- Patient Care & Health Information
- Diseases & Conditions
- Schizophrenia
Schizophrenia is a serious mental health condition that affects how people think, feel and behave. It may result in a mix of hallucinations, delusions, and disorganized thinking and behavior. Hallucinations involve seeing things or hearing voices that aren't observed by others. Delusions involve firm beliefs about things that are not true. People with schizophrenia can seem to lose touch with reality, which can make daily living very hard.
People with schizophrenia need lifelong treatment. This includes medicine, talk therapy and help in learning how to manage daily life activities.
Because many people with schizophrenia don't know they have a mental health condition and may not believe they need treatment, many research studies have examined the results of untreated psychosis. People who have psychosis that is not treated often have more-severe symptoms, more stays in a hospital, poorer thinking and processing skills and social outcomes, injuries, and even death. On the other hand, early treatment often helps control symptoms before serious complications arise, making the long-term outlook better.

Products & Services
- A Book: Mayo Clinic Family Health Book
- Newsletter: Mayo Clinic Health Letter — Digital Edition
Schizophrenia involves a range of problems in how people think, feel and behave. Symptoms may include:
- Delusions. This is when people believe in things that aren't real or true. For example, people with schizophrenia could think that they're being harmed or harassed when they aren't. They could think that they're the target for certain gestures or comments when they aren't. They may think they're very famous or have great ability when that's not the case. Or they could feel that a major disaster is about to occur when that's not true. Most people with schizophrenia have delusions.
- Hallucinations. These usually involve seeing or hearing things that other people don't observe. For people with schizophrenia, these things seem real. Hallucinations can occur with any of the senses, but hearing voices is most common.
- Disorganized speech and thinking. Disorganized speech causes disorganized thinking. It can be hard for people with schizophrenia to talk with other people. The answers people with schizophrenia give to questions may not be related to what's being asked. Or questions may not be answered fully. Rarely, speech may include putting together unrelated words in a way that can't be understood. Sometimes this is called word salad.
- Extremely disorganized or unusual motor behavior. This may show in several ways, from childlike silliness to being agitated for no reason. Behavior isn't focused on a goal, so it's hard to do tasks. People with schizophrenia may not want to follow instructions. They may move in ways that are not typical or not appropriate to the social setting. Or they may not move much or respond at all.
- Negative symptoms. People with schizophrenia may not be able to function in the way they could before their illness started. For example, they may not bathe, make eye contact or show emotions. They may speak in a monotone voice and not be able to feel pleasure. Also, they may lose interest in everyday activities, socially withdraw and have a hard time planning ahead.
Symptoms can vary in type and how severe they are. At times, symptoms may get better or worse. Some symptoms may be present at all times.
People with schizophrenia usually are diagnosed in the late teen years to early 30s. In men, schizophrenia symptoms usually start in the late teens to early 20s. In women, symptoms usually begin in the late 20s to early 30s. There also is a group of people — usually women — who are diagnosed later in life. It isn't common for children to be diagnosed with schizophrenia.
Symptoms in teenagers
Schizophrenia symptoms in teenagers are like those in adults, but the condition may be harder to pinpoint. That's because some early symptoms of schizophrenia — those that occur before hallucinations, delusions and disorganization — are commonly seen in many teens, such as:
- Withdrawing from friends and family.
- Not doing well in school.
- Having trouble sleeping.
- Feeling irritable or depressed.
- Lacking motivation.
Also, the use of recreational drugs, such as marijuana, stimulants like cocaine and methamphetamines, or hallucinogens, can cause similar symptoms. Compared with adults with schizophrenia, teens with the condition may be less likely to have delusions and more likely to have hallucinations.
When to see a doctor
People with schizophrenia often don't know that they have a mental condition that needs medical attention. As a result, family or friends often need to get them help.
Helping someone who may have schizophrenia
If people you know have symptoms of schizophrenia, talk to them about your concerns. While you can't force them to seek help, you can offer encouragement and support. You also can help them find a healthcare professional or mental health professional.
If people are a danger to themselves or others, or they don't have food, clothing or shelter, you may need to call 911 in the U.S. or other emergency responders for help. A mental health professional needs to evaluate them.
Some people may need an emergency stay in a hospital. Laws on mental health treatment against a person's will vary by state. You can contact community mental health agencies or police departments in your area for details.
Suicidal thoughts and behavior
Suicidal thoughts and attempts are much higher than average in people with schizophrenia. If a person is in danger of suicide or has made a suicide attempt, make sure that someone stays with that person. Contact a suicide hotline. In the U.S., call or text 988 to reach the 988 Suicide & Crisis Lifeline, available 24 hours a day, seven days a week. Or use the Lifeline Chat. Services are free and confidential. The Suicide & Crisis Lifeline in the U.S. has a Spanish language phone line at 1-888-628-9454 (toll-free).
Proper treatment of schizophrenia can reduce the risk of suicide.
There is a problem with information submitted for this request. Review/update the information highlighted below and resubmit the form.
From Mayo Clinic to your inbox
Sign up for free and stay up to date on research advancements, health tips, current health topics, and expertise on managing health. Click here for an email preview.
Error Email field is required
Error Include a valid email address
To provide you with the most relevant and helpful information, and understand which information is beneficial, we may combine your email and website usage information with other information we have about you. If you are a Mayo Clinic patient, this could include protected health information. If we combine this information with your protected health information, we will treat all of that information as protected health information and will only use or disclose that information as set forth in our notice of privacy practices. You may opt-out of email communications at any time by clicking on the unsubscribe link in the e-mail.
Thank you for subscribing!
You'll soon start receiving the latest Mayo Clinic health information you requested in your inbox.
Sorry something went wrong with your subscription
Please, try again in a couple of minutes
It isn't known what causes schizophrenia. But researchers believe that a mix of genetics, brain chemistry and environment can play a part.
Changes in certain naturally occurring brain chemicals, including neurotransmitters called dopamine and glutamate, may play a part in schizophrenia. Neuroimaging studies show changes in the brain structure and central nervous systems of people with schizophrenia. While researchers haven't yet been able to apply these findings to new treatments, the findings show that schizophrenia is a brain disease.
Risk factors
Although the cause of schizophrenia is not known, these factors seem to make schizophrenia more likely:
- A family history of schizophrenia.
- Life experiences, such as living in poverty, stress or danger.
- Some pregnancy and birth issues, such as not getting enough nutrition before or after birth, low birth weight, or exposure to toxins or viruses before birth that may affect brain development.
- Taking mind-altering — also called psychoactive or psychotropic — drugs as a teen or young adult.
Complications
Left untreated, schizophrenia can lead to severe problems that affect every area of life.
Complications that schizophrenia may cause or be related to include:
- Suicide, suicide attempts and thoughts of suicide.
- Anxiety disorders and obsessive-compulsive disorder, also known as OCD.
- Depression.
- Misuse of alcohol or other drugs, including nicotine.
- Not being able to work or attend school.
- Money problems and homelessness.
- Social isolation.
- Health and medical problems.
- Being victimized.
- Aggressive or violent behavior, though people with schizophrenia are more likely to be assaulted rather than assault others.
There's no sure way to prevent schizophrenia. But staying with your treatment plan can help stop symptoms from returning or getting worse. Researchers hope that learning more about risk factors for schizophrenia may lead to earlier diagnosis and treatment.
- Schizophrenia spectrum and other psychotic disorders. In: Diagnostic and Statistical Manual of Mental Disorders DSM-5-TR. 5th ed. American Psychiatric Association; 2022. https://dsm.psychiatryonline.org. Accessed Jan. 18, 2024.
- Fischer BA, et al. Schizophrenia in adults: Clinical features, assessment, and diagnosis. https://www.uptodate.com/contents/search. Accessed Jan. 18, 2024.
- Stroup TS, et al. Schizophrenia in adults: Maintenance therapy and side effect management. https://www.uptodate.com/contents/search. Accessed Jan. 18, 2024.
- Fisher DJ, et al. The neurophysiology of schizophrenia: Current update and future directions. International Journal of Psychophysiology. 2019; doi:10.1016/j.ijpsycho.2019.08.005.
- Schizophrenia. National Institute of Mental Health. https://www.nimh.nih.gov/health/topics/schizophrenia. Accessed Jan. 18, 2024.
- Schizophrenia. National Alliance on Mental Illness. https://www.nami.org/About-Mental-Illness/Mental-Health-Conditions/Schizophrenia. Accessed Jan. 18, 2024.
- What is schizophrenia? American Psychiatric Association. https://www.psychiatry.org/patients-families/schizophrenia/what-is-schizophrenia. Accessed Jan. 18, 2024.
- Schizophrenia. Merck Manual Professional Version. https://www.merckmanuals.com/professional/psychiatric-disorders/schizophrenia-and-related-disorders. Accessed Jan. 18, 2024.
- Supporting a family member with serious mental illness. American Psychological Association. https://www.apa.org/topics/mental-health/support-serious-mental-illness. Accessed Jan. 18, 2024.
- For friends and family members. Substance Abuse and Mental Health Services Administration. https://www.samhsa.gov/mental-health/how-to-talk/friends-and-family-members. Accessed Jan. 18, 2024.
- For people with mental health problems. Substance Abuse and Mental Health Services Administration. https://www.samhsa.gov/mental-health/how-to-talk/people-with-mental-health-problems. Accessed Jan. 18, 2024.
- Roberts LW, et al. Schizophrenia spectrum and other psychotic disorders. In: The American Psychiatric Association Publishing Textbook of Psychiatry. 7th ed. American Psychiatric Association Publishing; 2019. https://psychiatryonline.org. Accessed Jan. 18, 2024.
- Allen ND (expert opinion). Mayo Clinic. April 17, 2024.
- Leung JG (expert opinion). Mayo Clinic. April 16, 2024.
- Antipsychotic drugs. Merck Manual Professional Version. https://www.merckmanuals.com/professional/psychiatric-disorders/schizophrenia-and-related-disorders/antipsychotic-drugs. Accessed Jan. 19, 2024.
Associated Procedures
- Symptoms & causes
- Diagnosis & treatment
- Doctors & departments
Mayo Clinic does not endorse companies or products. Advertising revenue supports our not-for-profit mission.
- Opportunities
Mayo Clinic Press
Check out these best-sellers and special offers on books and newsletters from Mayo Clinic Press .
- Mayo Clinic on Incontinence - Mayo Clinic Press Mayo Clinic on Incontinence
- The Essential Diabetes Book - Mayo Clinic Press The Essential Diabetes Book
- Mayo Clinic on Hearing and Balance - Mayo Clinic Press Mayo Clinic on Hearing and Balance
- FREE Mayo Clinic Diet Assessment - Mayo Clinic Press FREE Mayo Clinic Diet Assessment
- Mayo Clinic Health Letter - FREE book - Mayo Clinic Press Mayo Clinic Health Letter - FREE book
5X Challenge
Thanks to generous benefactors, your gift today can have 5X the impact to advance AI innovation at Mayo Clinic.
Disorganized Schizophrenia (Hebephrenia)
Disorganized schizophrenia, or hebephrenia, is one of the five subtypes of schizophrenia that is no longer recognized as a separate diagnosis in the DSM but the symptoms still exist and may signal oncoming psychosis. Learn more here.

Disorganized schizophrenia (hebephrenia) is one of the five subtypes of schizophrenia that are no longer included in the Diagnositic and Statistical Manual of Mental Disorders (DSM), the manual used by health care professionals published by the American Psychiatric Association .
The symptoms of disorganized thoughts and behavior are known as hebephrenia. Hebephrenia is characterized by disorganized behavior and speech as well as disturbance in emotional expression, known as mood incongruence.
Hallucinations and delusions are less pronounced with disorganized schizophrenia , though there is evidence of these symptoms occurring.
Symptoms of Disorganized Schizophrenia
Disorganized speech in schizophrenia—sometimes referred to as clanging —can cause people to have difficulty concentrating and maintaining a train of thought, which manifests in the way they speak.
People with disorganized speech might speak incoherently, respond to questions with unrelated answers, say illogical things, or shift topics frequently. Signs of disorganized speech involve the following:
Loose associations: Rapidly shifting between topics with no connections between topics
Perseveration: Repeating the same things over and over again
Made up words that only have meaning to the speaker
Use of rhyming words without meaning
When cognitive disorganization is severe, it can be nearly impossible to understand what the person is saying.
Disorganized behavior in schizophrenia negatively impacts goal-directed behavior. A person with disorganized schizophrenia is likely to have difficulty beginning a specific task (ex: cooking a meal) or difficulty finishing a task. Independent functioning is exceptionally difficult due to this gross disorganization.
Disorganized behavior can manifest as the following:
A decline in overall daily functioning
Unpredictable or inappropriate emotional responses
Lack of impulse control
Behaviors that appear bizarre or lack purpose
Routine behaviors such as bathing, dressing, or brushing teeth can be severely impaired or lost.
Inappropriate affect refers to a person’s emotional responses, including the way emotions are expressed (ex: smiling when feeling happy.)
People with disorganized schizophrenia exhibit flat affect , which means that they show little or no emotions in their facial expressions, voice tone, or mannerisms. At times they exhibit affect that is inappropriate to the situation, such as laughing at something sad. In addition to lack of emotional expression, people with disorganized schizophrenia are likely to experience other negative symptoms, including failing to make eye contact and blunt facial expression.
Disorganized schizophrenia is more likely to occur during early onset of the illness—between the ages of 15 and 25. Earlier age of onset is traditionally associated with a worse prognosis due to lower educational achievement, more prominent negative symptoms, and cognitive impairments.
Early detection, diagnosis, and treatment of schizophrenia contributes to better outcomes.
Beginning treatment as soon as possible is crucial to making a recovery. Treatment for disorganized schizophrenia involves a multimodal approach, including the following:
Medication management : Medication for schizophrenia can help reduce hallucinations and delusions, paranoia, and disordered thinking. Finding the right medication depends on the prominent symptoms of the disease.
Psychotherapy : Cognitive Behavioral Therapy (CBT) is recommended to reduce certain symptoms and enhance overall functioning. Through CBT, individuals identify target problems and work to develop coping strategies specific to those issues.
Life skills training: Assistance with life skills can help individuals with disorganized schizophrenia improve social interactions and increase daily living skills, with a goal of increasing independence.
Supported employment services: Individuals with disorganized schizophrenia benefit from training in the area of finding and maintaining employment.
Family education and support: Individuals with disorganized schizophrenia benefit from ongoing contact with family. Support to educate family about treatment and how to support a family member with schizophrenia is crucial. Family support increases family member’s understanding of the disorder and helps family members develop coping strategies.
A multi-component treatment for the first episode of psychosis in the early stage of schizophrenia using a recovery-oriented model team approach known as coordinated specialty care (CSC) (e.g., psychotherapy, medication case management, employment, and education support and family resources) has been found to be effective.
Though the signs of disorganized schizophrenia tend to appear at a younger age, they can be difficult to spot. The symptoms of this subtype are often very gradual and unlikely to subside. With appropriate and ongoing treatment, however, the prognosis for disorganized schizophrenia improves.
Assistance with daily living skills, educational attainment, employment services, and family support play a key role in improving the course of the disease for individuals diagnosed with disorganized schizophrenia.
- American Psychiatric Association, “Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition”, American Psychiatric Publishing, Washington, DC, (2013): Pages 99-105.
- Shean, G., “Empirically Based Psychosocial Therapies for Schizophrenia: The Disconnection between Science and Practice”, Schizophrenia Research and Treatment, Volume 2013 (2013).
- National Institites of Health (NIH). National Institute of Mental Health (NIMH). What is schizophrenia? Available at https://www.nimh.nih.gov/health/publications/schizophrenia Accessed February 8, 2023.
- Share via facebook
- Share via pinterest
- Share via twitter
- Share via mail
More Like This
Is schizophrenia genetic.

