Thank you for visiting nature.com. You are using a browser version with limited support for CSS. To obtain the best experience, we recommend you use a more up to date browser (or turn off compatibility mode in Internet Explorer). In the meantime, to ensure continued support, we are displaying the site without styles and JavaScript.
- View all journals
- Explore content
- About the journal
- Publish with us
- Sign up for alerts
- Open access
- Published: 28 February 2018

Quantitative account of social interactions in a mental health care ecosystem: cooperation, trust and collective action
- Anna Cigarini 1 , 2 ,
- Julián Vicens ORCID: orcid.org/0000-0003-0643-0469 1 , 2 , 3 ,
- Jordi Duch ORCID: orcid.org/0000-0003-2639-6333 3 , 4 ,
- Angel Sánchez 5 , 6 , 7 , 8 &
- Josep Perelló ORCID: orcid.org/0000-0001-8533-6539 1 , 2
Scientific Reports volume 8 , Article number: 3794 ( 2018 ) Cite this article
9676 Accesses
12 Citations
51 Altmetric
Metrics details
- Applied mathematics
- Human behaviour
- Psychology and behaviour
- Public health
An Author Correction to this article was published on 26 September 2018
This article has been updated
Mental disorders have an enormous impact in our society, both in personal terms and in the economic costs associated with their treatment. In order to scale up services and bring down costs, administrations are starting to promote social interactions as key to care provision. We analyze quantitatively the importance of communities for effective mental health care, considering all community members involved. By means of citizen science practices, we have designed a suite of games that allow to probe into different behavioral traits of the role groups of the ecosystem. The evidence reinforces the idea of community social capital, with caregivers and professionals playing a leading role. Yet, the cost of collective action is mainly supported by individuals with a mental condition - which unveils their vulnerability. The results are in general agreement with previous findings but, since we broaden the perspective of previous studies, we are also able to find marked differences in the social behavior of certain groups of mental disorders. We finally point to the conditions under which cooperation among members of the ecosystem is better sustained, suggesting how virtuous cycles of inclusion and participation can be promoted in a ‘care in the community’ framework.
Similar content being viewed by others
Reformulating computational social science with citizen social science: the case of a community-based mental health care research
Investigation of turning points in the effectiveness of Covid-19 social distancing
An agent-based model of social care provision during the early stages of Covid-19
Introduction.
Approximately one fifth of the world population will suffer some mental disorder (MD) at some point in their lives, such as anxiety or depression 1 . The direct economic costs of MD, including care and indirect effects, is estimated to reach $6 trillion in 2030, which is more than cancer, diabetes, and respiratory diseases combined 2 . As part of a global effort to scale up services and bring down costs, reliance is increasingly made upon informal social networks 3 . A holistic approach to mental health promotion and care provision is then necessary, and emphasis is placed on the idea of individuals-in-community: individuals with MD are defined not just alone but in relationship to others 4 . Such a paradigm shift implies superseding the traditional physician-patient dyad to include caregivers, relatives, social workers, and the community as a whole, recognizing their crucial role in the recovery process.
A key aspect in the definition and aetiology of MD has to do with social behavior 5 : behavioral symptoms, or consequences at the behavioral level, characterize most MD. For instance, autism, social phobia, or personality disorders are determined by the presence of impairments in social interaction. Other disorders result in significant difficulties in the social domain, such as depression or psychotic disorders. Further, conditions that are intrinsically behavioral (as for eating disorders or substance abuse) seem to be exacerbated by the influence of social peers. A large body of research has therefore looked at the neural basis of social decision-making among individuals with MD to identify objective biomarkers that may prove useful for its diagnosis, therapy evaluation, and understanding 6 , 7 , 8 . However, such a methodology does not well fit into the individuals-in-community paradigm. We argue that an agent-based approach which draws upon experimental game theory might prove insightful and ecologically valid for the study of behavior in a given social environment.
Within the mental health literature, the use of game theory as a way to understand the multi-faceted dimensions of behavior has received already quite some attention 9 , 10 . Most research addressed the issue of behavioral differences between individuals with MD and healthy populations 6 , 7 , 11 , 12 , 13 , 14 , 15 , 16 . These works, that point to cognitive and affective processing impairments 6 , 16 , 17 , further support the idea that MDs are associated with significant and pervasive difficulties in social cognition and altered decision-making at various levels. Yet, despite these studies are of very much interest, they are primarly concerned with dyadic interactions among people with specific MDs. That is, they lack insights into the complexity of individual behaviors of MD within a specific social context.
Here we adopt a novel community perspective. Our objective is twofold: First, we aim to develop a thorough taxonomy of the behavioral traits of role groups within the collective. We thus account for both the heterogeneity of actors, and for multiple types of social interactions. We strongly believe that to predict and understand behavior is necessary to consider the relationship context in which individuals are embedded. Therefore diversity of roles, motivations or capabilities, must be taken into account. Also, real life social interactions occur in different forms; sometimes people must work together, some others they have to coordinate or anti-coordinate their behaviors, yet in other situations they find themselves in more or less disadvantaged positions. It is therefore of crucial importance to encompass a comprehensive range of strategic situations if we are to appreciate behavior. That is, traits such as trust, altruism, or reciprocity, along with the person’s own expectations, all play a role in the process of decision making in social contexts. This calls for an experimental approach in which participants face several strategic settings. Our second objective is to provide quantitative accounts of social capital within the mental health community, bringing the notion of social capital into the forefront of mental health care. Far from being universally defined, its core contention is that social networks are a valuable asset, providing a basis for social cohesion and cooperation towards a common goal 18 (which is, in our case, mental care provision). It thus encompasses those norms and forces that shape social interactions, serving as the glue that holds society together 19 .
For these purposes, we have designed an experimental setup that probes into the complexity of the interdependencies at play within the mental health ecosystem. Accordingly, our experiments take place in a socialized, lab-in-the-field setting 20 , in order to be as close as possible to the dynamic and unique nature of real-life social interactions. The design of our socialized setup is based on a participatory process and citizen science practices 20 which counted on the collaboration of all stakeholders of the mental health ecosystem. By combining all these ingredients, we have developed a framework that, as will be shown below, allows to capture some difficult-to-observe aspects of behavior and social capital within mental health ecosystems as a way to understand how communities contribute to care and resocialization.
A full description of the games we implemented can be found in the Methods section below, but for clarity we briefly describe here the games we used. We had participants play two dyadic games, namely the Trust game, in which they had to lend money to another player who then obtains a return, and has the option to send some money back to the lender; players played in both roles. They also played the well known Prisoner’s Dilemma, in which they had to choose to cooperate or to try to benefit from the other’s cooperation. Finally, they played a collective risk dilemma, in which the whole group had to reach a common goal to avert a catastrophe that most likely would wipe out their money. Participants belonging to the mental health ecosystem played with each other in group of six players. However, they could by no means guess with whom they were actually playing.
We begin the presentation of our results from the dyadic games of our suite of strategic interactions. Aggregate behavioral measures point to systematic deviations from self-interested predictions which are in line with previous literature on experimental game play 21 . In the Prisoner’s Dilemma (PD), the average cooperation rate across all individuals is c = 0.61 ± 0.03 (standard error of the mean), which is notoriously well above the Nash equilibrium prediction of c = 0. Participants behavior in the PD is also significantly associated with their estimates about the likely cooperation of the partner ( \({\chi }^{2}=32.48\) , p = 1.2 · 10 8 ), with 44% of all participants expecting the partner to cooperate, and thus cooperating themselves. This points to the crucial role of positive expectations on cooperative behavior 22 . Further, participants trust and reciprocate positive amounts in the Trust Game (5.79 ± 0.15 monetary units (MU) and 41.3 ± 1.37% of the amount available to return, respectively), again departing largely from Nash equilibrium conjectures of 0 MU transferred. The results also suggest that in considering the mental health community in its whole, thus accounting for the diversity of actors and roles, the global picture does not substantially differ from society at large.
Sectorial and dyadic behavior
As we stated above, our main interest is to delve into the behavior of the different actors who make up the mental health ecosystem Fig. 1 summarizes the results for the five groups of individuals concerned. The heatmap yields several insights that are worth commenting upon.
