah KM, Bode L, McGuire MA, et al. Relationships among microbial communities, maternal cells, oligosaccharides, and macronutrients in human Milk. J Hum Lact. 2017;33(3):540–51.
Karimi FZ, Sadeghi R, Maleki-Saghooni N, Khadivzadeh T. The effect of mother-infant skin to skin contact on success and duration of first breastfeeding: a systematic review and meta-analysis. Taiwan J Obstet Gynecol. 2019;58(1):1–9.
Dumas L. Safe skin-to-skin contact between mother and baby. Procedure and important notes. 2015. Available at: https://www.saskatoonhealthregion.ca/locations_services/Services/Maternal-Newborn-Care/Documents/Procedure%20for%20Safe%20Skin%20to%20Skin%20%28Louise%20Dumas%29.pdf . Accessed 26 Mar 2020.
Mörelius E, Theodorsson E, Nelson N. Salivary cortisol and mood and pain profiles during skin-to-skin care for an unselected group of mothers and infants in neonatal intensive care. Pediatrics. 2005;116(5):1105–13.
Császár-Nagy N, Bókkon I. Mother-newborn separation at birth in hospitals: a possible risk for neurodevelopmental disorders? Neurosci Biobehav Rev. 2018;84:337–51.
World Health Organization, (WHO). Infection prevention and control of epidemic- and pandemic-prone acute respiratory infections in health care. Available at: https://apps.who.int/iris/handle/10665/112656 . Accessed 20 Mar 2020.
Centers for Disease Control and Prevention. Coronavirus Disease 2019 (COVID 19). Pregnancy & Breastfeeding. Information about coronavirus disease 2019. Available at: https://www.cdc.gov/coronavirus/2019-ncov/prepare/pregnancy-breastfeeding.html . Updated June 2020. Accessed 17 Jun 2020.
Marinelli KA, Lawrence RW. Safe handling of containers of expressed human milk in all settings during the SARS-CoV-2 (COVID-19) pandemic. J Hum Lact. 2020. https://doi.org/10.1177/0890334420919083 .
Royal College of Obstetricians and Gynaecologists, Royal College of Midwives, Royal College of Paediatrics and Child Health, Public Health England and Health Protection Scotland. Coronavirus (COVID-19) infection in pregnancy. Information for healthcare professionals Version 10.1. 2020. Available at: https://www.rcog.org.uk/globalassets/documents/guidelines/2020-06-18-coronavirus-covid-19-infection-in-pregnancy.pdf . Updated 19 June 2020. Accessed 17 July 2020.
World Health Organization, (WHO). Breastfeeding and COVID-19 for health care workers. Available at: https://www.who.int/docs/default-source/maternal-health/faqs-breastfeeding-and-covid-19.pdf?sfvrsn=d839e6c0_5 . Issued 12 May 2020. Accessed June 2020.
Academy of Breastfeeding Medicine, (ABM). ABM Statement on coronavirus 2019 (COVID-19). Available at: https://www.bfmed.org/abm-statement-coronavirus . Issued 10 Mar 2020. Accessed 15 Mar 2020.
Moro GE, Bertino E. Breastfeeding, human milk collection and containers, and human milk banking: hot topics during the COVID-19 pandemic. J Hum Lact. 2020. https://doi.org/10.1177/0890334420934391 .
Mitchell KB, Weinstein SR. Concerns regarding the article entitled safe handling of containers of expressed human milk in all settings during the SARS-CoV-2. J Hum Lact. 2020. https://doi.org/10.1177/0890334420922580 .
World Health Organization (WHO). Clinical management of severe acute respiratory infection when novel coronavirus (nCoV) infection is suspected. 2020. Available at: https://www.who.int/publications-detail/clinical-management-of-severe-acute-respiratory-infection-when-novel-coronavirus-(ncov)-infection-is-suspected . Issued Mar 2020. Accessed 13 Mar 2020.
UNICEF. Coronavirus disease (COVID-19): What parents should know how to protect yourself and your children. Available at: https://www.unicef.org/stories/novel-coronavirus-outbreak-what-parents-should-know . Issued 29 Mar 2020. Accessed 20 June 2020.
Royal College of Obstetricians and Gynaecologists. Coronavirus (COVID-19) infection and pregnancy. Information for pregnant women and their families. 2020. Available at: https://www.rcog.org.uk/en/guidelines-research-services/guidelines/coronavirus-pregnancy/covid-19-virus-infection-and-pregnancy/ . Updated 10 July 2020. Accessed 17 July 2020.