Schizophrenia: Everything You Need to Know

Schizophrenia Stages: What to Know About Progression

How to Prevent Schizophrenia Symptoms

- Schizophrenia
- Schizophrenia in Teens
- Schizophrenia in Children
- Overview of Symptoms
- Positive Symptoms
- Negative Symptoms
- Tests & Diagnosis
- Overview of Treatment
- Drug Therapies
- Medication Side Effects
- Medication Compliance
- Complementary & Alternative Therapies
- Hospitalization
- Complications
- Diet & Exercise
- Family & Relationships
- View Full Guide
- Schizophrenia Symptoms

- What Is Schizophrenia?
Schizophrenia changes how you think, feel, and act. It might affect you differently from someone else. The symptoms can come and go, too. No one has all of them all of the time.
They usually start between the ages of 16 and 30. Those assigned male at birth (AMAB) often get them earlier than those assigned female. Often, there is a gradual change in the person before obvious symptoms start. This is sometimes called the prodrome phase.
When the disease is in full swing and symptoms are severe, the person with schizophrenia can't tell when certain ideas and perceptions they have are real or not. This happens less often as they get older.
People with the condition usually aren't aware that they have it until a doctor or counselor tells them. They won't even realize that something is seriously wrong. If they do happen to notice symptoms, such as not being able to think straight, they might blame it on things including stress or being tired.
If you're concerned that you or someone you know is showing signs of schizophrenia, talk to a doctor or counselor.
What Are the Five Symptoms of Schizophrenia?
When you have schizophrenia, typically there are five main categories of symptoms. These include:
Delusions. Strong beliefs that aren’t based on reality, such as fear that you’re being harassed or harmed by someone or are receiving secret messages.
Hallucinations. Seeing or hearing things (such as voices) that aren’t actually there.
Incoherent speech. Stopping mid-sentence, jumping from thought to thought, or using nonsensical words.
Unusual movements. Moving repetitively, having abnormal posture, or agitated movements.
Negative symptoms. Lacking typical behaviors such as bathing, socializing, taking care of basic needs, or showing emotion.
Positive Symptoms of Schizophrenia
Positive symptoms are highly exaggerated ideas, perceptions, or actions that show the person can’t tell what’s real from what isn’t. Here the word "positive" means the presence (rather than absence) of symptoms. They can include:
Hallucinations. People with schizophrenia might hear, see, smell, or feel things no one else does. The types of hallucinations in schizophrenia include:
- Auditory. The person most often hears voices in their head. They might be angry or urgent and demand that they do things. It can sound like one voice or many. They might whisper, murmur, or be angry and demanding.
- Visual. Someone might see lights, objects, people, or patterns. Often it’s loved ones or friends who are no longer alive. They may also have trouble with depth perception and distance.
- Olfactory and gustatory. This can include good and bad smells and tastes. Someone might believe they’re being poisoned and refuse to eat.
- Tactile. This creates a feeling of things moving on your body, such as hands or insects.
Delusions. These are beliefs that seem strange to most people and are easy to prove wrong. The person affected might think someone is trying to control their brain through a TV or that the FBI is out to get them. They might believe they're someone else, like a famous actor or the president, or that they have superpowers. Types of delusions include:
- Persecutory delusions. These may make you feel that someone is after you or that you’re being stalked, hunted, framed, or tricked.
- Referential delusions. When a person believes that public forms of communication, such as song lyrics or a gesture from a TV host, are a special message just for them.
- Somatic delusions. These center on the body. The person thinks they have a terrible illness or bizarre health problem such as worms under the skin or damage from cosmic rays.
- Erotomanic delusions. A person might be convinced a celebrity is in love with them or that their partner is cheating. Or they might think people they’re not attracted to are pursuing them.
- Religious delusions. Someone might think they have a special relationship with a deity or that they’re possessed by a demon.
- Grandiose delusions. The affected individuals might consider themselves to be a major figure on the world stage, such as an entertainer or a politician.
Confused thoughts and disorganized speech. People with schizophrenia can have a hard time organizing their thoughts. They might not be able to follow along when you talk to them. Instead, it might seem like they're zoning out or distracted. When they talk, their words can come out jumbled and not make sense.
Trouble concentrating. For example, someone might lose track of what's going on in a TV show as they're watching.
Movement disorders. Some people with schizophrenia can seem jumpy. At times, they'll make the same movements over and over again. But sometimes, they might remain perfectly still for hours at a stretch, which experts call being catatonic . Contrary to popular belief, people with the disease usually aren't violent.
Negative Symptoms of Schizophrenia: Things That Might Stop Happening
Negative symptoms refer to an absence or lack of normal mental function involving thinking, behavior, and perception. You might notice:
Lack of pleasure. The person may not seem to enjoy anything anymore. A doctor will call this anhedonia.
Trouble with speech. They might not talk much or show any feelings. Doctors call this alogia.
Flattening. The person with schizophrenia might seem like they have a terrible case of the blahs. When they talk, their voice can sound flat, like they have no emotions. They may not smile normally or show usual facial emotions in response to conversations or things happening around them. A doctor might call this affective flattening.
Withdrawal. This might include no longer making plans with friends or becoming a hermit. Talking to the person can feel like pulling teeth; if you want an answer, you have to really work to pry it out of them. Doctors call this apathy.
Struggling with the basics of daily life. They may stop bathing or taking care of themselves.
No follow-through. People with schizophrenia have trouble staying on schedule or finishing what they start. Sometimes, they can't get started at all. A doctor might call this avolition.
Decreased desire to socialize. There’s not much motivation to be around other people, and interactions can be awkward.
Depression has some of the same symptoms, too. They can be hard to spot, especially in teens, because even healthy teens can have big emotional swings between highs and lows.
Cognitive Symptoms and Thinking Problems
These symptoms reflect how well the person’s brain learns, stores, and uses information.
Someone with schizophrenia might have a hard time with their working memory. For example, they may not be able to keep track of different kinds of facts at the same time, such as a phone number plus instructions.
Along with having trouble paying attention, it can be hard for them to organize their thoughts and make decisions.
Schizophrenia Symptoms in Teenagers
When someone gets a schizophrenia diagnosis before the age of 18, it’s called early-onset schizophrenia . It can be tricky to diagnose schizophrenia in teens because many of the symptoms are typical for normal development, such as:
- Withdrawal from friends and family
- Difficulty keeping up with schoolwork
- Trouble sleeping
- Irritability or depressed mood
- Lack of motivation
Teens who use marijuana, methamphetamines, or LSD can also show symptoms similar to those of schizophrenia.
Unlike adults with the disorder, teens with schizophrenia are more likely to have visual hallucinations and less likely to have delusions. Some common complications of schizophrenia are alcohol and drug abuse, other mental disorders, self-harm, and thoughts of suicide.
Being aware of the symptoms of schizophrenia can help you recognize when someone may be dealing with the disorder. If you are concerned someone you love has schizophrenia, have a conversation about what you’re seeing. You can be a support and source of encouragement if they choose to seek medical help.
Although you can’t make someone go to the doctor for symptoms of schizophrenia, there are certain situations where you may need to call on emergency help. If someone is posing a danger to themselves or others, or if they can’t properly take care of themselves, certain support can help, such as 911 or other emergency responders. In some cases, your loved one may need to be hospitalized.
Schizophrenia Symptoms FAQs
Can a person with schizophrenia have a normal life?
With proper treatment, people with schizophrenia can lead fulfilling and meaningful lives. Although the symptoms of the disease can cause many disruptions and hardships, consistent use of medication, therapy, and social and emotional support can help people manage their disease well and function normally.
What are usually the first signs of schizophrenia?
Some of the earliest signs of schizophrenia can be subtle. You may notice someone is having mood swings, or calling or coming around less often. They may start neglecting things they’re supposed to do such as housework, schoolwork, or personal hygiene. After these early signs, you may start seeing active symptoms such as delusions and hallucinations.
- Early Signs of Schizophrenia
- Schizophrenia Tests
- Schizophrenia Medication

Top doctors in ,
Find more top doctors on, related links.
- Schizophrenia Health Reference
- Schizophrenia Health Slideshows
- Schizophrenia Health Blogs
- Schizophrenia Health Videos
- Schizophrenia Health Medications
- Find a Psychiatrist
- Anxiety/Panic Disorders
- Bipolar Disorder
- Mental Health
- Psychotic Depression
- Schizoaffective Disorder
- Schizophreniform Disorder
- Smoking Cessation
- Schizophrenia Overview
- Schizophrenia Causes
- Schizophrenia Diagnosis
- Schizophrenia Treatment
Search Results

