MRC Dyspnoea Scale
The mMRC (Modified Medical Research Council) Dyspnoea Scale is used to assess the degree of baseline functional disability due to dyspnoea.
It is useful in characterising baseline dyspnoea in patients with respiratory disease such as COPD. Whilst it moderately correlates with other healthcare-associated morbidity, mortality and quality of life scales (particularly in COPD) the scores are only variably associated with patients' perceptions of respiratory symptom burden. It is used as a component of the BODE Index, which predicts adverse outcomes, including mortality and risk of hospitalisation. The scale is easy and efficient to use.
| I only get breathless with strenuous exercise | 0 |
| I get short of breath when hurrying on level ground or walking up a slight hill | 1 |
| On level ground, I walk slower than people of my age because of breathlessness, or I have to stop for breath when walking at my own pace on the level | 2 |
| I stop for breath after walking about 100 yards or after a few minutes on level ground | 3 |
| I am too breathless to leave the house or I am breathless when dressing/undressing | 4 |
The mMRC breathlessness scale ranges from grade 0 to 4. It is very similar to the original version and is now widely used in studies. It should be noted that the MRC clearly states on its website that it is unable to give permission for use of any modified version of the scale (including therefore, the mMRC scale). Use of the MRC questionnaire is free but should be acknowledged.
The modified MRC was developed by D A Mahler, see https://pubmed.ncbi.nlm.nih.gov/3342669/

Diagnostic testing
Your essential guide to respiratory diagnostic testing from FeNO and spirometry to CRP Point of Care Testing.
Clinical resources
Step by step guides, expert opinion, the latest insights and case studies - our resources cover a range of respiratory topics and a vital resource for any practitioner working in the delivery of respiratory healthcare
PCRS Respiratory Conference
The UK's leading respiratory conference for clinicians working primary, community and integrated care comes to Telford in September.
You may also be interested in...
Step by step guides, podcasts and webinars cover prevention, diagnosis, testing and management. They will help you to support your patients and improve their outcomes.
Inhaler devices
Inhaler devices may seem simple to use but they are often used incorrectly by patients and healthcare professionals alike.
Chronic Obstructive Pulmonary Disease (COPD) is the fifth leading cause of death in the UK. It's a serious condition which calls for a patient centric approach.
Join PCRS Today
Become part of the UK's largest network of dedicated respiratory professionals working in primary, community and integrated care settings.
- Type 2 Diabetes
- Heart Disease
- Digestive Health
- Multiple Sclerosis
- Diet & Nutrition
- Health Insurance
- Public Health
- Patient Rights
- Caregivers & Loved Ones
- End of Life Concerns
- Health News
- Thyroid Test Analyzer
- Doctor Discussion Guides
- Hemoglobin A1c Test Analyzer
- Lipid Test Analyzer
- Complete Blood Count (CBC) Analyzer
- What to Buy
- Editorial Process
- Meet Our Medical Expert Board
Measuring Shortness of Breath (Dyspnea) in COPD
How the Perception of Disability Directs Treatment
Dyspnea is the medical term used to describe shortness of breath, a symptom considered central to all forms of chronic obstructive pulmonary disease (COPD) including emphysema and chronic bronchitis.
As COPD is both a progressive and non-reversible, the severity of dyspnea plays a key role in determining both the stage of the disease and the appropriate medical treatment.
Challenges in Diagnosis
From a clinical standpoint, the challenge of diagnosing dyspnea is that it is very subjective. While spirometry tests (which measures lung capacity) and pulse oximetry (which measures oxygen levels in the blood) may show that two people have the same level of breathing impairment, one may feel completely winded after activity while the other may be just fine.
Ultimately, a person's perception of dyspnea is important as it helps ensure the person is neither undertreated nor overtreated and that the prescribed therapy, when needed, will improve the person's quality of life rather than take from it.
To this end, pulmonologists will use a tool called the modified Medical Research Council (mMRC) dyspnea scale to establish how much an individual's shortness of breath causes real-world disability.
How the Assessment Is Performed
The process of measuring dyspnea is similar to tests used to measure pain perception in persons with chronic pain. Rather than defining dyspnea in terms of lung capacity, the mMRC scale will rate the sensation of dyspnea as the person perceives it.
The severity of dyspnea is rated on a scale of 0 to 4, the value of which will direct both the diagnosis and treatment plan.
| Grade | Description of Breathlessness |
|---|---|
| 0 | "I only get breathless with strenuous exercise." |
| 1 | "I get short of breath when hurrying on level ground or walking up a slight hill." |
| 2 | "On level ground, I walk slower than people of the same age because of breathlessness or have to stop for breath when walking at my own pace." |
| 3 | "I stop for breath after walking about 100 yards or after a few minutes on level ground." |
| 4 | "I am too breathless to leave the house, or I am breathless when dressing." |
Role of the MMRC Dyspnea Scale
The mMRC dyspnea scale has proven valuable in the field of pulmonology as it affords doctors and researchers the mean to:
- Assess the effectiveness of treatment on an individual basis
- Compare the effectiveness of a treatment within a population
- Predict survival times and rates
From a clinical viewpoint, the mMRC scale correlates fairly well to such objective measures as pulmonary function tests and walk tests . Moreover, the values tend to be stable over time, meaning that they are far less prone to subjective variability that one might assume.
Using the BODE Index to Predict Survival
The mMRC dyspnea scale is used to calculate the BODE index , a tool which helps estimate the survival times of people living with COPD.
The BODE Index is comprised of a person's body mass index ("B"), airway obstruction ("O"), dyspnea ("D"), and exercise tolerance ("E"). Each of these components is graded on a scale of either 0 to 1 or 0 to 3, the numbers of which are then tabulated for a final value.
The final value—ranging from as low as 0 to as high as 10—provides doctors a percentage of how likely a person is to survive for four years. The final BODE tabulation is described as follows:
- 0 to 2 points: 80 percent likelihood of survival
- 3 to 4 points: 67 percent likelihood of survival
- 5 of 6 points: 57 percent likelihood of survival
- 7 to 10 points: 18 percent likelihood of survival
The BODE values, whether large or small, are not set in stone. Changes to lifestyle and improved treatment adherence can improve long-term outcomes, sometimes dramatically. These include things like quitting smoking , improving your diet and engaging in appropriate exercise to improve your respiratory capacity.
In the end, the numbers are simply a snapshot of current health, not a prediction of your mortality. Ultimately, the lifestyle choices you make can play a significant role in determining whether the odds are against you or in your favor.
Janssens T, De peuter S, Stans L, et al. Dyspnea perception in COPD: association between anxiety, dyspnea-related fear, and dyspnea in a pulmonary rehabilitation program . Chest. 2011;140(3):618-625. doi:10.1378/chest.10-3257
Manali ED, Lyberopoulos P, Triantafillidou C, et al. MRC chronic Dyspnea Scale: Relationships with cardiopulmonary exercise testing and 6-minute walk test in idiopathic pulmonary fibrosis patients: a prospective study . BMC Pulm Med . 2010;10:32. doi:10.1186/1471-2466-10-32
Esteban C, Quintana JM, Moraza J, et al. BODE-Index vs HADO-score in chronic obstructive pulmonary disease: Which one to use in general practice? . BMC Med . 2010;8:28. doi:10.1186/1741-7015-8-28
Chhabra, S., Gupta, A., and Khuma, M. " Evaluation of Three Scales of Dyspnea in Chronic Obstructive Pulmonary Disease. " Annals of Thoracic Medicine. 2009; 4(3):128-32. DOI: 10.4103/1817-1737.53351 .
Perez, T.; Burgel, P.; Paillasseur, J.; et al. " Modified Medical Research Council scale vs Baseline Dyspnea Index to Evaluate Dyspnea in Chronic Obstructive Pulmonary Disease. " International Journal of Chronic Obstructive Pulmonary Disease . 2015; 10:1663-72. DOI: 10.2147/COPD.S82408 .
By Deborah Leader, RN Deborah Leader RN, PHN, is a registered nurse and medical writer who focuses on COPD.
Log in using your username and password
- Search More Search for this keyword Advanced search
- Thorax Education
- Latest content
- Current issue
- BMJ Journals
You are here
- Volume 54, Issue 7
- Usefulness of the Medical Research Council (MRC) dyspnoea scale as a measure of disability in patients with chronic obstructive pulmonary disease
- Article Text
- Article info
- Citation Tools
- Rapid Responses
- Article metrics
- J C Bestall b ,
- E A Paul a ,
- R Garrod a ,
- R Garnham a ,
- P W Jones b ,
- J A Wedzicha a
- a Academic Department of Respiratory Medicine, St Bartholomew’s and Royal London School of Medicine and Dentistry, London Chest Hospital, London, UK, b Division of Physiological Medicine, St George’s Hospital Medical School, London SW17 0RE, UK
- Professor P Jones.
BACKGROUND Methods of classifying chronic obstructive pulmonary disease (COPD) depend largely upon spirometric measurements but disability is only weakly related to measurements of lung function. With the increased use of pulmonary rehabilitation, a need has been identified for a simple and standardised method of categorising disability in COPD. This study examined the validity of the Medical Research Council (MRC) dyspnoea scale for this purpose.
METHODS One hundred patients with COPD were recruited from an outpatient pulmonary rehabilitation programme. Assessments included the MRC dyspnoea scale, spirometric tests, blood gas tensions, a shuttle walking test, and Borg scores for perceived breathlessness before and after exercise. Health status was assessed using the St George’s Respiratory Questionnaire (SGRQ) and Chronic Respiratory Questionnaire (CRQ). The Nottingham Extended Activities of Daily Living (EADL) score and Hospital Anxiety and Depression (HAD) score were also measured.
RESULTS Of the patients studied, 32 were classified as having MRC grade 3 dyspnoea, 34 MRC grade 4 dyspnoea, and 34 MRC grade 5 dyspnoea. Patients with MRC grades 1 and 2 dyspnoea were not included in the study. There was a significant association between MRC grade and shuttle distance, SGRQ and CRQ scores, mood state and EADL. Forced expiratory volume in one second (FEV 1 ) was not associated with MRC grade. Multiple logistic regression showed that the determinants of disability appeared to vary with the level of disability. Between MRC grades 3 and 4 the significant covariates were exercise performance, SGRQ and depression score, whilst between grades 4 and 5 exercise performance and age were the major determinants.
CONCLUSIONS The MRC dyspnoea scale is a simple and valid method of categorising patients with COPD in terms of their disability that could be used to complement FEV 1 in the classification of COPD severity.
- MRC dyspnoea scale
- chronic obstructive pulmonary disease
https://doi.org/10.1136/thx.54.7.581
Statistics from Altmetric.com
Request permissions.
If you wish to reuse any or all of this article please use the link below which will take you to the Copyright Clearance Center’s RightsLink service. You will be able to get a quick price and instant permission to reuse the content in many different ways.
Read the full text or download the PDF:

MRC Dyspnoea Scale - MRC
The MRC Dyspnoea Scale, also called the MRC Breathlessness Scale, has been in use for many years for grading the effect of breathlessness on daily activities. This scale measures perceived respiratory disability, using the World Health Organization (WHO) definition of disability being “any restriction or lack of ability to perform an activity in the manner or within the range considered normal for a human being”.
The MRC Dyspnoea Scale is simple to administer as it allows the patients to indicate the extent to which their breathlessness affects their mobility.
The 1-5 stage scale is used alongside the questionnaire to establish clinical grades of breathlessness.
MRC Breathlessness Scales: 1952 and 1959
Questionnaire on Respiratory Symptoms
The questionnaire was first published in 1960 under the approval of the MRC Committee on the Aetiology of Chronic Bronchitis. This was revised and a new version published in 1966. When the committee disbanded, the responsibility for it was passed to the newly formed MRC Committee for Research into Chronic Bronchitis who again revised it in 1976. When this committee disbanded, the responsibility for the questionnaire passed to the Committee on Environmental and Occupational Health (CEOH) who reviewed it and issued what remains to be the most recent version in 1986.
The Questionnaire on Respiratory Symptoms was designed to be used in large scale epidemiological studies only (100-1,000 people). It cannot be used on an individual basis.
Questionnaire on respiratory symptoms and instructions to interviewers (1966)
Questionnaire on respiratory symptoms and instructions to interviewers (1976)
Questionnaire on respiratory symptoms and instructions to interviewers (1986)
Permission to reuse the MRC Dyspnoea Scale
In accordance with MRC’s Open Access Policy , permission is granted from the MRC to use the MRC Dyspnoea Scale for any purpose (including research and commercial purposes) and MRC hereby agrees not to assert its rights in relation to the proposed use of the MRC Dyspnoea Scale.
You must give appropriate credit (“Used with the permission of the Medical Research Council”) and indicate if changes were made. You may do so in any reasonable manner, but not in any way that suggests that the MRC endorses you or your use.
We cannot give permission to use any modified versions of this scale including the MRC Scale.
Note: The MRC is not in a position to authorise translations or check back-translations
Contact information
Ask a question, or get further information about any of the MRC scales. Email: [email protected]
For information about licensing
To view the full Open Government Licence, visit National Archives: Open Government Licence Version 2 .
Further context, best practice and guidance can be found in the National Archives: UK Government Licensing Framework .
LifeArc manages MRC’s intellectual property rights and commercialises findings by licensing them to industry. They can be contacted for support via the contact information on their website .
Last updated: 24 January 2022
This is the website for UKRI: our seven research councils, Research England and Innovate UK. Let us know if you have feedback or would like to help improve our online products and services .
- NICE Guidance
- Conditions and diseases
- Respiratory conditions
- Chronic obstructive pulmonary disease
Chronic obstructive pulmonary disease in over 16s: diagnosis and management
NICE guideline [NG115] Published: 05 December 2018 Last updated: 26 July 2019
- Tools and resources
- Information for the public
Recommendations
- Recommendations for research
- Rationale and impact
- Finding more information and committee details
- Update information
1.1 Diagnosing COPD
1.2 managing stable copd, 1.3 managing exacerbations of copd, terms used in this guideline.
People have the right to be involved in discussions and make informed decisions about their care, as described in NICE's information on making decisions about your care .
Making decisions using NICE guidelines explains how we use words to show the strength (or certainty) of our recommendations, and has information about prescribing medicines (including off-label use), professional guidelines, standards and laws (including on consent and mental capacity), and safeguarding.
The diagnosis of chronic obstructive pulmonary disease (COPD) depends on thinking of it as a cause of breathlessness or cough. The diagnosis is suspected on the basis of symptoms and signs and is supported by spirometry.
Suspect a diagnosis of COPD in people over 35 who have a risk factor (generally smoking or a history of smoking) and who present with 1 or more of the following symptoms:
exertional breathlessness
chronic cough
regular sputum production
frequent winter 'bronchitis'
wheeze. [2004]
When thinking about a diagnosis of COPD, ask the person if they have:
weight loss
reduced exercise tolerance
waking at night with breathlessness
ankle swelling
occupational hazards
haemoptysis (coughing up blood). These last 2 symptoms are uncommon in COPD and raise the possibility of alternative diagnoses. [2004]
One of the primary symptoms of COPD is breathlessness. The Medical Research Council (MRC) dyspnoea scale (see table 1) should be used to grade the breathlessness according to the level of exertion required to elicit it. [2004]
| Grade | Degree of breathlessness related to activities |
|---|---|
| 1 | Not troubled by breathlessness except on strenuous exercise |
| 2 | Short of breath when hurrying or walking up a slight hill |
| 3 | Walks slower than contemporaries on level ground because of breathlessness, or has to stop for breath when walking at own pace |
| 4 | Stops for breath after walking about 100 metres or after a few minutes on level ground |
| 5 | Too breathless to leave the house, or breathless when dressing or undressing |
Adapted from Fletcher CM, Elmes PC, Fairbairn MB et al. (1959) The significance of respiratory symptoms and the diagnosis of chronic bronchitis in a working population . British Medical Journal 2: 257–66.
Perform spirometry:
at diagnosis
to reconsider the diagnosis, for people who show an exceptionally good response to treatment
to monitor disease progression. [2004, amended 2018]
Measure post-bronchodilator spirometry to confirm the diagnosis of COPD. [2010]
Think about alternative diagnoses or investigations for older people who have an FEV1/FVC ratio below 0.7 but do not have typical symptoms of COPD. [2010]
Think about a diagnosis of COPD in younger people who have symptoms of COPD, even when their FEV1/FVC ratio is above 0.7. [2010]
All healthcare professionals who care for people with COPD should have access to spirometry and be competent in interpreting the results. [2004]
Spirometry can be performed by any healthcare worker who has had appropriate training and has up-to-date skills. [2004]
Spirometry services should be supported by quality control processes. [2004]
It is recommended that European Respiratory Journal GLI 2012 reference values are used, but it is recognised that these values are not applicable for all ethnic groups. [2004, amended 2018]
Incidental findings on chest X‑ray or CT scans
Consider primary care respiratory review and spirometry (see the recommendations on symptoms and spirometry ) for people with emphysema or signs of chronic airways disease on a chest X-ray or CT scan. [2018]
If the person is a current smoker, their spirometry results are normal and they have no symptoms or signs of respiratory disease:
offer smoking cessation advice and treatment, and referral to specialist stop smoking services (see the NICE guideline on stop smoking interventions and services )
warn them that they are at higher risk of lung disease
advise them to return if they develop respiratory symptoms
be aware that the presence of emphysema on a CT scan is an independent risk factor for lung cancer. [2018]
If the person is not a current smoker, their spirometry is normal and they have no symptoms or signs of respiratory disease:
ask them if they have a personal or family history of lung or liver disease and consider alternative diagnoses, such as alpha‑1 antitrypsin deficiency
reassure them that their emphysema or chronic airways disease is unlikely to get worse
For a short explanation of why the committee made the 2018 recommendations and how they might affect practice, see the rationale and impact section on incidental findings on chest X-ray or CT scans .
Full details of the evidence and the committee's discussion are in evidence review D: Diagnosing COPD and predicting outcomes .
Further investigations
At the time of their initial diagnostic evaluation in addition to spirometry all patients should have:
a chest radiograph to exclude other pathologies
a full blood count to identify anaemia or polycythaemia
body mass index (BMI) calculated. [2004]
Perform additional investigations when needed, as detailed in table 2. [2004, amended 2018]
| Investigation | Role |
|---|---|
| Sputum culture | To identify organisms if sputum is persistently present and purulent |
| Serial home peak flow measurements | To exclude asthma if diagnostic doubt remains |
| ECG and serum natriuretic peptides | To assess cardiac status if cardiac disease or pulmonary hypertension are suspected because of: See the for recommendations on using serum natriuretic peptides to diagnose heart failure. |
| Echocardiogram | To assess cardiac status if cardiac disease or pulmonary hypertension are suspected |
| CT scan of the thorax | To investigate symptoms that seem disproportionate to the spirometric impairment To investigate signs that may suggest another lung diagnosis (such as fibrosis or bronchiectasis) To investigate abnormalities seen on a chest X-ray To assess suitability for lung volume reduction procedures |
| Serum alpha-1 antitrypsin | To assess for alpha-1 antitrypsin deficiency if early onset, minimal smoking history or family history |
| Transfer factor for carbon monoxide (TLCO) | To investigate symptoms that seem disproportionate to the spirometric impairment To assess suitability for lung volume reduction procedures |
Offer people with alpha 1 antitrypsin deficiency a referral to a specialist centre to discuss how to manage their condition. [2004]
Reversibility testing
For most people, routine spirometric reversibility testing is not necessary as part of the diagnostic process or to plan initial therapy with bronchodilators or corticosteroids. It may be unhelpful or misleading because:
repeated FEV1 measurements can show small spontaneous fluctuations
the results of a reversibility test performed on different occasions can be inconsistent and not reproducible
over-reliance on a single reversibility test may be misleading unless the change in FEV1 is greater than 400 ml
the definition of the magnitude of a significant change is purely arbitrary
response to long-term therapy is not predicted by acute reversibility testing. [2004]
Untreated COPD and asthma are frequently distinguishable on the basis of history (and examination) in people presenting for the first time. Whenever possible, use features from the history and examination (such as those listed in table 3) to differentiate COPD from asthma. For more information on diagnosing asthma see the NICE guideline on asthma . [2004, amended 2018]
| – | COPD | Asthma |
|---|---|---|
| Smoker or ex-smoker | Nearly all | Possibly |
| Symptoms under age 35 | Rare | Often |
| Chronic productive cough | Common | Uncommon |
| Breathlessness | Persistent and progressive | Variable |
| Night time waking with breathlessness and/or wheeze | Uncommon | Common |
| Significant diurnal or day-to-day variability of symptoms | Uncommon | Common |
In addition to the features in table 3, use longitudinal observation of people (with spirometry, peak flow or symptoms) to help differentiate COPD from asthma. [2004]
When diagnostic uncertainty remains, or both COPD and asthma are present, use the following findings to help identify asthma:
a large (over 400 ml) response to bronchodilators
a large (over 400 ml) response to 30 mg oral prednisolone daily for 2 weeks
serial peak flow measurements showing 20% or greater diurnal or day-to-day variability. Clinically significant COPD is not present if the FEV1 and FEV1/FVC ratio return to normal with drug therapy. [2004]
If diagnostic uncertainty remains, think about referral for more detailed investigations, including imaging and measurement of transfer factor for carbon monoxide (TLCO). [2004]
Reconsider the diagnosis of COPD for people who report a marked improvement in symptoms in response to inhaled therapy. [2004]
Assessing severity and using prognostic factors
COPD is heterogeneous, so no single measure can adequately assess disease severity in an individual. Severity assessment is, nevertheless, important because it has implications for therapy and relates to prognosis.
Do not use a multidimensional index (such as BODE) to assess prognosis in people with stable COPD. [2018]
From diagnosis onwards, when discussing prognosis and treatment decisions with people with stable COPD, think about the following factors that are individually associated with prognosis:
smoking status
breathlessness (MRC scale)
chronic hypoxia and/or cor pulmonale
severity and frequency of exacerbations
hospital admissions
symptom burden (for example, COPD Assessment Test [CAT] score)
exercise capacity (for example, 6‑minute walk test)
whether the person meets the criteria for long-term oxygen therapy and/or home non-invasive ventilation
multimorbidity
frailty. [2010, amended 2018]
For a short explanation of why the committee made the 2018 recommendation and how it might affect practice, see the rationale and impact section on assessing severity and using prognostic factors .
Assessing and classifying the severity of airflow obstruction
Assess the severity of airflow obstruction according to the reduction in FEV1, as shown in table 4. [2010]
For people with mild airflow obstruction, only diagnose COPD if they have one or more of the symptoms in the recommendation on symptoms . [2010]
| Post-broncho-dilator FEV1/FVC | FEV1 % predicted | NICE guideline CG12 (2004) severity of airflow obstruction | ATS/ERS 2004 severity of airflow obstruction (post-broncho-dilator) | GOLD 2008 severity of airflow obstruction (post-broncho-dilator) | NICE guideline CG101 (2010) severity of airflow obstruction (post-broncho-dilator) |
|---|---|---|---|---|---|
| < 0.7 | ≥ 80% | Not categorised | Mild | Stage 1 – Mild | Stage 1 – Mild |
| < 0.7 | 50–79% | Mild | Moderate | Stage 2 – Moderate | Stage 2 – Moderate |
| < 0.7 | 30–49% | Moderate | Severe | Stage 3 – Severe | Stage 3 – Severe |
| < 0.7 | < 30% | Severe | Very severe | Stage 4 – Very severe (or FEV1 below 50% with respiratory failure) | Stage 4 – Very severe (or FEV1 below 50% with respiratory failure) |
ATS/ERS guidance: Celli BR, MacNee W (2004) Standards for the diagnosis and treatment of patients with COPD: a summary of the ATS/ERS position paper. European Respiratory Journal 23(6): 932–46.
GOLD guidance: Global Initiative for Chronic Obstructive Lung Disease (GOLD; 2008) Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease.
Identifying early disease
Perform spirometry in people who are over 35, current or ex‑smokers, and have a chronic cough. [2004]
Consider spirometry in people with chronic bronchitis. A significant proportion of these people will go on to develop airflow limitation. [2004]
Referral for specialist advice
When clinically indicated, refer people for specialist advice. Referral may be appropriate at all stages of the disease and not solely in the most severely disabled people (see table 5). [2004]
| Reason | Purpose |
|---|---|
| There is diagnostic uncertainty | Confirm diagnosis and optimise therapy |
| Suspected severe COPD | Confirm diagnosis and optimise therapy |
| The person with COPD requests a second opinion | Confirm diagnosis and optimise therapy |
| Onset of cor pulmonale | Confirm diagnosis and optimise therapy |
| Assessment for oxygen therapy | Optimise therapy and measure blood gases |
| Assessment for long-term nebuliser therapy | Optimise therapy and exclude inappropriate prescriptions |
| Assessment for oral corticosteroid therapy | Justify need for continued treatment or supervise withdrawal |
| Bullous lung disease | Identify candidates for lung volume reduction procedures |
| A rapid decline in FEV1 | Encourage early intervention |
| Assessment for pulmonary rehabilitation | Identify candidates for pulmonary rehabilitation |
| Assessment for a lung volume reduction procedure | Identify candidates for surgical or bronchoscopic lung volume reduction |
| Assessment for lung transplantation | Identify candidates for surgery |
| Dysfunctional breathing | Confirm diagnosis, optimise pharmacotherapy and access other therapists |
| Onset of symptoms under 40 years or a family history of alpha‑1 antitrypsin deficiency | Identify alpha‑1 antitrypsin deficiency, consider therapy and screen family |
| Symptoms disproportionate to lung function deficit | Look for other explanations including cardiac impairment, pulmonary hypertension, depression and hyperventilation |
| Frequent infections | Exclude bronchiectasis |
| Haemoptysis | Exclude carcinoma of the bronchus |
People who are referred do not always have to be seen by a respiratory physician. In some cases they may be seen by members of the COPD team who have appropriate training and expertise. [2004]
NICE has also produced a visual summary covering non-pharmacological management and use of inhaled therapies .
For guidance on the management of multimorbidity, see the NICE guideline on multimorbidity . [2018]
Smoking cessation
Document an up-to-date smoking history, including pack years smoked (number of cigarettes smoked per day, divided by 20, multiplied by the number of years smoked) for everyone with COPD. [2004]
At every opportunity, advise and encourage every person with COPD who is still smoking (regardless of their age) to stop, and offer them help to do so. [2004]
Unless contraindicated, offer nicotine replacement therapy, varenicline or bupropion as appropriate to people who want to stop smoking, combined with an appropriate support programme to optimise smoking quit rates for people with COPD. [2010]
For more guidance on helping people to quit smoking, see the NICE guideline on stop smoking interventions and services . [2010]
For more guidance on varenicline see the NICE technology appraisal guidance on varenicline for smoking cessation . [2010]
Inhaled therapy
Short-acting beta2 agonists (saba) and short-acting muscarinic antagonists (sama).
Use short-acting bronchodilators, as necessary, as the initial empirical treatment to relieve breathlessness and exercise limitation. [2004]
Inhaled corticosteroids (ICS)
Do not use oral corticosteroid reversibility tests to identify which people should be prescribed inhaled corticosteroids, because they do not predict response to inhaled corticosteroid therapy. [2004]
Be aware of, and be prepared to discuss with the person, the risk of side effects (including pneumonia) in people who take inhaled corticosteroids for COPD. Follow the MHRA safety advice on the risk of psychological and behavioural side effects associated with inhaled corticosteroids. [2010, amended 2018]
Inhaled combination therapy
Inhaled combination therapy refers to combinations of long-acting muscarinic antagonists (LAMA), long-acting beta2 agonists (LABA), and inhaled corticosteroids (ICS).
Do not assess the effectiveness of bronchodilator therapy using lung function alone. Include a variety of other measures such as improvement in symptoms, activities of daily living, exercise capacity, and rapidity of symptom relief. [2004]
Offer LAMA+LABA to people who:
have spirometrically confirmed COPD and
do not have asthmatic features/features suggesting steroid responsiveness and
remain breathless or have exacerbations despite:
having used or been offered treatment for tobacco dependence if they smoke and
optimised non-pharmacological management and relevant vaccinations and
using a short-acting bronchodilator. [2018] Follow the MHRA safety advice on Respimat and Handihaler inhalers .
Consider LABA+ICS for people who:
have asthmatic features/features suggesting steroid responsiveness and
using a short-acting bronchodilator. [2018]
For people who are using long-acting bronchodilators outside of the recommendations on offering LAMA and LABA and considering LABA+ICS and whose symptoms are under control, explain to them that they can continue with their current treatment until both they and their NHS healthcare professional agree it is appropriate to change. [2018]
Before starting LAMA+LABA+ICS, conduct a clinical review to ensure that:
the person's non-pharmacological COPD management is optimised and they have used or been offered treatment for tobacco dependence if they smoke
acute episodes of worsening symptoms are caused by COPD exacerbations and not by another physical or mental health condition
the person's day-to-day symptoms that are adversely impacting their quality of life are caused by COPD and not by another physical or mental health condition . [2019]
For people with COPD who are taking LABA+ICS, offer LAMA+LABA+ICS if:
their day-to-day symptoms continue to adversely impact their quality of life or
they have a severe exacerbation (requiring hospitalisation) or
they have 2 moderate exacerbations within a year. [2019]
For people with COPD who are taking LAMA+LABA, consider LAMA+LABA+ICS if:
For people with COPD who are taking LAMA+LABA and whose day-to-day symptoms adversely impact their quality of life:
consider a trial of LAMA+LABA+ICS, lasting for 3 months only
after 3 months, conduct a clinical review to establish whether or not LAMA+LABA+ICS has improved their symptoms:
if symptoms have not improved, stop LAMA+LABA+ICS and switch back to LAMA+LABA
if symptoms have improved, continue with LAMA+LABA+ICS. [2019]
Document the reason for continuing ICS use in clinical records and review at least annually. [2019]
Base the choice of drugs and inhalers on:
how much they improve symptoms
the person's preferences and ability to use the inhalers
the drugs' potential to reduce exacerbations
their side effects
their cost. Minimise the number of inhalers and the number of different types of inhaler used by each person as far as possible. [2018]
When prescribing long-acting drugs, ensure people receive inhalers they have been trained to use (for example, by specifying the brand and inhaler in prescriptions). [2018]
For a short explanation of why the committee made the 2018 and 2019 recommendations and how they might affect practice, see the rationale and impact section on inhaled combination therapy.
Full details of the evidence and the committee's discussion are in evidence review F: Inhaled therapies and evidence review I: Inhaled triple therapy .
Delivery systems used to treat stable COPD
Most people with COPD – whatever their age – can develop adequate inhaler technique if they are given training. However, people with significant cognitive impairment may be unable to use any form of inhaler device. In most people with COPD, however, a pragmatic approach guided by individual patient assessment is needed when choosing a device.
In most cases bronchodilator therapy is best administered using a hand-held inhaler (including a spacer if appropriate). [2004]
Provide an alternative inhaler if a person cannot use a particular one correctly or it is not suitable for them. [2004]
Only prescribe inhalers after people have been trained to use them and can demonstrate satisfactory technique. [2004]
People with COPD should have their ability to use an inhaler regularly assessed and corrected if necessary by a healthcare professional competent to do so. [2004]
Provide a spacer that is compatible with the person's metered-dose inhaler. [2004]
Advise people to use a spacer with a metered-dose inhaler in the following way:
administer the drug by single actuations of the metered-dose inhaler into the spacer, inhaling after each actuation
there should be minimal delay between inhaler actuation and inhalation
normal tidal breathing can be used as it is as effective as single breaths
repeat if a second dose is required. [2004]
Advise people on spacer cleaning. Tell them:
not to clean the spacer more than monthly, because more frequent cleaning affects their performance (because of a build-up of static)
to hand wash using warm water and washing-up liquid, and allow the spacer to air dry. [2004, amended 2018]
Think about nebuliser therapy for people with distressing or disabling breathlessness despite maximal therapy using inhalers. [2004]
Do not prescribe nebulised therapy without an assessment of the person's and/or carer's ability to use it. [2004]
Do not continue nebulised therapy without assessing and confirming that 1 or more of the following occurs:
a reduction in symptoms
an increase in the ability to undertake activities of daily living
an increase in exercise capacity
an improvement in lung function. [2004]
Use a nebuliser system that is known to be efficient. [2004] Follow the MHRA safety advice on non-CE-marked nebulisers for COPD .
Offer people a choice between a facemask and a mouthpiece to administer their nebulised therapy, unless the drug specifically requires a mouthpiece (for example, anticholinergic drugs). [2004]
If nebuliser therapy is prescribed, provide the person with equipment, servicing, and ongoing advice and support. [2004]
Oral therapy
Oral corticosteroids.
Long-term use of oral corticosteroid therapy in COPD is not normally recommended. Some people with advanced COPD may need long-term oral corticosteroids when these cannot be withdrawn following an exacerbation. In these cases, the dose of oral corticosteroids should be kept as low as possible. [2004]
Monitor people who are having long-term oral corticosteroid therapy for osteoporosis, and give them appropriate prophylaxis. Start prophylaxis without monitoring for people over 65. [2004]
Oral theophylline
In this section of the guideline, the term theophylline refers to slow-release formulations of the drug.
Theophylline should only be used after a trial of short-acting bronchodilators and long-acting bronchodilators, or for people who are unable to use inhaled therapy, as plasma levels and interactions need to be monitored. [2004]
Take particular caution when using theophylline in older people, because of differences in pharmacokinetics, the increased likelihood of comorbidities and the use of other medications. [2004]
Assess the effectiveness of theophylline by improvements in symptoms, activities of daily living, exercise capacity and lung function. [2004]
Reduce the dose of theophylline for people who are having an exacerbation if they are prescribed macrolide or fluoroquinolone antibiotics (or other drugs known to interact). [2004]
Oral mucolytic therapy
Consider mucolytic drug therapy for people with a chronic cough productive of sputum. [2004]
Only continue mucolytic therapy if there is symptomatic improvement (for example, reduction in frequency of cough and sputum production). [2004]
Do not routinely use mucolytic drugs to prevent exacerbations in people with stable COPD. [2010]
Oral anti-oxidant therapy
Treatment with alpha-tocopherol and beta-carotene supplements, alone or in combination, is not recommended. [2004]
Oral anti-tussive therapy
Anti-tussive therapy should not be used in the management of stable COPD. [2004]
Oral prophylactic antibiotic therapy
Before starting prophylactic antibiotic therapy in a person with COPD, think about whether respiratory specialist input is needed. [2018]
Consider azithromycin (usually 250 mg 3 times a week) for people with COPD if they:
do not smoke and
have optimised non-pharmacological management and inhaled therapies, relevant vaccinations and (if appropriate) have been referred for pulmonary rehabilitation and
continue to have 1 or more of the following, particularly if they have significant daily sputum production:
frequent (typically 4 or more per year) exacerbations with sputum production
prolonged exacerbations with sputum production
exacerbations resulting in hospitalisation. [2018] In July 2019, this was an off-label use of azithromycin. See NICE's information on prescribing medicines .
Before offering prophylactic antibiotics, ensure that the person has had:
sputum culture and sensitivity (including tuberculosis culture), to identify other possible causes of persistent or recurrent infection that may need specific treatment (for example, antibiotic-resistant organisms, atypical mycobacteria or Pseudomonas aeruginosa )
training in airway clearance techniques to optimise sputum clearance (see the recommendation in the section on physiotherapy )
a CT scan of the thorax to rule out bronchiectasis and other lung pathologies. [2018]
Before starting azithromycin, ensure the person has had:
an electrocardiogram (ECG) to rule out prolonged QT interval and
baseline liver function tests. [2018]
When prescribing azithromycin, advise people about the small risk of hearing loss and tinnitus, and tell them to contact a healthcare professional if this occurs. [2018]
Review prophylactic azithromycin after the first 3 months, and then at least every 6 months. [2018]
Only continue treatment if the continued benefits outweigh the risks. Be aware that there are no long-term studies on the use of prophylactic antibiotics in people with COPD. [2018]
For people who are taking prophylactic azithromycin and are still at risk of exacerbations, provide a non-macrolide antibiotic to keep at home as part of their exacerbation action plan (see the recommendation on offering antibiotics to keep at home in the section on self-management ). [2018]
Be aware that it is not necessary to stop prophylactic azithromycin during an acute exacerbation of COPD. [2018]
For a short explanation of why the committee made the 2018 recommendations and how they might affect practice, see the rationale and impact section on oral prophylactic antibiotic therapy .
Full details of the evidence and the committee's discussion are in evidence review E: Predicting and preventing exacerbations .
Oral phosphodiesterase-4 inhibitors
For guidance on treating severe COPD with roflumilast, see NICE's technology appraisal guidance on roflumilast for treating chronic obstructive pulmonary disease . [2018]
Long-term oxygen therapy
Be aware that inappropriate oxygen therapy in people with COPD may cause respiratory depression. [2004]
Assess the need for oxygen therapy in people with:
very severe airflow obstruction (FEV1 below 30% predicted)
cyanosis (blue tint to skin)
polycythaemia
peripheral oedema (swelling)
a raised jugular venous pressure
oxygen saturations of 92% or less breathing air. Also consider assessment for people with severe airflow obstruction (FEV1 30–49% predicted). Be aware that some pulse oximeters can underestimate or overestimate oxygen saturation levels, especially if the saturation level is borderline. Overestimation has been reported in people with dark skin. See also the NHS England Patient Safety Alert on the risk of harm from inappropriate placement of pulse oximeter probes . [2004]
Assess people for long-term oxygen therapy by measuring arterial blood gases on 2 occasions at least 3 weeks apart in people who have a confident diagnosis of COPD, who are receiving optimum medical management and whose COPD is stable. [2004]
Consider long-term oxygen therapy for people with COPD who do not smoke and who:
have a partial pressure of oxygen in arterial blood (PaO 2 ) below 7.3 kPa when stable or
have a PaO 2 above 7.3 and below 8 kPa when stable, if they also have 1 or more of the following:
secondary polycythaemia
peripheral oedema
pulmonary hypertension. See the MHRA alert on the risk of death and severe harm from failure to obtain and continue flow from oxygen cylinders . [2018]
Conduct and document a structured risk assessment for people being assessed for long-term oxygen therapy who meet the criteria in the recommendation on considering long-term oxygen therapy . As part of the risk assessment, cover the risks for both the person with COPD and the people who live with them, including:
the risks of falls from tripping over the equipment
the risks of burns and fires, and the increased risk of these for people who live in homes where someone smokes (including e‑cigarettes). Base the decision on whether long-term oxygen therapy is suitable on the results of the structured risk assessment. [2018]
For people who smoke or live with people who smoke, but who meet the other criteria for long-term oxygen therapy, ensure the person who smokes is offered smoking cessation advice and treatment, and referral to specialist stop smoking services (see the NICE guidelines on stop smoking interventions and services and medicines optimisation ). [2018]
Do not offer long-term oxygen therapy to people who continue to smoke despite being offered smoking cessation advice and treatment, and referral to specialist stop smoking services. [2018]
Advise people who are having long-term oxygen therapy that they should breathe supplemental oxygen for a minimum of 15 hours per day. [2018]
Do not offer long-term oxygen therapy to treat isolated nocturnal hypoxaemia caused by COPD. [2018]
To ensure everyone eligible for long-term oxygen therapy is identified, pulse oximetry should be available in all healthcare settings. [2004]
Oxygen concentrators should be used to provide the fixed supply at home for long-term oxygen therapy. [2004]
People who are having long-term oxygen therapy should be reviewed at least once per year by healthcare professionals familiar with long-term oxygen therapy. This review should include pulse oximetry. [2004]
For a short explanation of why the committee made the 2018 recommendations and how they might affect practice, see the rationale and impact section on long-term oxygen therapy .
Full details of the evidence and the committee's discussion are in evidence review B: Oxygen therapy in people with stable COPD .
Ambulatory oxygen therapy
Do not offer ambulatory oxygen to manage breathlessness in people with COPD who have mild or no hypoxaemia at rest. [2018]
Consider ambulatory oxygen in people with COPD who have exercise desaturation and are shown to have an improvement in exercise capacity with oxygen, and have the motivation to use oxygen. [2004, amended 2018]
Prescribe ambulatory oxygen to people who are already on long-term oxygen therapy, who wish to continue oxygen therapy outside the home, and who are prepared to use it. [2004]
Only prescribe ambulatory oxygen therapy after an appropriate assessment has been performed by a specialist. The purpose of the assessment is to assess the extent of desaturation, the improvement in exercise capacity with supplemental oxygen, and the oxygen flow rate needed to correct desaturation. [2004]
Small light-weight cylinders, oxygen-conserving devices and portable liquid oxygen systems should be available for people with COPD. [2004]
When choosing which equipment to prescribe, take account of the hours of ambulatory oxygen use and oxygen flow rate needed. [2004]
Short-burst oxygen therapy
Do not offer short-burst oxygen therapy to manage breathlessness in people with COPD who have mild or no hypoxaemia at rest. [2018]
For a short explanation of why the committee made the 2018 recommendations and how they might affect practice, see the rationale and impact section on ambulatory and oxygen short-burst oxygen therapy .
Non-invasive ventilation
Refer people who are adequately treated but have chronic hypercapnic respiratory failure and have needed assisted ventilation (whether invasive or non-invasive) during an exacerbation, or who are hypercapnic or acidotic on long-term oxygen therapy, to a specialist centre for consideration of long-term non-invasive ventilation. [2004]
Managing pulmonary hypertension and cor pulmonale
In this guideline 'cor pulmonale' is defined as a clinical condition that is identified and managed on the basis of clinical features. It includes people who have right heart failure secondary to lung disease and people whose primary pathology is salt and water retention, leading to the development of peripheral oedema (swelling).
Diagnosing pulmonary hypertension and cor pulmonale
