

Learning, Remembering, Believing: Enhancing Human Performance (1994)
Chapter: self-confidence and performance, 8 self-confidence and performance.
Self-confidence is considered one of the most influential motivators and regulators of behavior in people's everyday lives (Bandura, 1986). A growing body of evidence suggests that one's perception of ability or self-confidence is the central mediating construct of achievement strivings (e.g., Bandura, 1977; Ericsson et al., 1993; Harter, 1978; Kuhl, 1992; Nicholls, 1984). Ericsson and his colleagues have taken the position that the major influence in the acquisition of expert performance is the confidence and motivation to persist in deliberate practice for a minimum of 10 years.
Self-confidence is not a motivational perspective by itself. It is a judgment about capabilities for accomplishment of some goal, and, therefore, must be considered within a broader conceptualization of motivation that provides the goal context. Kanfer (1990a) provides an example of one cognitively based framework of motivation for such a discussion. She suggests that motivation is composed of two components: goal choice and self-regulation. Self-regulation, in turn, consists of three related sets of activities: self-monitoring, self-evaluation, and self-reactions. Self-monitoring provides information about current performance, which is then evaluated by comparing that performance with one's goal. The comparison between performance and goal results in two distinct types of self-reactions: self-satisfaction or -dissatisfaction and self-confidence expectations. Satisfaction or dissatisfaction is an affective response to past actions; self-confidence expectations are judgments about one's future capabilities to attain one's goal. This framework allows a discussion of self-confidence as it relates to a number of motivational processes, including setting goals and causal attributions.
One theoretical perspective of self-confidence that fits well in Kanfer's (1990b) framework of motivation and has particular relevance to enhancing self-confidence in a variety of domains of psychosocial functioning is self-efficacy theory (Bandura, 1977, 1986). Self-efficacy theory is also useful in guiding the development of motivational programs because self-beliefs of confidence operate in most of the approaches to cognitive theories of motivation, particularly goal-setting theory and attribution theory (Bandura, 1990).
This chapter provides an overview of the self-efficacy concept of self-confidence and its relationship to other cognitively based motivational processes that influence learning and performance; it does not attempt to integrate the different theories of motivation that incorporate self-confidence constructs. (For summaries and comparisons of cognitive theories of motivation, see Frese and Sabini, 1985; Halisch and Kuhl, 1987; Kanfer, 1990b; Pervin, 1989.) We first define self-confidence and related concepts. Next, an overview of self-efficacy theory is given, along with a review of the relevant research. The third section covers applications of techniques for enhancing self-confidence. Lastly, we note the research questions that follow from what is currently known.
''SELF-CONFIDENCE" AND RELATED CONCEPTS
Terms such as "self-confidence," "self-efficacy," "perceived ability," and "perceived competence" have been used to describe a person's perceived capability to accomplish a certain level of performance. Bandura (1977) uses the term "self-efficacy" to describe the belief one has in being able to execute a specific task successfully (e.g., solving a math problem) in order to obtain a certain outcome (e.g., self-satisfaction or teacher recognition) and, thus, can be considered as situationally specific self-confidence. 1 Self-efficacy is not concerned with an individual's skills, but, rather, with the judgments of what an individual can accomplish with those skills (Bandura, 1986). Bandura (1986, 1990) distinguishes between "self-efficacy" and "self-confidence": self-confidence refers to firmness or strength of belief but does not specify its direction; self-efficacy implies that a goal has been set. We do not adopt Bandura's distinction, but use the term "self-confidence" because it is more familiar to most individuals. "Self-confidence," as the term is used here, is the belief that one can successfully execute a specific activity, rather than a global trait that accounts for overall performance optimism. For example, one may have a lot of self-confidence in one's ability at golf but very little self-confidence in one's tennis skills.
"Perceived competence" and "perceived ability" are terms that have been used in the research literature on achievement and mastery motivation. They indicate the perception that one has the ability to master a task resulting from cumulative interactions with the environment (Harter, 1981; Nicholls,
1984). In sports and physical movement, Griffin and Keogh (1982) developed the concept of "movement confidence" to describe a person's feeling of adequacy in a movement situation; Vealey (1986) used the term "sport confidence" to define the belief or degree of certainty individuals possess about their ability to be successful in sport. Some organizational psychologists use the term "state expectancy'' in essentially the same manner as Bandura's (1977) concept of self-efficacy (Eden, 1990).
Some terms related to self-confidence are occasionally confused with the construct. Some authors (e.g., Kirsch, 1985) have tried to implement Bandura's (1977) concept of self-confidence (self-efficacy) as an expectancy construct. Bandura distinguishes judgments of personal efficacy from the expectancy construct in expectancy-by-value theories (e.g., Fishbein and Ajzen, 1975; Triandis, 1977): self-confidence is a judgment of one's ability to perform at a certain level; expectancies pertain to the outcomes one expects from a given level of effort. In essence, confidence expectations are concerned with beliefs about one's competence and outcome expectations are concerned with beliefs about one's environment. For example, a person may believe that running a marathon in less than 2 hours will lead to social recognition, money, and self-satisfaction (outcome belief), but may question whether she can actually run that fast (confidence belief). Similarly, a woman may believe that Karate self-defense techniques will deter assault (outcome belief), but may doubt her capability to be effectively aggressive against a powerful assailant (confidence belief).
Bandura (1986) asserts that, in a responsive environment that rewards performance achievements, the outcomes people expect depend heavily on their self-confidence that they can perform the skill. However, in an environment in which outcomes are fixed at a minimum level of performance or in which a social condition restricts people's ability to perform successfully or control their circumstances, outcome and confidence expectations would not be causally linked. For example, a concentration camp inmate could have confidence that he or she is efficacious enough to maximize his or her survival probability without violating personal ethics while simultaneously believing that this survival probability is not very high at all. Such individuals may give up trying, not because they doubt their own capabilities, but because they expect their efforts to be futile. This type of outcome-based futility is hypothesized to lead to pessimism or learned helplessness (Bandura, 1986).
"Self-concept" represents a composite view of oneself that is developed through evaluative experiences and social interactions. As Bandura (1986) has noted, however, a person's self-conceptions become more varied across activities with increasing experience. Thus, global measures of self-concept will not predict the intra-individual variability in a performance situation as well as self-confidence perceptions that vary across activities and
circumstances. Rather, global measures of self-concept are helpful to understanding one's total outlook toward life. However, it should be noted that people's self-concepts have also been shown to be malleable in certain situations (Markus and Kunda, 1986). (For a thorough discussion of self-concept, see Hattie, 1992.)
"Self-esteem" is another global construct related to self-confidence and self-concept and pertains to one's personal perception of worthiness. Although self-confidence and self-esteem may be related, individuals can have one without necessarily having the other. Certain individuals may not have high self-confidence for a given activity, but still "like themselves"; by contrast, there are others who may regard themselves as highly competent at a given activity but do not have corresponding feelings of self-esteem. (For a thorough discussion of the concept of self-esteem with respect to work behavior, see Brockner, 1988.)
Other related concepts include locus of control, optimism or pessimism (learned helplessness), healthy illusions, and level of aspiration. Rotter's (1966) notion of locus of control is concerned with a person's generalized expectancies about his or her ability to control reinforcements in life: individuals who tend to perceive events as internally controlled behave more self-determinedly; those who tend to perceive events as beyond their control behave more fatalistically. Although an internal locus of control orientation may create a high sense of confidence, the two constructs must be distinguished. Bandura (1986) points out that locus of control is based on outcome expectancies rather than confidence expectancies. For instance, people who believe that their physical health is personally determined but find it is failing despite their efforts to improve it would experience low self-confidence. Studies have shown that task-specific self-confidence expectancies are better predictors of successful behavior in specific situations than are general measures of perceived control (Kaplan et al., 1984; Manning and Wright, 1983).
Optimism and pessimism have been defined by some authors in terms of generalized expectancies for internal or external locus of control (Scheier and Carver, 1992). Scheier and Carver (1992:203) define "dispositional optimism" as the "tendency to believe that one will generally experience good vs. bad outcomes in life." Optimism and pessimism have also been conceptualized within an attributional or explanatory style framework (Abramson et al., 1978; Peterson and Bossio, 1991). In an attributional view, individuals base their expectations for controlling future events on their causal explanations for past events. Optimism is the tendency to attribute negative events to causes that are unstable, specific, and external; pessimism or learned helplessness is the tendency to attribute negative events to causes that are stable, global, and internal. Optimism and pessimism or learned helplessness are considered to be much more global concepts than task-specific
self-confidence and, thus, are more resistant to short-term interventions to change them. In addition, optimism and pessimism emphasize perceptions of controllability of the environment rather than the sense of personal agency to control the environment.
A concept similar to optimism has been described as healthy illusions (Taylor and Brown, 1988) or positive denial (Lazarus, 1979), which involves a slight distortion of reality in the positive direction. Such illusions can help sustain one's hopes of success, keep morale high, and lower anxiety (Hackett and Cassem, 1974). As Peterson and Bossio (1991) explain in relation to severe illnesses, the immediate denial of the severity of an illness allows individuals to face crises slowly, which helps their motivation to recover. However, if denial or illusion is too far removed from reality, it can get in the way of recovery and taking action to improve one's situation or performance.
Level of aspiration, first conceptualized in the 1930s within the scientific analysis of goal-striving behavior, is concerned with people's estimation of their subsequent performance prior to trying a task. An early investigator (Frank, 1935:119) defined it specifically as "the level of future performance in a familiar task which an individual, knowing his level of past performance in that task, explicitly undertakes to reach." Once a level of aspiration has been set, the individual performs, examines the discrepancy between the level of aspiration and the performance, and reacts with feelings of success or failure (depending on discrepancy). These reactions could lead to trying harder, leaving the activity altogether, or continuing with a readjusted level of aspiration (Lewin et al., 1944). Early investigations on levels of aspiration were the precursors to modern research on various cognitive aspects of goal-setting, self-appraisal, and feeling of satisfaction regarding relative success and failure. Much of the basis for current views on self-regulation in terms of self-monitoring, self-evaluation, and self-reaction can be found within the level-of-aspiration paradigm (see Bandura, 1982; Carver and Scheier, 1990).
The earlier research, most of which occurred in the 1930s and 1940s (see, e.g., Festinger, 1942; Frank, 1935, 1941; Lewin et al., 1944), tried to determine the factors that influence the fluctuations in a person's level of aspiration (e.g., success and failure of comparison groups) or studied how well personality traits correlated with the phenomenon. One general finding in relation to success and failure was that subjects raised their level of aspiration after success and lowered it after failure. However, Bandura has shown that this finding does not automatically occur in real-life tasks: "Having surpassed a demanding standard through laborious effort does not automatically lead people to raise their aspiration" (Bandura, 1986:348). Whether one raises one's level of aspiration or not depends more on one's level of task-specific self-confidence. This is the additional self-evaluation mechanism
that Bandura (1977) has added to the old paradigm and the self-regulation model. In contrast, Carver and Scheier (1990) emphasize the rate of discrepancy reduction or rate of progress made toward a goal over time in determining one's level of aspiration.
Although many of the concepts related to self-confidence are investigated from different perspectives, the phenomenon of interest for most of them is the cognitive process by which a person regulates thoughts and action to attain desired outcomes or to control events in his or her life.
THEORETICAL PERSPECTIVES
Self-efficacy theory was developed within the framework of a social cognitive theory (Bandura, 1986). Bandura poses self-confidence as a common cognitive mechanism for mediating people's motivation, thought patterns, emotional reactions, and behavior. The theory was originally proposed to account for the different results achieved by the diverse methods used in clinical psychology for treating anxiety. It has since been expanded and applied to other domains of psychosocial functioning, including motivation, cognitive skill acquisition, career choice and development, health and exercise behavior, and motor performance. (For reviews on specific domains, see Feltz, 1988b; Lent and Hackett, 1987; McAuley, 1992; O'Leary, 1985; Schunk, 1984a). The theory has also been found to be equally predictive cross-culturally (Earley, 1993; Matsui, 1987; Matsui and Onglatco, 1991).
Self-Confidence Information
Self-confidence beliefs, defined as people's judgments of their capability to perform specific tasks, are a product of a complex process of self-persuasion that relies on cognitive processing of diverse sources of confidence information (Bandura, 1990). These sources of information include performance accomplishments, vicarious experiences, verbal persuasion, and physiological states.
Performance accomplishments are supposed to provide the most dependable confidence information because they are based on one's own mastery experiences. One's mastery experiences affect self-confidence beliefs through cognitive processing of such information. If one has repeatedly viewed these experiences as successes, self-confidence will increase; if these experiences were viewed as failures, self-confidence will decrease. Furthermore, the self-monitoring or focus on successes or failures should have differential effects on behavior and self-confidence, depending on which is monitored (Bandura, 1986): focusing on one's successes should provide more encouragement and greater confidence than focusing on one's failures.
The influence that performance experiences have on perceived self-confidence also depends on the perceived difficulty of the task, the effort expended, the amount of guidance received, the temporal patterns of success and failure, and one's conception of a particular "ability" as a skill that can be acquired versus an inherent aptitude (Bandura, 1986). Bandura has argued that performance accomplishments on difficult tasks, tasks attempted independently, and tasks accomplished early in learning with only occasional failures carry greater confidence value than easy tasks, tasks accomplished with external aids, or tasks in which repeated failures are experienced early in the learning process without any sign of progress.
Confidence information can also be derived through a social comparison process with others (Festinger, 1954). Vicarious sources of confidence information are thought to be generally weaker than performance accomplishments; however, their influence on self-confidence can be enhanced by a number of factors. For instance, the less experience people have had with performance situations, the more they will rely on others in judging their own capabilities. The effectiveness of modeling procedures on one's self-confidence has also been shown to be enhanced by perceived similarities to a model in terms of performance or personal characteristics (George et al., 1992; Gould and Weiss, 1981).
Persuasive techniques are widely used by instructors, managers, coaches, parents, and peers in attempting to influence a learner's confidence, motivation, and behavior. In acquiring expert performance, Ericsson and his colleagues put a great deal of emphasis on parents' and teachers' expectations and verbal persuasions that a child is "talented" as a major influence on the child's self-confidence, motivation, and perceived protection "against doubts about eventual success during the ups and downs of extended preparation" (Ericsson et al., 1993:399). Persuasive information includes verbal persuasion, evaluative feedback, expectations by others, self-talk, imagery, and other cognitive strategies. Self-confidence beliefs based on this type of information, however, are likely to be weaker than those based on one's accomplishments, according to the theory. In addition, persuasive techniques are thought to be most effective when the heightened appraisal is slightly beyond what the person can presently do but still within realistic bounds because people are generally aware that better performances are achievable through extra effort (Bandura, 1986). The extent of persuasive influence on self-confidence has also been hypothesized to depend on the prestige, credibility, expertise, and trustworthiness of the persuader.
The causal attributions that one makes regarding previous achievement behavior also can be thought of as a source of self-persuasive information in formulating future confidence expectations. Causal attributions for previous behavior have been shown to predict confidence expectations (McAuley, 1990; Schunk and Cox, 1986). (This relationship is discussed in more detail below.)
Confidence information can also be obtained from a person's physiological state or condition. Such information is provided through cognitive appraisal (Bandura, 1986), such as associating physiological arousal with fear and self-doubt or with being psyched up and ready for performance. Eden (1990) also suggests that the stress one experiences in work can influence confidence judgments about one's coping capacity for the job. Bandura (1986) also notes that physiological sources of self-confidence judgment are not limited to autonomic arousal. 2 People use their levels of fitness, fatigue, and pain in strength and endurance activities as indicators of their physical inefficacy (Feltz and Riessinger, 1990; Taylor et al., 1985).
These four categories of confidence information—performance accomplishments, vicarious experience, persuasion, and physiological states—are probably not mutually exclusive in terms of the information they provide, though some are more influential than others. How various sources of information are weighted and processed to make judgments given different tasks, situations, and individual skills is as yet unknown. The consequences of these judgments, however, are hypothesized to determine people's levels of motivation, as reflected in the challenges they undertake, the effort they expend in the activity, and their perseverance in the face of difficulties. People's self-confidence judgments can also influence certain thought patterns and emotional reactions (e.g., pride, shame, happiness, sadness) that also influence motivation (Bandura, 1986). For instance, self-confidence beliefs may influence people's success or failure images, worries, goal intentions, and causal attributions.
Self-Confidence, Behavior and Thought Patterns, and Motivation
Bandura (1977) states that self-efficacy (self-confidence) is a major determinant of behavior only when people have sufficient incentives to act on their self-perception of confidence and when they possess the requisite skills. He predicts that self-confidence beliefs will exceed actual performance when there is little incentive to perform the activity or when physical or social constraints are imposed on performance. An individual may have the necessary skill and high self-confidence beliefs, but no incentive to perform. Discrepancies will also occur, according to Bandura, when tasks or circumstances are ambiguous or when one has little information on which to base confidence judgments.
How individuals cognitively process confidence information also influences the relationship between self-confidence and behavior (Bandura, 1977). For example, successes and failures may be distorted in importance. People who overweigh their failures are believed to have lower expectations than those with the same performance levels who do not overweigh their failures.
The relationship between self-confidence expectations and performance accomplishments is also believed to be temporally recursive (Bandura, 1977:194): "Mastery expectations influence performance and are, in turn, altered by the cumulative effect of one's efforts." Bandura (1990) has emphasized the recursive nature of the relationship between self-confidence and thought patterns as well. The relationship between the major sources of confidence information, confidence expectations, and behavior and thought patterns, as predicted by Bandura's theory, is presented in Figure 8-1.
As just discussed, people's self-confidence beliefs are hypothesized to influence certain thought patterns and emotional reactions as well as behavior. Two thought patterns of particular interest to the study of performance motivation are goal intentions and causal attributions; a third thought pattern that can influence self-confidence beliefs is how one thinks about ability.
Self-confidence beliefs have been shown to influence future personal goal-setting and to mediate the relationship between goal intentions and motivation (Earley and Lituchy, 1991). Research has also shown that the stronger people's self-confidence beliefs (assessed independently from their goals), the higher the goals they set for themselves and the firmer their commitments are to them (Locke et al., 1984). In addition, as noted above (Kanfer, 1990a), motivation based on goal intentions is mediated by self-regulatory influences that include two types of self-reactive influences: affective self-evaluation (satisfaction/dissatisfaction), and perceived self-efficacy for goal attainment. Bandura (1990) includes a third type of self-reactive influence: adjustment of personal standards. Figure 8-2 summarizes, schematically, Kanfer's and Bandura's ideas of motivation that are based on goal intentions.
FIGURE 8-1 Relationship between sources of confidence information, confidence expectations, and behavior/thought patterns.
FIGURE 8-2 Conceptions of motivation based on goal intentions.
When performances fall short of people's personal goals (or level of aspiration), they become dissatisfied. Whether this dissatisfaction serves as an incentive or disincentive for enhanced effort is partly influenced by a person's self-confidence for goal attainment and the degree of the discrepancy (Bandura, 1986; Carver and Scheier, 1990). Bandura (1986) predicts that, in general, in the face of negative discrepancies between personal goals and attainments, those who have high self-confidence beliefs will heighten their level of effort and persistence and those who have self-doubts will quickly give up. However, if the degree of the negative discrepancy is perceived as quite large, people's self-confidence for goal attainment will be undermined. In this situation, research has shown that highly self-confident individuals will readjust their goals so as not to further undermine their self-confidence; those with little sense of self-confidence to begin with will become discouraged and abandon their goal altogether (Bandura and Cervone, 1983).
Bandura (1986, 1990) also suggests that confidence beliefs and causal attributions are reciprocal determinants of each other. According to Bandura, self-confidence beliefs help shape causal ascriptions for future behavior. People with self-beliefs of confidence have been shown to attribute failure to lack of effort; people with low self-beliefs of confidence ascribe their failures to lack of ability (Collins, 1982). Causal attributions also play a role in the formation of future confidence expectations (McAuley, 1990; Schunk and Cox, 1986). Successes are more likely to enhance self-confidence if performances are perceived as resulting from ability rather than from luck. Conversely, individuals can talk themselves out of succeeding
by attributing prior failure to inherent ability rather than to bad luck or reduced effort. Studies using causal analyses also indicate that the effects of causal attributions on performance are mediated through self-confidence beliefs (Schunk and Gunn, 1986; Schunk and Rice, 1986).
As noted above, the way that people construe ability may also influence self-confidence beliefs and other self-regulatory factors. Two conceptions of ability have been identified that lead to the development of two goal orientations (Dweck and Leggett, 1988; Elliott and Dweck, 1988; Nicholls, 1984). The first is the conception of ability as an acquirable skill: people who conceive of ability in this way adopt a learning or mastery goal (Ames, 1984; Dweck and Leggett, 1988; Nicholls, 1984). This type of goal-orientation is well suited for skill development because people seek to improve their competence, judge their capabilities in terms of personal improvement, and regard errors as a natural part of the skill-acquisition process. Furthermore, when performance falls short of their goals, they attribute the discrepancy to inadequate effort, and their self-confidence beliefs remain minimally affected.
The second conception of ability is as a more or less inherent aptitude or entity conception: people who have an entity conception of ability adapt a performance or ability-focused goal (Ames, 1984; Dweck, 1986; Nicholls, 1984). People with this conception of ability seek to prove their competence or demonstrate their ability; they avoid demonstrating low ability and use social comparison processes to judge their ability relative to others. This type of goal-orientation is not well suited for skill development because people view errors as a threat to being able to demonstrate their ability and, thus, they avoid adopting challenging goals. When a negative discrepancy occurs between their goals and current performances, they attribute it to low ability. Research has shown that this type of ability conception increases a person's vulnerability to the adverse effects of failure (Elliott and Dweck, 1988; Jourden et al., 1991; Wood and Bandura, 1989). The feeling of failure and the attribution to low ability may also lead to dissatisfaction and a decrease in confidence beliefs and subsequently to goal abandonment. It also diverts attention away from the task and to worry (Kanfer, 1990a). The negative effects of an inherent aptitude conception are most distinct among people with low self-confidence in their ability (Kanfer, 1990a).
The structure and demands of a learning environment establish a motivational climate that can evoke different goal orientations (see Ames, 1992). For instance, schools often establish learning environments that include evaluating student achievement on the basis of normative standards and with extrinsic rewards. This structure encourages learners to use social comparison processes to judge their ability and adopt a performance-goal orientation instead of a mastery-goal orientation. Students, especially those
who lack skills and self-confidence, do far better in school settings that foster a mastery orientation by designing activities for individual challenge, using flexible and heterogeneous grouping arrangements, helping students develop self-management and self-monitoring skills, recognizing individual progress, and involving them in self-evaluation (Ames, 1992).
Team Confidence
Much of the research on self-efficacy (self-confidence) beliefs has focused on the individual level of behavior. However, in many organizational settings, such as business, military, or sport, individuals perform as members of teams rather than just as individuals. Thus, many of the challenges and difficulties people face in organizations reflect team problems requiring team efforts to produce successful performance.
Bandura (1977, 1986) distinguishes between self-efficacy (self-confidence) and perceived collective efficacy (team confidence) in his theory of self-efficacy. Self-efficacy refers to people's judgments of individual capabilities and effort; collective efficacy or team confidence refers to people's judgments of group capabilities and influences "what people choose to do as a group, how much effort they put into it, and their staying power when group efforts fail to produce results" (Bandura, 1986:449). In this view, teams with high collective confidence beliefs should outperform and should persist longer than teams with low perceived collective confidence. Prior to the development of Bandura's theory, Bird and Brame (1978) found team confidence to be the most powerful discriminator of winning and losing teams.
Similarly to self-confidence, the confidence of a team or organization is most likely influenced by diverse sources of confidence information. As with self-confidence beliefs, performance accomplishments of the team are predicted to be the most powerful source of information for team confidence beliefs. Organizations that have an outstanding record of performance undoubtedly cultivate a strong sense of confidence among their members. Likewise, as Eden (1990) noted in his description of organizationwide self-fulfilling prophecies, a serious performance failure—such as the Challenger space shuttle disaster of the National Aeronautics and Space Administration—can decrease the collective confidence of the organization's members, which, in turn, can influence subsequent failures. The perceived collective confidence of a team or group might also be influenced through a collective social comparison process with other teams. It is also possible that reciprocal social influences within a team can raise or lower collective confidence for team performance. For example, the modeling of confidence or ineffectiveness by one member of the group may influence the rest of the group's sense of confidence (Bandura, 1990). In addition, just as persuasive information can influence an individual's sense of self-confidence, collective
efficacy theory suggests that it could also influence an entire group. Charismatic leaders seem to have such persuasive influence on their organization's members (Eden, 1990).
Bandura (1986) further suggests that team confidence is rooted in self-confidence. According to Bandura, a team that has a strong sense of collective confidence can enhance the perceived task-specific confidence of its members, although a team with a weak sense of collective confidence may not totally undermine the perceived self-confidence of its more resilient members (also see Parker, 1992). Members of a team who have weak beliefs in their own individual capabilities are unlikely to be easily transformed into a strong collective force.
In terms of the assessment of perceived team confidence, Bandura (1986) suggests that team confidence may be insufficiently represented as a predictor of team performance through just the sum of the perceived personal confidences of its members, especially on highly interactive tasks or in situations in which members must work together to achieve success. A study of predicting team performance on the basis of individual performances provides some evidence for the possible moderating influence of task type on the confidence-performance relationship in teams (Jones, 1974). Using baseball (which does not require a lot of interaction among team members for team outcome), Jones (1974) predicted team outcome 90 percent of the time. However, for basketball (which does require a lot of interaction), he predicted team outcome only 35 percent of the time. This outcome suggests that the average of team members' perceptions of their team's performance capability should be added to their personal confidence to execute their individual functions in a collective task to measure team confidence.
This construct of team confidence may be related to other constructs of group motivation. For example, a team's collective confidence beliefs may also be influenced by the nature of its collective goals. As interpreted from Bandura (1986), effective team performance would require the merging of diverse individual goals in support of common group goals. If a team consists of a group of members who are all pursuing their own individual goals, they are not as apt to work together to achieve the necessary team goals to be successful, especially on highly interactive tasks. In addition, when the overall success of a team calls for sustained efforts over a long time, short-term intermediate goals may be needed to provide incentives, provide evidence of progress along the way, and sustain team confidence beliefs.
The attributions a team ascribes for its successes and failures may also influence team confidence. For example, an athletic team that defeats a difficult opponent with minimal effort may perceive itself to be highly confident. Conversely, if that same team worked very hard but lost to an easier opponent, perceived team confidence may weaken. Perceived team confidence may, in turn, influence the types of causal attributions that
teams make about their performance (Bandura, 1986, 1990). Teams with little confidence may infer that poor performance was due to a lack of ability; highly confident teams may ascribe poor performance to a lack of effort.
Team confidence and cohesion may also be related. Both constructs have been shown to be positively associated with successful performance and persistence in the face of adversity (Spink, 1990). Thus, team confidence and team cohesion appear to share some common elements.
A team's collective confidence beliefs may similarly be related to a team's desire for success. For example, Zander (1971) found that groups with a strong desire for success outperformed groups with a weaker desire for success. Over time, when a group succeeded more often than it failed, members of that group were more interested in the activity and had a stronger desire for their group to perform well (Zander, 1971). Thus, successful outcome had a cyclical relationship with desire for success. Team confidence could also be part of this relationship. Successful performance can be expected to positively influence team confidence, which in turn should lead to behaviors and actions (e.g., setting higher goals, working harder) that enhance the ability of the group to succeed in the future, resulting in an even stronger desire for group success. This relationship may not hold for tasks that are not intrinsically motivating.
Social loafing may also be conceptualized in terms of team confidence. However, social loafing (conceptualized as the motivational losses in group performance) may represent the dark side of team confidence. In typical team performance situations, the evaluation potential for any one individual is not as strong as it would be for an individual performance, and this situation can give rise to social loafing. If individual team members believe that their team is highly capable of performing a task, they may loaf. Thus, high team confidence may actually undermine contributions to team performance unless there is individual identifiability. There has not yet been research to test this ''undermining" assumption, but a considerable body of research has shown that increasing the identifiability and recognition of individual performances in groups reduces social loafing (e.g., Latané et al., 1979).
Some work suggests that self-confidence mediates the relationship between identifiability of performance and loafing (Sanna, 1992). Highly confident individuals whose performances were identifiable as part of a group's performance were less likely to loaf than were individuals with little confidence in the same situation. The results of this study suggest that when individual contributions toward team performance are identifiable, highly confident members may exert more effort toward performance than members whose confidence is not high. Increased individual effort towards performance usually facilitates successful team performance, which in turn may enhance perceived team confidence.
RESEARCH ON SELF-CONFIDENCE
Evidence for the effectiveness of self-confidence as an influential mechanism in human agency comes from a number of diverse lines of research in various domains of psychosocial functioning, including achievement motivation (Bandura and Cervone, 1983; Schunk, 1984a), career choice and development (Betz and Hackett, 1981), health and exercise behavior (DiClemente, 1981; McAuley and Jacobson, 1991), anxiety disorders (Bandura et al., 1982) and sport and motor performance (Feltz, 1982). Results of these diverse lines of research provide converging evidence that people's perceptions of their performance capability significantly affect their motivational behavior (Bandura, 1986).
This section is not an exhaustive review of all the research on self-confidence and psychosocial functioning; rather, we focus on work that is relevant to enhancing perceived self-confidence and the effects of self-confidence beliefs on performance. The first part of this section looks at research on the effect of various techniques for enhancing self-confidence beliefs; the second part considers the effects of self-confidence on performance; the third part looks at research on team confidence; and the fourth part considers how to apply those research findings.
Enhancing Self-Confidence
Performance-based confidence information.
As noted above, Bandura (1977) proposed that performance accomplishments provide the most dependable source of information on which to base self-confidence judgments because they are based on one's mastery experiences. Techniques based on such performance accomplishments as participant modeling, guided exposure, physical guidance, external aids, and task modification have been effective in enhancing both self-confidence beliefs and performance in a wide variety of areas, including: reducing phobic dysfunction (Bandura et al., 1982; Biram and Wilson, 1981); mastering high-risk skills (Brody et al., 1988; Feltz et al., 1979; Weinberg et al., 1982); enhancing personal empowerment over physical threats (Ozer and Bandura, 1990); and increasing interest in mathematical tasks (Campbell and Hackett, 1986). Research has also supported the superiority of performance-based information over other sources of confidence information (e.g., Bandura and Adams, 1977; Bandura et al., 1977; Feltz et al., 1979; Lewis, 1974; McAuley, 1985).
For example, Feltz et al. (1979) investigated the effectiveness of participant, live, and videotaped modeling on learning the back dive, a high-avoidance task. Participant modeling involved an expert's demonstration
plus guided participation with the learner. On the first four performance trials (training period), the participant-modeling subjects were guided through the dives to ensure successful performance. On the second four trials (test period), the physical guidance was removed. As predicted, the participant-modeling treatment produced more successful dives and stronger confidence beliefs than either the live modeling or videotaped modeling treatments.
According to Bandura (1986), information acquired from mastery experiences does not influence self-confidence directly; rather, it depends on how the information is cognitively appraised, such as how difficult the task is perceived to be in comparison to the effort expended, how much external aid is received, the temporal pattern of one's successes and failures, and one's conception of ability. For instance, research in motor learning has shown that in initial learning the experience of a temporal pattern of early success followed by a series of failures resulted in less persistence at the task in the face of subsequent failure than the experience of early failure followed by a series of successes (Feltz et al., 1992). The early failure and subsequent success pattern was more representative of the typical learning pattern of a motor skill and, therefore, probably influenced perceptions of the skill as an acquirable one.
In another study researchers first induced different conceptions of ability—inherent aptitude or acquirable skill—for performance on a rotary pursuit task (a spinning disc with a quarter-sized target that a person tries to track and that records time on target) (Jourden et al., 1991). 3 Subjects who performed the task under the conception of ability as an acquirable skill showed increases in self-confidence, showed positive self-reactions to their performance, displayed widespread interest in the activity, and showed greater improvements in performance in comparison with those who performed the task under the inherent-aptitude conception of ability. These results suggest that instructors should use a positive approach, which emphasizes the learnability of the skill to be taught, to improve the speed and quality of skill acquisition, especially in the early phases.
Vicarious Confidence Information Information gained through vicarious experiences has been shown to influence perceived confidence in such areas as muscular endurance performance (Feltz and Riessinger, 1990; George et al., 1992; Weinberg et al., 1979); physical activity (Corbin et al., 1984); competitive persistence (Brown and Inouye, 1978); problemsolving (Schunk, 1981; Zimmerman and Ringle, 1981); phobic behavior (Bandura et al., 1977); and management training (Gist, 1989a, 1989b; Gist et al., 1989). These techniques have included modeling and social comparison. Weinberg et al. (1979) manipulated subjects' confidence beliefs about competing on a muscular endurance task by having them observe their competitor (a confederate) on a related task. The confederate either
performed poorly and was said to have a knee injury (belief of high self-confidence) or performed well and was said to be a varsity track athlete (belief of low self-confidence). Results indicated that the higher the induced self-confidence, the greater the muscular endurance. Subjects who competed against an "injured" (perceived as relatively weaker) competitor endured longer and had higher confidence expectations about winning against their opponent than those who thought they were competing against a varsity athlete—even though the subjects lost in both trials.
Modeling provides confidence information, according to Bandura (1986), through a comparative process between the model and the observer. George et al. (1992) demonstrated that a model who was similar to nonathletic observers in ability enhanced observers' confidence beliefs and endurance performance over a dissimilar model. In essence, the similar model seems to instill the attitude of "If he/she can do it, so can I." Also, the use of multiple models has been shown to enhance the modeling effect (Lewis, 1974). Bandura (1977) reasoned that observers would have a stronger basis on which to increase their own self-confidence if they could see a number of people of widely differing characteristics succeeding at a task.
Persuasory Confidence Information For many kinds of performance, people are influenced by the opinions of others—teachers, coaches, peers, and managers—in judging their ability to perform a task. People may also try to persuade themselves that they have the ability to perform a given task through imagery and causal attributions for previous performances. Verbal persuasion by itself is of limited influence, and for treating phobias in clinical psychology it is often used in combination with other techniques, such as hypnosis, relaxation, or performance deception. However, in athletic, educational, and work situations, for which the fear component is unlikely to be as paralyzing as in chronic phobias, persuasive techniques by themselves may improve performance more successfully than in phobic behavior; but there has been little research on this possibility.
The few studies that have been conducted in motor performance report mixed results (Feltz and Riessinger, 1990; Fitzsimmons et al., 1991; Weinberg, 1985; Wilkes and Summers, 1984; Yan Lan and Gill, 1984). Weinberg (1985) found no effects on endurance performance with the use of dissociation and positive self-talk strategies, and Yan Lan and Gill (1984) found that providing subjects with bogus feedback and the suggestion that elevated arousal levels were indicative of good performance did not induce higher self-confidence. In contrast, Wilkes and Summers (1984) found persuasive techniques that tried to enhance confidence and emotional arousal influenced strength performance, but confidence-related cognitions did not seem to mediate the effect. Fitzsimmons et al. (1991) found that false positive feedback increased self-confidence judgments and future weightlifting
performance. In addition, Feltz and Riessinger (1990) found significant effects on endurance performance using mastery imagery, with corresponding effects on self-confidence.
One explanation for the equivocal findings in these studies may be the differences in the degree of persuasive influence of their techniques and the extent of their subjects' personal experience on the task. In the Weinberg (1985) study, subjects were not told that the cognitive strategy they were to use would enhance their performance. There was no attempt at persuasion. In comparison, Wilkes and Summers (1984) instructed their subjects to persuade themselves that they were confident or to persuade themselves that they were "charged up."
The degree of persuasive influence also depends on the believability of the persuasive information. Yan Lan and Gill (1984) tried to lead subjects to believe that they had the same heightened pattern of physiological arousal as good competitors. However, there was no manipulation check that the subjects believed the persuasion. Fitzsimmons et al. (1991), in contrast, used pilot data to ensure that the deceptive feedback provided was believable.
The lack of persuasive effects in some of the research may also have been due to confounding with actual performance. All of the studies used multiple performance trials; thus, subjects may have formed perceptions on the basis of their performance experience that overshadowed much of the influence that the treatment variable had on self-confidence. This explanation is supported by research showing that the significant effects for endurance performance and self-confidence were short-lived after subjects experienced performance failure (Feltz and Riessinger, 1990).
A slightly different line of research in organizational behavior has shown consistent effects for instructors' expectancies on trainees' self-confidence and performance (Eden, 1990; Eden and Ravid, 1982; Eden and Shani, 1982). These studies induced military instructors to expect higher performance from some trainees than others. Not all of these studies measured self-confidence (or self-expectancy, as used in the studies), but those that did showed that high expectancy trainees had higher levels of self-confidence and performance than low expectancy trainees.
Performance Feedback Evaluation feedback about ongoing performances has also been used as a persuasive technique (Bandura, 1986). Instructors, managers, and coaches often try to boost perceived trainees' self-confidence by providing encouraging feedback. Positive feedback about ongoing performance has been shown to instill higher perceptions of confidence than no feedback at all (Vallerand, 1983). Also, feedback on causal attribution that credits progress to underlying ability or effort has been shown to raise perceived confidence more than no feedback or feedback that implies lesser ability (Schunk, 1983a). However, inappropriately high amounts of positive
feedback can be detrimental to self-perceptions and motivation when used on individuals differentially because it implies low ability (Horn, 1985; Meyer, 1982). For instance, Horn (1985) found that the frequent use of positive reinforcement by coaches for less-skilled players resulted in lower perceived competence in those athletes, while the use of higher amounts of mistake-contingent criticism for highly-skilled players led to higher levels of perceived competence. Horn reasoned that the liberal use of praise given to low-skilled players was not performance-contingent and thus communicated to them that their coach held lower expectations for them.
In addition to its use as a persuasive technique, evaluative feedback can also add to enactive confidence information regarding ongoing performance as it conveys signs of progress. In order to be informative and motivative, feedback must be provided in reaction to defined performance standards or goals (Bandura, 1986). Otherwise, there is no basis on which to form internal comparisons to be able to evaluate ongoing performance. A wealth of research has shown that both feedback and goal setting are needed to enhance performance (Bandura and Cervone, 1983; Erez, 1977; Feltz and Riessinger, 1990; Locke and Latham, 1990; Strang et al., 1978). Even in the face of substandard performance, Bandura (1986) suggests that subjects' motivation and self-confidence may not be undermined if the discrepancy is only moderate and they are given knowledge of that discrepancy.
Causal Attributions Studies that have examined the influence of causal attributions on self-confidence beliefs have either assessed the attributions that individuals have made for previous performances in relation to the confidence expectations for future performances (McAuley, 1990, 1991) or have manipulated attributional feedback concerning previous performance to examine the effect on subsequent confidence expectations (Schunk, 1983a, 1984a; Schunk and Cox, 1986; Schunk and Gunn, 1986). Much of this research, conducted on educational learning has generally shown that attributions made or induced for previous performance that are internal and subject to personal control (e.g., effort and ability) will raise self-confidence beliefs for subsequent performance. Therefore, helping individuals attribute good performance to ability, skill improvement, or hard work and their bad performances to lack of effort, lack of sufficient practice time, or use of an inappropriate strategy can be expected to improve their self-confidence beliefs and motivation for continued performance.
Physiological Confidence Information The few studies that have investigated the influence of physiological or emotional states on self-confidence are equivocal (Feltz, 1982, 1988a; Feltz and Mugno, 1983; Juneau et al., 1986; Kavanagh and Hausfeld, 1986). For diving tasks, Feltz (1988a) found that perceived autonomic arousal, rather than actual physiological arousal, significantly predicted confidence judgments. Juneau et al. (1986) found that individuals
who focused on their physical stamina as they mastered increasing workloads on a treadmill judged their cardiac confidence as more robust than those who focused on the negative signs. For strength tasks, however, Kavanagh and Hausfeld (1986) found that induced moods (happiness or sadness), as measured by self-reports, did not alter confidence expectations in any consistent manner. Bandura (1988) has argued that it is people's perceived coping confidence that is more indicative of capability than their perception of their physiological arousal condition. If people believe that they cannot cope with a potential threat, they experience disruptive arousal, which may further lower their confidence judgments that they can perform successfully. Evidence for this argument comes from research that has shown that it is not the frightful cognitions themselves that account for anxiety symptoms, but the perceived self-confidence to control them (Kent, 1987; Kent and Gibbons, 1987).
Contextual Influences
A number of instructional practices are important contextual influences on self-confidence that do not necessarily fit into any of the four principal sources of confidence information (Schunk, 1984b). In addition to evaluative and attributional feedback, these practices include goal setting and reward contingencies. Schunk (1985) has suggested that these contextual influences convey confidence information to learners by making salient certain cues that learners use to appraise their self-confidence.
The research on goal setting and self-confidence has generally shown that setting goals for oneself and attaining them, especially specific, difficult, and proximal goals, enhance perceptions of self-confidence (Bandura and Schunk, 1981; Locke et al., 1984; Manderlink and Harackiewicz, 1984; Schunk, 1983b; Stock and Cervone, 1990). Specific goals raise confidence expectations to a greater extent than more abstract goals because they provide more explicit information with which to gauge one's progress. Difficult goals raise confidence expectations more than do easy goals because they, too, offer more information about one's capability to achieve.
Although the research supports the setting of difficult goals, experts recommend that they be realistic (Locke and Latham, 1990). Garland (1983), however, has questioned the basis of the goal attainability assumption in setting difficult goals. Laboratory experiments on goal-setting have found positive relationships between goal difficulty and performance even when the goals assigned to individuals were difficult and beyond their reach (Weinberg, 1992). One factor that may resolve the differences between experts' recommendations and laboratory evidence is task type. The type of task used in goal-setting studies has been observed to mediate this positive relationship between goal difficulty and performance (Tubbs, 1986; Wood et al., 1987). Kanfer and Ackerman (1989) have provided a theoretical explanation for
this mediating effect in terms of resource capacity and attentional demands of the task: that is, setting and striving for goals impose additional attentional demands on the individual. In learning complex tasks, such as air-traffic control operations, the benefits of goal-setting are difficult to realize because of the already high attentional demands of the task (Kanfer and Ackerman, 1989). In simple tasks, such as performing sit-ups, attentional demands are minimal, which leaves plenty of room available for engaging in the self-regulatory activity of goal-setting.
One problem in being assigned specific and difficult goals (versus selecting one's own goals) is that it may create a performance goal orientation that focuses one's attention on proving one's ability (Kanfer, 1990a:229): "The assigned performance goal sets the objective standard for proving one's ability." In a learning situation, the adoption of a difficult goal when trying to prove one's ability emphasizes the negative discrepancy and, thus, the feeling of failure, attribution to low ability, and a decrease in self-confidence about the task. Research is needed to determine whether assigning specific and difficult goals creates a performance goal orientation and whether assigning less specific goals might offset some of the negative motivational effects of assigning difficult goals, including a decreased sense of self-confidence.
In addition to specific and difficult goals, immediate goals are also easier to gauge in terms of progress than are distant goals. They make a task appear more manageable, provide an indication of progress, and affect self-evaluative reactions to performance (Stock and Cervone, 1990). A few studies have found no difference between immediate and distant goals (e.g., Bandura and Simon, 1977; Dubbert and Wilson, 1984), but many of the subjects assigned long-term goals in these studies were found to have spontaneously set short-term subgoals for themselves, which contaminated the findings. However, research on long-term goal-setting programs to improve the study skills and grades of college students suggests that relatively long-term plans and goals are most beneficial because they allow flexible choice among daily activities (Kirschenbaum, 1985; Kirschenbaum et al., 1981, 1982). One way to reconcile these divergent findings is to view them in terms of stages of skill acquisition. For instance, it may be argued that short-term goals facilitate performance and perceived competence in the early stages of skill acquisition, but as competence develops over time, moderately long-term goals allow greater flexibility and choice and may be viewed as less controlling than short-term goals (Manderlink and Harackiewicz, 1984).
In addition to examining goal-setting influences on self-confidence and performance in relation to stages of skill acquisition, examining them in relation to one's rate of progress may also explain divergent findings. Carver and Scheier (1981) propose that when one encounters difficulty in executing a higher order (more distant) goal, attention is shifted back to a lower order (more immediate) subgoal. As discrepancy toward the subgoal is
reduced, attention shifts back to the higher order goal. As long as one is making good progress toward a long-term goal, one's attention does not need to shift to subgoals to feel confident and be successful. Future research is needed to determine under what conditions and with what tasks different goal-setting techniques enhance self-confidence and performance.
Another common instructional practice to enhance motivation is the use of rewards. Providing rewards (incentives) for desirable outcomes imparts information as well as motivation (Bandura, 1986). Informing learners that they can earn rewards on the basis of what they accomplish is hypothesized to influence their self-confidence for learning. As individuals work toward a task and note their progress, their sense of confidence can be validated through rewards. Rewards have been shown to heighten self-confidence beliefs more when they are contingent on performance than when offered simply for participation (Schunk, 1983c). As with feedback, rewards may actually reduce self-confidence beliefs if they are given in a noncontingent manner for some learners and not others or if they are distributed within a competitive reward structure (Ames, 1981); competitive reward structures emphasize social comparisons that can result in differential ability attributions (Schunk, 1985).
Effects of Self-Confidence on Performance
Numerous studies have examined the relationship between self-confidence and motivated behavior or performance across a number of tasks and situations (Bandura, 1986). Although these correlational results do not necessarily demonstrate a causal relationship between self-confidence and performance, they do provide convergent evidence of a consistent association between self-confidence and performance of at least a moderate magnitude. For instance, in sport and exercise, Feltz (1988b) found that the correlations between self-confidence and subsequent performance in 28 studies ranged from .19 to .73, with a median of .54. Other studies have experimentally manipulated perceived self-confidence levels and then measured subjects' motivation in coping behavior (Bandura et al., 1982), endurance performance (Feltz and Riessinger, 1990; Weinberg et al., 1979); problem solving (Cervone and Peake, 1986), and pain tolerance (Litt, 1988). In general, these diverse causal tests provide corroborating evidence that perceived self-confidence contributes significantly to motivated behavior and performance.
Attempting to demonstrate the causal influence of self-confidence on behavior and performance through experimental manipulation of self-confidence, however, has been criticized as leading to an arbitrary interpretation of the relationship of self-confidence to performance (Biglan, 1987). Biglan points out that when environmental variables are manipulated in order to manipulate self-confidence ratings, performance behavior or other factors are also af-
fected. Environmental manipulations may influence some other variable (e.g., anxiety) that influences self-confidence and performance without any causal role for self-confidence. "Third variable" causes must be considered, but this is difficult to do in traditional experimental studies, especially when considering a network of causal relationships. In such situations, path analysis or structural-equation modeling is an appropriate method to investigate a network of causal relationships (Anderson and Evans, 1974; Cook and Campbell, 1979; Duncan, 1975). Path analysis and structural-equation modeling allow one to test whether the model presented fits a set of data adequately by comparing the observed relationships among the variables with the predicted relationships. These methods also permit an estimation of the relative indirect and direct contributions of effects. Causal modeling methods are not techniques for discovering causal directions, but, rather, for testing directions of causation that have already been specified by a model.
Causal modeling techniques have been used in a number of self-confidence studies to control for the contribution of other possible factors and to test the network of causal relationships posed by a theory (Dzewaltowski, 1989; Dzewaltowski et al., 1990; Earley and Lituchy, 1991; Feltz, 1982, 1988a; Feltz and Mugno, 1983; Garland et al., 1988; Hackett, 1985; Locke et al., 1984; McAuley, 1985, 1990; Ozer and Bandura, 1990; Schunk, 1981; Wood and Bandura, 1989; Zimmerman et al., 1992). In general, these studies have found self-confidence to be a major determinant of motivated behavior or performance and to be influenced by performance in a recursive fashion. For motor behavior and performance, existing self-confidence has been shown to predict initial performance, but as one gains experience on the task, performance also becomes a strong predictor of both future performance and self-confidence (Feltz, 1982, 1988a; Feltz and Mugno, 1983; McAuley, 1985). These results indicate that performance-based treatments may be affecting behavior through other mechanisms, as well as perceived self-confidence. One of the mechanisms not investigated in these studies on motor performance is goal effects. Path-analytic studies that have included goal effects have generally found that assigned goals influence both self-confidence and personal goals and that both variables, in turn, have direct effects on performance (Earley and Lituchy, 1991; Locke et al., 1984; Wood and Bandura, 1989; Zimmerman et al., 1992).
Although team confidence is recognized as being important to group or team functioning, there has been little research on it (Bandura, 1986). Studies have examined group confidence in social dilemmas (Kerr, 1989), school systems (Parker, 1992), and sports (Feltz et al., 1989; Spink, 1990). Two of these studies (Feltz et al., 1989; Parker, 1992) found some support for
Bandura's (1986) proposition that an aggregate of group members' perceived confidence of the group as a whole would be more predictive of the group's performance than an aggregate of the members' judgments of their own confidence when there is at least a moderate level of interdependent effort required of the group.
Because school systems require at least a moderate level of interdependence among their teachers, Parker (1992) examined teachers' beliefs in their own instructional self-confidence and their beliefs about their schools' collective capability to predict schools' levels of academic achievements. Teachers were asked to rate their self-confidence in three teaching domains (reading, mathematics, and language), as well as their beliefs in the collective confidence of the school as a whole in the same three areas. Each teacher's self-confidence and school confidence ratings were then compared with the performances of the students in each teacher's school on a standardized test of reading, mathematics, and language proficiencies. The teachers' perceived confidence in their school's capability (perceived school confidence) predicted the academic achievements of the students in their school and that these collective confidence beliefs of the school were more predictive of the academic achievement of the students than were the teachers' beliefs of their own instructional self-confidence, thus, supporting Bandura's (1986) hypothesis.
Feltz et al. (1989) compared self-confidence and team confidence in the prediction of team performance of seven collegiate hockey teams across a 32-game season. A team confidence measure was constructed after conducting a conceptual analysis of the competence areas required in hockey (with the consultation of two collegiate hockey coaches). The resulting measure of team confidence had seven dimensions: (1) winning against opponents, (2) outskating opponents, (3) outchecking opponents, (4) forcing more turnovers than opponents, (5) bouncing back from poor performances more than opponents, (6) performing better in power play situations than opponents, and (7) performing better in short-handed situations than opponents. Initial analyses have indicated that team confidence was only slightly more predictive of team performance than was individual confidence. However, when wins and losses were analyzed by game, team confidence was more affected by losses than was individual confidence.
The construct of team or collective confidence is still in a rudimentary stage in terms of understanding and explaining motivation. Clearly, a greater understanding of its utility will come from rigorous and systematic research. Toward this end, Bandura (1990) suggests that advances in research on team confidence will be greatly influenced by the development of appropriate measures; specifically, measures of perceived team confidence need to be tied closely to explicit indices of group performance. This may be best accomplished by conducting conceptual analyses of the competence areas within a group's performance.
Although Bandura's theory of self-efficacy as a self-confidence concept is not without its criticisms (see Biglan, 1987; Eastman and Marzillier, 1984; Feltz, 1988b; Lee, 1989), research on self-confidence from divergent psychosocial domains of functioning and from different cultural environments (Earley, 1993; Matsui, 1987; Matsui and Onglatco, 1991) has consistently shown self-perceptions of ability to be an important and necessary cognitive mechanism in explaining motivated behavior and performance. However, self-confidence, as a common mechanism that mediates behavior, cannot be expected to account for all behavior change in human performance (Bandura, 1984). Even so, given the demonstrated importance of self-confidence in enhancing performance, numerous inferences can be drawn to help individuals develop and maintain self-confidence to improve motivation for performance.
Techniques for Enhancing Self-Confidence
In this section research and theory from self-efficacy, goal-setting, and attributions are used to speculate on practical ways to enhance self-confidence for motivation and performance. Applications for enhancing self-confidence are organized around techniques that are based on the four sources of confidence information within Bandura's theory of self-efficacy (Bandura, 1977): performance-based strategies, modeling, persuasion and communication, and anxiety-reduction strategies.
Performance-Based Approaches
Given that the relationship between self-confidence and motivated behavior or performance has been well documented, the important goal is to find ways to enhance self-confidence beliefs. Research has supported that the strongest and most durable determinant of self-confidence is the experience of mastery or performance accomplishments.
One way of facilitating performance mastery is through instructional strategies 4 (Schunk, 1985). The instructor can provide for maximum skill development through an instructional sequence of developmental or modified activities, breaking the skill into parts, providing performance aids, physical guidance, or a combination of these methods. For example, the instructor can physically guide learners through the movements, have them practice on a simulation training device, or design a series of progressive activities to challenge their improving skills. These successes should be based on relevant and realistic progressions: progress must be in small enough increments to ensure intermediary successes, which can lead to mastery of the final goal. Performance aids and physical guidance should be gradually removed as soon as possible, however, so that learners can engage in self-directed mastery experiences. As noted, self-directed experiences indi-
cate higher levels of self-confidence to individuals than do externally guided experiences because the performance is attributed to a person's own effort and ability rather than external aids (Bandura, 1986).
A second effective means of ensuring performance accomplishments is through goal-setting—defining realistic performance standards toward which individuals strive. For complex tasks, the goals should be specific and challenging but attainable. For easy or routine tasks, the harder the goal, the better the performance. Assuming an individual has the requisite skills and commitments, working toward difficult goals can build a strong sense of confidence because the goals offer more information about the performer's capability to acquire knowledge and skills than do easier goals. Some individuals, however, may need some persuasive help to be convinced that the goals are not too difficult (Schunk, 1983b). In addition, for complex and difficult tasks, short-term goals should be used along with long-term goals. Similarly, when using short-term goals, the performer's perceptions of self-confidence for attainment of future goals should be monitored, as well as perceptions of self-confidence that result from goal attainment. As Stock and Cervone (1990) point out, goal-setting strategies will not help individuals who lack a sense of efficacy for attaining the subgoals or those who do not experience enhanced feelings of confidence when they attain the subgoals.
Feedback also appears necessary for goals to have maximum effectiveness in enhancing self-confidence and improving performance. Furthermore, when one is first learning complex tasks, self-confidence beliefs and success can be enhanced by emphasizing process-related (or learning) goals over outcome-related (or performance) goals. Rather than defining success through outcome measures, such as winning and losing or number of tasks completed, success should be redefined to include process variables, such as effort, form, and strategy. These process-related goals are important because they help individuals focus on the learnability of a skill rather than viewing the skill as requiring inherent aptitude (Jourden et al., 1991).
Modeling Others
When individuals have had no prior experience with a task, observing others (modeling) is one means of providing information by which to judge one's own capabilities. For instance, observing others engaging in threatening activities without adverse consequences can reduce inhibitions in observers (Lewis, 1974). The models can be similar in terms of personal characteristics (e.g., age, sex, race) and skill levels, but similarity in skills appears to be more salient to observers than personal characteristics (George et al., 1992). The content of the model's statements is also an influential factor in raising perceptions of efficacy (Gould and Weiss, 1981; Schunk,
1981). Models can provide information and strategies about how to perform the task as well as confidence statements.
The use of multiple demonstrators and coping models has also been shown to influence the effectiveness of demonstrations (Bandura et al., 1982; Lewis, 1974). Bandura (1986) has reasoned that the more different types of people observers see succeeding at a skill, the stronger the convictions will be that they, too, can succeed. Coping models, who initially exhibit difficulty on the task in the same way as learners do but gradually overcome those difficulties, provide the learners with information that this task can be accomplished through perseverance.
The U.S. Olympic Training Center has used observational techniques in a slightly different manner in an attempt to increase an athlete's confidence expectations and performance. In this self-modeling technique, videotapes of an athlete's performance is altered to eliminate the mistakes and then replayed a number of times for the athlete in hopes of altering the athlete's performance beliefs. Research has not yet been provided to determine the effectiveness of this technique with athletes; however, it has been shown to be effective with persons exhibiting deficient speaking skills by editing out the mistakes, hesitancies, and external aids from the videotapes and playing them back to the speakers (Dowrick, 1983).
Persuasion and Positive Communication
Although persuasion and communication techniques alone may be of limited value in enhancing self-confidence beliefs, they may be effective when used in conjunction with performance-based techniques and are provided in a manner contingent to performance. Because it is difficult to evaluate one's own progress in many activities, credible and expert observers can help stretch one's confidence beliefs through effective persuasion techniques. Persuasive information is probably most important during early stages of skill acquisition, when learners lack task experience and knowledge of their capabilities.
As discussed above, to be effective the persuasive information must be believable and, therefore, should be only slightly beyond what the learners can do at that time. For instance, if one is using imagery to try to help convince individuals that they can endure more muscular fatigue, manage potential threats safely, achieve greater athletic feats, or return to performance from injury, the imagery should be structured so that the individuals imagine themselves performing just slightly better than what they think they can do. As with setting goals, the imagery should be challenging but attainable. Mastery experiences should then be arranged to facilitate effective performance.
For individuals who are experienced at a task but are in a performance
slump or plateau, false performance feedback (performance deception) has been used successfully to improve performance (Fitzsimmons et al., 1991). As with the other persuasion techniques, it is important that the deception is believable. For instance, if a coach is trying to improve an athlete's maximum press in weight lifting by persuading him to think he is lifting less weight than he is actually pressing, the difference between the two should be small. Instructors should also be aware that continually deceiving one's students may undermine the trust they need to have in order to attempt new skills.
A second category of persuasion techniques involves effective communication from instructor to learner. These strategies include performance feedback, rewards, causal attribution feedback, and positive communication. Performance feedback can provide clear information that learners are making progress toward their goals. As noted above, however, feedback must be given contingently in relation to defined performance standards or goals, and it must be given consistently to all learners so as not to create expectancy effects. If a wide discrepancy continues between performance and goals, short-term subgoals should be constructed to reduce the discrepancy.
Different types of performance feedback should be used, depending on a learner's phase of skill acquisition: progress feedback provides information on an individual's progress without regard to others; normative feedback compares an individual's progress in relation to others. Progress feedback should be used during the early phase of skill acquisition or with persons who are likely to perform more poorly in comparison with others because normative feedback can debilitate learning if used before an individual has developed a resilient sense of self-confidence for the task (Kanfer, 1990b). Normative feedback can be used during later phases of skill acquisition.
As with performance feedback, if rewards are used they must be clearly tied to performance progress in order to influence self-confidence (Schunk, 1983c, 1984a). The combination of performance-contingent rewards with short-term goals appears to enhance self-confidence beliefs better than either technique alone (Schunk, 1984a).
Attributional feedback and positive communication are especially important techniques when mistakes and setbacks occur. Because mistakes and failures are inevitable, the way in which an instructor communicates and interacts with a learner will have an important influence on the learner's self-confidence. Telling learners that their past failures were due to insufficient effort, rather than lack of ability, can help them meet their setbacks with renewed vigor and persistence because lack of effort can be rectified. But encouraging learners to emphasize external factors (e.g., bad luck or task difficulty) as the reason for a setback (as some athletic coaches do) could be a serious mistake if the mistake and attribution occur repeatedly, because the learners may start to perceive that the outcome is out of their control and not take responsibility for their performance.
of the task and a learner's actual efforts have to be taken into account. If an instructor tells a learner that her failure on a difficult task, for which she expended a lot of effort, was due to lack of effort, she is apt to interpret the feedback as lack of ability or start to distrust the instructor's feedback. In situations in which learners are expending great effort at difficult tasks and still not succeeding, the instructor needs to help them acknowledge the difficulty of the task and set up modified challenges that can be accomplished.
Positive communication by an instructor has been shown to be very helpful in reducing the negative affect that occurs in failure situations (Smith et al., 1979). Positive communication is performance contingent, but it focuses on positive aspects of performance while acknowledging mistakes, provides instructional feedback, and emphasizes the learning nature of task acquisition (Eden, 1990; Jourden et al., 1991). Most individuals feel discouraged and ashamed when they do not perform well and need the assurance and encouragement of the instructor in regard to their abilities. In response to a learner's mistakes, the instructor should not focus on the error itself, but instead find something positive and constructive to say about improving the performance. Four steps characterize this positive approach to mistakes. First, the learner's distress about the mistake is acknowledged. Second, the learner is complimented by the instructor's finding something about the performance that was correct. The compliment must be about an important and relevant aspect of the task; otherwise, it is likely to be discounted by the learners. Third, the instructor provides instructions on how the learner can improve the mistake. Fourth, the instructor ends with a positive note by encouraging the learner to keep trying. These four steps ''sandwich" skill instructions between words of encouragement and praise. A positive communication style allays feelings of embarrassment and promotes a sense of self-confidence.
Anxiety Reduction
Some individuals may interpret increases in their physiological arousal as a fear that they cannot perform a skill successfully. Thus, it is believed that if the arousal of these individuals can be reduced through such techniques as relaxation and biofeedback, fears will decrease and self-confidence will increase. However, as Bandura (1988) argued, it is one's perceived coping confidence that plays a central role in controlling fear arousal: people with low perceived coping confidence tend to focus on the danger and fear cues; those with high levels of coping confidence concentrate on the task at hand (Keinan, 1988).
Helping individuals believe that they can exercise control over potential threats and frightful cognitions is the way to decrease fears and increase
self-confidence. One way to help improve coping confidence is to teach individuals coping strategies to use to manage threatening situations, such as positive self-talk. Research has shown that positive self-talk can help individuals manage stressful situations if they believe that the technique will help them cope (Girodo and Wood, 1979). According to Bandura (1986), the persuasion that the technique will help the individual cope more effectively is what instills a sense of personal control, which enhances coping confidence.
Another technique that instructors can use to help improve coping confidence is to try to manipulate the environment to reduce the uncertainties of the situation. For example, sources of uncertainty might include how dangerous the situation is, how well one expects to perform, whether one will be asked to perform, or what one's coworkers, colleagues, or teammates will think. Uncertainty can be reduced by providing information of task requirements, providing assurance to the learner (or performer), and emphasizing realistic, short-term goals that take the attention away from long-range outcomes. Simulation training can also help to reduce uncertainties about stressors. However, simulation training that involves exposure to serious physical threats reduces anxiety only when it is perceived as successful (Keinan, 1988). Individuals who have low coping self-confidence might require some preparatory coping interventions before they are exposed to simulation training that is physically dangerous or threatening.
Self-confidence is a potent predictor of an individual's performance, given the appropriate skills and adequate incentives. The role of an instructor, manager, or coach, therefore, is to develop and sustain a learner's high level of self-confidence by ensuring performance success, using modeling and persuasion techniques, communicating effectively, and reducing anxiety-producing factors. These techniques can be used in combination with each other in various ways, depending on the task and the learner, to enhance self-confidence.
Many of these techniques can also be applied to enhance team confidence. For instance, if a team is having some difficulty achieving a task or solving a problem, the instructor or leader can design a series of progressive activities for the team and help them set short-term team goals that emphasize process variables (e.g., strategy) rather than outcome variables. Teams can also observe other, similar teams that persevere in the face of adversity or that demonstrate successful strategies about how to perform the group task. Self-modeling techniques, in which mistakes are edited out of a performance, can also be used to enhance confidence, although no research to date has explored the effectiveness of this technique with teams.
The communication techniques described can be used with teams as well as individuals. Team confidence can be expected to be enhanced when contingent performance feedback and rewards are provided to the team and
when the feedback is positively focused and the causal attribution is appropriate to the difficulty of the task and the team's effort expenditure.
Lastly, as with individual coping confidence in threatening situations, team coping confidence can be enhanced and anxiety reduced by reducing the uncertainties that a team faces. Techniques for reducing uncertainties for teams also include simulation training, observing other teams performing the task, and providing as much information regarding the task as possible.
Four major categories of techniques have been described to enhance self- and team confidence. Evidence for the use of these techniques has come from an extensive and diverse research literature, but there are still a number of areas of research that are needed to better understand self-confidence and to enhance performance.
FUTURE RESEARCH DIRECTIONS
Most of the research and applications on self-confidence have been concerned with the influence of unidimensional confidence information on individual performance. Other areas that deserve attention are how people process multidimensional confidence information; the study of self-confidence over time and in different situations; the relationships among self-confidence, goals and goal orientations; individual differences in self-confidence; and team confidence.
Scant research has been conducted on how people process multidimensional confidence information and the heuristics they use in weighting and integrating these sources of information in forming their confidence judgments (Bandura, 1986). The importance of different types of information may vary across different types of activities and situations. For instance, in some sport and exercise situations, physiological information may be a more pertinent source of confidence information than previous performance. In addition, people may weight sources of information differently in different phases of skill acquisition. In processing multidimensional information, people may also misjudge or ignore relevant information in trying to integrate different information (Bandura, 1986). Results from research on these questions will help to understand how self-confidence expectations gain their predictive power; it will also have implications for the type and amount of confidence information provided to individuals for particular types of activities and situations.
Other motivational variables, such as goal orientations and conceptions of ability as they relate to goal setting and self-confidence, have received little attention in research except for Kanfer (1990a), who has noted that different goal orientations may be called for at different phases of skill acquisition. Research is needed to examine induced differential goal orientations in relation to goal-setting and self-confidence at different phases of skill acquisition and for different kinds of tasks (e.g., complex, physically
threatening, mundane). Studying confidence judgments across extended periods of performance and across situations or tasks may be the most informative paradigm for testing the relative contribution of self- or team confidence and other cognitions to performance over time, as well as for testing changes in sources of confidence information.
Besides goal orientation and conceptions of ability, other individual difference variables—such as gender, gender role orientations, and self-focus (see Carver and Scheier, 1981) or action control (Kuhl, 1984)—may play a role in determining self-confidence. For instance, research has generally shown that males view themselves as more confident than females in achievement activities that have been stereotypically linked with males (Campbell and Hackett, 1986; Fennema and Sherman, 1978; Lirgg, 1991). Further research is needed to explore the extent to which individual differences mediate the relationship between confidence judgments and performance.
The resiliency of confidence beliefs may also be an important factor in the relationships between self- or team confidence and performance. Bandura (1986, 1990) has suggested that self-confidence must be resilient in order for one to persist and sustain effort in the face of failure. Ericsson et al. (1993) also allude to this in their discussion of the role of deliberate practice in the acquisition of expert performance. According to Bandura, experience with failures and setbacks is needed to develop this robust sense of self-confidence. Future research might examine how different patterns of success and failure influence the development of a robust sense of confidence. In addition, Bandura (1990) notes that when self-doubt sets in after failure, some individuals recover from their perceived low confidence more quickly than others. Similarly, some teams may be able to regain their sense of confidence after a setback more quickly than other teams. Knowing how and why some individuals and teams are able to regain their sense of confidence more quickly than others would be a valuable source of information for designing interventions that would help confidence recovery. Furthermore, although according to Bandura (1986, 1989), an optimistic sense of self-confidence is advantageous to continued effort and persistence, substantial overestimates of one's competence provide a dangerous basis for action (Baumeister, 1989). Research is needed to determine the optimal distortion necessary to foster the persistence needed for mastering various tasks.
In the area of team confidence, a number of other issues are in need of further investigation, such as sources of team confidence information, the relationship of team confidence to group attributions and other group motivation concepts, and the influence of team leaders on team confidence. Although Bandura (1986) postulated that teams are influenced by the same sources of confidence information as individuals, there may be other sources that are unique to a team. Perhaps social, community, or political support provides important team confidence information. For sports teams, the
media may provide a source of team confidence information (although this may also be the case for individual athletes).
Research has also yet to examine the relationship between team confidence and other conceptual and theoretical perspectives of group motivation. For example, relationships between team confidence and team attributions, desire for team success, and social loafing have yet to be studied. Only one study has examined team confidence and team cohesion (Spink, 1990).
Lastly, the influence of team leaders may also provide some insight on team confidence and performance. Bandura (1990) has suggested that a performance slump, especially by a key member of the team or the team leader, could influence the confidence that other members have in the team's ability to be successful.
Similarly, managers' and team leaders' leadership confidence may affect team confidence and performance. Wood and Bandura (1989) found evidence that perceived managerial self-confidence both directly and indirectly influenced organizational performance by the effect it had on people's goal setting and use of analytic strategies. Other research has shown that a high sense of personal confidence enhances strategic thinking and facilitates organizational performance under varying levels of organizational complexity and goal assignments (Wood et al., 1990). It could be argued, therefore, that the confidence a team has in a key member or in its leader may also have an important effect on team effectiveness. In addition to the confidence a team has in its leader, the confidence that a leader has in his or her team may also affect team performance. Some support has been found for this argument (Chase et al., 1993), but further research is required to link antecedents and consequences of such confidence beliefs.
In addition to leadership confidence, different kinds of leaders' behaviors may also influence individual and team confidence for certain tasks and certain team members. Research on leadership behavior has suggested a path-goal theory of leadership: this theory argues that the central function of a leader is to create positive performance expectancies (or self-confidence beliefs) among team members (subordinates) (Evans, 1974; Fulk and Wendler, 1982; House and Mitchell, 1974). Certain leader behaviors (supportive, directive, participative, and achievement oriented) are hypothesized to differentially influence the self-confidence and effort-performance expectancies among team members, depending on the task and its characteristics. For instance, supportive leadership behavior (e.g., concern for welfare of team members) should lead to increased self-confidence among team members for tasks that are stressful, boring, tedious, or dangerous, but not for tasks that are interesting and enjoyable and for which team members are confident in their ability to complete the task. Leadership behaviors that are directive (e.g., giving specific guidance, close supervision), participative (e.g., consulting with team members), and achievement oriented (e.g.,
setting challenging goals) should increase self-confidence when the task is unstructured and complex, but not when the task is simple, repetitive, or highly structured. Although Yukl (1989) suggests that the theory has yet to be adequately tested, it can provide a framework in which to investigate possible moderating variables of leadership influences on both self-confidence and team confidence.
1 The large number of citations in this chapter to Bandura's work reflects the fact that most of the research on self-efficacy has been done in his laboratory. One advantage of relying on the research of one team of investigators is that the work displays an analytical progression as later studies build on the results obtained from earlier work. Another advantage of Bandura's work is that the approach identifies sources of confidence information that provide a basis for practical ways of enhancing performance, as discussed below. A disadvantage is that this work is based largely on a particular theoretical perspective, which may not be the only framework for studying the relationship between self-confidence and performance.
2 Autonomic arousal is the physiological arousal that is under the control of the autonomic nervous system (e.g., changes in heart rate, respiration rate, adrenaline in the blood).
3 Although the subjects in the "inherent aptitude" condition were deceived, they were fully debriefed, told of the difficult nature of the task and assured that it did not indicate "aptitudes."
4 In clinical psychology, these strategies are referred to as participant modeling or performance desensitization.
Can such techniques as sleep learning and hypnosis improve performance? Do we sometimes confuse familiarity with mastery? Can we learn without making mistakes? These questions apply in the classroom, in the military, and on the assembly line.
Learning, Remembering, Believing addresses these and other key issues in learning and performance. The volume presents leading-edge theories and findings from a wide range of research settings: from pilots learning to fly to children learning about physics by throwing beanbags. Common folklore is explored, and promising research directions are identified. The authors also continue themes from their first two volumes: Enhancing Human Performance (1988) and In the Mind's Eye (1991).
The result is a thorough and readable review of:
- Learning and remembering. The volume evaluates the effects of subjective experience on learning—why we often overestimate what we know, why we may not need a close match between training settings and real-world tasks, and why we experience such phenomena as illusory remembering and unconscious plagiarism.
- Learning and performing in teams. The authors discuss cooperative learning in different age groups and contexts. Current views on team performance are presented, including how team-learning processes can be improved and whether team-building interventions are effective.
- Mental and emotional states. This is a critical review of the evidence that learning is affected by state of mind. Topics include hypnosis, meditation, sleep learning, restricted environmental stimulation, and self-confidence and the self-efficacy theory of learning.
- New directions. The volume looks at two new ideas for improving performance: emotions induced by another person—socially induced affect—and strategies for controlling one's thoughts. The committee also considers factors inherent in organizations—workplaces, educational facilities, and the military—that affect whether and how they implement training programs.
Learning, Remembering, Believing offers an understanding of human learning that will be useful to training specialists, psychologists, educators, managers, and individuals interested in all dimensions of human performance.
READ FREE ONLINE
Welcome to OpenBook!
You're looking at OpenBook, NAP.edu's online reading room since 1999. Based on feedback from you, our users, we've made some improvements that make it easier than ever to read thousands of publications on our website.
Do you want to take a quick tour of the OpenBook's features?
Show this book's table of contents , where you can jump to any chapter by name.
...or use these buttons to go back to the previous chapter or skip to the next one.
Jump up to the previous page or down to the next one. Also, you can type in a page number and press Enter to go directly to that page in the book.
Switch between the Original Pages , where you can read the report as it appeared in print, and Text Pages for the web version, where you can highlight and search the text.
To search the entire text of this book, type in your search term here and press Enter .
Share a link to this book page on your preferred social network or via email.
View our suggested citation for this chapter.
Ready to take your reading offline? Click here to buy this book in print or download it as a free PDF, if available.
Get Email Updates
Do you enjoy reading reports from the Academies online for free ? Sign up for email notifications and we'll let you know about new publications in your areas of interest when they're released.
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
Preview improvements coming to the PMC website in October 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- Int J Environ Res Public Health