- Disorganised symptoms
What are disorganised symptoms in people with schizophrenia?
Key features of the symptoms of disorganisation include disorganised speech and behaviour, as well as inappropriate affect. Severely disorganised speech is difficult to follow, being incoherent, irrelevant and/or illogical. These symptoms are sometimes referred to as positive formal thought disorder. Disorganised speech may also be deprived of content, which is sometimes referred to as negative formal thought disorder symptoms. Disorganised behaviour includes bizarre or inappropriate behaviour, actions or gestures. Inappropriate (incongruous) affect involves exhibiting incorrect emotional responses for a given context.
Symptoms of disorganisation have been identified as risk factors for poor illness outcome, and have a significant negative effect on a person’s day-to-day functioning and quality of life. There is evidence to suggest that disorganisation symptoms may be associated with impaired cognitive performance .
What is the evidence regarding disorganised symptoms?
Moderate to high quality evidence found small to medium-sized associations between positive and negative formal thought disorder and poor cognition in the areas of memory , attention , processing speed , planning , semantic processing , social cognition , and social functioning . Positive formal thought disorder was particularly associated with poor inhibition and syntactic comprehension, while negative formal thought disorder was particularly associated with poor fluency. There was also a medium-sized association between poor insight (overall unawareness of having a mental disorder) and increased disorganised symptoms.
There was a small to medium-sized effect of more formal thought disorder symptoms in people with schizophrenia than in people with bipolar disorder. This effect was significant only in non-acute, stable patients.
High quality evidence shows significant concordance of disorganisation symptoms in siblings with schizophrenia. Low quality evidence suggests unclear concordance in twins with schizophrenia.
February 2022
Image: ©carlosgardel – stock.adobe.com
NeuRA Libraries
Bipolar disorders library.
- Early detection
- Outcome assessment tools
- Attachment styles
- Dissociation
- Minor physical anomalies
- Mixed symptoms
- Mood cycling
- Movement disorders
- Neurological soft signs
- Olfactory functioning
- Personality and temperament
- Predominant polarity
- Psychotic symptoms
- Self-esteem
- Sleep disturbance
- Cognition and bipolar disorder symptoms
- Cognition and bipolar disorder type
- Cognition and functioning
- Cognition in bipolar disorder and major depression
- Cognition in bipolar disorder and schizophrenia
- Cognition in children with bipolar disorder
- Cognition in first-episode bipolar disorder
- Cognition in late-life bipolar disorder
- Cognition in relatives
- Decision making
- Episodic future thinking
- Executive functioning
- IQ and global cognition
- Metacognition
- Processing speed
- Reasoning and problem solving
- Social cognition
- Visuospatial ability
- Acupuncture
- Blue light blocking glasses
- Bright light therapy
- Electroconvulsive therapy
- Exercise therapy
- Sleep deprivation
- Transcranial direct-current stimulation
- Transcranial magnetic stimulation
- Vagus nerve stimulation
- Carbamazepine
- Lamotrigine
- Levetiracetam
- Licarbazepine
- Oxcarbazepine
- All antidepressants
- Tranylcypromine
- Venlafaxine
- Aripiprazole
- Cariprazine
- Haloperidol
- Paliperidone
- Risperidone
- Ziprasidone
- Adenosine modulators
- Anti-inflammatories
- Antidiabetics
- Benzodiazepines
- Calcium channel blockers
- Cholinesterase inhibitors
- Dopaminergic modulators
- Essential fatty acids
- Estrogen modulators
- Glutamatergic modulators
- Herbal and nutrients
- Medicinal cannabis
- Norepinephrine inhibitors
- Thyroid hormones
- Medication during pregnancy and breastfeeding
- Medication for aggression and agitation
- Medication for bipolar II disorder
- Medication for bipolar versus unipolar depression
- Medication for children
- Medication for cognitive symptoms
- Medication for dual diagnosis
- Medication for elderly people
- Medication for first-episode bipolar disorder
- Medication for high-risk groups
- Medication for mixed states
- Medication for rapid cycling
- Medication for relapse prevention
- Medication for suicide and self-harm prevention
- Medication for treatment resistance
- Mode of administration
- Placebo response
- Polypharmacy
- Switching medications
- Cognitive behavioural therapy
- Cost of therapies
- Crisis planning
- Educational therapies
- Family intervention
- Group therapy
- Integrated care
- Interpersonal and social rhythm therapy
- Mindfulness
- Peer support
- Shared decision making
- Telemental health
- Therapeutic relationships
- User-held records
- Vocational therapies
- Therapies for children
- Therapies for cognition
- Therapies for dual diagnosis
- Therapies for first-episode bipolar disorder
- Therapies for high-risk groups
- Therapies for internalised stigma
- Therapies for parents with bipolar disorder
- Therapies for trauma-related symptoms
- Therapies for treatment non-adherence
- Therapies for weight gain
- Autonomic nervous system anomalies
- Behaviour and psychopathology
- Eye tracking anomalies
- Face emotion processing
- Height and BMI
- IQ and academic performance
- Motor dysfunction
- Stress responsivity
- Adult life events
- Childhood adversity
- Environmental toxins
- Familial factors
- Infectious agents
- Maternal diet during pregnancy
- Maternal illness during pregnancy
- Obstetric complications
- Parental age at birth
- Parental education
- Parental psychological factors
- Rheumatoid arthritis
- Socioeconomic status
- Substance use
- Traumatic brain injury
- Winter birth
- Age at onset
- Attitudes to medication
- Criminal offending, aggression and violence
- Criminal victimisation
- Cultural differences
- Dietary intake
- Drug and alcohol use
- First-episode bipolar disorder
- Functional outcomes
- Homelessness
- Pathways to care
- Pediatric bipolar disorder
- Physical activity
- Physical health monitoring
- Quality of care
- Quality of life
- Relationships
- Religiosity
- Suicide and self-harm
- Treatment non-adherence
- Treatment resistance
- Familial coaggregation
- Impact on families
- Physical anomalies in relatives
- Psychopathology in relatives
- Brain pH and lactate
- Complex I and IV
- Gut microbiota
- Homocysteine
- Hypothalamic-pituitary-adrenal axis
- Inflammation and immune system dysfunction
- Insulin-like growth factor
- Neurometabolites
- Neuropeptides
- Neurotrophins
- NMDA receptor function
- Oxidative stress
- S100 proteins
- Functional magnetic resonance imaging
- Positron emission tomography / single-photon emission computed tomography
- Eye movement dysfunction
- Mismatch negativity
- Prepulse inhibition
- Cellular changes
- Diffusion tensor imaging
- Magnetic resonance imaging
- Optical coherence tomography
- Dermatoglyphics
- Morphometrics
- Telomere length
- Anxiety disorders
- Attention deficit hyperactivity disorder
- Eating disorders
- Impulsivity-related disorders
- Obsessive-compulsive disorder
- Personality disorders
- Pervasive developmental disorders
- Post-traumatic stress disorder
- Somatic symptom disorder
- Autoimmune disease
- Blood disorders
- Cerebrovascular disease
- Digestive disorders
- Fibromyalgia
- Heart disease
- Infectious diseases
- Metabolic syndrome
- Musculoskeletal and connective tissues
- Optical alterations
- Osteoporosis
- Pain and migraine
- Parkinson’s disease
- Peripheral vascular disease
- Premenstrual syndrome
- Respiratory disease
- Skin disorders
- Sleep apnea
- Thyroid disorders
- Venous thromboembolism
- Visual impairment
- Wilson’s disease
- Policy and law
- Incidence in children
- Incidence in elderly people
- Incidence in forensic settings
- Incidence in homeless people
- Incidence in indigenous populations
- Incidence in males vs. females
- Incidence in migrants
- Incidence in veterans
- Worldwide incidence
- Prevalence in children
- Prevalence in elderly people
- Prevalence in forensic settings
- Prevalence in homeless populations
- Prevalence in indigenous populations
- Prevalence in males vs. females
- Prevalence in migrants
- Prevalence in primary care settings
- Prevalence in problem gamblers
- Prevalence in veterans
- Spatial variation in prevalence
- Worldwide prevalence
- Privacy and security
- What is bipolar disorder and how is it diagnosed?
- Which risk factors are associated with bipolar disorder?
- Which treatments are most effective?
- Will family members be affected?
Post-Traumatic Stress Disorder Library
- Anger and aggression
- Hyperarousal
- Negative thoughts and mood
- Perceptions of defeat and entrapment
- Cognitive failures
- General cognition
- Information processing
- Biofeedback
- Hyperbaric oxygen
- All pharmaceutical treatments for prevention of PTSD
- All pharmaceutical vs. psychological treatments
- Alpha blockers
- Anticonvulsants
- Antidepressants
- Antipsychotics
- Placebo effect
- Psychedelics
- Acceptance and commitment therapy
- All psychological therapies for PTSD
- Animal-assisted psychotherapy
- Brief eclectic psychotherapy
- Cognitive therapies
- Creative arts therapy
- Emotion-focussed therapies
- Emotional freedom techniques
- Exposure therapies
- Expressive writing
- Eye movement desensitization and reprocessing
- Family therapies
- Group therapies
- Hypnotherapy
- ICU diaries
- Imagery rehearsal therapy
- Interpersonal psychotherapy
- Memory specificity training
- Metacognitive therapy
- Mindfulness and meditation
- Narrative exposure therapy
- Present-centred therapy
- Psychoeducation
- Self-help treatment
- Stress inoculation training
- Stress management
- Structured approach therapy
- Supportive counselling
- Trauma affect regulation
- Therapies for adults with a history of childhood abuse
- Therapies for children and adolescents
- Therapies for complex PTSD
- Therapies for people living in low- and middle-income countries
- Therapies for prevention of PTSD
- Therapies for refugees and asylum seekers
- Therapies for soldiers and veterans
- Cognitive and psychological factors
- Family and social factors
- Previous trauma exposure
- Abuse and violence
- Bereavement
- Direct vs. indirect exposure
- Epidemics and pandemics
- Imprisonment
- Intentional vs. unintentional traumas
- Interpersonal vs. non-interpersonal traumas
- Migration and displacement
- Moral injury
- Physical injury and illness
- Pregnancy and childbirth
- Road traffic accidents
- Time post-trauma
- Trauma severity
- War and terrorism
- Criminal offending
- Forgiveness
- Functioning
- Illness onset
- Post-traumatic growth
- Catecholamines
- fMRI and PET
- Hypothalamic-Pituitary-Adrenal axis
- Immune system
- Bipolar disorder
- Conduct disorder
- Conversion disorder
- Depressive disorders
- Chronic fatigue syndrome
- Chronic pain and fibromyalgia
- Irritable bowel syndrome
- Temporomandibular disorder
- Drugs, alcohol and smoking
- Incidence in abuse and violence survivors
- Incidence in bereaved people
- Incidence in caregivers
- Incidence in children and adolescents
- Incidence in criminal offenders
- Incidence in disaster survivors
- Incidence in epidemic and pandemic survivors
- Incidence in firefighters
- Incidence in healthcare workers
- Incidence in homeless populations
- Incidence in humanitarians
- Incidence in indigenous people
- Incidence in journalists
- Incidence in jurors
- Incidence in medical patients
- Incidence in police officers
- Incidence in problem gamblers
- Incidence in psychiatric inpatients
- Incidence in public transport drivers
- Incidence in refugees and asylum seekers
- Incidence in rescue teams
- Incidence in road traffic accident survivors
- Incidence in soldiers and veterans
- Incidence in war and terrorism survivors
- Prevalence in abuse and violence survivors
- Prevalence in bereaved people
- Prevalence in caregivers
- Prevalence in children and adolescents
- Prevalence in disaster survivors
- Prevalence in epidemic and pandemic survivors
- Prevalence in firefighters
- Prevalence in healthcare workers
- Prevalence in humanitarians
- Prevalence in indigenous people
- Prevalence in journalists
- Prevalence in jurors
- Prevalence in medical patients
- Prevalence in police officers
- Prevalence in psychiatric patients
- Prevalence in refugees
- Prevalence in rescue teams
- Prevalence in road traffic accident survivors
- Prevalence in soldiers and veterans
- Prevalence in train drivers
- Prevalence in war and terrorism survivors
Schizophrenia Library
- Schizoaffective disorder
- Schizophrenia
- Schizophreniform disorder
- Functional laterality
- Negative symptoms
- Pain sensitivity
- Positive symptoms
- Psychotic relapse
- Temperature regulation
- Cognition in high-risk groups
- Cognition in schizophrenia and bipolar disorder
- Cognitive functioning related to symptoms
- Defeatist performance beliefs
- Psychomotor ability
- Time perception
- Tone perception
- Voice patterns
- All antipsychotics versus placebo
- Bromperidol
- Chlorpromazine
- First versus second generation
- Flupentixol
- Fluphenazine
- Fluspirilene
- Levomepromazine
- Penfluridol
- Perphenazine
- Piperacetazine
- Pipotiazine
- Thioridazine
- Trifluoperazine
- Zuclopenthixol
- Amisulpride
- Blonanserin
- Brexpiprazole
- Carpipramine
- Clocapramine
- Iloperidone
- Mosapramine
- Perospirone
- Remoxipride
- Second versus second generation
- Amphetamines
- Anti-inflammatory
- Anticholinergic
- Anticraving agents
- Beta blockers
- Cholinergic medications
- Erythropoietin
- GABA agonists
- Glutamate receptor modulators
- Herbal medicines
- Mood stabilisers
- Promethazine
- Serotonin modulators
- Sodium nitroprusside
- Testosterone
- Cannabidiol
- Herbal medicine
- Medications during pregnancy and breastfeeding
- Medications for aggression and agitation
- Medications for best adherence
- Medications for childhood and early-onset schizophrenia
- Medications for cognitive symptoms
- Medications for constipation
- Medications for depressive symptoms
- Medications for dual diagnosis
- Medications for elderly people and people with late-onset schizophrenia
- Medications for first-episode psychosis
- Medications for hyperprolactinemia
- Medications for hypersalivation
- Medications for movement disorders
- Medications for negative symptoms
- Medications for relapse prevention
- Medications for schizoaffective disorder
- Medications for sexual dysfunction
- Medications for sleep disturbance
- Medications for smoking cessation
- Medications for social functioning
- Medications for treatment-resistant schizophrenia
- Medications for weight gain
- Therapies and medications for high-risk groups
- Bone density
- Cardiometabolic changes and weight gain
- Constipation
- Extrapyramidal
- Hyperprolactinaemia
- Hypersalivation
- Hyponatraemia
- Neuroleptic malignant syndrome
- Neutropenia
- Oculogyric crisis
- Pancreatitis
- Polycystic ovarian syndrome
- Sexual dysfunction
- Thyroid dysfunction
- Transcranial direct current stimulation
- Animal-assisted therapy
- Art and drama therapies
- Case management
- Community care
- Crisis intervention
- Dance therapy
- Day centres and day hospitals
- Dialectical behavioural therapy
- Distraction techniques
- Enriched intervention
- Genetics counselling
- Home-based care
- Inpatient and outpatient care
- Life skills programs
- Metacognitive training
- Monetary incentives
- Morita therapy
- Music therapy
- Nidotherapy
- Open dialogue approach
- Physical restraint
- Prevention programs
- Problem solving skills training
- Psychodynamic psychotherapy
- Strengths-based delivery
- Supported housing
- Supportive therapy
- Therapeutic relationship
- Token economies
- Trauma-focused therapies
- Virtual reality and avatar therapy
- Therapies for childhood onset and early onset schizophrenia
- Therapies for fathers with schizophrenia
- Therapies for first-episode psychosis
- Therapies for insight
- Therapies for mothers with schizophrenia
- Therapies for negative symptoms
- Therapies for positive symptoms
- Therapies for PTSD symptoms
- Therapies for quality of life
- Therapies for schizoaffective disorder
- Therapies for smoking
- Therapies for social functioning
- Therapies for treatment resistance
- Therapies for unemployment
- Behavioural disturbances and psychopathology
- Dermatoglyphic anomalies
- Face emotion processing anomalies
- Height and body mass index
- Olfactory identification deficits
- Speech and hearing deficits
- Stress responsivity anomalies
- Family relationships
- Genetic and non-genetic risk
- Latitude, climate and winter birth
- Marital status
- Maternal diet and body mass index
- Sex differences
- Social capital
- Urban environment
- Genetics overview
- Childhood and early-onset schizophrenia
- Duration of untreated psychosis
- Duration of untreated psychosis and outcomes
- Electronic device use
- First-episode psychosis
- Late-onset schizophrenia
- Remission and recovery
- Stigma and attitudes towards mental health
- Treatment adherence
- Treatment-resistance
- Cognition in first-degree relatives
- Collection of family history
- Familial coaggregation with bipolar disorder
- Physical anomalies in first-degree relatives
- Cortical release signs
- Cholesterol
- Endocannabinoids
- Hormonal changes
- Inflammation and the immune system
- Nitric oxide
- S100 Proteins
- Synaptic proteins
- Trace elements
- Vascular endothelial growth factor
- Magnetic resonance spectroscopy
- Positron emission tomography
- Single photon emission computed tomography
- Electroencephalography
- Magnetoencephalography
- Brain weight
- Computed tomography
- Neuronal changes
- Arcuate fasciculus
- Basal ganglia
- Cingulate cortex
- Corpus callosum
- Default mode network
- Frontal lobe
- Hippocampus
- Occipital lobe
- Parietal lobe
- Temporal lobe
- Ventricular system
- Whole brain volume
- Autism spectrum disorders
- Dissociative disorders
- Intellectual and learning disabilities
- Auditory system dysfunction
- Autoimmune diseases
- Dental disease
- Polycistic ovary syndrome
- Postoperative complications
- Reproductive and urological disorders
- Respiratory system dysfunction
- Underweight
- Incidence in ethnic groups
- Incidence in refugees
- Spatial variation in incidence
- Prevalence in inpatients
- Prevalence in veterans and conflict settings
- What is schizophrenia and how is it diagnosed?
- Which risk factors are associated with schizophrenia?
- Would my treatment change if I also have another disorder?
Podcast Library
- Hallucinations
- The placebo effect
Mind Diagnostics is user-supported. If you buy through a link on the site, we earn a commission from BetterHelp at no cost to you. Learn More
The DSM-5 Criteria for Schizophrenia
Written by Kyrsten Rice · Reviewed by Melinda (Santa) Gladden, LCSW · December 09, 2023 ·
- Share to Facebook
- Send as Email
- Copy link Copied
Schizophrenia is a chronic and severe mental health disorder that affects how a person thinks, feels, and behaves. It's often characterized by episodes of psychosis, featuring delusions, hallucinations, and disorganized thinking. This disorder can be profoundly disabling, impacting daily functioning and quality of life.
DSM-5 Criteria for Schizophrenia
The DSM-5, a critical tool for mental health professionals, defines schizophrenia with specific criteria. A diagnosis requires two or more of the following symptoms, present for a significant portion of time during a one-month period:
- Hallucinations.
- Disorganized speech.
- Grossly disorganized or catatonic behavior.
- Negative symptoms (e.g., reduced emotional expression).
One of the symptoms must be either (1), (2), or (3). Additionally, continuous signs of the disturbance must persist for at least six months.
Causes of Schizophrenia
- Genetics: A higher risk if there is a family history of schizophrenia.
- Brain structure and chemistry: Imbalances in neurotransmitters may play a role.
- Environmental factors: Stressful or traumatic events might trigger schizophrenia in those predisposed to it.
- Developmental factors: Issues during brain development before birth.
Treatment Options for Schizophrenia
- Antipsychotic medications: These are the cornerstone of schizophrenia treatment.
- Psychotherapy: Cognitive-behavioral therapy (CBT) and other forms can help manage symptoms.
- Psychosocial interventions: These include skills training, employment assistance, and social skills training.
- Coordinated specialty care: A team-based, holistic approach to treatment, especially effective in early-stage schizophrenia.
Support Resources for Schizophrenia
- Mental Health America (MHA) and National Alliance on Mental Illness (NAMI): Provide educational resources and support groups.
- Local community mental health centers: Offer various services, from therapy to social support.
- Online forums: Offer a platform for sharing experiences and advice.
Understanding schizophrenia is the first step in combating stigma and ensuring those affected receive the support and treatment they need. As research continues to evolve, more effective treatments and support systems are likely to emerge.
Find out if you have Schizophrenia
Take this mental health test. It's quick, free, and you'll get your confidential results instantly.
Mental health conditions are real, common, and treatable. If you or someone you know thinks you are suffering from schizophrenia then take this quick online test or click to learn more about the condition.
Take test Learn more
Related articles

Mild Schizophrenia: What It Means for You
Schizophrenia is a mental health condition that makes it very tough for people to differentiate delusions from reality. People who have schizophrenia often experience...

Should You Take a Schizophrenia Test?
You probably have at least a modest idea of what schizophrenia is already. Still, you need to know that it is a mental health condition that can cause people to experience...