Suspect a diagnosis of cor pulmonale for people with:
a raised venous pressure
a systolic parasternal heave
a loud pulmonary second heart sound. [2004]
It is recommended that the diagnosis of cor pulmonale is made clinically and that this process should involve excluding other causes of peripheral oedema (swelling). [2004]
Treating pulmonary hypertension
Do not offer the following treatments solely to manage pulmonary hypertension caused by COPD, except as part of a randomised controlled trial:
nitric oxide
pentoxifylline
phosphodiesterase-5 inhibitors
statins. [2018]
Treating cor pulmonale
Ensure that people with cor pulmonale caused by COPD are offered optimal COPD treatment, including advice and interventions to help them stop smoking. For people who need treatment for hypoxia, see the section on long-term oxygen therapy . [2018]
Oedema associated with cor pulmonale can usually be controlled symptomatically with diuretic therapy. [2004]
Do not use the following to treat cor pulmonale caused by COPD:
alpha-blockers
angiotensin-converting enzyme inhibitors
calcium channel blockers
digoxin (unless there is atrial fibrillation). [2018]
For a short explanation of why the committee made the 2018 recommendations and how they might affect practice, see the rationale and impact section on managing pulmonary hypertension and cor pulmonale .
Full details of the evidence and the committee's discussion are in evidence review A: Managing pulmonary hypertension and cor pulmonale .
Pulmonary rehabilitation
Pulmonary rehabilitation is defined as a multidisciplinary programme of care for people with chronic respiratory impairment. It is individually tailored and designed to optimise each person's physical and social performance and autonomy.
Make pulmonary rehabilitation available to all appropriate people with COPD (see the recommendation on offering pulmonary rehabilitation ), including people who have had a recent hospitalisation for an acute exacerbation. [2010]
Offer pulmonary rehabilitation to all people who view themselves as functionally disabled by COPD (usually Medical Research Council [MRC] grade 3 and above). Pulmonary rehabilitation is not suitable for people who are unable to walk, who have unstable angina or who have had a recent myocardial infarction. [2004]
For pulmonary rehabilitation programmes to be effective, and to improve adherence, they should be held at times that suit people, in buildings that are easy to get to and that have good access for people with disabilities. Places should be available within a reasonable time of referral. [2004]
Pulmonary rehabilitation programmes should include multicomponent, multidisciplinary interventions that are tailored to the individual person's needs. The rehabilitation process should incorporate a programme of physical training, disease education, and nutritional, psychological and behavioural intervention. [2004]
Advise people of the benefits of pulmonary rehabilitation and the commitment needed to gain these. [2004]
Vaccination and anti-viral therapy
Offer pneumococcal vaccination and an annual flu vaccination to all people with COPD, as recommended by the Chief Medical Officer. [2004]
For guidance on preventing and treating flu, see the NICE technology appraisals on oseltamivir, amantadine (review) and zanamivir for the prophylaxis of influenza and amantadine, oseltamivir and zanamivir for the treatment of influenza . [2004]
Lung surgery and lung volume reduction procedures
Offer a respiratory review to assess whether a lung volume reduction procedure is a possibility for people with COPD when they complete pulmonary rehabilitation and at other subsequent reviews, if all of the following apply:
they have severe COPD, with FEV1 less than 50% and breathlessness that affects their quality of life despite optimal medical treatment (see recommendations 1.2.11 to 1.2.17 in the section on inhaled combination therapy )
they do not smoke
they can complete a 6‑minute walk distance of at least 140 m (if limited by breathlessness). [2018]
At the respiratory review, refer the person with COPD to a lung volume reduction multidisciplinary team to assess whether lung volume reduction surgery or endobronchial valves are suitable if they have:
hyperinflation, assessed by lung function testing with body plethysmography and
emphysema on unenhanced CT chest scan and
optimised treatment for other comorbidities. [2018]
Only offer endobronchial coils as part of a clinical trial and after assessment by a lung volume reduction multidisciplinary team. [2018]
For more guidance on lung volume reduction procedures, see the NICE interventional procedures guidance on lung volume reduction surgery , endobronchial valves and endobronchial coils . [2018]
Refer people with COPD for an assessment for bullectomy if they are breathless and a CT scan shows a bulla occupying at least one third of the hemithorax. [2018]
Consider referral to a specialist multidisciplinary team to assess for lung transplantation for people who:
have severe COPD, with FEV1 less than 50% and breathlessness that affects their quality of life despite optimal medical treatment (see recommendations 1.2.11 to 1.2.17 in the section on inhaled combination therapy ) and
have completed pulmonary rehabilitation and
do not have contraindications for transplantation (for example, comorbidities or frailty). [2018]
Do not use previous lung volume reduction procedures as a reason not to refer a person for assessment for lung transplantation. [2018]
For a short explanation of why the committee made the 2018 recommendations and how they might affect practice, see the rationale and impact section on lung volume reduction procedures, bullectomy and lung transplantation .
Full details of the evidence and the committee's discussion are in evidence review G: Referral criteria for lung volume reduction procedures, bullectomy or lung transplantation .
Alpha‑1 antitrypsin replacement therapy
Alpha‑1 antitrypsin replacement therapy is not recommended for people with alpha‑1 antitrypsin deficiency (see also the recommendation on referral in the section on further investigations ). [2004]
Multidisciplinary management
COPD care should be delivered by a multidisciplinary team. [2004]
When defining the activity of the multidisciplinary team, think about the following functions:
assessment (including performing spirometry, assessing which delivery systems to use for inhaled therapy, the need for aids for daily living and assessing the need for oxygen)
care and treatment, including:
pulmonary rehabilitation
identifying and managing anxiety and depression
advising people on relaxation techniques
dietary issues
social security benefits and travel
hospital-at-home/early discharge schemes
non-invasive ventilation and palliative care
advising people on self-management strategies
identifying and monitoring people at high risk of exacerbations and undertaking activities to avoid emergency admissions
education for people with COPD, their carers, and for healthcare professionals. [2004]
Respiratory nurse specialists
It is recommended that the multidisciplinary COPD team includes respiratory nurse specialists. [2004]
Physiotherapy
If people have excessive sputum, they should be taught:
how to use positive expiratory pressure devices
active cycle of breathing techniques. [2004, amended 2018]
Identifying and managing anxiety and depression
Be alert for anxiety and depression in people with COPD. Consider whether people have anxiety or depression, particularly if they:
have severe breathlessness
are hypoxic
have been seen at or admitted to a hospital with an exacerbation of COPD. [2004, amended 2018]
For guidance on diagnosing and managing depression, see the NICE guideline on depression in adults with a chronic physical health problem . [2004]
For guidance on managing anxiety, see the NICE guideline on generalised anxiety disorder and panic disorder in adults . [2018]
Nutritional factors
Calculate BMI for people with COPD:
the normal range for BMI is 20 to less than 25 kg/m 2
refer people for dietetic advice if they have a BMI that is abnormal (high or low) or changing over time
for people with a low BMI, give nutritional supplements to increase their total calorific intake and encourage them to exercise to augment the effects of nutritional supplementation. [2004] The NICE guideline on obesity states that a healthy BMI range is 18.5 to 24.9 kg/m 2 , but note that this may not be appropriate for people with COPD.
For guidance on nutrition support, see the NICE guideline on nutrition support for adults . [2004]
Pay attention to changes in weight in older people, particularly if the change is more than 3 kg. [2004]
Palliative care
When appropriate, use opioids to relieve breathlessness in people with end-stage COPD that is unresponsive to other medical therapy. [2004]
When appropriate, use benzodiazepines, tricyclic antidepressants, major tranquillisers and oxygen for breathlessness in people with end-stage COPD that is unresponsive to other medical therapy. [2004]
People with end-stage COPD and their family members or carers (as appropriate) should have access to the full range of services offered by multidisciplinary palliative care teams, including admission to hospices. [2004]
For standards and measures on palliative care, see the NICE quality standard on end of life care for adults . [2018]
For guidance on care for people in the last days of life, see the NICE guideline on care of dying adults . [2018]
Assessment for occupational therapy
Regularly ask people with COPD about their ability to undertake activities of daily living and how breathless these activities make them. [2004]
Clinicians that care for people with COPD should assess their need for occupational therapy using validated tools. [2004]
Social services
Consider referring people for assessment by social services if they have disabilities caused by COPD. [2004]
Advice on travel
Assess people who are using long-term oxygen therapy and who are planning air travel in line with the British Thoracic Society recommendations . [2004]
Assess people with an FEV1 below 50% predicted who are planning air travel in line with the BTS recommendations. [2004]
Warn people with bullous disease that they are at a theoretically increased risk of a pneumothorax during air travel. [2004]
Advice on diving
Scuba diving is not generally recommended for people with COPD. Advise people with queries to seek specialist advice. [2004]
There are significant differences in the response of people with COPD and asthma to education programmes. Programmes designed for asthma should not be used in COPD. [2004]
At diagnosis and at each review appointment, offer people with COPD and their family members or carers (as appropriate):
written information about their condition
opportunities for discussion with a healthcare professional who has experience in caring for people with COPD. [2018]
Ensure the information provided is:
available on an ongoing basis
relevant to the stage of the person's condition
tailored to the person's needs. [2018]
At minimum, the information should cover:
an explanation of COPD and its symptoms
advice on quitting smoking (if relevant) and how this will help with the person's COPD
advice on avoiding passive smoke exposure
managing breathlessness
physical activity and pulmonary rehabilitation
medicines, including inhaler technique and the importance of adherence
vaccinations
identifying and managing exacerbations
details of local and national organisations and online resources that can provide more information and support
how COPD will affect other long-term conditions that are common in people with COPD (for example hypertension, heart disease, anxiety, depression and musculoskeletal problems). [2018]
Be aware of the obligation to provide accessible information as detailed in the NHS Accessible Information Standard . For more guidance on providing information to people and discussing their preferences with them, see the NICE guideline on patient experience in adult NHS services . [2018]
For a short explanation of why the committee made the 2018 recommendations and how they might affect practice, see the rationale and impact section on self-management, education and telehealth monitoring .
Full details of the evidence and the committee's discussion are in evidence review C: Self-management interventions, education and telehealth monitoring .
Advise people with COPD that the following factors increase their risk of exacerbations:
continued smoking or relapse for ex‑smokers
exposure to passive smoke
viral or bacterial infection
indoor and outdoor air pollution
lack of physical activity
seasonal variation (winter and spring). [2018]
For a short explanation of why the committee made the 2018 recommendation and how it might affect practice, see the rationale and impact section on risk factors for COPD exacerbations .
Self-management
Develop an individualised self-management plan in collaboration with each person with COPD and their family members or carers (as appropriate), and:
include education on all relevant points from the recommendation on the information that should be covered in the section on education
review the plan at future appointments. [2018]
Develop an individualised exacerbation action plan in collaboration with each person with COPD who is at risk of exacerbations. [2018]
Offer people a short course of oral corticosteroids and a short course of oral antibiotics to keep at home as part of their exacerbation action plan if:
they have had an exacerbation within the last year, and remain at risk of exacerbations
they understand and are confident about when and how to take these medicines, and the associated benefits and harms
they know to tell their healthcare professional when they have used the medicines, and to ask for replacements. [2018]
For guidance on the choice of antibiotics see the NICE guideline on antimicrobial prescribing for acute exacerbations of COPD . [2018]
At all review appointments, discuss corticosteroid and antibiotic use with people who keep these medicines at home, to check that they still understand how to use them. For people who have used 3 or more courses of oral corticosteroids and/or oral antibiotics in the last year, investigate the possible reasons for this. [2018]
See the recommendations on systemic corticosteroids for more guidance on oral corticosteroids. [2018]
Encourage people with COPD to respond promptly to exacerbation symptoms by following their action plan, which may include:
adjusting their short-acting bronchodilator therapy to treat their symptoms
taking a short course of oral corticosteroids if their increased breathlessness interferes with activities of daily living
adding oral antibiotics if their sputum changes colour and increases in volume or thickness beyond their normal day-to-day variation
telling their healthcare professional. [2018]
Ask people with COPD if they experience breathlessness they find frightening. If they do, consider including a cognitive behavioural component in their self-management plan to help them manage anxiety and cope with breathlessness. [2018]
For people at risk of hospitalisation, explain to them and their family members or carers (as appropriate) what to expect if this happens (including non-invasive ventilation and discussions on future treatment preferences, ceilings of care and resuscitation). [2018]
Telehealth monitoring
Do not offer routine telehealth monitoring of physiological status as part of management for stable COPD. [2018]
Fitness for general surgery
The ultimate clinical decision about whether or not to proceed with surgery should rest with a consultant anaesthetist and consultant surgeon, taking account of comorbidities, functional status and the need for the surgery. [2004]
It is recommended that lung function should not be the only criterion used to assess people with COPD before surgery. Composite assessment tools such as the ASA scoring system are the best predictors of risk. [2004]
If time permits, optimise the medical management of people with COPD before surgery. This might include a course of pulmonary rehabilitation. [2004]
Follow-up of people with COPD
Follow-up of all people with COPD should include:
highlighting the diagnosis of COPD in the case record and recording this using Read Codes on a computer database
recording the values of spirometric tests performed at diagnosis (both absolute and percent predicted)
offering advice and treatment to help them stop smoking, and referral to specialist stop smoking services (see the NICE guideline on stop smoking interventions and services )
recording the opportunistic measurement of spirometric parameters (a loss of 500 ml or more over 5 years will show which people have rapidly progressing disease and may need specialist referral and investigation). [2004, amended 2018]
Review people with COPD at least once per year and more frequently if indicated, and cover the issues listed in table 6. [2004]
For most people with stable severe COPD regular hospital review is not necessary, but there should be locally agreed mechanisms to allow rapid access to hospital assessment when needed. [2004]
When people with very severe COPD are reviewed in primary care they should be seen at least twice per year, and specific attention should be paid to the issues listed in table 6. [2004]
Specialists should regularly review people with severe COPD who need interventions such as long-term non-invasive ventilation. [2004]
| Mild/moderate/severe (stages 1 to 3) | Very severe (stage 4) | |
|---|---|---|
| Frequency | At least annual | At least twice per year |
| Clinical assessment |
|
|
| Measurements to make |
Definition of an exacerbation
An exacerbation is a sustained worsening of the patient's symptoms from their usual stable state which is beyond normal day-to-day variations, and is acute in onset. Commonly reported symptoms are worsening breathlessness, cough, increased sputum production and change in sputum colour. The change in these symptoms often necessitates a change in medication.
Assessing the need for hospital treatment
Use the factors in table 7 to assess whether people with COPD need hospital treatment. Be aware that some pulse oximeters can underestimate or overestimate oxygen saturation levels, especially if the saturation level is borderline. Overestimation has been reported in people with dark skin. See also the NHS England Patient Safety Alert on the risk of harm from inappropriate placement of pulse oximeter probes . [2004]
| Factor | Treat at home | Treat in hospital |
|---|---|---|
| Able to cope at home | Yes | No |
| Breathlessness | Mild | Severe |
| General condition | Good | Poor/deteriorating |
| Level of activity | Good | Poor/confined to bed |
| Cyanosis | No | Yes |
| Worsening peripheral oedema | No | Yes |
| Level of consciousness | Normal | Impaired |
| Already receiving long-term oxygen therapy | No | Yes |
| Social circumstances | Good | Living alone/not coping |
| Acute confusion | No | Yes |
| Rapid rate of onset | No | Yes |
| Significant comorbidity (particularly cardiac disease and insulin-dependent diabetes) | No | Yes |
| SaO < 90% | No | Yes |
| Changes on chest radiograph | No | Present |
| Arterial pH level | ≥ 7.35 | < 7.35 |
| Arterial PaO | ≥ 7 kPa | < 7 kPa |
Investigating an exacerbation
The diagnosis of an exacerbation is made clinically and does not depend on the results of investigations. However, investigations may sometimes be useful in ensuring appropriate treatment is given. Different investigation strategies are needed for people in hospital (who will tend to have more severe exacerbations) and people in the community.
Primary care
For people who have their exacerbation managed in primary care:
sending sputum samples for culture is not recommended in routine practice
pulse oximetry is of value if there are clinical features of a severe exacerbation. Be aware that some pulse oximeters can underestimate or overestimate oxygen saturation levels, especially if the saturation level is borderline. Overestimation has been reported in people with dark skin. See also the NHS England Patient Safety Alert on the risk of harm from inappropriate placement of pulse oximeter probes . [2004]
People referred to hospital
In all people presenting to hospital with an acute exacerbation:
obtain a chest X-ray
measure arterial blood gas tensions and record the inspired oxygen concentration
record an ECG (to exclude comorbidities)
perform a full blood count and measure urea and electrolyte concentrations
measure a theophylline level on admission in people who are taking theophylline therapy
send a sputum sample for microscopy and culture if the sputum is purulent
take blood cultures if the person has pyrexia. [2004, amended 2018]
Hospital-at-home and assisted-discharge schemes
Hospital-at-home and assisted-discharge schemes are safe and effective and should be used as an alternative way of caring for people with exacerbations of COPD who would otherwise need to be admitted or stay in hospital. [2004]
The multiprofessional team that operates these schemes should include allied health professionals with experience in managing COPD, and may include nurses, physiotherapists, occupational therapists and other health workers. [2004]
There are currently insufficient data to make firm recommendations about which people with COPD with an exacerbation are most suitable for hospital-at-home or early discharge. Selection should depend on the resources available and absence of factors associated with a worse prognosis (for example, acidosis). [2004]
Include people's preferences about treatment at home or in hospital in decision-making. [2004]
Pharmacological management
Increased breathlessness is a common feature of COPD exacerbations. This is usually managed by taking increased doses of short-acting bronchodilators.
Delivery systems for inhaled therapy during exacerbations
Both nebulisers and hand-held inhalers can be used to administer inhaled therapy during exacerbations of COPD. [2004]
The choice of delivery system should reflect the dose of drug needed, the person's ability to use the device, and the resources available to supervise therapy administration. [2004]
Change people to hand-held inhalers as soon as their condition has stabilised, because this may allow them to be discharged from hospital earlier. [2004]
If a person with COPD is hypercapnic or acidotic the nebuliser should be driven by compressed air rather than oxygen (to avoid worsening hypercapnia). If oxygen therapy is needed, administer it simultaneously by nasal cannulae. [2004]
The driving gas for nebulised therapy should always be specified in the prescription. [2004]
Systemic corticosteroids
In the absence of significant contraindications, use oral corticosteroids, in conjunction with other therapies, in all people admitted to hospital with a COPD exacerbation. [2004]
In the absence of significant contraindications, consider oral corticosteroids for people in the community who have an exacerbation with a significant increase in breathlessness that interferes with daily activities. [2004]
Encourage people who need corticosteroid therapy to present early to get maximum benefits. [2004]
Offer 30 mg oral prednisolone daily for 5 days. [2019]
For guidance on stopping oral corticosteroid therapy it is recommended that clinicians refer to the BNF. [2004]
Think about osteoporosis prophylaxis for people who need frequent courses of oral corticosteroids. [2004]
Make people aware of the optimum duration of treatment and the adverse effects of prolonged therapy. [2004]
Give people (particularly people discharged from hospital) clear instructions on why, when and how to stop their corticosteroid treatment. [2004]
For a short explanation of why the committee made the 2019 recommendation and how it might affect practice, see the rationale and impact section on duration of oral corticosteroid for managing exacerbations .
Full details of the evidence and the committee's discussion are in evidence review J: Length of corticosteroid use during exacerbations .
Antibiotics
For guidance on using antibiotics to treat COPD exacerbations, see the NICE guideline on antimicrobial prescribing for acute exacerbations of COPD . [2018]
Theophylline and other methylxanthines
Only use intravenous theophylline as an adjunct to exacerbation management if there is an inadequate response to nebulised bronchodilators. [2004]
Take care when using intravenous theophylline, because of its interactions with other drugs and potential toxicity if the person has been taking oral theophylline. [2004]
Monitor theophylline levels within 24 hours of starting treatment, and as frequently as indicated by the clinical circumstances after this. [2004]
Respiratory stimulants
It is recommended that doxapram is used only when non-invasive ventilation is either unavailable or inappropriate. [2004]
Oxygen therapy during exacerbations of COPD
Measure oxygen saturation in people with an exacerbation if there are no facilities to measure arterial blood gases. [2004]
If necessary, prescribe oxygen to keep the oxygen saturation of arterial blood (SaO 2 ) within the individualised target range. [2010]
Pulse oximeters should be available to all healthcare professionals involved in the care of people with exacerbations of COPD, and they should be trained in their use. Clinicians should be aware that pulse oximetry gives no information about the PaCO 2 or pH. Be aware that some pulse oximeters can underestimate or overestimate oxygen saturation levels, especially if the saturation level is borderline. Overestimation has been reported in people with dark skin. See also the NHS England Patient Safety Alert on the risk of harm from inappropriate placement of pulse oximeter probes . [2004]
Measure arterial blood gases and note the inspired oxygen concentration in all people who arrive at hospital with an exacerbation of COPD. Repeat arterial blood gas measurements regularly, according to the response to treatment. [2004]
Non-invasive ventilation (NIV) and COPD exacerbations
Use NIV as the treatment of choice for persistent hypercapnic ventilatory failure during exacerbations despite optimal medical therapy. [2004]
It is recommended that NIV should be delivered in a dedicated setting, with staff who have been trained in its application, who are experienced in its use and who are aware of its limitations. [2004]
When people are started on NIV there should be a clear plan covering what to do in the event of deterioration, and ceilings of therapy should be agreed. [2004]
Invasive ventilation and intensive care
Treat hospitalised exacerbations of COPD on intensive care units, including invasive ventilation when this is thought to be necessary. [2004]
When assessing suitability for intubation and ventilation during exacerbations, think about functional status, BMI, need for oxygen when stable, comorbidities and previous admissions to intensive care units, in addition to age and FEV1. Neither age nor FEV1 should be used in isolation when assessing suitability. [2004]
Consider NIV for people who are slow to wean from invasive ventilation. [2004]
Respiratory physiotherapy and exacerbations
Consider physiotherapy using positive expiratory pressure devices for selected people with exacerbations of COPD, to help with clearing sputum. [2004, amended 2018]
Monitoring recovery from an exacerbation
Monitor people's recovery by regular clinical assessment of their symptoms and observation of their functional capacity. [2004]
Use pulse oximetry to monitor the recovery of people with non-hypercapnic, non-acidotic respiratory failure. [2004]
Use intermittent arterial blood gas measurements to monitor the recovery of people with respiratory failure who are hypercapnic or acidotic, until they are stable. [2004]
Do not routinely perform daily monitoring of peak expiratory flow (PEF) or FEV1 to monitor recovery from an exacerbation, because the magnitude of changes is small compared with the variability of the measurement. [2004]
Discharge planning
Measure spirometry in all people before discharge. [2004]
Re-establish people on their optimal maintenance bronchodilator therapy before discharge. [2004]
People who have had an episode of respiratory failure should have satisfactory oximetry or arterial blood gas results before discharge. [2004]
Assess all aspects of the routine care that people receive (including appropriateness and risk of side effects) before discharge. [2004]
Give people (or home carers) appropriate information to enable them to fully understand the correct use of medications, including oxygen, before discharge. [2004]
Make arrangements for follow-up and home care (such as visiting nurse, oxygen delivery or referral for other support) before discharge. [2004]
The person, their family and their physician should be confident that they can manage successfully before they are discharged. A formal activities of daily living assessment may be helpful when there is still doubt. [2004]
Asthmatic features/features suggesting steroid responsiveness
This includes any previous, secure diagnosis of asthma or of atopy, a higher blood eosinophil count, substantial variation in FEV1 over time (at least 400 ml) or substantial diurnal variation in peak expiratory flow (at least 20%).
Exacerbation
A general classification of the severity of an acute exacerbation (from a Cochrane Library systematic review ) is:
mild exacerbation, the person has an increased need for medication, which they can manage in their own normal environment
moderate exacerbation, the person has a sustained worsening of respiratory status that requires treatment with systemic corticosteroids and/or antibiotics
severe exacerbation, the person experiences a rapid deterioration in respiratory status that requires hospitalisation.
Mild or no hypoxaemia
People who are not taking long-term oxygen and who have a mean PaO 2 greater than 7.3k Pa.
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
- My Bibliography
- Collections
- Citation manager
Save citation to file
Email citation, add to collections.
- Create a new collection
- Add to an existing collection
Add to My Bibliography
Your saved search, create a file for external citation management software, your rss feed.
- Search in PubMed
- Search in NLM Catalog
- Add to Search
Usefulness of the Medical Research Council (MRC) dyspnoea scale as a measure of disability in patients with chronic obstructive pulmonary disease
Affiliation.
- 1 Division of Physiological Medicine, St George's Hospital Medical School, London SW17 0RE, UK.
- PMID: 10377201
- PMCID: PMC1745516
- DOI: 10.1136/thx.54.7.581
Background: Methods of classifying chronic obstructive pulmonary disease (COPD) depend largely upon spirometric measurements but disability is only weakly related to measurements of lung function. With the increased use of pulmonary rehabilitation, a need has been identified for a simple and standardised method of categorising disability in COPD. This study examined the validity of the Medical Research Council (MRC) dyspnoea scale for this purpose.
Methods: One hundred patients with COPD were recruited from an outpatient pulmonary rehabilitation programme. Assessments included the MRC dyspnoea scale, spirometric tests, blood gas tensions, a shuttle walking test, and Borg scores for perceived breathlessness before and after exercise. Health status was assessed using the St George's Respiratory Questionnaire (SGRQ) and Chronic Respiratory Questionnaire (CRQ). The Nottingham Extended Activities of Daily Living (EADL) score and Hospital Anxiety and Depression (HAD) score were also measured.
Results: Of the patients studied, 32 were classified as having MRC grade 3 dyspnoea, 34 MRC grade 4 dyspnoea, and 34 MRC grade 5 dyspnoea. Patients with MRC grades 1 and 2 dyspnoea were not included in the study. There was a significant association between MRC grade and shuttle distance, SGRQ and CRQ scores, mood state and EADL. Forced expiratory volume in one second (FEV1) was not associated with MRC grade. Multiple logistic regression showed that the determinants of disability appeared to vary with the level of disability. Between MRC grades 3 and 4 the significant covariates were exercise performance, SGRQ and depression score, whilst between grades 4 and 5 exercise performance and age were the major determinants.
Conclusions: The MRC dyspnoea scale is a simple and valid method of categorising patients with COPD in terms of their disability that could be used to complement FEV1 in the classification of COPD severity.
PubMed Disclaimer
Similar articles
- Stages of disease severity and factors that affect the health status of patients with chronic obstructive pulmonary disease. Hajiro T, Nishimura K, Tsukino M, Ikeda A, Oga T. Hajiro T, et al. Respir Med. 2000 Sep;94(9):841-6. doi: 10.1053/rmed.2000.0804. Respir Med. 2000. PMID: 11001074
- Analysis of clinical methods used to evaluate dyspnea in patients with chronic obstructive pulmonary disease. Hajiro T, Nishimura K, Tsukino M, Ikeda A, Koyama H, Izumi T. Hajiro T, et al. Am J Respir Crit Care Med. 1998 Oct;158(4):1185-9. doi: 10.1164/ajrccm.158.4.9802091. Am J Respir Crit Care Med. 1998. PMID: 9769280
- Analysis of longitudinal changes in dyspnea of patients with chronic obstructive pulmonary disease: an observational study. Oga T, Tsukino M, Hajiro T, Ikeda A, Nishimura K. Oga T, et al. Respir Res. 2012 Sep 25;13(1):85. doi: 10.1186/1465-9921-13-85. Respir Res. 2012. PMID: 23006638 Free PMC article.
- Measurement of dyspnoea in chronic obstructive pulmonary disease. Eakin EG, Kaplan RM, Ries AL. Eakin EG, et al. Qual Life Res. 1993 Jun;2(3):181-91. doi: 10.1007/BF00435222. Qual Life Res. 1993. PMID: 8401454 Review.
- Fixed-intensity exercise tests to measure exertional dyspnoea in chronic heart and lung populations: a systematic review. Palmer T, Obst SJ, Aitken CR, Walsh J, Sabapathy S, Adams L, Morris NR. Palmer T, et al. Eur Respir Rev. 2023 Aug 9;32(169):230016. doi: 10.1183/16000617.0016-2023. Print 2023 Sep 30. Eur Respir Rev. 2023. PMID: 37558262 Free PMC article. Review.
- Self-perceived barriers to healthcare access for patients with post COVID-19 condition. Brus IM, Spronk I, Polinder S, Loohuis AGMO, Tieleman P, Heemskerk SCM, Biere-Rafi S, Haagsma JA. Brus IM, et al. BMC Health Serv Res. 2024 Sep 6;24(1):1035. doi: 10.1186/s12913-024-11488-w. BMC Health Serv Res. 2024. PMID: 39243076 Free PMC article.
- SPECT/CT to quantify early small airway disease and its relationship to clinical symptoms in smokers with normal lung function: a pilot study. Juneau D, Leblond A, Chatta R, Lévesque V, Lussier A, Dubé BP. Juneau D, et al. Front Physiol. 2024 Aug 15;15:1417463. doi: 10.3389/fphys.2024.1417463. eCollection 2024. Front Physiol. 2024. PMID: 39210972 Free PMC article.
- Breaking down barriers to COPD management in primary care: applying the updated 2023 Canadian Thoracic Society guideline for pharmacotherapy. Kaplan A, Babineau A, Hauptman R, Levitz S, Lin P, Yang M. Kaplan A, et al. Front Med (Lausanne). 2024 Aug 6;11:1416163. doi: 10.3389/fmed.2024.1416163. eCollection 2024. Front Med (Lausanne). 2024. PMID: 39165372 Free PMC article. Review.
- Baseline Characteristics in the Remote Diet Intervention to REduce long-COVID Symptoms Trial (ReDIRECT). Haag L, Richardson J, Haig C, Cunningham Y, Fraser H, Brosnahan N, Ibbotson T, Ormerod J, White C, McIntosh E, O'Donnell K, Sattar N, McConnachie A, Lean M, Blane D, Combet E. Haag L, et al. NIHR Open Res. 2024 Mar 5;4:7. doi: 10.3310/nihropenres.13522.1. eCollection 2024. NIHR Open Res. 2024. PMID: 39145102 Free PMC article.
- Frequency, persistence and relation of disease symptoms, psychosomatic comorbidity and daily life impairment after COVID-19: a cohort study in general practice. Hapfelmeier A, Donhauser J, Teusen C, Eck S, Schneider A. Hapfelmeier A, et al. BMC Prim Care. 2024 Aug 10;25(1):295. doi: 10.1186/s12875-024-02551-w. BMC Prim Care. 2024. PMID: 39127653 Free PMC article.
- Br Med J (Clin Res Ed). 1983 Jan 15;286(6360):171-3 - PubMed
- Acta Psychiatr Scand. 1983 Jun;67(6):361-70 - PubMed
- Thorax. 1987 Oct;42(10):773-8 - PubMed
- Disabil Rehabil. 1992 Jan-Mar;14(1):41-3 - PubMed
- Am Rev Respir Dis. 1992 Jun;145(6):1321-7 - PubMed
Publication types
- Search in MeSH
Related information
- Cited in Books