Revisiting the Self-Confidence and Sport Performance Relationship: A Systematic Review with Meta-Analysis
Marc lochbaum.
1 Education Academy, Vytautas Magnus University, 44248 Kaunas, Lithuania
2 Department of Kinesiology and Sport Management, Texas Tech University, Lubbock, TX 79409, USA; [email protected]
Mackenzie Sherburn
Cassandra sisneros.
3 Honors College, Texas Tech University, Lubbock, TX 79409, USA; [email protected] (C.S.); ude.utt@ocyendys (S.C.)
Sydney Cooper
Andrew m. lane.
4 Faculty of Education, Health and Well-Being, University of Wolverhampton, Walsall WV1 1LY, UK; [email protected]
Peter C. Terry
5 Division of Research & Innovation, University of Southern Queensland, Toowoomba, QLD 4350, Australia; [email protected]
Associated Data
All data are contained in the article tables.
Self-confidence is a common research topic, and most applied textbooks include interventions designed to enhance athlete confidence. Our purpose was to quantify the self-confidence and sport performance literature using meta-analytic techniques. We also examined potential risk of bias indicators, and the moderation effects of study quality, sport characteristics, timing of confidence measurement, and individual differences among participants. Following a review of two past meta-analyses, a systematic search of APA PsycArticles, ERIC, Psychology and Behavioral Sciences Collection, PsychINFO, and SPORTDiscus within the EBSCOhost platform, and some hand searching, 41 articles published between 1986 and 2020 met the inclusion criteria. Collectively, the included studies investigated 3711 athletes from 15 countries across 24 sports. The overall random effects estimate of the relationship (expressed as r ) between self-confidence and performance was 0.25 (95% CI 0.19, 0.30), with little evidence of publication bias. The summed total risk of the individual study bias score did not moderate the confidence–performance relationship, whereas significant moderator effects emerged for individual sports (0.29) compared with team sports (0.14), objective (0.29) compared to subjective (0.14) performance measures, and 100% male (0.35) compared to 100% female (0.07) samples. In conclusion, the confidence–performance relationship is small in magnitude, nearly free of bias, and moderated by sport type, performance objectivity, and athlete sex.
1. Introduction
Strategies to enhance self-confidence are common sport psychology interventions for athletes [ 1 , 2 ] but evidence of the relationship between self-confidence and athletic performance is equivocal. Several studies have reported significant benefits of self-confidence for athletes [ 3 , 4 , 5 , 6 ], whereas other investigations have shown no benefit [ 7 , 8 , 9 , 10 ]. The most recent quantitative summaries of the self-confidence in sport literature were published nearly 20 years ago in the form of two meta-analyses [ 11 , 12 ]. Since then, many studies are new to the literature, suggesting that an updated meta-analysis is timely.
Self-confidence has intuitive appeal as a contributor to successful sport performance and therefore sport psychology researchers [ 11 , 12 ] have frequently investigated the confidence–performance relationship. Several related but distinct terms have been used in this area of the literature, including self-confidence, self-efficacy, sport confidence, or simply, confidence. For the purposes of this review, self-confidence is defined as “the perceived ability to accomplish a certain level of performance” [ 13 ] (p. 279), whereas self-efficacy is more situationally specific, and defined in sport as “a performer’s belief that he or she can execute a behavior required to produce a certain outcome successfully” [ 14 ] (p. 314). We delimited our review to studies that have explicitly evaluated the relationship between state self-confidence and sport performance, that is, used the term confidence rather than efficacy and as such excludes data sets related to self-efficacy and sport performance. We acknowledge that it is possible that researchers used the term confidence when assessing efficacy and vice versa. We use the terms sport confidence and confidence as synonyms for self-confidence as reported by athletes.
Self-confidence is both a personality trait (i.e., “a relatively stable predisposition” [ 14 ] (p. 368)) and a psychological state (i.e., “a transitory emotional condition” [ 14 ] (p. 339)). This means that some athletes, by nature, will tend to be more confident than others. However, even the most naturally confident athlete may experience low self-confidence in specific circumstances (e.g., following an unexpected defeat) or unfamiliar territory (e.g., the football quarterback on the 10 m diving board). Our review is specific to studies that evaluated the relationship between state self-confidence and sport performance and excludes investigations of trait self-confidence traits.
Previous efforts to summarize the evidence base for the benefits of self-confidence on athletic performance have included two published meta-analyses [ 11 , 12 ]. Woodman and Hardy [ 12 ] summarized 47 studies in their meta-analysis, 40 of which (85.1%) had used the Competitive State Anxiety Inventory-2 (CSAI-2) [ 15 ] to assess self-confidence. The mean effect size reported for the relationship between self-confidence and performance ( r = 0.24, p < 0.001) represents a small positive effect [ 16 ], accounting for 5.8% of shared variance. The confidence–performance relationship was moderated by participant sex (male > female), standard of competition (high standard > low standard), and measurement scale (CSAI-2 < other measures). Craft et al. [ 11 ] limited their meta-analysis to studies using the CSAI-2 to assess self-confidence, identifying 29 studies that met their inclusion criteria. They reported an identical relationship with performance ( r = 0.24, p < 0.001) to Woodman and Hardy [ 12 ], which was moderated by type of sport (individual > team), type of skill (open > closed), level of athlete (higher ability > lower ability), and time of CSAI-2 administration (31–59 min. pre-competition > other periods).
Meta-analyses related to self-confidence in domains other than sport have shown similar results. For example, a meta-analytic review of 114 studies investigating the relationship between self-efficacy and work-related performance [ 17 ] reported a weighted mean correlation of 0.38, with task complexity (low > medium > high) and study setting (laboratory > field) moderating the relationship. Further, research has demonstrated that self-efficacy is one of the strongest correlates of academic performance [ 18 , 19 ].
There are compelling reasons to hypothesize that characteristics of the sport in question and the athletes involved moderate the relationship between self-confidence and sport performance. In 1995, Terry [ 20 ] identified a range of factors that he proposed would moderate the relationship between mood states and sport performance, and indicated that the same moderation effects would apply to other psychological states, including self-confidence. For example, he proposed that the relationship would be stronger in individual sports than team sports because individual sports remove the influence of team dynamics. A test of this hypothesis among 100 tennis players in singles and doubles competition showed the confidence–performance relationship to be of moderate strength in singles and close to zero in doubles [ 21 ]. Further exploration of the confidence–performance relationship in team sports compared to individual sports will form part of our review.
A related proposition [ 20 ] refers to the nature of the skills involved in the sport performance. The confidence–performance relationship would tend to be stronger in sports that involve primarily closed skills (i.e., skills performed in a predictable, unchanging environment, such as archery [ 22 ]) than in sports that involve primarily open skills (i.e., skills performed in a dynamic, rapidly changing environment, such as soccer [ 22 ]) because the direct influence of opponents is removed. However, of note, Craft et al. reported the opposite, that the confidence–performance relationship was stronger in open-skill sports than closed-skill sports [ 11 ]. Further, given the potential for self-confidence to increase or decrease after performance is underway, Terry [ 20 ] proposed that the confidence–performance relationship should be stronger in sports of shorter duration, in which performance outcome is determined closer in time to the pre-performance assessment of self-confidence.
Another proposition relates to whether the sport performance in question is self-referenced (e.g., running a personal record time) or other-referenced (e.g., finish position). Terry [ 20 ] proposed that the confidence–performance relationship would be stronger when performance is self-referenced than when it is other-referenced. For example, running a sub-3 h marathon is an exceptional performance for an average runner even though they would have placed outside the top-1500 finishers in the 2019 New York City Marathon [ 23 ], whereas an elite runner posting a time of 2 h 30 min would have underperformed, despite finishing inside the top-70 runners in the same race. This principle extended, involves comparison of the confidence–performance relationship according to whether the performance measure is objective (e.g., win–loss, time to complete) or subjective (e.g., self-rated, coach-rated). Objective measures tend to be more precise indicators of performance than subjective measures, and therefore we expect to show a stronger relationship with self-confidence. Conversely, subjective ratings may be more sensitive to individual variations in performance. On balance, although both objective and subjective performance measures can be self-referenced (e.g., personal record time, self-rating of performance) or other-referenced (e.g., finish position, coach rating of performance), we anticipate that objective performance measures would show the stronger relationship with self-confidence.
The next proposed moderator of the confidence–performance relationship is the relative skill level of the athletes involved [ 20 ]. For example, tennis legend Raphael Nadal will beat any club-level player in the world regardless of confidence level simply because his skill level is so much higher. Psychological factors, including self-confidence, tend to play a more important role in determining performance outcome among athletes who are homogeneous rather than heterogeneous in terms of skill and fitness. This is more likely to occur at the higher echelons of sport where athletes win or lose medals by tiny margins. Previous meta-analyses have reported a moderating effect of athlete level of competition, with stronger confidence–performance relationships found among higher-level athletes [ 11 , 12 ].
Finally, athlete sex may moderate the confidence–performance relationship, given the tendency for male athletes to report higher self-confidence than female athletes [ 24 ]. Woodman and Hardy [ 12 ] reported a stronger confidence–performance relationship for male athletes whereas Craft et al. [ 11 ] did not test the moderating effect of athlete sex. We will explore the veracity of the above propositions in our review, as far as the reported characteristics of the primary studies allow.
Research Questions
Given the continued interest in sport confidence, we aimed to update and extend the work of Craft et al. [ 11 ] and Woodman and Hardy [ 12 ] by aligning our inclusion criteria and pre-planned analyses to answer the following replication and extension research questions.
- Q1: What is the overall relationship between a measure of state self-confidence and sport performance? Moreover, does the risk of individual study bias or across study bias (i.e., publication bias) moderate this relationship?
- Q2: Do Terry’s [ 20 ] sport propositions moderate the confidence–performance relationship?
- Q3: Does the objectivity and reference of the performance measure moderate the confidence–performance relationship?
- Q4: Does the time of the self-confidence measure prior to performance moderate the confidence–performance relationship?
- Q5: Do selected individual difference variables, namely sex and athlete sport level, moderate the confidence–performance relationship?
2. Materials and Methods
This systematic review with meta-analyses reported followed Page et al.’s [ 25 ] Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) publication. Although we did not register our review protocol with the PROSPERO database, we did search the database before and after conducting our systematic review to check that we were not duplicating a recent study.
2.1. Eligibility Criteria and Selection Process
Included studies, in any printed language, met the following criteria: (a) use of a state self-confidence measure; (b) measure of sport performance; (b) self-confidence assessed before sport performance; (c) data provided, group differences (e.g., winners, losers) or relational (e.g., correlation between self-confidence and performance) for effect size calculation; and (d) original data published in peer-reviewed scholarly journals by 1 December 2021. We did not consider participants in a non-athletic setting, such as Gould and colleagues’ [ 26 ] police academy participants. We discriminated self-confidence from self-efficacy by the questionnaire used and thus the language used to describe the construct. For sport performance, we excluded physical performance measures associated with athletic performance, such as vertical jump height, but included measures of performance skills (e.g., tennis serving percentage). All authors reviewed articles considering our inclusion criteria. We did not inquire about missing data or clarifications. We imposed no language restriction. Articles found in our search resulted from the search terms found in either the title, keywords, or abstract. If an article itself was not in English ( n = 2), then all pertinent non-English articles sections were copy and pasted into Google Translate ( https://translate.google.com/ , accessed on 1 March 2021).
2.2. Information Sources, Search Strategy, and Search Protocol
The systematic search included references from the two published state confidence and performance meta-analyses [ 11 , 12 ] and databases found within EBSCOhost (search ended 1 December 2021). The specific databases were APA PsycArticles, ERIC, Psychology and Behavioral Sciences Collection, PsychINFO, and SPORTDiscus. The search terms were combinations of sport performance with confidence, competitive, CSAI-2, TSCI, state confidence, and sport confidence measures. Our Supplemental file contains the record of our complete protocol. When reading the Supplemental file , the term ‘Box’ refers to the EBSCO interface, whereby one types search terms in the advanced search setting. The following is an example of our search protocol:
- APA PsycArticles, APA PsychINFO
- ERIC, Psychology and Behavioral Sciences Collection, SPORTDiscus
- Typed key terms
- CSAI-2 typed in Box 1 in the EBSCO interface
- Sport performance typed in Box 2 in the EBSCO interface
- Competitive typed in Box 3 in the EBSCO interface
- Limit to scholarly peer-reviewed journals
- Page options: 50
- Limit time: 2002–2020 [computer changed to 2003]
2.3. Study Selection
We checked the title, abstract, and keywords of all articles identified in our search procedure for mention of the term confidence, but not confidence interval(s). Articles mentioning confidence went forward for full-text assessment. If there was any doubt about whether a study included confidence as a measured variable despite having no mention of it in the title, abstract, and keywords, we retained the study for full-text screening. ML, MS, and CS assessed studies for eligibility, independently and then collectively. AL and PT then independently verified that all included studies met the inclusion criteria and identified two additional eligible studies. Figure 1 depicts our search process via a PRISMA 2020 flow diagram template ( http://prisma-statement.org/prismastatement/flowdiagram.aspx , accessed on 1 March 2021).