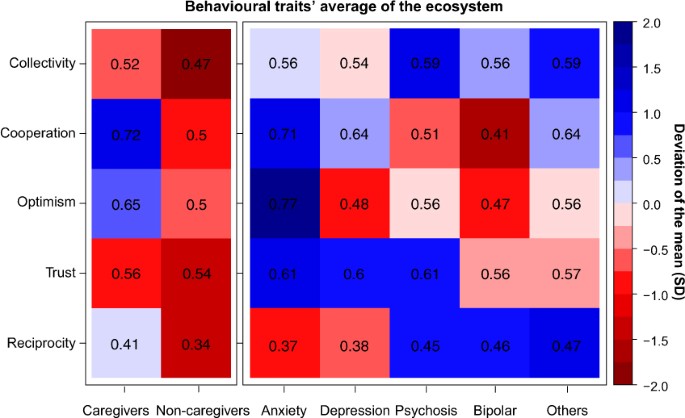
Heatmap of behavioural traits’ average and deviation of the mean across games. Collectivity refers to the ratio of contribution in the Collective-Risk Social Dilemma. Cooperation and Optimism refers to the ratio of cooperation and expected cooperation, respectively, in Prisoner’s Dilemma. Trust and Reciprocity refers to the ratio of capital trusted and reciprocated in Trust Game. The left part shows the ratio of individuals without mental conditions: caregivers (professionals and relatives with caregiving tasks) and non-caregivers (relatives without caregiving tasks, friends and others). The right part shows the actions of individuals with mental conditions. Therefore, the number in each cell indicates the ratio of social preferences per subjects in each social dilemma and the color scale shows the deviation of the mean measured in SD units.
In one-shot dyadic interactions some marked differences in the frequency of cooperative behaviors (PD) arise within the collective formed by affected with MD, caregivers, non-caregivers (Kruskal-Wallis rank sum test, \(H=6.04,df=2,p=0.0488\) ). Further pairwise comparisons (see Supplementary Table S1 ) show that participants with anxiety and caregivers are more likely to opt for the cooperative strategy compared to participants with bipolar disorder, psychosis or other members of the collective. Participants with anxiety are also the ones with the most positive expectations about the partner’s behavior compared to all but caregivers (see Supplementary Table S2 ). Also, relatives, friends and other members with no MD defect more than caregivers (Mann-Whitney U test, \(U=1352,p=0.02839\) ), being relatives remarkably less cooperative than the rest of the collective c = 0.33 ± 0.16. This suggests that cooperation among members of the mental health ecosystem is contextually based, depending on the role that actors play in the recovery process. It also varies across diagnostics, revealing a marked cooperativeness and optimism of individuals with anxiety disorders.
On the other hand, in sequential dyadic interactions (TG) all participants trust more than half of their endowment, being the distribution of initial transfers similar across groups. No variation is indeed found in trust levels between participants with MD, caregivers and non caregivers (Kruskal-Wallis rank sum test, \(H=2.75,df=2,p=0.25\) ). Yet, at the time of reciprocating the partner’s behavior, participants with anxiety and depression return the least (37.5 ± 3.3%). The difference is significant if compared to return transfers of participants with psychosis or other diagnostics (see Supplementary Table S4 ).
Group interaction
Our experimental setup has proven extremely informative in its most novel section, namely the analysis of group interactions framed within the Collective Risk Dilemma (CRD), with no prior result within the mental health literature. In global terms, the average amount contributed to the public good (22.6 MUs) is much more than the fair contribution of 20 MUs, where by fair we understand sharing equally the total amount needed for the threshold (120 MUs) among all six participants. Here it is important to keep in mind that participants were told that all money contributed would go to reforestation projects, so it is not irrational to keep contributing beyond the threshold as many of our subjects did. The key result in the CRD is that large, significant differences (t-test, \(t=2.85,df=242,p=0.0047\) ) are found between participants with and without mental disorders. The former contribute with 22.95 ± 0.63 MUs compared to 20.34 ± 0.68 MUs from the latter, and therefore it appears that when repeated interaction and sustained teamwork (CRD) are required, people with MD contribute much more to the common goal (See Supplementary Section 1.6.2).
Contribution dynamics vary according to group composition in terms of number of participants with mental disorder conditions and other actors involved in the recovery process. All groups successfully reach the target collecting on average 135.64 ± 1.75 MUs (see Supplementary Section 1.6.1). Similarly to other public good experiments, contributions decrease over time 23 . While in the first round participants contribute around 56.3% of the allowed contribution per round (2.2 ± 0.07 MUs, where the social optimum is 2 MU), contributions drop when the endgame effect sets in. A Spearman’s rank-order correlation of contributions over rounds corroborates this negative time trend ( \(\rho =-0.757,p < 0.05\) ). Both patients and actors involved in the recovery process reduce their contributions by the end of the game. However, in almost all rounds, participants with a mental condition contribute more than caregivers and non caregivers, for whom motivations to contribute decline steadily (see Fig. 2 ).
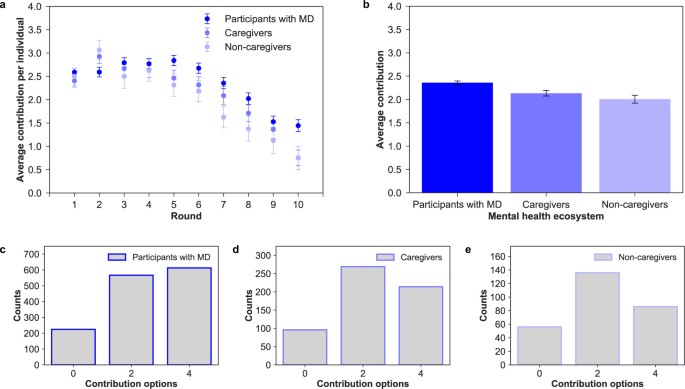
(a) Individual contribution over rounds. Evolution of contributions (mean and standard error of the mean) during the game between participants with mental disorder conditions, caregivers and non-caregivers. We can see that all groups behave similarly and in an identical way to a previous experiment run outside the mental health ecosystem 40 . (b) Average individual contribution per round. Average contribution and standard error of the mean in the mental health ecosystem. There are significant differences between participant with MD and the rest of actors, caregivers (t-test, \(t=2.107,df=155,p < 0.0294\) ) and non-caregivers (t-test, \(t=2.499,df=48,p=0.01588\) ). Distribution of choices by participants with MD ( c ), caregivers (d) and non-caregivers ( e ). The most of participants with MD (43.6%) selected the maximum contribution (4), while the caregivers (46.5%) and non-caregivers (48.9%) mostly selected the fair contribution (2).
In terms of the group composition, groups where individuals with MD conditions constitute half or the majority of the group (n = 36) do much better in sustaining cooperation compared to groups where firsthand affected are the minority (n = 9). It is here worth to mention that participants may see who the rest of the members are but ignore who is exactly making the choice in the game (see Methods for further details). As Fig. 3b shows, while average individual contributions are similar in the last periods (rounds 6–10 t-test, t = 0.19, p = 0.85), groups with half or more individuals with MD contribute significantly more at the beginning of the game (rounds 1–5 t-test, t = 2.79, p = 0.0054). Hence, the presence of three or more individuals with a mental condition in the group has a positive and stabilizing effect on average individual contributions. Likewise, in games with a low proportion of participants affected with MD the group achieved the goal, on average, later than in games with more than 50% of participants affected with MD (see Fig. 3a ).
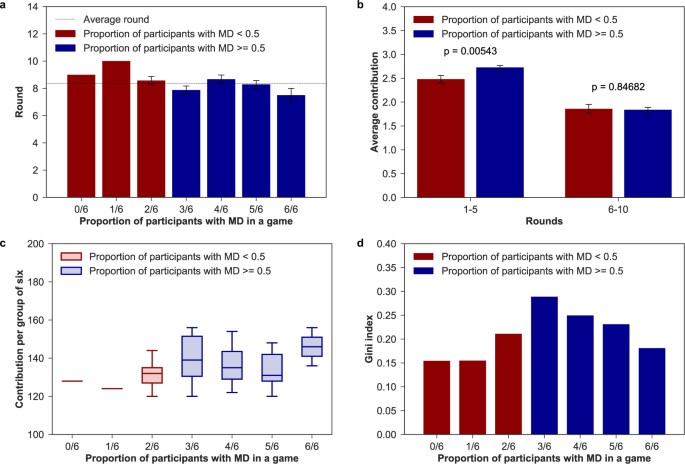
(a) Average round of achievement. Round (mean and standard error of the mean) in which the group of six achieved the target. (b) Aggregated contributions per group composition. Contributions (mean and standard error of the mean) in the first and last five-rounds per number of individuals with MD in a group. There are significant differences (t-test p < 0.01) in contributions in the first part of the game. (c ) Contributions per group of six. Total group contributions by number of individuals with mental conditions in the group. (d ) Gini index of final payoff within groups. Level of inequality in final payoff based on the number of individuals with MD in each group.