LinkOut - more resources
Full text sources.
- Europe PubMed Central
- Ovid Technologies, Inc.
- PubMed Central
Other Literature Sources
- The Lens - Patent Citations
- MedlinePlus Health Information
- Citation Manager
NCBI Literature Resources
MeSH PMC Bookshelf Disclaimer
The PubMed wordmark and PubMed logo are registered trademarks of the U.S. Department of Health and Human Services (HHS). Unauthorized use of these marks is strictly prohibited.

Symptoms of COPD
3) medical research council dyspnoea (breathlessness) scale.
During your appointment your doctor or nurse will assess your breathlessness to see how it affects your day to day living by asking a series of questions such as;
- How far you can walk before you get breathless?
- How fast you can walk on level ground or going up a hill?
- How quickly you get breathless when you are walking?
These questions are part of an assessment known as the CAT score and the MRC score.
In the table below you can see the MRC score
| 1 | 2 | 3 | 4 | 5 |
|---|---|---|---|---|
| You are not troubled by breathlessness except on strenuous exercise. | You are short of breath when hurrying on the level or walking up a slight hill. | You walk slower than most people on the level, stop after a mile or so, or stop after 15 minutes walking at own pace. | You stop for breath after walking about 100 yards (60 metres) or after a few minutes on level ground. | You are too breathless to leave the house, or breathless when dressing or undressing. |
Source: The MRC breathlessness scale adapted from Fletcher C.M, Discussion on the Diagnosis of Pulmonary Emphysema J R Soc Med September 1952 45: 576-586
Thank you for visiting nature.com. You are using a browser version with limited support for CSS. To obtain the best experience, we recommend you use a more up to date browser (or turn off compatibility mode in Internet Explorer). In the meantime, to ensure continued support, we are displaying the site without styles and JavaScript.
- View all journals
- Explore content
- About the journal
- Publish with us
- Sign up for alerts
- Open access
- Published: 10 September 2024
Pilot study of home-based monitoring for early prediction of acute exacerbations in patients with fibrosing interstitial lung diseases
- Hongyan Fu 1 , 3 ,
- Zhaojun Wang 4 ,
- Zhengyu Hu 1 , 2 , 8 ,
- Tingting Zhao 1 , 2 ,
- Hongxia Xin 1 , 2 ,
- Jia Hou 2 ,
- Yanjuan Yang 2 ,
- Yanan Zhang 2 ,
- Wangshu Jiang 6 ,
- Faxuan Wang 7 ,
- Ning Deng 6 &
- Juan Chen 1 , 2
Scientific Reports volume 14 , Article number: 21101 ( 2024 ) Cite this article
Metrics details
- Health care
- Predictive markers
- Respiration
This study aimed to assess the potential of home monitoring using a monitoring application for the early prediction of acute exacerbations (AEs) in patients with fibrosing interstitial lung diseases (F-ILDs) by tracking symptoms, peripheral blood oxygen saturation (SpO 2 ), and heart rate (HR). Data on symptoms, SpO 2 , and HR before and after a 1-min sit-to-stand test (1STST) were collected using an online home monitoring application. Symptoms were recorded at least 3 times a week, including cough intensity and frequency (Cough Assessment Test scale (COAT) score), breathlessness grade (modified Medical Research Council (mMRC) score), and SpO 2 and HR before and after 1STST. Eighty-five patients with stable F-ILDs were enrolled. We observed a significant increase in COAT and mMRC scores, alongside a significant decrease in SpO 2 before and after 1STST, 2 weeks before the first recorded AE. Furthermore, a combination of variables-an increase in COAT (≥ 4) and mMRC(≥ 1) scores, a decrease in SpO 2 at rest (≥ 5%), and a decrease in SpO 2 after 1STST (≥ 4%)- proved the most effective in predicting AE onset in patients with F-ILDs at 2 weeks before the first recorded AE. Home telemonitoring of symptoms, SpO 2 holds potential value for early AE detection in patients with F-ILDs.
Similar content being viewed by others

Development of airflow limitation, dyspnoea, and both in the general population: the Nagahama study