World Health Organization, (WHO). Infant and young child feeding. Available at: https://www.who.int/news-room/fact-sheets/detail/infant-and-young-child-feeding . Updated 1 Apr 2020. Accessed 17 July 2020.
Carvalho WB, Gibelli MABC, Krebs VLJ, Calil VMLT, Johnston C. Expert recommendations for the care of newborns of mothers with COVID-19. Clinics. 2020;75:e1932.
Wei M, Yuan J, Liu Y, Fu T, Yu X, Zhang Z. Novel coronavirus infection in hospitalized infants under 1 year of age in China. JAMA. 2020;323(13):1313–4.
Kampf G. Potential role of inanimate surfaces for the spread of coronaviruses and their inactivation with disinfectant agents. Infect Prev Pract. 2020;2(2):100044.
Siddharta A, Pfaender S, Vielle NJ, Dijkman R, Friesland M, Becker B, et al. Virucidal activity of World Health Organization–recommended formulations against enveloped viruses, including Zika, Ebola, and emerging coronaviruses. J Infect Dis. 2017;215(6):902–6.
Widstrom A-M, Brimdyr K, Svensson K, Cadwell K, Nissen E. Skin-to-skin contact the first hour after birth, underlying implications and clinical practice. Acta Paediatr. 2019;108(7):1192–204.
Kelvin AA, Halperin S. COVID-19 in children: the link in the transmission chain. Lancet Infect Dis. 2020;20(6):633–4.
Aghdam K, Jafari N, Eftekhari K. Novel coronavirus in a 15-day-old neonate with clinical signs of sepsis, a case report. Infect Dis. 2020;52(6):427–9.
The American College of Obstetricians and Gynecologists, (ACOG). Novel coronavirus 2019 (COVID-19). Available at: https://www.acog.org/clinical/clinical-guidance/practice-advisory/articles/2020/03/novel-coronavirus-2019 . Updated 1 July 2020. Accessed 18 July 2020.
Centers for Disease Control and Prevention, (CDC). CDC infection prevention and control guidance for PUIs. Available at: https://www.cdc.gov/coronavirus/2019-ncov/php/guidance-evaluating-pui.html . Issued 10 Apr 2020. Accessed 18 July 2020.
National Health Commission of the People’s Republic of China. National Health Commission (NHC) of the People’s Republic of China. Notice on strengthening maternal disease treatment and safe midwifery during the prevention and control of new coronavirus pneumonia. Available at: http://www.nhc.gov.cn/xcs/zhengcwj/202002/4f80657b346e4d6ba76e2cfc3888c630.shtml . Accessed 8 Feb 2020.
American Academy of Pediatrics, (AAP). Guidance on breastfeeding during the COVID-19 pandemic. Available at: https://www.aappublications.org/news/2020/04/23/covid19breastfeeding042320 . Issued 23 Apr 2020. Accessed 19 June 2020.
Centers for Disease Control and Prevention, (CDC). Evaluation and management considerations for neonates at risk for COVID-19. Available at: https://www.cdc.gov/coronavirus/2019-ncov/hcp/caring-for-newborns.html . Updated 20 May 2020. Accessed 19 June 2020.
Bystrova K, Ivanova V, Edhborg M, Matthiesen AS, Ransjö-Arvidson AB, Mukhamedrakhimov R, et al. Early contact versus separation: effects on mother-infant interaction one year later. Birth. 2009;36(2):97–109.
Download references
Acknowledgements
The authors received no funding for this publication and have no competing interested associated with this publication to declare.
Author information
All authors contributed equally to this work.
Authors and Affiliations
NuMIQ – Quality in Nursing and Midwifery, North-West University, 11 Hoffman St, Potchefstroom, South Africa
Welma Lubbe
School of Health, Midwifery, Tampere University of Applied Sciences, Tampere, Finland
Elina Botha
Department of Nursing Science, University of Turku, Turku, Finland
Hannakaisa Niela-Vilen
Department of Paediatrics and Child Health, University of KwaZulu Natal, Durban, South Africa
Penny Reimers
You can also search for this author in PubMed Google Scholar
Contributions
WL conceptualised and drafted the article, designed table and critical review. EB were involved in data collection and analysis as well as design of supplements and critical review. HN were responsible for methodology section and critical review. PR were responsible breastfeeding characteristics section and critical review. All authors read and approved the final manuscript.