PRISMA flow chart for the identification of the included studies.
2.4. Data Collection and Items Retrieved
ML and MS planned the extraction of data. After examining the two past meta-analyses [ 11 , 12 ], they examined Beedie et al. [ 27 ] and Lochbaum et al. [ 28 ], given that the methodologies of mood states measured before sport performance is akin to confidence measured before sport performance. ML and MS, independent of each other, began the data extraction. Next, all remaining authors received data collection training. ML worked with each to finalize the retrieval process. The data items retrieved were as follows: sample age, country, number, percent male, and sport; confidence (name of scale) and performance specifics (objective or subjective, other- or self-referenced); and the sport type (individual or team), duration (less than or greater than 10 min in duration), and skill (closed or open).
2.5. Risk of Bias in Individual Studies
We used Hoy and colleagues’ [ 29 ] risk of bias tool to rate risk of individual study bias. At the outset, ML, CS, MS, and SC worked on the coding for the potential of individual study risk of bias in groups. Next, AL, PT, and ML worked to consensus on each risk category. We coded all studies (see Table 1 ) on the following nine risks of bias: (1) target population is a close representation of the national population in relation to relevant variables; (2) some form of random selection was used to select the sample; (3) likelihood of nonresponse bias is minimal; (4) data were collected directly from the participants; (5) confidence measure has validity and reliability; (6) performance measure is valid and relevant to sport; (7) same mode of data collection was used for all participants; (8) assurance of participant anonymity is stated in methods; (9) assessment period for the parameter of interest is appropriate. We assigned point values to each of the three ratings (high, medium, and low), and computed a study quality score (range 9 to 27 points), where higher scores equals lower risk.
Risk of individual study bias questions and rating explanations.
| Rating Explanations | |||
|---|---|---|---|
| Bias | Low Risk (3 Points) | Medium Risk (2 Points) | High Risk (1 Point) |
| Sample | Sample is a group of athletes, in the sport; performance is score, outcome of that sport. | Sample is like the high category, but sport outcome is like the low category or vice versa. | Sample includes recreational athletes, but not in a realistic sport context, and/or performance is based on assessment of a skill rather than a game statistic or sport outcome. |
| Random selection | Stated random selection occurred from a much larger group (e.g., from all athletes at an event). | Random selection occurred within a group of athletes (e.g., college team at an event). | No random selection of any kind stated. |
| Nonresponse | Appears most participants completed the measures. | Some non response occurred. | Seems most did not do it, e.g., a big race, subjects recruited at the race, most likely most did not do it. |
| Direct collection | Yes, all in person. | A mix of online and in person. | All online or mail. |
| Confidence measure | Study level reliability presented. | Valid and reliable measure (e.g., all except the 1-item measure) but study level reliability not presented. | Made up confidence measure. |
| Sport measure | Event time, win–loss, outcome, golf score, judge rated (gymnastics). | Participant statistics. | Self or other rated subjective, or vague (good vs. bad performers), team selection. |
| Data collection | Yes, all the same. | No option for a medium rating. | A mix of ways (e.g., individual for some, in large groups of others). |
| Anonymity | Yes, stated. | Participants presented informed consent. | Not stated in methodology. |
| Time | ≤15 min | 16–60 min | >1 h |
2.6. Summary Measures and Planned Methods of Analysis
We chose the correlation coefficient ( r ) as the primary effect size parameter. We followed Cohen’s [ 30 ] interpretation for correlation values of 0.10–0.29 as small, 0.30–0.49 as medium, and 0.50 or greater as large. We assumed heterogeneity of effects. Thus, we planned both random- and mixed-effects analyses. We based our expectancy of heterogeneity on a recent systematic review of meta-analyses in sport psychology with performance as an outcome [ 31 ]. For the test of the state self-confidence and performance relationship, we used a random-effects model. We reported the number of cases, sample size, r , 95% confidence intervals, heterogeneity, and publication bias statistics. We looked at heterogeneity measured as inconsistency and reported the I 2 statistic or the ratio of excess dispersion to total dispersion. Higgins et al. [ 32 ] state that I 2 is the overlap of confidence, explaining the total variance attributed to the covariates. To help interpret I 2 , Higgins and Thompson [ 33 ] suggested a tentative classification of 25 (low), 50 (medium), and 75 (high). For our moderator tests, study quality, Terry’s [ 20 ] propositions, performance measure characteristics, and athlete standard, we used a mixed-effects analysis. For these analyses, we reported the number of cases, sample size, r , 95% confidence intervals, and the Q total between (Q TB ) with associated p -value. The Q TB indicates the level of difference between different moderator levels. We used a random-effects meta-regression model to test the impact of percent male athletes on the confidence–performance relationship. Last, we examined our results with the aim of assessing certainty. We conducted our meta-analyses using the Comprehensive Meta-Analysis (CMA) version-3 software (version 3.3.070, Biostat, Inc., Englewood, NJ, USA, 20 November 2014).
2.7. Risk of Bias across Studies
We examined publication bias as the risk of bias across studies. We examined the fail-safe n calculation, the funnel plot, and the ‘trim and fill’ results for random effects found in the CMA program. The fail-safe n statistic is the number of null effect samples required to change a significant effect size into a non-significant effect size [ 34 ]. The greater the value, the greater the confidence that the meta-analyzed result is indeed safe from publication bias (based on the one-tail test in our analyses). Thus, the larger number of studies per reported study value, the greater the confidence in the effect size being free of publication bias. The random-effects funnel plot of precision determined whether the entered studies dispersed equally on either side of the overall effect [ 35 ], as symmetry theoretically represents the notion that entered studies captured the essence of all relevant studies. Concerning sample size and the funnel plot, smaller studies are closer to the bottom and larger studies closer to the top of the graph. We used Duval and Tweedie’s [ 36 ] trim and fill analysis to fix asymmetry. The data points are either filled to the left (i.e., lowering the effect size value) or right (i.e., increasing the effect size value) of the mean.
3.1. Study Selection and Characteristics
Table 2 shows the 41 studies meeting all inclusion criteria of which a few provided more than one data set for 49 total samples. None of the studies provided data from more than one sport nor more than one country. The studies spanned from 1986 to 2020, with 3711 total participants (range = 7–416, mean = 80.84, SD = 92.13) with data coming from 15 countries on the following continents: Australia and Oceania, Europe, and North and South America. Most participants were adolescents and young adults, as only three sample age group means were greater than 30 years of age. Of the studies identifying participant sex, the majority were males with a mean percent male of 65.46 (SD = 36.25) and a range from 0% to 100%. The included studies contained a variety of sports, both individual (e.g., boxing, golf, taekwondo) and team (e.g., basketball, softball, volleyball).
Study characteristics.
| Participant Characteristics | Confidence and Performance Characteristics | ||||||
|---|---|---|---|---|---|---|---|
| Study | Age (yr.) | Ctry. | N | % Male | Sport | Confidence | Performance |
| Armes Alejo [ ] | 17.00, 22.60 | BR | 60 | NA | Boxing | CSAI-2 | Medalists, non-medalists |
| Barnes et al. [ ] | College | US | 13 | 100 | Swim | CSAI-2 | Event time |
| Beattie et al. [ ] | 22.50 | UK | 81 | 76.54 | Canoeing | CSAI-2 | Event time |
| Bejek & Hagtvet [ ] | Adolescent | HU | 20 | 0 | Gymnastics | CSAI-2 | Event score |
| Bejek & Hagtvet [ ] | Adolescent | HU | 49 | 0 | Gymnastics | CSAI-2 | Event score |
| Bird & Horn [ ] | 14.00–17.00 | US | 161 | 0 | Softball | CSAI-2 | Coach rating of athlete mental errors |
| Bueno et al. [ ] | 31.01 | ES | 90 | 88.89 | Endurance | CSAI-2 | Successful, not successful achieving objective |
| Burton 1988 [ ] | 18.00–23.00 | US | 28 | 53.57 | Swim | CSAI-2 | Event performance compared to personal best |
| Burton 1988 [ ] | 17.40 | US | 70 | 44.28 | Swim | CSAI-2 | Event performance compared to personal best |
| Chapman et al. [ ] | 21.23 | UK | 142 | 100 | Taekwondo | CSAI-2 | Winners, losers |
| Cox et al. [ ] | NR | US | 248 | 75.81 | Basketball | ARS-2 | Margin of victory |
| Draper et al. [ ] | 25.60 | NZ | 20 | 60 | Rock climbing | CSAI-2R | Completed route, not completed route |
| Edwards & Hardy [ ] | 21.80 | UK | 45 | 0 | Netball | CSAI-2 | Athlete rated performance |
| Gayton & Nickless [ ] | 34.74 | US | 35 | 71.42 | Running | TSCI | Event time |
| Hassmén et al. [ ] | 21.00 | SE | 8 | 100 | Golf | CSAI-2 | Season score average |
| Heazlewood & Burke [ ] | NR | AU | 416 | NA | Triathlon | CSAI-2 | Event time |
| Iso-Ahola & Blanchard [ ] | NR | US | 73 | 78.08 | Racquetball | 1-item | Athlete standard-winners, losers |
| Jerome & Williams [ ] | 41.00 | US | 143 | 62.94 | Bowling | CSAI-2 | Event performance compared to league average |
| Jones et al. 1993 [ ] | 14.00–16.00 | UK | 48 | 0 | Gymnastics | CSAI-2 | Good performers, poor performers |
| Kais et al. 2004 [ ] | 28.20 | EE | 66 | 100 | Volleyball | CSAI-2 | Expert rating of athlete performance |
| Kais et al. 2005 [ ] | NR | EE | 24 | NA | Team sports | CSAI-2 (Int.) | Coach rating of athlete performance |
| Laborde et al. [ ] | 23.88 | DE | 28 | 53.57 | Tennis | CSAI-2 | Tennis serving errors |
| Lautenbach et al. [ ] | 24.04 | DE | 23 | 56.52 | Tennis | CSAI-2 | Tennis serving errors |
| Levy et al. [ ] | 21.63 | UK | 415 | 53.49 | NR | SSCI | Athlete rated performance satisfaction |
| Martin et al. [ ] | 16.00 | US | 73 | 100 | Running | SSCI | Event time |
| Maynard & Howe [ ] | 19.00–24.00 | CA | 22 | 100 | Rugby | CSAI-2 | Coach rating of athlete performance |
| McAuley [ ] | College | US | 7 | 0 | Golf | CSAI-2 | Event score |
| McCann et al. [ ] | 19–26 | US | 42 | 92.86 | Cycling | CSAI-2 | Time maintained pace |
| Nicholls et al. [ ] | 21.30 | UK | 307 | 73.28 | Mix | CSAI-2R | Athlete rated performance satisfaction |
| Perreault & Marisi [ ] | 25–40 | CA | 37 | 100 | Basketball | CSAI-2 | Event performance statistics |
| Pessoa da Costa et al. [ ] | 17.00 | 16 | 100 | B. volleyball | CSAI-2R | Performance statistics | |
| Pinto & Vázquez [ ] | 16.14 | 77 | 81.82 | Golf | CSAI-2 | Event placement | |
| Psychountaki & Zervas [ ] | 11.20 | GR | 143 | 53.85 | Swim | SSCQ-C | Coach rating of athlete performance |
| Rodrigo et al. [ ] | 18.00–31.00 | UY | 51 | 100 | Soccer | CSAI-2 | Athlete and observer rated performance |
| Sanchez et al. [ ] | 24.60 | GB | 19 | 100 | Rock climbing | CSAI-2 | Event score |
| Swain & Jones [ ] | 21.10 | UK | 10 | 100 | Basketball | CSAI-1 | Performance statistics |
| Terry & Slade [ ] | 25.35 | UK | 199 | 100 | Karate | CSAI-2 | Winners, losers |
| Terry & Youngs [ ] | 20.40 | UK | 128 | 50 | Field hockey | CSAI-2 | Team selection |
| Terry et al. [ ] | 19.90 | UK | 100 | 32 | Tennis | CSAI-2 | Winners, losers |
| Totterdell [ ] | 26.00 | UK | 33 | 100 | Cricket | UWIST | Batting/bowling average |
| Tsopani et al. [ ] | 11.50 | GR | 74 | 0 | Gymnastics | CSAI-2 | Event score |
| Vadocz et al. [ ] | 15.39 | UK | 57 | 59.65 | Roller skating | CSAI-2 | Medalists, non-medalists |
| Zienius et al. [ ] | 16.70 | LT | 10 | 100 | Golf | CSAI-2 | Event score |
Bold country abbreviation = study written in non-English. Country abbreviations: Country (Ctry.), Australia (AU), Argentina (AR), Brazil (BR), Canada (CA), Estonia (EE), Germany (DE), Greece (GR), Hungary (HU), Lithuania (LT), New Zealand (NZ), Spain (ES), Sweden (SE), Uruguay (UY), United Kingdom (UK), United States (US); Sport abbreviation: Beach (B). Confidence abbreviations: Cognitive Somatic Anxiety Inventory (CSAI), Revised (R), State Sport Confidence Questionnaire for Children (SSCQ-C), University of Wales Institute of Sciences and Technology (UWIST).
3.2. Risk of Bias within Studies
The Supplemental file contains all the risk of bias within studies details. The two samples from Bejek and Hagtvet [ 8 ] differed in methodology; hence, both samples are listed. Across the risk of bias topics, the mean score (possible range 9–27 points) was 20.58 (SD = 1.76). We rated each study as either high ( n = 15), medium ( n = 9), and low ( n = 19) quality (i.e., risk of bias) based on being above, below or at the median score. The median score of 21 is the medium quality group. We tested study quality as a moderator of the overall confidence–performance relationship. The mixed effects Q Tb statistics was not significant ( p = 0.37), and the random effects r [95% CI] were as follows for the three quality of rating groupings: high 0.27 [0.16, 0.37], medium 0.29 [0.18, 0.40], and low 0.20 [0.11, 0.29]. Each random effects mean r was different from zero ( p values < 0.001).
3.3. Results of Individual Studies, Synthesis of Results, and Risk of Bias across Studies
Figure 2 contains the individual study data. From those data, the overall effect of the confidence–performance relationship was different from zero (Z-value = 8.30, p < 0.001), small in magnitude with a point estimate calculated as r of 0.25, and with medium-to-high heterogeneity ( I 2 = 64.49). The 95% confidence intervals spanned from small (0.19) to medium (0.30) in magnitude. As represented in Figure 3 , little publication bias existed in the data (trim n = 1, adjusted point estimate of 0.24% and 95% confidence intervals, ranging from 0.19 to 0.30), were almost identical to the non-trimmed results. Last, relative to the 49 samples from 41 studies, the fail-safe n was large at 3601.

Study effect size statistics expressed as correlations and corresponding forest plot.

Random effects plot trimmed and filled. The open circles are the data points, and the one filled circle is the result of the trim and fill analysis. The clear rhombus is the point estimate, and the filled rhombus is the trim and filled point estimate.
3.4. Moderators
3.4.1. terry’s propositions and performance characteristics.
Table 3 contains our coded moderators, and Table 4 contains the mixed-effects analysis results. Concerning Terry’s [ 20 ] propositions, the confidence–performance relationship was higher for sports of less than 10 min, closed skilled, and individual when compared to sports greater than 10 min, open skilled, and team. The sport type mixed-effects analysis was significant at the traditional level ( p < 0.05). The upper 95% confidence intervals for sports of less than 10 min, closed skilled, and individual were all medium ( r > 0.30) in magnitude. For the two performance characteristic moderators, the effect size values were greater in magnitude for objective compared to subjective ( p < 0.05) and other-referenced compared to self-referenced performance measures. The upper 95% confidence intervals for objective and other-referenced performance measures were medium ( r > 0.30) in magnitude.
Moderator Coding for Terry’s Proposition, Performance Characteristics, and Confidence Time to Event Measured.
| Terry’s Propositions | Performance | Athlete | ||||||
|---|---|---|---|---|---|---|---|---|
| Study | Time | Skill | Type | Type | Reference | Time to Event | Groupings | Standard |
| Armes Alejo [ ] | >10 | O | I | OBJ | OTH | >1 h | Elite | High |
| Barnes et al. [ ] | <10 | C | I | OBJ | Self | 16–30 | College | High |
| Beattie et al. [ ] | <10 | O | I | OBJ | OTH | 16–30 | Elite | High |
| Bejek & Hagtvet [ ] | <10 | C | I | SUB | OTH | 16–30 | Elite | High |
| Bejek & Hagtvet [ ] | <10 | C | I | SUB | OTH | 16–30 | Rec | Low |
| Bird & Horn [ ] | >10 | O | T | SUB | Self | 31–60 | HS | Low |
| Bueno et al. [ ] | >10 | C | I | SUB | Self | >1 h | Mix | ? |
| Burton 1988 [ ] | <10 | C | I | OBJ | Self | 31–60 | College | High |
| Burton 1988 [ ] | <10 | C | I | OBJ | Self | 31–60 | College | High |
| Chapman et al. [ ] | <10 | O | I | OBJ | OTH | 31–60 | Rec | Low |
| Cox et al. [ ] | >10 | O | T | OBJ | Self | <15 | Rec | Low |
| Draper et al. [ ] | <10 | C | I | OBJ | OTH | <15 | Rec | Low |
| Edwards & Hardy [ ] | >10 | O | T | SUB | Self | <15 | EC | Low |
| Gayton & Nickless [ ] | >10 | C | I | OBJ | OTH | <15 | Rec | Low |
| Hassmén et al. [ ] | >10 | C | I | OBJ | OTH | 31–60 | Elite | High |
| Heazlewood & Burke [ ] | >10 | C | I | OBJ | OTH | >1 h | Rec | Low |
| Iso-Ahola & Blanchard [ ] | >10 | O | I | OBJ | OTH | <15 | Rec | Low |
| Jerome & Williams [ ] | >10 | C | I | OBJ | Self | 31–60 | Rec | Low |
| Jones et al. 1993 [ ] | <10 | C | I | SUB | OTH | <15 | EC | Low |
| Kais et al. 2004 [ ] | >10 | O | T | OBJ | OTH | >1 h | Elite | High |
| Kais et al. 2005 [ ] | >10 | O | T | SUB | Self | 31–60 | Elite | High |
| Laborde et al. [ ] | <10 | C | I | OBJ | OTH | <15 | Mix | ? |
| Lautenbach et al. [ ] | <10 | C | I | OBJ | OTH | <15 | Rec | Low |
| Levy et al. [ ] | Both | Both | Both | SUB | Self | 31–60 | Mix | ? |
| Martin et al. [ ] | <10 | C | I | OBJ | OTH | 16–30 | HS | Low |
| Maynard & Howe [ ] | >10 | O | T | SUB | Self | 31–60 | College | High |
| McAuley [ ] | >10 | C | I | OBJ | OTH | <15 | College | High |
| McCann et al. [ ] | <10 | C | I | OBJ | OTH | <15 | Elite | High |
| Nicholls et al. [ ] | ? | ? | Both | SUB | Self | >1 h | Rec | Low |
| Perreault & Marisi [ ] | >10 | O | T | OBJ | OTH | 16–30 | Elite | High |
| Pessoa da Costa et al. [ ] | >10 | O | T | OBJ | OTH | 16–30 | Elite | High |
| Pinto & Vázquez [ ] | >10 | C | I | OBJ | OTH | >1 h | USAC | Low |
| Psychountaki & Zervas [ ] | <10 | C | I | SUB | Self | 31–60 | EC | Low |
| Rodrigo et al. [ ] | >10 | O | T | SUB | Self | 31–60 | Elite | High |
| Sanchez et al. [ ] | <10 | C | I | OBJ | OTH | 16–30 | Elite | High |
| Swain & Jones [ ] | >10 | O | T | OBJ | OTH | 16–30 | EC | High |
| Terry & Slade [ ] | <10 | O | I | OBJ | OTH | 31–60 | Rec | Low |
| Terry & Youngs [ ] | >10 | O | T | OBJ | OTH | 31–60 | College | High |
| Terry et al. [ ] | >10 | C | I | OBJ | OTH | 31–60 | Rec | Low |
| Totterdell [ ] | >10 | O | T | Both | Self | <15 | Elite | High |
| Tsopani et al. [ ] | <10 | C | I | OBJ | OTH | 31–60 | EC | Low |
| Vadocz et al. [ ] | Both | Mix | Mix | OBJ | OTH | >1 h | Elite | High |
| Zienius et al. [ ] | >10 | C | I | OBJ | OTH | <15 | EC | Low |
Abbreviations: L = low, M = medium, H = high; ? = not enough information presented to decide, O = open skill sport, C = closed skill sport, I = individual sport, T = team sport, OBJ = objective, SUB = subjective, OTH = performance other-referenced, Self = performance self-referenced; Rec = recreational, EC = European Club, USAC = United States of America club, HS = High school; Groupings are based on our attempt to examine Craft et al. [ 11 ]; Standard is our attempt to examine Woodman and Hardy [ 12 ].
Moderator Results for Terry’s Proposition, Performance Characteristics, and Confidence Time to Event Measured.
| Moderator | Group | k | r | 95% CI LL | 95% CI UL | Q | -Value | |
|---|---|---|---|---|---|---|---|---|
| Sport time | <10 | 19 | 1144 | 0.304 | 0.213 | 0.389 | ||
| >10 | 27 | 2034 | 0.201 | 0.128 | 0.281 | 2.677 | 0.102 | |
| Sport skill | Closed | 25 | 1591 | 0.280 | 0.194 | 0.362 | ||
| Open | 21 | 1587 | 0.212 | 0.122 | 0.298 | 1.202 | 0.273 | |
| Sport type | Individual | 32 | 2295 | 0.288 | 0.221 | 0.353 | ||
| Team | 14 | 883 | 0.142 | 0.032 | 0.249 | 5.199 | 0.023 | |
| Performance type | Objective | 35 | 2527 | 0.290 | 0.223 | 0.357 | ||
| Subjective | 13 | 1397 | 0.137 | 0.027 | 0.245 | 5.591 | 0.018 | |
| Performance reference | Other | 30 | 2065 | 0.289 | 0.218 | 0.358 | ||
| Self | 19 | 1892 | 0.187 | 0.098 | 0.273 | 3.197 | 0.074 | |
| Confidence time | <15 | 13 | 627 | 0.246 | 0.120 | 0.364 | ||
| 16–30 | 9 | 336 | 0.187 | 0.024 | 0.340 | |||
| 31–60 | 19 | 1886 | 0.255 | 0.165 | 0.340 | |||
| >1 h. | 8 | 1108 | 0.274 | 0.146 | 0.393 | 0.771 | 0.856 | |
| Athlete level # | Elite | 14 | 566 | 0.215 | 0.109 | 0.316 | ||
| College | 8 | 277 | 0.221 | 0.061 | 0.369 | |||
| European club | 6 | 330 | 0.195 | 0.038 | 0.343 | 0.062 | 0.969 | |
| Athlete standard ^ | Higher | 22 | 843 | 0.220 | 0.121 | 0.314 | ||
| Lower | 25 | 2609 | 0.252 | 0.177 | 0.324 | 0.270 | 0.603 | |
| Sex | 100% female | 7 | 404 | 0.066 | -0.099 | 0.227 | ||
| 100% male | 14 | 699 | 0.349 | 0.236 | 0.453 | 8.025 | 0.005 |
Abbreviation: k = number of samples, n = number of participants in moderator level, CI = confidence interval, LL = lower limit, UL = upper limit; # Groupings attempting to matching Craft et al. [ 11 ]; ^ Groupings attempting to match Woodman and Hardy [ 12 ].
3.4.2. Timing of Confidence Measure and Individual Difference Moderators
For the confidence measurement before performance period, all periods mean values were small in magnitude. The upper 95% confidence interval crossed the medium threshold ( r > 0.30) for each time category. Last, for our attempts to examine individual difference moderators, neither the Craft et al. [ 11 ] nor Woodman and Hardy [ 12 ] moderator categories differed, and all mean values were small in meaningfulness. However, results for percent male participants were significant in both the meta-regression (see Figure 4 ) and mean difference analyses.

Meta-regression plot of the relationship of percent male in each study sample and the overall self-confidence and sport performance relationship, R 2 = 0.22, F (1,43) = 6.62, p < 0.01, Goodness of fit Q(43) = 112.73, p < 0.0001, expressed as Fisher’s Z. Larger circles represent studies with more participants. Middle line is the regression line; the upper and lower lines are the 95% confidence intervals.
3.5. Certainty of Evidence
Table 5 contains our research questions, our rating of certainty of evidence corresponding to the research question, and the basis for our certainty rating. The second Supplemental file contains details of data extracted and compared with our results and those of Craft et al. [ 11 ] and Woodman and Hardy [ 12 ].
Certainty of Results by Research Question.
| Research Question | Certainty Basis | Rating | ||
|---|---|---|---|---|
| Q1: What was the overall relationship between a measure of state self-confidence and performance? Moreover, does the risk of individual study bias or across study bias (i.e., publication bias) moderate this relationship? No (not moderated by bias). | We replicated the overall confidence–performance relationship reported by Craft et al. [ ] and Woodman and Hardy [ ] with different inclusion criteria and many non-overlapping studies. Risk of individual study bias and publication bias had no impact on the overall relationship. | High | ||
| Q2: Did Terry’s [ ] sport propositions moderate the confidence–performance relationship? Yes. | All compared moderator levels were in line with Terry’s [ ] propositions. Individual vs. team findings were consistent with Craft et al. [ ] and Woodman and Hardy [ ] with many non-overlapping samples. Only inconsistency related to Craft et al. [ ] large open vs. closed skill values (incongruent with Terry’s [ ] propositions). Unable to replicate Craft et al. [ ] given non-overlapping samples. | Moderate to High | ||
| Q3: Did the objectivity and reference of the performance measure moderate the confidence–performance relationship? Yes. | Significant difference between objective vs. subjective performance measure although both mean correlation values are small. Similar result with self-referenced vs. other-referenced performance measures. | Moderate | ||
| Q4: Did the time of self-confidence assessment prior to performance moderate the confidence–performance relationship? No. | The correlation values and 95% confidence intervals did not differ significantly by time of self-confidence assessment. Failed to replicate Craft et al. [ ]. | Moderate | ||
| Q5: Did selected individual difference variables, namely sex and athlete sport level, moderate the confidence–performance relationship? Yes (sex question). | Our meta-regression results and mean difference values were significant and replicated the Woodman and Hardy [ ] finding that sex moderates the confidence–performance relationship. | High | ||
| No (sport level, athlete level question). | Small correlation was consistent with Woodman and Hardy [ ]. Inconsistent but still wide 95% confidence intervals with the high standard sport level. Consistent with Craft et al. as all our values were small. However, we did not replicate Craft et al. [ ] European Club relationship. | Moderate |
4. Discussion
The present study was a systematic review with meta-analysis of the published literature on the state of the confidence–performance relationship. We distinguished self-confidence from self-efficacy based on the terms used by authors in their article. Overall, results showed that self-confidence has a positive effect on performance, moderated by sport-type, measure of performance, and athlete sex. Our findings mirrored those of the two past meta-analyses [ 11 , 12 ]. Given the congruencies and the minimal bias in our data, the certainty is high that the confidence–performance relationship is small in magnitude. Even at its strongest, the relationship in our mean level data rarely crossed the moderate threshold ( r > 0.30) in meaningfulness.
An intriguing question is why is the confidence–performance relationship not as strong as theory would predict? Michie et al. [ 69 ] proposed self-confidence impacts performance via mechanisms such as increasing effort, selecting appropriate strategies, and regulating unwanted emotions. One explanation is that the central premise of higher confidence leading to better performance is overstated. To address this question, researchers would need to test the mechanisms by which the confidence–performance relationship occurs, which relies on using methods that enable the accurate detection of the influence of self-confidence on performance. It is apparent by reviewing the 41 included studies and the literature overall, that researchers have focused primarily on testing the strength of the confidence–performance relationships and have given little attention to investigating the mechanisms that underpin them. Thus, future research should investigate possible confidence–performance mechanisms.
Concerning Terry’s [ 20 ] propositions, our results showed a stronger relationship between confidence and performance in short duration sports compared to longer duration sports and individual sports compared to team sports. These results speak to the idea that self-confidence may change during performance, either increasing or decreasing. In team sports, self-confidence could be dependent upon teammates’ actions and confidence could change once performance begins. Thus, the longer the sport event, the greater the possibility that confidence changes and thus the confidence–performance relationship weakens. Likewise, in team sports, one individual’s confidence may have little to do with performance outcome if they get minimal playing time and/or the actions of teammates determine the performance outcome. It is possible that self-confidence will be influential on performance, but to detect its effect requires a more sensitive research design, such as repeated measures within the event. Emotion research has faced similar challenges, whether it be measuring emotions prior to performance [ 28 ] or using retrospective designs [ 70 ]. In our included studies, only Totterdell [ 66 ] used a repeated-measures design. A few excellent examples in the emotion research exist whereby researchers captured multiple emotion–performance relationships during competition [ 71 , 72 ]. Hence, to understand the confidence–performance relationship, we suggest repeated confidence testing within the event while recording performance.
Continuing our questioning as to why the confidence–performance relationship is small though moderated by performance characteristics (i.e., type and reference), another issue when measuring self-confidence is the extent to which participants have accurate knowledge of tasks demands. For example, if people have recently completed the task, then they have an experiential basis to rate future expectancies. Bandura [ 73 ] highlighted that when there is an abundance of feedback on a specific task, confidence estimates tend to mirror previous performance closely. Such an assertion works well when the performance task remains stable, such as with a math puzzle. In sports competition, even closed skills contain factors that change and when the level of competition rises, and differences between winners and losers are marginal, such uncontrollable factors grow in importance.
A further issue when assessing self-confidence is the extent to which people have access to relevant information on which to base self-confidence estimates. Athletes may base their confidence on belief in skill execution, physical fitness, and intended effort, but confidence estimates remain hypotheses until tested by situational factors. There is an ongoing feedback loop between behavior and perception, whereby athletes assess and re-assess their confidence estimates from continuous performance feedback. Failing to meet the standard expected tends to activate unpleasant emotions that serve as a signal to improve performance possibly by increasing effort or changing strategy. However, at the time athletes self-report their confidence, the information used comes from memories distal from the current competition. Therefore, given the importance of having accurate and available information to inform self-confidence ratings, objective (vs. subjective) and other-referenced (vs. self-referenced) performance measures are more accurate and available to the performer.
A limitation of research investigating sport confidence is that neither the information used by athletes to rate self-confidence, nor the strategies they plan to use to achieve their goals are known. Therefore, we do not know how athletes arrive at their ratings, only what ratings they provide. Research has been conducted into the antecedents of self-confidence ratings among athletes [ 74 , 75 ], which provides additional insights. However, further exploration, perhaps using qualitative techniques, of exactly how athletes arrive at their self-confidence ratings and develop their beliefs about the effectiveness of planned competition strategies would be particularly germane.
Examination of the evidence base and strategies to deliver performance expectations might be particularly useful when exploring sex differences in the confidence–performance relationship. Although male athletes tend to report higher self-confidence compared to female athletes [ 24 ], this does not in itself explain sex differences in the confidence–performance relationship. Using intra-individual analysis of performance in the shooting phase of 254 international biathlon competitions, Ahammer et al. [ 76 ] showed that a one standard deviation reduction in self-confidence increased the number of missed shots by 0.53 standard deviations for men, but there was no effect of self-confidence on missed shots for women. Further investigation of sex-based differences in cognitive, behavioral, and emotional processes that occur between the pre-competition assessment of self-confidence and the outcome of performance may provide valuable insights into the confidence–performance relationship. Last, an interesting observation relates to the age of samples used to study self-confidence. Nearly all samples were younger adults, with mean age exceeding 30 in only three studies. With aging and gathering experiences, athletes might accrue greater knowledge of task demands and therefore provide more accurate confidence estimates. We suggest that future research should investigate the confidence–performance relationship in targeted populations, such as all-female and master athletes.
Study Limitations
Even having closely followed the PRISMA statement [ 25 ], limitations within our meta-analysis are evident. First, although we identified 41 studies meeting our inclusion criteria, it is possible we missed relevant studies because the CSAI-2 measure is more closely associated with anxiety than with confidence, and article titles, abstracts, and keywords might make no mention of confidence despite having measured it. Likewise, studies with multiple psychological measures might exclude mention of confidence in the title, abstract, and keywords. We ameliorated this potential limitation by retaining studies for full-text screening if there was even a suspicion that confidence was a measured variable despite not being mentioned in the title, abstract, nor keywords. Second, we decided, given the decades covered in our search, from the 1980s or potentially earlier to the 2020s, not to contact authors for missing data. Our reasoning was the passage of time for data storage and even deceased researchers would bias the data available. However, the minimal publication bias found eased our concerns of these two limitations. Third, with 41 studies contributing 49 samples, small sample sizes were present in some of our moderator analyses. Smaller samples limited statistical power to detect significant between-level differences and may have contributed to larger confidence intervals. Fourth, we attempted to test the individual difference moderators reported in Craft et al. [ 11 ] and Woodman and Hardy [ 12 ]. Without exact operational definitions and coding for levels such as elite, European club, and top and lower standard, we may have coded our samples differently to previous research teams. Last, we sought to include eligible studies with no language restriction. To do so, we used Google Translate ( https://translate.google.com/ , accessed on 1 March 2021). It is possible that Google Translate is not 100% accurate and we either excluded eligible studies or included ineligible studies. Although we have mentioned use of Google Translate as a limitation, including studies without a language restriction was a clear strength of our meta-analysis, instead of including only studies published in English.
5. Conclusions
Self-confidence dominates the sport media and the athletic rhetoric as vital to performance, in such statements such as “If you don’t have confidence, you will always find a way to not win” (Carl Lewis, 9-time Olympic Gold Medalist). However, based on our meta-analysis and two past meta-analyses, the confidence–performance relationship is small in magnitude with a few important moderators. It might be true, as Carl Lewis asserts, that without confidence one cannot win. However, it might be simply that without more confidence than the other team or competitor at a critical moment, one will find a way not to win.
Acknowledgments
The research team wishes to acknowledge the Department of Kinesiology and Sport Management for supporting the research by purchasing the Comprehensive Meta-Analysis software.
Supplementary Materials
The following supporting information can be downloaded at: https://www.mdpi.com/article/10.3390/ijerph19116381/s1 , Supplement 1. Search strategy, Supplement 2. Risk of individual study bias ratings, Supplement 3. Comparison of Results, and Supplement 4. PRISMA Checklist.
Funding Statement
This research was funded by the Texas Tech University Office of the Vice-Provost and the Texas Tech University TrUE SPARK program. MS was funded by Texas Tech University Office of the Vice-Provost. CS and SC were funded by Texas Tech University TrUE SPARK program.
Author Contributions
Conceptualization, M.L. and P.C.T.; methodology, M.L., M.S., A.M.L. and P.C.T. software use, M.L.; formal analysis, M.L. and C.S.; data curation, M.L., M.S., C.S. and S.C.; writing—original draft preparation, M.L., P.C.T. and A.M.L.; writing—review and editing, M.L., P.C.T., A.M.L. and S.C.; supervision, M.L. and P.C.T.; project administration, M.L.; funding acquisition, M.L. All authors have read and agreed to the published version of the manuscript.
Institutional Review Board Statement
Not applicable for studies not involving humans or animals.
Informed Consent Statement
Not applicable for studies not involving humans.
Data Availability Statement
Conflicts of interest.
The authors declare no conflict of interest. The funders for M.S., C.S., and S.C. had no role in the design of the study; in the collection, analyses, or interpretation of data; in the writing of the manuscript, or in the decision to publish the results.
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.
- SUGGESTED TOPICS
- The Magazine
- Newsletters
- Managing Yourself
- Managing Teams
- Work-life Balance
- The Big Idea
- Data & Visuals
- Reading Lists
- Case Selections
- HBR Learning
- Topic Feeds
- Account Settings
- Email Preferences
How Confidence Is Weaponized Against Women
- Darren T. Baker
- Juliet Bourke