Top 5 Movies to Understand Schizophrenia Better
Schizophrenia is a very serious mental health condition, but many people fail to understand what it’s really all about. Some people have misconceptions about schizophrenia...
Need help? We recommend the following therapists
Gwendolyn downing.
- Gwendolyn can help you with: Stress
- Trauma and abuse
- Self esteem
- Relationship issues
- Family conflicts
- Intimacy-related issues
- Eating disorders
- Parenting issues
- Anger management
- Career difficulties
- Bipolar disorder
- Coping with life changes
- Compassion fatigue
Connie Drew
- Connie can help you with: Stress
Ingrid Johnson
Ma, lpc, ncc.
- Ingrid can help you with: Stress
- Sleeping disorders
- Disorders & Issues
- Schizophrenia
Positive Symptoms Of Schizophrenia: The Disorganized Dimension And Negative Symptoms
Symptoms of schizophrenia disorganization.
Schizophrenia is a complex mental health condition characterized by a variety of symptoms that can significantly impact an individual's ability to think, feel, and behave clearly. Among these, disorganized symptoms are particularly challenging as they directly affect the coherence and structure of thought and action. Disorganized symptoms can be broadly categorized into disorganized speech and behavior, each with its own set of manifestations.
- Derailment— Individuals may abruptly shift from one topic to another without any logical connection. This makes it difficult for the listener to follow the conversation.
- Word Salad—Speech may become so fragmented and disconnected that it resembles a "word salad," where words are put together without any apparent meaning or logic, rendering the conversation nearly impossible to comprehend.
- Contrary Actions—Actions that defy social norms are a hallmark of disorganized behavior. For instance, a person might wear heavy winter clothing on a hot summer day without any logical reason.
- Inappropriate Emotions—Emotional responses may be completely out of sync with the situation, such as laughing during a serious or sad moment.
These symptoms of disorganization in schizophrenia stand out because they significantly disrupt an individual's ability to function normally in daily life. Disorganized speech makes effective communication a challenge, while disorganized behavior can lead to difficulties in performing routine tasks and social interactions. Understanding these symptoms is crucial for recognizing the challenges faced by individuals with schizophrenia and providing them with the appropriate support and treatment.
Exploring Disorganized Thinking
Disorganized thinking in schizophrenia is characterized by a severe disruption in the logical flow of thoughts, manifesting in speech that makes little sense, if any. This condition can significantly impair communication, rendering normal conversation difficult. Patients may frequently lose their train of thought, respond to questions with unrelated answers, or be unable to focus on a single topic. Illustrative case vignettes include a patient who, in the middle of a sentence about their day, suddenly begins discussing unrelated past events without realizing the abrupt topic change, highlighting the challenges faced in daily functioning due to these thought disturbances.
Therapists are Standing By to Treat Your Depression, Anxiety or Other Mental Health Needs
Explore Your Options Today
Impact of Disorganized Behavior
The direct impact of disorganized behavior on sufferers includes significant challenges in managing self-care routines, maintaining employment, and engaging in social interactions. For instance, an individual may struggle to follow basic hygiene practices or appear in socially inappropriate attire, affecting their relationships and professional life. Personal anecdotes or short case studies reveal how these behaviors can lead to isolation or misunderstanding from others, emphasizing the profound effects on the individual’s quality of life.
Root Causes of Disorganized Behavior
Current understanding links the root causes of disorganized behavior in schizophrenia primarily to neurobiological factors, including dysfunctions in brain regions responsible for thought organization and processing. Ongoing research continues to explore these connections, seeking to elucidate the exact mechanisms and thus opening pathways for new treatment modalities. The emphasis on neurobiological underpinnings hints at a complex interplay of genetics and brain chemistry.
Diagnosing Disorganized Schizophrenia
Diagnosis of disorganized schizophrenia heavily relies on identifying key symptoms of disorganized speech and behavior during clinical assessment. Healthcare professionals play a critical role in noticing these symptoms, differentiating them from other types of schizophrenia, and determining the extent to which they affect the patient's life. Comprehensive evaluation, often involving interviews and observations, is crucial for an accurate diagnosis.
Managing Disorganized Symptoms
Effective management of disorganized symptoms in schizophrenia includes a combination of antipsychotic medication and psychosocial interventions tailored to the individual’s needs. Treatment plans often prioritize restoring functionality and aiding patients in achieving a better quality of life through improved thought coherence and behavior regulation. The significance of personalized care plans cannot be overstated, as they are key to addressing the unique challenges faced by each individual suffering from disorganized schizophrenia.
- Internet Addiction
- Childhood Mental Disorders
- ADHD: Attention Deficit Hyperactivity Disorder
- Anxiety Disorders
- Bipolar Disorder
- Depression: Major Depression & Unipolar Varieties
- Eating Disorders
- Childhood Mental Disorders And Illnesses
- Dissociative Disorders
- Impulse Control Disorders
- Internet Addiction And Media Issues
- Intellectual Disabilities
- Obsessive-Compulsive Spectrum Disorders
- Post-Traumatic Stress Disorder
- Somatic Symptom And Related Disorders
- Tourettes And Other Tic Disorders
- Physical Mental Illness Flipbook
- Suicide Rates Vector Map
- Identification Of Schizophrenic Patients
- History And Current Understanding
- Schizopheniform Diagnoses
- What Schizophrenia Is Not
- Medications
- Schizoid Personality Disorder
- Evidence As A Brain Disease
- Institutionalization
- Symptoms, Patterns And Statistics
- Antipsychotic Drugs
- Schizotypal Personality
- Hospitalization
- Stigma And Violence
- Factors In Prognosis And Recovery
- Brief Psychotic Episode
- Shared Psychotic Disorder
- Outpatient Options
- Psychosis Induced By A Medical Condition
- Housing And Self-Help
- Family Support
- Substance-Induced Psychotic Disorder
- The Psychotic Dimension
- Delusional Disorder
- The Disorganized Dimension
- Other Symptoms
- Schizoaffective Disorder
- Schizophreniform Disorder And Psychotic NOS
- Other Diagnostic Considerations
- Day Hospital Treatment
- Schizophrenia & Supportive Services
- Kendra's Law On Anti-Psychotic Meds
- Nature Of Psychosis
- Mentally Ill Daughter
- I Think I Have A Mental Illness
- How To Handle My Mothers State Of Mind?
- Pregnant With A Mental Illness
- Am I Schizophrenic?
- What Are Some Coping Skills For Paranoia?
- A Very Low Threshold For Stress Tolerance
- Am I Going To Do This?
- Night Fears
- Is This Schizophrenia?
- Losing Personality Wholness
- Medication Problem
- My Schizophrenic Sister Refuses Treatment
- My Nephew Sees Angels
- Two Cases Of Likely Paranoia ...
- I Have Always Believed Someone Was Watching Me
- A Librarian In Illinois Asks:
- Is Paranoia A Destiny?
- Extreme Psychopathy/sociopathy?
- My Little Girl
- What To Do?
- On Having Hallucinations
- Asylum Squad Comic Strip 69
- Asylum Squad Comic Strip 68
- Asylum Squad Comic Strip 67
- Asylum Squad Comic Strip 66
- Asylum Squad Comic Strip 65
- Asylum Squad Comic Strip 64
- Asylum Squad Comic Strip 63
- The Navy Yard Shooting: Can Violence Be Predicted?
- Asylum Squad Comic Strip 62
- Asylum Squad Comic Strip 60
- Gun Violence, Reporting And Listing Names Of The Mentally Ill?
- Politics And The Needs Of Disabled People
- Living With Schizophrenia
- Living With Schizophrenia, An Inspiring Story
- Asylum Squad Comic Strip 59
- Asylum Squad Comic Strip 58
- Asylum Squad Comic Strip 57
- Asylum Squad Comic Strip 56
- Asylum Squad Comic Strip 55
- Asylum Squad Comic Strip 54
- Asylum Squad Comic Strip 53
- Asylum Squad Comic Strip 52
- The Mentally Ill, Fear And Misunderstanding
- Asylum Squad Comic Strip 51
- Asylum Squad Comic Strip 50
- Asylum Squad Comic Strip 49
- Mental Illness And Innocence?
- Asylum Squad Comic Strip 48
- Asylum Squad Comic Strip 47
- Asylum Squad Comic Strip 46
- Asylum Squad Comic Strip 45
- Asylum Squad Comic Strip 44
- Asylum Squad Comic Strip 43
- Asylum Squad Comic Strip 42
- Asylum Squad Comic Strip 41
- Asylum Squad Comic Strip 40
- Asylum Squad Comic Strip 39
- Asylum Squad Comic Strip 38
- Asylum Squad Comic Stric 37
- Asylum Squad Comic Strip 36
- Asylum Squad Comic Strip 35
- Asylum Squad Comic Strip 34
- Asylum Squad Comic Strip 33
- Asylum Squad Comic Strip 32
- Asylum Squad Comic Strip 31
- Asylum Squad Comic Strip 30
- Asylum Squad Comic Strip 29
- Asylum Squad Comic Strip 28
- Asylum Squad Comic Strip 27
- Schizophrenia - Ricky's Story
- Aslyum Squad Comic Strip 26
- Asylum Squad Comic Strip 25
- Asylum Squad Comic Strip 24
- Asylum Squad Comic Strip 23
- Marijuana And Mental Health, Here We Go Again!
- Asylum Squad Comic Strip 22
- Asylum Squad Comic Strip 21
- Asylum Squad Comic Strip 20
- Asylum Squad Comic Strip 19
- Asylum Squad: Comic Strip 18
- Asylum Squad Comic Strip 17
- Asylum Squad Comic Strip 16
- Asylum Squad Comic Strip 15
- Schizophrenia: An Infection?
- Asylum Squad Comic Strip 14
- Is Schizophrenia Curable?
- Asylum Squad: Comic Strip 13
- Asylum Squad: Comic Strip 12
- Asylum Squad: Comic Strip 11
- Asylum Squad: Comic Strip 10
- Asylum Squad: Comic Strip 9
- Asylum Squad Comic Strip 8
- Asylum Squad: Comic Strip 7
- Asylum Squad: Comic Strip 6
- Asylum Squad: Comic Strip 5
- Asylum Squad: Comic Strip 4
- Asylum Squad: Comic Strip 3
- Asylum Squad: Comic Strip 2
- My Mother Has Schizophrenia: Von Allan's "the Road To God Knows..."
- When Psychiatric Diagnosis And Culture Clash
- Spotlight On A Live Journal
- Schizotypal Personality Disorder And Schizophrenia
- Brain Traffic Jam And Schizophrenia: Possible New Treatments?
- Study Finds Artistic Tendencies Linked To 'Schizophrenia Gene'
- A Tragic Story Of Paranoid Schizophrenia: Lowboy, By John Wray
- Amber Osterhout's Artwork Combats Mental Illness Stigma
- Stigma, Stereotyping And Schizophrenia
- On Hearing Voices
- Study Finds Need for Improved Schizophrenia Care
- Researchers Evaluate Blood Test for Psychosis
- Stem Cell Research Offers Clues About Schizophrenia
- People With OCD May Have Higher Odds for Schizophrenia: Study
- Many With Schizophrenia Say They're Happy: Study
- Gene Discoveries Could Shed New Light on Schizophrenia
- Antipsychotics Linked to Lower Brain Volume in Schizophrenia Patients
- Premature Death, Suicides Up Among People With Schizophrenia, Study Says
- Schizophrenia May Raise Dementia Risk in Older Adults
- Personality Disorders
- Information On Specific Drugs
- Oppositional Defiant Disorder
- Mens Health
- What Is Addiction?
- Signs, Symptoms, & Effects Of Addiction
- What Causes Addiction?
- Mental Health, Dual-Diagnosis, & Behavioral Addictions
- Addiction Treatment
- Addiction Recovery
- Homosexuality And Bisexuality
- Alzheimers Disease And Other Cognitive Disorders
- Chronic Obstructive Pulmonary Disease
- Colds And Flu
- Crohns Disease / Irritable Bowel
- Heart Disease
- High Blood Pressure
- Memory Problems
- Men's Health
- Sexually Transmitted Diseases
- Sleep Disorders
- Women's Health
- Anger Management
- Mindfulness
- Stress Reduction And Management
- Weight Loss
- Disabilities
- Domestic Violence And Rape
- Family & Relationship Issues
- Grief & Bereavement Issues
- Pain Management
- Relationship Problems
- Self Esteem
- Terrorism & War
- Health Insurance
- Health Policy & Advocacy
- Health Sciences
- Mental Health Professions
- Alternative Mental Health Medicine
- Psychological Testing
- Psychotherapy
- Virtual Outpatient Eating Disorder Treatment
- Child Development And Parenting: Infants
- Child Development And Parenting: Early Childhood
- Sexuality & Sexual Problems
- Homosexuality & Bisexuality
- Aging & Geriatrics
- Death & Dying
- Physical Development: Motor Development
- Vygotsky's Social Developmental Emphasis
- Bullying & Peer Abuse
- Family And Relationship Issues
- Grief And Bereavement
- Search the site GO Please fill out this field.
- Newsletters
- Health Conditions A-Z
- Mental Illness
- Schizophrenia
What Are the Different Types of Schizophrenia?
:max_bytes(150000):strip_icc():format(webp)/LauraDorwartprofile-45488b2a9c1347a0a262aaadc4fd23e2.jpg)
- Disorganized
- Undifferentiated
- Related Conditons
- Seeking Care
Uma Shankar Sharma / Getty Images
Schizophrenia is a mental health condition that affects your thoughts, emotions, behaviors, and ability to communicate, plan, and relate to others. Generally, the condition is pretty rare and affects less than 1% of the U.S. population. Most people with this condition typically start showing symptoms in their late teens, 20s, and early 30s.
In the Diagnostic and Statistical Manual of Mental Disorders, 5th Edition (DSM-5), schizophrenia is not categorized into different types. The previous edition (the DSM-4), however, organized schizophrenia into five types: paranoid, catatonic, disorganized, undifferentiated, and residual schizophrenia. Some researchers still refer to these types during the diagnostic process, though.
Paranoid Schizophrenia
Paranoid schizophrenia typically causes psychotic (or psychosis-related) symptoms such as delusions and hallucinations. Delusions are false beliefs that you might have even though there's evidence to a contrary belief, whereas hallucinations occur when you see, hear, smell, taste, or feel things that aren’t actually there—such as voices or visual images.
For people with paranoid schizophrenia, delusions and hallucinations are often grandiose, meaning that they involve an inflated sense of self-importance. They can also be persecutory, which refers to believing that someone or something is “out to get you.” For example, a person with paranoid schizophrenia may think they hear voices threatening them or people chasing them. They may also believe that a person or organization is spying on them, even if they don't have proof of that claim.
Catatonic Schizophrenia
Catatonic schizophrenia (or schizophrenia with catatonia ) affects the way a person moves their body, responds to stimuli, and relates to the world around them. A person with this type may exhibit signs of either catatonic stupor (which involves moving very little and appearing withdrawn) or catatonic excitement (which refers to agitated, restless, and excessive movements).
People with catatonic schizophrenia may also often be unresponsive when others try to interact with them. Some also experience echolalia (repeating the same words or phrases over and over) or echopraxia (repetitive movements).
Disorganized Schizophrenia
Disorganized schizophrenia involves severe cognitive, behavioral, and emotional symptoms. People with disorganized schizophrenia typically experience disorganized thinking, which means that they may have racing or illogical thoughts or make connections between unrelated ideas. They also tend to express their thoughts and emotions in ways that others find confusing, bizarre, or unsettling, such as speaking in unusual patterns and laughing or scowling at inappropriate times.
This type of schizophrenia is often considered the most serious type, as it typically affects daily functioning to the greatest extent.
Undifferentiated Schizophrenia
Undifferentiated schizophrenia historically referred to a condition that caused symptoms of another type of schizophrenia (such as psychotic or disorganized schizophrenia), but a person with these symptoms didn't meet the full diagnostic criteria for a specific type of schizophrenia. This term has since been considered outdated, and most healthcare providers use the term "schizophrenia spectrum disorder" to highlight how symptoms of schizophrenia can vary across a spectrum.
Residual Schizophrenia
Someone may be diagnosed with residual schizophrenia if they have had at least some positive symptoms of schizophrenia (which refer to symptoms like hallucinations or disorganized thinking) but now only have negative symptoms. In schizophrenia terms, negative symptoms are related to your emotions and how you interact with others. Some negative symptoms include speaking very little, lack of motivation, social withdrawal, and depression .
In other words, people with residual schizophrenia may still have beliefs and behaviors that others might consider eccentric, but they no longer experience severe or positive symptoms associated with the condition.
Other Related Conditions
Symptoms of mental health conditions tend to overlap. There are several other conditions that share certain symptoms with schizophrenia, including:
- Schizoaffective disorder: Causes symptoms of both schizophrenia and a mood disorder (such as bipolar disorder or depression) at the same time
- Schizophreniform disorder: Causes the same symptoms of schizophrenia, such as delusions, hallucinations, negative symptoms, and disorganized speech—but these are short-term and only last between one and six months
- Delusional disorder: Causes persistent delusions for a month or more, with no additional symptoms
- Brief psychotic disorder: Causes psychotic symptoms for a short period, usually between a day to a month
- Schizotypal personality disorder : Causes symptoms like reclusiveness, disorganized speech patterns, bizarre and distorted thinking, and difficulty forming meaningful relationships with others—but these symptoms tend to be less severe than schizophrenia
- Substance-induced psychotic disorder: Causes psychosis as a side effect of a drug, like hallucinogens or certain prescription medications
- Psychotic disorder due to another medical condition: Causes symptoms of psychosis due to underlying conditions like brain tumors , Parkinson’s disease, Alzheimer’s disease , fever, and hypoglycemia (extremely low blood sugar levels)
If you or a loved one are experiencing signs of schizophrenia, seeing a healthcare provider about your symptoms is important. The earlier you receive a diagnosis for your condition, the sooner you can get started on treatment that helps you improve your symptoms and quality of life. Getting mental health support can feel worrisome or scary, but it's important to know that support is out there. Knowing what to expect during the diagnostic process can also help ease any anxiety.
When you go in for an appointment, your primary healthcare provider will ask about your symptoms, conduct a physical exam, and often refer you to a mental health provider such as a psychiatrist or psychologist . Your mental health provider will then evaluate your symptoms and behavior on an ongoing basis—generally lasting around six months. They may also order other tests to rule out other conditions that may cause similar symptoms, such as a brain tumor or substance use disorder .
After they complete the necessary testing and evaluation period, your provider can determine whether or not you meet the criteria for schizophrenia, according to the DSM-5. Should you receive a diagnosis for schizophrenia, your provider will work with you to find the best treatment options for your individual needs.
Treatment Options for Schizophrenia
While there is no cure for schizophrenia at this time, several treatments can help keep symptoms at bay and boost your quality of life significantly. The goal of treatment is to improve your daily life so you can meet your goals, form healthy relationships, participate in your community, and attain educational or career outcomes if you desire them. Your exact treatment plan will likely involve a combination of these treatment options:
- Medication: Using antipsychotic medications, benzodiazepines, antidepressants , or anti-seizure medications
- Coordinated specialty care (CSC) programs: Includes in-patient care, out-patient care, or a mix of both to help you improve symptoms and work with trained professionals (like case managers, psychotherapists, and social workers) to help you perform daily activities well
- Psychosocial intervention: Incorporates a variety of interventions such as individual therapy , group therapy, family education, support groups, behavioral skills training, vocational rehabilitation, educational counseling, psychoeducation, and cognitive remediation
- Drug and alcohol counseling: Offers healthier coping mechanisms to help you manage symptoms, especially because people with schizophrenia have higher-than-average rates of substance use disorder
In some cases, healthcare providers may recommend electroconvulsive therapy (ECT) to treat schizophrenia. ECT places electrodes on specific points of your head to send electric shock signals to induce a seizure and improve brain activity. This treatment is particularly effective for treating catatonic schizophrenia. If you think this treatment may be a good option for you, consider talking to your provider for advice.
When to Contact a Healthcare Provider
If you think you may have signs of schizophrenia, it's better to see a healthcare provider sooner rather than later. They can refer you to a mental health provider and offer in-patient care if necessary. You can also find local resources for yourself or a loved one through the Substance Abuse and Mental Health Services Administration (SAMHSA).
Family members, friends, and partners of people with schizophrenia should also gently encourage their loved ones to seek treatment and help them find resources if possible. Family education programs may help you understand the condition in more detail, while support groups can offer compassion, help, and advice as you navigate this journey.
A Quick Review
According to the DSM-5, schizophrenia is no longer divided into separate subtypes. However, the DSM-4, which was released before the fifth edition, recognized five types of schizophrenia: paranoid, catatonic, disorganized, undifferentiated, and residual. Some healthcare providers still use subtype classification during diagnosis, while others do not. Regardless of which type you have, schizophrenia can significantly affect your life, so getting support and treatment is essential to living well.
:max_bytes(150000):strip_icc():format(webp)/sr-a21a100afbf343f481150ff49b3a733e.jpeg)
MedlinePlus. Schizophrenia .
American Psychological Association. Schizophrenia .
American Psychological Association. Paranoid schizophrenia .
American Psychological Association. Catatonic schizophrenia .
American Psychological Association. Disorganized schizophrenia .
American Psychological Association. Undifferentiated schizophrenia .
American Psychological Association. Residual schizophrenia .
Radua J, Ramella-Cravaro V, Ioannidis JPA, et al. What causes psychosis? An umbrella review of risk and protective factors . World Psychiatry . 2018;17(1):49-66. doi:10.1002/wps.20490
American Psychological Association. Schizotypal personality disorder .
American Psychological Association. Substance-induced psychotic disorder .
American Psychiatric Association. What is schizophrenia? .
National Alliance on Mental Illness. Schizophrenia .
Grover S, Chakrabarti S, Kulhara P, Avasthi A. Clinical practice guidelines for management of schizophrenia . Indian J Psychiatry . 2017;59(Suppl 1):S19-S33. doi:10.4103/0019-5545.196972
National Institute of Mental Health. Schizophrenia .
Caroff SN, Ungvari GS, Gazdag G. Treatment of schizophrenia with catatonic symptoms: A narrative review . Schizophr Res . 2024;263:265-274. doi:10.1016/j.schres.2022.11.015
Related Articles