If we then break down the analysis by group type, we find that group members contribute and benefit differently from cooperation (see Fig. 3c ). Indeed, final payoffs within groups are far from being equally distributed (see Fig. 3d ), with the highest inequality found in the group where the number of patients equals the number of actors involved in the recovery process (Gini coefficient = 0.289). We thus see clearly that the cost of collective action is mainly supported by individuals with a mental disorder. Given that they contribute the most within all groups, lower investments are needed for other members of the collective to reach the common target. Yet, in 4/6 and 5/6 groups caregivers reduce average individual contributions while non-caregivers pay more than their fair share. In 1/6 and 2/6 groups, on the other hand, caregivers are the ones who compensate the unfair contributions of other members. These last groups are the ones that ensure the lowest inequality in final payoffs. Therefore, while our results are unambiguous about the larger readiness for collective action among people with MD, we cannot claim nothing about the rest of the collective.
Let us now turn to the discussion of the above results and their implications (see Table 1 for a summary of the key findings). As a first general remark, through our lab-in-the field experiment we found that an ecosystem approach to mental health care brings with it a quite complex scenario with several interesting insights. To begin with, participants with anxiety symptoms display a markedly different behavior compared to other diagnostics: they are more likely to opt for the cooperative strategy compared to individuals with bipolar disorder or depression, and return significantly less than participants with psychosis or other disorders. Since the current study is the first to investigate social decision-making within a heterogeneous population of individuals diagnosed with MD, a comparison with previous research is only possible referring to studies focusing on specific clinical and quite homogeneous populations. Several experiments have demonstrated deficits in cooperative behavior among individuals with anxiety or depression when playing iterated versions of the PD 11 , 17 , 24 , 25 , but results about altruism (Ultimatum Game) and trust are inconsistent between studies 6 , 7 , 11 , 12 , 17 , 26 . Individuals with major depressive disorders (which include anxiety and depressive symptoms) have also been found to systematically differ when their emotional responses to fairness are compared 6 , 17 , showing higher levels of negative feelings when faced with unfair treatments. One of the hypothesis advanced to explain the systematic behavioral differences of individuals with anxiety relates to a potentiated sensitivity to negative stimuli as well as a tendency to treat neutral or ambiguous stimuli as negative or as less positive 6 , 12 , 17 , 27 . This hypothesis might find support in our results as for the low returns in the Trust Game, despite displaying relatively high trust in the partner’s behavior and very high expectations. Indeed, participants with depressive or anxiety symptoms in our experiment significantly over-punish trustee transfers, but the low returns are independent of the amount received. This seems to imply that participants with mood disorders respond negatively to their partner behavior, as if they interpret their partner’s choice in a negative sense. Alternatively, fairness considerations may be playing a role: low returns of participants with mood disorders might therefore be due to different fairness perceptions 6 , 12 , 17 , which result in a bias towards negative reactions rather than positive rewarding.
Deficits in economic game play have also been documented for individuals with bipolar disorder. Studies report low and decreasing trust levels over sequential interactions, skeptical beliefs about the partner’s behavior and a tendency to break cooperative interactions 28 , 29 . Again, this is partly supported by our results. Negative expectations of participants with bipolar disorder indeed agree with a low frequency of cooperative choices, little amounts of money sent to trustees, and low contributions to collective action. In line with King-Casas et al . results 29 , while individuals with depression trust in the cooperativeness of other people, those with bipolar personality disorders do not. Cognitive dysfunctions (insula response) might possibly reflect an atypical social norm in this group 29 . Consequently, defection by partners might not violate the social expectations of individuals with BPD. In contrast, in our experiment, participants with bipolar disorder return the most within the group of individuals with a mental disorder. That is, they report a strong willingness to positively respond to a norm of trust as to signal their partner trustworthiness. Therefore, conditioned on the previous action of the partner, it seems that individuals with BPD are willing to show cooperative behavior. Considering now individuals with high levels of psychopathy, they have been found to make less fair offers, accept less fair offers, and show very high levels of defection 15 , 16 , 30 . Major explanations for such behavior point to deficits in emotion regulations (amygdala dysfunctions), which would lead to lack of anxiety, empathy, and guilt, coupled with exaggerated levels of anger and frustration 30 and to the absence of prepotent biases toward minimizing the distress of others 16 . In this case, our experiments do not confirm those previous results: Indeed, participants with psychosis are the ones who trust, contribute the most to the public good, and are willing to take costly actions to reciprocate their partner’s behavior. It could be possible that, as psychopathic disorders are in fact a large group of different ones, behavioral differences among subgroups may lead to this discrepancy. In connection with these results, it is interesting to note that recent results on a large population of patients with paranoia suggest that distrust is not the best explanation for reduced cooperation and alternative explanations incorporating self-interest might be more relevant 31 , 32 . This calls for further research into this particular family of MD to clarify whether or not the behavioral characterization applies to all or to a subclass of them.
However, pointing to deficits in social cognition can only account for a partial explanation of individual behavior, and does not contribute to community care narratives. The fact that nothing in this direction has been reported before also reinforces the need to adopt a more holistic view on the interdependencies at play within the mental health collective. Indeed, if statistically relevant differences in cooperative behavior are found across diagnostics, they also depend on the role that actors play in the recovery process. That is, caregivers display exceedingly large degrees of cooperativeness and optimism in one-shot interactions. Caregivers can be thus considered the strong ties of the mental health ecosystem, of particular value when one seeks emotional support. With the de-institutionalization of health systems, caregivers have indeed become key players in care provision. Taking into account their behavior and expectations is therefore of particular interest to extend the support tailored to their needs. These actions should improve the effectiveness of their role by guiding them 33 . Yet, relatives who do not strictly contribute to caregiving practices turn out to be the weak links. It is thus likely that interventions designed to increase their participation in the community might help improve the recovery process.
Also, members of the mental health ecosystem do not equally contribute and benefit from collective action. Rather, systematic behavioral differences arise as the number of social interactions increase, i.e., when teamwork is required for the collective to benefit as a whole. This suggests that considering repeated games may prove extremely insightful for the purpose of the research. Indeed, our experiments show that individuals with MD are the ones who contribute the most to the public good: they make larger efforts towards reaching the collective goal, thus playing a leading role for the functioning of the ecosystem. As a consequence, groups with half or more participants with MD do better in sustaining cooperation in the first rounds, which implies that a community care setting might prove successful for capability building. Yet, large proportions of individuals with MD in a group result in higher inequalities in final gains, which reach the maximum when the number of individuals with MD equals the number of caregivers or relatives. This means that community care perspectives might also take account of group composition to deal with potential inequalities arising from differential capabilities. In summary, we have explored the behavior of all individuals and role groups who make up the mental health ecosystem through an extensive suite of games that simulate strategic social situations. Overall, the results point to the availability of large social capital in the mental health community that can make a difference in the welfare and recovery process of firsthand affected, and suggest that the community-centered approach to mental care may turn out to be very beneficial. Indeed, the behavior of individuals with MD can be better explained by examining not only their cognitive abilities, but also the web of relationships in which they are embedded. Yet, that web of relationships presents opportunities and imposes constraints.
Though we depicted some behavioral differences in dyadic interactions, most importantly we found that individuals with MD show a remarkably larger disposition towards sustaining cooperation within groups. The larger readiness of individuals with MD to contribute to the collective action problem can thus be seen as a way to claim their place in the community. By having participants unaware of their partner’s identity, we could indeed measure participants decisions based solely on the value they placed on the group’s welfare, independently of its composition or other factors. Yet, the fact that participants with MD contribute the most implies for other members of the group lower investments to reach the common target. This, on the other hand, unveils the vulnerability of individuals with a diagnosis of MD. Repeated or periodic and more situated experiments with digital platforms 34 , in the future, can surely provide further valuable insights into the effect of participants prior knowledge of and relation with the partner on their behavior. We are indeed sure that our experimental setup can prove helpful in complementing the diagnostic process of physicians and health professionals and even to evaluate care service providers. On the other hand, other possible application of this approach arises in the realm of behavior change interventions 35 , that should focus on the aspects that are more specific of every disorder.
In conclusion, the results reinforce the idea of community social capital as a key approach to the recovery process based on an ecosystem paradigm (see also the recent results in ref. 36 about the role and impact of family and community social capital on MD in children and adolescents). Also, if on the one hand the fact that the results of our dyadic games are in general agreement with previous studies validates our procedure; on the other hand it supports the validity and contributions of neuroeconomics and experimental approaches to the study of MD. Finally, given that our work has been carried out in a fully socialized context, this approach can be applied to any similar’ ‘care in the community’ initiative. The adoption of our setup could lead to the identification of core groups that can boost and sustain cooperation within a given community. It can also help in discriminating among different communities in order to identify best practices and optimize resource allocation 37 .