Pulmonary function testing in COPD: looking beyond the curtain of FEV1
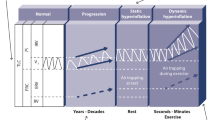
Targeting exertional breathlessness to improve physical activity: the role of primary care
Introduction.
Fibrosing interstitial lung diseases (F-ILDs) are a group of heterogeneous diseases characterized by a high symptom burden and often poor prognosis 1 . Patients with F-ILDs may experience acute respiratory deterioration, known as acute exacerbations (AEs), which are associated with hospitalization and reduced short-term survival 2 . Retrospective studies have reported 1-year incidences of AE-IPF, ranging from 7 to 19.1% 3 , 4 . However, data on AE-ILD frequency in non-IPF F-ILDs are scarce. The estimated 1-year incidence of AE-connective tissue disease (CTD) ranges from 1.25 to 3.3% 5 . Pathophysiologically, AEs of F-ILDs often present as diffuse alveolar damage 6 .
AE of F-ILDs is difficult to be predicted or prevented; therefore, efforts should focus on identifying the early window of AE onset in these patients 7 . Symptoms, such as increased breathlessness and cough may correlate with disease progression in patients with IPF 8 , 9 . Thus, assessing predictive symptoms of AE onset in patients with F-ILDs is crucial in clinical practice 10 .
Exertional hypoxemia is a critical feature in patients with F-ILDs 11 . The 6-min walk test (6MWT) is a validated submaximal exercise test used to assess exercise tolerance and exercise-induced desaturation in patients with various chronic lung diseases 12 . Low peripheral blood oxygen saturation (SpO 2 ) during the 6MWT is a strong predictor of AE and mortality in patients with IPF 13 . International guidelines recommend assessing exercise-induced desaturation in patients with interstitial lung diseases (ILDs) 14 . However, the 6MWT is not feasible for home care. Thus, the 1-min sit-to-stand (1STST) test can serve as an alternative indicator for monitoring exertional SpO 2 desaturation in patients with ILDs 15 . Further study is needed to assess the utility of SpO 2 desaturation monitoring during the 1STST test in evaluating disease progression in patients with F-ILDs.
Home monitoring of symptoms and physiological variables has become increasingly feasible with telemonitoring applications 16 . Home monitoring application offers an acceptable and accessible platform for collecting patient-reported objective and subjective data as demonstrated in IPF cases 17 , 18 . However, whether adopting a similar approach is feasible or clinically significant for F-ILDs remains unknown. Currently, there is limited information regarding the clinical benefits of remote monitoring in identifying the risk factors for AE onset in patients with F-ILDs. Therefore, this study aims to assess the potential of the 1STST and the home monitoring of symptoms, SpO 2 , and heart rate (HR) at rest for the early detection of AE in patients with F-ILDs.
Participants
This prospective pilot study was conducted at the General Hospital of Ningxia Medical University (Yinchuan, China). Approval was obtained from the Medical ethics committee (No. KYLL-2021-456), and participants provided written informed consent. This study adhered to the principles of the Declaration of Helsinki, and patients’ privacy was strictly upheld during the statistical analysis. Recruitment occurred between November 2020 and July 2023. The inclusion criteria were as follows: (1) a clinical diagnosis of F-ILDs, including IPF, interstitial pneumonia with autoimmune features (IPAF), fibrotic idiopathic nonspecific interstitial pneumonitis (F-iNSIP), connective tissue disease- associated ILD (CTD-ILD), fibrotic hypersensitivity pneumonitis (F-HP), and unclassified ILD, confirmed through multidisciplinary evaluation by pulmonologists, radiologists, pathologists, and rheumatologists 1 , (2) age ≥ 18 years 19 ; (3) stability of disease stage, with no history of AE in the past month; and (4) capability of using a smartphone. The exclusion criteria were as follows: (1) diagnosis of unstable cardiac disease, limb dysfunction, or pulmonary diseases other than ILDs, (e.g., chronic obstructive pulmonary disease (COPD), asthma, and obstructive sleep apnea-hypopnea syndrome); (2) significant mental health disorder; (3) inability to understand or use smartphones; and (4) participation in another home monitoring program for at least 3 months. The workflow of study is illustrated in Fig. 1 . AE was diagnosed following the 2016 definition and the diagnostic criteria for AE of IPF: acute worsening of breathlessness (typically < 1 month), new bilateral ground glass abnormality or consolidation superimposed on a background reticular or honeycomb pattern on high-resolution computed tomography (HRCT), and exclusion of alternative causes such as left heart failure and pulmonary embolism 20 . Once the participants were suspected of having AE and admitted to the emergency department, AE diagnosis was confirmed through multidisciplinary treatment (MDT) based on clinical manifestations. The treatment of AE is mainly based on correcting hypoxemia, looking for reversible etiologies of respiratory decline, and palliation of symptoms.
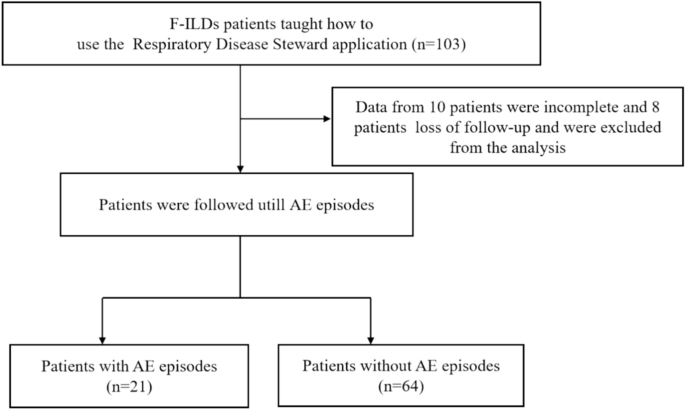
Study profile summarizing participant recruitment and their AE recorded in the study. Abbreviations: AE, Acute exacerbations; F-ILDs, fibrosing interstitial lung diseases.
Description of the home monitoring system
All the patients were enrolled in the home monitoring system collaboration with Zhejiang University, Hangzhou, China. The home monitoring system was described in our previous study 21 . The Closed-Loop Care Pathway System includes risk evaluation, follow-up, warnings, and medication management. Healthcare providers regularly follow up with patients to track their health status. The patients’ self-monitoring data and compliance were assessed daily to identify abnormal conditions. Initially, we designed and applied this system to patients with COPD, and we modified parts of the application modules for use by patients with F-ILD in this study. The system comprises a patient application, a doctor workstation, and a cloud server. The application ran on a smartphone and had two main modules: a diary and an education module. The diary module guided patients in recording their daily symptoms and physiological variables. Symptoms were recorded at least 3 times weekly. Patients were required to complete a questionnaire that included the modified Medical Research Council (mMRC) score 22 and the Cough Assessment Test scale (COAT) score 23 ). Additionally, a video-based 1STST was provided. At enrollment, patients were trained in person how to conduct 1STST, and participants were confirmed that they could conduct it correctly. Participant was required to conduct it at home at least 3 times weekly. The patients were initially enrolled in the study, and healthcare professionals provided detailed guidance to ensure their correct cooperation. The 1STST protocol adhered to previously published studies and guidelines 15 , 24 . SpO 2 and HR before and after 1STST were recorded using pulse oximeters (Yuwell, FS20D, China) and transferred to system. Home monitoring system includes symptoms, COAT, mMRC scale, 1STST, SpO 2 , HR at rest and after 1-min sit-to-stand test (1STST) were measured at least 3 times weekly. Due to patient dependency, all three or more weekly patient completion records were included for data analysis. All the completed data from above listed monitoring indicators during the entire period of study were included in the final data analysis. Home oxygen therapy was recommended when patients had an SpO 2 < 88%. Healthcare professionals monitored the data and followed up with the patients through telephone calls. The education module comprised ILD-related educational materials presented as videos and texts. All participants underwent training and received a hard copy of the instruction manual to ensure proper utilization of the home monitoring system. The proposed algorithm for telemonitoring during F-ILDs is shown in Fig. 2 . Description of Home Monitoring system was summarized in Supplemental file 1 .
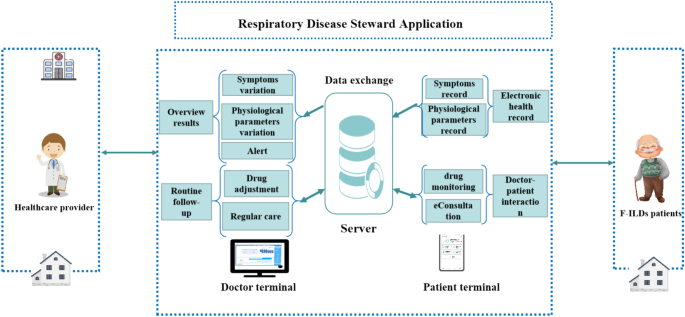
Propositions of the algorithm for telemonitoring in F-ILDs. Abbreviations: F-ILDs, fibrotic interstitial lung diseases.
Warning monitoring
We established an acceptable range of daily symptoms and physiological variables. If any of the following conditions were observed during home monitoring—COAT score ≥ 6, mMRC score ≥ 2 and SpO 2 ≤ 88% at rest and after 1STST,—the system could automatically generate appropriate reminders for the patient. If a readout exceeded the acceptable range or if there were other unintended effects of the study, an alert was sent to the healthcare website, and the healthcare providers supervised patients through the website.
Clinical follow-up
All enrolled patients with F-ILDs were monitored using a home monitoring platform, with routine investigations conducted face-to-face and over the telephone. Respiratory symptoms, HRCT findings, and pulmonary function tests were assessed at the outpatient clinic every 3 months. The patients maintained a diary to record unscheduled medical visits, acute worsening of their respiratory symptoms, and changes in SpO 2 and HR. Once a participant was suspected of having an AE, they were admitted to the emergency department for further diagnosis and treatment by MDT. The treatment is mainly based on correcting hypoxemia, looking for reversible etiologies of respiratory decline, and palliation of symptoms. Before discharge, he/she was assessed by a clinician. Within 1 month after discharge, the patients would not participate in the monitoring program but could continue to participate in the monitoring program after evaluation by the clinician. Survival was calculated from the first visit to the outcome or the end of the follow-up period.
Statistical analysis
Data were analyzed using the IBM SPSS Statistics 26 ( https://www.ibm.com/support/pages/ downloading-ibm-spss-statistics-26). All quantitative variables are presented as mean ± standard deviation (SD), non-parametric data as median and interquartile range (IQR). A generalized linear model was used to analyze changes in symptoms and physiological dynamic variables during four phases: stable state and 3, 2, and 1 week before the first recorded AE. A receiver operating characteristic (ROC) curve was utilized to identify the optimal combination of symptoms and physiological variables monitored in the respiratory disease ward to predict AE onset. Survival curves were generated using the Kaplan–Meier method. Statistical significance was set at p < 0.05.
Patient demographics
Patients demographics are presented in Table 1 . Initially, 103 patients with F-ILDs were enrolled in our cohort. However, 10 patients were excluded due to incomplete data and eight were excluded owing to loss of follow-up. Overall, we analyzed 85 participants, Among them, 52 (61.2%) had IPF, while 33 (38.8%) had non-IPF F-ILDs. Among the non-IPF F-ILDs cases, nine were IPAF (10.6%), nine were F-iNSIP (10.6%), eight were CTD-ILD (9.4%), three were F-HP (3.5%), four were unclassified ILD (4.7%). The average recording time was 255.4 ± 78.1 d. The mean duration of follow-up was 18.0 months, ranged from 12 to 26 months. The mean age was 62.3 ± 8.3 years and 70 of the 85 (82.4%) patients were men. Among the 85 patients, 21 experienced AEs during follow-up. The predominant comorbidities were pulmonary hypertension (9.4%), lung cancer (4.7%), and gastrooesophageal reflux disease (4.7%). During the follow-up period, 25 (29.4) patients died. Kapla–Meier curves showed that patients with recorded AEs had a shorter median survival than those with non-recorded AEs (Fig. 3 ).
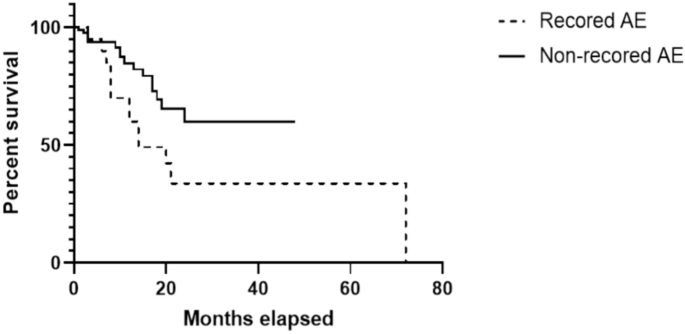
Kaplan–Meier curves for the survival according to recorded or without unrecorded AE (log-rank test, p < 0.05).
Patient satisfaction and use of the home monitoring application
Patients experiences with home monitoring application are presented in Table 2 . Overall, 82 out of the 85 patients (96.5%) measured symptoms (mMRC and COAT score), 70 out of 85 patients (82.4%) measured 1STST, 73 out of 85 patients (85.9%) recorded medicication use, and 44 out of 85 patients (52.9%) used the information library. Patient satisfaction with the home monitoring program was high. 65 out of 85 patients (76.5%) were satisfied with the application, 61 out of 85 patients (71.8%) found it easy to use, 69 out of 85 patients (81.2%) recommend it to others, and 67 out of 85 patients (78.8%) considered it easily accessible to the hospital.
Symptoms monitored in patients with F-ILDs
We examined symptom variations, including breathlessness and cough scores, and observed changes at baseline and during AE. We divided the disease progression into four phases: stable state, and 3, 2, and 1 week before the first recorded AE. COAT scores of the stable state and 3, 2, and 1 week before the first recorded AE were 6.0, 7.0, 10.0 and 12.0, respectively, and the differences were statistically significant ( p < 0.001). For COAT scores, there was no significant difference between the stable state and 3 weeks before the first recorded AE. However, there was a significant difference between the stable state and 2 weeks and the stable state and 1 week before the first recorded AE ( p < 0.001). Thus, patients had statistically high COAT scores from the stable state to 2 weeks before the first recorded AE. The variability of the COAT score increased by 4.4 ± 1.0 in the 2 weeks before the first recorded AE compared to the stable state. mMRC scores for the stable state and 3, 2 and 1 week before the the first recorded AE were 2.0, 2.0, 3.0 and 3.0, respectively and the differences were statistically significant ( p < 0.001). For mMRC scores, there was no significant difference between the stable state and 3 weeks before the first recorded AE. However, a significant difference was observed between the stable state and 2 weeks ( p = 0.005), and the stable state and 1 week ( p < 0.001) before the first recorded AE. The variability of the mMRC score increased by 0.9 ± 0.2 2 weeks before the first recorded AE compared to the stable state. Thus, these symptom indicators indicate that the patients exhibited statistically and clinically elevated COAT and mMRC scores 2 weeks before the first recorded AE. Table 3 and Fig. 4 compare the telemonitored symptom parameters, while Table 4 shows the variations in in these parameters.
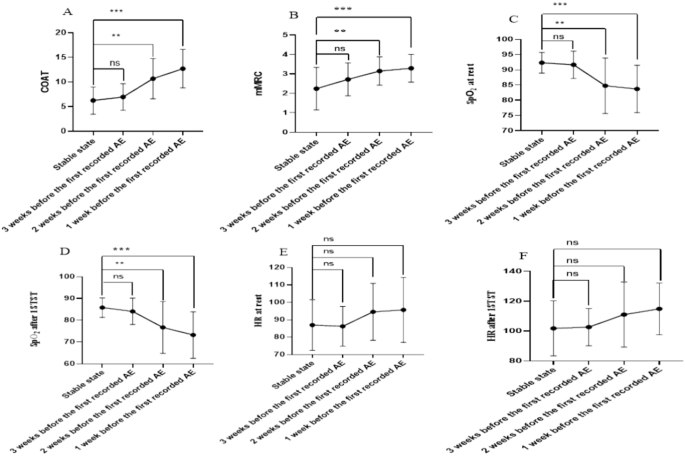
Comparison of telemonitoring symptoms and physiological parameters. ( A ) Comparison of COAT during the four phases of disease progression. ( B ) Comparison of mMRC scores during the four phases of disease progression. ( C ) Comparison of SpO 2 at rest during the four phases of disease progression. ( D ) Comparison of SpO 2 after 1STST during the four phases of disease progression. ( E ) Comparison of HR at rest during the four phases of disease progression course. ( F ) Comparison of HR after the 1STST during the four phases of disease progression course. ** p < 0.01, *** p < 0.001, ns P > 0.05.
Physiological indicator monitoring in patients with F-ILD
Subsequently, we observed change of SpO 2 and HR at rest and after 1STST during the four disease progression phases. The SpO 2 at rest in these phases were 92.3%, 91.7%, 86.4% and 83.7%, respectively ( p < 0.001). For SpO 2 at rest, there was no significant difference between the stable state and 3 weeks before the first recorded AE; however, significant differences were observed between the stable state and 2 weeks ( p = 0.002), and the stable state and 1 week ( p < 0.001) before the first recorded AE. Thus, patients exhibited statistically decreased SpO 2 at rest from 2 weeks before the first recorded AE. The variability of SpO 2 at rest decreased by −6.0% ± 1.7 at 2 weeks before the first recorded AE compared to the stable state. The SpO 2 after 1STST of the four phases was 85.8%, 84.1%, 76.7% and 73.2%, respectively. For SpO 2 after 1STST, there was no significant difference between the stable state and 3 weeks before the first recorded AE. However, significant differences were observed between the stable state and 2 weeks ( p = 0.007) and between the stable state and 1 week ( p < 0.001) before the first recorded AE. Hence, patients had significantly decreased SpO 2 after 1STST 2 weeks before the first recorded AE. The variability of SpO 2 after 1STST decreased by −9.1%±2.3 at 2 weeks before the first recorded AE compared to the stable state. There was no significant difference in HR at rest and after 1STST between the four phases of disease progression. Table 3 and Fig. 4 compare the telemonitored physiological parameters, while Table 4 shows their variations.
Monitoring symptoms and physiological indicators for prediction of the onset of AE
Next, we identified the best-monitored symptoms and physiological indicators for predicting AE onset in patients with F-ILDs. We used changes in COAT scores, mMRC scores, and SpO 2 to test the probability of the AE occurrence in patients with F-ILDs as nodes through the ROC curve, which are presented in Table 5 . The best cut-off value for the change in the COAT score was 4.0 (sensitivity: 52.4%, specificity: 94.1%), with an area under the curve (AUC) of 0.773. The best cut-off value for the change in mMRC score was 1.0 (sensitivity: 66.7%, specificity: 52.9%), with an AUC of 0.592; The best cut-off value for the change in SpO 2 at rest was −5.0 (sensitivity: 88.2%, specificity: 71.4%), with an AUC of 0.881; The best cut-off value for the change in SpO 2 after 1STST was −4.0 (sensitivity: 64.7%, specificity: 61.9%), with an AUC of 0.633. Notably, a combination of parameters showing changes in COAT score (≥ 4), mMRC score (≥ 1), SpO 2 at rest (≥ −5), and SpO 2 after 1STST (≥ −4) was the best indicator for predicting AE occurrence in patients with F-ILDs 2 weeks before the first recorded AE (AUC = 0.854). This combination demonstrated sensitivity and specificity of 81.4% and 88.2%, respectively.
The widespread use of smartphones and the internet has facilitated the home monitoring of heterogeneous group of F-ILDs, which primarily affect the lung parenchyma, causing dyspnea and often resulting in high mortality 25 . Crucial health changes can be detected using bedside monitors, which provide vital data noninvasively. Consequently, home monitoring has been recommended for the early detection of AEs in lung diseases, such as COPD. A similar technology may offer an early and and effective signal that could aid in distinguishing AE in patients with ILD 16 . However, the usefulness of measuring symptoms and physiological variables to detect AE in patients with F-ILDs remains unclear. We conducted this pilot study to assess the efficacy of home monitoring symptoms and variation in physiological parameters in predicting the onset of AE in patients with F-ILDs. Our results revealed high patient satisfaction and successful application of the home monitoring program. This approach can be readily integrated into home monitoring devices, providing alerts to physicians about patients at risk of experiencing AE. To our knowledge, this is the first study of such a home monitoring approach for predicting patients with F-ILDs.
Patients experiencing AE undergo a rapid decline in lung function, leading to poor quality of life, decreased physical activity and increased mortality 2 . Consequently, AE imposes a substantial burden on health-care costs, emphasizing the importance of early identification. AE may be differentiated from variations in the symptoms and physiological parameters that characterize F-ILDs 7 . Our findings revealed that median survival was shorter in patients with F-ILDs and AE than in those without AE. Symptoms of particular concern in patients with F-ILDs, such as breathlessness and cough, have been previously overlooked but are now gaining increased attention 10 , 26 . We utilized the mMRC and COAT questionnaires to assess breathlessness and cough, respectively. We observed a significant increase in COAT and a decrease in mMRC 2 weeks before the first recorded AE in patients with F-ILDs. A Japanese study reported that SpO 2 could predict disease prognosis in patients with IPF. SpO 2 measurements using a pulse oximeter are widely used to evaluate oxygen saturation and can be estimated rapidly and noninvasively 27 . For patients with idiopathic interstitial pneumonia (IIP), oxygen desaturation during the 6MWT is a strong predictor of mortality 28 . However, the 6MWT is time-consuming and requires a 30 m corridor, which is rare in healthcare settings. Conversely, the 1STST requires only a chair and can be efficiently conducted quickly, making it feasible in healthcare settings. Oishi et al. 15 found that nadir desaturation during the 1STST correlated with nadir desaturation during 6MWT in patients with ILDs. Fedi et al. 24 suggested that 1STSTs may be valuable for evaluating displacement and exercise-induced changes in SpO 2 in patients with IPF. Therefore, we selected the 1STST as an alternative to the 6MWT to assess patients' SpO 2 , and HR. Furthermore, our findings revealed that before and after 1STST, the mean value of SpO 2 significantly decrease 2 weeks before the first recorded AE. These findings corroborate the hypothesis that monitoring symptoms (including breathlessness and cough), and SpO 2 (at rest and after 1STST) in patients with F-ILDs may facilitate the early detection of AE.
Furthermore, our findings indicated that a combination of variables, including an increase in COAT (≥ 4) and mMRC (≥ 1) scores and, a decrease in SpO 2 at rest (≥ 5%), and after 1STST (≥ 4%) yielded the highest predictive value for AE onset in patients with F-ILDs 2 weeks before the first recorded AE (AUC = 0.854). Ultimately, SpO 2 is cost-efficient and reliable parameter, while symptom monitoring can aid in predict the AE of F-ILDs.
Our study has several strengths and numerous potential limitations that warrant acknowledgment. First the study was conducted at a single center study and small smaple size. Second, An inherent bias was present due to comorbidities, notably, the predominant comorbidities in this study included pulmonary hypertension (9.4%), lung cancer (4.7%), and gastrooesophageal reflux disease (4.7%), which could potentially impact the validity and reliability of the monitoring parameters results. Third, a latent safety risk is associated with participants conducting the 1STST at home. To mitigate this, we designed warning monitoring and feedback from healthcare providers to address any potential events. Furthermore, home oxygen therapy was recommended for patients with a SpO 2 < 88%. Fourth, our pilot study could not yield the highest evidence level, so a randomized controlled trial should be conducted in further studies.
In summary, this study is the first to provide data on weekly variations in symptoms and physiological parameters in patients with stable F-ILDs. We further outlined how this information could facilitate the confirmation of AE onset in these patients.
Data availability
The data that supporting the findings of this study are available upon reasonable request from the corresponding author.
Wijsenbeek, M. & Cottin, V. Spectrum of fibrotic lung diseases. N. Engl. J. Med. 383 (10), 958–968 (2020).
Article PubMed Google Scholar
Suzuki, A. et al. Acute exacerbations of fibrotic interstitial lung diseases. Respirology 25 (5), 525–534 (2020).
Kim, D. S. et al. Acute exacerbation of idiopathic pulmonary fibrosis: Frequency and clinical features. Eur. Respir. J. 27 , 143–150 (2006).
Song, J. W., Hong, S. B., Lim, C. M., Koh, Y. & Kim, D. S. Acute exacerbation of idiopathic pulmonary fibrosis: Incidence, risk factors and outcome. Eur. Respir. J. 37 , 356–363 (2011).
Suda, T. et al. Acute exacerbation of interstitial pneumonia associated with collagen vascular diseases. Respir. Med. 103 , 846–853 (2009).
Article PubMed PubMed Central Google Scholar
Oda, K. et al. Autopsy analyses in acute exacerbation of idiopathic pulmonary fibrosis. Respir. Res. 15 , 109 (2014).
Biondini, D. et al. Acute exacerbations of idiopathic pulmonary fibrosis (AE-IPF): An overview of current and future therapeutic strategies. Expert Rev. Respir. Med. 14 (4), 405–414 (2020).
Ryerson, C. J. et al. Cough predicts prognosis in idiopathic pulmonary fibrosis. Respirology 16 (6), 969–975 (2011).
Ley, B., Bradford, W. Z. & Vittinghoff, E. Predictors of mortality poorly predict common measures of disease progression in idiopathic pulmonary fibrosis. Am. J. Respir. Crit. Care Med. 194 (6), 711–718 (2016).
Kreuter, M. et al. Palliative care in interstitial lung disease: Living well. Lancet Respir. Med. 5 (12), 968–980 (2017).
Marillier, M. et al. Influence of exertional hypoxemia on cerebral oxygenation in fibrotic interstitial lung disease. Respir. Physiol. Neurobiol. 285 , 103601 (2021).
Eaton, T., Young, P., Milne, D. & Wells, A. U. Six-minute walk, maximal exercise tests: Reproducibility in fibrotic interstitial pneumonia. Am. J. Respir. Crit. Care Med. 171 (10), 1150–1157 (2005).
Kondoh, Y. et al. Disease severity staging system for idiopathic pulmonary fibrosis in Japan. Respirology 22 (8), 1609–1614 (2017).
Raghu, G. et al. An official ATS/ERS/JRS/ALAT statement: Idiopathic pulmonary fibrosis: Evidence-based guidelines for diagnosis and management. Am. J. Respir. Crit. Care Med. 183 (6), 788–824 (2011).
Oishi, K. et al. The 1-min sit-to-stand test to detect desaturation during 6-min walk test in interstitial lung disease. NPJ Prim. Care Respir. Med. 32 (1), 5 (2022).
Althobiani, M. A. et al. Home monitoring of physiology and symptoms to detect interstitial lung disease exacerbations and progression: A systematic review. ERJ Open Res. 7 (4), 00441–02021 (2021).
Moor, C. C. et al. A home monitoring program including real-time wireless home spirometry in idiopathic pulmonary fibrosis: A pilot study on experiences and barriers. Respir. Res. 19 , 105 (2018).
Marcoux, V. et al. Mobile health monitoring in patients with idiopathic pulmonary fibrosis. Ann. Am. Thorac. Soc. 16 (10), 1327–1329 (2019).
Moor, C. C. et al. Home monitoring in patients with idiopathic pulmonary fibrosis: A randomized controlled trial. Am. J. Respir. Crit. Care Med. 202 (3), 393–401 (2020).
Collard, H. R. et al. Acute exacerbation of idiopathic pulmonary fibrosis. An international working group report. Am. J. Respir. Crit. Care Med. 194 (3), 265–275 (2016).
Deng, N. et al. A home-based pulmonary rehabilitation mHealth system to enhance the exercise capacity of patients with COPD: Development and evaluation. BMC Med. Inform. Decis. Mak. 21 (1), 325 (2021).
Nishiyama, O. et al. A simple assessment of dyspnoea as a prognostic indicator in idiopathic pulmonary fibrosis. Eur. Respir. J. 36 (5), 1067–1072 (2010).
Koo, H. K. et al. Development and validation of the COugh assessment test (COAT). Respirology 24 (6), 551–557 (2019).
Fedi, A. et al. Concurrence of 1- and 3-min sit-to-stand tests with the 6-min walk test in idiopathic pulmonary fibrosis. Respiration 100 (7), 571–579 (2021).
Wijsenbeek, M. S. et al. Home monitoring in interstitial lung diseases. Lancet Respir. Med. 11 (1), 97–110 (2023).
Carvajalino, S., Reigada, C., Johnson, M. J., Dzingina, M. & Bajwah, S. Symptom prevalence of patients with fibrotic interstitial lung disease: A systematic literature review. BMC Pulm. Med. 18 (1), 78 (2018).
Takei, R. et al. Pulse oximetry saturation can predict prognosis of idiopathic pulmonary fibrosis. Respir. Investig. 58 , 190–195 (2020).
Lama, V. N. et al. Prognostic value of desaturation during a 6-min walk test in idiopathic interstitial pneumonia. Am. J. Respir. Crit. Care Med. 168 , 1084–1090 (2003).
Download references
Acknowledgements
The authors thank Xiaoming Liu for invaluable scientific feedback on the manuscript.
This work was supported by grants from the National Natural Science Foundation of China (No. 81760004; 82060013), the Natural Science Foundation of Ningxia Hui Autonomous Region (No. 2020AAC02001; 2020AAC03404), and the Key Research and Development Program of Ningxia Hui Autonomous Region (No. 2018BEG03035; 2023BEG02021).
Author information
Authors and affiliations.
Department of Key Laboratory of Ningxia Stem Cell and Regenerative Medicine, Institute of Medical Sciences, General Hospital of Ningxia Medical University, Yinchuan, 750004, Ningxia, People’s Republic of China
Hongyan Fu, Zhengyu Hu, Tingting Zhao, Hongxia Xin & Juan Chen
Department of Pulmonary and Critical Care Medicine, General Hospital of Ningxia Medical University, Yinchuan, 750004, Ningxia, People’s Republic of China
Zhengyu Hu, Tingting Zhao, Hongxia Xin, Jia Hou, Yanjuan Yang, Yanan Zhang & Juan Chen
Department of Pulmonary and Critical Care Medicine, The Second Affiliated Hospital of Xi’an Jiaotong University, Xi’an, Shanxi, 710049, People’s Republic of China
Department of Critical Care Medicine, General Hospital of Ningxia Medical University, Yinchuan, 750004, Ningxia, People’s Republic of China
Zhaojun Wang
Guangzhou Institute of Respiratory Health and State Key Laboratory of Respiratory Disease and National Clinical Research Center for Respiratory Disease and National Center for Respiratory Medicine, The First Affiliated Hospital of Guangzhou Medical University, Guangzhou National Laboratory, Guangzhou, People’s Republic of China
Ministry of Education Key Laboratory of Biomedical Engineering, College of Biomedical Engineering and Instrument Science, Zhejiang University, Hangzhou, People’s Republic of China
Wangshu Jiang & Ning Deng
School of Public Health, Ningxia Medical University, Yinchuan, 750004, Ningxia, People’s Republic of China
Faxuan Wang
School of Ningxia Medical University, Yinchuan, 750004, Ningxia, People’s Republic of China
You can also search for this author in PubMed Google Scholar
Contributions
F.H.Y. and C.J. conceived the idea, designed the experiments, analyzed and interpreted the data, and approved the final version of the manuscript. W.Z.J. conceived the idea, performed the experiments, and drafted the main critically reviewed manuscript. H.Z.Y., W.F., H.J. and Z.Y.N. contributed to the interpretation of data. Z.T.T., X.H.X., J.W.S., W.F.X. and D.N. contributed to the drafting and revision of the manuscript.
Corresponding author
Correspondence to Juan Chen .
Ethics declarations
Competing interests.
The authors declare no conflict of interests. This manuscript has not been published previously and is not under consideration for publication elsewhere. All authors have approved the contents of this paper and agreed to the journal’s submission policies.
Ethics approval and consent to participants
This study was conducted in accordance with the Declaration of Helsinki. The study protocol was approved by the Human Research Ethics Committee of the General Hospital of Ningxia Medical University (KYLL-2021-456). Informed consent was obtained from all patients to collect and publishing the data.
Additional information
Publisher's note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Supplementary information., rights and permissions.
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/ .
Reprints and permissions
About this article
Cite this article.
Fu, H., Wang, Z., Hu, Z. et al. Pilot study of home-based monitoring for early prediction of acute exacerbations in patients with fibrosing interstitial lung diseases. Sci Rep 14 , 21101 (2024). https://doi.org/10.1038/s41598-024-71942-x
Download citation
Received : 02 October 2023
Accepted : 02 September 2024
Published : 10 September 2024
DOI : https://doi.org/10.1038/s41598-024-71942-x
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Fibrosing interstitial lung diseases
- Acute exacerbations
- Home monitoring
- Early detection
By submitting a comment you agree to abide by our Terms and Community Guidelines . If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.
Quick links
- Explore articles by subject
- Guide to authors
- Editorial policies
Sign up for the Nature Briefing newsletter — what matters in science, free to your inbox daily.
Advertisement
Evaluation of Dyspnea, Physical Activity, Muscle Strength, and Quality of Life in Frail Older Adults with COPD
- Original Paper
- Published: 07 September 2024
- Volume 6 , article number 95 , ( 2024 )
Cite this article