Schizophrenia Symptoms
The formal diagnosis of schizophrenia rests on these symptoms, which can be evaluated by psychiatrists and other mental health professionals.
Associated features
Symptoms of schizophrenia.
The following specific diagnostic criteria are reproduced verbatim (except for codings and page references) from the DSM-IV, the immediate predessor of the current DSM-IV TR (where ‘IV TR’ indicates fourth edition, text revision).
Diagnostic Criteria for Schizophrenia
A. Characteristic symptoms: Two (or more) of the following, each present for a significant portion of time during a 1-month period (or less if successfully treated):
- hallucinations
- disorganized speech (e.g., frequent derailment or incoherence)
- grossly disorganized or catatonic behavior
- negative symptoms, i.e., affective flattening, alogia, or avolition
Note: Only one Criterion A symptom is required if delusions are bizarre or hallucinations consist of a voice keeping up a running commentary on the person’s behavior or thoughts, or two or more voices conversing with each other.
B. Social/occupational dysfunction: For a significant portion of the time since the onset of the disturbance, one or more major areas of functioning such as work, interpersonal relations, or self-care are markedly below the level achieved prior to the onset (or when the onset is in childhood or adolescence, failure to achieve expected level of interpersonal, academic, or occupational achievement).
Talk to a Psychiatrist or Therapist Online (Please read our important explanation below.)
C. Duration: Continuous signs of the disturbance persist for at least 6 months. This 6-month period must include at least 1 month of symptoms (or less if successfully treated) that meet Criterion A (i.e., active-phase symptoms) and may include periods of prodromal or residual symptoms. During these prodromal or residual periods, the signs of the disturbance may be manifested by only negative symptoms or two or more symptoms listed in Criterion A present in an attenuated form (e.g., odd beliefs, unusual perceptual experiences).
D. Schizoaffective and Mood Disorder exclusion: Schizoaffective Disorder and Mood Disorder With Psychotic Features have been ruled out because either (1) no Major Depressive Episode, Manic Episode, or Mixed Episode have occurred concurrently with the active-phase symptoms; or (2) if mood episodes have occurred during active-phase symptoms, their total duration has been brief relative to the duration of the active and residual periods.
E. Substance/general medical condition exclusion: The disturbance is not due to the direct physiological effects of a substance (e.g., a drug of abuse, a medication) or a general medical condition.
F. Relationship to a Pervasive Developmental Disorder: If there is a history of Autistic Disorder or another Pervasive Developmental Disorder, the additional diagnosis of Schizophrenia is made only if prominent delusions or hallucinations are also present for at least a month (or less if successfully treated).
1. Paranoid Type
A type of Schizophrenia in which the following criteria are met:
- Preoccupation with one or more delusions or frequent auditory hallucinations.
- None of the following is prominent: disorganized speech, disorganized or catatonic behavior, or flat or inappropriate affect.
2. Catatonic Type
A type of Schizophrenia in which the clinical picture is dominated by at least two of the following:
- motoric immobility as evidenced by catalepsy (including waxy flexibility) or stupor
- excessive motor activity (that is apparently purposeless and not influenced by external stimuli)
- extreme negativism (an apparently motiveless resistance to all instructions or maintenance of a rigid posture against attempts to be moved) or mutism
- peculiarities of voluntary movement as evidenced by posturing (voluntary assumption of inappropriate or bizarre postures),
- stereotyped movements, prominent mannerisms, or prominent grimacing
- echolalia or echopraxia
3. Disorganized Type
- disorganized speech
- disorganized behavior
- flat or inappropriate affect
- The criteria are not met for Catatonic Type.
4. Undifferentiated Type
A type of Schizophrenia in which symptoms that meet Criterion A are present, but the criteria are not met for the Paranoid, Disorganized, or Catatonic Type.
5. Residual Type
- Absence of prominent delusions, hallucinations, disorganized speech, and grossly disorganized or catatonic behavior.
- There is continuing evidence of the disturbance, as indicated by the presence of negative symptoms or two or more symptoms listed in Criterion A for Schizophrenia, present in an attenuated form (e.g., odd beliefs, unusual perceptual experiences).
- Learning Problem
- Hypoactivity
- Euphoric Mood
- Depressed Mood
- Somatic or Sexual Dysfunction
- Hyperactivity
- Guilt or Obsession
- Sexually Deviant Behavior
- Odd/Eccentric or Suspicious Personality
- Anxious or Fearful or Dependent Personality
- Dramatic or Erratic or Antisocial Personality
Sections Available
- Schizoaffective Disorder Symptoms: DSM
- Schizoid Personality Disorder Symptoms: DSM
- Schizophrenia Symptoms: DSM
- Schizophreniform Disorder Symptoms: DSM
- Schizotypal Personality Disorder Symptoms: DSM
- ICD Approach to Schizophrenia
- Schizophrenia and Schizophrenic Disorders
- DSM Approach to Schizophrenia
All clinical material on this site is peer reviewed by one or more qualified mental health professionals. This specific article was originally published by MH Resource Research Staff on April 2, 2011 and was last reviewed or updated by Dr Greg Mulhauser, Managing Editor on February 15, 2016 .
https://mhreference.org/schizophrenic/schizophrenia-dsm/schizophrenia-symptoms/
- Personality
- Schizophrenia
Disorders & Symptoms
- Anxiety Disorders
- Mood Disorders
- Personality Disorders
Screening Tests & Quizzes (External)
- Alcohol and Drug Use
- Bipolar Test
- Depression Tests
- Dissociative Experiences Scale
- Love & Relationship Quiz
- Schizophrenia Test
Finding Help: Directories & Resources
- CBTtherapist.com (UK)
- RightTherapist.com (UK)
- RightCounsellor.com (Australia)
- PsychTap.com (US)
- Ask The Psychologist
- Online Counseling Options
Our material is not intended as a substitute for direct consultation with a qualified mental health professional. Please seek professional advice if you are experiencing any mental health concern.
- About the Site, Privacy, Cookies and Terms of Use
How To Prevent Schizophrenia From Worsening
Navigating schizophrenia usually has its ups and downs, but understanding this complex disorder and what might trigger worsening symptoms can empower you to make a difference. You might keep a journal tracking your moods and symptoms to recognize the factors that seem to influence them the most. Prioritizing self-care and building a healthy support network to navigate symptoms and look out for flare-ups can also be helpful alongside consistent treatment. Common treatment methods often includes doctor-prescribed medication and regular therapy sessions.

Understanding schizophrenia
Schizophrenia spectrum disorder (SSD) is a chronic mental disorder that can disrupt how a person experiences reality. Schizophrenia can cause unexpected and sometimes overwhelming changes in perception. This disorder often causes a wide range of symptoms that may sometimes be overwhelming. These symptoms, which generally fall within three main categories:
- Positive symptoms: These are usually the ones that get the most attention — symptoms like hallucinations (perceiving things that aren't there) and delusions (fixed, false beliefs).
- Negative symptoms: Less obvious but equally challenging, these symptoms might manifest as feeling emotionally flat, losing interest in everyday activities, or finding it hard to experience joy.
- Cognitive symptoms: Like roadblocks for your thinking, cognitive symptoms can make it difficult to concentrate, hold onto information, or make decisions.
Recognizing that your symptoms might change in intensity over time can be beneficial for managing schizophrenia. This understanding may empower you to plan and build the right support systems for managing these fluctuations.
Risk factors for schizophrenia
The cause of schizophrenia may be considered a puzzle that scientists are still working to solve. However, research has identified several contributors that can increase a person's susceptibility to this disorder. Understanding potential risk factors can help with early identification and support strategies for proactive care.
- Family history: If you have a close relative, like a parent or sibling, with schizophrenia, your risk of developing the disorder tends to be significantly higher. However, many people with a family history of schizophrenia never develop the disorder themselves.
- Early brain development: Scientists are discovering that subtle differences in brain structure and the way the central nervous system develops may contribute to an increased risk of schizophrenia. These changes can sometimes be traced back to prenatal development.
- Birth complications: Studies suggest a potential link between complications during pregnancy or birth , such as exposure to viruses, malnutrition, or oxygen deprivation, and a slightly increased risk of developing schizophrenia later in life.
- Other factors: Additional factors that might play a role in increased susceptibility to schizophrenia can include older paternal age and using psychoactive substances during adolescence.
Sometimes, changes in a person's usual behavior or thinking patterns can precede the more noticeable symptoms of schizophrenia. Paying attention to these subtle shifts can help with early detection. These early symptoms might include the following:
- Social withdrawal and isolation
- Increased suspicion or paranoia
- Unusual thoughts or beliefs
- Decline in personal hygiene or self-care
- Difficulty expressing emotions and appearing emotionally flat
- Disorganized speech or trouble concentrating
A combination of genetic and environmental factors likely influences schizophrenia. While having risk factors may increase a person’s susceptibility, it doesn't guarantee that a person will develop the disorder. Research into risk factors can offer insights for early detection, proactive care, and, ultimately, improved outcomes for people with schizophrenia.
If changes in thinking, mood, or behavior seem concerning but don't perfectly match a schizophrenia diagnosis, seeking a professional evaluation can provide a more accurate assessment of what's going on. Mental illness is usually more than a checklist of symptoms, and only a qualified professional can make a diagnosis.