All participants were fully informed about the purpose, methods and intended uses of the research. No participant could approach any experimental station without having signed a written informed consent. The use of pseudonyms ensured the anonymity of participants’ identity, in agreement with the Spanish Law for Personal Data Protection. No association was ever made between the participants’ real names and the results. The whole procedure was approved by the Ethics Committee of Universitat de Barcelona. All methods were performed in accordance with the relevant guidelines and regulations.
Experimental design
As indicated in the main text, the dialogue with the main stakeholders of the mental health ecosystem was at the centre of the project. Around 20 representatives including members of the Catalonia Federation of Mental Health (Federació Salut Mental Catalunya), firsthand affected, relatives, caregivers, and other professionals related to both the health and social sector, informed and validated the whole research through focus groups and further discussions, leading to the largest experiment of this kind ever carried out. Citizen science principles guided the whole experimental design process in order to raise concerns grounded in the daily life of mental health professionals and service users, and to increase public awareness. The experimental dilemmas being proposed served both to advance in knowledge on the social dynamics at play within ‘care in the community’ settings and as a self-reflection experience for all participants. The experimental design process developed in four main phases: (i) identification of the behavioral traits perceived as of fundamental importance within the community, (ii) operationalization of those same behavioral traits thorugh game theoretical paradigms and literature reviews, (iii) definition of the socio-demographic information relevant for the analysis, and (iv) a beta testing of the digital interface (including contents, time duration, and language used). The locations where the experiments took place were accorded with the Catalonia Federation of Mental Health in an attempt to explore the functioning of some communities of interest for inclusive and effective policy making. The Federation provided a fundamental support throughout the whole experiments’ implementation, serving as a crucial intermediaire between the scientists and different mental health collectives. It also provided valuable insights to better interpret the data obtained.
Participants and procedure
To our knowledge, experimental work on this issue has been conducted only recently and on specific collectives of orders of magnitude smaller. A total of 270 individuals participated in the experiments, that were run over 45 sessions between October 2016 and March 2017. The experiments were carried out in Girona (n = 60), Lleida (n = 120), Sabadell (n = 48) and Valls (n = 42). Participants were either diagnosed with a mental condition (n = 169) or members of the broader mental health ecosystem (n = 101), including professionals of the health and social sector (n = 52), formal and informal caregivers (n = 17), relatives (n = 9), friends (n = 4) and other members of the collective (n = 19). Individuals with a mental condition had to self-assess their diagnosis selecting one from a spectrum of options agreed upon with representatives of the mental health ecosystem during the co-design phases of the experiment. Those participants who had received more than one diagnosis had to select the one they considered to be the most relevant. Overall, they had received a diagnosis of psychosis (n = 63), depression (n = 33), anxiety (n = 31), bipolar disorder (n = 17) or other unspecified diagnosis (n = 25). They ranged in age from 21 to 77 years old (these are weighted values since for ethical and privacy reasons participants were only asked to choose among different age ranges) with 47.2 years on average. Further, 55.6% were men and 44.4% were women. Yet, actors involved in the recovery process were predominantly women (76.2%), and up to 21.8% of them was over 60 years old (see Supplementary Section 1.1). Participants were told that they would play against each others a set of games meant to explore human decision-making processes. They played in random groups of six players through a web interface specifically developed for the research. They were informed that they had to make a decision under different conditions and against different opponents in every round. Every game represented an interactive situation requiring the participants to make a decision, the result of which depended also on the opponent’s behavior. To incentivize the participation, they would earn a voucher worth their final score (the experimental settings and instructions, can be found in the Supplementary Section 1.2 and 1.3 respectively). First, participants participated in a Collective Risk Dilemma 23 against five opponents. Briefly, the game is a public goods game with threshold: If the participants’ total contribution after 10 rounds is lower than a given threshold, they loose all the money they kept with a probability of 90%. Otherwise, they are told that the money collected in the common fund are spent in reforesting land plots in Catalonia, where the experimental sessions took place, and each participants earns the money left in the personal account. After completing the task, participants played one round of the Trust Game 38 in both roles: as trustors and as trustees. They played against different partners in each role. Finally, they played one round of a Prisoner Dilemma 39 with (unincentivized) belief elicitation about their counterpart’s behavior prior to playing. Before starting the games, participants had to complete a brief survey covering some key dimensions of their sociodemographic background. The assignment of players’ partners in the dyadic games was completely random and every action was made with a different partner. The average (standard error of the mean) time for completing the three experiments (CRD, PD and TG and tutorials) is around 12 minutes, 705.86 ± 17.93 s. At the end of each session, participants received a gift card worth their earnings. The average individual earning is 46.84 ± 0.77 MUs equivalent to a 4.04 ± 0.077 EUR voucher. The behavioral patterns that emerged do not reveal significant variation across the different experiments, which may suggest that our results are robust to generalizations (see Supplementary Section 1.7).
Statistical analysis
Results were analyzed at two levels: first, we tested for behavioral differences between the whole group of individuals with mental condition compared to members of the mental health ecosystem; we then checked for systematic behavioral variation across diagnostics and role played in the recovery process. In one shot, two-person dyadic interactions we performed Mann-Whitney-U tests for independent groups to compare the distributions of cooperative choices (PD), and initial and back transfers (TG), between individuals with and without a mental condition. We then checked for marginal differences within groups using Kruskal-Wallis tests, and post-hoc comparisons were run with Mann-Whitney-U tests adjusting for p-values with the Holm-Bonferroni method. Welch’s two-tailed t-tests were performed to check for differences in average contributions (CRD) between participants with and without a MD, controlling for unequal variances and sample sizes. Finally, ANOVA and further Tukey HSD post-hoc comparisons served to check for differences in average contributions over round across diagnostics and members of the mental health community.
Accession codes
Data is available in an structured way at Zenodo public repository with DOI 10.5281/zenodo.1175627.
Change history
26 september 2018.
A correction to this article has been published and is linked from the HTML and PDF versions of this paper. The error has not been fixed in the paper.
Steel, Z. et al . The global prevalence of common mental disorders: A systematic review and meta-analysis 1980–2013. Int. J. Epidemiol. 43 , 476–493 (2014).
Article Google Scholar
Insel, T. R., Collins, P. Y. & Hyman, S. E. Darkness invisible: The hidden global costs of mental illness. Foreign Affairs 94 (2015).
White, R. G., Jain, S., Orr, D. M. R. & Read, U. M. The Palgrave handbook of sociocultural perspectives on global mental health. The Palgrave handbook of sociocultural perspectives on global mental health. (2017).
Chapter Google Scholar
World Health Organisation. The World Health Report 2001: mental health, new understanding, new hope. World Health Report 1–169 (2001).
American Psychiatric Association. Diagnostic and statistical manual of mental disorders. Diagnostic and Statistical Manual of Mental Disorders 4th edition TR. (2000).
Gradin, V. B. et al . Abnormal brain responses to social fairness in depression: an fMRI study using the Ultimatum Game. Psychol. Med. 45 , 1241–51 (2015).
Article CAS Google Scholar
Shao, R., Zhang, H. & Lee, T. M. C. The neural basis of social risky decision making in females with major depressive disorder. Neuropsychologia 67 , 100–10 (2015).
Guroglu, B., van den Bos, W., Rombouts, S. A. R. B. & Crone, E. A. Unfair? It depends: Neural correlates of fairness in social context. Soc. Cogn. Affect. Neurosci. 5 , 414–423 (2010).
Wang, Y., Yang, L. –Q., Li, S. & Zhou, Y. Game Theory Paradigm: A New Tool for Investigating Social Dysfunction in Major Depressive Disorders. Front. Psychiatry 6 , 128 (2015).
PubMed PubMed Central Google Scholar
King–Casas, B. & Chiu, P. H. Understanding interpersonal function in psychiatric illness through multiplayer economic games. Biol. Psychiatry 72 , 119–125 (2012).
Pulcu, E. et al . Social–economical decision making in current and remitted major depression. Psychol. Med. 45 , 1–13 (2015).
Wang, Y. et al . Impaired social decision making in patients with major depressive disorder. BMC Psychiatry 14 , 18 (2014).
Csukly, G., Polgár, P., Tombor, L., Réthelyi, J. & Kéri, S. Are patients with schizophrenia rational maximizers? Evidence from an ultimatum game study. Psychiatry Res. 187 , 11–17 (2011).
Agay, N., Kron, S., Carmel, Z., Mendlovic, S. & Levkovitz, Y. Ultimatum bargaining behavior of people affected by schizophrenia. Psychiatry Res. 157 , 39–46 (2008).
Mokros, A. et al . Diminished cooperativeness of psychopaths in a prisoner’s dilemma game yields higher rewards. J. Abnorm. Psychol. 117 , 406–413 (2008).