- Meral Sertel ORCID: orcid.org/0000-0002-7575-9762 1 ,
- İlayda Karabayir ORCID: orcid.org/0000-0003-0924-9614 1 ,
- Yasemin Köse ORCID: orcid.org/0000-0001-7532-7524 1 ,
- Döndü Nur Keskin ORCID: orcid.org/0000-0001-6624-5295 1 ,
- Selma Demir ORCID: orcid.org/0000-0001-8205-0586 2 &
- Eylem Tütün Yümin ORCID: orcid.org/0000-0002-6994-9391 3
Explore all metrics
This study aimed to assess dyspnea, physical activity, muscle strength, and health-related quality of life in older adults diagnosed with chronic obstructive pulmonary disease (COPD) who are also considered frail. The study included volunteers aged 65 and over, diagnosed with COPD according to GOLD criteria. Individuals with COPD were divided into two groups according to the FRAIL Frailty Scale: frail ( n = 32) and non-frail ( n = 30). At the assessment stage, various tools were used to evaluate different aspects for all individuals, including respiratory function test for assessing respiratory functions, Modified Medical Research Council Dyspnea Scale (MMRC) for evaluating dyspnea, Saint George’s Respiratory Questionnaire (SGRQ) for assessing quality of life, FRAIL Frailty Scale and PRISMA-7 Frailty Scale for detecting frailty, Physical Activity Scale for Elderly (PASE) for evaluating physical activity, digital hand dynamometer for assessing quadriceps femoris muscle strength, and Jamar hand dynamometer for evaluating hand strength. Comparing the results of the Respiratory Function Test, SGRQ, PASE scores, and quadriceps femoris and handgrip strengths of frail and non-frail older adults with COPD was similar ( p > 0.05), while frail and non-frail older adults with COPD showed statistical differences in the MMRC scores results ( p < 0.05). MMRC score was worse in the frail group. Early diagnosis of COPD in frail older adults is very important for the health and quality of life of the patients. In order to prevent deterioration in frail COPD patients, both pharmacological and rehabilitative treatment methods should be started early.
Clinical trial number: NCT05811832.
This is a preview of subscription content, log in via an institution to check access.
Access this article
Subscribe and save.
- Get 10 units per month
- Download Article/Chapter or eBook
- 1 Unit = 1 Article or 1 Chapter
- Cancel anytime
Price includes VAT (Russian Federation)
Instant access to the full article PDF.
Rent this article via DeepDyve
Institutional subscriptions

Similar content being viewed by others

Daily living activities, exercise capacity, cognition, and balance in COPD patients with and without frailty
Prevalence and clinical characteristics of Sarcopenia in older adult patients with stable chronic obstructive pulmonary disease: a cross-sectional and follow-up study

Physical frailty characteristics have a differential impact on symptoms as measured by the CAT score: an observational study
Data availability.
Data will be made available on request. The data that has been used is confidential.
Code Availability
Not applicable.
Abbreviations
Chronic obstructive pulmonary disease
Forced expiratory volume in the 1st second
FEV1/FVC ratio
Forced expiratory flow at 25–75%
Modified Medical Research Council Dyspnea Scale
Saint George Respiratory Questionnaire
Physical Activity Scale for the Elderly
Body mass ındex
Forced vital capacity
Peak expiratory flow
Standard deviation.
Global Initiative for Chronic Obstructive Lung Disease. Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease (2017 Report). Available From: https://goldcopd.org/ . Accessed 02.08.2024.
GBD 2015 Mortality and Causes of Death Collaborators. Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980–2015: a systematic analysis for the Global Burden of Disease study 2015. The Lancet (London, England). 2016;388:1459–544. https://doi.org/10.1016/S0140-6736(16)31012-1 .
Article Google Scholar
Temiz Hava Hakkı Platformu, 2018; Kocabaş A. And et al. Türkiye Kronik Hava Yolu Hastalıkları Önleme ve Kontrol Programı 2014;2018–2023. Ankara. Available From: chrome-extension://efaidnbmnnnibpcajpcglclefindmkaj/ https://hsgm.saglik.gov.tr/depo/birimler/kronik-hastaliklar-ve-yasli-sagligi-db/Dokumanlar/Kitaplar/Turkiye_Kronik_Hava_Yolu_Hastaliklari_Onleme_ve_Kontrol_Programi_2018-2023.pdf . Accessed 02.08.2024.
GBD 2017 Causes of Death Collaborators. Global, regional, and national age-sex-specific mortality for 282 causes of death in;195 countries and territories, 1980-2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet. 2018;392:1736.
Global strategy for the diagnosis, management, and prevention of chornic obstructive pulmonary disease 2020 Report.
Man WD-C, Kemp P, Moxham J, et al. Exercise and muscle dysfunction in COPD: implications for pulmonary rehabilitation. Clin Sci (Lond). 2009;117(8):281–91.
Kapucu S, Ünver G. Kırılgan Yaşlı ve Hemşirelik Bakımı/Frail Elderly and Nursing Care. Osmangazi Tıp Dergisi. 2017;39(1):122–9.
Google Scholar
Clegg A, Young J, Iliffe S, et al. Frailty in elderly people. Lancet. 2013;381(9868):752–62.
Article PubMed Google Scholar
Lahousse L, Ziere G, Verlinden VJ, et al. Risk of frailty in elderly with COPD: a population-based study. J Gerontol Series A: Biomed Sci Med Sci. 2016;71(5):689–95.
Article CAS Google Scholar
Park SK, Richardson CR, Holleman RG, et al. Frailty in people with COPD, using the National Health and Nutrition Evaluation Survey dataset (2003–2006). Heart Lung. 2013;42(3):163–70.
Article PubMed PubMed Central Google Scholar
Akın S, Mazıcıoglu MM, Mucuk S, et al. The prevalence of frailty and related factors in community-dwelling Turkish elderly according to modified Fried Frailty Index and FRAIL scales. Aging Clin Exp Res. 2015;27(5):703–9.
Bousquet J, Dinh-Xuan A, Similowski T, et al. Should we use gait speed in COPD, FEV1 in frailty and dyspnoea in both? Eur Respir J. 2016;48(2):315.
Article PubMed CAS Google Scholar
Ierodiakonou D, Kampouraki M, Poulonirakis I, et al. Determinants of frailty in primary care patients with COPD: the Greek UNLOCK study. BMC Pulm Med. 2019;19(1):1–9.
Miller MR, Crapo R, Hankinson J, et al. General considerations for lung function testing. Eur Respir J. 2005;26(1):153–61.
Stenton C. The MRC breathlessness scale. Occup Med. 2008;58(3):226–7.
Bestall J, Paul E, Garrod R, et al. Usefulness of the Medical Research Council (MRC) dyspnoea scale as a measure of disability in patients with chronic obstructive pulmonary disease. Thorax. 1999;54(7):581–6.
Article PubMed PubMed Central CAS Google Scholar
Raîche M, Hébert R, Dubois MF, et al. User guide for the PRISMA-7 questionnaire to identify elderly people with severe loss of autonomy. In Integrated service delivery to ensure persons' functional autonomy, ed. R. Hébert, A. Tourigny, and M. Gagnon, 147- 65. Quebec: Edisem. https://doi.org/10.19082/7266 .
Jones PW. Health status measurement in chronic obstructive pulmonary disease. Thorax. 2001;56(11):880–7.
Morley JE, Malmstrom TK, Miller DK. A simple frailty questionnaire (FRAIL) predicts outcomes in middle aged African Americans. J Nutr Health Aging. 2012;16(7):601–8.
Jung HW, Yoo HJ, Park SY, Kim SW, et al. The Korean version of the FRAIL scale: clinical feasibility and validity of assessing the frailty status of Korean elderly. Korean J Intern Med. 2016;31(3):594–600.
de Leon Diaz, Gonzalez E, Gutierrez Hermosillo H, Martinez Beltran JA, et al. Validation of the FRAIL scale in Mexican elderly: results from the Mexican Health and Aging Study. Aging Clin Exp Res. 2016;28(5):901–8.
Dong L, Qiao X, Tian X, et al. Cross-cultural adaptation and validation of the FRAIL scale in Chinese community-dwelling older adults. J Am Med Dir Assoc. 2017;18(2):301–7.
Gardiner PA, Mishra GD, Dobson AJ. Validity and responsiveness of the FRAIL scale in a longitudinal cohort study of older Australian women. J Am Med Dir Assoc. 2015;16(9):781–3.
Hymabaccus Muradi BAB. Yaşlılarda Kırılganlığı Ölçmeye Yönelik FRAİL Ölçeğinin Türkçe Geçerlik ve Güvenirlik Çalışması. Master Thesis, Ankara, 2017. http://hdl.handle.net/11655/4102 .
Ayvat E, Kılınc M, Kırdi N. The Turkish version of the Physical Activity Scale for the Elderly (PASE): its cultural adaptation, validation, and reliability. Turk J Med Sci. 2017;47(3):908–15.
Leung AS, Chan KK, Sykes K, et al. Reliability, validity, and responsiveness of a 2-min walk test to assess exercise capacity of COPD patients. Chest. 2006;130(1):119–25. https://doi.org/10.1378/chest.130.1.119 .
Şahin F, Büyükavcı R, Sağ, S. et al. Berg Denge Ölçeği'nin Türkçe Versiyonunun &# 304; nmeli Hastalarda Geçerlilik ve Güvenilirliği. Journal of Physical Medicine & Rehabilitation Sciences/Fiziksel Tup ve Rehabilitasyon Bilimleri Dergisi. 2013;16(3).
Kesilmiş İ, Manolya A. Can quadriceps and hamstring muscle strenght effect on dynamic balance performance? The Journal of Turkish Sport Sciences. 2020;3(1):1–7.
Puhan MA, Siebeling L, Zoller M, et al. Simple functional performance tests and mortality in COPD. Eur Respir J. 2013;42:956–63.
Spruit MA, Sillen MJ, Groenen MT, et al. New normative values for handgrip strength: Results from the UK Biobank. J Am Med Dir Assoc. 2013;14:e5-11.
Jones PW, Quirk FH, Baveystock CM. The St George & Respiratory Questionnaire. Respir Med. 1991;85(25–31):3–7.
Brooks SMC. Task group on surveillance for respiratory hazards in the occupational setting. Surveill Respir Hazards ATS News. 1982;126:952–6.
Polatli M, Yorgancioglu A, Aydem İÖ, Yilmaz Demirci N, et al. Validity and reliability of Turkish version of St. George’s Respir Questionnaire Tuberkuloz ve Toraks. 2013;61(2):81–7.
Mathiowetz V, Kashman N, Volland G, et al. Grip and pinch strength: Normative data for adults. Arch Phys Med Rehabil. 1985;66:69–74.
PubMed CAS Google Scholar
Dias, LDS, Ferreira, ACG, da Silva Junior, JLR, et al. KOAH hastalarında kırılganlık prevalansı ve ilişkili değişkenlerin değerlendirilmesi. Uluslararası Kronik Obstrüktif Akciğer Hastalığı Dergisi . 2020;1349–1356.
Park SK, Richardson CR, Holleman RG, et al. Ulusal sağlık ve beslenme değerlendirme araştırması veri setini kullanarak KOAH’lı kişilerde fiziksel aktivite (2003–2006). Lung J Akut Krit Bakımını duyun. 2013;42(4):235–40. https://doi.org/10.1016/j.hrtlng.2013.04.005 .
Çakıcı M, Meti ZG. Kronik Obstrüktif Akciğer Hastalığı Olan Geriatrik Bireylerde Dispne, Bakım Bağımlılığı ve Kırılganlık Arasındaki Etkileşim. İzmir Göğüs Hastanesi Dergisi. 2020;34(3):95–104.
Hanlon P, Guo X, McGhee E, et al. KOAH’ta kırılganlığın prevalansı, gidişatı ve klinik sonuçlarının sistematik olarak gözden geçirilmesi ve meta-analizi. NPJ Birinci Basamak Solunum Tıbbı. 2023;3(1):1.
Kagiali S, İnal-İnce D, Çakmak A, et al. Kırılganlığı olan ve olmayan KOAH hastalarında günlük yaşam aktiviteleri, egzersiz kapasitesi, biliş ve denge. İrlanda Tıp Bilimleri Dergisi. 2022;191(2):817–24.
Keskin T, Başkurt Z. KOAH Tanılı Yaşlı Bireylerde Pulmoner Rehabilitasyon. Celal Bayar Üniversitesi Sağlık Bilimleri Enstitüsü Dergisi. 2021;81:157–61.
Langlois F, Vu TT, Chasse K, et al. Benefits of physical exercise training on cognition and quality of life in frail older adults. J Gerontol Ser B: Psychol Sci. 2013;68(3):400–4.
Gökçek, Ö., Doğru Hüzmeli, E., & Katayıfçı, N. Kronik obstrüktif akciğer hastalarında dispnenin yaşam kalitesi ve depresyona etkisi, 2019;1:84-88
Fiatarone MA, O’Neill EF, Ryan ND, et al. Exercise training and nutritional supplementation for physical frailty in very elderly people. N Engl J Med. 1994;330(25):1769–75.
da Silva VD, Tribess S, Meneguci J, et al. Association between frailty and the combination of physical activity level and sedentary behavior in older adults. BMC Public Health. 2019;19(1):1–6.
Baş KG. Yaşlılarda fiziksel aktivitenin kırılganlık düzeyi ile ilişkisinin incelenmesi (Master's thesis, Hitit Üniversitesi. 2022.
Gephine S, Mucci P, Grosbois JM, et al. Kronik solunum yetmezliği olan KOAH hastalarında fiziksel kırılganlık. Uluslararası Kronik Obstrüktif Akciğer Hastalığı Dergisi. 2021;1381–1392.
Pegorari MS, Tavares DMdS. Factors associated with the frailty syndrome in older adults living in the urban area. Revista latino-americana de enfermagem. 2014;22(5):874–82.
Ierodiakonou D, Kampouraki M, Poulonirakis I, et al. Determinants of frailty in primary care patients with COPD: the Greek UNLOCK study. BMC Pulm Med. 2019;19:1–9.
Valenza MC, Torres-Sánchez I, Cabrera-Martos I, et al. Physical activity as a predictor of absence of frailty in subjects with stable COPD and COPD exacerbation. Respir Care. 2016;61(2):212–9.
Ulusoy S. KOAH’ta kırılganlık düzeyinin denge, kognisyon ve günlük yaşam aktiviteleri üzerine etkisi (Master's thesis, Sağlık Bilimleri Enstitüsü). Ankara. 2020. URL: https://acikbilim.yok.gov.tr/bitstream/handle/20.500.12812/488764/yokAcikBilim_10214550.pdf?sequence=-1&isAllowed=y .
Kemik AE, Hepgul N, Kon S, et al. Kronik solunum hastalığında sarkopeni ve kırılganlık. Chron Solunum Dis. 2017;14(1):85–99. https://doi.org/10.1177/147997231667966427923981 .
Chainani V, Shaharyar S, Dave K, et al. Kırılganlık sendromunun (el kavrama gücü ve yürüme hızı) ve kardiyovasküler mortalitenin nesnel ölçümleri: Sistematik bir inceleme. Int J Cardiol. 2016;215:487–93. https://doi.org/10.1016/j.ijcard.2016.04.068 .
Spositon T, Oliveira JM, Rodrigues A, et al. Quadriceps weakness associated with mortality in individuals with chronic obstructive pulmonary disease. Ann Phys Rehabil Med. 2022;65(5):101587. https://doi.org/10.1016/j.rehab.2021.101587 .
Jeong M, Kang HK, Song P, et al. Hand grip strength in patients with chronic obstructive pulmonary disease. Int J Chronic Obstructive Pulm Dis. 2017;12:2385–90.
Fonseca J, Machado FVC, Santin LC, et al. Handgrip strength as a reflection of general muscle strength in chronic obstructive pulmonary disease. COPD: J Chronic Obstructive Pulm Dis. 2021;18(3):299–306.
Pitta F, Troosters T, Spruit MA, et al. Characteristics of physical activities in daily life in chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2005;171:972–7.
Hopkinson NS, Nickol AH, Payne J, et al. Angiotensin converting enzyme genotype and strength in chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2004;170:395–9.
Spruit MA, Gosselink R, Troosters T, et al. Muscle force during an acute exacerbation in hospitalised patients with COPD and its relationship with CXCL8 and IGF-I. Thorax. 2003;58:752–6.
Bernabeu-Mora R, Oliveira-Sousa SL, Sa´nchez-Martinez MP, et al. Frailty transitions and associated clinical outcomesinpatients with stable COPD: a longitudinal study. Plos One. 2020. https://doi.org/10.1371/journal.pone.0230116 .
Miyamoto E, Kaneko M, Ichimaru S, et al. Upper extremıty muscle volume and functıon as ındıcators of pre-fraılty ın older adult patıents wıth chronıc obstructıve pulmonary dısease (COPD). J Aging Res Clin Practice. 2016;5(3):147–54.
Download references
Author information
Authors and affiliations.
Health Sciences Faculty Physiotherapy and Rehabilitation Department, Kırıkkale University, Kirikkale, Turkey, TR71450
Meral Sertel, İlayda Karabayir, Yasemin Köse & Döndü Nur Keskin
Department of Chest Diseases, Kırıkkale Yüksek İhtisas Hospital, Kirikkale, Turkey, TR71450
Selma Demir
Health Sciences Faculty Physiotherapy and Rehabilitation Department, Bolu Abant Izzet Baysal University, Bolu, Turkey, TR71450
Eylem Tütün Yümin
You can also search for this author in PubMed Google Scholar
Contributions
MS: substantial contributions to conception and design of the study and the article, data analysis and interpretation, drafting the article, final approval of the version to be published. İK: data analysis and interpretation, drafting the article. YK: data analysis and interpretation, drafting the article. DNK: data analysis and interpretation, drafting the article. SD: substantial contributions to conception and design of the study. ETY: revising the article critically for important intellectual content, final approval of the version to be published. All authors discussed the results and commented on the manuscript.
Corresponding author
Correspondence to Meral Sertel .
Ethics declarations
Ethical approval.
The study received approval and written consent from the Kırıkkale University Non-Interventional Research Ethics Committee (Dated 21.12.2022, numbered 2022/15, Decision number: 2022.12.06) for its execution and obtaining participants' written consent.
Consent to participate
All individuals declared consent before participating in the current study. They also state that the research reported in the paper was undertaken in compliance with the Helsinki Declaration and the International Principles governing research on people.
Consent for Publication
The authors transfer all copyright ownership of the manuscript to the journal. The copy right to this article is transferred SN Comprehensive Clinical Medicine. The effective if and when the article is accepted for publication. The copyright transfer covers the exclusive right to reproduce and distribute the article, including reprints, translations, photographic reproductions, microform, electronic form (offline, online) orany reproductions of similar nature.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Medicine
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
Reprints and permissions
About this article
Sertel, M., Karabayir, İ., Köse, Y. et al. Evaluation of Dyspnea, Physical Activity, Muscle Strength, and Quality of Life in Frail Older Adults with COPD. SN Compr. Clin. Med. 6 , 95 (2024). https://doi.org/10.1007/s42399-024-01723-0
Download citation
Accepted : 21 August 2024
Published : 07 September 2024
DOI : https://doi.org/10.1007/s42399-024-01723-0
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Physical activity
- Muscle strength
- Find a journal
- Publish with us
- Track your research
- Yaroslavl Tourism
- Yaroslavl Hotels
- Yaroslavl Bed and Breakfast
- Flights to Yaroslavl
- Yaroslavl Restaurants
- Things to Do in Yaroslavl
- Yaroslavl Travel Forum
- Yaroslavl Photos
- Yaroslavl Map
- All Yaroslavl Hotels
- Yaroslavl Hotel Deals
flying from moscow to usa - Yaroslavl Forum
- Europe
- Russia
- Central Russia
- Yaroslavl Oblast
- Yaroslavl
flying from moscow to usa
- United States Forums
- Europe Forums
- Canada Forums
- Asia Forums
- Central America Forums
- Africa Forums
- Caribbean Forums
- Mexico Forums
- South Pacific Forums
- South America Forums
- Middle East Forums
- Honeymoons and Romance
- Business Travel
- Train Travel
- Traveling With Disabilities
- Tripadvisor Support
- Solo Travel
- Bargain Travel
- Timeshares / Vacation Rentals
- Yaroslavl Oblast forums
- Yaroslavl forum