It’s a problem when women are perceived as too confident. Or not confident enough.
When women fail to achieve career goals, leaders are prone to attribute it to a lack of self-confidence. And when women demonstrate high levels of confidence through behaviors, such as being extroverted or assertive, they risk overdoing it and, ironically, being perceived as lacking confidence. No matter the outcome, women’s lack of career progression is blamed on them, an attack they share with other underrepresented groups. This leads women to beat themselves up, which can weaken self-esteem and, in a downward spiral, further erode self-perceptions of confidence.
Women are regularly exhorted to demonstrate self-confidence as a strategy to progress their careers, raise their pay, and become more successful at work. Self-help guides commend women to “lean in” to reach their goals, “stand their ground,” make strong eye contact, attune their voices, postures, and gestures to come across more assertively, and to “fake it ‘til they make it.” Women have to do all this while balancing on a knife edge the need to remain likeable/ warm by appearing unintimidating, unforceful, and undomineering.
- Darren T. Baker , PhD, is assistant professor of business in society at UCD Michael Smurfit Graduate Business School, Ireland. His work provides an ethical and psychoanalytic analysis of the key challenges and opportunities in business and society, including sustainability, CSR, diversity and leadership across sectors. Follow him @Darren_T_Baker . Email him at [email protected]
- Juliet Bourke , PhD, is a professor of practice in the School of Management and Governance, UNSW Business School, UNSW. She is the author of Which Two Heads Are Better Than One: The Extraordinary Power of Diversity of Thinking and Inclusive Leadership . Email her at [email protected]
Partner Center
- Bipolar Disorder
- Therapy Center
- When To See a Therapist
- Types of Therapy
- Best Online Therapy
- Best Couples Therapy
- Managing Stress
- Sleep and Dreaming
- Understanding Emotions
- Self-Improvement
- Healthy Relationships
- Student Resources
- Personality Types
- Sweepstakes
- Guided Meditations
- Verywell Mind Insights
- 2024 Verywell Mind 25
- Mental Health in the Classroom
- Editorial Process
- Meet Our Review Board
- Crisis Support
11 Signs of Low Self-Esteem
Verywell / Madelyn Goodnight
- Coping With
- Improvement Tips
Low self-esteem refers to a person having an overall poor sense of self-value. It essentially means having a poor opinion of yourself. Low self-esteem can encompass a range of factors, such as your sense of identity, self-confidence, feelings of competence, and feelings of belonging.
Self-esteem is about more than just generally liking yourself—it also means believing that you deserve love and valuing your own thoughts, feelings, opinions, interests, and goals. It can also play a role in how you allow others to treat you .
Having self-esteem not only impacts how you feel about and treat yourself, but it can even affect your motivation to go after the things you want in life and your ability to develop healthy, supportive relationships. It plays an important role in a variety of areas in life, which is why having low self-esteem can be such a serious problem.
Having low self-esteem means that you often think negatively about yourself, judge yourself badly, and lack confidence in your abilities.
Signs of Low Self-Esteem
While not a mental illness, poor self-esteem can still affect a person’s thoughts, emotions, and patterns of behavior. Sometimes its signs can be fairly apparent. Other times, low self-esteem symptoms are much more subtle.
For example, some people with low self-esteem talk negatively about themselves, while others go out of their way to make sure other people are pleased with them. In either case, a lack of personal worth and value can have a negative impact on life and wellness.
Some common signs or symptoms of low self-esteem include:
- Lack of confidence
- External locus of control
- Negative social comparisons
- Trouble asking for help
- Worry and doubt
- Difficulty accepting compliments
- Negative self-talk
- Fear of failure
- Poor outlook of the future
- Lack of boundaries
- Being a people-pleaser
You can also find online self-esteem tests to help determine whether your self-worth may be low. For instance, the Open-Source Psychometrics Projects offers free access to a version of the Rosenberg Self Esteem Scale , which is a test used to measure self-esteem in research.
Poor Confidence
People with low self-confidence tend to have low self-esteem, and vice versa. Low self-esteem can play a role in causing a lack of confidence, but poor confidence can also contribute to or worsen poor self-esteem.
Being confident in yourself and your abilities allows you to know that you can rely on yourself to manage different situations. This self-trust means that you feel comfortable and confident navigating many different things you might encounter in life, which can play an important role in your overall well-being .
Finding ways to gain confidence in yourself and your abilities can be helpful. Acquiring and practicing new skills is one tactic you might try. This may even help reduce feelings of anxiousness as research connects a lack of confidence with higher anxiety levels, especially when under stress.
Lack of Control
People who have low self-esteem often feel that they have little control over their lives or what happens to them. This can be due to the feeling that they have little ability to create changes in themselves or in the world. Because they have an external locus of control , they feel powerless to do anything to fix their problems.
Research has found that in situations where people have little control over what happens, having higher self-esteem can help relieve some of the negative effects of this loss of control, which ultimately benefits mental health.
If you feel like you have no control over your life or situation, finding ways to improve your self-esteem may be helpful for your well-being.
Negative Social Comparison
Social comparison can sometimes serve a positive function and enhance a person's sense of self. But comparing yourself to others can also damage self-esteem. People with low self-esteem may be more likely to engage in what is known as upward social comparison, or comparing themselves to people who they think are better than themselves.
Upward social comparison isn't always bad. For instance, these comparisons can be a source of information and inspiration for improvement. When people are left with feelings of inadequacy or hopelessness , however, it can inhibit self-esteem.
Social media can also play a role in such comparisons, contributing to low self-esteem. If you often compare yourself unfavorably to people on social media sites such as Facebook and Instagram, your self-esteem may take a hit.
Problems Asking for What You Need
When a person has low self-esteem, they may struggle to ask for what they need. Trouble asking for what you need can be caused by feeling embarrassed. Or you may feel that a need for assistance and support is a sign that you are incompetent.
Because their self-regard is low, someone with low self-esteem might also feel that they don't deserve help. They don't prioritize their own desires, so they struggle to assert themselves when they are in need.
Worry and Self-Doubt
Even after making a decision, people who have low self-worth often worry that they’ve made the wrong choice. They doubt their own opinions and may defer to what others think instead of sticking to their choices.
This can lead to a great deal of second-guessing and self-doubt. This makes it harder for people with low self-esteem to make decisions about their lives.
Trouble Accepting Positive Feedback
A 2017 study published in the Journal of Experimental Social Psychology found that low self-esteem is directly correlated to not being able to accept or capitalize on compliments from others.
Positive feedback is often met with suspicion and distrust. Complimentary words do not align with their beliefs about themselves, so people with self-esteem issues may feel that the other person is being flippant or even cruel.
Because they don’t have a positive opinion about themselves, people who have low self-esteem find it difficult to accept compliments from others.
Negative Self-Talk
Low self-esteem causes people to focus on their flaws rather than their strengths. Rather than build themselves up with positive self-talk, they always seem to have something negative to say about themselves, engaging in negative self-talk instead.
When things go wrong, people with low self-esteem often blame themselves. They find fault with some aspect of themselves, whether it is their appearance, their personality, or their abilities.
Fear of Failure
Because they lack confidence in their abilities, people with low self-esteem doubt their ability to achieve success. Because they fear failure, they tend to either avoid challenges or give up quickly without really trying.
This fear of failure can be seen in behaviors such as acting out when things go wrong or looking for ways to hide feelings of inadequacy. People with low self-esteem might also make excuses, blame external factors, or try to downplay the importance of the task.
Poor Outlook
Low self-worth can cause people to feel that there is little chance that the future will be any better than the present. These feelings of hopelessness can make it hard for people with low self-esteem to engage in behaviors that will bring about positive changes in their lives.
Self-sabotage is a common way of coping with such feelings. By finding obstacles to prevent success, people with low self-esteem are able to find something else to blame for not achieving their goals or finding greater levels of happiness in their lives.
Lack of Boundaries
The ability to set boundaries is often established early in life. Children with caregivers who show them that they are respected and valued are better able to create good boundaries in adult relationships. They are also more likely to have a more positive view of themselves in general.
People with low self-esteem can have a difficult time setting boundaries with others. They may feel guilty or fear that people will stop liking them if they try to establish or maintain a boundary.
A lack of healthy boundaries can create problems when others don't respect a person's space and time. The lack of respect not only adds to the person's stress levels but may also make them feel less valued.
Trying to Please Others
People-pleasing is another common symptom of low self-esteem. In order to gain external validation, people who don't feel good about themselves may go above and beyond to make sure that others are comfortable and happy.
Pleasing others often involves neglecting their own needs. The person with low self-esteem winds up saying yes to things they may not want to do and feeling guilty about saying no.
Impact of Low Self-Esteem
Research suggests that there are numerous effects of low self-esteem. For instance, having lower levels of self-esteem is linked to a number of mental health issues, including:
- Eating disorders
- Emotional distress
- Internet addiction
- Panic disorder
- Risky behaviors
- Social anxiety disorder
- Substance use
Low self-esteem may even play a role in the development of certain mental health conditions, such as depression . Research has also shown that people with low self-esteem are more likely to be at risk for suicidal thinking.
If you are having suicidal thoughts, contact the National Suicide Prevention Lifeline at 988 for support and assistance from a trained counselor. If you or a loved one are in immediate danger, call 911.
For more mental health resources, see our National Helpline Database .
Another effect of low self-esteem is that you may find it more difficult to achieve your goals and form healthy, supportive relationships. It might also make you more sensitive to criticism or rejection.
Where someone with high self-esteem is likely to be able to shake off negative feedback, someone with poor self-value might take it more personally. This can also make people with self-esteem issues more likely to give up when faced with challenges or obstacles.
Research has found that people with low self-esteem often engage in behaviors that are designed to help preserve their limited self-worth. Actions such as acting sad or sulking are used to garner support from others.
Unfortunately, these behaviors tend to backfire. Instead of getting the support and encouragement they desire to help boost their self-esteem, the person often ends up generating negative reactions from other people.
Causes of Low Self-Esteem
What causes lower self-esteem in some individuals? Several factors could be at play, some of which include:
- Brooding, or being pre-occupied with dark or sad memories or thoughts
- Engaging in negative self-talk or self-criticism
- Having a mental health disorder
- Low levels of resilience
- Maladaptive coping skills
- Rumination , or obsessively thinking about one thing
Some studies connect high amounts of social media use with lower self-esteem in adolescents. However, others warn that social media use, in general, doesn't always have this effect. Instead, it's more a matter of the purpose behind its use.
Specifically, social media can have negative effects if it is used as a way to measure your popularity or likeability. But if you use social media to share your interests with like-minded individuals, its impact can be more positive.
Physical health and appearance are additional factors contributing to low self-esteem. For instance, one study found that having missing teeth or untreated dental decay negatively contribute to self-esteem.
Low self-esteem often stems from many causes. Five common factors that play a role include negative self-talk, mental health disorders, poor coping skills, rumination, and low resilience to stress.
Coping With Low Self-Esteem
Building or fixing low self-esteem often takes time. But there are things you can do to help protect your mental well-being while taking steps to improve your self-regard.
Focus on Hopeful Thoughts
Spend a little time each day focusing on positive, hopeful thoughts . Notice the little things that you are good at and allow yourself to feel proud of them.
Also, think about times in the past when you made it through something really difficult. Remind yourself that even though you might not feel your best right now, you have the ability and strength to get through it.
Care for Yourself
Poor self-esteem can sometimes leave you feeling like you don’t deserve care and consideration. Work on reminding yourself that you need care and look for things that you can do to show kindness to yourself, no matter how small they may be.
One way to practice self-care is to spend some time doing something that you enjoy. Go for a walk, chat with a friend, or engage in a hobby. Caring for yourself also involves regularly making time to rest and relax, giving your body and mind time to recoup and regroup.
Investing in your own care and comfort isn’t an indulgence or reward you have to earn—it’s absolutely vital to both your physical and mental health.
Get Outside Support
If you have low self-esteem, it can be helpful to share your struggles with someone who offers unconditional support. This might be a friend or family member, but it can also be a healthcare provider, therapist, teacher, or clergy member.
Having a network of caring people who value you and want you to value yourself can be beneficial as you work toward improving your self-esteem.
How to Build Self-Esteem
If you are dealing with low self-esteem, there are several things you can do to help improve how you feel about yourself.
How to Fix Low Self-Esteem
- Think positively
- Treat yourself well
- Practice self-acceptance and forgiveness
- Get support from friends and loved ones
- Do things that bring you joy
- Feel good about your achievements and progress
- Actively challenge negative thoughts and self-criticism
Notice Your Thoughts
Start paying attention to the automatic negative thoughts you have each day. When these negative thoughts take hold, work to actively identify cognitive distortions , such as all-or-nothing thinking and jumping to conclusions. Then, replace these distortions with more positive thoughts.
Forgive Yourself
If you tend to ruminate over your mistakes or failures, learn how to forgive yourself and move on. Doing so can keep you focused on the things you can do better in the future instead of the negative things that have happened in the past.
Practice Self-Acceptance
Let go of the idea that you need to be perfect in order to have value. If this is how you feel, it can be helpful to work on accepting who you are today.
Self-acceptance doesn't mean that you don't have goals or things that you might want to work on changing. But it's important to recognize that you are worthy of love and esteem—from yourself and from others—exactly as you are right now.
Value Yourself
Spend time thinking about the things you have accomplished and the things you are proud of. Allow yourself to appreciate your worth and your talents without making comparisons or focusing on areas you'd like to improve.
You don’t need to be better in order to value yourself—but learning to value yourself can help you work toward your goals.
It can be helpful to think of yourself as you would a friend. How would you treat someone you care about who was in the same situation? In many cases, you may find that you would give them understanding, patience, empathy , and kindness. Show yourself the same unconditional support instead of beating yourself up.
Additional Ways to Increase Low Self-Esteem
Here are a few additional things you can do to help boost your self-esteem:
- Do something that makes you feel good.
- Stay physically active— exercise can help improve mood.
- Think about something you are good at.
- Keep a gratitude journal .
- Challenge negative thoughts.
- Spend time with people who make you feel good about yourself.
- Volunteer to help others.
- Remember that everyone makes mistakes.
- Celebrate your accomplishments, both the big and the small achievements.
Keep in Mind
Self-esteem plays an important role in your ability to pursue goals, develop healthy relationships , and feel good about who you are. While everyone struggles with their confidence once in a while, low self-esteem can affect your ability to feel happy. It can even make you more susceptible to mental health conditions such as anxiety and depression.
If you are experiencing symptoms of poor self-esteem, help is available. Consider talking to a healthcare provider or mental health professional to learn your treatment options. A therapist can help you change the thought patterns that contribute to low self-esteem and boost your confidence and opinion of yourself and your abilities.
Raising your self-esteem may take some time and effort. But over time, you can learn to better see and appreciate yourself for who you are.
Bayat B, Akbarisomar N, Tori NA, Salehiniya H. The relation between self-confidence and risk-taking among the students . J Educ Health Promot . 2019;8:27. doi:10.4103/jehp.jehp_174_18
Goette L, Bendahan S, Thorensen J, Hollis F, Sandi C. Stress pulls us apart: Anxiety leads to differences in competitive confidence under stress . Psychoneuroendocrinol . 2015;54:115-123. doi:10.1016/j.psyneuen.2015.01.019
Gabriel AS, Erickson RJ, Diefendorff JM, Krantz D. When does feeling in control benefit well-being? The boundary conditions of identity commitment and self-esteem . J Vocation Behav . 2020;119:103415. doi:10.1016/j.jvb.2020.103415
Vogel EA, Rose JP, Roberts LR, Eckles K. Social comparison, social media, and self-esteem . Psychol Pop Media Culture . 2014;3:206–222. doi:10.1037/ppm0000047
Wang JL, Wang HZ, Gaskin J, Hawk S. The mediating roles of upward social comparison and self-esteem and the moderating role of social comparison orientation in the association between social networking site usage and subjective well-being . Front Psychol . 2017;8:771. doi:10.3389/fpsyg.2017.00771
Kille DR, Eibach RP, Wood JV, Holmes, JG. Who can't take a compliment? The role of construal level and self-esteem in accepting positive feedback from close others . J Experiment Soc Psychol . 2017;68:40-49. doi:10.1016/j.jesp.2016.05.003
Naseri L, Mohamadi J, Sayehmiri K, Azizpoor Y. Perceived social support, self-esteem, and internet addiction among students of Al-Zahra University, Tehran, Iran . Iran J Psychiatry Behav Sci . 2015;9(3):e421. doi:10.17795/ijpbs-421
Gartland D, Riggs E, Muyeen S, et al. What factors are associated with resilient outcomes in children exposed to social adversity? A systematic review . BMJ Open . 2019;9(4):e024870. doi:10.1136/bmjopen-2018-024870
Maldonado L, Huang Y, Chen R, Kasen S, Cohen P, Chen H. Impact of early adolescent anxiety disorders on self-esteem development from adolescence to young adulthood . J Adolesc Health . 2013;53(2):287-292. doi:10.1016/j.jadohealth.2013.02.025
Nguyen DT, Wright EP, Dedding C, Pham TT, Bunders J. Low self-esteem and its association with anxiety, depression, and suicidal ideation in Vietnamese secondary school students: A cross-sectional study . Front Psychiatry . 2019;10:698. doi:10.3389/fpsyt.2019.00698
Kalvin CB, Bierman KL, Gatzke-Kopp LM. Emotional Reactivity, Behavior Problems, and Social Adjustment at School Entry in a High-risk Sample . J Abnorm Child Psychol . 2016;44(8):1527-1541. doi:10.1007/s10802-016-0139-7
Don BP, Girme YU, Hammond MD. Low self-esteem predicts indirect support seeking and its relationship consequences in intimate relationships . Pers Soc Psychol Bull . 2019;45(7):1028-1041. doi:10.1177/0146167218802837
Hagen R, Havnen A, Hjemdal O, Ryum T, Solem S. Protective and vulnerability factors in self-esteem: The role of metacognitions, brooding, and resilience . Front Psychol . 2020;11:1447. doi:10.3389/fpsyg.2020.01447
Woods HC, Scott H. #Sleepyteens: Social media use in adolescence is associated with poor sleep quality, anxiety, depression and low self-esteem . J Adolescence . 2016;51:41-49. doi:10.1016/j.adolescence.2016.05.008
Pennsylvania State University. Social media and self-esteem .
Kaur P, Singh S, Mathur A, et al. Impact of dental disorders and its influence on self esteem levels among adolescents . J Clin Diagn Res . 2017;11(4):ZC05-ZC08. doi:10.7860/JCDR/2017/23362.9515
By Kendra Cherry, MSEd Kendra Cherry, MS, is a psychosocial rehabilitation specialist, psychology educator, and author of the "Everything Psychology Book."

Students Experiencing Low Self-esteem or Low Perceptions of Competence

This information is designed to help teachers respond to students who may need support. It is not intended to be used as a diagnostic tool or to replace the use of formal assessments employed by mental health professionals. Additionally, it is important to consider the context of the situation, individual differences, and cultural and linguistic considerations.
Teachers are an important part of establishing and maintaining healthy environments for children to learn and grow. Teachers can help students who are not confident in themselves or who are afraid to make a mistake to build their feelings of confidence. Teachers can also play an important role in referring students experiencing low self-esteem to professionals in the building who can be of assistance.
Download this Primer
More Primers
What is Self-esteem?
Self-esteem is the degree to which students feel satisfied with themselves and feel valuable and worthy of respect.
Perceived competence is a belief that one has skills in a particular area (e.g., math, spelling, peer relationships). Self-esteem and perceived competence are necessary for students to take risks in their learning and to bounce back after failure or adversity. Low self-esteem or lack of confidence leaves students doubting their ability to succeed, making them hesitant to engage in learning or take appropriate academic growth risks. Self-esteem is often built and buttressed through estimable acts and achievements—even small ones.
How Might Low Self-esteem Be Expressed by Students in School?
Students may make self-disparaging comments such as, “I’m stupid,” “I can’t do this,” “I always do everything wrong,” “No one likes me,” etc.
Students with low self-esteem may take blame for things that are not their fault or are out of their control, or they may try to control other children’s behavior to alleviate a sense of helplessness.
Students may react to adversity by giving up, avoiding risks, or disengaging from tasks, or turning off their cameras during virtual learning (VL).
Students may be reluctant to try new things or be unable to tolerate typical levels of frustration. They also may pretend they don’t care, may clown around, or may be aggressive to cover up their lack of confidence, or log off from the virtual learning environment (VLE) abruptly.
Students may do very well for a period of time, then suddenly underperform.
Students may be afraid their success was a fluke or be worried that expectations from others are suddenly too high.
What Can Teachers Do?
Do : Give specific and genuine positive feedback on effort rather than outcome, when warranted. For example, “You made a lot of progress on that project in just an hour,” or, “The topic sentence of that paragraph is really strong.”
Don’t praise excessively or vaguely or provide generic praise like, “Good job.”
Do : Point out concrete signs of progress, even if they are small.
Don’t give repeated, general pep talks that include, “You can do it!”
Do : Showcase accomplishments by displaying students’ work in class or calling parents to tell them how proud you are of the students’ efforts.
Don’t focus solely on suboptimal behaviors or performance.
Do : Engage students in a conversation about their interests, and point out students’ skills privately.
Don’t address the behavior publicly or assume a student is just like other students.
Do : Engage the students’ interests by setting them up for success: give them specific tasks at which they will excel, such as caring for the class pet or running things to the front office. In a VLE, this may look like choosing music for the virtual classroom, posting a math question on the discussion board, or reflecting on their strengths on a particular assignment with a peer in a breakout.
Don't ignore or avoid the students or the issues they’re facing or assume they aren’t up to a task.
Do : Be mindful of ensuring equity in terms of acknowledging and providing positive feedback to all students.
Don't continually affirm certain/the same students or compare achievements between students.
Do : Remember that students transitioning from the classroom to VLE, or vice versa, may experience different levels of success depending on the environment.
Don't base feedback upon historical achievements, expectations, or successes; the transition between learning environments impacts many students.
When to Act
- If the student continues to exhibit a significant shift in behavior occurring over several weeks, or the frequency or severity increases, seek extra support from administration or school mental health professionals.
- If the student displays similar patterns of behavior with other subject teachers.
- If you have concerns about the student engaging in self-harming behaviors.
Refer Students to Further Help if Needed
- Be sure to follow relevant school and district policies regarding students experiencing inattention and distractibility in school.
- Contact school counselors, psychologists, social workers, and other mental health or relevant personnel.
- American Psychological Association Topics
- Using Praise to Enhance Student Resilience and Learning Outcomes
- Maximizing children’s resilience
- Building Self-Esteem
- Being Me: A Kid’s Guide to Boosting Confidence and Self-Esteem
- I Want Your Moo: A Story for Children About Self-Esteem, Second Edition
- Institute of Education Sciences Research-Based Strategies for Effective Remote Learning
Related Mental Health Primers
Stress , sadness , bullying
Empirical Research
Beghetto, R. A. (2007). Factors associated with middle and secondary students' perceived science competence. Journal of Research in Science Teaching: The Official Journal of the National Association for Research in Science Teaching, 44 (6), 800-814.
Guay, F., Boggiano, A.K., & Vallerand, R.J. (2001). Autonomy support, intrinsic motivation, and perceived competence: Conceptual and empirical linkages. Personality and Social Psychology Bulletin, 27 , 643-650.
Kamins, M. & Dweck, C.S. (1999). Person vs. process praise and criticism: Implications for contingent self-worth and coping. Developmental Psychology , 35, 835-847.
Pesu, L., Viljaranta, J., & Aunola, K. (2016). The role of parents’ and teachers’ beliefs in children’s self-concept development. Journal of Applied Developmental Psychology, 44, 63-71.
Zentall, S. R., & Morris, B. J. (2010). "Good job, you're so smart": The effects of inconsistency of praise type on young children's motivation. Journal of Experimental Psychology, 107 (2), 155-163.
The Mental Health Primers are developed by the Coalition for Psychology in Schools and Education . This resource was updated in October 2021 with support from cooperative agreement NU87PS004366 funded by the Centers for Disease Control and Prevention (CDC). Its contents are solely the responsibility of the authors and do not necessarily represent the official views or endorsement of the CDC or the Department of Health and Human Services.
- Teaching and Learning Evidence-based Resources
- Science, Technology, Engineering and Mathematics Education
- Gifted and Talented Development
- APA Pre-K to 12 Education Advocacy
Academia.edu no longer supports Internet Explorer.
To browse Academia.edu and the wider internet faster and more securely, please take a few seconds to upgrade your browser .
Enter the email address you signed up with and we'll email you a reset link.
- We're Hiring!
- Help Center

The Impact of Lack of Self Confidence When Performing Oral Assignments For EFL Junior Students

2018, Sabratha University
Abstract The study was designed to examine the impact of lack of self-confidence when EFL junior students perform their oral assignments during their academic career. The participants of this study are eight students at the third year in the English Department of Sabratha College of Arts, Libya. A semi-structured interview is used as an instrument to collect the data in this study. The research is aimed to investigate the impact of lack of self-confidence for EFL junior students while they are delivering their oral assignments. After interviewing participants and analyzing the acquired data, researchers found out that lack of self-confidence has a negative impact on EFL junior students at and that due to psychological and linguistic barriers which prevented them from accomplishing good oral assignments. Keywords: Self-confidence, Oral assignment, self-confidence deficiency
Related Papers
JEELS (Journal of English Education and Linguistics Studies)
JEELS (Journal of English Education and Linguistics Studies) , Agus Salim
In speaking course, the teachers usually ask the students to present their projects in front of the class through an activity called Oral Presentation. However, many of students are afraid of public speaking due to the effect of self-confidence. This study is aimed to (1) describe general self-confidence among Indonesian EFL learners, (2) describe their academic achievement in oral presentation, and (3) find out the relationship between self-confidence and their academic achievement in oral presentation. Correlational design is used to investigate the existence or non existence of the relationship between the variables. The subjects of this study are 68 students at the second semester in English Department of one private university in Lamongan, Indonesia. Documentation and questionnaire are used as instruments to collect the data in this study. The findings reveal that (1) the students' general self-confidence is quite strong, (2) the students' academic achievement in the oral presentation is good, and (3) the two variables show high correlation. Therefore, the teachers are suggested to enforce activities that could increase students' self-confidence which in turn could decrease their anxiety in public speaking.
Amalia Hasanah
The aims of this study were to investigate whether there is a correlation between Self-Confidence with EFL students’ speaking achievement. The participants of this study were the Undergraduate EFL Students of UIN Raden Fatah Palembang. purpose. The participants that were chosen can meet certain criteria from this study. In this study, the student’s self-confidence and their speaking achievement are correlated. Therefore, in order to know the students’ speaking achievement, a group of students who had already taken the informal speaking courses from the population were considered as the sample. Nonetheless, most of the third semester students have already finished the informal speaking class on last semester and they are on the next level of speaking class on this semester. Quantitative method was used in this study. The data gained from self-confidence questionnaire and the list of students’ speaking achievement was analyzed by using SPSS. The result of the study showed that there i...
dinda mucus
The study was particularly aim an investigating the correlation between self confidence and academic achievement in speaking skill. The participants were 20 pairs freshmen undergraduate students from Kanjuruhan University of Malang. SPSS was used to analyze the data from self Confidence questionnaires and compared to the final score of speaking skill. The result of the computation revealed a negative, significant correlation between self confidence and academic achievement in speaking skill. Finally, it presented that the evidences found in the field of study fail to reject the Null Hypothesis. INTRODUCTION In learning second language, some people make faster progress than some others do. Some students try hard and get many difficulties. They seem stuck on something that make them really hard to reach the learning goal. They make struggle along the learning and get only very slow progress. It is clearly when someone learn a new language, they will have factors that contribute to the success of language learning. Learning is a process that involve in it, not only cognitive factors but also affective factors. The researcher realizes that cognitive factors are easy to show while affective factors are difficult to describe scientifically. But it does not mean that the affective factors give less contribution than the cognitive do. Cognitive factors defined as the something immaterial as the circumstance or influence that contributes to producing a result. Cognitive factors refer to characteristics of the person that affect performance and learning. In this way, cognition has to do with how the world will be understood by a person and act in it. Messick's (1993: 199) says that cognitive styles are characteristic modes of perceiving, remembering, thinking, problem solving, decision making that are reflective of information processing regularities that develop in congenial ways. Affective factors defined as emotional factors which influence learning. They can have a negative or positive effect. Because affective factors also produce negative effects, the lecturers or the instructors in the classroom should build the learning atmosphere to decrease the negative effects. These factors involve cognitive functions like attention, memory, and reasoning (Danili & Reid, 2006). Thus, from those affective factors we know, learning foreign language is not a simple thing to do. It is a complex process when a learner speaks language which is not spoken in his mother tongue. Learner will get some obstacles and difficulty to do. As Bialystok, E. (1991) suggests that Language learning is a complex process. That affective factors play important role, it should contribute to the progress of learning. Some of those affective factors clearly mentioned by Brown (2000) He says that the affective domain is the emotional side of human behavior and it involve a variety of
Nutin Nasih
Abstract: Speaking is a productive skill which leads the ones have an effective communication. Then, Self-confidence is a psychological factor which plays a supportive role in speaking performance. The current study was aimed to know whether there is a significant correlation between self-confidence and speaking performance. The researcher used quantitative approach in which correlation research design was used. The total number of participants was of 30 students from the fourth semester of English Department. To obtain the data, the researcher used Confidence in Speaking English as a Foreign Language (CSEFL) questionnaire in order to know the students’ level of self-confidence and speaking performance score was used to measure the level of the students speaking performance. The finding of the present study showed that the r observed of the students’ self-confidence and speaking performance was .261 with level of significance was .163 which is greater than .05. It means that the co...
Omidullah Akbari
The purpose of this study was to measure students' self-confidence and finds its impacts on their learning process at Kandahar University. The study is descriptive in nature where quantitative questionnaire is used to collect data through stratified sampling from 1375 male and female students. The findings revealed only some of the students were low self-confident and most students were highly self-confident. In addition, students' self-confidence effected their learning in areas of students' participation, in seeking goal, developing interest in lessons, in decreasing students' anxiety, they are being comfortable with their instructors and classmates and also in sharing their opinions related to lessons in class.
Journal of General Education and Humanities
Journal of General Education and Humanities (GEHU)
Self-confidence plays a crucial part in speaking English, and many students are still less confident when speaking, which causes them to not engage more in speaking activities. This research aimed to know how self-confidence works in students speaking to ninth-grade students, specifically at SMP Negeri 9 Palu, and the factors that contributed to their lack of confidence. For the topic, 30 students were selected as the sample and given twelve questions from the questionnaire and five interview questions. The research method was a descriptive qualitative method. The results that the researcher has done are self - confidence indeed works on students’ speaking. Students’ lack of confidence is caused by some factors, which are afraid of making mistakes when they speak, they still have lack of vocabulary, lack of grammar, feel of under pressure every time the teacher asks them to speak, shyness, nervous, feel of uncomfortable, not enjoying when they attempt to speak, insecurities of their friends who have the good ability more than them. This study is expected to contribute to developing students’ speaking ability and solve students’ problems by knowing their speaking and what factors contribute to their unconfident. Moreover, this study also may help teachers treat students so they can participate actively in class without being constrained with self–confidence.
Dawood A Mahdi
This article is concerned with strategies and techniques for fostering EFL students " confidence and reducing their oral communication apprehension. This paper aims to explore strategies and techniques that could be implemented in the EFL classroom to encourage students " oral communication and foster their confidence. The first part starts with a brief introduction to present the research topic. It states the aims, purpose, research questions, and significance of the study. The second part features the relevant literature review, focusing on the current body of knowledge. The literature review provides a detailed description of the substantive findings as well as methodological and theoretical contributions to this topic. The study furnishes a wide range of reflections on English as a foreign language, and the special needs of students learning the language. It can be described as the impact of confidence on EFL students " oral communication apprehension in EFL students. In the third part, the paper discusses the methodology used in this study, followed by a discussion of an analysis of the findings in the fourth part. These two areas, i.e. discussion and findings answer the research questions and justify the research hypothesis. The last part of this work provides a conclusion to the study, accompanied by some recommendations.
Ismail Gurler
Abstract Self-confidence has a key characteristics to start any action especially for speaking in L2. Among all other language skills, speaking is of an exclusive place to have effective communication, and self-confidence is one of the facilitators to start conversation. In this regard, this study aims to find out whether there is a relationship between self-confidence and speaking skill achievement in speaking courses of the preparatory students attending both English Language Teaching (ELT) Department and English Language and Literature (ELL) Department and it also aims to determine if there is a difference between the departments and gender. Participants were 77 male and female preparatory students from both departments and all the students got English speaking courses throughout the fall semester in 2014-2015 academic year. Within a correlational research model, self-confidence questionnaire (SCQ) was applied to the participants. The collected quantitative data were analyzed by Statistical Package for the Social Sciences (SPSS) 20.0 program. The Pearson product-moment correlation coefficient and independent sample t-test were used to analyze the data. Results indicate that there is significant correlation between self-confidence and speaking skill within the level of .01. Moreover, speaking achievements reveal significant differences according to department but not gender. Self-confidence levels have significant differences regarding to the gender but not department.
Acuity: Journal of English Language Pedagogy, Literature and Culture
Marlin Marpaung
English Education Journal
Asti Wahyuni B
This research intended to analyze factors of students’ lack of self confidence in speaking English. It was also aimed to present possible strategies used to overcome students’ lack of self confidence in speaking English. The type of this research was qualitative. This research was conducted in SMA Negeri 4 BauBau. This research focused on obtaining data from the English teacher and students at eleventh grade of SMA Negeri 4 BauBau in the academic year 2018/2019 as the subjects of the research. In collecting data, the researchers used observation, interview. The technique used in analyzing data were three steps, those were data reduction, data display, and conclusion drawing. The result of this research showed that the factors which cause students’ lack of self confidence were anxiety, shyness, fear of making mistakes, and lack of vocabulary. Meanwhile, the possible strtaegies to overcome students’ lack of self confidence in speaking English were lowering students’ anxiety in classro...
Loading Preview
Sorry, preview is currently unavailable. You can download the paper by clicking the button above.
RELATED PAPERS
AL-ISHLAH: Jurnal Pendidikan
balqis husain
Frida Alifah
Rusdiana Junaid
Morteza Bakhtiarvand , Farshad Mahnegar
Kimberly K V Vipinosa
Norma Murga
Efi Kurniati
Fahimeeh Aleabbass
Psychology and Education: A Multidisciplinary Journal
Psychology and Education , Nicole gawan , Crisalyn R. Montoyo , Quirr Millendez
Tono SUWARTONO
Australian International Academic Centre PTY. LTD. (AIAC PTY.LTD.)
Listyani Listyani
MANI SAMIDURAI
Badran A Hassan
Hengki hengki
Ariyanti Ariyanti
ASIAN TEFL , Ariyanti Ariyanti
JES Journal 14. 84-99
Adrian Leis
Self-Esteem, Self-Expectancy and Oral Achievement in the Tunisian EFL Context: Multiple Perspectives
Marwa Mekni Toujani
COMSERVA Indonesian Jurnal of Community Services and Development
fitri alfarisy
Şakire Erbay Çetinkaya
Elaheh Tavakoli
Research Article
Asst. Prof. Dr. Budi Waluyo, FHEA
International Journal for Innovative research in Multidiciplinary Field
Abdullah Rahimi
International Journal of Research and Innovation in Social Science
RELATED TOPICS
- We're Hiring!
- Help Center
- Find new research papers in:
- Health Sciences
- Earth Sciences
- Cognitive Science
- Mathematics
- Computer Science
- Academia ©2024
- Open access
- Published: 03 September 2024
Navigating the skies: a cross-sectional study of depression among Saudi Arabian airline pilots
- Sarah AlMuammar 1 ,
- Rahaf Alkhaldi 1 ,
- Roaa Alsharif 1 ,
- Daniah Allbdi 1 ,
- Mashael Alasmari 1 ,
- Bashair Alasmari 1 ,
- Afaf Alkhaldi 1 ,
- Refaal Aldealij 1 &
- Nabeela Ismail 1
Journal of Occupational Medicine and Toxicology volume 19 , Article number: 36 ( 2024 ) Cite this article
Metrics details
Depression poses a significant challenge globally, including in safety-critical industries such as aviation. In Saudi Arabia, where the aviation sector is rapidly expanding, pilots encounter unique stressors inherent to their profession. However, research on pilot mental health, particularly within the Saudi context, remains limited despite its critical role in flight safety.
This cross-sectional survey was designed to estimate the self-reported prevalence of depression in a convenience sample of airline pilots in Saudi Arabia. Participants were recruited from various commercial airlines in Saudi Arabia. Recruitment efforts utilized targeted outreach on social media platforms, focusing on pilot forums and groups. The survey was administered online for accessibility and convenience. The structured questionnaire, developed through a literature review and expert consultation, comprises sections on demographic and professional characteristics, occupational information, health habits, and depression assessment via the Patient Health Questionnaire-9 (PHQ-9).
This study enrolled 310 participants, with the largest cohort (34.8%, n = 108) falling within the 30–39 years age group, closely followed by individuals under 30 years (30.0%, n = 93). Males dominated the sex distribution (99.0%, n = 307). The mean PHQ-9 score was 8.2 ± 5.4. Notably, 40.6% ( n = 126) of the participants had a score of 10 or higher, indicating the potential for moderate, moderate-severe, or severe depression. Multivariable binary logistic regression analysis revealed that pilots with 11–15 years of experience had greater odds of experiencing depression than did those with 0–10 years of experience did (odds ratio [OR]: 3.0, 95% confidence interval [CI]: [1.1–8.4], p = 0.04). Pilots with rest times exceeding 24 h had lower odds of depression than did those with rest times less than 1 h (OR: 0.3, 95% CI: [0.1–0.8], p = 0.02). Engaging in regular exercise was associated with reduced odds of depression (OR: 0.3, 95% CI: [0.2–0.5], p < 0.01), as was longer sleep duration (> 8 h) (OR: 0.2, 95% CI: [0.1–1.0], p = 0.04).
Our study estimates the prevalence and severity of self-reported depressive symptoms among airline pilots in Saudi Arabia, surpassing global estimates. The identified factors, including lack of regular exercise, short sleep duration, and insufficient rest between flights, underscore the complex mental health challenges faced by pilots in this region. Addressing these issues is crucial not only for pilot well-being but also for flight safety.
Depression is a pervasive mental health disorder with profound implications for individuals, communities, and societies worldwide, representing a leading cause of disability and contributing significantly to the global burden of disease [ 1 ]. Its impact spans diverse populations and professions, drawing particular attention to its ramifications within safety-critical industries [ 2 ].
The aviation sector serves as a cornerstone of modern transportation systems, facilitating global connectivity and economic growth. In Saudi Arabia, a country experiencing rapid growth in its aviation sector, pilots play a crucial role in ensuring the safety of air travel. However, operating within the aviation industry entails a complex and demanding environment characterized by irregular working hours, long flights, time zone changes, and extended periods away from home [ 3 , 4 , 5 ]. These factors can disrupt circadian rhythms, exacerbate sleep disturbances, and contribute to chronic fatigue, which are recognized risk factors for depression [ 6 , 7 ].
Pilots are exposed to various physical stressors, including cosmic radiation and electromagnetic fields, which may increase their cancer risk. Chemical stressors, such as pollutants from jet fuels and aircraft materials, can impact air quality. Additionally, the associated biological risks include exposure to foodborne pathogens and airborne microorganisms, further complicating health management. Environmental factors such as acceleration forces, hypoxia, and noise also pose significant health risks [ 8 , 9 ].
Research on pilot mental health has garnered increasing attention in recent years because of its profound implications for flight safety. The mental well-being of pilots is crucial because it directly affects their cognitive function, decision-making ability, situational awareness, and overall performance during flight operations, thereby compromising flight safety [ 10 ].
Limited research has been conducted on mental health disorders among commercial pilots globally. A systematic review by Terouz et al. [ 11 ] in 2018 included 20 studies, shedding light on the prevalence and types of mental health challenges faced by commercial airline pilots. The review revealed a wide range of depression prevalence rates, ranging from 1.9 to 12.6%. The study also identified various contributing factors to pilots’ mental health challenges, including substance abuse, exposure to verbal or sexual abuse, disrupted sleep patterns, and chronic fatigue. However, none of the studies included in the review were conducted in Saudi Arabia or the broader Middle East region, indicating a significant research gap within this specific geographical context.
Understanding the unique challenges shaping pilot mental health in Saudi Arabia is crucial not only for ensuring the well-being of these individuals but also for safeguarding the safety of air travel passengers and crews. This study aimed to address this knowledge gap by requesting self-reported data on depressive symptom prevalence and severity in a convenience sample of pilots in Saudi Arabia.
Study design and settings
This cross-sectional survey was designed to estimate the self-reported prevalence of depression in a convenience sample of airline pilots in Saudi Arabia and identify associated demographic, occupational, and health behavior factors.
In Saudi Arabia, the General Authority of Civil Aviation (GACA) is responsible for establishing and overseeing health surveillance protocols for pilots. Saudi aviation medical examiners conduct thorough evaluations during mandatory occupational health visits. These examinations are typically performed at least annually for medical certification [ 12 ].
Study participants
Participants were recruited from various commercial airlines in Saudi Arabia. The inclusion criterion included active pilots. Pilots were recruited through targeted outreach on social media platforms, with a focus on pilot forums and groups to ensure diverse representations. Referrals within professional networks were encouraged, and no incentives were provided for referrals to maintain voluntary participation. Approximately 500 pilots were estimated to be targeted for recruitment.
Survey administration
To ensure accessibility and convenience, the questionnaire was administered online. A survey link was disseminated through social media platforms, including LinkedIn, Twitter, and Facebook, allowing diverse types of participation. This mode accommodates pilots’ busy schedules, with an estimated completion time of 7 min. The data were collected over 6 weeks, from August 1, 2023, to September 12, 2023.
Questionnaire development
A structured questionnaire was developed through a literature review and expert consultation. The questionnaire comprises sections on demographic and professional characteristics, occupational information, health habits, and the Patient Health Questionnaire-9 (PHQ-9) questionnaire for depression assessment [ 13 ]. Prior to the main study, the questionnaire underwent preliminary testing through a pilot study involving 20 participants to ensure its clarity, relevance, and comprehensiveness.
Content of questionnaire
Exposure variables.
The questionnaire covered various demographic variables, such as age group (< 30 years, 30–39 years, 40–49 years, ≥ 50 years), sex (male or female), marital status (single, married, divorced), self-reported weight (kg), height (cm), and the presence of chronic disease. Occupational information included position (captain or senior officer), years of experience, total flying hours (< 3,000, 3,000–5,000, 5,000–10,000, > 10,000), flying hours in the past year (< 500, 500–700, > 700), rest time between flights (< 1 h, 1–4 h, 4–24 h, > 24 h), and flight route duration (< 6 h, 6–12 h, > 12 h). The health behavior habit questions included whether the participant engaged in regular exercise, defined as exercising at least 3 times per week, exercise intensity (low, moderate, or high), smoking status (nonsmoker or smoker), and sleep duration (< 5 h, 5–8 h, or > 8 h). The survey questionnaire also included a section about musculoskeletal complaints, which were reported separately.
Outcome variables
Depression severity was assessed via the PHQ-9 questionnaire, which categorizes scores into different severity levels. The PHQ-9 scores were categorized into five distinct severity levels: minimal depression (scores ranging from 0 to 4), mild depression (scores between 5 and 9), moderate depression (scores ranging from 10 to 14), moderately severe depression (scores ranging from 15 to 19), and severe depression (scores falling within the range of 20–27). The cutoff point for significant depression on the PHQ-9 questionnaire was defined as a score of 10 or higher, indicating the presence of moderate to severe depressive symptoms requiring clinical attention [ 13 ]. The primary outcome was the prevalence of depression among pilots. The secondary outcomes included associations between depression and demographic, occupational, and health behavior factors.
Statistical analysis
The data were analyzed via IBM SPSS Statistics version 26 (IBM Corp., Armonk, NY, USA). The chi-square test was used for comparisons between variables. Multivariable logistic regression analysis was conducted to identify independent factors associated with depression, with odds ratios (ORs) and 95% confidence intervals (CIs) estimated. All p values were calculated via two-tailed tests with an alpha level of 0.05.
To assess the potential confounding effects of age on the relationships between flying hours, years of experience, and depression, a sensitivity analysis was performed. This analysis included interaction terms between age groups and years of experience to explore whether age influenced these relationships. The results of the sensitivity analysis revealed no significant interactions, indicating that age did not substantially confound the associations between flying hours, years of experience, and depression.
Ethical considerations
Ethical approval was obtained from the Ethics Committee of King Abdulaziz University. Informed consent was obtained, ensuring voluntary participation and confidentiality. Stringent data privacy and security measures were implemented to uphold ethical standards. The participants were informed that the survey was not a diagnostic tool and encouraged them to consult their healthcare provider if they were concerned about their mental health.
Demographic characteristics of the participants
The study included 310 participants. The largest cohort comprised 34.8% (108 participants) of the 30–39 age group, closely followed by individuals under 30 years, constituting 30.0% (93 participants) of the sample. Males heavily dominated the sex distribution, representing 99.0% (307 participants) of the cohort. Marital status analysis revealed that 59.7% (185 individuals) were married. Regarding body mass index categories, the majority of participants were classified as normal (42.6%, 132 participants), followed by overweight (39.7%, 123 participants) and obese (17.1%, 53 participants) (Table 1 ).
Occupational characteristics of the participants
Occupationally, the distribution between captains and senior officers was fairly balanced, with senior officers slightly outnumbering captains at 54.5% (169 participants) and 45.5% (141 participants), respectively. The number of years of experience varied, with the majority (57.7%, 179 participants) having between 0 and 10 years of experience. Flying hours were diverse, with nearly half of the participants (47.7%, 148 participants) accumulating fewer than 3,000 flying hours. Approximately one-third of the participants (31.0%, 96 participants) logged less than 500 h in the past year. The remaining time between flights varied as well, with 49.0% of participants (152 individuals) having less than 1 h of rest, 21.9% (68 individuals) having 1–4 h, 18.7% (58 individuals) having 4–24 h, and 10.3% (32 individuals) having more than 24 h. The flight route duration data revealed that the majority of flights (65.5%, 203 participants) lasted less than 6 h, followed by 23.9% (74 participants) lasting more than 12 h and 10.6% (33 participants) lasting between 6 and 12 h (Table 1 ).
Participants’ health behaviors
Regarding the health habits of the participants, 194 participants (62.6%) identified as smokers. With respect to exercise, 158 participants (51.0%) engaged in physical activity regularly 3–5 times per week. The majority, 176 individuals (56.8%), reported exercising at a low intensity, whereas 86 participants (27.7%) exercised at a medium intensity. Additionally, 48 participants (15.5%) engaged in high-intensity exercise. The sleep duration among the participants varied, with 259 participants (83.5%) reporting a sleep duration of 5–8 h, 32 participants (10.3%) reporting more than 8 h, and 19 participants (6.1%) reporting less than 5 h (Fig. 1 ).
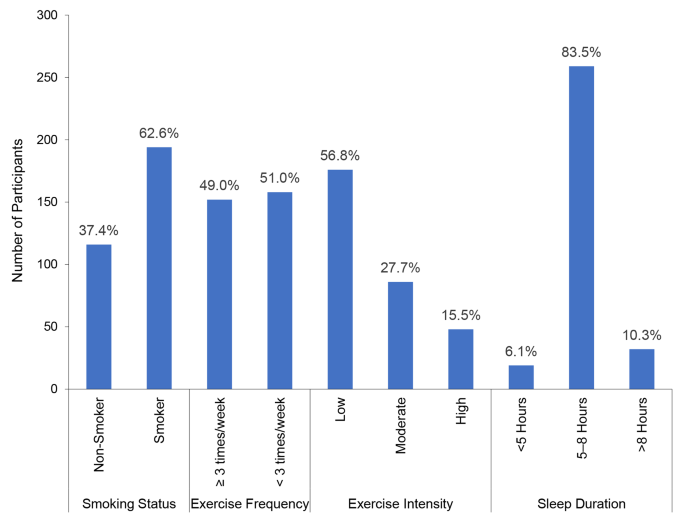
Health habits of the participants ( N = 310)
PHQ-9 score and depression severity
The mean PHQ-9 score among the study participants was 8.2 ± 5.4. Notably, 126 participants (40.6%) had a score of 10 or higher, indicating significant depression. Analysis of the PHQ-9 score distribution revealed that 88 participants (28.4%) exhibited minimal depression, 96 (31.0%) reported mild depression, 87 (28.1%) indicated moderate depression, 30 (9.7%) had moderately severe depression, and 9 (2.9%) had severe depression (Fig. 2 ).