Rilling, J. K. et al . Neural Correlates of Social Cooperation and Non-Cooperation as a Function of Psychopathy. Biol. Psychiatry 61 , 1260–1271 (2007).
Scheele, D., Mihov, Y., Schwederski, O., Maier, W. & Hurlemann, R. A negative emotional and economic judgment bias in major depression. Eur. Arch. Psychiatry Clin. Neurosci. 263 , 675–683 (2013).
Putnam, R. D. Bowling Aalone: The Collapse and Revival of American Community. J. Democr. 6 , 1–18 (2000).
Google Scholar
Ostrom, E. In Handbook of Social Capital: The troika of sociology, political science and economics, pp. 17–35 (2009).
Sagarra, O., Gutiérrez-Roig, M., Bonhoure, I. & Perelló, J. Citizen science practices for computational social science research: The conceptualization of pop-up experiments. Front. Phys. 3 , 93 (2016).
Camerer, C.F., Behavioral Game Theory: Experiments in Strategic Interaction (Princeton University Press, 2003).
Brañas-Garza, P., Rodríguez-Lara, I. & Sánchez, A. Humans expect generosity. Sci. Rep. 7 , 42446 (2017).
Article ADS Google Scholar
Milinski, M., Sommerfeld, R. D., Krambeck, H.-J., Reed, F. A. & Marotzke, J. The collective-risk social dilemma and the prevention of simulated dangerous climate change. Proc. Nat’l. Acad. Sci. USA 105 , 2291–2294 (2008).
Article ADS CAS Google Scholar
Surbey, M. K. Adaptive significance of low levels of self-deception and cooperation in depression. Evol. Hum. Behav. 32 , 29–40 (2011).
Clark, C. B., Thorne, C. B., Hardy, S. & Cropsey, K. L. Cooperation and depressive symptoms. J. Affect. Disord. 150 , 1184–1187 (2013).
Destoop, M., Schrijvers, D., De Grave, C., Sabbe, B. & De Bruijn, E. R. A. Better to give than to take? Interactive social decision–making in severe major depressive disorder. J. Affect. Disord. 137 , 98–105 (2012).
Harlé, K. M., Allen, J. J. B., Sanfey, A. G., Harlé, K. M. & Sanfey, A. G. The impact of depression on social economic decision making. J. Abnorm. Psychol. 119 , 440–446 (2010).
Unoka, Z., Seres, I., Aspán, N., Bódi, N. & Kéri, S. Trust game reveals restricted interpersonal transactions in patients with borderline personality disorder. J. Pers. Disord. 23 , 399–409 (2009).
King-Casas, B. et al . The rupture and repair of cooperation in borderline personality disorder. Science 321 , 806–810 (2008).
Koenigs, M., Kruepke, M. & Newman, J. P. Economic decision-making in psychopathy: A comparison with ventromedial prefrontal lesion patients. Neuropsychologia 48 , 2198–2204 (2010).
Raihani, N. J. & Bell, V. Paranoia and the social representation of others: a large-scale game theory approach. Scientific Reports 7 , 4544, https://doi.org/10.1038/s41598-017-04805-3 (2017).
Article ADS CAS PubMed PubMed Central Google Scholar
Raihani, N. J. & Bell, V. Conflict and cooperation in paranoia: a large-scale behavioural experiment. Psychological Medicine 1–11, https://doi.org/10.1017/S0033291717003075 (2017).
Collins, L. G. & Swartz, K. Caregiver care. American family physician 83 , 1309–1317 (2011).
PubMed Google Scholar
Aledwood, T. et al . Data collection for mental health studies through digital platforms: requirements and design of a prototype. JMIR research protocols 6 (6), 1–11 (2017).
Blaga, O. M., Vasilescu, L. & Chereches, R. M. Use and effectiveness of behavioural economics in interventions for lifestyle risk factors of non-communicable diseases: a systematic review with policy implications. Perspectives in Public Health 20 (10), 1–11 (2017).
McPherson, K. E. et al . The association between social capital and mental health and behavioural problems in children and adolescents: an integrative systematic review. BMC psychology 2 , 7, https://doi.org/10.1186/2050-7283-2-7 (2014).
Article PubMed PubMed Central Google Scholar
Almedom, A. M. Social capital and mental health: An interdisciplinary review of primary evidence. Social Science and Medicine 61 , 943–964 (2005).
Berg, J., Dickhaut, J. & McCabe, K. Trust, reciprocity, and social history. Games Econ. Behav. 10 , 122–142 (1995).
Rapoport, A. & Chammah, A. M. Prisoner’s Dilemma (University of Michigan Press, 1965).
Vicens, J. et al . Resource heterogeneity leads to unjust effort distribution in climate change mitigation. Preprint at https://arxiv.org/abs/1709.02857 (2017).
Download references
Acknowledgements
We thank the community of patients, caregivers and families working within the Federació de Salut Mental Catalunya (Catalonia Mental Health Federation) for the enthusiasm and for their invaluable help in the design and realization of the experiments. We are also especially thankful to I Bonhoure for the necessary logistics to make the experiments possible, to F Español for contributing in the first steps in the experimental design, to M Poll for always giving us the institutional support from inside the Federation, to both E Ferrer and F Muñoz for building the bridge between us and the mental health ecosystem and to X Trabado for encouraging us to run this research. This work was partially supported by Federació de Salut Mental Catalunya; by MINEICO (Spain), Agencia Estatal de Investigación (AEI) and Fondo Europeo de Desarrollo Regional (FEDER) through grants FIS2013-47532-C3-1-P (JD), FIS2016-78904-C3-1-P (JD), FIS2013-47532-C3-2-P (JP), FIS2016-78904-C3-2-P (JP, AC); by Generalitat de Catalunya (Spain) through Complexity Lab Barcelona (contract no. 2014 SGR 608, JP) and through Secretaria d’Universitats i Recerca (contract no. 2013 DI 49, JD, JV); and by the EU through FET Open Project IBSEN (contract no. 662725, AS) and FET-Proactive Project DOLFINS (contract no. 640772, AS).
Author information
Authors and affiliations.
Departament de Física de la Matèria Condensada, Universitat de Barcelona, 08028, Barcelona, Spain
Anna Cigarini, Julián Vicens & Josep Perelló
Universitat de Barcelona Institute of Complex Systems UBICS, 08028, Barcelona, Spain
Departament d’Enginyeria Informàtica i Matemàtiques, Universitat Rovira i Virgili, 43007, Tarragona, Spain
Julián Vicens & Jordi Duch
Northwestern Institute on Complex Systems (NICO), Northwestern University, 60208, Evanston, IL, USA
Grupo Interdisciplinar de Sistemas Complejos (GISC), Unidad de Matemática, Modelización y Ciencia Computacional, Universidad Carlos III de Madrid, 28911, Leganés, Spain
Angel Sánchez
Unidad Mixta Interdisciplinar de Comportamiento y Complejidad Social (UMICCS) UC3M-UV-UZ, Universidad Carlos III de Madrid, 28911, Leganés, Spain
Institute UC3M-BS of Financial Big Data, Universidad Carlos III de Madrid, 28903, Getafe, Spain
Instituto de Biocomputación y Física de Sistemas Complejos (BIFI), Universidad de Zaragoza, 50009, Zaragoza, Spain
You can also search for this author in PubMed Google Scholar
Contributions
J.D., A.S., and J.P. conceived the original idea for the experiment; J.V. and J.D. prepared the software for the final experimental setup; A.C. and J.V. analyzed the data; and all authors carried out the experiments, discussed the analysis results, and wrote the paper.
Corresponding author
Correspondence to Josep Perelló .
Ethics declarations
Competing interests.
The authors declare no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Supplementary information, rights and permissions.
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/ .
Reprints and permissions
About this article
Cite this article.
Cigarini, A., Vicens, J., Duch, J. et al. Quantitative account of social interactions in a mental health care ecosystem: cooperation, trust and collective action. Sci Rep 8 , 3794 (2018). https://doi.org/10.1038/s41598-018-21900-1
Download citation
Received : 15 November 2017
Accepted : 01 February 2018
Published : 28 February 2018
DOI : https://doi.org/10.1038/s41598-018-21900-1
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Mental Health
- Community Social Capital
- Group Roles
- Dyadic Games
- Average Individual Contribution
This article is cited by
Gender-based pairings influence cooperative expectations and behaviours.
- Anna Cigarini
- Julián Vicens
- Josep Perelló
Scientific Reports (2020)
By submitting a comment you agree to abide by our Terms and Community Guidelines . If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.
Quick links
- Explore articles by subject
- Guide to authors
- Editorial policies
Sign up for the Nature Briefing: AI and Robotics newsletter — what matters in AI and robotics research, free to your inbox weekly.