I met a girl online and she wants to come here but says after purchasing visa, passport, tickets, etc. she was told she still needs $1525 for a required insurance. any info on this would be greatly appriciated.
It is not true...
I am going to USA in December. I paid about $15 for medical insurance for two weeks. Any other insurances are not required.

This looks like a scam, and she is most probably a he. I hope you did not pay for "her" visa, passport, tickets, etc...
Thank you all. I it seems too good to be true...It usualy is.
This topic has been closed to new posts due to inactivity.
- Yaroslavl and Rostov in two days - too much? May 31, 2019
- Need a car and driver in Yaroslavl Oct 05, 2018
- Self Service Laundry May 29, 2018
- 6 Hours to travel in Yaroslavl Jan 28, 2018
- Yaroslavl Mar 30, 2017
- hire car and driver--Yaroslavl-Uglic-Rostov-Uglic Jan 28, 2016
- Distance between ISKCON Yaroslavl and state university yaros Jun 24, 2015
- shoping in Yaroslavl Aug 02, 2014
- hi guys im talking to a women from Sovetsk Mar 06, 2013
- Looking for my girlfriend from Yaroslavl Feb 24, 2013
- Anybody talking to this girl from Sovetsky? Feb 20, 2013
- apartment in yaroslavl Dec 02, 2012
- Stop-over between St Petersburg and Yaraslavl Dec 01, 2011
- train yaroslavl to novgorod Jul 03, 2011
- Train travel from Moscow to Yaroslavl 5 replies
- Apartments in Yaroslavl 2 replies
- can anyone help traveling from UK to Kirov 7 replies
- kirov to moscow flight? 2 replies
- Stop-over between St Petersburg and Yaraslavl 2 replies
- Meeting a Young Lady from Sovetsk, Kirov 22 replies
- Looking for my girlfriend from Yaroslavl 6 replies
- train yaroslavl to novgorod 5 replies
- hi guys im talking to a women from Sovetsk 4 replies
- Sovetsk (Kirov oblast) 3 replies
Yaroslavl Hotels and Places to Stay
- GreenLeaders

Yaroslavl', Yaroslavskaya oblast', RU Traffic Cameras
Yaroslavl State Medical University Russia 2024-25: Admission, Courses, Fees, Eligibility, Ranking etc.

Yaroslavl State Medical University (YSMU) is a public university in Yaroslavl, Russia. It was founded in 1944 and is a leading regional center of medical education and biomedical research. Yaroslavl State Medical University Russia is recognized by the World Health Organization (WHO) and the National Medical Commission (NMC) of India. Yaroslavl State Medical University Russia is known for its rigorous academic programs and high standards of education. It offers undergraduate, graduate, and postgraduate programs in various medical disciplines, including General Medicine, Dentistry, Pharmacy, and Nursing. The curriculum is designed to meet international standards and is regularly updated to incorporate the latest advancements in medical science.
| Abroad University MBBS Application Form 2024 | |
|---|---|
| Manipal Pokhara College of Medical Science, Pokhara, Nepal | |
| Kursk State Medical University, Russia | |
| Grigol Robakidze University, Georgia | |
Yaroslavl State Medical University is a highly regarded medical university, and its graduates are in high demand around the world. Throughout this article, we provide information about Yaroslavl State Medical University, such as Admission procedure, Courses, Fee structure, living cost, MBBS Syllabus, Eligibility Criteria and advantages & disadvantages of studying MBBS in Russia and more.
College Summary
Before we go through Yaroslavl State Medical University detailed information, Let’s look at the college’s essential details.
| Yaroslavl State Medical University Russia | |
| YSMU Russia | |
| Yaroslavl, Russia | |
| 1944 | |
| Public | |
| English & Russian | |
| , | |
| Ministry of Health of the Russian Federation | |
| MBBS | |
| USD- $ 4450 (Per-Annual) INR- Rs. 3,56,000 (Per-Annual) | |
| Country- 186 World- 6505 ( : EduRank ) | |
| September Intake | |
| Yes (Male & Female) | |
| https://ysmu.ru/ |
Affiliation and Recognition
- World Health Organization (WHO)
- National Medical Commission (NMC)
- Ministry of Science and Higher Education of the Russian Federation
Yaroslavl State Medical University Russia Student Support
The Yaroslavl Medical University Student Support are:-
| Anti Ragging | Counselling Services |
| Healthcare Services | Hostel |
| Report | Query |
| Local Language Learning Classes | NMC Screening Test Help Centre |
Yaroslavl State Medical University Russia Courses Offered
Yaroslavl State University Russia Courses offer quality medical programs under highly qualified faculty and state-of-the-art infrastructure. The College is famous for its undergraduate medical programs ( MBBS ).
| MBBS | 6 Years (English Medium) 7 Years (Russian Medium) |
Why study MBBS at Yaroslavl State Medical University in Russia?
- Yaroslavl Medical University is the big regional centre of excellent medical education and biomedical research.
- Yaroslavl Medical University has highly skilled and well-experienced academic staff that provides world-class teaching to students.
- The University consists of a big library with two reading halls and facilities that are equipped in terms of the use of databases and Internet resources.
- Yaroslavl State Medical University has good social facilities and structures, such as a student healthcare centre, a garden of medical plants, sports centres, five hostels, and the Volga River summer camp.
- The staff of this university consists of foreign international societies, well-known scientists and clinicians from not only Russia but all over the world.
Yaroslavl State Medical University Russia Faculty & Staff
Yaroslavl State Medical University places a strong emphasis on research, and the faculty actively engages in cutting-edge research projects. Professors and researchers contribute to advancements in medical science, publishing research papers in reputed journals and participating in national and international conferences. These staff members handle admissions, student services, library services, and various administrative functions.

Yaroslavl State Medical University Russia Admission Procedure
If you want to take admission to Yaroslavl State Medical University Russia in 2024, you must qualify for the National Eligibility Entrance Exam (NEET) For Indian Students.
Yaroslavl State Medical University Russia Eligibility Criteria
If you too want to study MBBS at Yaroslavl State University Russia, check the eligibility below.
| Your age should be at least 17 years old on or before 31st December of the admission year. *No Upper Age Limit. | |
| Class 12th in Science, with PCB and English subjects from a board recognized by the authorities in India. | |
| 60% in 10+2 (UR) 50% (SC/OBC/ST) | |
| (For Indian Students) | |
| Not Required |
Yaroslavl State Medical University Russia Documents Required
Before taking admission at Yaroslavl State Medical University Russia, please do not forget to carry all these related documents.
- Passport (Minimum 18 months validity).
- 10th Certificate & Mark sheet.
- 12th Certificate & Mark sheet.
- Birth Certificate.
- 10 passport-size Photographs
- Official Invitation letter from the Medical University of Russia.
- Authorization of all documents from the Ministry of External Affairs, New Delhi.
- Legalization of all documents from the Russian Embassy.
- Bank receipt of 1st Year of Yaroslavl State Medical University Tuition fee (required for some Universities).
- HIV test documents.
Yaroslavl State Medical University Russia Fee Structure 2024-25
The Yaroslavl State Medical University MBBS fee structure is mentioned below in this section.
| Tuition Fee | $4000 | $4000 | $4000 | $4000 | $4000 | $4000 |
| Hostel Fee | $ 350 | $ 350 | $ 350 | $ 350 | $ 350 | $ 350 |
| Medical + Insurance + Registration Fee | $100 | $100 | $100 | $100 | $100 | $100 |
| Total (USD) | $4450 | $4450 | $4450 | $4450 | $4450 | $4450 |
| Fees in Indian Rupees | Rs. 3,56,000 | Rs. 3,56,000 | Rs. 3,56,000 | Rs. 3,56,000 | Rs. 3,56,000 | Rs. 3,56,000 |
Yaroslavl State Medical University Russia Ranking 2024-25
According to Edurank, the Yaroslavl State Medical University ranking in Russia and all over the world:
| Yaroslavl State Medical University Country Rank | 186 |
| Yaroslavl State Medical University World Rank | 6505 |
Yaroslavl State Medical University Russia MBBS Syllabus in Russia
Before applying for Yaroslavl Medical University Russia, please compare the MBBS Syllabus of some of Russia’s top-ranked, NMC-approved medical universities.
| 1st Semester | First aid in the pre-hospital phase, Medical physics and mathematics, Medical Chemistry, Basic Bioorganic Chemistry, Medical Economics, History of Russia, Latin Language, Anatomy, Medical Biology, Russian Language. |
| 2nd Semester | Anatomy, Latin language, Medical Biology, Medical informatics, Jurisprudence, Mineral Metabolism, History of Medicine, Psychology and Pedagogy, Histology, Embryology, Cytology. |
| 3rd Semester | Anatomy, History of Medicine, Psychology and Pedagogy, Bioethics, Clinical Physiology, Microbiology and Virology, Hygiene, Propaedeutics of internal Diseases and radiodiagnosis, Life safety and disaster medicine Russian Language. |
| 4th Semester | Philosophy, Biochemistry, Histology, Embryology, Cytology, Anatomy of systems of neuroimmunoendocrinology, Histophysiology of digestive systems, and Information technology in medicine, Philosophy and Biochemistry. |
About Russia
Russia is a country spanning Eastern Europe and Northern Asia. It is the largest country in the world by area, extending across eleven time zones, and shares land boundaries with fourteen countries. Russia is a major economic power with a large and diversified economy. It is the world’s largest exporter of oil and natural gas. Russia also has a significant manufacturing sector and a growing services sector. Russia is a popular tourist destination, with many attractions, such as the Red Square in Moscow, the Hermitage Museum in St. Petersburg, and the Lake Baikal in Siberia.
Contact Details
Yaroslavl State Medical University Russia Address: Revolyutsionnaya Ulitsa, 5, Yaroslavl, Yaroslavl Oblast, Russia, 150000 Official Website: https://ysmu.ru/
Frequently Asked Question(FAQ)
Where is yaroslavl state medical university russia located.
150000, Yaroslavl region, Yaroslavl, st. Revolutionary, 5.
What is the MBBS course duration at Yaroslavl State Medical University Russia?
The MBBS course duration at Yaroslavl State Medical University is 6 Years.
What is the language of teaching while studying MBBS at Yaroslavl State Medical University Russia?
The university provides the medical degree in English language for Indian students.
Carrier scope for Indian students after studying MBBS in Russia?
After completing their MBBS in Russia, candidates can work in any of the country’s private nursing facilities or hospitals.
Related Posts
- Akaki Tsereteli State University 2024-25: Admission, Courses, Fees, Ranking etc.
- Caucasus International University Georgia 2024-25: Admission, Course, Fees, Ranking etc.
- Tbilisi State Medical University 2024-25: Admission, Course, Fees, Ranking etc.
- Kutaisi Medical University Georgia 2024-25: Admission, Courses, Fees, Ranking etc.
About Rahul
Hi, I'm Rahul Kumar, with a year of expertise in MBBS and Ayush courses. I have detailed knowledge of various colleges' fee structures, cutoffs, and intake procedures. If you're looking for insights or assistance in pursuing MBBS or BAMS courses, feel free to comment below—I'm here to help!
Leave a Comment Cancel reply
Notify me via e-mail if anyone answers my comment.
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
Preview improvements coming to the PMC website in October 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- ERJ Open Res
- v.3(4); 2017 Oct

mMRC dyspnoea scale indicates impaired quality of life and increased pain in patients with idiopathic pulmonary fibrosis
Kaisa rajala.
1 Helsinki University Hospital, Comprehensive Cancer Center, Dept of Palliative Care, Helsinki, Finland
2 Faculty of Medicine, University of Helsinki, Helsinki, Finland
Juho T. Lehto
3 Dept of Oncology, Palliative Care Unit, Tampere University Hospital, Tampere, Finland
4 Faculty of Medicine and Life Sciences, University of Tampere, Tampere, Finland
Eva Sutinen
Hannu kautiainen.
5 Primary Health Care Unit, Kuopio University Hospital, Kuopio, Finland
6 Folkhälsan Research Center, Helsinki, Finland
Marjukka Myllärniemi
7 University of Helsinki and Helsinki University Hospital, Heart and Lung Center, Dept of Pulmonary Medicine, Helsinki, Finland
Tiina Saarto
Associated data.
J.T. Lehto 00084-2017_Lehto
M. Myllärniemi 00084-2017_Myllarniemi
K. Rajala 00084-2017_Rajala
E. Sutinen 00084-2017_Sutinen
This study was undertaken to investigate idiopathic pulmonary fibrosis (IPF) patients' health-related quality of life (HRQoL) and symptoms in a real-life cross-sectional study. Our secondary aim was to create a simple identification method for patients with increased need for palliative care by studying the relationship between modified Medical Research Council (mMRC) dyspnoea scale, HRQoL and symptoms.
We sent a self-rating HRQoL questionnaire (RAND-36) and modified Edmonton Symptom Assessment Scale (ESAS) to 300 IPF patients; 84% of the patients responded to these questionnaires.
The most prevalent (>80%) symptoms were tiredness, breathlessness, cough and pain in movement. An increasing mMRC score showed a linear relationship (p<0.001) to impaired HRQoL in all dimensions of RAND-36 and the severity of all symptoms in ESAS. Dimensions of RAND-36 fell below general population reference values in patients with mMRC score ≥2. The intensity of pain in movement (p<0.001) and at rest (p=0.041), and the prevalence of chest pain (p<0.001) had a positive linear relationship to increased mMRC score.
An increasing mMRC score reflects impaired HRQoL and a high symptom burden. In clinical practice, the mMRC scale could be used for screening and identification of IPF patients with increased need for palliative care.
Short abstract
mMRC indicates impaired HRQoL and pain in IPF http://ow.ly/oRB430gIW7U
Introduction
Idiopathic pulmonary fibrosis (IPF) is a chronic, progressive and severe disease of unknown cause, seen primarily in older adults [ 1 ]. Even with recent advances in pharmacological treatment, IPF is still a disease with a high morbidity and poor survival [ 2 – 4 ]. As the disease trajectory in IPF is comparable to many advanced malignant disorders, guidelines recommend early-integrated palliative care in addition to pharmacological treatment and referral for lung transplantation [ 5 , 6 ].
Patients with IPF suffer from difficult symptoms, of which breathlessness and cough are the most common ones [ 7 , 8 ]. In addition, there is some evidence that IPF patients frequently experience pain, although the location and mechanism of the pain have not been reported [ 7 ]. Comorbidities are frequently reported in IPF patients, as shown in a recent study, where 88% of the patients had at least one and 30% more than four other diagnoses [ 9 ]. The total number of comorbidities and especially the occurrence of cardiovascular disease are associated with increased mortality [ 9 – 12 ].
There exist a limited number of studies on the heath-related quality of life (HRQoL) of IPF patients in a real-life setting [ 13 ]. Most recent studies have either concentrated on pharmaceutical treatment or have included a very limited number of patients [ 7 , 13 ]. However, there are clear indications of a decreased HRQoL in IPF patients [ 13 , 14 ].
The primary aim of this cross-sectional study was to describe the HRQoL and symptom burden among IPF patients derived from a national IPF registry (FinnishIPF). The secondary aim was the identification of patients with increased need for palliative care by investigating the relationship between dyspnoea score and HRQoL.
Materials and methods
Study population.
The FinnishIPF study is a prospective national clinical registry study of IPF patients initiated in 2012. IPF diagnosis is made according to the American Thoracic Society/European Respiratory Society/Japanese Respiratory Society/Latin American Thoracic Society 2011/2015 criteria [ 1 , 6 ]. In Finland, practically all IPF patients are initially evaluated in public hospitals (university and central hospitals). The FinnishIPF registry consists of all IPF patients from specialist centres who have given their informed consent to participate to the study. K aunisto et al . [ 2 ] have published a detailed description of the FinnishIPF study. Overall, 76% of confirmed IPF patients have given consent to participate to the study [ 2 ].
This study was initiated in April 2015, when all 300 patients registered to FinnishIPF study at that time were contacted and asked for a written informed consent to participate in this substudy. The questionnaires were sent to the patients with the consent form. The patients who did not respond within 2 weeks were contacted by telephone and reminded to answer to the questionnaire.
Data collection and questionnaires
Sociodemographic and disease characteristics were collected from patient records and by a separate questionnaire. Collected data included age, sex, date of birth, marital status, living conditions, education, physical activity, the need for help in daily activities, the date of IPF diagnosis, comorbidities and smoking status. The participants' exercise habits during the preceding 6 months (≥30 min at least moderate-intensity leisure time physical exercise, i.e. causing breathless and sweating) were asked.
The specific questionnaires of symptoms and HRQoL were modified Edmonton Symptom Assessment Scale (ESAS), modified Medical Research Council (mMRC) dyspnoea scale and the RAND 36-Item Health Survey (RAND-36).
The ESAS is a self-rated, numeric-rating, symptom-based scale developed for assessing the symptoms of cancer patients [ 15 ]. ESAS measures different symptoms on a scale from 0 (no symptoms) to 10 (the worst possible symptoms) [ 16 , 17 ]. In this study, we used a modified version, including 12 questions on symptoms, one question on general wellbeing and a standardised body diagram on which patients could mark the areas of pain.
The mMRC scale is a self-rating tool to measure the degree of disability that breathlessness poses on day-to-day activities on a scale from 0 to 4: 0, no breathlessness except on strenuous exercise; 1, shortness of breath when hurrying on the level or walking up a slight hill; 2, walks slower than people of same age on the level because of breathlessness or has to stop to catch breath when walking at their own pace on the level; 3, stops for breath after walking ∼100 m or after few minutes on the level; and 4, too breathless to leave the house, or breathless when dressing or undressing [ 18 , 19 ].
The RAND-36 [ 20 ] is a general HRQoL measurement tool, for which Finnish general population reference values exist [ 21 ]. The Short Form-36, which is commonly used in IPF patients, is similar to RAND-36 [ 21 ]. It is divided into eight health concepts, as explained by H ays et al. [ 20 ] and A alto [ 21 ], with scale from 0 to 100 (lower score meaning worse HRQoL). The concepts are: “physical functioning” (10 questions from ability to move and exercise to the ability to take care of personal hygiene), “role physical” (four questions on role limitations due to physical health), “bodily pain” (two questions), “general health” (five questions), “vitality” (four questions on energy level and tiredness), “social functioning” (two questions), “role emotional” (three questions on role limitations due to emotional problems) and “mental health” (five questions on anxiety, depression and mood) during the past 4 weeks [ 20 , 21 ].
Statistics and ethical aspects
The data are presented as mean± sd or n (%). The statistical significance for the hypothesis for linearity across groups in RAND-36 domains and symptoms were determined by ANCOVA and logistic regression analysis with an appropriate contrast (orthogonal polynomial). In the case of violation of the assumptions ( e.g. non-normality), a bootstrap-type test was used. The normality of the variables was tested by using the Shapiro–Wilk W-test. Stata 14.1 (StataCorp LP, College Station, TX, USA) was used for the analysis.
The ethical committee of Helsinki University Central Hospital (Helsinki, Finland) approved this study (381/13/03/01/2014). Permission to screen hospital registries for patients with IPF was approved by the Finnish National Institute for Health and Welfare (Dnro THL/1161/5.05.01/2012). All patients who participated to this study gave a written informed consent to participate this substudy.
Of 300 registered patients, 47 were excluded: 42 did not want to participate or did not answer our questionnaire; one received lung transplantation and one was found not to be IPF patient, so these two also were excluded; three patients died before they answered.
Patient characteristics
The patient characteristics are shown in table 1 . The mean duration of IPF at the time of the study entry was 3.9 years. At least one comorbidity was reported in 79% (n=200) and more than two comorbidities in 30% (n=77) of the patients, respectively. 37% of the patients had performed at least moderate-intensity leisure time physical exercise for ≥30 min a week during the last 6 months, whereas 21% had not been engaged in any physical exercise. A majority (65%) of the patients did not need help in everyday life, whereas 26% had received assistance in their daily routines. The remaining patients ( 9% ) did not receive help but considered themselves to be in need of it.
TABLE 1
| 74±9 | |
| 165 (65%) | |
| 3.9±2.5 | |
| 10±4 | |
| 70 (28%) | |
| 22 (9%) | |
| Smokers | 26 (10%) |
| Ex-smokers | 109 (43%) |
| Never-smokers | 118 (47%) |
| 3.0±0.9 | |
| 83±17% | |
| Hypertension | 105 (42%) |
| Coronary heart disease | 64 (25%) |
| Diabetes | 50 (20%) |
| Heart insufficiency | 46 (18%) |
| COPD | 43 (17%) |
| Cancer | 41 (16%) |
| Asthma | 24 (10%) |
| Others | 93 (37%) |
| No comorbidities | 53 (21%) |
| 1.8±1.5 |
Data are presented as mean± sd unless otherwise stated. IPF: idiopathic pulmonary fibrosis; FVC: forced vital capacity; COPD: chronic obstructive pulmonary disease. # : smoking status and FVC were recorded at the time of diagnosis, and other factors at the time of questionnaire; ¶ : including three patients with lung cancer.
mMRC for breathlessness
The severity of breathlessness on exertion reported by mMRC score was 0 (no breathlessness) in 33 (13%), 1 (breathless when hurrying or walking up a hill) in 88 (35%), 2 (breathless when walking slower than people of same age or has to stop when walking) in 75 (30%), 3 (breathlessness stops walking after ∼100 m or a few minutes) in 34 (13%) and 4 (breathless when dressing or not able to leave the house) in 23 (9%) of the patients.
RAND-36 for HRQoL
The different dimensions of HRQoL measured by RAND-36 are presented in table 2 . There was a linear relationship between impaired HRQoL and all RAND-36 dimensions and a higher mMRC score (linearity p<0.001) ( figure 1 ). All HRQoL dimensions of RAND-36 were significantly impaired in patients with mMRC 2–4 as compared to the general population except “bodily pain”, which was significantly below the general population level only in patients with mMRC score 4 ( figure 1 ). Physical dimensions (“physical functioning” and “role physical”) were the most impaired ones. “Role physical” derives from four questions in the questionnaire and reflects limitations in everyday life due physical health problems [ 20 , 21 ].
TABLE 2
Symptoms by Edmonton Symptom Assessment Scale (ESAS) questionnaire and health-related quality of life by RAND 36-Item Health Survey (RAND-36)
| 95% | 4.7±2.6 | 72±28 | ||
| 88% | 4.9±3.0 | 72±20 | ||
| 85% | 4.1±2.9 | 62±27 | ||
| 82% | 3.7±2.9 | 53±23 | ||
| 79% | 3.8±3.0 | 51±42 | ||
| 67% | 2.8±2.8 | 47±29 | ||
| 66% | 2.2±2.3 | 40±19 | ||
| 63% | 2.1±2.4 | 31±39 | ||
| 61% | 2.1±2.4 | |||
| 57% | 1.9±2.5 | |||
| 48% | 1.6±2.3 | |||
| 40% | 1.1±1.8 | |||
| 90% | 4.4±2.4 |
Data are presented as mean± sd unless otherwise stated. # : numeric rating scale, 0–10.