Categorization of depression severity on the basis of PHQ-9 scores ( N = 310)
Associations with depression: bivariate analysis
Table 2 presents the bivariate associations of depression with demographic, occupational, and health behavior factors. A total of 59.0% of the pilots aged 40–49 years presented with depression, whereas 34.4% of those aged < 30 years presented with depression ( p = 0.01). In terms of occupational factors, pilots with 0–10 years of experience had a lower prevalence of depression than did those with 11–15 years of experience (35.8% vs. 58.1%, p = 0.03). Similarly, pilots with 3,000–5,000 and 5,000–10,000 flying hours presented greater proportions of depression than did those with fewer flying hours (< 3,000) (49.0% and 51.6% vs. 37.2%, respectively; p = 0.04). Additionally, pilots with shorter rest times between flights (< 1 h) had a greater prevalence of depression than did those with longer rest times of 24 h (48.0% vs. 21.9%, p = 0.03).
In examining the associations between health habits and the prevalence of moderate to severe depression among the study participants, several noteworthy patterns emerged. With respect to smoking status, no significant difference was observed between nonsmokers (37.9%, 44 individuals) and smokers (42.3%, 82 individuals) in terms of experiencing depression ( p = 0.45). However, a statistically significant association was found between regular exercise and depression status ( p < 0.01). The participants who engaged in regular exercise presented a lower prevalence of depression (27.8%, 44 individuals) than did those who did not (53.9%, 82 individuals). Those engaging in low-intensity exercise had a greater prevalence of depression (51.1%, 90 individuals), followed by individuals engaging in moderate-intensity exercise (26.7%, 23 individuals) and those engaging in high-intensity exercise (27.1%, 13 individuals). Additionally, sleep duration was significantly associated with depression ( p = 0.01). Individuals reporting less than 5 h of sleep had a greater prevalence of moderate to severe depression (42.1%, 8 individuals), whereas those reporting 5–8 h of sleep presented a slightly greater prevalence (43.3%, 113 individuals), and individuals reporting more than 8 h of sleep had a lower prevalence (15.6%, 5 individuals).
Associations with depression: multivariable analysis
Table 3 presents the findings from the multivariable analysis examining the relationships between various factors and depression among airline pilots. Notably, pilots with 11–15 years of experience had markedly greater odds of experiencing depression than did those with 0–10 years of experience (OR: 3.0, 95% CI: [1.1–8.4], p = 0.04). Additionally, pilots who had rest times between flights exceeding 24 h had significantly lower odds of depression than did those who had rest times less than 1 h (OR: 0.3, 95% CI: [0.1–0.8], p = 0.02). Furthermore, engaging in regular exercise was significantly associated with reduced odds of depression (OR: 0.3, 95% CI: [0.2–0.5], p < 0.01). Similarly, individuals with longer sleep durations (> 8 h) had a significantly lower likelihood of depression than did those with shorter sleep durations did (OR: 0.2, 95% CI: [0.1–1.0], p = 0.04).
The present study revealed an alarmingly high prevalence of depression among airline pilots, with 40.6% of the sample screening positive for depression via the PHQ-9. This figure is notably higher than the rates reported in previous studies, which range from 1.9 to 12.6% [ 11 , 14 ]. This substantial discrepancy raises important questions regarding the factors contributing to such elevated rates.
A key consideration is the screening tool used. Our study employed the PHQ-9, whereas other studies in the field have utilized different measures, including the Beck Depression Inventory-II (BDI-II) [ 10 ], Symptoms of Stress Questionnaire [ 15 ], Symptom Checklist 90 (SCL 90) [ 16 ], New Zealand Health Survey [ 17 ], and Self-Reporting Questionnaire-20 items (SRQ-20) [ 18 ]. The variation in tools across studies may partly account for differences in reported prevalence rates.
While it might be tempting to attribute this difference to the screening tool used—in our case, the PHQ-9—a deeper examination reveals that this explanation may not be sufficient. For example, Wu et al. [ 19 ] conducted a cross-sectional study focusing on mental health among airline pilots and utilized the PHQ-9. Their findings indicated that 12.6% of pilots met the depression threshold according to the PHQ-9 and that 4.1% reported suicidal thoughts within the past two weeks. A recent study by Minoretti et al. [ 14 ] investigated the impact of mild depressive symptoms on executive functions in airline pilots and revealed that 12% of the study population experienced mild depression according to the BDI-II. In fact, a previous study comparing the PHQ-9 and the BDI-II often categorized a greater proportion of participants with severe depression than did the PHQ-9.
Given this, the elevated depression rate observed in our study likely results from other factors. These could include unique characteristics of our sample, such as higher exposure to occupational stressors, fatigue, or other environmental and psychological factors specific to the airline pilot population in our country. In particular, occupational factors have emerged as significant contributors to the mental health outcomes of airline pilots in Saudi Arabia. Rest time between flights, in particular, has emerged as a critical determinant of mental health among pilots. Pilots with shorter intervals between flights demonstrated a greater prevalence of moderate to severe depression than did those with longer rest times exceeding 24 h. Sleep duration has emerged as another critical determinant of mental health among airline pilots. Sleep plays a pivotal role in regulating mood, cognitive function, and emotional stability [ 20 ]. Prolonged sleep deprivation can disrupt neurobiological processes, exacerbate stress responses, and increase vulnerability to mental health disorders [ 21 ]. Pilots who reported participating in regular physical activity presented lower prevalence rates of moderate to severe depression than did those who did not engage in regular exercise. It is unclear from our results whether those who exercised more frequently had fewer/milder depressive symptoms or whether those with more depressive symptoms felt less motivated to exercise.
Our findings reveal a concerning prevalence of depression among Saudi airline pilots. According to the GACA standards for Class 1 medical certification, pilots are disqualified if they have a history or clinical diagnosis of mood disorders, including clinical depression. The GACA guidelines explicitly state that mood disorders are grounds for disqualification [ 12 ]. The high prevalence of depression observed in our study raises questions about the fitness-to-fly licensing of pilots in Saudi Arabia. Given that pilots with severe depression may be at risk of disqualification under these standards, it is crucial to investigate whether affected pilots are being appropriately evaluated and treated. The reluctance to pursue treatment due to concerns about medical certification may result in pilots remaining untreated, potentially compromising their safety and performance. This issue underscores the need for a supportive framework that encourages pilots to seek help without fear of negative repercussions for their careers.
While our study provides valuable insights into the prevalence and correlates of depression among airline pilots in Saudi Arabia, several limitations should be acknowledged to contextualize the findings and guide future research endeavors. First, the cross-sectional nature of the survey design restricts our ability to establish causal relationships between variables. Although we can identify associations between certain factors and depression incidence, we cannot infer causation or temporal sequencing. Second, self-reporting biases may have influenced the accuracy and reliability of the data collected in our study. The participants may have underreported or overreported their symptoms of depression due to social desirability bias or recall errors. Third, the sampling strategy employed in our study may limit the generalizability of the results to the broader population of airline pilots in Saudi Arabia. Convenience sampling via online recruitment methods may have introduced selection bias, favoring participation among certain demographic groups or individuals with specific characteristics. Fourth, self-reported measures of depression relied upon the use of the PHQ-9. While the PHQ-9 is a validated screening tool for depression, it does not substitute for a comprehensive clinical evaluation conducted by trained mental health professionals. Finally, the questionnaire did not undergo formal validation, which should be considered a limitation of the study.
In conclusion, this study recruited pilots to self-report their depressive symptoms, and a greater percentage of the pilots experienced more severe symptoms than the authors expected on the basis of their background research. The identification of associated factors such as lack of regular exercise, short sleep duration, and inadequate rest between flights underscores the multifaceted nature of the mental health challenges faced by pilots in this region. Addressing these issues is paramount not only for safeguarding the well-being of pilots but also for ensuring flight safety. In the future, targeted interventions and policy initiatives should be implemented to promote mental health awareness, facilitate access to support services, and mitigate occupational stressors within the aviation industry. By prioritizing the mental well-being of pilots, stakeholders can contribute to a safer and healthier aviation environment for all.
Data availability
No datasets were generated or analysed during the current study.
Collaborators GBDMD. Global, regional, and national burden of 12 mental disorders in 204 countries and territories, 1990–2019: a systematic analysis for the global burden of Disease Study 2019. Lancet Psychiatry. 2022;9(2):137–50.
Article Google Scholar
Laditka JN, Laditka SB, Arif AA, Adeyemi OJ. Psychological distress is more common in some occupations and increases with job tenure: a thirty-seven year panel study in the United States. BMC Psychol. 2023;11(1):95.
Article PubMed PubMed Central Google Scholar
Aljurf TM, Olaish AH, BaHammam AS. Assessment of sleepiness, fatigue, and depression among Gulf Cooperation Council commercial airline pilots. Sleep Breath. 2018;22(2):411–9.
Article PubMed Google Scholar
O’Hagan AD, Issartel J, Nevill A, Warrington G. Flying Into Depression. Workplace Health Saf. 2017;65(3):109–17.
Venus M, Holtforth MG. Short and long Haul pilots rosters, stress, sleep problems, fatigue, Mental Health, and well-being. Aerosp Med Hum Perform. 2021;92(10):786–97.
Fang H, Tu S, Sheng J, Shao A. Depression in sleep disturbance: a review on a bidirectional relationship, mechanisms and treatment. J Cell Mol Med. 2019;23(4):2324–32.
Mendoza J. Circadian insights into the biology of depression: symptoms, treatments and animal models. Behav Brain Res. 2019;376:112186.
Kim JN, Lee BM. Risk factors, health risks, and risk management for aircraft personnel and frequent flyers. J Toxicol Environ Health B Crit Rev. 2007;10(3):223–34.
Article CAS PubMed Google Scholar
Minoretti P, Emanuele E. Health in the skies: a narrative review of the issues faced by Commercial Airline pilots. Cureus. 2023;15(4):e38000.
PubMed PubMed Central Google Scholar
Minoretti P, Santiago Sáez AS, García Martín ÁF, Liaño Riera M, Gómez Serrano M, Emanuele E. Mild depressive symptoms in Airline pilots Associated with impaired executive functions. Cureus. 2023;15(7):e41616.
Pasha T, Stokes PRA. Reflecting on the Germanwings Disaster: a systematic review of depression and suicide in Commercial Airline pilots. Front Psychiatry. 2018;9:86.
Aviation GAC. GACA Regulation: Sect. 1, Personnel Licensing. Edition 4.0. In. Kingdom of Saudi Arabia; 2014.
Kroenke K, Spitzer RL, Williams JB. The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med. 2001;16(9):606–13.
Article CAS PubMed PubMed Central Google Scholar
Minoretti P, Liaño Riera M, Gómez Serrano M, Santiago Sáez A. García Martín Á: brushing away the blues: self-reported oral Hygiene practices are Associated with mild depressive symptoms in Airline pilots. Cureus. 2024;16(5):e60695.
Little LF, Gaffney IC, Rosen KH, Bender MM. Corporate instability is related to airline pilots’ stress symptoms. Aviat Space Environ Med. 1990;61(11):977–82.
CAS PubMed Google Scholar
Widyahening IS. High level of work stressors increase the risk of mental-emotional disturbances among airline pilots. Med J Indonesia. 2007;16(2):117–21.
Sykes AJ, Larsen PD, Griffiths RF, Aldington S. A study of airline pilot morbidity. Aviat Space Environ Med. 2012;83(10):1001–5.
Feijó D, Luiz RR, Camara VM. Common mental disorders among civil aviation pilots. Aviat Space Environ Med. 2012;83(5):509–13.
Wu AC, Donnelly McLay D, Weisskopf MG, McNeely E, Betancourt TS, Allen JG. Airplane pilot mental health and suicidal thoughts: a cross-sectional descriptive study via anonymous web-based survey. Environ Health. 2016;15(1):121.
Vandekerckhove M, Wang YL. Emotion, emotion regulation and sleep: an intimate relationship. AIMS Neurosci. 2018;5(1):1–17.
Medic G, Wille M, Hemels ME. Short- and long-term health consequences of sleep disruption. Nat Sci Sleep. 2017;9:151–61.
Download references
Acknowledgements
We would like to thank AJE’s Curie platform for their assistance in preparing and reviewing this manuscript. Their support was invaluable in enhancing the clarity and quality of our work.
This research received no specific funding from any external source. All the authors contributed their time and resources voluntarily.
Author information
Authors and affiliations.
Family Medicine Department, Faculty of Medicine, King Abdulaziz University, Jeddah, Saudi Arabia
Sarah AlMuammar, Rahaf Alkhaldi, Roaa Alsharif, Daniah Allbdi, Mashael Alasmari, Bashair Alasmari, Afaf Alkhaldi, Refaal Aldealij & Nabeela Ismail
You can also search for this author in PubMed Google Scholar
Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Corresponding author
Correspondence to Sarah AlMuammar .
Ethics declarations
Ethics approval and informed consent.
The study was conducted in strict adherence to the principles outlined in the Declaration of Helsinki, with ethical clearance obtained from the Institutional Review Board at King Abdulaziz University. The informed consent process included a comprehensive explanation of the voluntary nature of participation, with a particular emphasis on measures taken to ensure the confidentiality of participant information.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/ .
Reprints and permissions
About this article
Cite this article.
AlMuammar, S., Alkhaldi, R., Alsharif, R. et al. Navigating the skies: a cross-sectional study of depression among Saudi Arabian airline pilots. J Occup Med Toxicol 19 , 36 (2024). https://doi.org/10.1186/s12995-024-00435-4
Download citation
Received : 04 May 2024
Accepted : 28 August 2024
Published : 03 September 2024
DOI : https://doi.org/10.1186/s12995-024-00435-4
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Airline pilots
- Occupational stress
- Mental health
- Saudi Arabia
- Sleep duration
- Flight safety
- Cross-sectional study
Journal of Occupational Medicine and Toxicology
ISSN: 1745-6673
- General enquiries: [email protected]
- Open access
- Published: 02 September 2024
Clinical supervisor’s experiences of peer group clinical supervision during COVID-19: a mixed methods study
- Owen Doody ORCID: orcid.org/0000-0002-3708-1647 1 ,
- Kathleen Markey ORCID: orcid.org/0000-0002-3024-0828 1 ,
- James Turner ORCID: orcid.org/0000-0002-8360-1420 2 ,
- Claire O. Donnell ORCID: orcid.org/0000-0003-2386-7048 1 &
- Louise Murphy ORCID: orcid.org/0000-0003-2381-3963 1
BMC Nursing volume 23 , Article number: 612 ( 2024 ) Cite this article
Metrics details
Providing positive and supportive environments for nurses and midwives working in ever-changing and complex healthcare services is paramount. Clinical supervision is one approach that nurtures and supports professional guidance, ethical practice, and personal development, which impacts positively on staff morale and standards of care delivery. In the context of this study, peer group clinical supervision provides allocated time to reflect and discuss care provided and facilitated by clinical supervisors who are at the same grade/level as the supervisees.
To explore the clinical supervisor’s experiences of peer group clinical supervision a mixed methods study design was utilised within Irish health services (midwifery, intellectual disability, general, mental health). The Manchester Clinical Supervision Scale was used to survey clinical supervisors ( n = 36) and semi-structured interviews ( n = 10) with clinical supervisors were conducted. Survey data were analysed through SPSS and interview data were analysed utilising content analysis. The qualitative and quantitative data’s reporting rigour was guided by the CROSS and SRQR guidelines.
Participants generally had a positive encounter when providing clinical supervision. They highly appreciated the value of clinical supervision and expressed a considerable degree of contentment with the supervision they provided to supervisees. The advantages of peer group clinical supervision encompass aspects related to self (such as confidence, leadership, personal development, and resilience), service and organisation (including a positive working environment, employee retention, and safety), and patient care (involving critical thinking and evaluation, patient safety, adherence to quality standards, and elevated levels of care).
There are many benefits of peer group clinical supervision at an individual, service, organisation, and patient level. Nevertheless, there is a need to address a lack of awareness and misconceptions surrounding clinical supervision to create an environment and culture conducive to realising its full potential. It is crucial that clinical supervision be accessible to nurses and midwives of all grades across all healthcare services, with national planning to address capacity and sustainability.
Peer Review reports
Within a dynamic healthcare system, nurses and midwives face growing demands, underscoring the necessity for ongoing personal and professional development. This is essential to improve the effectiveness and efficiency of care delivery for patients, families, and societies. Despite the increased emphasis on increasing the quality and safety of healthcare services and delivery, there is evidence highlighting declining standards of nursing and midwifery care [ 1 ]. The recent focus on re-affirming and re-committing to core values guiding nursing and midwifery practice is encouraging such as compassion, care and commitment [ 2 ], competence, communication, and courage [ 3 ]. However, imposing value statements in isolation is unlikely to change behaviours and greater consideration needs to be given to ways in which compassion, care, and commitment are nurtured and ultimately applied in daily practice. Furthermore, concerns have been raised about global staff shortages [ 4 ], the evidence suggesting several contributing factors such as poor workforce planning [ 5 ], job dissatisfaction [ 6 ], and healthcare migration [ 7 ]. Without adequate resources and staffing, compromising standards of care and threats to patient safety will be imminent therefore the importance of developing effective strategies for retaining competent registered nurses and midwives is paramount in today’s climate of increased staff shortages [ 4 ]. Clinical supervision serves as a means to facilitate these advancements and has been linked to heightened job satisfaction, enhanced staff retention, improved staff effectiveness, and effective clinical governance, by aiding in quality improvements, risk management, and heightened accountability [ 8 ].
Clinical supervision is a key component of professional practice and while the aim is largely known, there is no universally accepted definition of clinical supervision [ 8 ]. Clinical supervision is a structured process where clinicians are allowed protected time to reflect on their practice within a supportive environment and with the purpose of developing high-quality clinical care [ 9 ]. Recent literature published on clinical supervision [ 8 , 9 , 10 , 11 , 12 , 13 , 14 , 15 , 16 ] highlights the advantages and merits of clinical supervision. However, there are challenges also identified such as a lack of consensus regarding the meaning and goal, implementation issues, variations in approaches in its operationalisation, and an absence of research evidence on its effectiveness. Duration and experience in clinical supervision link to positive benefits [ 8 ], but there is little evidence of how clinical supervision altered individual behaviours and practices. This is reinforced by Kuhne et al., [ 15 ] who emphasise that satisfaction rather than effectiveness is more commonly examined. It is crucial to emphasise that reviews have pinpointed that clinical supervision lowers the risks of adverse patient outcomes [ 9 ] and demonstrates enhancements in the execution of certain care processes. Peer group clinical supervision is a form of clinical supervision whereby two or more practitioners engage in a supervision or consultation process to improve their professional practice [ 17 ]. There is limited evidence regarding peer group clinical supervision and research on the experiences of peer clinical supervision and stakeholders is needed [ 13 ]. In Ireland, peer group clinical supervision has been recommended and guidelines have been developed [ 18 ]. In the Irish context, peer clinical supervision is where both clinical supervisees and clinical supervisors are peers at the same level/grade. However, greater evidence is required to inform future decisions on the implementation of peer group clinical supervision and the purpose of this study is to explore clinical supervisors’ experiences of peer group clinical supervision. As the focus is on peer group supervisors and utilising mixed methods the experiences of the other stakeholders were investigated and reported separately.
A mixed methods approach was used (survey and semi-structured interviews) to capture clinical supervisor’s experiences of clinical supervision. The study adhered to the Consensus-Based Checklist for Reporting of Survey Studies guidelines [ 19 ] (Supplementary File S1 ) and Standards for Reporting Qualitative Research guidelines [ 20 ] (Supplementary File S2 ).
Participants
This study was conducted with participants who successfully completed a professionally credited award: clinical supervision module run by a university in Ireland (74 clinical supervisors across 5 programmes over 3 years). The specific selection criteria for participants were that they were registered nurses/midwives delivering peer group clinical supervision within the West region of Ireland. The specific exclusion criteria were as follows: (1) nurses and midwives who haven’t finished the clinical supervision module at the University, (2) newly appointed peer group clinical supervisors who have yet to establish their groups and initiate the delivery of peer group clinical supervision.
Measures and procedures
The Manchester Clinical Supervision Scale-26 was used to survey participants in February/March 2022 and measure the peer group clinical supervisors’ overall experiences of facilitating peer group clinical supervision. The Manchester Clinical Supervision Scale-26 is a validated 26-item self-report questionnaire with a Likert-type (1–5) scale ranging from strongly disagree (1) to strongly agree (5) [ 21 ]. The Manchester Clinical Supervision Scale-26 measures the efficiency of and satisfaction with supervision, to investigate the skills acquisition aspect of clinical supervision and its effect on the quality of clinical care [ 21 ]. The instrument consists of two main sections to measure three (normative, restorative, and formative) dimensions of clinical supervision utilising six sub-scales: (1) trust and rapport, (2) supervisor advice/support, (3) improved care/skills, (4) importance/value of clinical supervision, (5) finding time, (6) personal issues/reflections and a total score for the Manchester Clinical Supervision Scale-26 is also calculated. Section two consisted of the demographic section of the questionnaire and was tailored to include eight demographic questions concerning the supervisor’s demographics, supervisee characteristics, and characteristics of clinical supervision sessions. There were also two open field questions on the Manchester Clinical Supervision Scale-26 (model of clinical supervision used and any other comments about experience of peer group clinical supervision). The main question about participants’ experiences with peer clinical supervision was “What was your experience of peer clinical supervision?” This was gathered through individual semi-structured interviews lasting between 20 and 45 min, in March/April 2022 (Supplementary file 3 ).
Ethical considerations
Health service institutional review boards of two University hospitals approved this study (Ref: 091/19 and Ref: C.A. 2199). Participants were recruited after receiving a full explanation of the study’s purpose and procedure and all relevant information. Participants were aware of potential risks and benefits and could withdraw from the study, or the survey could be stopped at any time. Informed consent was recorded, and participant identities were protected by using a pseudonym to protect anonymity.
Data analysis method
Survey data was analysed using the data analysis software package Statistical Package for the Social Sciences, version 26 (SPSS Inc., Chicago, Il, USA). Descriptive analysis was undertaken to summarise responses to all items and categorical variables (nominal and ordinal) were analysed using frequencies to detail the number and percentage of responses to each question. Scores on the Manchester Clinical Supervision Scale-26 were reverse scored for 9 items (Q1-Q6, Q8, Q20,21) and total scores for each of the six sub-scales were calculated by adding the scores for each item. Raw scores for the individual sub-scales varied in range from 0 to 20 and these raw scores were then converted to percentages which were used in addition to the raw scores for each sub-scale to describe and summarise the results of the Manchester Clinical Supervision Scale-26. Cronbach’s alpha coefficient was undertaken with the 26 questions included within the Manchester Clinical Supervision Scale-26 and more importantly with each of the dimensions in the Manchester Clinical Supervision Scale-26. The open-ended questions on the Manchester Clinical Supervision Scale-26 and interviews were analysed using content analysis guided by Colorafi and Evans [ 22 ] and categories were generated using their eight steps, (1) creating a coding framework, (2) adding codes and memos, (3) applying the first level of coding, (4) categorising codes and applying the second level of coding, (5) revising and redefining the codes, (6) adding memos, (7) visualising data and (8) representing the data.