- Systematic review
- Open access
- Published: 10 October 2019
An integrative review on methodological considerations in mental health research – design, sampling, data collection procedure and quality assurance
- Eric Badu ORCID: orcid.org/0000-0002-0593-3550 1 ,
- Anthony Paul O’Brien 2 &
- Rebecca Mitchell 3
Archives of Public Health volume 77 , Article number: 37 ( 2019 ) Cite this article
24k Accesses
20 Citations
1 Altmetric
Metrics details
Several typologies and guidelines are available to address the methodological and practical considerations required in mental health research. However, few studies have actually attempted to systematically identify and synthesise these considerations. This paper provides an integrative review that identifies and synthesises the available research evidence on mental health research methodological considerations.
A search of the published literature was conducted using EMBASE, Medline, PsycINFO, CINAHL, Web of Science, and Scopus. The search was limited to papers published in English for the timeframe 2000–2018. Using pre-defined inclusion and exclusion criteria, three reviewers independently screened the retrieved papers. A data extraction form was used to extract data from the included papers.
Of 27 papers meeting the inclusion criteria, 13 focused on qualitative research, 8 mixed methods and 6 papers focused on quantitative methodology. A total of 14 papers targeted global mental health research, with 2 papers each describing studies in Germany, Sweden and China. The review identified several methodological considerations relating to study design, methods, data collection, and quality assurance. Methodological issues regarding the study design included assembling team members, familiarisation and sharing information on the topic, and seeking the contribution of team members. Methodological considerations to facilitate data collection involved adequate preparation prior to fieldwork, appropriateness and adequacy of the sampling and data collection approach, selection of consumers, the social or cultural context, practical and organisational skills; and ethical and sensitivity issues.
The evidence confirms that studies on methodological considerations in conducting mental health research largely focus on qualitative studies in a transcultural setting, as well as recommendations derived from multi-site surveys. Mental health research should adequately consider the methodological issues around study design, sampling, data collection procedures and quality assurance in order to maintain the quality of data collection.
Peer Review reports
In the past decades there has been considerable attention on research methods to facilitate studies in various academic fields, such as public health, education, humanities, behavioural and social sciences [ 1 , 2 , 3 , 4 ]. These research methodologies have generally focused on the two major research pillars known as quantitative or qualitative research. In recent years, researchers conducting mental health research appear to be either employing both qualitative and quantitative research methods separately, or mixed methods approaches to triangulate and validate findings [ 5 , 6 ].
A combination of study designs has been utilised to answer research questions associated with mental health services and consumer outcomes [ 7 , 8 ]. Study designs in the public health and clinical domains, for example, have largely focused on observational studies (non-interventional) and experimental research (interventional) [ 1 , 3 , 9 ]. Observational design in non-interventional research requires the investigator to simply observe, record, classify, count and analyse the data [ 1 , 2 , 10 ]. This design is different from the observational approaches used in social science research, which may involve observing (participant and non- participant) phenomena in the fieldwork [ 1 ]. Furthermore, the observational study has been categorized into five types, namely cross-sectional design, case-control studies, cohort studies, case report and case series studies [ 1 , 2 , 3 , 9 , 10 , 11 ]. The cross-sectional design is used to measure the occurrence of a condition at a one-time point, sometimes referred to as a prevalence study. This approach of conducting research is relatively quick and easy but does not permit a distinction between cause and effect [ 1 ]. Conversely, the case-control is a design that examines the relationship between an attribute and a disease by comparing those with and without the disease [ 1 , 2 , 12 ]. In addition, the case-control design is usually retrospective and aims to identify predictors of a particular outcome. This type of design is relevant when investigating rare or chronic diseases which may result from long-term exposure to particular risk factors [ 10 ]. Cohort studies measure the relationship between exposure to a factor and the probability of the occurrence of a disease [ 1 , 10 ]. In a case series design, medical records are reviewed for exposure to determinants of disease and outcomes. More importantly, case series and case reports are often used as preliminary research to provide information on key clinical issues [ 12 ].
The interventional study design describes a research approach that applies clinical care to evaluate treatment effects on outcomes [ 13 ]. Several previous studies have explained the various forms of experimental study design used in public health and clinical research [ 14 , 15 ]. In particular, experimental studies have been categorized into randomized controlled trials (RCTs), non-randomized controlled trials, and quasi-experimental designs [ 14 ]. The randomized trial is a comparative study where participants are randomly assigned to one of two groups. This research examines a comparison between a group receiving treatment and a control group receiving treatment as usual or receiving a placebo. Herein, the exposure to the intervention is determined by random allocation [ 16 , 17 ].
Recently, research methodologists have given considerable attention to the development of methodologies to conduct research in vulnerable populations. Vulnerable population research, such as with mental health consumers often involves considering the challenges associated with sampling (selecting marginalized participants), collecting data and analysing it, as well as research engagement. Consequently, several empirical studies have been undertaken to document the methodological issues and challenges in research involving marginalized populations. In particular, these studies largely addresses the typologies and practical guidelines for conducting empirical studies in mental health. Despite the increasing evidence, however, only a few studies have yet attempted to systematically identify and synthesise the methodological considerations in conducting mental health research from the perspective of consumers.
A preliminary search using the search engines Medline, Web of Science, Google Scholar, and Scopus Index and EMBASE identified only two reviews of mental health based research. Among these two papers, one focused on the various types of mixed methods used in mental health research [ 18 ], whilst the other paper, focused on the role of qualitative studies in mental health research involving mixed methods [ 19 ]. Even though the latter two studies attempted to systematically review mixed methods mental health research, this integrative review is unique, as it collectively synthesises the design, data collection, sampling, and quality assurance issues together, which has not been previously attempted.
This paper provides an integrative review addressing the available evidence on mental health research methodological considerations. The paper also synthesises evidence on the methods, study designs, data collection procedures, analyses and quality assurance measures. Identifying and synthesising evidence on the conduct of mental health research has relevance to clinicians and academic researchers where the evidence provides a guide regarding the methodological issues involved when conducting research in the mental health domain. Additionally, the synthesis can inform clinicians and academia about the gaps in the literature related to methodological considerations.
Methodology
An integrative review was conducted to synthesise the available evidence on mental health research methodological considerations. To guide the review, the World Health Organization (WHO) definition of mental health has been utilised. The WHO defines mental health as: “a state of well-being, in which the individual realises his or her own potentials, ability to cope with the normal stresses of life, functionality and work productivity, as well as the ability to contribute effectively in community life” [ 20 ]. The integrative review enabled the simultaneous inclusion of diverse methodologies (i.e., experimental and non-experimental research) and varied perspectives to fully understand a phenomenon of concern [ 21 , 22 ]. The review also uses diverse data sources to develop a holistic understanding of methodological considerations in mental health research. The methodology employed involves five stages: 1) problem identification (ensuring that the research question and purpose are clearly defined); 2) literature search (incorporating a comprehensive search strategy); 3) data evaluation; 4) data analysis (data reduction, display, comparison and conclusions) and; 5) presentation (synthesising findings in a model or theory and describing the implications for practice, policy and further research) [ 21 ].
Inclusion criteria
The integrative review focused on methodological issues in mental health research. This included core areas such as study design and methods, particularly qualitative, quantitative or both. The review targeted papers that addressed study design, sampling, data collection procedures, quality assurance and the data analysis process. More specifically, the included papers addressed methodological issues on empirical studies in mental health research. The methodological issues in this context are not limited to a particular mental illness. Studies that met the inclusion criteria were peer-reviewed articles published in the English Language, from January 2000 to July 2018.
Exclusion criteria
Articles that were excluded were based purely on general health services or clinical effectiveness of a particular intervention with no connection to mental health research. Articles were also excluded when it addresses non-methodological issues. Other general exclusion criteria were book chapters, conference abstracts, papers that present opinion, editorials, commentaries and clinical case reviews.
Search strategy and selection procedure
The search of published articles was conducted from six electronic databases, namely EMBASE, CINAHL (EBSCO), Web of Science, Scopus, PsycINFO and Medline. We developed a search strategy based on the recommended guidelines by the Joanna Briggs Institute (JBI) [ 23 ]. Specifically, a three-step search strategy was utilised to conduct the search for information (see Table 1 ). An initial limited search was conducted in Medline and Embase (see Table 1 ). We analysed the text words contained in the title and abstract and of the index terms from the initial search results [ 23 ]. A second search using all identified keywords and index terms was then repeated across all remaining five databases (see Table 1 ). Finally, the reference lists of all eligible studies were manually hand searched [ 23 ].