Health-related quality of life measured by the RAND 36-Item Health Survey according to modified Medical Research Council (mMRC) dyspnoea scale groups. Data are presented as mean values with 95% confidence intervals. Values adjusted for age, sex, comorbidities, education and living status. Dashed lines mark Finnish general population levels.
ESAS for symptoms
The prevalence and mean intensity of symptoms as measured by ESAS are shown in table 2 . There was positive linear relationship between the intensity of all symptoms in ESAS questionnaire and increasing mMRC breathlessness score ( figure 2 ).

Symptoms measured by Edmonton Symptom Assessment Scale according to modified Medical Research Council (mMRC) dyspnoea scale groups. Data are presented as mean numeric rating scale (NRS) values with 95% confidence intervals. Values adjusted for age, sex, comorbidities, education and living status.
A striking increase in pain intensity in movement (p<0.001) and, to lesser extent, at rest (p=0.041) was found with an increased mMRC score ( figure 2 ). The prevalence of pain in different locations of body diagram according to mMRC groups is shown in table 3 . The prevalence of chest pain and increasing mMRC score showed a positive linear relationship (linearity p<0.001).
TABLE 3
Localisation of pain
| 33 | 88 | 75 | 34 | 23 | ||
| 9 (27%) | 17 (19%) | 16 (21%) | 7 (21%) | 9 (39%) | 0.66 | |
| 4 (12%) | 19 (22%) | 35 (47%) | 10 (29%) | 11 (48%) | <0.001 | |
| 7 (21%) | 24 (27%) | 20 (27%) | 3 (9%) | 8 (35%) | 0.41 | |
| 2 (6%) | 11 (12%) | 18 (24%) | 4 (12%) | 4 (17%) | 0.27 | |
| 8 (24%) | 38 (43%) | 38 (51%) | 11 (32%) | 7 (30%) | 0.56 | |
| 8 (24%) | 28 (32%) | 26 (35%) | 10 (29%) | 10 (43%) | 0.56 | |
| 18 (55%) | 45 (51%) | 32 (43%) | 16 (47%) | 15 (65%) | 0.77 | |
| 5 (15%) | 18 (20%) | 20 (27%) | 3 (9%) | 8 (35%) | 0.94 | |
mMRC: modified Medical Research Council dyspnoea scale. # : for linearity, adjusted for age, sex, comorbidities, education and living status; ¶ : four or more of the seven pain areas marked by the patient.
This was a cross-sectional, real-life study of the quality of life and symptoms of IPF patients. Our results show that increased breathlessness as measured by the mMRC questionnaire is related to impaired HRQoL and symptom burden. In addition to breathlessness and cough, pain in movement was detected in a majority of the patients. However, only chest pain had a linear relationship with increased mMRC breathlessness score. We suggest that pain and, more importantly, chest pain, may be an underdiagnosed symptom of IPF.
In our study, the HRQoL of IPF patients with at least moderate shortness of breath (mMRC ≥2), was impaired in all areas of HRQoL, especially physical function, when compared to the Finnish general population [ 21 ]. Our findings are in line with an American Internet survey of 220 IPF patients in which HRQoL was measured with PROMIS-29 [ 22 ]. A correlation between mMRC scores and all domains except sleep disturbance was found [ 22 ]. In a small, cross-sectional, longitudinal study of 32 Japanese IPF patients, lower scores were reported in all eight domains (HRQoL questionnaire SF-36) when compared to the general population [ 13 ]. Similarly, in another small observational validation study of 34 IPF patients, a decline was seen in seven of the eight measured domains of SF-36 compared to sex- and age-matched controls [ 14 ]. That particular study also showed correlation between baseline dyspnoea index and five SF-36 components: physical functioning, general health perceptions, vitality, social functioning and mental health [ 14 ]. Even though there was a significant correlation between baseline dyspnoea index and pulmonary function parameters, dyspnoea index seemed to predict HRQoL more sensitively than pulmonary function parameters [ 14 ]. Dyspnoea in daily living, measured by mMRC, is also stronger prognostic parameter than most physiological markers in the diagnostic phase of IPF [ 23 ]. N ishiyama et al. [ 23 ] showed that low arterial oxygen saturation in a 6-min walk test and mMRC score were the strongest predictors of IPF patient's survival.
In line with the American Internet survey, increasing mMRC score was related to the symptom burden of IPF patients in our study [ 22 ]. The three most common symptoms in our study were tiredness, shortness of breath and cough, which are in line with earlier findings [ 7 ]. Interestingly, however, pain in movement was the next most common symptom reported by the majority of our patients, and pain in rest was the sixth most common symptom, present in two thirds of the patients. In a Swedish register study of oxygen-dependent interstitial lung disease patients, pain was reported in 51% of the patients [ 7 ]. Similarly to our findings, Y ount et al . [ 22 ] demonstrated an association between dyspnoea severity in mMRC score and intensity of pain. In another small observational study, no correlation between baseline dyspnoea index and pain index was found [ 14 ]. These differences could be related to different stage of the disease in different study populations.
In our study, every third patient reported chest pain, which also had linear relationship to the intensity of breathlessness measured by mMRC. Unspecified thoracic pain has been reported in pulmonary sarcoidosis and chronic obstructive pulmonary disease but, to our knowledge, this is the first study to report chest pain in IPF [ 24 , 25 ]. The exact aetiology of chest pain in IPF falls beyond the scope of our study, and should be an aim of further studies. However, as the relationship between chest pain and breathlessness was maintained after adjusting for comorbidities and age, the results suggest that chest pain may be a symptom related to IPF itself. This finding should be taken into account when considering diagnostic tests and treatment strategies for patients with advanced IPF.
Study limitations
The cross-sectional nature of the study limits our results to a single time-point and does not allow us to describe the changes in symptoms or HRQoL over time. Our cohort may be subjected to some selection bias, as some patients at a very advanced stage of the disease or close to death are likely to be lost from the cohort. Another limitation is that although the diagnosis of IPF was made by pulmonologists according to international guidelines, there was no central confirmation of the diagnoses. The strength of our study is a relatively large population of IPF patients in different phases of disease trajectory, evaluated by several assessment tools in real-life setting, and a high response rate.
Conclusions
Pain is a relatively common symptom in IPF. In particular, chest pain is related to increasing mMRC score. This could indicate a causal relationship between chest pain and progressive IPF, but further studies are necessary to confirm and explain these findings. Our results show that mMRC not only reflects breathlessness in patients with IPF but indicates HRQoL and overall symptom burden. The HRQoL was significantly deteriorated and symptom burden rose in patients with mMRC score ≥2. Thus, mMRC could be used as a simple screening tool for palliative care needs of IPF patients.
In Yaroslavl ended the competition on ski races among customs officers in the Central region
In Yaroslavl ended the championship of the Central customs administration in skiing. This event is one of the stages of the Spartakiad of the customs authorities and held in celebration of the 75th anniversary of the Victory in the great Patriotic war of 1941-1945. The championship was held at the center of skiing “Demino” (Yaroslavl oblast) from 11 to 14 February. The fight for the medals were 56 athletes representing 14 teams from customs of the Central Federal district. “Such a tournament is a great honor and responsibility for us. We are pleased to welcome all athletes on the hospitable land of Yaroslavl. I am sure that our competition will be a real feast, serve to strengthen the friendly relations between customs and will contribute to popularization of sport and healthy lifestyle. I wish all the participants good luck, success, good team spirit, fair play and high results!”, addressed the participants at the opening of the championship, acting head of the Yaroslavl customs Sergey Komissarov. The program of the Championship included two competition days: the first day of the ski race was held in free style among men in the individual championship in 5 km, women 3 km. on the second day of the championship held a mixed ski relay race. Women overcame the free first and second stage of the race and the men ran the third and fourth stage. As noted by the chief judge of competitions Svetlana Smirnova: “Despite the fact that in the days of the tournament is warm weather, the track is prepared good includes not challenging workers climbs and not steep slopes. We have tried to develop a distance so that the athletes did not reduce speed in the course of its overcoming and showed his best result.” This year’s team-the mistress of tournament the Yaroslavl customs for prize-winning places fought: Venir a Rufov, Anton Ignatov, Elena Pyatova, Lesya Gromova and in the individual championship Alexey Gordeev. On the first day of the competition places in the individual standings were as follows: in the women’s race on 3 km freestyle first place was taken by Olga Bogdanova from the Tula customs, the second – Palina Lazarenkova from Smolensk and closes the top three winners of the first competition day among women – Anna Kulbakina of Bryansk customs. In the men’s race 5 km freestyle first to the finish came the representative of the Bryansk customs Roman Timokhin, the second place of the podium was occupied by Maxim Ippolitov from Smolensk, third place – Alexey Mukhortova from the Kursk customs. The second day of competition – perhaps the most spectacular day of the Championship. Because this day determined the winners of the mixed relay and team championship. The main struggle was for second place between Tula and Bryansk customs. During the three stages of the Tula customs was ahead, but in the final stage of the Bryansk customs snatched victory. With the team result, 40 minutes and 10 seconds faster than all the distance relays overcame four skiers from Smolensk customs in the composition of Pliny Lazarenkova, Tatiana Braccini, Denis and Maxim Nahaeva Ippolitov. In the second place, the representatives of the Bryansk customs – Irina Motina Anna Kulbakina, Mikhail Motorin and Roman Timohin. “Bronze” – four from the Tula customs – Olga Bogdanova, Tatyana Stanovova, Ilyas Hidersine and Valentine Hinderance. Fourth to finish came the hosts of the event and the athletes from the Yaroslavl customs. In the team standings, at the end of two days of competition, the winner of the championship of the Central customs administration in ski racing was the team of the Smolensk customs, second place – skiers Bryansk customs, third place went to the team of Tula customs. Fourth place went to the team of the Yaroslavl customs. At the end of last championship of the winners of the Championship will be formed team of the Central customs administration, which will act in competitions on ski races held in the framework of the Federal customs service of Russia.
Phillip Kushnarev, press Secretary of the Yaroslavl customs
In Purovsky district withdrawn from circulation benactyzine cigarette
The Pskov customs officers found the “extra” wine
Central Customs Administration

IMAGES
VIDEO
COMMENTS
The modified Medical Research Council (mMRC) scale is recommended for conducting assessments of dyspnea and disability and functions as an indicator of exacerbation. The modified Medical Research Council (mMRC) scale. An mMRC scale grade of 3 have a significantly poorer prognosis and that the mMRC scale can be used to predict hospitalization ...
The mMRC (Modified Medical Research Council) Dyspnoea Scale is used to assess the degree of baseline functional disability due to dyspnoea. It is useful in characterising baseline dyspnoea in patients with respiratory disease such as COPD. Whilst it moderately correlates with other healthcare-associated morbidity, mortality and quality of life ...
The mMRC dyspnea scale is used to calculate the BODE index, a tool which helps estimate the survival times of people living with COPD. The BODE Index is comprised of a person's body mass index ("B"), airway obstruction ("O"), dyspnea ("D"), and exercise tolerance ("E"). Each of these components is graded on a scale of either 0 to 1 or 0 to 3 ...
This study examined the validity of the Medical Research Council (MRC) dyspnoea scale for this purpose. METHODS One hundred patients with COPD were recruited from an outpatient pulmonary rehabilitation programme. Assessments included the MRC dyspnoea scale, spirometric tests, blood gas tensions, a shuttle walking test, and Borg scores for ...
The physical limitation or functional impact of breathlessness can be assessed using the Medical Research Council dyspnea scale (MRC; or modified MRC [mMRC] 39, 40 which is more widely used), 41 Dyspnea Exertion Scale (DES), 42 Oxygen Cost Diagram (OCD), 43 Baseline Dyspnea Index (BDI), 29 or Disability Related to COPD Tool (DIRECT). 44 The ...
The MRC Dyspnoea Scale is simple to administer as it allows the patients to indicate the extent to which their breathlessness affects their mobility. The 1-5 stage scale is used alongside the questionnaire to establish clinical grades of breathlessness. MRC Breathlessness Scales: 1952 and 1959.
The Medical Research Council (MRC) Dyspnoea Scale may allow a more precise assessment of functional status and improve current risk models. We investigated the ability of the MRC Dyspnoea Scale to assess survival in PAH and compared performance to WHO FC and the COMPERA 2.0 models. Patients with Idiopathic, Hereditary or Drug‐induced PAH who ...
Introduction: Health-related quality of life (HRQoL) is an important patient-centred outcome in chronic obstructive pulmonary disease (COPD). The aim of the current study is to compare the discriminative capacity of the modified Medical Research Council (mMRC) dyspnoea scale and the Global Initiative for Chronic Obstructive Lung Disease (GOLD) spirometric classification of COPD on HRQoL, as ...
The modified Medical Research Council (mMRC) dyspnoea scale is a measure of breathlessness severity recommended by guidelines and utilised as an inclusion criterion or endpoint for clinical trials. No studies have been conducted to validate the categorical descriptors against the dyspnoea severity grade.
The Medical Research Council (MRC) dyspnoea scale (see table 1) should be used to grade the breathlessness according to the level of exertion required to elicit it. ... Offer pulmonary rehabilitation to all people who view themselves as functionally disabled by COPD (usually Medical Research Council [MRC] grade 3 and above). Pulmonary ...
Modified Medical Research Council Dyspnoea Scale Grade 0 "I only get breathless with strenuous exercise" 1 "I get short of breath when hurrying on the level or walking up a slight hill" 2 "I walk slower than people of the same age on the level because of breathlessness or have to stop for breath when walking at my own pace on
MRC dyspnoea scale. Last edited 3 Feb 2021. Authoring team. Medical Research Council dyspnoea scale for grading the degree of a patient's breathlessness. 1. I only get breathless with strenuous exercise. 2. I get short of breath when hurrying on level ground or walking up a slight hill. 3.
This study examined the validity of the Medical Research Council (MRC) dyspnoea scale for this purpose. Methods: One hundred patients with COPD were recruited from an outpatient pulmonary rehabilitation programme. Assessments included the MRC dyspnoea scale, spirometric tests, blood gas tensions, a shuttle walking test, and Borg scores for ...
You stop for breath after walking about 100 yards (60 metres) or after a few minutes on level ground. You are too breathless to leave the house, or breathless when dressing or undressing. Source: The MRC breathlessness scale adapted from Fletcher C.M, Discussion on the Diagnosis of Pulmonary Emphysema J R Soc Med September 1952 45: 576-586.
The Modified Medical Research Council (MMRC) scale, baseline dyspnea index (BDI) and the oxygen cost diagram (OCD) are widely used tools for evaluation of limitation of activities due to dyspnea in patients with chronic obstructive pulmonary disease (COPD). There is, however, limited information on how these relate with each other and with ...
Symptoms were recorded at least 3 times a week, including cough intensity and frequency (Cough Assessment Test scale (COAT) score), breathlessness grade (modified Medical Research Council (mMRC ...
This study aimed to assess dyspnea, physical activity, muscle strength, and health-related quality of life in older adults diagnosed with chronic obstructive pulmonary disease (COPD) who are also considered frail. The study included volunteers aged 65 and over, diagnosed with COPD according to GOLD criteria. Individuals with COPD were divided into two groups according to the FRAIL Frailty ...
I met a girl online and she wants to come here but says after purchasing visa, passport, tickets, etc. she was told she still needs $1525 for a required insurance. any info on this would be greatly appriciated.
This study examined the validity of the Medical Research Council (MRC) dyspnoea scale for this purpose. METHODS—One hundred patients with COPD were recruited from an outpatient pulmonary rehabilitation programme. Assessments included the MRC dyspnoea scale, spirometric tests, blood gas tensions, a shuttle walking test, and Borg scores for ...
Access Yaroslavl' traffic cameras on demand with WeatherBug. Choose from several local traffic webcams across Yaroslavl', Yaroslavskaya oblast', RU. Avoid traffic & plan ahead!
Yaroslavl State Medical University (YSMU) is a public university in Yaroslavl, Russia. It was founded in 1944 and is a leading regional center of medical education and biomedical research. Yaroslavl State Medical University Russia is recognized by the World Health Organization (WHO) and the National Medical Commission (NMC) of India.
The specific questionnaires of symptoms and HRQoL were modified Edmonton Symptom Assessment Scale (ESAS), modified Medical Research Council (mMRC) dyspnoea scale and the RAND 36-Item Health Survey (RAND-36). The ESAS is a self-rated, numeric-rating, symptom-based scale developed for assessing the symptoms of cancer patients .
In Yaroslavl ended the championship of the Central customs administration in skiing. This event is one of the stages of the Spartakiad of the customs authorities and held in celebration of the 75th anniversary of the Victory in the great Patriotic war of 1941-1945.