Corresponding author
Correspondence to Welma Lubbe .
Ethics declarations
Ethics approval and consent to participate.
No human participants were included in this article. The article review current evidence on breastfeeding and COVID-19 and no ethical approval apply.
Consent for publication
Competing interests.
“The authors declare that they have no competing interests”
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Additional file 1..
Professional guide to breastfeeding and COVID-19.
Additional file 2.
Mothers guide to breastfeeding and COVID-19.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/ . The Creative Commons Public Domain Dedication waiver ( http://creativecommons.org/publicdomain/zero/1.0/ ) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
Reprints and permissions
About this article
Cite this article.
Lubbe, W., Botha, E., Niela-Vilen, H. et al. Breastfeeding during the COVID-19 pandemic – a literature review for clinical practice. Int Breastfeed J 15 , 82 (2020). https://doi.org/10.1186/s13006-020-00319-3
Download citation
Received : 03 April 2020
Accepted : 10 August 2020
Published : 14 September 2020
DOI : https://doi.org/10.1186/s13006-020-00319-3
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Breastfeeding
- Coronavirus; mother-infant dyad
- Skin-to-skin contact
- Breast milk expressing
- Mother-infant separation
International Breastfeeding Journal
ISSN: 1746-4358
- General enquiries: [email protected]
- DOI: 10.1108/jpmh-04-2024-0055
- Corpus ID: 272230078
Defining mental health literacy: a systematic literature review and educational inspiration
- Shengnan Zeng , Richard Bailey , +1 author Xiaohui Chen
- Published in Journal of Public Mental… 2 September 2024
- Psychology, Education
56 References
A systematic review of the limitations and associated opportunities of chatgpt, deductive qualitative analysis: evaluating, expanding, and refining theory, conceptualising and measuring positive mental health literacy: a systematic literature review, mental health education integration into the school curriculum needs to be implemented, review: school-based mental health literacy interventions to promote help-seeking - a systematic review., public opinion towards mental health (the case of the vologda region), quantifying the global burden of mental disorders and their economic value, mental health literacy: it is now time to put knowledge into practice, clarifying the concept of mental health literacy: protocol for a scoping review, positive mental health literacy: a concept analysis, related papers.
Showing 1 through 3 of 0 Related Papers

IMAGES
VIDEO
COMMENTS
A Literature Review of the Factors That Influence Breastfeeding: An A pplicatio n of the Health Believe Model. International Journal of Nursing and Health Science. V ol. 2, No. 3, 2015, pp. 28-36.
included for review. Results: Shortterm and longterm benefits of exclusive breastfeeding for children were identified. such as he althier eating habits, reduced length of hospital stay, fa vorable ...
very low, because there are man y factors that in fluence exclusive breastfeeding such as, lack of knowledge, lactation problem s, poor family and. social support, social norms, embarrassment ...
Structural. Breastfeeding is much more than the transfer of breastmilk from mother to baby. Suckling from the mother's breast is a crucial part of the nurturing of infants. Direct breastfeeding versus feeding breastmilk with a bottle, cup, or spoon has important implications for infant health and development.
Review. Lactation and the stress response. There is a strong correlation between lactation and reduced stress responses, specifically that of cortisol [].A study conducted among 10 lactating and 10 non-lactating women discovered that plasma ACTH (p < 0.001), cortisol (p < 0.05), and glucose (p < 0.001) responses to exercise were significantly reduced in lactating women [].
Perceptions about breastfeeding. Women's perceptions about breastfeeding were covered in 83% (n = 49) of the papers.Most articles (n = 31) suggested that women perceived breastfeeding as a positive experience and believed that breastfeeding had many benefits [19, 20].The phrases "breast is best" and "breastmilk is best" were repeatedly used by the participants of studies included in ...
The vast majority ( n = 50) of the reviewed literature identified various barriers for successful breastfeeding. A sizeable proportion of literature (41%, n = 24) explored women's experiences with the physical aspects of breastfeeding [ 23, 33 ]. In particular, problems with latching and the pain associated with breastfeeding were commonly ...
Abstract. Objectives: Breastfeeding during pregnancy has unintended repercussions that have yet to be determined. Previous research employed various approaches and reached varied outcomes, with some emphasizing on advantages and others focusing on hazards. With this study we aim at shedding light on the effects of breastfeeding during pregnancy ...
effects of breastfeeding on mental health were screened and included in this review. Search terms related to breastfeeding, postpartum, and mental health were used. This review on breastfeeding and postpartum depression (PPD) begins by discussing the correlation between lactation and the maternal stress response.