The selection of eligible articles adhered to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) [ 24 ] (see Fig. 1 ). Firstly, three authors independently screened the titles of articles that were retrieved and then approved those meeting the selection criteria. The authors reviewed all the titles and abstracts and agreed on those needing full-text screening. E.B (Eric Badu) conducted the initial screening of titles and abstracts. A.P.O’B (Anthony Paul O’Brien) and R.M (Rebecca Mitchell) conducted the second screening of titles and abstracts of all the identified papers. The authors (E.B, A.P.O’B and R.M) conducted full-text screening according to the inclusion and exclusion criteria.
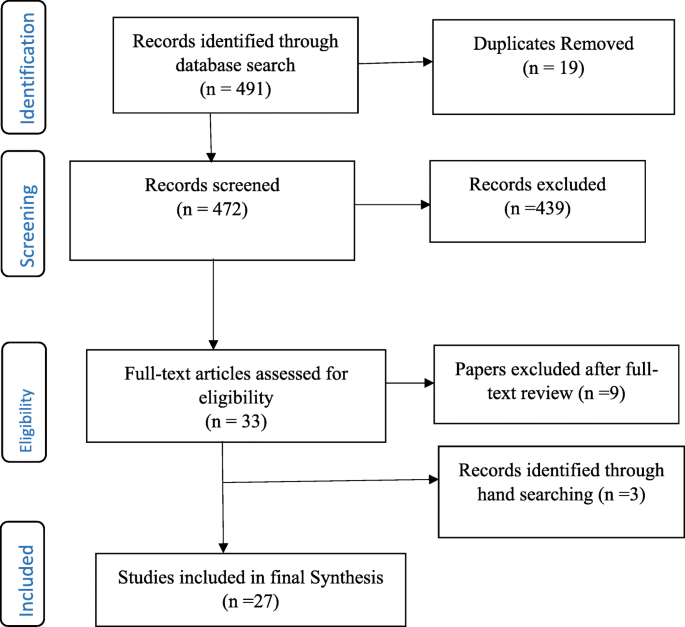
Flow Chart of studies included in the review
Data management and extraction
The integrative review used Endnote ×8 to screen and handle duplicate references. A predefined data extraction form was developed to extract data from all included articles (see Additional file 1 ). The data extraction form was developed according to Joanna Briggs Institute (JBI) [ 23 ] and Cochrane [ 24 ] manuals, as well as the literature associated with concepts and methods in mental health research. The data extraction form was categorised into sub-sections, such as study details (citation, year of publication, author, contact details of lead author, and funder/sponsoring organisation, publication type), objective of the paper, primary subject area of the paper (study design, methods, sampling, data collection, data analysis, quality assurance). The data extraction form also had a section on additional information on methodological consideration, recommendations and other potential references. The authors extracted results of the included papers in numerical and textual format [ 23 ]. EB (Eric Badu) conducted the data extraction, A.P.O’B (Anthony Paul O’Brien) and R.M (Rebecca Mitchell), conducted the second review of the extracted data.
Data synthesis
Content analysis was used to synthesise the extracted data. The content analysis process involved several stages which involved noting patterns and themes, seeing plausibility, clustering, counting, making contrasts and comparisons, discerning common and unusual patterns, subsuming particulars into general, noting relations between variability, finding intervening factors and building a logical chain of evidence [ 21 ] (see Table 2 ).
Study characteristics
The integrative review identified a total of 491 records from all databases, after which 19 duplicates were removed. Out of this, 472 titles and abstracts were assessed for eligibility, after which 439 articles were excluded. Articles not meeting the inclusion criteria were excluded. Specifically, papers excluded were those that did not address methodological issues as well as papers addressing methodological consideration in other disciplines. A total of 33 full-text articles were assessed – 9 articles were further excluded, whilst an additional 3 articles were identified from reference lists. Overall, 27 articles were included in the final synthesis (see Fig. 1 ). Of the total included papers, 12 contained qualitative research, 9 were mixed methods (both qualitative and quantitative) and 6 papers focused on quantitative data. Conversely, a total of 14 papers targeted global mental health research and 2 papers each describing studies in Germany, Sweden and China. The papers addressed different methodological issues, such as study design, methods, data collection, and analysis as well as quality assurance (see Table 3 ).
Mixed methods design in mental health research
Mixed methods research is defined as a research process where the elements of qualitative and quantitative research are combined in the design, data collection, and its triangulation and validation [ 48 ]. The integrative review identified four sub-themes that describe mixed methods design in the context of mental health research. The sub-themes include the categories of mixed methods, their function, structure, process and further methodological considerations for mixed methods design. These sub-themes are explained as follows:
Categorizing mixed methods in mental health research
Four studies highlighted the categories of mixed methods design applicable to mental health research [ 18 , 19 , 43 , 48 ]. Generally, there are differences in the categories of mixed methods design, however, three distinct categories predominantly appear to cross cut in all studies. These categories are function, structure and process. Some studies further categorised mixed method design to include rationale, objectives, or purpose. For instance, Schoonenboom and Johnson [ 48 ] categorised mixed methods design into primary and secondary dimensions.
The function of mixed methods in mental health research
Six studies explain the function of conducting mixed methods design in mental health research. Two studies specifically recommended that mixed methods have the ability to provide a more robust understanding of services by expanding and strengthening the conclusions from the study [ 42 , 45 ]. More importantly, the use of both qualitative and quantitative methods have the ability to provide innovative solutions to important and complex problems, especially by addressing diversity and divergence [ 48 ]. The review identified five underlying functions of a mixed method design in mental health research which include achieving convergence, complementarity, expansion, development and sampling [ 18 , 19 , 43 ].
The use of mixed methods to achieve convergence aims to employ both qualitative and quantitative data to answer the same question, either through triangulation (to confirm the conclusions from each of the methods) or transformation (using qualitative techniques to transform quantitative data). Similarly, complementarity in mixed methods integrates both qualitative and quantitative methods to answer questions for the purpose of evaluation or elaboration [ 18 , 19 , 43 ]. Two papers recommend that qualitative methods are used to provide the depth of understanding, whilst the quantitative methods provide a breadth of understanding [ 18 , 43 ]. In mental health research, the qualitative data is often used to examine treatment processes, whilst the quantitative methods are used to examine treatment outcomes against quality care key performance targets.
Additionally, three papers indicated that expansion as a function of mixed methods uses one type of method to answer questions raised by the other type of method [ 18 , 19 , 43 ]. For instance, qualitative data is used to explain findings from quantitative analysis. Also, some studies highlight that development as a function of mixed methods aims to use one method to answer research questions, and use the findings to inform other methods to answer different research questions. A qualitative method, for example, is used to identify the content of items to be used in a quantitative study. This approach aims to use qualitative methods to create a conceptual framework for generating hypotheses to be tested by using a quantitative method [ 18 , 19 , 43 ]. Three papers suggested that using mixed methods for the purpose of sampling utilize one method (eg. quantitative) to identify a sample of participants to conduct research using other methods (eg. qualitative) [ 18 , 19 , 43 ]. For instance, quantitative data is sequentially utilized to identify potential participants to participate in a qualitative study and the vice versa.
Structure of mixed methods in mental health research
Five studies categorised the structure of conducting mixed methods in mental health research, into two broader concepts including simultaneous (concurrent) and sequential (see Table 3 ). In both categories, one method is regarded as primary and the other as secondary, although equal weight can be given to both methods [ 18 , 19 , 42 , 43 , 48 ]. Two studies suggested that the sequential design is a process where the data collection and analysis of one component (eg. quantitative) takes place after the data collection and analysis of the other component (eg qualitative). Herein, the data collection and analysis of one component (e.g. qualitative) may depend on the outcomes of the other component (e.g. quantitative) [ 43 , 48 ]. An earlier review suggested that the majority of contemporary studies in mental health research use a sequential design, with qualitative methods, more often preceding quantitative methods [ 18 ].
Alternatively, the concurrent design collects and analyses data of both components (e.g. quantitative and qualitative) simultaneously and independently. Palinkas, Horwitz [ 42 ] recommend that one component is used as secondary to the other component, or that both components are assigned equal priority. Such a mixed methods approach aims to provide a depth of understanding afforded by qualitative methods, with the breadth of understanding offered by the quantitative data to elaborate on the findings of one component or seek convergence through triangulation of the results. Schoonenboom and Johnson [ 48 ] recommended the use of capital letters for one component and lower case letters for another component in the same design to indicate that one component is primary and the other is secondary or supplemental.