Early warning systems to detect symptom flare-ups
Being aware of them can empower you to be proactive and lessen their impact:
- Stress overload: Big life transitions, being overwhelmed, or experiencing the pressure of daily responsibilities can all take a toll.
- Sleep deprivation: When your mind and body are exhausted, it's usually harder to cope, and symptoms might intensify.
- Substance use and misuse (formerly referred to as drug abuse): Illicit drugs and alcohol can disrupt your treatment and make schizophrenia harder to manage.
- The dangers of isolation: Loneliness and feeling disconnected can worsen symptoms. Finding supportive connections may be beneficial.
Identifying the situations that make your symptoms worsen can offer a sense of control, helping you manage challenges before they escalate. By using a mood diary, you can uncover patterns in your life that might influence symptom intensity.
Treatment and tools
Treatment can be part of your support system as you navigate schizophrenia and help you manage the ever-changing circumstances of your journey.
Medication for schizophrenia treatment
Antipsychotics, as prescribed by a psychiatrist or doctor, are often a useful part of schizophrenia treatment. They usually work by balancing chemicals in your brain to reduce the intensity of symptoms.
Therapy to manage thought patterns and mental health
Different types of therapy can offer a complement to medication:
- Cognitive-behavioral therapy (CBT) generally changes unhelpful thinking patterns and teaches healthy coping skills.
- Psychosocial therapies can provide tools for navigating daily tasks and building a fulfilling life.
- Family therapy may offer support and guidance to those who love you, strengthening your support network.
Finding the right treatment approach is usually a collaborative process. Open and honest communication with your healthcare team can improve symptom management. Research indicates early intervention and a combination of treatment options can be beneficial for long-term symptom management.
Self-care for supporting well-being
Beyond formal treatment, small daily acts of self-care can bolster your well-being and counterbalance the effects of schizophrenia. The following can serve as practical tools for building resilience:
- Nurturing routines: Predictable bedtimes, nutrient-rich eating habits, and regular exercise can promote mental and physical health.
- Stress management techniques: Many practices can calm your mind: deep breathing exercises, meditation, spending time in nature, and gentle physical activity are just a few.
- The strength of connection: You can reach out to friends and family, join a support group, or find a community where you feel safe and understood to reduce isolation.
- Focusing on goals: Small, achievable goals can keep you moving forward. It can be motivating to celebrate each step along the way, no matter how small.
Managing schizophrenia is often a continuous journey of learning, finding effective treatments, and building resilience. Treatment can be a process of discovery — what helps you one day might need to be adjusted the next, and that's okay.
Finding the right mental health support and preventing symptoms
Navigating schizophrenia doesn't need to be a lonely endeavor. Building a team of trusted healthcare professionals can transform your journey:
- Psychiatrists: These professionals are medical doctors specializing in mental health. They can prescribe medication and monitor its effectiveness.
- Therapists: Psychologists and licensed therapists may offer guidance and coping skills as they help you process the emotional challenges of schizophrenia.
- Social workers: Social workers can connect you with resources in your community, offer support in navigating practical needs, and advocate for your well-being.
Importance of self-advocating
Seeking professional support can be a sign of strength in managing schizophrenia. A trusted healthcare team usually makes a difference in your journey, but your input matters just as much. Being an advocate for your own care frequently means speaking up and actively shaping your treatment path. How do you advocate for yourself when you’re feeling overwhelmed? Building a toolkit to help you in moments of uncertainty can be empowering:
- Cultivating self-awareness: It can be helpful to pay attention to your moods, track medication effects, and identify what seems to worsen or improve your symptoms.
- Speaking up: When you clearly share your needs and concerns with your healthcare team, they can be better informed. Preparing questions beforehand and asking for clarification when needed can keep you on track.
- Seeking support: Organizations like NAMI and peer support groups can help you advocate for yourself more effectively.

Online therapy as a support tool
Navigating schizophrenia often means finding the right combination of support. We all deserve mental health support that works for us. While traditional in-person therapy can offer many benefits, it's understandable if factors like finding the right therapist or navigating logistical challenges get in the way.
Online therapy can provide a convenient alternative. The online format typically offers increased flexibility, potentially making care more attainable. Online platforms can also provide a wider range of therapists from which to choose, likely increasing the chance of finding someone who understands your experiences and challenges.
The path to successfully managing schizophrenia often involves trying different approaches to find what works best for you. Recent studies suggest online therapy holds promise as a complementary tool, offering another effective way to address symptoms and improve your quality of life .
- What To Expect When You Are Dating Someone With Schizophrenia Medically reviewed by Nikki Ciletti , M.Ed, LPC
- New Schizophrenia Studies And Research Medically reviewed by Melissa Guarnaccia , LCSW
- Schizophrenia
- Relationships and Relations
How Is Schizophrenia Diagnosed? DSM-5 Diagnosis Criteria

Schizophrenia is a serious mental illness that deeply affects people. Because a correct schizophrenia diagnosis can improve someone’s quality of life, it’s important that it be made as soon as possible after the symptoms of schizophrenia appear.
Currently, no tests can provide a schizophrenia diagnosis. To determine whether someone has the disorder, doctors follow established criteria for a schizophrenia diagnosis.
Criteria for Schizophrenia Diagnosis in DSM-5
The Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) is the authority on mental illness. Created and published by the American Psychiatric Association, this comprehensive manual describes all known mental disorders, among them schizophrenia.
Mental health professionals use the DSM-5 when determining what someone is experiencing. Doctors use the information and analyze:
- diagnostic features and symptoms
- level of impairment
- duration of symptoms
- other conditions that share symptoms
They also look at age. While it’s not part of the diagnostic criteria, they do consider someone’s age. The typical age of schizophrenia diagnosis is between late adolescence and the mid-30s. This varies, though, with peak ages ranging from the early- to mid-20s for males and late-20s for females ( Are Schizophrenia Symptoms in Males and Females Different? ). Further, while it’s rare, schizophrenia can be diagnosed as early as childhood and as late as the 40s ( What Are the Schizophrenia Symptoms in Children and Teens? ).
Age provides a general idea of the likelihood that someone has schizophrenia. Schizophrenia won’t be the first consideration for a man in his 40s, for example. Beyond this, age isn’t a diagnostic criterion. Just what are the diagnostic criteria for schizophrenia?
Diagnosing Schizophrenia Using Symptoms and Features
Professionals use specific diagnostic features in the DSM-5 to help determine whether someone meets the criteria for schizophrenia. The DSM-5 delineates five main criteria. Paraphrased:
A. Two or more of
- Hallucinations
- Disorganized speech (such as speaking incoherently, losing track of thoughts)
- Disorganized or catatonic behavior
- Negative symptoms
B. Level of functioning has declined C. The symptoms in Criterion A have persisted for at least 6 months D. Schizoaffective disorder , major depression , and bipolar disorder have been ruled out E. Substance use/abuse has been ruled out as a cause
In order for someone to be diagnosed with schizophrenia, he must experience a group of these symptoms and features. One or two are not enough.
To receive a schizophrenia diagnosis, someone can have any of the symptoms and features, but he must have the following:
- At least two symptoms from Criteria A
- One of those two must be delusions, hallucinations, or disorganized speech.
- These must have been present for at least one month.
The symptoms must impair one’s life and get in the way of her ability to work (or go to/participate in school), have positive relationships (or any relationships at all), and practice self-care. The problems in these areas must be new, a decline in the previous status.
Duration of the symptoms is also important for a schizophrenia diagnosis. Someone must have been experiencing steady symptoms for at least one month. Symptoms must be present some of the time for six consecutive months.
Other Considerations in Diagnosing Schizophrenia
The DSM-5 includes other things that can help determine schizophrenia. They’re not necessary diagnostic criteria, but their presence points to this serious mental illness.
- Prodromal (early) symptoms , similar to the symptoms of schizophrenia but too mild and sporadic for a diagnosis
- Inappropriate emotions (like loud, random laughter in public)
- Dysphoria (low mood)
- Sleep problems
- Lack of interest in or refusing food
- Memory problems
- Language/speech problems
- Shortened attention span
- Inability to understand someone’s intentions
- Thinking insignificant things are highly, personally meaningful
- Manic behavior
In addition to these, people with schizophrenia often experience what is known as neurological soft sign, subtle abnormalities that aren’t severe enough to fit into any disorder but are problematic and indicative of a bigger problem, like schizophrenia. They can include:
- Coordination problems
- Sensory-integration problems
- Left-right confusion
- Difficulty with complex movement
To diagnose schizophrenia, professionals examine all of the symptoms and features that are present ( Complete List of Schizophrenia Symptoms ). They also must look at what is not present.
Schizophrenia Diagnosis: Rule out Other Conditions
A diagnosis involves what someone is experiencing as well as what he is not. Some disorders have some features or symptoms that are shared with schizophrenia; therefore, doctors check to see if something else fits better than schizophrenia. Some of the conditions that, according to criteria in the DSM-5 , have some similarities with schizophrenia are
- Mood disorders (depression and/or bipolar disorder) with psychotic features
- Schizophreniform
- Brief psychotic disorder
- Schizotypal personality disorder
- Obsessive-compulsive disorder
- Body dysmorphic disorder
- Autism spectrum disorder
- Communication disorders
- Substance use disorders
Schizophrenia is a complex disorder, and doctors take the diagnosis of it seriously. In addition to all of the above concerns, professionals also take into consideration the individual. Schizophrenia is unique, and each person experiences it differently. This makes perfect sense, of course, for no matter what their individualized symptoms, people with schizophrenia are above all, human.
article references
APA Reference Peterson, T. (2021, December 17). How Is Schizophrenia Diagnosed? DSM-5 Diagnosis Criteria, HealthyPlace. Retrieved on 2024, September 3 from https://www.healthyplace.com/thought-disorders/schizophrenia-symptoms/how-is-schizophrenia-diagnosed
Medically reviewed by Harry Croft, MD
Related Articles

What Melancholia Feels Like
Associated features of schizoaffective disorder, how long should people with schizophrenia take antipsychotic drugs, schizoaffective disorder: life on a roller coaster, articles on schizophrenia causes, schizophrenia support: schizophrenia forums, support groups, causes of schizoaffective disorder.
2024 HealthyPlace Inc. All Rights Reserved. Site last updated September 3, 2024
- Type 2 Diabetes
- Heart Disease
- Digestive Health
- Multiple Sclerosis
- Diet & Nutrition
- Health Insurance
- Public Health
- Patient Rights
- Caregivers & Loved Ones
- End of Life Concerns
- Health News
- Thyroid Test Analyzer
- Doctor Discussion Guides
- Hemoglobin A1c Test Analyzer
- Lipid Test Analyzer
- Complete Blood Count (CBC) Analyzer
- What to Buy
- Editorial Process
- Meet Our Medical Expert Board
Types of Psychosis and Their Causes
Psychotic disorders.
- Other Psychiatric Causes
- Medical Causes
- Drug Causes
Psychosis is a break from reality characterized by delusions and hallucinations. There are several conditions classified as psychotic disorders, most notably schizophrenia , and others like major depression where psychosis is a complication rather than a feature of the disorder. It can also occur with a brain injury, substance abuse, and other causes.
Approximately three of every 100 people will experience an episode of psychosis in their lifetime. Psychosis is not a condition on its own, but rather a symptom of a psychiatric or medical condition.
Psychotic disorders and other mental disorders are diagnosed based on criteria outlined in the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) . Other causes may require blood tests and brain scans to determine the underlying cause.
FollowTheFlow / Getty Images
What Is Psychosis?
Psychosis is the distortion of reality in which you have difficulty knowing what is real and what is not. It can be temporary, ongoing, or cause recurring symptoms. People experiencing psychosis have little or no awareness of their symptoms.
Psychosis is characterized by two main features:
- Hallucinations : The experience of sensing things (including sounds, sights, tastes, physical sensations, or smells) that only exist in your mind
- Delusions : A false belief that is strongly held despite irrefutable evidence to the contrary
These may be accompanied by two others that can help differentiate if the cause is psychiatric, medical, or substance-related:
- Disorganized speech : A rapid, incoherent switch between disconnected thoughts and speech
- Catatonia : Strange, purposeless movement or complete unresponsiveness despite being awake
The manifestations of psychosis can vary by the individual as can the causes.
A primary psychiatric cause of psychosis is classified in the DSM-5 as "Schizophrenia Spectrum and Other Psychotic Disorders." These are conditions in which psychosis is a defining feature of the disorder (rather than a symptom that may or may not occur).
Psychotic disorders in this category include:
- Schizophrenia : Characterized by two or more symptoms (either hallucinations, delusions, disorganized speech, or disorganized/catatonic behaviors) for more than a month
- Schizophreniform disorder : A condition similar to schizophrenia lasting less than one month
- Schizoaffective disorder : Involving schizophrenia and a mood disorder like depression
- Delusional disorder : The presence of one or more delusions lasting one month or more
Early Signs of Psychosis
In people with schizophrenia and other psychotic disorders, early signs may develop before a full-blown psychotic break occurs, such as:
- New unusual thoughts or beliefs
- A marked drop in grades or job performance
- Difficulty concentrating
- Increased isolation and withdrawal from family, friends, and colleagues
- A sudden decline in self-care and hygiene
- Extreme emotions or a noticeable lack of emotions
- Suspiciousness or distrust of others
By recognizing the early signs, you can seek treatment and potentially abort a serious psychotic episode.
Other Psychiatric Disorders
People with other mental disorders can sometimes experience psychosis as a complication of their condition. The difference is that people with these disorders may never have a psychotic episode, while people with psychotic disorders by definition do.
These condtions include:
- Major depressive disorder (MDD)
- Bipolar 1 disorder , during manic or depressive episodes
- Bipolar 2 disorder , during depressive episodes
- Post-traumatic stress disorder (PTSD)
- Borderline personality disorder (BPD)
- Obsessive-compulsive disorder (OCD)
- Dissociative identity disorder (previously known as "multiple personality")
The diagnostic criteria for each of these disorders are individually described in the DSM-5.
Medical Conditions
Psychosis is primarily associated with psychiatric conditions, but some medical conditions can also cause psychosis. This may be due to an injury or changes to the brain that cause a transient break or recurrent episodes.
Examples include:
- Traumatic brain injury
- Postpartum psychosis , generally occurring within three months of childbirth
- Alzheimer's disease
- Lewy body dementia
- Advanced multiple sclerosis (MS)
- Brain tumors
- Viral encephalitis
- HIV encephalopathy , also known as HIV dementia
- Hepatic encephalopathy , common with end-stage liver disease
- Thyrotoxic crisis , also known as "thyroid storm"
- Acute kidney failure , causing uremic toxicity
These and other medical conditions are listed in the DSM-5 as "Psychotic Disorders Due to Another Medical Condition." With these condtions, hallucinations and/or delusions are the primary features.
Psychoactive Drugs
Certain psychoactive substances, both legal and legal, can cause psychotic episodes either as a result of intoxication, prolonged use, or drug withdrawal. These episodes differ in that the person will often be aware of their psychotic break and experience suicidal thoughts or actions.
Drugs known to induce psychosis include:
- Methamphetamine
- Hallucinogenics, like LSD and ketamine
- Cannabis, typically with prolonged use
- MDMA ("ecstasy")
- Psilocybin ("magic mushrooms")
- Alcohol abuse
Psychosis caused by these and other drugs is classified in the DSM-5 as "Substance/Medication-Induced Psychotic Disorder." Under the DSM-5 definition, either hallucinations or delusions occur in the absence of catatonia or disorganized speech.
Diagnosing Psychosis
All of the conditions associated with psychosis—from schizophrenia to alcohol use—are described in the DSM-5's definition of "Schizophrenia Spectrum and Other Psychotic Disorders." This is because the mind and brain are closely linked, and you can't necessarily isolate psychosis to one or the other.
To this end, a clinician will want to investigate whether the appearance of psychosis is purely psychiatric, purely medical, or a combination of both. This may involve a battery lab and imaging tests to detect or exclude medical causes.
- Blood tests to check for signs of infection
- Urinalysis to check for signs of uremic toxicity
- Drug testing, also known as a 10-panel blood test
- STI panel , including an HIV test
- Brain imaging scans
- Electroencephalogram (EEG)
- Kidney function tests
- Liver functions tests
- Thyroid blood tests
Even if a psychiatric illness or substance use is suspected, these and other tests may be ordered to ensure that the diagnosis is correct and that an underlying or co-occurring condition is not involved.
(For instance, a severe urinary tract infection in an adult with dementia can trigger episodes of psychosis. Diagnosing this can direct the appropriate treatment.)
Sometimes, a person only has one psychotic episode. If the episode lasts longer than one day but is shorter than one month, it might be diagnosed as a brief psychotic disorder.
Treatment of Psychosis
Treatment for psychosis depends on the cause but may include medications, therapy, or both. In cases of substance use, detoxification may be the primary (or sole) form of treatment.
Even if the cause is medical, antipsychotic drugs may be prescribed to help bring symptoms under control. With schizophrenia and other psychiatric conditions, the drugs can not only treat acute episodes but prevent recurrence.
These include first-generation typical antipsychotics like:
- Haldol (haloperidol)
- Prolixin (fluphenazine)
- Adasuve (loxapine)
- Mellaril (thioridazine)
- Stelazine (trifluoperazine)
- Thiothixene
Second-generation atypical antipsychotics may also be used:
- Clozaril (clozapine)
- Abilify (aripiprazole)
- Risperdal (risperidone)
- Zyprexa (olanzapine)
- Seroquel (quetiapine)
Generally speaking, typical antipsychotics are suited for both the treatment of acute psychosis and the long-term management of psychotic disorders. Atypical antipsychotics are reserved for long-term management and tend to be less effective in treating hallucinations and delusions.
People with schizophrenia and psychiatric conditions would also benefit from psychotherapy, most often in the form of cognitive-behavior therapy (CBT) or dialectical behavioral therapy (DBT) .
Psychosis occurs when you lose touch with reality and experience hallucinations and/or delusions. It can be caused by psychiatric disorders like schizophrenia, major depression, bipolar disorder, and PTSD. It can also occur with medical conditions like dementia, stroke, encephalopathy, and psychoactive drugs.
Antipsychotic drugs may be used to treat acute episodes and prevent recurrence in people with psychotic disorders.
Arciniegas DB. Psychosis . Continuum (Minneap Minn) . 2015;21(3):715-736. doi:10.1212/01.CON.0000466662.89908.e7
National Institute of Mental Health. Fact sheet: first episode psychosis .
Substance Abuse and Mental Health Services Administration (SAMHSA). Table 3.20: DSM-IV to DSM-5 psychotic disorders . In: Impact of the DSM-IV to DSM-5 Changes on the National Survey on Drug Use and Health . Rockville (MD): SAMHSA; 2016.
National Association of Mental Illness. Early psychosis and psychosis .
Griswold KS, Del Regno PA, Berger RC. Recognition and differential diagnosis of psychosis in primary care . Am Fam Physician . 2015;91(12):856-863
Postpartum Support International. Postpartum psychosis .
Fiorentini A, Cantu F, Cristani C, Cereda G, Oldani L, Barmbilla P. Substance-induced psychoses: an updated literature review . Front Psychiatry. 2021;12:694863. doi:10.3389/fpsyt.2021.694863
Alzheimer's Society. Urinary tract infections and dementia .
MedlinePlus. Psychosis .
Marcinkowska M, Śniecikowska J, Fajkis N, Paśko P, Franczyk W, Kołaczkowski M. Management of dementia-related psychosis, agitation and aggression: a review of the pharmacology and clinical effects of potential drug candidates . CNS Drugs . 2020;34(3):243-268. doi:10.1007/s40263-020-00707-7
Sedgwick O, Hardy A, Newbery K, Cella M. A systematic review of adherence to group interventions in psychosis: do people attend? . Psychol Med . 2021;51(5):707-715. doi:10.1017/S0033291721000404
By Sarah Bence, OTR/L Bence is an occupational therapist with a range of work experience in mental healthcare settings. She is living with celiac disease and endometriosis.