Research rigour
To ensure the validity and rigour of this study the researchers utilised the Manchester Clinical Supervision Scale-26 a recognised clinical supervision tool with good reliability and wide usage. Interviews were recorded, transcribed, and verified by four participants, data were collected until no new components appeared, data collection methods and analysis procedures were described, and the authors’ biases were minimised throughout the research process. The Manchester Clinical Supervision Scale-26 instrument internal consistency reliability was assessed which was overall good (α = 0.878) with individual subscale also good e.g., normative domain 0.765, restorative domain 0.864, and formative domain 0.900. Reporting rigour was demonstrated using the Consensus-Based Checklist for Reporting of Survey Studies guidelines [ 19 ] and Standards for Reporting Qualitative Research guidelines [ 20 ].
Quantitative data
Participant and clinical supervision characteristics.
Thirty-six of the fifty-two (69.2%) peer group clinical supervisors working across a particular region of Ireland responded to the Manchester Clinical Supervision Scale-26 survey online via Qualtrics. Table 1 identifies the demographics of the sample who were predominantly female (94.4%) with a mean age of 44.7 years (SD. 7.63).
Peer group clinical supervision session characteristics (Table 2 ) highlight over half of peer group clinical supervisors ( n = 20, 55.6%) had been delivering peer group clinical supervision for less than one year and were mainly delivered to female supervisees ( n = 28, 77.8%). Most peer group clinical supervision sessions took place monthly ( n = 32, 88.9%) for 31–60 min ( n = 27, 75%).
Manchester Clinical Supervision Scale-26 results
Participants generally viewed peer group clinical supervision as effective (Table 3 ), the total mean Manchester Clinical Supervision Scale-26 score among all peer group clinical supervisors was 76.47 (SD. 12.801) out of 104, Surpassing the clinical supervision threshold score of 73, which was established by the developers of the Manchester Clinical Supervision Scale-26 as the benchmark indicating proficient clinical supervision provision [ 21 ]. Of the three domains; normative, formative, and restorative, the restorative domain scored the highest (mean 28.56, SD. 6.67). The mean scores compare favourably to that of the Manchester Clinical Supervision Scale-26 benchmark data and suggest that the peer group clinical supervisors were satisfied with both the level of support, encouragement, and guidance they provided and the level of trust/rapport they had developed during the peer group clinical supervision sessions. 83.3% ( n = 30) of peer group clinical supervisors reported being either very satisfied ( n = 12, 33.3%) or moderately satisfied ( n = 18, 50%) with the peer group clinical supervision they currently delivered. Within the peer group clinical supervisor’s supervisee related issues ( n = 17, 47.2%), work environment-related issues ( n = 16, 44.4%), staff-related issues ( n = 15, 41.7%) were reported as the most frequent issues, with patient/client related issues being less frequent ( n = 8, 22.2%). The most identified model used to facilitate peer group clinical supervision was the Proctors model ( n = 8, 22.22%), which was followed by group ( n = 2, 5.55%), peer ( n = 2, 5.55%), and a combination of the seven-eyed model of clinical supervision and Proctors model ( n = 1, 2.77%) with some not sure what model they used ( n = 2, 5.553%) and 58.33% ( n = 21) did not report what model they used.
Survey open-ended question
‘Please enter any additional comments , which are related to your current experience of delivering Peer Group Clinical Supervision.’ There were 22 response comments to this question, which represented 61.1% of the 36 survey respondents, which were analysed using content analysis guided by Colorafi & Evans [ 22 ]. Three categories were generated. These included: personal value/benefit of peer group clinical supervision, challenges with facilitating peer group clinical supervision, and new to peer group clinical supervision.
The first category ‘personal value/benefit of peer group clinical supervision’ highlighted positive experiences of both receiving and providing peer group clinical supervision. Peer group clinical supervisors reported that they enjoyed the sessions and found them both worthwhile and beneficial for both the group and them as peer group clinical supervisors in terms of creating a trusted supportive group environment and motivation to develop. Peer group clinical supervision was highlighted as very important for the peer group clinical supervisors working lives and they hoped that there would be more uptake from all staff. One peer group clinical supervisor expressed that external clinical supervision was a ‘lifeline’ to shaping their supervisory journey to date.
The second category ‘challenges with facilitating peer group clinical supervision’, identified time constraints, lack of buy-in/support from management, staff shortages, lack of commitment by supervisees, and COVID-19 pandemic restrictions and related sick leave, as potential barriers to facilitating peer group clinical supervision. COVID-19 was perceived to have a negative impact on peer group clinical supervision sessions due to staff shortages, which resulted in difficulties for supervisees attending the sessions during work time. Peer group clinical supervisors felt that peer group clinical supervision was not supported by management and there was limited ‘buy-in’ at times. There was also a feeling expressed that peer group clinical supervision was in its infancy, as COVID-19 and its related restrictions impacted on this by either slowing down the process of commencing peer group clinical supervision in certain areas or having to move online. However, more recently improvements in managerial support and supervisee engagement with the peer group clinical supervision process are noted.
The final category ‘new to peer group clinical supervision’ highlighted that some peer group clinical supervisors were new to the process of providing peer group clinical supervision and some felt that this survey was not a true reflection of their experience of delivering peer group clinical supervision, as they were not fully established yet as clinical supervisors due to the impact of COVID-19. Peer group clinical supervisors identified that while they were new to providing peer group clinical supervision, they were enjoying it and that it was a learning curve for them.
Qualitative data
The qualitative phase explored peer group clinical supervisors’ ( n = 10) own experiences of preparation received and experiences of being a peer group clinical supervisor. Three themes were identified through data analysis, building the foundations, enacting engagement and actions, and realities (Table 4 ).
Building the foundations
This theme highlights the importance of prior knowledge, awareness, and training but also the recruitment process and education in preparing peer group clinical supervisors.
Knowledge and awareness
Participant’s prior knowledge and awareness of peer group clinical supervision was mixed with some reporting having little or no knowledge of clinical supervision.
I’m 20 years plus trained as a nurse , and I had no awareness of clinical supervision beforehand , I really hadn’t got a clue what all of this was about , so it was a very new concept to me (Bernie) .
Others were excited about peer group clinical supervision and while they could see the need they were aware that there may be limited awareness of the value and process of clinical supervision among peers.
I find that there’s great enthusiasm and passion for clinical supervision as it’s a great support mechanism for staff in practice , however , there’s a lack of awareness of clinical supervision (Jane) .
Recruitment
Some participants highlighted that the recruitment process to become a peer group clinical supervisor was vague in some organisations with an unclear and non-transparent process evident where people were chosen by the organisation’s management rather than self-selecting interested parties.
It was just the way the training was put to the people , they were kind of nominated and told they were going and there was a lot of upset over that , so they ended up in some not going at all (Ailbhe) .
In addition, the recruitment process was seen as top loaded where senior grades of staff were chosen, and this limited staff nurse grade opportunities where there was a clear need for peer group clinical supervisors and support.
We haven’t got down to the ground level like you know we’ve done the directors , we’ve done the CNM3s the CNM2s we are at the CNM1s , so we need to get down to the staff nurse level so the nurses at the direct frontline are left out and aren’t receiving supervision because we don’t have them trained (Bernie) .
Training and education
Participants valued the training and education provided but there was a clear sense of ‘imposter syndrome’ for some peer group clinical supervisors starting out. Participants questioned their qualifications, training duration, and confidence to undertake the role of peer group clinical supervisor.
Because it is group supervision and I know that you know they say that we are qualified to do supervision and you know we’re now qualified clinical supervisors but I’m not sure that a three-month module qualifies you to be at the top of your game (Maria) .
Participants when engaged in the peer group clinical supervisor educational programme did find it beneficial and the true benefit was the actual re-engagement in education and published evidence along with the mix of nursing and midwifery practice areas.
I found it very beneficial , I mean I hadn’t been engaged in education here in a while , so it was great to be back in that field and you know with the literature that’s big (Claire) .
Enacting engagement and actions
This theme highlights the importance of forming the groups, getting a clear message out, setting the scene, and grounding the group.
Forming the groups
Recruitment for the group was of key importance to the peer group clinical supervisor and they all sent out a general invitation to form their group. Some supervisors used invitation letters or posters in addition to a general email and this was effective in recruiting supervisees.
You’re reaching out to people , I linked in with the ADoN and I put together a poster and circulated that I wasn’t ‘cherry picking , and I set up a meeting through Webex so people could get a sense of what it was if they were on the fence about it or unsure if it was for them (Karen) .
In forming the peer clinical supervision groups consideration needs to be given to the actual number of supervisees and participants reported four to six supervisees as ideal but that number can alter due to attendance.
The ideal is having five or six consistent people and that they all come on board and that you get the dynamics of the group and everything working (Claire) .
Getting a clear message out
Within the recruitment process, it was evident that there was a limited and often misguided understanding or perception of peer group clinical supervision.
Greater awareness of what actually clinical supervision is , people misjudge it as a supervision where someone is appraising you , when in fact it is more of a support mechanism , I think peer support is the key element that needs to be brought out (Jane) .
Given the lack of clarity and understanding regarding peer group clinical supervision, the participants felt strongly that further clarity is needed and that the focus needs to be on the support it offers to self, practice, and the profession.
Clinical supervision to me is clinical leadership (Jane) .
Setting the scene and grounding the group
In the initial phase of the group coming together the aspect of setting the scene and grounding the group was seen as important. A key aspect of this process was establishing the ground rules which not only set the boundaries and gave structure but also ensured the adoption of principles of trust, confidentiality, and safety.
We start with the ground rules , they give us structure it’s our contract setting out the commitment the expectation for us all , and the confidentiality as that’s so important to the trust and safety and building the relationships (Brid) .
Awareness of group dynamics is important in this process along with awareness of the group members (supervisees) as to their role and expectations.
I reiterate the role of each person in relation to confidentiality and the relationship that they would have with each other within the group and the group is very much aware that it is based on respect for each person’s point of view people may have a fear of contributing to the group and setting the ground rules is important (Jane) .
To ground the group, peer group clinical supervisors saw the importance of being present and allowing oneself to be in the room. This was evident in the time allocated at the start of each session to allow ‘grounding’ to occur in the form of techniques such as a short meditation, relaxation, or deep breathing.
At the start , I do a bit of relaxation and deep breathing , and I saw that with our own external supervisor how she settled us into place so very much about connecting with your body and you’ve arrived , then always come in with the contract in my first sentence , remember today you know we’re in a confidential space , of course , you can take away information , but the only information you will take from today is your own information and then the respect aspect (Mary Rose) .
This settling in and grounding was seen as necessary for people to feel comfortable and engage in the peer group clinical supervision process where they could focus, be open, converse, and be aware of their role and the role of peer group clinical supervision.
People have to be open, open about their practice and be willing to learn and this can only occur by sharing, clinical supervision gives us the space to do it in a space where we know we will be respected, and we can trust (Claire) .
This theme highlights the importance of the peer group clinical supervisors’ past experiences, delivering peer group clinical supervision sessions, responding to COVID-19, personal and professional development, and future opportunities.
Past experiences
Past experiences of peer group clinical supervisors were not always positive and for one participant this related to the lack of ground rules or focus of the sessions and the fact it was facilitated by a non-nurse.
In the past , I suppose I would have found it very frustrating as a participant because I just found that it was going round in circles , people moaning and you know it wasn’t very solution focused so I came from my situation where I was very frustrated with clinical supervision , it was facilitated by somebody that was non-nursing then it wasn’t very , there wasn’t the ground rules , it was very loose (Caroline) .
However, many did not have prior experience of peer group clinical supervision. Nonetheless, through the education and preparation received, there was a sense of commitment to embrace the concept, practice, and philosophy.
I did not really have any exposure or really much information on clinical supervision , but it has opened my eyes , and as one might say I am now a believer (Brid) .
Delivering peer group clinical supervision
In delivering peer group clinical supervision, participants felt supervisees were wary, as they did not know what peer group clinical supervision was, and they had focused more on the word supervision which was misleading to them. Nonetheless, the process was challenging, and buy-in was questioned at an individual and managerial level.
Buy-in wasn’t great I think now of course people will blame the pandemic , but this all happened before the pandemic , there didn’t seem to be you know , the same support from management that I would have expected so I kind of understood it in a way because then there wasn’t the same real respect from the practitioners either (Mary Rose) .
From the peer group clinical supervisor’s perspective, they were all novices in delivering/facilitating peer group clinical supervision sessions, and the support of the external clinical supervisors, and their own peer group clinical supervision sessions were invaluable along with a clinical supervision model.
Having supervision myself was key and something that is vital and needed , we all need to look at our practice and how we work it’s no good just facilitating others without being part of the process yourself but for me I would say the three principles of clinical supervision , you know the normative , formative and restorative , I keep hammering that home and bring that in regularly and revisit the contract and I have to do that often you know (Claire) .
All peer group clinical supervisors commented on the preparation for their peer group clinical supervision sessions and the importance of them having the right frame of mind and that often they needed to read over their course work and published evidence.
I want everybody to have a shared voice and you know that if one person , there is something that somebody feels very strongly and wants to talk about it that they e-mail in advance like we don’t have a set agenda but that’s agreed from the participant at the start (Caroline) .
To assist this, the peer group clinical supervisors noted the importance of their own peer group clinical supervision, the support of their peers, and external clinical supervisors. This preparation in an unpredictable situation can be difficult but drawing on one’s experience and the experience within the group can assist in navigating beyond unexpected situations.
I utilise the models of clinical supervision and this helps guide me , I am more of a facilitator of the group we are experts in our own area and our own role but you can only be an expert if you take the time to examine your practice and how you operate in your role (Brid) .
All clinical supervisors noted that the early sessions can be superficial, and the focus can be on other practice or management issues, but as time moves on and people become more engaged and involved it becomes easier as their understanding of supervision becomes clearer. In addition, there may be hesitancy and people may have difficulty opening up with certain people in the group and this is a reality that can put people off.
Initially there was so much managerial bashing and I think through supervision , I began to kind of think , I need the pillars of supervision , the governance , bringing more knowledge and it shifted everything in the room , trying to marry it with all the tensions that people have (Mary Rose) .
For some clinical supervisors, there were expected and unexpected challenges for them as clinical supervisors in terms of the discussions veering off course and expectations of their own ability.
The other big challenge is when they go off , how do you bring him back , you know when they veer off and you’re expected to be a peer , but you have to try and recoil that you have to get the balance with that right (Mary Rose) .
While peer group clinical supervision is accepted and seen as a valuable process by the peer group clinical supervisors, facilitating peer group supervision with people known to you can be difficult and may affect the process.
I’d love to supervise a group where I actually don’t know the people , I don’t know the dynamics within the group , and I’d love to see what it would be like in a group (Bernie) .
Of concern to clinical supervisors was the aspect of non-attendance and while there may be valid reasons such as COVID-19 the absence of a supervisee for several sessions can affect the group dynamics, especially if the supervisee has only engaged with early group sessions.
One of the ones that couldn’t attend because of COVID and whatever , but she’s coming to the next one and I just feel there’s a lot of issues in her area and I suppose I’m mindful that I don’t want that sort of thing to seep in , so I suppose it’s just for me just to keep reiterating the ground rules and the boundaries , that’s something I just have to manage as a facilitator , but what if they don’t attend how far will the group have progressed before she attends (Caroline) .
Responding to COVID-19
The advent of COVID-19 forced peer group clinical supervisors to find alternative means of providing peer group clinical supervision sessions which saw the move from face-to-face to online sessions. The online transition was seen as seamless for many established groups while others struggled to deliver sessions.
With COVID we did online for us it was fine because we were already formed (Corina) .
While the transition may have been positive many clinical supervisors came across issues because they were using an online format that would not be present in the face-to-face session.
We did have a session where somebody was in the main office and they have a really loud booming voice and they were saying stuff that was not appropriate to say outside of clinical supervision and I was like are you in the office can you lower it down a bit can you put your headphones on (Maria) .
However, two peer group clinical supervisors ceased or hasted the progress of rolling out peer group clinical supervision sessions mainly due to redeployment and staff availability.
With COVID it just had to be canceled here , it’s just the whole thing was canceled so it was very , very difficult for people (Mary Rose) .
It was clear from clinical supervisors that online sessions were appropriate but that they felt they were only appropriate for existing established groups that have had the opportunity to build relationships, develop trust, embed the ground rules, and create the space for open communication and once established a combined approach would be appropriate.
Since we weren’t as established as a group , not everybody knew each other it would be difficult to establish that so we would hold off/reschedule , obviously COVID is a major one but also I suppose if you have an established group now , and again , you could go to a remote one , but I felt like since we weren’t established as a group it would be difficult to develop it in that way (Karen) .
Within practice COVID-19 took priority and other aspects such as peer group clinical supervision moved lower down on the priority list for managers but not for the clinical supervisors even where redeployment occurred.
With COVID all the practical side , if one of the managers is dealing with an outbreak , they won’t be attending clinical supervision , because that has to be prioritised , whereas we’ve prioritised clinical supervision (Maria) .
The valuing of peer group clinical supervision was seen as important by clinical supervisors, and they saw it as particularly needed during COVID-19 as staff were dealing with many personal and professional issues.
During the height of COVID , we had to take a bit of a break for four months as things were so demanding at work for people but then I realised that clinical supervision was needed and started back up and they all wanted to come back (Brid) .
Having peer group clinical supervision during COVID-19 supported staff and enabled the group to form supportive relationships.
COVID has impacted over the last two years in every shape and they needed the supervision and the opportunity to have a safe supportive space and it gelled the group I think as we all were there for each other (Claire) .
While COVID-19 posed many challenges it also afforded clinical supervisors and supervisees the opportunity for change and to consider alternative means of running peer group clinical supervision sessions. This change resulted in online delivery and in reflecting on both forms of delivery (face-to-face and online) clinical supervisors saw the benefit in both. Face-to-face was seen as being needed to form the group and then the group could move online once the group was established with an occasional periodic face-to-face session to maintain motivation commitment and reinforce relationships and support.
Online formats can be effective if the group is already established or the group has gone through the storming and forming phase and the ground rules have been set and trust built , then I don’t see any problem with a blended online version of clinical supervision , and I think it will be effective (Jane) .
Personal and professional development
Growth and development were evident from peer group clinical supervisors’ experiences and this growth and development occurred at a personal, professional, and patient/client level. This development also produced an awakening and valuing of one’s passion for self and their profession.
I suppose clinical supervision is about development I can see a lot of development for me and my supervisees , you know personally and professionally , it’s the support really , clinical supervision can reinvigorate it’s very exciting and a great opportunity for nursing to support each other and in care provision (Claire) .
A key to the peer group clinical supervisor’s development was the aspect of transferable skills and the confidence they gained in fulfilling their role.
All of these skills that you learn are transferable and I am a better manager because of clinical supervision (Maria) .
The confidence and skills gained translated into the clinical supervisor’s own practice as a clinical practitioner and clinical supervisor but they were also realistic in predicting the impact on others.
I have empowered my staff , I empower them to use their voice and I give my supervisees a voice and hope they take that with them (Corina) .
Fundamental to the development process was the impact on care itself and while this cannot always be measured or identified, the clinical supervisors could see that care and support of the individual practitioner (supervisee) translated into better care for the patient/client.
Care is only as good as the person delivering it and what they know , how they function and what energy and passion they have , and clinical supervision gives the person support to begin to understand their practice and how and why they do things in a certain way and when they do that they can begin to question and even change their way of doing something (Brid) .
Future opportunities
Based on the clinical supervisor’s experiences there was a clear need identified regarding valuing and embedded peer group clinical supervision within nursing/midwifery practice.
There has to be an emphasis placed on supervision it needs to be part of the fabric of a service and valued by all in that service , we should be asking why is it not available if it’s not there but there is some work first on promoting it and people knowing what it actually is and address the misconceptions (Claire) .
While such valuing and buy-in are important, it is not to say that all staff need to have peer group clinical supervision so as to allow for personal choice. In addition, to value peer group clinical supervision it needs to be evident across all staffing grades and one could question where the best starting point is.
While we should not mandate that all staff do clinical supervision it should become embedded within practice more and I suppose really to become part of our custom and practice and be across all levels of staff (Brid) .
When peer group clinical supervision is embedded within practice then it should be custom and practice, where it is included in all staff orientations and is nationally driven.
I suppose we need to be driving it forward at the coal face at induction , at orientation and any development for the future will have to be driven by the NMPDUs or nationally (Ailbhe) .
A formalised process needs to address the release of peer group clinical supervisors but also the necessity to consider the number of peer group clinical supervisors at a particular grade.
The issue is release and the timeframe as they have a group but they also have their external supervision so you have to really work out how much time you’re talking about (Maria) .
Vital within the process of peer group clinical supervision is receiving peer group clinical supervision and peer support and this needs to underpin good peer group clinical supervision practice.
Receiving peer group supervision helps me , there are times where I would doubt myself , it’s good to have the other group that I can go to and put it out there to my own group and say , look at this , this is what we did , or this is what came up and this is how (Bernie) .
For future roll out to staff nurse/midwife grade resourcing needs to be considered as peer group clinical supervisors who were managers could see the impact of having several peer group clinical supervisors in their practice area may have on care delivery.
Facilitating groups is an issue and needs to be looked at in terms of the bigger picture because while I might be able to do a second group the question is how I would be supported and released to do so (Maria) .
While there was ambiguity regarding peer group clinical supervision there was an awareness of other disciplines availing of peer group clinical supervision, raising questions about the equality of supports available for all disciplines.
I always heard other disciplines like social workers would always have been very good saying I can’t meet you I have supervision that day and I used to think my God what’s this fabulous hour that these disciplines are getting and as a nursing staff it just wasn’t there and available (Bernie) .
To address this equity issue and the aspect of low numbers of certain grades an interdisciplinary approach within nursing and midwifery could be used or a broader interdisciplinary approach across all healthcare professionals. An interdisciplinary or across-services approach was seen as potentially fruitful.
I think the value of interprofessional or interdisciplinary learning is key it addresses problem-solving from different perspectives that mix within the group is important for cross-fertilisation and embedding the learning and developing the experience for each participant within the group (Jane) .
As we move beyond COVID-19 and into the future there is a need to actively promote peer group clinical supervision and this would clarify what peer group clinical supervision actually is, its uptake and stimulate interest.
I’d say it’s like promoting vaccinations if you could do a roadshow with people , I think that would be very beneficial , and to launch it , like you have a launch an official launch behind it (Mary Rose) .
The advantages of peer group clinical supervision highlighted in this study pertain to self-enhancement (confidence, leadership, personal development, resilience), organisational and service-related aspects (positive work environment, staff retention, safety), and professional patient care (critical thinking and evaluation, patient safety, adherence to quality standards, elevated care standards). These findings align with broader literature that acknowledges various areas, including self-confidence and facilitation [ 23 ], leadership [ 24 ], personal development [ 25 ], resilience [ 26 ], positive/supportive working environment [ 27 ], staff retention [ 28 ], sense of safety [ 29 ], critical thinking and evaluation [ 30 ], patient safety [ 31 ], quality standards [ 32 ] and increased standards of care [ 33 ].
In this study, peer group clinical supervision appeared to contribute to the alleviation of stress and anxiety. Participants recognised the significance of these sessions, where they could openly discuss and reflect on professional situations both emotionally and rationally. Central to these discussions was the creation of a safe, trustworthy, and collegial environment, aligning with evidence in the literature [ 34 ]. Clinical supervision provided a platform to share resources (information, knowledge, and skills) and address issues while offering mutual support [ 35 ]. The emergence of COVID-19 has stressed the significance of peer group clinical supervision and support for the nursing/midwifery workforce [ 36 ], highlighting the need to help nurses/midwifes preserve their well-being and participate in collaborative problem-solving. COVID-19 impacted and disrupted clinical supervision frequency, duration and access [ 37 ]. What was evident during COVID-19 was the stress and need for support for staff and given the restorative or supportive functions of clinical supervision it is a mechanism of support. However, clinical supervisors need support themselves to be able to better meet the supervisee’s needs [ 38 ].
The value of peer group clinical supervision in nurturing a conducive working environment cannot be overstated, as it indorses the understanding and adherence to workplace policies by empowering supervisees to understand the importance and rationale behind these policies [ 39 ]. This becomes vital in a continuously changing healthcare landscape, where guidelines and policies may be subject to change, especially in response to situations such as COVID-19. In an era characterised by international workforce mobility and a shortage of healthcare professionals, a supportive and positive working environment through the provision of peer group clinical supervision can positively influence staff retention [ 40 ], enhance job satisfaction [ 41 ], and mitigate burnout [ 42 ]. A critical aspect of the peer group clinical supervision process concerns providing staff the opportunity to reflect, step back, problem-solve and generate solutions. This, in turn, ensures critical thinking and evaluation within clinical supervision, focusing on understanding the issues and context, and problem-solving to draw constructive lessons for the future [ 30 ]. Research has determined a link between clinical supervision and improvements in the quality and standards of care [ 31 ]. Therefore, peer group clinical supervision plays a critical role in enhancing patient safety by nurturing improved communication among staff, facilitating reflection, promoting greater self-awareness, promoting the exchange of ideas, problem-solving, and facilitating collective learning from shared experiences.
Starting a group arose as a foundational aspect emphasised in this study. The creation of the environment through establishing ground rules, building relationships, fostering trust, displaying respect, and upholding confidentiality was evident. Vital to this process is the recruitment of clinical supervisees and deciding the suitable group size, with a specific emphasis on addressing individuals’ inclination to engage, their knowledge and understanding of peer group clinical supervision, and dissipating any lack of awareness or misconceptions regarding peer group supervision. Furthermore, the educational training of peer group clinical supervisors and the support from external clinical supervisors played a vital role in the rollout and formation of peer group clinical supervision. The evidence stresses the significance of an open and safe environment, wherein supervisees feel secure and trust their supervisor. In such an environment, they can effectively reflect on practice and related issues [ 41 ]. This study emphasises that the effectiveness of peer group supervision is more influenced by the process than the content. Clinical supervisors utilised the process to structure their sessions, fostering energy and interest to support their peers and cultivate new insights. For peer group clinical supervision to be effective, regularity is essential. Meetings should be scheduled in advance, allocate protected time, and take place in a private space [ 35 ]. While it is widely acknowledged that clinical supervisors need to be experts in their professional field to be credible, this study highlights that the crucial aspects of supervision lie in the quality of the relationship with the supervisor. The clinical supervisor should be supportive, caring, open, collaborative, sensitive, flexible, helpful, non-judgmental, and focused on tacit knowledge, experiential learning, and providing real-time feedback.
Critical to the success of peer group clinical supervision is the endorsement and support from management, considering the organisational culture and attitudes towards the practice of clinical supervision as an essential factor [ 43 ]. This support and buy-in are necessary at both the management and individual levels [ 28 ]. The primary obstacles to effective supervision often revolve around a lack of time and heavy workloads [ 44 ]. Clinical supervisors frequently struggle to find time amidst busy environments, impacting the flexibility and quality of the sessions [ 45 ]. Time constraints also limit the opportunity for reflection within clinical supervision sessions, leaving supervisees feeling compelled to resolve issues on their own without adequate support [ 45 ]. Nevertheless, time-related challenges are not unexpected, prompting a crucial question about the value placed on clinical supervision and its integration into the culture and fabric of the organisation or profession to make it a customary practice. Learning from experiences like those during the COVID-19 pandemic has introduced alternative ways of working, and the use of technology (such as Zoom, Microsoft Teams, Skype) may serve as a means to address time, resource, and travel issues associated with clinical supervision.
Despite clinical supervision having a long international history, persistent misconceptions require attention. Some of these include not considering clinical supervision a priority [ 46 ], perceiving it as a luxury [ 41 ], deeming it self-indulgent [ 47 ], or viewing it as mere casual conversation during work hours [ 48 ]. A significant challenge lies in the lack of a shared understanding regarding the role and purpose of clinical supervision, with past perceptions associating it with surveillance and being monitored [ 48 ]. These negative connotations often result in a lack of engagement [ 41 ]. Without encouragement and recognition of the importance of clinical supervision from management or the organisation, it is unlikely to become embedded in the organisational culture, impeding its normalisation [ 39 ].
In this study, some peer group clinical supervisors expressed feelings of being impostors and believed they lacked the knowledge, skills, and training to effectively fulfil their roles. While a deficiency in skills and competence are possible obstacles to providing effective clinical supervision [ 49 ], the peer group clinical supervisors in this study did not report such issues. Instead, their concerns were more about questioning their ability to function in the role of a peer group clinical supervisor, especially after a brief training program. The literature acknowledges a lack of training where clinical supervisors may feel unprepared and ill-equipped for their role [ 41 ]. To address these challenges, clinical supervisors need to be well-versed in professional guidelines and ethical standards, have clear roles, and understand the scope of practice and responsibilities associated with being a clinical supervisor [ 41 ].
The support provided by external clinical supervisors and the peer group clinical supervision sessions played a pivotal role in helping peer group clinical supervisors ease into their roles, gain experiential learning, and enhance their facilitation skills within a supportive structure. Educating clinical supervisors is an investment, but it should not be a one-time occurrence. Ongoing external clinical supervision for clinical supervisors [ 50 ] and continuous professional development [ 51 ] are crucial, as they contribute to the likelihood of clinical supervisors remaining in their roles. However, it is important to interpret the results of this study with caution due to the small sample size in the survey. Generalising the study results should be approached with care, particularly as the study was limited to two regions in Ireland. However, the addition of qualitative data in this mixed-methods study may have helped offset this limitation.
This study highlights the numerous advantages of peer group clinical supervision at individual, service, organisational, and patient/client levels. Success hinges on addressing the initial lack of awareness and misconceptions about peer group clinical supervision by creating the right environment and establishing ground rules. To unlock the full potential of peer group clinical supervision, it is imperative to secure management and organisational support for staff release. More crucially, there is a need for valuing and integrating peer group clinical supervision into nursing and midwifery education and practice. Making peer group clinical supervision accessible to all grades of nurses and midwives across various healthcare services is essential, necessitating strategic planning to tackle capacity and sustainability challenges.
Data availability
Data are available from the corresponding author upon request owing to privacy or ethical restrictions.
Zelenikova R, Gurkova E, Friganovic A, Uchmanowicz I, Jarosova D, Ziakova K, Plevova I, Papastavrou E. Unfinished nursing care in four central European countries. J Nurs Manage. 2020;28(8):1888–900. https://doi.org/10.1111/jonm.12896 .
Article Google Scholar
Department of Health, Office of the Chief Nursing Officer. Position paper 1: values for nurses and midwives in Ireland. Dublin: The Stationery Office; 2016.
Google Scholar
Cummings J, Bennett V. Developing the culture of compassionate care: creating a new vision for nurses, midwives and care-givers. London: Department of Health; 2012.
Both-Nwabuwe JM, Dijkstra MT, Klink A, Beersma B. Maldistribution or scarcity of nurses: the devil is in the detail. J Nurs Manage. 2018;26(2):86–93. https://doi.org/10.1111/jonm.12531 .
Squires A, Jylha V, Jun J, Ensio A, Kinnunen J. A scoping review of nursing workforce planning and forecasting research. J Nurs Manage. 2017;25:587–96. https://doi.org/10.1111/jonm.12510 .
Sasso L, Bagnasco A, Catania G, Zanini M, Aleo G, Watson R. Push and pull factors of nurses’ intention to leave. J Nurs Manage. 2019;27:946–54. https://doi.org/10.1111/jonm.12745 .
Gea-Caballero V, Castro-Sánchez E, Díaz‐Herrera MA, Sarabia‐Cobo C, Juárez‐Vela R, Zabaleta‐Del Olmo E. Motivations, beliefs, and expectations of Spanish nurses planning migration for economic reasons: a cross‐sectional, web‐based survey. J Nurs Scholarsh. 2019;51(2):178–86. https://doi.org/10.1111/jnu.12455 .
Article PubMed Google Scholar
Cutcliffe J, Sloan G, Bashaw M. A systematic review of clinical supervision evaluation studies in nursing. Int J Ment Health Nurs. 2018;27:1344–63. https://doi.org/10.1111/inm.12443 .
Snowdon DA, Hau R, Leggat SG, Taylor NF. Does clinical supervision of health professionals improve patient safety? A systematic review and meta-analysis. Int J Qual Health C. 2016;28(4):447–55. https://doi.org/10.1093/intqhc/mzw059 .
Turner J, Hill A. Implementing clinical supervision (part 1): a review of the literature. Ment Health Nurs. 2011;31(3):8–12.
Dilworth S, Higgins I, Parker V, Kelly B, Turner J. Finding a way forward: a literature review on the current debates around clinical supervision. Contemp Nurse. 2013;45(1):22–32. https://doi.org/10.5172/conu.2013.45.1.22 .
Buss N, Gonge H. Empirical studies of clinical supervision in psychiatric nursing: a systematic literature review and methodological critique. Int J Ment Health Nurs. 2009;18(4):250–64. https://doi.org/10.1111/j.1447-0349.2009.00612.x .
Pollock A, Campbell P, Deery R, Fleming M, Rankin J, Sloan G, Cheyne H. A systematic review of evidence relating to clinical supervision for nurses, midwives and allied health professionals. J Adv Nurs. 2017;73(8):1825–37. https://doi.org/10.1111/jan.13253 .
Snowdon DA, Leggat SG, Taylor NF. Does clinical supervision of healthcare professionals improve effectiveness of care and patient experience: a systematic review. BMC Health Serv Res. 2017;17(1):1–11. https://doi.org/10.1186/s12913-017-2739-5 .
Kühne F, Maas J, Wiesenthal S, Weck F. Empirical research in clinical supervision: a systematic review and suggestions for future studies. BMC Psychol. 2019;7(1):1–11. https://doi.org/10.1186/s40359-019-0327-7 .
Snowdon DA, Sargent M, Williams CM, Maloney S, Caspers K, Taylor NF. Effective clinical supervision of allied health professionals: a mixed methods study. BMC Health Serv Res. 2020;20(1):1–11. https://doi.org/10.1186/s12913-019-4873-8 .
Borders LD. Dyadic, triadic, and group models of peer supervision/consultation: what are their components, and is there evidence of their effectiveness? Clin Psychol. 2012;16(2):59–71.
Health Service Executive. Guidance document on peer group clinical supervision. Mayo: Nursing and Midwifery Planning and Development Unit Health Service Executive West Mid West; 2023.
Sharma A, Minh Duc NT, Lam Thang L, Nam T, Ng NH, Abbas SJ, Huy KS, Marušić NT, Paul A, Kwok CL. Karamouzian, M. A consensus-based checklist for reporting of survey studies (CROSS). J Gen Intern Med. 2021;36(10):3179–87. https://doi.org/10.1007/s11606-021-06737-1 .
Article PubMed PubMed Central Google Scholar
O’Brien BC, Harris IB, Beckman TJ, Reed DA, Cook DA. Standards for reporting qualitative research: a synthesis of recommendations. Acad Med. 2014;899:1245–51. https://doi.org/10.1097/ACM.0000000000000388 .
Winstanley J, White E. The MCSS-26©: revision of the Manchester Clinical Supervision Scale© using the Rasch Measurement Model. J Nurs Meas. 2011;193(2011):160–78. https://doi.org/10.1891/1061-3749.19.3.160 .
Colorafi KJ, Evans B. Qualitative descriptive methods in health science research. HERD-Health Env Res. 2016;9:16–25. https://doi.org/10.1177/1937586715614171 .
Agnew T, Vaught CC, Getz HG, Fortune J. Peer group clinical supervision program fosters confidence and professionalism. Prof Sch Couns. 2000;4(1):6–12.
Mc Carthy V, Goodwin J, Saab MM, Kilty C, Meehan E, Connaire S, O’Donovan A. Nurses and midwives’ experiences with peer-group clinical supervision intervention: a pilot study. J Nurs Manage. 2021;29:2523–33. https://doi.org/10.1111/jonm.13404 .
Rothwell C, Kehoe A, Farook SF, Illing J. Enablers and barriers to effective clinical supervision in the workplace: a rapid evidence review. BMJ Open. 2021;119:e052929. https://doi.org/10.1136/bmjopen-2021-052929 .
Francis A, Bulman C. In what ways might group clinical supervision affect the development of resilience in hospice nurses. Int J Palliat Nurs. 2019;25:387–96. https://doi.org/10.12968/ijpn.2019.25.8.387 .
Chircop Coleiro A, Creaner M, Timulak L. The good, the bad, and the less than ideal in clinical supervision: a qualitative meta-analysis of supervisee experiences. Couns Psychol Quart. 2023;36(2):189–210. https://doi.org/10.1080/09515070.2021.2023098 .
Stacey G, Cook G, Aubeeluck A, Stranks B, Long L, Krepa M, Lucre K. The implementation of resilience based clinical supervision to support transition to practice in newly qualified healthcare professionals. Nurs Educ Today. 2020;94:104564. https://doi.org/10.1016/j.nedt.2020.104564 .
Feerick A, Doyle L, Keogh B. Forensic mental health nurses’ perceptions of clinical supervision: a qualitative descriptive study. Issues Ment Health Nurs. 2021;42:682–9. https://doi.org/10.1080/01612840.2020.1843095 .
Corey G, Haynes RH, Moulton P, Muratori M. Clinical supervision in the helping professions: a practical guide. Alexandria, VA: American Counseling Association; 2021.
Sturman N, Parker M, Jorm C. Clinical supervision in general practice training: the interweaving of supervisor, trainee and patient entrustment with clinical oversight, patient safety and trainee learning. Adv Health Sci Educ. 2021;26:297–311. https://doi.org/10.1007/s10459-020-09986-7 .
Alfonsson S, Parling T, Spännargård Å, Andersson G, Lundgren T. The effects of clinical supervision on supervisees and patients in cognitive behavioral therapy: a systematic review. Cogn Behav Therapy. 2018;47(3):206–28. https://doi.org/10.1080/16506073.2017.1369559 .
Coelho M, Esteves I, Mota M, Pestana-Santos M, Santos MR, Pires R. Clinical supervision of the nurse in the community to promote quality of care provided by the caregiver: scoping review protocol. Millenium J Educ Technol Health. 2022;2:83–9. https://doi.org/10.29352/mill0218.26656 .
Toros K, Falch-Eriksen A. Structured peer group supervision: systematic case reflection for constructing new perspectives and solutions. Int Soc Work. 2022;65:1160–5. https://doi.org/10.1177/0020872820969774 .
Bifarin O, Stonehouse D. Clinical supervision: an important part of every nurse’s practice. Brit J Nurs. 2017;26(6):331–5. https://doi.org/10.12968/bjon.2017.26.6.331 .
Turner J, Simbani N, Doody O, Wagstaff C, McCarthy-Grunwald S. Clinical supervision in difficult times and at all times. Ment Health Nurs. 2022;42(1):10–3.
Martin P, Tian E, Kumar S, Lizarondo L. A rapid review of the impact of COVID-19 on clinical supervision practices of healthcare workers and students in healthcare settings. J Adv Nurs. 2022;78:3531–9. https://doi.org/10.1111/jan.15360 .
van Dam M, van Hamersvelt H, Schoonhoven L, Hoff RG, Cate OT, Marije P. Hennus. Clinical supervision under pressure: a qualitative study amongst health care professionals working on the ICU during COVID-19. Med Edu Online. 2023;28:1. https://doi.org/10.1080/10872981.2023.2231614 .
Martin P, Lizarondo L, Kumar S, Snowdon D. Impact of clinical supervision on healthcare organisational outcomes: a mixed methods systematic review. PLoS ONE. 2021;1611:e0260156. https://doi.org/10.1371/journal.pone.0260156 .
Article CAS Google Scholar
Hussein R, Salamonson Y, Hu W, Everett B. Clinical supervision and ward orientation predict new graduate nurses’ intention to work in critical care: findings from a prospective observational study. Aust Crit Care. 2019;325:397–402. https://doi.org/10.1016/j.aucc.2018.09.003 .
Love B, Sidebotham M, Fenwick J, Harvey S, Fairbrother G. Unscrambling what’s in your head: a mixed method evaluation of clinical supervision for midwives. Women Birth. 2017;30:271–81. https://doi.org/10.1016/j.wombi.2016.11.002 .
Berry S, Robertson N. Burnout within forensic psychiatric nursing: its relationship with ward environment and effective clinical supervision? J Psychiatr Ment Health Nurs. 2019;26:7–8. https://doi.org/10.1111/jpm.12538 .
Markey K, Murphy L, O’Donnell C, Turner J, Doody O. Clinical supervision: a panacea for missed care. J Nurs Manage. 2020;28:2113–7. https://doi.org/10.1111/jonm.13001 .
Brody AA, Edelman L, Siegel EO, Foster V, Bailey DE Jr., Bryant AL, Bond SM. Evaluation of a peer mentoring program for early career gerontological nursing faculty and its potential for application to other fields in nursing and health sciences. Nurs Outlook. 2016;64(4):332–8. https://doi.org/10.1016/j.outlook.2016.03.004 .
Bulman C, Forde-Johnson C, Griffiths A, Hallworth S, Kerry A, Khan S, Mills K, Sharp P. The development of peer reflective supervision amongst nurse educator colleagues: an action research project. Nurs Educ Today. 2016;45:148–55. https://doi.org/10.1016/j.nedt.2016.07.010 .
Pack M. Unsticking the stuckness’: a qualitative study of the clinical supervisory needs of early-career health social workers. Brit J Soc Work. 2015;45:1821–36. https://doi.org/10.1093/bjsw/bcu069 .
Bayliss J. Clinical supervision for palliative care. London: Quay Books; 2006.
Kenny A, Allenby A. Implementing clinical supervision for Australian rural nurses. Nurs Educ Pract. 2013;13(3):165–9. https://doi.org/10.1016/j.nepr.2012.08.009 .
MacLaren J, Stenhouse R, Ritchie D. Mental health nurses’ experiences of managing work-related emotions through supervision. J Adv Nurs. 2016;72:2423–34. https://doi.org/10.1111/jan.12995 .
Wilson HM, Davies JS, Weatherhead S. Trainee therapists’ experiences of supervision during training: a meta-synthesis. Clinl Psychol Psychother. 2016;23:340–51. https://doi.org/10.1002/cpp.1957 .
Noelker LS, Ejaz FK, Menne HL, Bagaka’s JG. Factors affecting frontline workers’ satisfaction with supervision. J Aging Health. 2009;21(1):85–101. https://doi.org/10.1177/0898264308328641 .
Download references
Acknowledgements
The research team would like to thank all participants for their collaboration, the HSE steering group members and Carmel Hoey, NMPDU Director, HSE West Mid West, Dr Patrick Glackin, NMPD Area Director, HSE West, Annette Cuddy, Director, Centre of Nurse and Midwifery Education Mayo/Roscommon; Ms Ruth Hoban, Assistant Director of Nursing and Midwifery (Prescribing), HSE West; Ms Annette Connolly, NMPD Officer, NMPDU HSE West Mid West.
The authors declare that there are no sources of funding associated with this paper.
Author information
Authors and affiliations.
Department of Nursing and Midwifery, Health Research Institute, University of Limerick, Limerick, Ireland
Owen Doody, Kathleen Markey, Claire O. Donnell & Louise Murphy
Department of Nursing and Midwifery, Sheffield Hallam University, Sheffield, UK
James Turner
You can also search for this author in PubMed Google Scholar
Contributions
OD: Conceptualization, Methodology, Formal analysis, Investigation, Writing - Original Draft, Writing - Review & Editing, Project administration, Funding acquisition. COD: Methodology, Formal analysis, Investigation, Writing - Original Draft, Writing - Review & Editing, Funding acquisition. KM: Methodology, Formal analysis, Investigation, Writing - Original Draft, Writing - Review & Editing, Funding acquisition. JT: Methodology, Formal analysis, Writing - Original Draft, Writing - Review & Editing. LM: Methodology, Formal analysis, Investigation, Writing - Original Draft, Writing - Review & Editing, Funding acquisition.
Corresponding author
Correspondence to Owen Doody .
Ethics declarations
Ethics approval and consent to participate.
This study was approved by two health service institutional review boards University Hospital Limerick (Ref: 091/19) and Galway University Hospitals (Ref: C.A. 2199). The study was conducted in accordance with the principles of the Declaration of Helsinki and all study details were fully disclosed to participants, who were assured of the voluntary nature of participation and withdrawal. The study questionnaires were coded, and identities were not disclosed to guarantee participants’ anonymity and all participants provided written informed consent before interviews.
Consent for publication
No identifying images or other personal or clinical details of participants are presented in this paper that would compromise anonymity and all participants were aware and informed through the Participant Information Leaflet that the data collected may be reported through article and/or conference publications and this was reiterated during the qualitative data collection stage.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary Material 1
Supplementary material 2, supplementary material 3, rights and permissions.
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/ .
Reprints and permissions
About this article
Cite this article.
Doody, O., Markey, K., Turner, J. et al. Clinical supervisor’s experiences of peer group clinical supervision during COVID-19: a mixed methods study. BMC Nurs 23 , 612 (2024). https://doi.org/10.1186/s12912-024-02283-3
Download citation
Received : 04 January 2024
Accepted : 22 August 2024
Published : 02 September 2024
DOI : https://doi.org/10.1186/s12912-024-02283-3
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Clinical supervision
BMC Nursing
ISSN: 1472-6955
- General enquiries: [email protected]
share this!
August 28, 2024
This article has been reviewed according to Science X's editorial process and policies . Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
Study finds people are consistently and confidently wrong about those with opposing views
by King's College London

Despite being highly confident that they can understand the minds of people with opposing viewpoints, the assumptions humans make about others are often wrong, according to new research from the Institute of Psychiatry, Psychology & Neuroscience (IoPPN) at King's College London, in partnership with the University of Oxford.
"Poorer representation of minds underpins less accurate mental state inference for out-groups" was published in Scientific Reports . The research explores the psychology behind why people come to the wrong conclusions about others, and suggests how society could start to change that.
In all, 256 participants were recruited from the U.S. and split evenly between those with left- and right-leaning political views. They were presented with various political statements (e.g. Immigrants are beneficial to society) and asked to rate on a 5-point scale how much they agreed with it (i.e. strongly agree to strongly disagree).
For each statement, the participant would then be presented with someone else's response to the same statement. If the two shared a similar opinion, they were deemed "in-group" to one another. If the two held different opinions, they were deemed "out-group" to each other.
The participant was then asked to predict the other person's response on a second statement (e.g. all women should have access to legal abortion), and to state their confidence in their answer, from "Not at all' to "Extremely."
Participants could then choose to receive up to five more of the other person's responses to different statements to help the participant build up a better idea—or "representation"—of the other person's mind. After receiving any further information, participants could update their initial prediction and reclarify their confidence on their final answer.
Analysis of the data found that, even though participants were prepared to seek out as much—and often more—information about someone they disagreed with, their predictions were consistently incorrect, even after receiving further information about them.
Participants demonstrated a high degree of confidence in their answers, suggesting that participants thought they had a good understanding of the people in their out-group, despite this not being the case. In comparison, participants could consistently make accurate predictions about those in their in-group with less information.
"Our study shows that people have a good understanding of people who are similar to themselves and their confidence in their understanding is well-placed. However, our understanding of people with different views to our own is demonstrably poor. The more confident we are that we can understand them, the more likely it is that we are wrong. People have poor awareness of their inability to understand people that differ from themselves," says Dr. Bryony Payne.
"There are clear consequences to this lack of awareness, and we have seen countless real-world examples. The recent UK riots were borne out of a small group of people who were probably very confident in their (mis)understanding of the views and beliefs of Muslims and asylum seekers , and these misconceptions are often fueled by disinformation on social media or echoed back to them by others within their in-group."
Dr. Caroline Catmur, Reader in Cognitive Psychology at King's IoPPN and the study's senior author, said, "We live in an increasingly polarized society and many people are very confident in their understanding of those who don't share their beliefs. However, our research shows that people are willing to reconsider once they are made aware of their mistakes.
"While there is no quick fix in a real-world setting, if everyone interacted with a more diverse group of people, talked directly to them and got to know them, it's likely we would understand each other better. Conversations with people who hold different beliefs could help challenge our incorrect assumptions about each other."
Journal information: Scientific Reports
Provided by King's College London
Explore further
Feedback to editors

Assorted, distinctive behavior of molten uranium salt revealed by neutrons
2 hours ago

Tropical forests face increased soil carbon loss due to climate change
14 hours ago
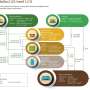
Beef industry can reduce emissions by up to 30%, says new research

Supercomputer simulations provide new insights into calcium-48's controversial nuclear magnetic excitation

Preventing cell damage: Working principle of proton-activated chloride channels revealed

The world's fastest single-shot 2D imaging technique films ultrafast dynamics in flames

Drosophila study discovers mechanism that could control longevity, cancer cell production
15 hours ago

SpaceX Polaris Dawn mission set to launch early Friday

Bioengineers develop protein assembly road map for nature-derived nanobubbles

Research shows 50-year generation gap in the bigmouth buffalo, Minnesota's longest-lived fish
Relevant physicsforums posts, definition of maoil.
7 hours ago
Favorite songs (cont.)
Sep 2, 2024
Purpose of the Roman bronze dodecahedrons: are you convinced?
Talent worthy of wider recognition, favorite mashups - all your favorites in one place, cover songs versus the original track, which ones are better.
Sep 1, 2024
More from Art, Music, History, and Linguistics
Related Stories

Study suggests ambivalence and polarized views can promote political violence
Jun 12, 2024

Lie-detection AI could provoke people into making careless accusations, researchers warn
Jun 27, 2024

Education level, social media skills linked to cancer fatalism
Jul 31, 2024

Why humans aren't as egocentric as you might think—new research
Oct 30, 2023
Radicals aren't good at knowing when they're wrong
Dec 17, 2018

How people go from vaccine supporters to vaccine advocates
Dec 6, 2022
Recommended for you

Simulation study explores how gift giving drives social change
16 hours ago

How new words arise in social media

The right to be wrong: How context or human rationality may influence our decisions
17 hours ago

Early exposure to diverse faces helps babies overcome prejudices later in life, study suggests

Warning labels from fact checkers work—even if you don't trust them—says study
20 hours ago

Study suggests gun-free zones do not attract mass shootings
Let us know if there is a problem with our content.
Use this form if you have come across a typo, inaccuracy or would like to send an edit request for the content on this page. For general inquiries, please use our contact form . For general feedback, use the public comments section below (please adhere to guidelines ).
Please select the most appropriate category to facilitate processing of your request
Thank you for taking time to provide your feedback to the editors.
Your feedback is important to us. However, we do not guarantee individual replies due to the high volume of messages.
E-mail the story
Your email address is used only to let the recipient know who sent the email. Neither your address nor the recipient's address will be used for any other purpose. The information you enter will appear in your e-mail message and is not retained by Phys.org in any form.
Newsletter sign up
Get weekly and/or daily updates delivered to your inbox. You can unsubscribe at any time and we'll never share your details to third parties.
More information Privacy policy
Donate and enjoy an ad-free experience
We keep our content available to everyone. Consider supporting Science X's mission by getting a premium account.
E-mail newsletter
- Credit cards
- View all credit cards
- Banking guide
- Loans guide
- Insurance guide
- Personal finance
- View all personal finance
- Small business
- Small business guide
- View all taxes
You’re our first priority. Every time.
We believe everyone should be able to make financial decisions with confidence. And while our site doesn’t feature every company or financial product available on the market, we’re proud that the guidance we offer, the information we provide and the tools we create are objective, independent, straightforward — and free.
So how do we make money? Our partners compensate us. This may influence which products we review and write about (and where those products appear on the site), but it in no way affects our recommendations or advice, which are grounded in thousands of hours of research. Our partners cannot pay us to guarantee favorable reviews of their products or services. Here is a list of our partners .
Survey: Many Americans Lack Confidence in Financial Decision-Making