This systematic literature review synthesises published evidence on the factors and barriers associated with the initiation of breastfeeding within 1 h of birth in South Asian countries to inform a future of relevant, context-specific actions. Methods Protocol of the systematic literature review was pro-
erm consequences of breastfeeding. The Department of Maternal, Newborn, Child and Adolescent Health of the World Health Organization has now com. issioned an update of this review. The following long-term out-comes were reviewed: blood pressure, type-2 diabetes, serum cholesterol, overweight and obe.
A review of the breastfeeding literature specific to this region had not yet been done prior to writing this report. In 2019, only one-third of infants were exclusively breastfed in West and Central Africa. 5 METHODS The literature review included quantitative, qualitative, and mixed-method studies on feeding practices of infants aged zero to six
Findings reveal that maternal sociodemograhpic characteristic like age, education, parity, economic status, and employment may influence breastfeeding. Breastfeeding is beneficial for both mother and child. Exclusive breastfeeding rate and early initiation of breastfeeding has not reached desirable level in many countries. Understanding the factors that influence infant feeding will help in ...
Aim: This is a systematic literature review that investigates the benefits of, risks of, and questions about breastfeeding. Methods: A literature search was performed in Pubmed for "breastfeeding ...
The US National breastfeeding recommendations are that infants need to be exclusively breastfed for at least the first 6 months of life [].However, the US national rates show that only 58% of the infants born in 2017 were breastfeeding until 6 months [].Furthermore, breastfeeding rates for Black infants are disproportionately lower with only 17% of Black infants exclusively breastfed until the ...
ur from birth) and exclusive breastfeeding for the first 6 months. The exclusive breastfeeding rate and early initiation to breastfeeding are still very low, because there are many factors that influence exclusive breastfeeding such as, lack of knowledge, lactation problems, poor family and social support, social n.
The review then shifts to focus more on the psychological aspects of breastfeeding, notably on changes to the sleep-wake cycle and mother-infant interactions. The final part of the review emphasizes the danger that early breastfeeding cessation imposes on a mother's mental health, portraying how prenatal and early-onset postpartum depression ...
A literature review THESIS CENTRIA UNIVERSITY OF APPLIED SCIENCES Degree Programme in Nursing March 2014. ABSTRACT Unit Unit of Kokkola-Pietarsaari Date March 2014 ... Breastfeeding is a natural process of infant feeding involving two main methods; exclusive and partial with the latter being trendiest. Nevertheless, exclusivity is the ...
Breastfeeding for reducing the risk of pneumonia morbidity and mortality in children under two: a systematic literature review and meta-analysis. BMC Public Health. (2013) 13 Suppl 3:S18. 10.1186/1471-2458-13-S3-S18 [ PMC free article ] [ PubMed ] [ CrossRef ] [ Google Scholar ]
Early or timely initiation of breastfeeding is crucial in preventing newborn deaths and influences childhood nutrition however remains low in South Asia and the factors and barriers warrant greater consideration for improved action. This review synthesises the evidence on factors and barriers to initiation of breastfeeding within 1 h of birth in South Asia encompassing Afghanistan, Bangladesh ...
Problem: Early discharge following birth has become an emerging phenomenon in many countries. It is likely early discharge has an impact on the establishment of breastfeeding. Objective: To critically appraise the evidence on what women value in relation to breastfeeding initiation and support, and investigate the impact early discharge can have on these values.
Background The COVID-19 pandemic is disrupting normal life globally, every area of life is touched. The pandemic demands quick action and as new information emerges, reliable synthesises and guidelines for care are urgently needed. Breastfeeding protects mother and child; its health benefits are undisputed and based on evidence. To plan and support breastfeeding within the current pandemic ...
Purpose This paper aims to explore how the term "mental health literacy" (MHL) is defined and understand the implications for public mental health and educational interventions. Design/methodology/approach An extensive search was conducted by searching PubMed, ERIC, PsycINFO, Scopus and Web of Science. Keywords such as "mental health literacy" and "definition" were used. The ...
babies against harm caused by pathogens (3, 4). Breast-. feeding is also an important source of antioxidants, such. as vitamin C and vitamin E, that prevent or reduce oxida-. tive damages to ...