Personalize Your Experience
Log in or create an account for a personalized experience based on your selected interests.
Already have an account? Log In
Free standard shipping is valid on orders of $45 or more (after promotions and discounts are applied, regular shipping rates do not qualify as part of the $45 or more) shipped to US addresses only. Not valid on previous purchases or when combined with any other promotional offers.
Home / Mental Health / The do’s and don’ts of managing schizophrenia
The do’s and don’ts of managing schizophrenia
Please login to bookmark.
Username or Email Address
Remember Me

Schizophrenia is a serious mental health condition affecting an estimated 24 million people worldwide — that is 1 in every 300 people. Although the exact symptoms can vary from person to person, schizophrenia may cause hallucinations, delusions and disorganized behavior, as well as loss of interest in activities and social withdrawal. Cognitive symptoms might also impact functions such as attention and memory.
Unlike mental health conditions that appear in childhood, schizophrenia tends to develop during someone’s late teens or twenties. Navigating this diagnosis — especially during what is, for most people, a pivotal time of transition to adulthood — takes grit, a support system and a solid understanding of what it means to manage schizophrenia.
To get you started, Jonathan G. Leung, Pharm.D., R.Ph., a Mayo Clinic expert and psychiatric clinical pharmacist, discusses some of the most foundational do’s and don’ts of managing schizophrenia.
Just remember — while there’s no way to prevent or fully resolve schizophrenia, a comprehensive treatment strategy can lessen the severity of symptoms and, for some people, stop symptoms from coming back altogether.
Do get educated on your condition
As with many other serious mental health conditions, there are a number of misconceptions about schizophrenia. Learning about the condition can help you separate stigma from fact .
Dr. Leung says there are a number of people who can help you better understand schizophrenia and the resources available to you. These people include psychiatrists, nurses, social workers, and pharmacists. You may also learn from the experiences of people who have been affected by mental illness firsthand.
In addition to learning more generally about schizophrenia, pay attention to how the condition tends to “show up” in your own life, thoughts, moods and behaviors. “Early intervention is particularly important when schizophrenia is recognized,” says Dr. Leung. “Delays in appropriate medication management, psychosocial treatments and general support have been associated with greater symptom burden and decreased functioning and quality of life.
Learning about schizophrenia and understanding warning signs of worsening symptoms can help you receive timely and appropriate follow-up care to proactively control symptoms before they become too severe.
Do understand your treatment options
After diagnosis, it can be overwhelming to parse different treatments. However, understanding your options and the full scope of available treatments is a crucial step in managing schizophrenia.
Antipsychotic medications are often the primary treatment for schizophrenia, but mood stabilizers and antidepressants also may be beneficial for some people. Research has shown that medication can effectively treat symptoms and behaviors associated with schizophrenia, including hallucinations and delusions. However, it’s also important to understand that many of these medications, particularly antipsychotics, can cause significant side effects. Part of assessing your treatment options means carefully considering possible side effects and working with your healthcare team to mitigate or avoid their impact.
Often, medication alone isn’t enough to completely manage schizophrenia. To more fully address symptoms and quality of life, you may pair medication with talk therapy or other psychosocial resources like family interventions and education, cognitive-behavioral therapy (CBT), and social skills training. Dr. Leung says that some people also find help through peer support sessions or other community-based groups.
In practice, however, access to comprehensive care is often limited by cost, local resource availability, social stigma, medical mistreatment, discrimination, and housing and economic disparities. If you are having trouble accessing quality care or affording treatment, do speak with your healthcare team about the full scope of your options or consult with the Substance Abuse and Mental Health Services Administration (SAMSA) for free . Social services staff also may be able to help coordinate affordable housing, transportation or other care.
Do avoid alcohol and other recreational substances
Alcohol and other recreational substances can jeopardize management of schizophrenia. Critically, substances can change the way medications work in the body — potentially making them less effective or more dangerous to take.
“Substance use can certainly influence or worsen schizophrenia-related symptoms,” says Dr. Leung. “Even cigarette smoking can decrease the effectiveness of certain antipsychotics, and abruptly stopping smoking may cause side effects.” It is important to know how any substance may impact treatment and, in general, it’s best to refrain from using alcohol or other recreational substances.
People with schizophrenia are at a higher risk of developing alcohol use disorder — often referred to as alcoholism — or a substance use disorder. Though it can be difficult to talk openly about your typical drinking or substance use habits, being honest with your healthcare team can help flag any potential substance use issues and ensure your treatment plan is as effective as possible.
Don’t lapse on your treatment plan
Although it’s easy to get discouraged while seeking care, Dr. Leung says it’s critical to stick to your treatment plan.
“Stopping medications abruptly or tapering off or discontinuing medications by yourself and without the support of your healthcare team can lead to relapse of severe symptoms,” says Dr. Leung. Likewise, he advises following through with appointments and staying in regular contact with your healthcare team.
If you are unhappy with your treatment plan or are experiencing any side effects or circumstances that are hurting your quality of life, work with your team to make realistic and effective adjustments that work with your needs. There are so many medication options, Dr. Leung says, that it is highly likely a change is possible. For example, if you don’t like taking pills every day, rather than discontinuing use, you may talk with your healthcare team about medications that are effective longer and aren’t taken as frequently.
“This all gets back to establishing relationships with your care team,” says Dr. Leung. “It has to be a two-way street, where people have input and make shared decisions with their doctors about their treatment.”
Don’t forget to ask questions
Finally, ask questions — especially when you’re unsure about treatment options, may be experiencing new or unexpected symptoms or side effects, or simply need more help .
If you tend to feel overwhelmed during appointments with your care team, talk therapy or group sessions, consider writing down your questions beforehand so you can refer to them in the moment. You may also find it helpful to take notes during conversations with your healthcare team or to bring a trusted friend or family member to help you navigate conversations about your condition or treatment.
“Sometimes not knowing what questions to ask can be a barrier to care,” says Dr. Leung. To help get you started, he recommends always asking about:
- Medication options and their potential short-term and long term-side effects.
- Resources for people in your area and how to connect with them.
- What a long-term treatment plan looks like for you.

Discover more Mental Health content from articles, podcasts, to videos.
You May Also Enjoy