Many, or all, of the products featured on this page are from our advertising partners who compensate us when you take certain actions on our website or click to take an action on their website. However, this does not influence our evaluations. Our opinions are our own. Here is a list of our partners and here's how we make money .
How much money should you have in your emergency fund? What percentage of your income should you be saving for retirement?
Financial questions like these can be high-stakes. And reaching the right decision on them can seem complex and difficult, in part because there’s just so much information out there.
If you feel daunted by making financial decisions like these, you’re not alone. Less than half (47%) of Americans feel confident in their ability to make good financial decisions, according to a recent NerdWallet survey conducted online by The Harris Poll in July.
Financial confidence grows with age and wealth
People’s confidence in their financial decision-making increases with their age, income and education.
Less than a third (30%) of Gen Zers (ages 18-27) say they are confident in their ability to make good financial decisions. Thirty-nine percent of Millennials (ages 28-43), 47% of Gen Xers (ages 44-59), and 62% of baby boomers (ages 60-78) say they are confident.
Just 38% of Americans with an annual household income of less than $50,000 reported feeling confident in their ability to make good financial decisions. That compares with 49% of those making $75,000-$99,999 and 55% of those making $100,000 and more.
It’s a similar story when it comes to education.
Thirty-seven percent of Americans with a high school diploma or less education reported feeling confident in their ability to make good financial decisions, while 45% of Americans who attended some college and 58% of Americans who graduated from college felt the same way.
Reliable information is key — and readily available
The first step in making smart financial decisions is knowing where to go to gather reliable information. And you likely already have access to many free or low-cost resources .
Financial institution: Consider starting with your bank or credit union. Many financial institutions offer online and in-person resources to help guide their customers to solid financial decisions. In addition to informational content related to the products they offer — such as checking accounts and certificates of deposit — employees on the other end of customer service phone numbers or in a local bank branch can provide answers to some of the more common and basic banking questions.
Employers: Many companies offer financial planning services to their employees — either through a financial planning service with which they partner or through the company that manages their retirement plan. If you’re uncertain whether your job offers this kind of perk, ask your human resources department.
Online brokerages: If you currently invest, there’s a good chance you can access educational materials and possibly even advisors through your brokerage. They can help with topics such as how to invest , how much to invest and how to help ensure you’re on track for retirement.
Nonprofit foundations or trade associations: Some financial advisors offer their services for free or at a reduced rate to people who might not otherwise be able to afford them. The Financial Planning Association is one example of a trade organization that offers pro bono financial planning services. Local community organizations and even public libraries may host financial education events, too.
Phone apps: There are also many free or low-cost apps you can use for tasks such as creating and sticking to a budget , checking your credit score and understanding what it means, and analyzing your credit card usage.
This survey was conducted online within the United States by The Harris Poll on behalf of NerdWallet from July 11-15, 2024, among 2,096 U.S. adults ages 18 and older. The sampling precision of Harris online polls is measured by using a Bayesian credible interval. For this study, the sample data is accurate to within +/- 2.5 percentage points using a 95% confidence level. For complete survey methodology, including weighting variables and subgroup sample sizes, please contact [email protected] .
NerdWallet disclaims, expressly and impliedly, all warranties of any kind, including those of merchantability and fitness for a particular purpose or whether the article’s information is accurate, reliable or free of errors. Use or reliance on this information is at your own risk, and its completeness and accuracy are not guaranteed. The contents in this article should not be relied upon or associated with the future performance of NerdWallet or any of its affiliates or subsidiaries. Statements that are not historical facts are forward-looking statements that involve risks and uncertainties as indicated by words such as “believes,” “expects,” “estimates,” “may,” “will,” “should” or “anticipates” or similar expressions. These forward-looking statements may materially differ from NerdWallet’s presentation of information to analysts and its actual operational and financial results.
On a similar note...

on Capitalize's website
Get Your Free Credit Score
Pay off debt: tools and tips, monthly 50/30/20 budget calculator.
- Open access
- Published: 04 September 2024
Comparing hospitalized adult patients with chronic anorexia nervosa with versus without prior hospitalizations
- Mary K. Martinelli 1 ,
- Colleen C. Schreyer 1 &
- Angela S. Guarda 1
Journal of Eating Disorders volume 12 , Article number: 132 ( 2024 ) Cite this article
Metrics details
Anorexia nervosa (AN) is a severe psychiatric disorder, from which recovery is often protracted. The role of prior specialized inpatient treatment on subsequent treatment attempts for adults with chronic AN and predictors of treatment response for severe and enduring AN (SE-AN) are needed to improve outcomes.
Participants ( N = 135) with chronic AN (ill ≥7 years) admitted to an integrated inpatient-partial hospitalization eating disorders (ED) unit with prior ED hospitalization(s) (+ PH; n = 100) were compared to those without prior ED hospitalizations (-PH; n = 35) on admission characteristics (BMI, length of illness, outpatient ED treatment history, symptomatology (ED, anxiety, and depressive), history of suicide attempts or non-suicidal self-injury (NSSI)), treatment motivation and recovery self-efficacy, and discharge outcomes (discharge BMI, rate of weight gain, length of stay, clinical improvement).
Groups were similar with regard to age, years ill, and admission BMI. The + PH group had lower desired weight, lifetime nadir BMI and self-efficacy for normative eating, and higher state and trait anxiety than the -PH group. +PH were also more likely to endorse history of NSSI and suicide attempt. Regarding discharge outcomes, most patients achieved weight restoration at program discharge (mean discharge BMI = 19.8 kg/m 2 ). Groups did not differ on rate of weight gain, likelihood of attending partial hospital, partial hospital length of stay, program discharge BMI, or likelihood of clinical improvement ( p ’s > 0.05) although inpatient length of stay was longer for the + PH group.
Conclusions
Participants with chronic AN + PH exhibited more severe psychiatric comorbidity and lower self-efficacy for normative eating than AN -PH, however short-term discharge outcomes were similar. Future research should determine whether weight restoration and targeting comorbidities impacts relapse risk or need for rehospitalization among chronic and severe + PH. Despite similar illness durations, those with chronic AN -PH may be able to transition to partial hospital earlier. Conversely there is risk of undertreatment of chronic AN + PH given the recent shift promoting briefer self-directed admissions for adults with SE-AN. Research comparing + PH and -PH adults with chronic AN may facilitate efforts to individualize care and characterize relapse risk following intensive treatment.
Plain English summary
Some individuals with longstanding anorexia nervosa (AN) remain ill despite multiple attempts at intensive treatment. Others reach a high level of specialty care (e.g. inpatient or residential) for the first time only late in their illness. This study compared 100 hospitalized patients with chronic AN (ill ≥ 7 years) who previously received specialty inpatient eating disorder care to 35 hospitalized patients with chronic AN and no prior intensive treatment. Participants completed questionnaires at admission and weight change and hospital course were assessed at program discharge by chart review. At admission, individuals with prior hospitalizations reported greater difficulties with anxiety and suicidal behavior, lower confidence for changing their eating habits, and lower desired body weight compared to those with no prior inpatient treatment. Both groups had similar weight change and clinical improvement during treatment with mean discharge BMI consistent with weight restoration. These outcomes suggest equivalent short term improvement and weight restoration for individuals with chronic AN regardless of whether they previously received inpatient treatment and call into question whether the recent shift to brief admissions for those with chronic and severe AN may result for some in undertreatment, given that weight restoration remains the strongest predictor of long-term recovery.
Anorexia nervosa (AN) is a severe, complex psychiatric disorder from which recovery is often protracted. An estimated 20% of individuals with AN experience a chronic or persistent course [ 1 ], often referred to as severe and enduring anorexia nervosa (SE-AN) [ 2 , 3 ]. Improving outcomes for SE-AN is critical given the medical sequelae, healthcare utilization costs, and high mortality associated with chronic AN [ 1 , 4 , 5 , 6 ]. Research aimed at clarifying the etiology, maintenance, and course of those with chronic AN is urgently needed to improve treatment efficacy.
One challenge is the lack of an accepted definition of SE-AN, with current definitions emphasizing illness duration (7 years being the most common duration cutoff but some advocating for as few as 3 years) [ 2 , 7 ]. Some definitions also require a history of non-response to evidence-based specialized eating disorder (ED) treatment [ 7 , 8 ]. Problematically, however, most that include this criterion do not clearly specify how to define an adequate attempt at treatment [ 8 ]. Is a previous failure of outpatient cognitive-behavioral therapy (CBT) or a brief hospitalization for medical stabilization sufficient? Or should failure include at least one past admission and achievement of weight restoration in an intensive behavioral specialty treatment program for eating disorders? Or in the case of those who leave intensive treatment against medical advice or due to other family or financial concerns, how many premature discharges from intensive treatment constitute treatment failure? Few empirical studies of SE-AN have incorporated measures of treatment history when defining groups [ 9 , 10 ], and results are mixed with some finding poorer outcomes among patients with previous ED treatment [ 11 , 12 , 13 ] and others not finding a relationship between history of previous treatment [ 14 ] or number of previous inpatient treatments [ 15 ] and outcomes.
The rationale for including treatment history in definitions of SE-AN is that individuals who do not improve, do not achieve remission, or quickly relapse following evidence-based treatment may represent a particularly vulnerable group for greater persistence of illness and for whom more targeted treatments are needed. Including prior treatment history in definitions of SE-AN is complicated, however. First, many individuals with diagnosable AN never seek treatment or receive inadequate treatment [ 16 ]. Others experience a long duration of untreated illness prior to engaging in evidence-based treatment [ 17 ] or engage in treatment, sometimes repeatedly, but drop out prematurely [ 18 ]. Potential obstacles to treatment include practical barriers (e.g., cost of treatment, wait times, geographic access to specialized care), stigma, low motivation to change, ambivalence or anxiety about intensive treatment, negative attitudes towards seeking help, low health literacy, and lack of social encouragement [ 19 , 20 , 21 , 22 , 23 ]. Additional barriers, such as low insight or lack of recognition of illness severity [ 19 , 20 , 23 ] may predict the severity or chronicity of AN [ 15 , 24 ]. Thus, those who do not seek or complete treatment or who have a long duration of untreated illness may themselves represent a group more vulnerable to chronic, severe AN. In one retrospective study, individuals with a longer duration of untreated illness were less likely to have achieved remission at 20-year follow-up [ 25 ]. Finally, another challenge in incorporating prior treatment attempts in the definition of SE-AN is the issue of how best to classify type and intensity of treatment (e.g., brief medical stabilization admissions versus achieving full weight restoration in a multidisciplinary intensive behavioral specialty program for eating disorders).
Prior studies often compare individuals with a long duration of illness to those with early-stage AN (e.g., 26 , 27 , 28 , 29 ). Given that individuals with longer duration of illness are more likely to have engaged in prior treatment [ 11 ], it remains unclear whether long illness duration, history of treatment non-response, or both should be included in definitions of SE-AN. On one hand, a longer illness duration may make it more difficult to recover from AN regardless of prior treatment history due to factors such as greater genetic risk, greater physical complications [ 30 ], diminished social and psychological functioning [ 31 , 32 ], and increased habit strength of AN behaviors [ 31 , 33 ]. On the other hand, experiencing prior treatment non-response may uniquely influence subsequent treatment outcomes, by leading to diminished motivation or confidence in treatment [ 34 , 35 ]. There may additionally be iatrogenic risks of treatment (e.g. traumatic experiences of care, or institutionalization) that contribute to persistent illness or treatment avoidance.
Investigating the role of prior treatment attempts independent of illness duration may help clarify definitional criteria and utility of the SE-AN label and inform treatment for severely and chronically ill adults with AN for whom treatment options are often more limited and evidence-based approaches sparse [ 9 , 10 ]. This exploratory study of inpatients admitted to an integrated inpatient partial hospitalization ED program compared patients with long-term AN (ill ≥ 7 years) plus a prior history of inpatient ED behavioral treatment (+ PH) to patients with long-term AN seeking inpatient treatment for the first time (-PH). Groups were compared on admission characteristics, treatment outcomes, and hospital course. Given the exploratory nature of this study, no specific hypotheses were generated.
Participants and procedure
Data were collected as part of an ongoing, Institutional Review Board approved longitudinal study of response to intensive treatment in patients diagnosed with EDs. All first admissions to the Johns Hopkins Eating Disorder Inpatient-Partial Hospitalization Program between 2003 and 2022 were invited to participate. Eligible participants were individuals with AN who completed at least seven days of treatment, endorsed a length of illness ≥ 7 years at admission, provided informed consent, and completed questionnaires. Participants ( N = 135) were divided into two groups: those who reported no previous specialized high level of ED care or hospitalization (inpatient or residential) at admission (-PH; n = 35) and those who endorsed a history of at least one prior specialized ED inpatient treatment (+ PH; n = 100).
Participants were diagnosed at hospital admission by trained raters, supervised by a licensed clinical psychologist, using the ED section of the Structured Clinical Interview for DSM-5 (SCID-5-RV) [ 36 ]. Participants admitted prior to 2015 were evaluated using the SCID-IV-TR, and diagnoses were later re-assessed using DSM-5 criteria. Participants completed a battery of self-report measures within the first week of admission. Clinical hospital course data were abstracted from the electronic medical record.
Treatment protocol
The eating disorders program follows a structured behavioral treatment protocol delivered within a multidisciplinary integrated, inpatient-partial hospitalization stepdown program. Primary treatment targets include rapid weight restoration for underweight patients and normalization of eating behaviors. Cognitive behavioral therapy (CBT) and dialectical behavior therapy (DBT) informed psychotherapeutic interventions are delivered primarily in group format. Participants admitted below target weight were placed on a previously described standardized weight gain 100% meal-based nutritional protocol [ 37 ]. See Guarda et al. [ 38 ] for additional description of the treatment program.
Demographic and clinical variables
Age, race, sex, marital status, income, education, and current employment were collected at admission via participant questionnaires. Measures pertaining to ED treatment history and illness course, including age of ED onset, length of illness (years), number of hospitalization(s) on a specialized ED unit prior to this admission, history of outpatient ED treatment, lifetime nadir body mass index (BMI), age at lifetime nadir BMI, and desired weight, were also gathered at admission. The + PH group was asked to report the length of stay (days) of their longest prior hospitalization for an ED.
Height and gowned morning weight at program admission and discharge were used to calculate admission and discharge BMI. Individual target weight was set as a four-pound range (1.8 kg) based on the patient’s age, sex, and height centered on a BMI of 20.5 kg/m 2 for patients over age 25 [ 37 ]. For those aged 18–24, target weight was adjusted by subtracting one pound (0.45 kg) per year of age below 25.
Motivational factors
The University of Rhode Island Change Assessment (URICA) [ 39 ], a self-report measure of motivational readiness to change, was administered at admission. A 12-item version of the measure was adapted from the alcohol reduction version [ 40 ]. Responses were rated on a 5-point scale from 1 (Strongly Disagree) to 5 (Strongly Agree) and used to compute four Stage of Change subscales: pre-contemplation, contemplation, preparation or action, and maintenance. The URICA Readiness Score was computed by summing the contemplation, preparation or action, and maintenance subscales, and then subtracting the precontemplation subscale. Higher readiness scores indicate greater readiness to change.
Current ED symptomatology
The Eating Disorder Inventory-2 (EDI-2) [ 41 ] is a 91-item self-report questionnaire designed to measure psychological features and behavioral traits commonly associated with AN and bulimia nervosa (BN). The Drive for Thinness, Bulimia, and Body Dissatisfaction subscales were included in the current study. The EDI-2 has demonstrated good reliability and validity in individuals with EDs [ 42 ]. Internal consistencies in this study ranged from good to excellent (Drive for Thinness, α = 0.88; Bulimia, α = 0.92; Body Dissatisfaction, α = 0.91). The Eating Disorder Recovery Self-Efficacy Questionnaire (EDRSQ) [ 43 ] is a 23-item self-report measure of self-efficacy to cope with eating disorder behaviors and attitudes. The Normative Eating Self-Efficacy subscale measures confidence to eat without engaging in disordered behavior and without undue distress. The Body Image Self-Efficacy subscale measures confidence to maintain a realistic body image and not place undue influence of body weight and shape on self-esteem. The EDRSQ has demonstrated good validity and reliability [ 43 , 44 ]. In the current study, internal consistencies for Normative Eating and Body Image were excellent (α = 0.96, α = 0.90). Frequency of Compensatory Behaviors was assessed via three self-report items at admission; participants rated their frequency of vomiting, laxative use to control weight, and excessive exercise over the past 8 weeks on a scale from 1 (Never) to 7 (More than once a day).
Comorbid psychopathology
The State-Trait Anxiety Inventory (STAI) [ 45 ] is a 40-item self-report scale measuring anxiety experienced in the moment (state anxiety) and as a stable personality trait (trait anxiety). The STAI has demonstrated good reliability and validity [ 46 , 47 ]. The STAI state (STAI-S) and trait (STAI-T) subscale total raw scores demonstrated excellent internal consistencies in this study (α = 0.94, α = 0.91). Beck Depression Inventory-II (BDI-II) [ 48 ], a 21-item self-report measure of depression symptoms, has strong psychometric properties, including internal consistency and factor validity [ 49 ]. Internal consistency was excellent in the current study (Cronbach’s α = 0.91). Non-Suicidal Self-Injury (NSSI) was measured dichotomously as history of self-injurious behavior. Participants were asked if they had ever engaged in the following self-injurious behaviors (yes or no): cutting, burning, bruising, scratching. Due to low rates of endorsement for most of these behaviors and to avoid potential problems caused by zero-inflated data, the current study used only the responses for cutting to represent NSSI, as this was the most frequently endorsed behavior of those listed. Suicide Attempt was measured dichotomously with a yes or no to, “Have you ever attempted suicide in the past?”
Hospital course (discharge variables)
Length of Stay (days) for inpatient and partial hospital was calculated by subtracting admission date from discharge date for each participant. Reason for Discharge was dichotomized into “for clinical improvement” versus “not for clinical improvement” with the latter including discharge for non-compliance, elopement, financial reasons, patient/family reasons, or transfer. Partial Hospital Attendance was examined as percentage of participants per group transitioning to an integrated stepdown partial hospitalization program following inpatient treatment. Rate of Weight Gain was measured as kilograms gained per week and computed by dividing total weight gained in kilograms by the number of weeks spent on a weight gain nutritional protocol.
Data analysis
Data were analyzed in SPSS version 28. Mann-Whitney U tests (continuous variables) and chi-square analyses (dichotomous variables) were conducted to explore differences between groups on demographic, clinical, and self-report measures at admission and discharge. Mann-Whitney U tests were chosen in lieu of independent-samples t -tests due to unequal sample sizes between groups and non-normality of variables. To test for differences between groups in discharge BMI, a linear regression model was conducted to control for admission BMI. Differences between groups were determined by examining the significance value and confidence intervals for the group variable coefficient. To account for non-normality and unequal sample sizes between groups, robust statistical methods for regression were employed (bootstrapping with confidence intervals and standard errors based on 1000 bootstrapped samples). All available data was utilized, and missing data is reported for each analysis.
Sociodemographic characteristics
Descriptive data for participant sociodemographic characteristics are presented in Table 1 . The majority of the sample was White (94.8%) and female (97.8%) with a mean age of 36.9 ( SD = 11.2, range = 18–70) years. Participants with prior hospitalizations were more likely to be single or never married ( n = 66, 67%) compared to those in the first-time hospitalization group ( n = 14, 40%). Groups did not differ on age, sex, race, education, source of income, or current employment. The sample was highly educated with 90% of participants having at least some college education, however approximately half the sample reported their primary source of income as coming from social security or disability payments and only 28% earned income from salary/wages.
Weight variables and ED history at admission
Results of analyses comparing groups by weight and ED history at admission are presented in Table 2 . Both groups had similar age and length of illness at admission. The mean admission BMI for the sample was 15.52 kg/m 2 ( SD = 1.98). Groups did not significantly differ on admission BMI, however participants in the + PH group endorsed a lower desired body weight ( Mdn = 45.35 kg) compared to the -PH group ( Mdn = 49.89 kg) and a lower lifetime nadir BMI ( Mdn = 13.60) compared to the -PH group ( Mdn = 15.01). Groups did not differ with regard to age of lifetime nadir BMI ( M = 30.41, SD = 11.35), age of ED onset ( M = 17.92, SD = 6.89), or length of illness ( M = 19.01, SD = 9.84). The + PH group was significantly more likely to have received outpatient ED treatment, with 85% of the + PH group endorsing a history of outpatient ED treatment compared to 63% in the -PH group.
Participants in the + PH group were asked to respond to a multiple-choice question that queried them on the length of stay for their longest previous ED admission: 67% reported at least one prior admission lasting more than 30 days and only 8% reported that their longest prior stay was less than 15 days. These findings indicate that the majority of + PH participants had at least one prolonged hospitalization prior to the current admission.
Motivation at admission
With regard to treatment motivation, no differences between groups were observed for URICA Readiness Score at admission (Table 2 ). The majority of the sample fell within the pre-contemplation or contemplation stages of change ( n = 104, 77.6%) as opposed to the preparation or action stage of change ( n = 30, 22.4%).
ED symptomatology at admission
Results from analyses comparing groups by AN subtype and ED symptomatology at admission are displayed in Table 2 . 64% of the sample was diagnosed with AN-BP ( n = 86) and 36% was diagnosed with AN-R ( n = 49). The proportion of AN-R subtype vs. AN-BP subtype did not differ by group. Groups did not differ on frequency of vomiting, laxative use, or excessive exercise over the past 8 weeks. The full sample reported vomiting ( M = 3.45, SD = 2.63) and excessive exercise ( M = 3.37, SD = 2.42) somewhere between several times per month and once per week, on average, and engaged in laxative use ( M = 2.21, SD = 2.11) somewhere between once a month and several times per month, on average. Regarding self-report ED measures at admission, participants in the + PH group endorsed lower self-efficacy for normative eating ( Mdn = 1.64) compared to participants in the -PH group ( Mdn = 2.50). No differences between groups were observed for EDI-2 subscales or EDRSQ body image self-efficacy.
Comorbid psychopathology at admission
Group comparisons on comorbid psychopathology are presented in Table 3 . The majority of the sample ( n = 75, 56%) met cutoffs for severe depression on the BDI-II (scores ≥ 29) at admission. No differences between groups were observed for BDI-II total ( M = 29.88, SD = 12.55). With regard to anxiety, only 59% of the sample ( n = 79) had data available on the STAI (60% in the -PH group and 58% in the + PH group) as the STAI was added to the study protocol in 2008. Using all available data, results show that the + PH group had significantly higher State Anxiety total scores ( Mdn = 63) and Trait Anxiety total scores ( Mdn = 65) compared to the -PH group (STAI-S: Mdn = 52; STAI-T: Mdn = 57). Of the participants with valid STAI data, approximately 47% and 65% fell into the clinically significant range (i.e., T-score ≥ 75) for state and trait anxiety, respectively. Participants in the + PH group were also significantly more likely to endorse a history of suicide attempt and NSSI (cutting) compared to the -PH group.
Discharge outcomes and hospital course
Results from the regression model testing whether group membership at admission (+ PH or -PH) was associated with BMI at program discharge, controlling for admission BMI, are displayed in Table 4 . Across the sample, the average BMI at discharge was 19.81 kg/m 2 ( SD = 1.99). Group membership at admission was not associated with BMI at discharge controlling for BMI at admission.
Results of Mann-Whitney U tests and Chi-square analyses comparing groups on discharge outcomes are presented in Table 5 . No group differences were observed for rate of weight gain during treatment (inpatient: M = 1.91 kg/week, SD = 0.88; partial hospital: M = 1.29 kg/week, SD = 0.68), however, individuals in the + PH group had a longer length of inpatient stay ( Mdn = 37 days) compared to those in the -PH group ( Mdn = 30 days). No group differences were observed for partial hospital length of stay ( M = 33.72 days, SD = 19.79) or likelihood of attending partial hospital, with 65% of the total sample transitioning from the inpatient to the partial hospitalization program. Groups also did not differ with regard to likelihood of discharge for clinical improvement, with 52% of the full sample classified as discharged for clinical improvement.
Effective treatments for adults with SE-AN are currently lacking and opinion is divided on how to best meet the needs of this chronically ill patient group characterized by high rates of morbidity, mortality, and functional impairment and lower quality of life [ 2 , 4 , 50 ]. Amongst psychiatric conditions, many patients with SE-AN account for disproportionate health care utilization costs [ 51 , 52 ]. Long-term follow up studies, however, suggest that a majority of individuals with chronic AN will eventually recover, sometimes following several decades of illness, or multiple prolonged hospitalizations [ 53 ]. Weight restoration is the strongest predictor of recovery from AN, however relapse is not uncommon even among those discharged at a normative BMI [ 34 ]. It is unclear, however, whether successful weight restoration in a specialized inpatient behavioral treatment program confers longer term therapeutic advantages compared to brief admissions for medical stabilization or outpatient therapy alone for this group of patients. This is an important question for the field given the recent focus of the SE-AN literature on approaches to care that prioritize patient autonomy and choice, and focus on maximizing quality of life [ 3 ]. These priorities, along with economic forces and limited availability of intensive treatment, especially for severely and chronically ill adults with AN, have contributed to a shift favoring brief patient-directed admissions aimed at medical stabilization in lieu of repeated prolonged hospitalizations targeting full weight restoration and normalization of eating behavior. The purpose of the current study was to contribute to ongoing efforts within the field to clarify definitional criteria and utility of the SE-AN label to improve clinical decision-making and develop more effective treatments for chronic AN.
We compared voluntarily hospitalized adult patients with chronic AN who had previously received inpatient treatment to those hospitalized for the first time on admission characteristics, treatment outcomes, and hospital course. Sample descriptives and demographics were consistent with an adult SE-AN cohort. Average age was mid- to late thirties, average length of illness was 19 years, lifetime nadir BMI was reflective of extreme AN and the cohort had elevated rates of disability and functional impairment. Despite a high-level of educational attainment, the majority relied on social security or family or spousal financial support. Groups were similar at admission on age, duration of illness, BMI, ED and depressive symptomatology, and on motivation (readiness to change), although some cross-sectional group differences were observed suggestive of lower psychopathology in the -PH group on several admission variables including desired weight, lifetime nadir BMI, self-efficacy for normative eating, anxiety symptomatology, history of non-suicidal self-injury, and past suicide attempts. These differences may prove helpful in distinguishing illness course amongst those with chronic AN, independent of illness duration. For example, those with a lower lifetime nadir BMI in the + PH group may have been more likely to be identified or pressured into intensive treatment earlier by healthcare providers or social supports due to unstable labs or other medical or psychological symptoms. The -PH group were more likely to be married; having a spouse may reflect lower psychopathology or represent a protective factor by decreasing isolation and providing support. Conversely, a spouse may inadvertently accommodate the illness thereby facilitating treatment avoidance despite illness severity. The presence of greater psychiatric comorbidity (anxiety, NSSI, suicide) in the + PH vs. the –PH group is consistent with research indicating that comorbid mental health problems facilitate earlier help-seeking among individuals with EDs [ 16 ]. Higher psychiatric comorbidity may also explain the + PH group’s longer length of hospitalization despite similar admission BMI and rate of weight gain to the -PH group. Specific symptoms, for example greater behavioral dysregulation, comorbid anxiety, or self-injury, may have influenced the treatment team’s clinical assessment of readiness and safety to transition to a lower level of care. Despite these differences, both groups achieved similar short-term weight restoration and clinical outcomes at discharge.
Findings are consistent with previous research indicating that illness duration is not a good indicator for likelihood of weight restoration [ 26 , 27 ] and suggest prior non-response to inpatient treatment in adults with SE-AN is not a strong predictor of subsequent short-term weight restoration and discharge outcomes. However, further research is clearly needed to clarify longer term outcomes (e.g., relapse rates 1-year post-discharge) following weight restoration among those with SE-AN.
Study findings have several important clinical and research implications. Some have called for alternative treatment approaches for individuals with SE-AN or for those with prior treatment non-response or relapsing illness [ 54 ]. These alternative approaches often emphasize harm reduction, focus on improving quality of life, and de-emphasize weight restoration and typically do not achieve weight restoration despite statistical increases in BMI [ 50 , 55 , 56 ]. More recently a focus on palliative care as a primary approach for some patients with SE-AN has also been promoted [ 57 ] and in rare cases recommendations have included consideration of hospice care, or in the extreme physician assisted suicide or medical aid in dying for some individuals with SE-AN [ 58 ]. The need for a primary palliative approach in SE-AN, however, remains controversial [ 59 ]. Principles of palliative care are already inherent in the competent practice of psychotherapy, including focus on quality of life and wellbeing as well as more targeted behavioral, supportive, and motivational approaches that promote clinical improvement and foster hope in eventual recovery.
Findings from this exploratory study suggest caution in deploying a harm reduction approach for individuals with chronic AN. Regardless of prior treatment history, most participants with long-term AN met criteria for weight restoration with an average discharge BMI of 19.8 kg/m 2 across groups. The timing or likelihood of AN recovery can be difficult to predict, and the possibility of eventual recovery even in protracted cases of AN [ 11 , 26 , 27 , 60 ] argues for maintaining an optimistic stance even for those who may not have responded to prior attempts at intensive treatment. As others have noted, we lack a reliable staging model for AN predictive of prognosis or of intensive treatment response [ 7 , 61 ]. Similarly, a uniform definition for what comprises optimal evidence-based multidisciplinary inpatient treatment remains elusive and confounds any definition of SE-AN based on past treatment non-response. Both treatment length and context matter. Brief admissions for medical stabilization are unlikely to be as effective as achievement of full weight restoration in a multidisciplinary behavioral specialty treatment program for eating disorders. And for those who achieve weight restoration yet subsequently relapse, we do not know whether each successful cycle through treatment decreases both the gravitational pull of the eating disorder and the risk of relapse. AN is increasingly seen as a disorder of learning [ 31 , 33 ] in which repeated behaviors become increasingly automatic and cue driven over time. Recovery, however, may also be a process of learning and repeated cycles of treatment associated with weight restoration may incrementally increase likelihood of eventual recovery. Qualitative interviews of recovered individuals with SE-AN and longitudinal studies are needed to assess this question. We do not know, for example, whether skills learned in prior treatment can be implemented by patients at a later date when motivation for recovery increases.
This study has several important limitations. Missing data for some variables as well as a limited sample size in the -PH group resulted in unequal sample sizes between groups. Measures were taken during data analyses to address these issues; however, results should be replicated with larger sample sizes and multisite research. Two central limitations relate to challenges presented by the lack of an accepted definition of SE-AN [ 2 ]. We based duration of illness ≥ 7 years on patients’ recall of the “age symptoms started to interfere with functioning”. Others, however, have defined illness onset as age at which all DSM diagnostic criteria are first met. Second, there is no accepted definition of what constitutes prior intensive treatment [ 3 , 62 ]. We focused on history of inpatient ED treatment consistent with several extant studies [ 12 , 63 ] but did not have information as to whether past treatments included achievement of weight restoration or were ended prematurely. This is especially significant given that the former remains the best predictor of recovery for AN [ 64 ]. Approximately two thirds of the -PH group had a history of outpatient ED treatment however close to one-third were treatment naïve. Future studies should also assess factors that may contribute to longer duration of untreated illness (e.g., lack of availability of specialized treatment units, inadequate insurance coverage) and/or individual factors (e.g., treatment anxiety or avoidance, low motivation).
Although correlational and exploratory in nature, this study provides novel contributions to our understanding of intensive treatment for adults with chronic AN. Study findings help inform our understanding of differences in presenting characteristics and treatment course for individuals with chronic AN who have never been admitted compared to those with previous specialized ED hospitalizations. In the absence of a meaningful construct or definition of evidence-based intensive treatment, we believe these data support continued attempts to encourage patients to engage in active treatment with the goal of normalizing eating and weight control behaviors, treating co-occurring psychiatric conditions, restoring weight, and improving quality of life and functional level. Results support hopefulness for a good response to treatment even in those with chronic AN, whether or not they have received prior intensive treatment and reinforce the need for longitudinal studies of SE-AN that assess treatment course and predictors of outcome.
Data availability
The data that support the findings of this study are available on request from the corresponding author. The data are not publicly available due to privacy or ethical restrictions.
Abbreviations
- Anorexia nervosa
Anorexia nervosa, restricting type
Anorexia nervosa, binge/purge type
Severe and enduring anorexia nervosa
Eating disorder
Prior hospitalization
No prior hospitalization
Body mass index
Non-suicidal self-injury
Steinhausen HC. The outcome of anorexia nervosa in the 20th century. Am J Psychiatry. 2002;159(8):1284–93.
PubMed Google Scholar
Broomfield C, Stedal K, Touyz S, Rhodes P. Labeling and defining severe and enduring anorexia nervosa: a systematic review and critical analysis. Int J Eat Disord. 2017;50(6):611–23.
Wonderlich SA, Bulik CM, Schmidt U, Steiger H, Hoek HW. Severe and enduring anorexia nervosa: update and observations about the current clinical reality. Int J Eat Disord. 2020;53(8):1303–12.
Agras WS. The consequences and costs of the eating disorders. Psychiatr Clin North Am. 2001;24(2):371–9.
Fichter MM, Quadflieg N. Mortality in eating disorders - results of a large prospective clinical longitudinal study. Int J Eat Disord. 2016;49(4):391–401.
Fichter MM, Quadflieg N, Hedlund S. Twelve-year course and outcome predictors of anorexia nervosa. Int J Eat Disord. 2006;39(2):87–100.
Hay P, Touyz S. Classification challenges in the field of eating disorders: can severe and enduring anorexia nervosa be better defined? J Eat Disord. 2018;6:41.
PubMed PubMed Central Google Scholar
Broomfield C, Noetel M, Stedal K, Hay P, Touyz S. Establishing consensus for labeling and defining the later stage of anorexia nervosa: a Delphi study. Int J Eat Disord. 2021;54(10):1865–74.
Zhu J, Hay PJ, Yang Y, Le Grange D, Lacey JH, Lujic S, et al. Specific psychological therapies versus other therapies or no treatment for severe and enduring anorexia nervosa. Cochrane Database Syst Rev. 2023;8(8):CD011570.
Zhu J, Yang Y, Touyz S, Park R, Hay P. Psychological treatments for people with severe and Enduring Anorexia Nervosa: a Mini Review. Front Psychiatry. 2020;11:206.
Fernandez-Aranda F, Treasure J, Paslakis G, Aguera Z, Gimenez M, Granero R, et al. The impact of duration of illness on treatment nonresponse and drop-out: exploring the relevance of enduring eating disorder concept. Eur Eat Disord Rev. 2021;29(3):499–513.
Fichter MM, Quadflieg N, Crosby RD, Koch S. Long-term outcome of anorexia nervosa: results from a large clinical longitudinal study. Int J Eat Disord. 2017;50(9):1018–30.
Zipfel S, Lowe B, Reas DL, Deter HC, Herzog W. Long-term prognosis in anorexia nervosa: lessons from a 21-year follow-up study. Lancet. 2000;355(9205):721–2.
Wildes JE, Forbush KT, Hagan KE, Marcus MD, Attia E, Gianini LM, et al. Characterizing severe and enduring anorexia nervosa: an empirical approach. Int J Eat Disord. 2017;50(4):389–97.
Errichiello L, Iodice D, Bruzzese D, Gherghi M, Senatore I. Prognostic factors and outcome in anorexia nervosa: a follow-up study. Eat Weight Disord. 2016;21(1):73–82.
Hart LM, Granillo MT, Jorm AF, Paxton SJ. Unmet need for treatment in the eating disorders: a systematic review of eating disorder specific treatment seeking among community cases. Clin Psychol Rev. 2011;31(5):727–35.
Neubauer K, Weigel A, Daubmann A, Wendt H, Rossi M, Lowe B, et al. Paths to first treatment and duration of untreated illness in anorexia nervosa: are there differences according to age of onset? Eur Eat Disord Rev. 2014;22(4):292–8.
Wallier J, Vibert S, Berthoz S, Huas C, Hubert T, Godart N. Dropout from inpatient treatment for anorexia nervosa: critical review of the literature. Int J Eat Disord. 2009;42(7):636–47.
Ali K, Farrer L, Fassnacht DB, Gulliver A, Bauer S, Griffiths KM. Perceived barriers and facilitators towards help-seeking for eating disorders: a systematic review. Int J Eat Disord. 2017;50(1):9–21.
Ali K, Fassnacht DB, Farrer L, Rieger E, Feldhege J, Moessner M, et al. What prevents young adults from seeking help? Barriers toward help-seeking for eating disorder symptomatology. Int J Eat Disord. 2020;53(6):894–906.
Hamilton A, Mitchison D, Basten C, Byrne S, Goldstein M, Hay P, et al. Understanding treatment delay: perceived barriers preventing treatment-seeking for eating disorders. Aust N Z J Psychiatry. 2022;56(3):248–59.
Regan P, Cachelin FM, Minnick AM. Initial treatment seeking from professional health care providers for eating disorders: a review and synthesis of potential barriers to and facilitators of first contact. Int J Eat Disord. 2017;50(3):190–209.
Weigel A, Rossi M, Wendt H, Neubauer K, von Rad K, Daubmann A, et al. Duration of untreated illness and predictors of late treatment initiation in anorexia nervosa. J Public Health. 2014;22(6):519–27.
Google Scholar
Greenfeld DG, Anyan WR, Hobart M, Quinlan DM, Plantes M. Insight into illness and outcome in anorexia nervosa. Int J Eat Disord. 1991;10(1):101–9.
Andres-Pepina S, Plana MT, Flamarique I, Romero S, Borras R, Julia L, et al. Long-term outcome and psychiatric comorbidity of adolescent-onset anorexia nervosa. Clin Child Psychol Psychiatry. 2020;25(1):33–44.
Calugi S, El Ghoch M, Dalle Grave R. Intensive enhanced cognitive behavioural therapy for severe and enduring anorexia nervosa: a longitudinal outcome study. Behav Res Ther. 2017;89:41–8.
Raykos BC, Erceg-Hurn DM, McEvoy PM, Fursland A, Waller G. Severe and enduring anorexia nervosa? Illness severity and duration are unrelated to outcomes from cognitive behaviour therapy. J Consult Clin Psychol. 2018;86(8):702–9.
Takakura S, Aso CS, Toda K, Hata T, Yamashita M, Sudo N. Physical and psychological aspects of anorexia nervosa based on duration of illness: a cross-sectional study. Biopsychosoc Med. 2019;13:32.
Redgrave GW, Schreyer CC, Coughlin JW, Fischer LK, Pletch A, Guarda AS. Discharge body Mass Index, not illness chronicity, predicts 6-Month Weight Outcome in patients hospitalized with Anorexia Nervosa. Front Psychiatry. 2021;12:641861.
Robinson P. Severe and enduring eating disorders: recognition and management. Adv Psychiatr Treat. 2018;20(6):392–401.
Treasure J, Willmott D, Ambwani S, Cardi V, Clark Bryan D, Rowlands K et al. Cognitive interpersonal model for Anorexia Nervosa Revisited: the perpetuating factors that contribute to the development of the severe and Enduring Illness. J Clin Med. 2020;9(3).
Arkell J, Robinson P. A pilot case series using qualitative and quantitative methods: biological, psychological and social outcome in severe and enduring eating disorder (anorexia nervosa). Int J Eat Disord. 2008;41(7):650–6.
Davis L, Walsh BT, Schebendach J, Glasofer DR, Steinglass JE. Habits are stronger with longer duration of illness and greater severity in anorexia nervosa. Int J Eat Disord. 2020;53(5):413–9.
Berends T, Boonstra N, Van Elburg A. Relapse in anorexia nervosa: a systematic review and meta-analysis. Curr Opin Psychiatry. 2018;31(6):445–55.
Carter JC, Mercer-Lynn KB, Norwood SJ, Bewell-Weiss CV, Crosby RD, Woodside DB, et al. A prospective study of predictors of relapse in anorexia nervosa: implications for relapse prevention. Psychiatry Res. 2012;200(2–3):518–23.
First MB, Williams JB. Structured clinical interview for DSM-5: Research Version (SCID-5-RV): Biometrics Research, Psychiatry. Columbia University at the New York State; 2017.
Redgrave GW, Coughlin JW, Schreyer CC, Martin LM, Leonpacher AK, Seide M, et al. Refeeding and weight restoration outcomes in anorexia nervosa: challenging current guidelines. Int J Eat Disord. 2015;48(7):866–73.
Guarda AS, Cooper M, Pletch A, Laddaran L, Redgrave GW, Schreyer CC. Acceptability and tolerability of a meal-based, rapid refeeding, behavioral weight restoration protocol for anorexia nervosa. Int J Eat Disord. 2020;53(12):2032–7.
McConnaughy EA, Prochaska JO, Velicer WF. Stages of change in psychotherapy: measurement and sample profiles. Psychotherapy: Theory Res Pract. 1983;20(3):368.
Soderstrom CA, DiClemente CC, Dischinger PC, Hebel JR, McDuff DR, Auman KM, et al. A controlled trial of brief intervention versus brief advice for at-risk drinking trauma center patients. J Trauma. 2007;62(5):1102–11. discussion 11 – 2.
Garner DM. Eating disorder Inventory-2: Professional Manual. Psychological Assessment Resources; 1991.
Clinton D, Birgegard A. Classifying empirically valid and clinically meaningful change in eating disorders using the eating disorders Inventory, version 2 (EDI-2). Eat Behav. 2017;26:99–103.
Pinto AM, Heinberg LJ, Coughlin JW, Fava JL, Guarda AS. The Eating Disorder Recovery Self-Efficacy Questionnaire (EDRSQ): change with treatment and prediction of outcome. Eat Behav. 2008;9(2):143–53.
Marinilli Pinto A, Guarda AS, Heinberg LJ, Diclemente CC. Development of the eating disorder recovery self-efficacy questionnaire. Int J Eat Disord. 2006;39(5):376–84.
Spielberger C, Gorsuch R, Lushene R, Vagg P, Jacobs G. State trait anxiety inventory for adults manual. Palo Alto. CA: Mind Garden; 1983.
Guillen-Riquelme A, Buela-Casal G. [Meta-analysis of group comparison and meta-analysis of reliability generalization of the state-trait anxiety Inventory Questionnaire (STAI)]. Rev Esp Salud Publica. 2014;88(1):101–12.
Oei TP, Evans L, Crook GM. Utility and validity of the STAI with anxiety disorder patients. Br J Clin Psychol. 1990;29(4):429–32.
Beck AT, Steer RA, Brown G. Beck depression inventory–II. Psychological assessment; 1996.
Steer RA, Clark DA. Psychometric characteristics of the Beck Depression Inventory-II with college students. Meas Evaluation Couns Dev. 1997;30(3):128–36.
Hay PJ, Touyz S, Sud R. Treatment for severe and enduring anorexia nervosa: a review. Aust N Z J Psychiatry. 2012;46(12):1136–44.
Kaye WH, Bulik CM. Treatment of patients with Anorexia Nervosa in the US-A Crisis in Care. JAMA Psychiatry. 2021;78(6):591–2.
Guarda AS, Schreyer CC, Fischer LK, Hansen JL, Coughlin JW, Kaminsky MJ, et al. Intensive treatment for adults with anorexia nervosa: the cost of weight restoration. Int J Eat Disord. 2017;50(3):302–6.
Eddy KT, Tabri N, Thomas JJ, Murray HB, Keshaviah A, Hastings E, et al. Recovery from Anorexia Nervosa and Bulimia Nervosa at 22-Year Follow-Up. J Clin Psychiatry. 2017;78(2):184–9.
Yager J, Gaudiani JL, Treem J. Eating disorders and palliative care specialists require definitional consensus and clinical guidance regarding terminal anorexia nervosa: addressing concerns and moving forward. J Eat Disord. 2022;10(1):135.
Hay P, Touyz S. Treatment of patients with severe and enduring eating disorders. Curr Opin Psychiatry. 2015;28(6):473–7.
Touyz S, Le Grange D, Lacey H, Hay P, Smith R, Maguire S, et al. Treating severe and enduring anorexia nervosa: a randomized controlled trial. Psychol Med. 2013;43(12):2501–11.
Yager J. Managing patients with severe and Enduring Anorexia Nervosa: when is Enough. Enough? J Nerv Ment Dis. 2020;208(4):277–82.
Gaudiani JL, Bogetz A, Yager J. Terminal anorexia nervosa: three cases and proposed clinical characteristics. J Eat Disord. 2022;10(1):23.
Guarda AS, Hanson A, Mehler P, Westmoreland P. Terminal anorexia nervosa is a dangerous term: it cannot, and should not, be defined. J Eat Disord. 2022;10(1):79.
Lowe B, Zipfel S, Buchholz C, Dupont Y, Reas DL, Herzog W. Long-term outcome of anorexia nervosa in a prospective 21-year follow-up study. Psychol Med. 2001;31(5):881–90.
Crow SJ. Terminal anorexia nervosa cannot currently be identified. Int J Eat Disord. 2023;56(7):1329–34.
Austin A, Flynn M, Richards K, Hodsoll J, Duarte TA, Robinson P, et al. Duration of untreated eating disorder and relationship to outcomes: a systematic review of the literature. Eur Eat Disord Rev. 2021;29(3):329–45.
Marzola E, Longo P, Sardella F, Delsedime N, Abbate-Daga G. Rehospitalization and revolving door in Anorexia Nervosa: are there any predictors of Time to Readmission? Front Psychiatry. 2021;12:694223.
Frostad S, Rozakou-Soumalia N, Darvariu S, Foruzesh B, Azkia H, Larsen MP et al. BMI at Discharge from Treatment predicts Relapse in Anorexia Nervosa: a systematic scoping review. J Pers Med. 2022;12(5).
Download references
Acknowledgements
Thank you to the research participants and to all the patients and staff of Johns Hopkins Eating Disorders Program.
Supported in part by the Stephen and Jean Robinson Family Professorship Fund.
Author information
Authors and affiliations.
Department of Psychiatry and Behavioral Sciences, Johns Hopkins University School of Medicine, Baltimore, MD, USA
Mary K. Martinelli, Colleen C. Schreyer & Angela S. Guarda
You can also search for this author in PubMed Google Scholar
Contributions
MM contributed to the conceptualization of the project, conducted data analysis, wrote the original draft, and reviewed and edited the manuscript. CS contributed to the study design and reviewed and edited the manuscript. AG conceived of the study, provided supervision, and reviewed and edited the manuscript.
Corresponding author
Correspondence to Mary K. Martinelli .
Ethics declarations
Ethics approval and consent to participate.
This study was reviewed and approved by the Johns Hopkins University Institutional Review Board. Written informed consent was obtained from study participants.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/ .
Reprints and permissions
About this article
Cite this article.
Martinelli, M.K., Schreyer, C.C. & Guarda, A.S. Comparing hospitalized adult patients with chronic anorexia nervosa with versus without prior hospitalizations. J Eat Disord 12 , 132 (2024). https://doi.org/10.1186/s40337-024-01092-y
Download citation
Received : 17 May 2024
Accepted : 21 August 2024
Published : 04 September 2024
DOI : https://doi.org/10.1186/s40337-024-01092-y
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Inpatient treatment
- Eating disorders
- Severe and enduring anorexia nervosa (SE-AN)
- Severe and enduring eating disorders (SEED)
- Hospitalization
Journal of Eating Disorders
ISSN: 2050-2974
- General enquiries: [email protected]
- Open access
- Published: 28 August 2024
Using PACS for teaching radiology to undergraduate medical students
- Mojtahedzadeh Rita 1 ,
- Mohammadi Aeen 1 ,
- Farnood Rajabzadeh ORCID: orcid.org/0000-0001-6581-4716 2 &
- Akhlaghi Saeed 3
BMC Medical Education volume 24 , Article number: 935 ( 2024 ) Cite this article
Metrics details
Traditional radiology education for medical students predominantly uses textbooks, PowerPoint files, and hard-copy radiographic images, which often lack student interaction. PACS (Picture Archiving and Communication System) is a crucial tool for radiologists in viewing and reporting images, but its use in medical student training remains limited.
This study investigates the effectiveness of using PACS (Picture Archiving and Communication System) for teaching radiology to undergraduate medical students compared to traditional methods.
Fifty-three medical students were divided into a control group (25 students) receiving traditional slide-based training and an intervention group (28 students) using PACS software to view complete patient images. Pre- and post-course tests and satisfaction surveys were conducted for both groups, along with self-evaluation by the intervention group. The validity and reliability of the assessment tools were confirmed through expert review and pilot testing.
No significant difference was found between the control and intervention groups regarding, gender, age, and GPA. Final multiple-choice test scores were similar (intervention: 10.89 ± 2.9; control: 10.76 ± 3.5; p = 0.883). However, the intervention group demonstrated significantly higher improvement in the short answer test for image interpretation (intervention: 8.8 ± 2.28; control: 5.35 ± 2.39; p = 0.001). Satisfaction with the learning method did not significantly differ between groups (intervention: 36.54 ± 5.87; control: 39.44 ± 7.76; p = 0.129). The intervention group reported high familiarity with PACS capabilities (75%), CT principles (71.4%), interpretation (64.3%), appropriate window selection (75%), and anatomical relationships (85.7%).
PACS-based training enhances medical students’ diagnostic and analytical skills in radiology. Further research with larger sample sizes and robust assessment methods is recommended to confirm and expand upon theses results
Peer Review reports
Introduction
Radiology is a fundamental component in basic medical education, bridging the gap between anatomy and clinical practice. Like other fields of medical education, radiology education faces the challenge of transitioning from passive learning to interactive and experiential learning [ 1 , 2 ]. With the expansion of the field of radiology, radiology education has undergone a revolution. Doctors used to carry plain films and show them using projectors or view boxes because plain films were the only main diagnostic method in radiology during the 1970s. Since the introduction of computed tomography (CT) and magnetic resonance imaging (MRI) in the late 1980s, the increase in the amount of image data associated with these imaging modalities has led to a greater demand for compatible information storage systems. Therefore, the picture archiving and communication system (PACS), capable of storing, retrieving, distributing, analyzing, and digitally processing medical images, has become an essential tool in clinical work today [ 3 , 4 , 5 ]. However, due to hardware and software limitations, the use of PACS in radiology education remains somewhat limited [ 6 , 7 ]. Currently, most radiology education still relies heavily on textbooks and traditional computer media such as PowerPoint or Word files both of which lack student interaction. PACS offers advantages such as interactive image viewing, 3D reconstruction capabilities, and the ability to simulate real-life radiology practice, which traditional methods lack. These features enhance students’ understanding and interpretation of radiological images, addressing the shortcomings of conventional methods. There is a minimal probability for a medical student to see whole images like a real radiologist in class. It is often a challenge for them to understand 3D anatomical images, as well as a comprehensive view of diseases. Consequently, some students may attempt to independently identify abnormal findings and analyze and formulate radiological diagnoses. According to one study, only a limited number of final-year medical students had satisfactory basic radiology interpretation skills, which necessitates the search for a more effective method of training [ 8 ].
Recent advancements in radiology teaching methods have previously been reported in addition to face-to-face teaching, including problem-based learning (discussion of a case or scenario consistent with curriculum objectives and students’ independent research to complete subject knowledge and share findings), case-based learning (showing several radiographs of the same subject and discussing them), and team-based learning (student collaboration by creating learning groups) [ 8 ].
In contrast to these conventional methods, a new method was created under the concept of learning from experience. This virtual method is based on individual learning in the PACS software environment, enabling students in the role of radiologists to interpret and diagnose radiology in a simulation environment. All common items are shown to the student using PACS instead of selected specific images. Students are allowed to see the whole image, do basic reconstructions of the images freely, and find specific features of the image by themselves. During this process, students can access PACS and clinical information, integrating clinical knowledge and 3D reconstruction ability, essential to arriving at radiological diagnoses PACS enables efficient archiving and transfer of medical images. Initially developed in the U.S. in the 1980s, it later expanded to Europe and Asia, including China, Japan, and Korea [ 9 ]. Iran has also implemented PACS, improving its medical imaging infrastructure with global DICOM standards.
The goal of this learning method was to compare the effectiveness of practical radiology training through traditional face-to-face interactive lectures with the virtual practical radiology training method based on individual learning in the PACS software environment for medical students.
The use of PACS in healthcare in Iran has only recently become widespread, primarily for patient management and diagnosis, and is rarely used for educational purposes. Iran, as a country with a rapidly developing healthcare system, faces unique challenges in medical education. This study seeks to compare radiology education in Iran with existing literature and to understand its context in relation to the region and worldwide. Managing medical education effectively is a significant challenge. And this research addresses this by introducing innovative teaching methods. Specifically, current study investigates the effectiveness of using PACS on medical students radiology education compared to traditional methods.
The research population was the medical students of the Islamic Azad University of Mashhad during the academic year 2021–2022. The entry criteria were: being a medical trainee student, consent to enter the study, and the exclusion criteria were: students who had previously graduated in radiology or other medical sciences and students who had renewed their course in radiology. participation in the study was voluntary, and students were informed that it would not impact their end-of-section evaluation After obtaining informed consent, they participated in the study. Ethical approval for this study was obtained from the Virtual University of medical sciences with the reference number [IR.VUMS.REC.1400.022]. This proposal was implemented after being approved by the ethics committee and obtaining the code of ethics.
Participants
The sample size was calculated using power analysis to ensure the study had sufficient power to detect a statistically significant difference between the control and intervention groups. Assuming an effect size of 0.5, a significance level (alpha) of 0.05, and a power of 0.80, it was determined that at least 50 participants were needed. To account for potential dropouts and ensure robustness, a total of 53 students were included in the study. According to the calculated sample size, four rotations of radiology internship students were included in the study for each of the control and intervention groups (each rotation is about 5–10 students). Due to the prevention of contamination, the first four rotations were assigned to the control group and the next four rotations to the intervention group.
The validity of the tools used in this study was established through expert review and pilot testing. Content validity was confirmed by 10 faculty members specializing in radiology. Reliability was assessed using Cronbach’s Alpha, yielding a coefficient of 0.91, indicating high internal consistency. In this study, three tools were used: measuring the level of knowledge, measuring the level of performance, and measuring the satisfaction of students in both groups (Appendix 1 ) and self-evaluation for PACS learning in the intervention group (Appendix 2 ). After one month of class, the final exam was taken which was a combination of 20 multiple choice questions and 5 short answer type questions (description and image recognition). The scores of the questions were collected as an objective assessment. To provide a subjective assessment of radiology learning, all students were invited to complete a satisfaction questionnaire on how radiology was taught. Also, the students of the intervention group were invited to complete a questionnaire for their self-evaluation of the amount of PACS learning. A 5-point Likert scale was used in both researcher-made questionnaires. The questionnaire used was created for this study. Informed consent was obtained from each patient whose data was used in the study, ensuring they were fully aware of how their medical images would be utilized for educational purposes.
Familiarization with PACS
Before starting the study with the PACS system, students were given an introductory session that covered the basics of PACS functionality, including how to navigate the software, view and manipulate images, and use the various tools available for image analysis.
Knowledge and performance measurement tools
In the knowledge section, questions evaluated theoretical content, and the performance section involved diagnosing radiographic image. Students described the type of radiography, pathological signs, and the final diagnosis. Multiple-choice questions and short answer questions were used to assess knowledge and performance The specific type of radiography used in this study included plain radiographs, computed tomography (CT) scans, and magnetic resonance imaging (MRI). These imaging modalities were chosen to cover a broad spectrum of radiological techniques relevant to the medical curriculum. In the subject of knowledge, 20 multiple-choice questions were proposed based on the objectives of the lesson and the blueprint, which was approved by two colleagues of the radiology department, which must have been consistent with the objectives of the lesson. In the discussion of the performance of 5 of radiology images, which again corresponded to the objectives of the lesson and the blueprint, and it was approved by two colleagues of the radiology department that the objectives of the lesson were covered, they were provided to the students, and the students had to describe and diagnose the radiographies. The radiology images in both groups adequately covered the goals, but they were taught to the students in two different ways described.
Student satisfaction questionnaire
This questionnaire aimed to determine student’s satisfaction with the educational method. It consisted of ten questions graded on a 5-point Likert scale the range of scores was between 10 and 50 and higher scores indicating greater satisfaction. The content and form validity were confirmed by 10 faculty members and reliability was obtained by Cronbach’s Alpha test of 0.91.
Student self-assessment questionnaire
This questionnaire evaluated the learning rate of the PACS teaching method. It consisted of twelve questions graded on a 5-point Likert scale, and the range of scores was between 12 and 60, and higher scores indicate learning. Content and form validity were confirmed by 10 faculty members and reliability was assessed with a Cronbach’s Alpha of 0.91.
Implementation method in the control group
The teaching strategy involved traditional face-to-face interactive lectures using PowerPoint presentations. The practical part included demonstrating selected radiographic images on slides and discussing their interpretation.
This method aimed to develop the student’s ability to diagnose and interpret radiographs through structured lectures and guided discussions. A pre-test was conducted in the first session to determine the student’s initial knowledge and performance levels. The classes were held daily in person. After teaching the theoretical part with a PowerPoint presentation, radiographic images were shown to the control group for interpretation and discussion. This conventional method aimed to develop the ability to diagnose and interpret radiographs. The post-test to determine knowledge and performance was performed and the education satisfaction questionnaire was completed at the end of each rotation.
Bias caused by human factors during the teaching of the two groups was controlled by standardizing the teaching materials and methods across both groups. Additionally, the instructors were blinded to the group assignments to prevent any conscious or unconscious bias in teaching and assessment.
Implementation method in the intervention group
The stages of developing the training course using PACS software and DICOM were as follows: 1). Initial planning and curriculum alignment, 2) Selection of relevant radiographic cases, 3) Configuration of PACS workstations, 4) Training faculty on PACS software, and 5) Implementation of PACS-based learning sessions for students, followed by assessment and feedback.
After the control group, the rotations of the intervention group were included in the study, and the pre-test was administered to the students of the intervention group. Assessment of knowledge with multiple choice questions and performance with radiographic images was with short answer questions. The classes were held daily in person. In the intervention group, after participating in the theoretical part of the course, which was similar to the control group and was held face-to-face, for the practical part, they were trained in a virtual way with Adobe Connect software, and there was no face-to-face class for radiography images. In this way, students were given access to PACS Radiant software (installation on personal desktop). Following the teaching of the theoretical part, based on the goals of the radiology course for medical trainees, a number of images of the brain, lungs, bones, urinary tract, and digestive system (including radiography, CT and MRI) were assigned to the students of the intervention group, and the images of these patients were completely at their disposal.
The computers used were personal desktops with standardized configurations. Adjustments and calibrations were made to ensure all students could view images with consistent quality and brightness, replicating the clinical environment as closely as possible. This software enables students to perform basic operations with images, such as windowing, comparing different MRI sequences, and performing cross-sectional reconstruction (MPR) or 3D reconstruction, exactly as a radiologist does and has the facilities. After studying the material and checking the images, the students were required to announce the completion of their study to the teacher and they were given the opportunity to review the pictures, ask questions, and solve problems with the teacher in the virtual space.
The post-test to determine knowledge and performance was performed in the intervention group. The education satisfaction questionnaire was completed at the end of each rotation. The self-assessment questionnaire for PACS learning was completed at the end of each rotation.
Data analysis
The data was analyzed with SPSS-17 software, IBM, US. Central and dispersion indices were used in the descriptive statistics report, and a T-test was used in the analytical section, independent t-test, paired t-test and, chi-square test were used to compare the data. The confidence level was set at p < 0.05.
A total of 52 students entered this study, 28 students in the intervention group and 25 in the control group. The students were similar in terms of age, gender, and overall academic average ( p = 0.05) (Table 1 ). The average age in the control group is 26.04 ± 3.96 and in the intervention group is 24.29 ± 2.14. The result of the independent t-test shows that the average age in the two groups is not different ( P = 0.060). The average overall academic grade point average of the medical course in the control group is 15.73 and in the intervention group is 16.01, which has no difference ( P = 0.383) (Table 1 ).
The control group included 25 people, 16 of whom were women and 9 of whom were men, and the intervention group included 28 people of whom 16 were women and 12 were men. The result of the chi-square test shows that the two groups do not differ in terms of gender ( P = 0.610). Evaluation result: At the beginning of the exam, there were two parts of a multiple-choice test and a short answer for the interpretation of radiology images (pre-test). The same exam was done twice at the end of the one-month session (post-test). It was a multiple-choice test to check knowledge and a short answer test to check performance.
The result of the independent t-test shows that the score of the multiple-choice test before and after the intervention, as well as the changes in the test score, are not different in the two groups. ( P = 0.084, P = 0.883, P = 0.764) The result of the paired t-test shows that the multiple-choice test scores of the students before and after the intervention differ between the case and control groups, and it is higher after the intervention. ( P < 0.001, P < 0.001) (Table 2 ) The result of the independent t-test shows that the score of the student’s short answer test, which was for the interpretation of radiology images, is not different before and after the intervention ( P = 0.002 and P = 0.444, respectively). The changes in the test scores are different in the two groups and are more in the intervention group. ( P < 0.001) The result of the paired t-test shows that the score of the short answer test of the students before and after the intervention is different according to the case and control groups, and it is higher after the intervention. ( P < 0.001, P < 0.001)
The result of the independent t-test shows that there is no difference in the level of satisfaction with the teaching method between the two control groups with a score of 39.44 ± 7.76 and the intervention group with a score of 36.54 ± 5. ( P = 0.129) (Table 3 ).
The analysis of the satisfaction questionnaire in the intervention group showed that most students were satisfied with the organization (64%) and interaction of the learning activity (64%) (Table 3 ). Most students use this learning activity to learn radiology (85%). They found it useful. More importantly, a large percentage of students stated that PACS training encouraged personal interest in radiology (82%) as well as satisfaction with the quality of learning (71%). Also, in the intervention group, based on the self-evaluation form, they stated that with the abilities of PACS (75%), the principles of CT (71.4%) and its interpretation (64.3%), choosing the appropriate window (75%), the location of different organs in the image (82.9%) and their vicinity (85.7%) are familiar (Table 3 ). An evaluation of the impact of the intervention on participants’ knowledge is included, showing significant improvements in their understanding and diagnostic skills, highlighting the effectiveness of the PACS-based training method.
Traditional practical radiology training that continues to be used today provides only a cross-section of the entire routine imaging. While this teaching method may be useful in helping students manage the features of routine imaging, it may be inadequate for learning anatomy [ 10 ]. Hence, students may have difficulty interpreting images independently during clinical practice when they are expected to do so [ 11 ]. Although a variety of radiology educational models such as problem-based learning and the use of dynamic images can solve part of this problem, images of the main workplace are the most ideal learning method [ 12 , 13 ]. The experiential learning theory, developed by Dewey, Kolb and others provide explanations for how students learn things in their own way as they react to their perceptions of a real experiences. This concept is explained by principle of constructionism, which is the base of experiential learning [ 13 ].
During this study, a training course using PACS software and DICOM viewer was developed to simulate a work environment that reflects the typical clinical work of a radiologist. The results of the study indicated that this educational approach allows for better clinical guidance, which is necessary to help students form a holistic view of anatomy and pathology. Most importantly, this educational method helps students to develop critical thinking and a systematic approach to formulating imaging interpretation and differential diagnosis, which may be partially due to the exploratory atmosphere of the experiential learning mode. Apart from the objective improvement in imaging descriptions and interpretations, subjective improvements in self-confidence from students’ feedback to self-assessment questionnaires, as well as skills including determining the order of imaging reading, choosing the appropriate window, and also choosing the reconstruction method, which may result under the influence of direct activity during The course of learning and discussion should be free. In addition, the experiential approach allows for better interactions that increase interest in radiology [ 14 ].
To provide students with access to the Radiant PACS software (installed on their personal desktops), following the theoretical section and based on the objectives of the radiology course for medical trainees, a number of images from the brain, lungs, bones, urinary, and gastrointestinal systems (including radiography, CT, MRI) were assigned to the intervention group. These patient images were fully available to them. This software enables students to perform basic operations on images, such as window adjustment, comparing different MRI sequences, and performing multiplanar reconstruction (MPR) or 3D reconstruction, exactly as a radiologist does within the PACS system.
To resolve the issue of patient confidentiality, all patient identifiers were removed from the images before they were made accessible to students. Additionally, access to PACS was restricted to ensure that students could only view and analyze the images without accessing sensitive patient information.
Undergraduate students had limited access to PACS, ensuring they could not modify or delete any content. Additional software controls were implemented to restrict access and prevent any unauthorized changes. This ensured that the integrity of the medical images was maintained, and patient care data was not compromised.
Our study shows the effectiveness of PACS in training in the study of anatomical imaging. Anatomy is the basis of radiology training. In theory, reading CT and MRI images is a good way to study anatomy because continuous scanning helps students understand the three-dimensional concepts of the relative adjacencies of body parts [ 15 , 16 ]. Globally, they concluded that anatomical imaging increases the quality and efficiency of teaching human anatomy [ 17 ]. However, it is difficult to discern the entire anatomical structure from a single cross-section of the image, which increases students’ confusion [ 16 ]. The results of this study provide evidence that continuous scan reading improves students’ comprehensive understanding of anatomy. Furthermore, by using multiple reconstruction methods, 3D images are more comprehensively examined by students, which has been confirmed by other studies [ 18 ].
The integration of PACS in medical education has been shown to enhance the learning experience by providing students with interactive and practical tools for understanding radiological images. Recent advancements in healthcare technology acceptance highlight the importance of user-friendly interfaces and training for successful implementation [ 19 ]. Moreover, the current state of medical education in the UK emphasizes the adoption of advanced technologies like PACS to improve educational outcomes and prepare students for real-world clinical environments [ 20 ]. The utilization of big data technologies in conjunction with PACS further enhances the management and analysis of medical images, facilitating a more personalized and effective learning experience for medical students [ 21 ]. Additionally, recent market reports indicate a steady growth in the adoption of medical imaging technologies, including PACS, driven by advancements in AI and machine learning, which are poised to revolutionize medical education [ 22 ]. These developments collectively underscore the critical role of PACS in modernizing medical education and improving the quality of training for future healthcare professionals. Also, the implementation of PACS could significantly enhance radiology education by providing access to digital imaging resources that may otherwise be unavailable.
Compared to Chen et al.‘s study [ 1 ], the study was conducted on 101 students, but our study was on 52 students. Satisfaction with PACS training in Chen’s study was on average 80% and in our study, it was about 65%. The percentage of being interested in radiology in this study and Chen’s study was almost similar. Also, in our study, similar to Chen’s study, there was no difference in pre-test scores between the two intervention and control groups. Also, the final scores in Chen’s study and our study were not significantly different, but the scores of interpretations of pictures, which in our study were equivalent to a number of stereotypes in the form of PowerPoint with short answer questions, showed a significant difference in both our study and Chen’s study.
In the study of Restauri [ 6 ] and Soman [ 23 ], as in our study, PACS was used to teach medical students, and at the end of the course, only a survey form was filled by the students, and the impact of using PACS on the ability to interpret radiology images by students was not done. In the above two studies, after using PACS, students stated that they gained more confidence on interpreting images and would use PACS in the future, which was similar to the survey results in our study. It takes a lot of effort to do this kind of training. PACS and a suitable DICOM viewer represent basic software requirements for training and to protect patient privacy, DICOM data from PACS rather than linking to the original PACS. Copied In this way, a PACS simulation for medical education was obtained [ 6 ]. In addition, teacher guidance is a vital element in education. A minimum of 3 instructors with experience in standard radiology training is required for a class, as team discussion is a major component of the training. In experimental courses, students need educational help both to guide reading the picture and to answer the questions. Therefore, teaching professors need specific work experience in the radiology department. Having said that, the lack of a radiology professor prevents the use of this training and this training model acts as a limitation on a larger scale. There are several limitations to the study. First, due to the limited number of supervisors, the sample size was correspondingly limited. Secondly, it was a single study center. Thirdly, due to the limitation of the operation, some students did not answer some of the questions in the questionnaire. Although the probability is very low, it still has the chance to bias the result. Fourth, although we control for faculty and teaching standards between the two groups, human bias is still a factor that cannot be completely avoided in practice. Fifth, although we used objective assessment measures, the study also revealed the weakness of our assessment system in radiology education. The study instrument consisted of paper and pencil tests, with most questions consisting of objective items that test memory, such as multiple-choice questions and short answer questions. Furthermore, the mental items used to test application ability are limited. As a result, only a small part of the final test reflects the difference between the experimental training group and the control group. Other test forms such as bedside examinations and multi-station examinations should be used in the future for better evaluation [ 24 , 25 ]. In this study, according to the curriculum, students entered the radiology department with different numbers during different periods, and 4 periods of students were entered into the study for each group. The exams were held at the end of the one-month section, so the exam was held in the control group and in the intervention group at different times, although we tried to make the questions the same in terms of number and content similarity. In the study of Chen et al [ 8 ], the test was conducted at the end of the semester and simultaneously for two groups. If this study is conducted with a larger number of students and in multiple centers, the results will be more valid.
PACS-based training is beneficial for medical students, enhancing their diagnostic and analytical skills in radiology. Further research with larger sample sizes and robust assessment methods is recommended to confirm and expand upon theses results. We believe that our findings suggest that PACS which is used routinely in healthcare diagnostic context, can also be used in medical students’ education and healthcare can be integrated in education.
Data availability
The demographic and clinical datasets generated and/or analyzed during the current study are available from the corresponding author (Dr. Farnood Rajabzadeh ) upon reasonable request.
Abbreviations
Picture Archiving and Communication System
Computed Tomography
Magnetic Resonance Imaging
Grade Point Average
Digital Imaging and Communications in Medicine
Statistical Package for the Social Sciences
Multi planar Reconstruction
Artificial Intelligence
Bhogal P, Booth TC, Phillips AJ, Golding SJ. Radiology in the undergraduate medical curriculum -- who, how, what, when, and where? Clin Radiol. 2012;67(12):1146–52.
Article Google Scholar
Naeger DM, Webb EM, Zimmerman L, Elicker BM. Strategies for incorporating radiology into early medical school curricula. J Am Coll Radiol. 2014;11(1):74 – 9.
Forsberg D, Rosipko B, Sunshine JL. Factors affecting Radiologist’s PACS usage. J Digit Imaging. 2016;29(6):670–6.
Mirsadraee S, Mankad K, McCoubrie P, Roberts T, Kessel D. Radiology curriculum for undergraduate medical studies–a consensus survey. Clin Radiol. 2012;67(12):1155–61.
Arriero A, Bonomo L, Calliada F, Campioni P, Colosimo C, Cotroneo A, Cova M, Ettorre GC, Fugazzola C, Garlaschi G, Macarini L, Mascalchi M, Meloni GB, Midiri M, Mucelli RP, Rossi C, Sironi S, Torricelli P, Beomonte BZ, Zompatori M, Zuiani C. E-learning in radiology: an Italian multicentre experience. Eur J Radiol. 2012;81(12):3936–41.
Restauri N, Bang T, Hall B. Sachs P Development and Utilization of a Simulation PACS in Undergraduate Medical Education. J Am Coll Radiol. 2018;15(2):346–9.
Zafar S, Safdar S, Zafar AN. Evaluation of use of e-Learning in undergraduate radiology education: a review. Eur J Radiol. 2014;83(12):2277–87.
Chen Y, Zheng K, Ye S, Wang J, Xu L, Li Z, Meng Q, Yang J, Feng ST. Constructing an experiential education model in undergraduate radiology education by the utilization of the picture archiving and communication system (PACS). BMC Med Educ. 2019;19(1):383.
Huang -HK. Twenty-five years of Picture Archiving and Communication Systems (PACS). Dev Iran J Radiol. 2007;4(2):1.
Google Scholar
-Pascual TN, Chhem R, Wang SC, Vujnovic S. Undergraduate radiology education in the era of dynamism in medical curriculum: an educational perspective. Eur J Radiol. 2011;78(3):319–25.
-Sendra-Portero F, Torales-Chaparro OE, Ruiz-Gomez MJ, Martinez-Morillo. M.A pilot study to evaluate the use of virtual lectures for undergraduate radiology teaching. Eur J Radiol. 2013;82(5):888–93.
-Zhang S, Xu J, Wang H, Zhang D, Zhang Q, Zou L. Effects of problem-based learning in Chinese radiology education: a systematic review and metaanalysis. Med (Baltim). 2018;97(9):e0069.
Yardley S, Teunissen PW, Dornan T. Experiential learning: transforming theory into practice. Med Teach. 2012;34(2):161–4.
Branstetter BF. Humphrey AL,Schumann JB.The long-term impact of preclinical education on medical students’ pinions about radiology. Acad Radiol. 2008;15(10):1331–9.
Schober A, Pieper CC, Schmidt R, Wittkowski W. Anatomy and imaging: 10 years of experience with an interdisciplinary teaching project in preclinical medical education - from an elective to a curricular course. Rofo. 2014;186(5):458–65.
Jang HW, Oh CS, Choe YH, Jang DS. Use of dynamic images in radiology education: movies of CT and MRI in the anatomy classroom. Anat Sci Educ. 2018;11(6):547–53.
Grignon B, Oldrini G, Walter F. Teaching medical anatomy: what is the role of imaging today? Surg Radiol Anat. 2016;38(2):253–60.
Loke YH, Harahsheh AS, Krieger A, Olivieri LJ. Usage of 3D models of tetralogy of Fallot for medical education: impact on learning congenital heart disease. BMC Med Educ. 2017;17(1):54.
AlQudah, Adi A, Al-Emran M, Khaled Shaalan. Technology Acceptance in Healthcare: a systematic review Applied sciences 2021;11(22):10537. https://doi.org/10.3390/app112210537
GMC. (2022). The state of medical education and practice in the UK.
Geroski T, Jakovljević D, Filipović N. Big Data in multiscale modelling: from medical image processing to personalized models. J Big Data. 2023;10:72. https://doi.org/10.1186/s40537-023-00763-y .
-Visage Imaging. Medical imaging market size. Share & Growth Report; 2024.
Soman S, Amorosa JK, Mueller L, Hu J, Zou L, Masand A, Cheng C, Virk J, Rama H, Tseng I, Patel K, Connolly SE. Evaluation of medical student experience using medical student created StudentPACS flash based PACS simulator tutorials for learning radiological topics. Acad Radiol. 2010;17(6):799–807.
Reddy S, Straus CM, McNulty NJ, Tigges S, Ayoob A, Randazzo W, Neutze J, Lewis P. Development of the AMSER standardized examinations in radiology for medical students. Acad Radiol. 2015;22(1):130–4.
Monticciolo DL. The ACR diagnostic radiology in-training examination: evolution, current status, and future directions. J Am Coll Radiol. 2010;7(2):132–7.
Download references
Acknowledgements
Farbod Rajabzadeh for helping in data gathering, Ladan Goshayeshi for helping in editing, Lena Goshayeshi for helping in editing.
This study was supported by the Smart university of medical sciences and Mashhad Azad University of Medical Sciences.
Author information
Authors and affiliations.
Department of e-Learning in Medical Education, School of Medicine, Center of Excellence for E- learning in Medical Education, Tehran University of Medical Sciences, Tehran, Iran
Mojtahedzadeh Rita & Mohammadi Aeen
Department of Radiology, Faculty of Medicine, Mashhad Medical Sciences, Islamic Azad university, Mashhad, Iran
Farnood Rajabzadeh
Department of Community Medicine, University of Medical Sciences, Mashhad, Mashhad, Iran
Akhlaghi Saeed
You can also search for this author in PubMed Google Scholar
Contributions
RM, FR, designed the study. FR was involved in the data gathering and interpretation of the results. AM and SA performed analyses. FR wrote the first draft of the manuscript. FR and RM edited the final version of the manuscript. All authors read and approved the final version of the manuscript.
Corresponding author
Correspondence to Farnood Rajabzadeh .
Ethics declarations
Ethics approval and consent to participate.
This study was approved by the Ethics Committee of Smart University of Medical Sciences (ethics code: IR.VUMS.REC.1400.022, 4/12/2021) and conformed to the ethical principles contained in the Declaration of Helsinki. For experiments involving human participants the participants signed an informed consent form before the study.
Consent for publication
Competing interests.
The authors declare no competing interests.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary Material 1
Supplementary material 2, rights and permissions.
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/ .
Reprints and permissions
About this article
Cite this article.
Rita, M., Aeen, M., Rajabzadeh, F. et al. Using PACS for teaching radiology to undergraduate medical students. BMC Med Educ 24 , 935 (2024). https://doi.org/10.1186/s12909-024-05919-9
Download citation
Received : 05 December 2023
Accepted : 16 August 2024
Published : 28 August 2024
DOI : https://doi.org/10.1186/s12909-024-05919-9
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Radiology education
- Medical students
BMC Medical Education
ISSN: 1472-6920
- General enquiries: [email protected]
- Language Teaching
Academic Speaking Students’ Efforts in Minimizing Their Lack of Self- Confidence
- Prominent 5(2):141-167
- 5(2):141-167