Privacy Policy
We've made some updates to our Privacy Policy. Please take a moment to review.
Table of Contents - Symptoms of Schizophrenia and Schizophrenia Diagnosis
- How is Schizophrenia Diagnosed?
- Free, On-line Early Schizophrenia Screening test - Try It!
- What to do if you suspect you or your loved one may have a psychiatric disorder
- Worldwide list of early psychosis/schizophrenia diagnosis and treatment clinics
- Finding a good psychiatrist - an important first step in the treatment process
The Common Symptoms of Schizophrenia
- Childhood-Onset Schizophrenia (under age 13 years)
- Other Types of Schizophrenia
Potential Problems
- Related Disorders - sometimes mistaken for schizophrenia, or vice-versa
- Schizophrenia and Psychosis - What's the Difference?
- Schizophrenia - Hypothetical Examples
- What if my family member refuses to see a doctor? (information from our FAQ guide)
What to do Next
- After Recieving a Diagnosis - What family members can do
- Information on Treating Schizophrenia
- Support groups in the United States and other countries
More information on Schizophrenia Diagnosis and Treatment
- Articles on Diagnosing Schizophrenia and Advances in Schizophrenia Science
- The Importance of Schizophrenia Early Detection and Treatment
- What to do when someone can't understand they have schizophrenia - Assisted Treatment
- Dual Diagnosis (Schizophrenia and Drug Addiction/Alcoholism)
Schizophrenia Diagnosis-related News Stories:
Archive: Full List of News on Schizophrenia Diagnosis
Schizophrenia Symptoms and Diagnosis
There is currently no physical or lab test that can absolutely diagnose schizophrenia - a psychiatrist usually comes to the diagnosis based on clinical symptoms. What physical testing can do is rule out a lot of other conditions (seizure disorders, metabolic disorders, thyroid disfunction, brain tumor, street drug use, etc) that sometimes have similar symptoms. Current research is evaluating possible physical diagnostic tests (such as a blood test for schizophrenia , special IQ tests for identifying schizophrenia , eye-tracking , brain imaging , 'smell tests ', etc), but these are still in trial stages at only a few universities and companies and are not yet widely used. It will likely be a few years before these on the market, and adopted by hospitals, etc.
People diagnosed with schizophrenia usually experience a combination of positive (i.e. hallucinations, delusions, racing thoughts), negative (i.e. apathy, lack of emotion, poor or nonexistant social functioning), and cognitive (disorganized thoughts, difficulty concentrating and/or following instructions, difficulty completing tasks, memory problems). Please refer to the information available on this page ( see below ) for common signs and symptoms, as well as consumer/family stories of how they identified schizophrenia in their own experiences. However, only a psychiatrist can make a diagnosis and start a treatment program. If you are experiencing symptoms are bothersome, debilitating, or harmful, please we recommend you try the on-line Screening test for identification of early schizophrenia symptoms (click here to go to the test) that we offer on this web site. The on-line test is also available in an "off-line version" for print-out (valuable for testing a family member who is not on-line, or who may not like the site of a schizophrenia-focused web site) - and the responses can then be entered into the on-line version of the test for scoring. If you test positive you may want to go to to an early psychosis diagnosis and treatment center or make an appointment with your doctor and/or a psychiatrist.
The First Steps Towards Proper Diagnosis
The first step in getting treatment for schizophrenia is getting a correct diagnosis. This is important to do quickly because research has shown that the sooner you get diagnosed and treated, the better the long-term outcome (which is the same for all serious illnesses). This can be a more difficult than it might seem, because the symptoms of schizophrenia can be similar at times to other major brain disorders, such as bipolar disorder (manic-epression) or even major depression. Another issue is that a person with schizophrenia may be paranoid or believe that nothing is wrong with them, and therefore may not want to go to see a doctor. Because many regular family doctors may not be very familiar with schizophrenia, it is important to see a good psychiatrist that is experienced in the diagnosis and treatment of schizophrenia.
The best place for proper diagnosis of psychosis (hallucinations & delusions) and schizophrenia - are at the increasing number of centers focused on early diagnosis and treatment of psychosis and schizophrenia. See the following list to find out if there is one in your area: Worldwide list of early psychosis/schizophrenia diagnosis and treatment clinics .
Another way to do find a good psychiatrist is to contact a local support group that deals with brain disorders such as schizophrenia, and talk to the other members that already have experience with the local psychiatrists. If that is not convenient, we recommend you join in our discussion areas (see "parents" area or "Main Area" listed on home page ) and ask there if anyone can recommend a good psychiatrist in your area. Local members may be able to recommend a good psychiatrist experienced in schizophenia that they have worked with.
See our FAQ guide, with sections on finding and working with a good psychiatrist. This is a vital part of the treatment and recovery process, as research and anecdotal evidence both confirm that a good patient-doctor relationship can be important for enhancing treament compliance.
If you have a family history of schizophrenia, psychiatric illness, or other serious conditions in your family, it can be a great help to the doctor if you create a Health Family Tree that tracks such diseases through family generations. Having a family health history in front of them can help providers decide which diagnostic and screening tests are most appropriate for you or your loved one. Create your own Health Family Tree with this free, web-based software (provided by the Health and Human Services Dept).
As with most serious illnesses, its important to get diagnosis and treatment as quickly as possible. Getting treatment early can significantly improve an individual's chances at a partial or complete recovery by preventing further brain damage or other damage caused by the disease symptoms. More information on the importance of early diagnosis and treatment
- A comprehensive list of early signs - compiled by a schizophrenia.com member. Note: please use as a reference only, not as a diagnostic tool. Only a doctor can diagnose schizophrenia, or any other psychiatric disorder. Many of the common signs/symptoms are also present in healthy people, usually to a lesser degree.
- The Importance of Keeping a Journal - For best diagnosis and recovery of person with schizophrenia
- Early Predictions of Schizophrenia are Possible (BBC News, January 05)
Symptoms are typically divided into positive and negative symptoms because of their impact on diagnosis and treatment. Positive symptoms are those that appear to reflect an excess or distortion of normal functions. The diagnosis of schizophrenia, according to DSM-IV, requires at least 1-month duration of two or more positive symptoms, unless hallucinations or delusions are especially bizarre, in which case one alone suffices for diagnosis. Negative symptoms are those that appear to reflect a diminution or loss of normal functions. These often persist in the lives of people with schizophrenia during periods of low (or absent) positive symptoms. Negative symptoms are difficult to evaluate because they are not as grossly abnormal as positives ones and may be caused by a variety of other factors as well (e.g., as an adaptation to a persecutory delusion). However, advancements in diagnostic assessment tools are being made.
Diagnosis is complicated by early treatment of schizophrenia�s positive symptoms. Antipsychotic medications, particularly the traditional ones, often produce side effects that closely resemble the negative symptoms of affective flattening and avolition. In addition, other negative symptoms are sometimes present in schizophrenia but not often enough to satisfy diagnostic criteria (DSM-IV): loss of usual interests or pleasures (anhedonia); disturbances of sleep and eating; dysphoric mood (depressed, anxious, irritable, or angry mood); and difficulty concentrating or focusing attention.
Currently, discussion is ongoing within the field regarding the need for a third category of symptoms for diagnosis: disorganized symptoms. Disorganized symptoms include thought disorder, confusion, disorientation, and memory problems. While they are listed by DSM-IV as common in schizophrenia�especially during exacerbations of positive or negative symptoms (DSM-IV)�they do not yet constitute a formal new category of symptoms. Some researchers think that a new category is not warranted because disorganized symptoms may instead reflect an underlying dysfunction common to several psychotic disorders, rather than being unique to schizophrenia.
| : - false beliefs strongly held in spite of invalidating evidence, especially as a symptom of mental illness: for example, - Hallucinations can take a number of different forms - they can be: Disorganized speech (e.g., frequent derailment or incoherence) - these are also called "word salads". Ongoing disjointed or rambling monologues - in which a person seems to talking to himself/herself or imagined people or voices. (An abnormal condition variously characterized by stupor/innactivity, mania, and either rigidity or extreme flexibility of the limbs). "Negative" symptoms of Schizophrenia , these symptoms are the lack of important abilities. Some of these include: or poverty of speech, is the lessening of speech fluency and productivity, thought to reflect slowing or blocked thoughts, and often manifested as short, empty replies to questions. Affective flattening is the reduction in the range and intensity of emotional expression, including facial expression, voice tone, eye contact (person seems to stare, doesn't maintain eye contact in a normal process), and is not able to interpret body language nor use appropriate body language. is the reduction, difficulty, or inability to initiate and persist in goal-directed behavior; it is often mistaken for apparent disinterest. (examples of avolition include: no longer interested in going out and meeting with friends, no longer interested in activities that the person used to show enthusiasm for, no longer interested in much of anything, sitting in the house for many hours a day doing nothing.) Only one Criterion A symptom is required if delusions are bizarre or hallucinations consist of a voice keeping up a running commentary on the person�s behavior or thoughts, or two or more voices conversing with each other. |
| Positive Symptoms of Schizophrenia are firmly held erroneous beliefs due to distortions or exaggerations of reasoning and/or misinterpretations of perceptions or experiences. Delusions of being followed or watched are common, as are beliefs that comments, radio or TV programs, etc., are directing special messages directly to him/her. are distortions or exaggerations of perception in any of the senses, although auditory hallucinations (�hearing voices� within, distinct from one�s own thoughts) are the most common, followed by visual hallucinations. also described as �thought disorder� or �loosening of associations,� is a key aspect of schizophrenia. Disorganized thinking is usually assessed primarily based on the person�s speech. Therefore, tangential, loosely associated, or incoherent speech severe enough to substantially impair effective communication is used as an indicator of thought disorder by the DSM-IV. includes difficulty in goal-directed behavior (leading to difficulties in activities in daily living), unpredictable agitation or silliness, social disinhibition, or behaviors that are bizarre to onlookers. Their purposelessness distinguishes them from unusual behavior prompted by delusional beliefs. are characterized by a marked decrease in reaction to the immediate surrounding environment, sometimes taking the form of motionless and apparent unawareness, rigid or bizarre postures, or aimless excess motor activity. sometimes present in schizophrenia but not often enough to be definitional alone include affect inappropriate to the situation or stimuli, unusual motor behavior (pacing, rocking), depersonalization, derealization, and somatic preoccupations. is the reduction in the range and intensity of emotional expression, including facial expression, voice tone, eye contact, and body language.or poverty of speech, is the lessening of speech fluency and productivity, thought to reflect slowing or blocked thoughts, and often manifested as short, empty replies to questions. is the reduction, difficulty, or inability to initiate and persist in goal-directed behavior; it is often mistaken for apparent disinterest. (examples of avolition include: no longer interested in going out and meeting with friends, no longer interested in activities that the person used to show enthusiasm for, no longer interested in much of anything, sitting in the house for many hours a day doing nothing.) |
- Paranoid schizophrenia - These persons are very suspicious of others and often have grand schemes of persecution at the root of their behavior. Halluciations, and more frequently delusions, are a prominent and common part of the illness.
- Disorganized schizophrenia (Hebephrenic Schizophrenia) - In this case the person is verbally incoherent and may have moods and emotions that are not appropriate to the situation. Hallucinations are not usually present.
- Catatonic schizophrenia - In this case, the person is extremely withdrawn, negative and isolated, and has marked psychomotor disturbances.
- Residual schizophrenia - In this case the person is not currently suffering from delusions, hallucinations, or disorganized speech and behavior, but lacks motivation and interest in day-to-day living.
- Schizoaffective disorder - These people have symptoms of schizophrenia as well as mood disorder such as major depression, bipolar mania, or mixed mania.
- Undifferentiated Schizophrenia - Conditions meeting the general diagnostic criteria for schizophrenia but not conforming to any of the above subtypes, or exhibiting the features of more than one of them without a clear predominance of a particular set of diagnostic characteristics.
- Additional Information on Types of Schizophrenia
Misdiagnosis Issues Because there is currently no physical test that confirms the presence of schizophrenia, and because schizophrenia often shares a significant number symptoms with other disorders, misdiagnosis is a common problem. According to one study surveying members of the National Depression and Bipolar Support Alliance, there is an average delay of 10 years from the first onset of symptoms to correct diagnosis and treatment of psychiatric disorders.
However, getting a correct diagnosis is necessary for finding a treatment program that works for you.
Being aware of the potential for misdiagnosis, and knowing what other disorders may appear like schizophrenia or vice-versa, will hopefully help you get started on the right treatment as soon as possible.
- Article on Schizophrenia Misdiagnosis Problems
- An overview of bipolar disorder symptoms and diagnostic criteria (ext. link)
- A true story of misdiagnosis - a case where a blood test might have averted the mistake.
- Schizoid Personality
- Schizophreniform Disorder
- Schizotypal Personality
- Bipolar Disorder (Manic Depression) - frequently misdiagnosed as schizophrenia (and vise versa)
- Example of Misdiagnosis - BBC News
- It is valuable to understand the difference between psychosis and schizophreia. Psychosis is a general term used to describe psychotic symptoms. Schizophrenia is a kind of psychosis. Several different brain disorders can lead to psychotic symptoms, including lesions in the brain resulting from head traumas, strokes, tumors, infections or the use of illegal drugs. If a serious depression goes untreated for a long time, psychotic symptoms may develop. These examples demonstrate that not all psychosis is schizophrenia. If is for this reason that doctors may take quite some time (6 months or more) to diagnose someone, because while the symptoms of schizophrenia are quite obvious - the fact that the symptoms are not being caused by some other brain disorder is frequently not obvious.
- Stages of Psychosis
- The Prodromal (early) Phase of First-episode Psychosis: Past and Current Conceptualizations
Articles on Diagnosing Schizophrenia and Advances in the Science
Before a psychiatrist or doctor will arrive at a diagnosis of schizophrenia they must make a thorough psychiatric evaluation. This includes a medical evaluation, a physical exam, a mental status exam and appropriate laboratory tests. Also a full history of the illness should be conveyed to the doctor (see "The Importance of a Journal for the person with schizophrenia ") that includes any changes in thinking, behavior, movement, mood, etc. - as seen by the family or patient. Increasingly doctors are also using Magnetic Resonance Imaging (MRIs) to create images of the brain and compare them with known abnormalities in the brain that are frequently caused by, or associated with, schizophrenia.
- Decoding Schizophrenia (Scientific American, January, 2004)
- The Diagnostic Criteria for Schizophrenia - American [external. link]
- The Diagnostic Criteria for Schizophrenia - European [ext. link]
Although there are currently no physical tests that absolutely confer a diagnosis of schizophrenia, the science is becoming increasingly more specific. Recent advances in diagnostic screening tests for schizophrenia include the following:
EEG Scan for Schizophrenia (News, July 2005) Brain Scans for Schizophrenia Brain Imaging May Detect Schizophrenia in Early Stages Blood Test for Schizophrenia (in development - preliminary results promising as of Feb 2005) Smell Test for Schizophrenia Schizophrenia Test Moves Closer
- Early Detection and Treatment for Schizophrenia - Articles and Recent Research/Tests
- Early Diagnosis of Schizophrenia Improves Results of Treatment (Yale University, Feb. 2004)
- The Importance of Early Detection and Treatment in Schizophrenia (8/96)
- The Importance and The Rationale for Early Detection and Intervention
- Early Detection and Intervention for Initial Episodes of Schizophrenia
- Detection as a Baby - Early Detection of Schizophrenia via Movement Analysis (12/96) Note: this technique would seem to be valuable in families with a history of mental illness.
- Dual Diagnosis Program in Australia (3/97)
- Livengrin Foundation Announces Dual Diagnosis Program (7/96)
- Dual Diagnosis - Drugs and Mental Illness
- What to do if some one is mentally ill and has a chemical dependency












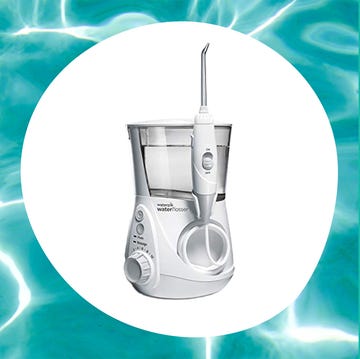







COMMENTS
In addition to schizophrenia, other mental health conditions that may present with symptoms of disorganized speech include: dementia (neurocognitive disorder) schizoaffective disorder
It's a part of formal thought disorder, which can also manifest as disorganized behaviors. Signs and symptoms may include: atypical communication patterns. responding externally to internal ...
Symptoms of disorganized speech include: Difficulty forming or structuring complete words, sentences, or paragraphs. Responding to questions with unrelated or irrelevant matter. Indirect, rambling speech that appears to have no goal. Difficulty following conversations. Repeating words.
incoherent speech or rambling. severely disorganized behavior in one or more aspects. negative symptoms like avolition, lack of pleasure, blunted affect, or alogia. Clinicians also need to confirm ...
For people with schizophrenia, these things seem real. Hallucinations can occur with any of the senses, but hearing voices is most common. Disorganized speech and thinking. Disorganized speech causes disorganized thinking. It can be hard for people with schizophrenia to talk with other people.
Disorganized or hebephrenic schizophrenia describes a person with schizophrenia who has symptoms including: disorganized thinking. unusual speech patterns. flat affect. emotions that don't fit ...
The symptoms of disorganized thoughts and behavior are known as hebephrenia. Hebephrenia is characterized by disorganized behavior and speech as well as disturbance in emotional expression, known ...
P & T : a peer-reviewed journal for formulary management, 39(9), 638-645. of the primary symptoms of the disorder, such as delusions, hallucinations, disorganized speech and behavior, catatonia, and negative symptoms, consistently for a month or longer.
Confused thoughts and disorganized speech. ... Being aware of the symptoms of schizophrenia can help you recognize when someone may be dealing with the disorder. If you are concerned someone you ...
Disorganised symptoms. What are disorganised symptoms in people with schizophrenia? Key features of the symptoms of disorganisation include disorganised speech and behaviour, as well as inappropriate affect. Severely disorganised speech is difficult to follow, being incoherent, irrelevant and/or illogical. These symptoms are sometimes referred ...
Disorganized schizophrenia, or hebephrenia, ... expression of the disorganization syndrome that has been hypothesized to be one aspect of a three-factor model of symptoms in schizophrenia, [3] ... The prominent characteristics of this form are disorganized behavior and speech (see formal thought disorder), ...
Common symptoms include hallucinations, delusions, disordered thoughts, and disorganized speech. People with schizophrenia may also experience cognitive problems like low motivation and trouble ...
Disorganized speech. Grossly disorganized or catatonic behavior. Negative symptoms (e.g., reduced emotional expression). One of the symptoms must be either (1), (2), or (3). Additionally, continuous signs of the disturbance must persist for at least six months. Causes of Schizophrenia. Genetics: A higher risk if there is a family history of ...
Disorganized speech makes effective communication a challenge, while disorganized behavior can lead to difficulties in performing routine tasks and social interactions. Understanding these symptoms is crucial for recognizing the challenges faced by individuals with schizophrenia and providing them with the appropriate support and treatment.
Schizophreniform disorder: Causes the same symptoms of schizophrenia, such as delusions, hallucinations, negative symptoms, and disorganized speech—but these are short-term and only last between ...
Also, at least one symptom must be from among the first three on this list: delusions. hallucinations. disorganized speech, such as frequent derailment or incoherence. grossly disorganized or ...
A. Characteristic symptoms: Two (or more) of the following, each present for a significant portion of time during a 1-month period (or less if successfully treated): delusions. hallucinations. disorganized speech (e.g., frequent derailment or incoherence) grossly disorganized or catatonic behavior.
Disorganized speech or trouble concentrating; A combination of genetic and environmental factors likely influences schizophrenia. While having risk factors may increase a person's susceptibility, it doesn't guarantee that a person will develop the disorder. ... Schizophrenia symptoms can be sensitive to seemingly minor stimuli. Researchers ...
To receive a schizophrenia diagnosis, someone can have any of the symptoms and features, but he must have the following: At least two symptoms from Criteria A. One of those two must be delusions, hallucinations, or disorganized speech. These must have been present for at least one month. The symptoms must impair one's life and get in the way ...
Schizophrenia: Characterized by two or more symptoms (either hallucinations, delusions, disorganized speech, or disorganized/catatonic behaviors) for more than a month; Schizophreniform disorder: A condition similar to schizophrenia lasting less than one month; Schizoaffective disorder: Involving schizophrenia and a mood disorder like depression
Schizophrenia is a serious mental health condition affecting an estimated 24 million people worldwide — that is 1 in every 300 people. Although the exact symptoms can vary from person to person, schizophrenia may cause hallucinations, delusions and disorganized behavior, as well as loss of interest in activities and social withdrawal.
Disorganized speech/thinking, also described as "thought disorder" or "loosening of associations," is a key aspect of schizophrenia. Disorganized thinking is usually assessed primarily based on the person's speech.
Anosognosia can make treating schizophrenia more difficult. 4. Concentration and memory problems. Cognitive difficulties are another common sign of schizophrenia, though admittedly, these can ...
The severity of schizophrenia symptoms ranges widely; it is a lifelong condition that requires treatment with a combination of medication and therapy. ... Disorganized thinking and speech, or ...
In addition to hallucinations, sufferers can exhibit delusions, disorganized speech, difficulty thinking and lack of motivation, according to the American Psychiatric Association.
Schizophrenia • Diagnostic Criteria: - Persistent presence of two or more core symptoms: hallucinations, delusions, disorganized speech, disorganized or catatonic behavior, negative symptoms. - Significant social or occupational dysfunction. ... Symptoms identical to schizophrenia but duration of an episode is at least 1 month but less than 6 ...
Psychosis involves a different perception of reality and includes symptoms like delusions and hallucinations. Clanging is considered disorganized speech, a formal symptom of schizophrenia ...
Over time, his condition progressed to include memory impairment, disorganized behavior, and seizures. Initially misdiagnosed with schizophrenia, the correct diagnosis of LGI1 antibody-associated encephalitis was eventually established through positive serum and cerebrospinal fluid (CSF) tests for LGI1 antibodies.