- Universitas Kristen Satya Wacana

Discover the world's research
- 25+ million members
- 160+ million publication pages
- 2.3+ billion citations
- Aries Fachriza

- Mohammad Luthfi

- Desi Riyanti Sihombing
- Zakia Oktafiani
- Yusri Yusri
- Pratiwi Samad

- Rina Listia

- Euis Meinawati
- Danang Dwi Harmoko
- Nazzala Aulia Rahmah

- Gaya Tridinanti

- Aisyah Mumary Songbatumis
- Recruit researchers
- Join for free
- Login Email Tip: Most researchers use their institutional email address as their ResearchGate login Password Forgot password? Keep me logged in Log in or Continue with Google Welcome back! Please log in. Email · Hint Tip: Most researchers use their institutional email address as their ResearchGate login Password Forgot password? Keep me logged in Log in or Continue with Google No account? Sign up

IMAGES
VIDEO
COMMENTS
We first define self-confidence and related concepts. Next, an overview of self-efficacy theory is given, along with a review of the relevant research. The third section covers applications of techniques for enhancing self-confidence. Lastly, we note the research questions that follow from what is currently known.
Relevant answer. Ehsan Shabahang. Dec 13, 2023. Answer. Imagery training and self-confidence can significantly impact sports anxiety among junior high school judokas. Imagery training, a mental ...
Self-esteem is an individual's sense of satisfaction with oneself and reflects the relationship between personal self-image and ideal self-image. 1 Self-esteem is a measure of self-assessment because it is considered the most important psychological formula. 2 Self-esteem has 2 types, specific and global. Global self-esteem is more relevant to the psychological aspect, while specific self ...
1. Introduction. Strategies to enhance self-confidence are common sport psychology interventions for athletes [1,2] but evidence of the relationship between self-confidence and athletic performance is equivocal.Several studies have reported significant benefits of self-confidence for athletes [3,4,5,6], whereas other investigations have shown no benefit [7,8,9,10].
Social self confiden ce, sometimes t ermed social self effi cacy, is a strong belief in one's. ability to interact in soci al settings to build and/or maintain interpersonal ties (Bandura, 1993 ...
The self-efficacy theory of Bandura (1986) suggests that confidence is enhanced by four main factors: successful performances (competence), vicarious experience, verbal persuasion (including praise and encouragement), and physiological feedback. Furthermore, Bandura and Locke (2003) have found that one's own belief in self-efficacy can significantly impact on confidence in motivation and ...
In regards of students' confidence in being able to. study independently, 16% of students were extremely con fident, 29.4% of students were more confident, 33.6% of students. were confident, 17. ...
Women are regularly exhorted to demonstrate self-confidence as a strategy to progress their careers, raise their pay, and become more successful at work. Self-help guides commend women to "lean ...
students' and teachers' perceptions of self-confidence and their impact on academic performance. The research was guided by Weiner's attribution and Bandura's self-efficacy theories. The research questions focused on 3 areas: students' and teachers 'perceptions of academic self-confidence as factors impacting students' academic
Specifically, self-confidence and parental support had a significant and positive impact on academic achievement among higher secondary school students. Ballane (2019) reported that self-confidence had significant role in academic performance development, learning and success. Self-confidence was found as a predictor of academic performance.
Participants predicted level on the aspirations and goals scale is equal to 2.591 + 0.445(confidence with self-direction score). That is, a one unit increase on the confidence with self-direction scale leads to an increase of 0.445 on the aspirations and goals scale. 4.4.3. Multiple linear regressions
In either case, a lack of personal worth and value can have a negative impact on life and wellness. Some common signs or symptoms of low self-esteem include: Lack of confidence. External locus of control. Negative social comparisons. Trouble asking for help. Worry and doubt.
Perceived competence is a belief that one has skills in a particular area (e.g., math, spelling, peer relationships). Self-esteem and perceived competence are necessary for students to take risks in their learning and to bounce back after failure or adversity. Low self-esteem or lack of confidence leaves students doubting their ability to ...
The outcome of the study revealed that undergraduates lacked the confidence to ask and answer questions, seek help from lecturers, have a study plan and engage in academic discussion and note-taking. ... a plethora of widely cited academic research about-confidence and many related concepts like self-esteem and self-efficacy emerged.[14][15][16 ...
The steps for future research on the short-term: Design research article into an intervention to increase self-confidence amongst first-year game design students within project-based education at ...
According to Loubazid, Students may experience different 2 psychological barriers including lack of self confidence, language anxiety, shyness and fear … etc. ( 2012, P. 10) 2.3.1 Lack of self confidence Some students who do not trust their abilities in performing oral presentations often feel hesitated and embarrassed, they are afraid of ...
The disruption of health and medical education by the COVID-19 pandemic made educators question the effect of online setting on students' learning, motivation, self-efficacy and preference. In light of the health care staff shortage online scalable education seemed relevant. Reviews on the effect of online medical education called for high quality RCTs, which are increasingly relevant with ...
Background Depression poses a significant challenge globally, including in safety-critical industries such as aviation. In Saudi Arabia, where the aviation sector is rapidly expanding, pilots encounter unique stressors inherent to their profession. However, research on pilot mental health, particularly within the Saudi context, remains limited despite its critical role in flight safety ...
Despite the overall improvement in the headline Index, confidence declined for consumers earning less than $25K. On a six-month moving average basis, consumers earning over $100K remained the most confident. Confidence among consumers earning $15K to $24.9K continued to trend down and was almost as low as for those earning less than $15K."
Manchester Clinical Supervision Scale-26 results. Participants generally viewed peer group clinical supervision as effective (Table 3), the total mean Manchester Clinical Supervision Scale-26 score among all peer group clinical supervisors was 76.47 (SD. 12.801) out of 104, Surpassing the clinical supervision threshold score of 73, which was established by the developers of the Manchester ...
The participant was then asked to predict the other person's response on a second statement (e.g. all women should have access to legal abortion), and to state their confidence in their answer ...
Abstract. This article indicates the level of self-confidence during the oral performance of. the students such as in speaking activities as well as the self-efficacy in their oral task ...
For this study, the sample data is accurate to within +/- 2.5 percentage points using a 95% confidence level. For complete survey methodology, including weighting variables and subgroup sample ...
Anorexia nervosa (AN) is a severe psychiatric disorder, from which recovery is often protracted. The role of prior specialized inpatient treatment on subsequent treatment attempts for adults with chronic AN and predictors of treatment response for severe and enduring AN (SE-AN) are needed to improve outcomes. Participants (N = 135) with chronic AN (ill ≥7 years) admitted to an integrated ...
was to enhance the confidence of students in speaking English by using interactive practices. The present study was conducted at one of the private sector. universities in Lahore, Pakistan. The ...
Background Traditional radiology education for medical students predominantly uses textbooks, PowerPoint files, and hard-copy radiographic images, which often lack student interaction. PACS (Picture Archiving and Communication System) is a crucial tool for radiologists in viewing and reporting images, but its use in medical student training remains limited. Objective This study investigates ...
The data were collected from thirty-three Academic Speaking students using open-ended questions and semi-structured interviews. The findings indicated the causes of the lack of self-confidence ...