Process of mixed methods in mental health research
Five papers highlighted the process for the use of mixed methods in mental health research [ 18 , 19 , 42 , 43 , 48 ]. The papers suggested three distinct processes or strategies for combining qualitative and quantitative data. These include merging or converging the two data sets, connecting the two datasets by having one build upon the other; and embedding one data set within the other [ 19 , 43 ]. The process of connecting occurs when the analysis of one dataset leads to the need for the other data set. For instance, in the situation where quantitative results lead to the subsequent collection and analysis of qualitative data [ 18 , 43 ]. A previous study suggested that most studies in mental health sought to connect the data sets. Similarly, the process of merging the datasets brings together two sets of data during the interpretation, or transforms one type of data into the other type, by combining the data into new variables [ 18 ]. The process of embedding data into mixed method designs in mental health uses one dataset to provide a supportive role to the other dataset [ 43 ].
Consideration for using mixed methods in mental health research
Three studies highlighted several factors that need to be considered when conducting mixed methods design in mental health research [ 18 , 19 , 45 ]. Accordingly, these factors include developing familiarity with the topic under investigation based on experience, willingness to share information on the topic [ 19 ], establishing early collaboration, willingness to negotiate emerging problems, seeking the contribution of team members, and soliciting third-party assistance to resolve any emerging problems [ 45 ]. Additionally, Palinkas, Horwitz [ 18 ] recommended that mixed methods in the context of mental health research are mostly applied in studies that assess needs of services, examine existing services, developing new or adapting existing services, evaluating services in randomised control trials, and examining service implementation.
Qualitative study in mental health research
This theme describes the various qualitative methods used in mental health research. The theme also addresses methodological considerations for using qualitative methods in mental health research. The key emerging issues are discussed below:
Considering qualitative components in conducting mental health research
Six studies recommended the use of qualitative methods in mental health research [ 19 , 26 , 28 , 32 , 36 , 44 ]. Two qualitative research paradigms were identified, including the interpretive and critical approach [ 32 ]. The interpretive methodologies predominantly explore the meaning of human experiences and actions, whilst the critical approach emphasises the social and historical origins and contexts of meaning [ 32 ]. Two studies suggested that the interpretive qualitative methods used in mental health research are ethnography, phenomenology and narrative approaches [ 32 , 36 ].
The ethnographic approach describes the everyday meaning of the phenomena within a societal and cultural context, for instance, the way phenomena or experience is contrasted within a community, or by collective members over time [ 32 ]. Alternatively, the phenomenological approach explores the claims and concerns of a subject with a speculative development of an interpretative account within their cultural and physical environments focusing on the lived experience [ 32 , 36 ].
Moreover, the critical qualitative approaches used in mental health research are predominantly emancipatory (for instance, socio-political traditions) and participatory action-based research. The emancipatory traditions recognise that knowledge is acquired through critical discourse and debate but are not seen as discovered by objective inquiry [ 32 ]. Alternatively, the participatory action based approach uses critical perspectives to engage key stakeholders as participants in the design and conduct of the research [ 32 ].
Some studies highlighted several reasons why qualitative methods are relevant to mental health research. In particular, qualitative methods are significant as they emphasise naturalistic inquiry and have a discovery-oriented approach [ 19 , 26 ]. Two studies suggested that qualitative methods are often relevant in the initial stages of research studies to understand specific issues such as behaviour, or symptoms of consumers of mental services [ 19 ]. Specifically, Palinkas [ 19 ] suggests that qualitative methods help to obtain initial pilot data, or when there is too little previous research or in the absence of a theory, such as provided in exploratory studies, or previously under-researched phenomena.
Three studies stressed that qualitative methods can help to better understand socially sensitive issues, such as exploring the solutions to overcome challenges in mental health clinical policies [ 19 , 28 , 44 ]. Consequently, Razafsha, Behforuzi [ 44 ] recommended that the natural holistic view of qualitative methods can help to understand the more recovery-oriented policy of mental health, rather than simply the treatment of symptoms. Similarly, the subjective experiences of consumers using qualitative approaches have been found useful to inform clinical policy development [ 28 ].
Sampling in mental health research
The theme explains the sampling approaches used in mental health research. The section also describes the methodological considerations when sampling participants for mental health research. The sub-themes emerging are explained in the following sections:
Sampling approaches (quantitative)
Some studies reviewed highlighted the sampling approaches previously used in mental health research [ 25 , 34 , 35 ]. Generally, all quantitative studies tend to use several probability sampling approaches, whilst qualitative studies used non-probability techniques. The quantitative mental health studies conducted at community and population level employ multi-stage sampling techniques usually involving systematic sampling, stratified and random sampling [ 25 , 34 ]. Similarly, quantitative studies that recruit consumers in the hospital setting employ consecutive sampling [ 35 ]. Two studies reviewed highlighted that the identification of consumers of mental health services for research is usually conducted by service providers. For instance, Korver, Quee [ 35 ] research used a consecutive sampling approach by identifying consumers through clinicians working in regional psychosis departments, or academic centres.
Sampling approaches (qualitative)
Seven studies suggested that the sampling procedures widely used in mental health research involving qualitative methods are non-probability techniques, which include purposive [ 19 , 28 , 32 , 42 , 46 ], snowballing [ 30 , 32 , 46 ] and theoretical sampling [ 31 , 32 ]. The purposive sampling identifies participants that possess relevant characteristics to answer a research question [ 28 ]. Purposive sampling can be used in a single case study, or for multiple cases. The purposive sampling used in mental health research is usually extreme, or deviant case sampling, criterion sampling, and maximum variation sampling [ 19 ]. Furthermore, it is advised when using purposive sampling in a multistage level study, that it should aim to begin with the broader picture to achieve variation, or dispersion, before moving to the more focused view that considers similarity, or central tendencies [ 42 ].
Two studies added that theoretical sampling involved sampling participants, situations and processes based on concepts on theoretical grounds and then using the findings to build theory, such as in a Grounded Theory study [ 31 , 32 ]. Some studies highlighted that snowball sampling is another strategy widely used in mental health research [ 30 , 32 , 46 ]. This is ascribed to the fact that people with mental illness are perceived as marginalised in research and practically hard-to-reach using conventional sampling [ 30 , 32 ]. Snowballing sampling involves asking the marginalised participants to recommend individuals who might have direct knowledge relevant to the study [ 30 , 32 , 46 ]. Although this approach is relevant, some studies advise the limited possibility of generalising the sample, because of the likelihood of selection bias [ 30 ].
Sampling consideration
Four studies in this section highlighted some of the sampling considerations in mental health research [ 30 , 31 , 32 , 46 ]. Generally, mental health research should consider the appropriateness and adequacy of sampling approach by applying attributes such as shared social, or cultural experiences, or shared concern related to the study [ 32 ], diversity and variety of participants [ 31 ], practical and organisational skills, as well as ethical and sensitivity issues [ 46 ]. Robinson [ 46 ] further suggested that sampling can be homogenous or heterogeneous depending on the research questions for the study. Achieving homogeneity in sampling should employ a variety of parameters, which include demographic, graphical, physical, psychological, or life history homogeneity [ 46 ]. Additionally, applying homogeneity in sampling can be influenced by theoretical and practical factors. Alternatively, some samples are intentionally selected based on heterogeneous factors [ 46 ].
Data collection in mental health research
This theme highlights the data collection methods used in mental health research. The theme is explained according to three sub-themes, which include approaches for collecting qualitative data, methodological considerations, as well as preparations for data collection. The sub-themes are as follows:
Approaches for collecting qualitative data
The studies reviewed recommended the approaches that are widely applied in collecting data in mental health research. The widely used qualitative data collection approaches in mental health research are focus group discussions (FGDs) [ 19 , 28 , 30 , 31 , 41 , 44 , 47 ], extended in-depth interviews [ 19 , 30 , 34 ], participant and non-participant observation [ 19 ], Delphi data collection, quasi-statistical techniques [ 19 ] and field notes [ 31 , 40 ]. Seven studies suggest that FGDs are widely used data collection approaches [ 19 , 28 , 30 , 31 , 41 , 44 , 47 ] because they are valuable in gathering information on consumers’ perspectives of services, especially regarding satisfaction, unmet/met service needs and the perceived impact of services [ 47 ]. Conversely, Ekblad and Baarnhielm [ 31 ] recommended that this approach is relevant to improve clinical understanding of the thoughts, emotions, meanings and attitudes towards mental health services.
Such data collection approaches are particularly relevant to consumers of mental health services, due to their low self-confidence and self-esteem [ 41 ]. The approach can help to understand specific terms, vocabulary, opinions and attitudes of consumers of mental health services, as well as their reasoning about personal distress and healing [ 31 ]. Similarly, the reliance on verbal rather than written communication helps to promote the participation of participants with serious and enduring mental health problems [ 31 , 41 ]. Although FGD has several important outcomes, there are some limitations that need critical consideration. Ekblad and Baarnhielm [ 31 ] for example suggest, that marginalised participants may not always feel free to talk about private issues regarding their condition at the group level mostly due to perceived stigma and group confidentiality.
Some studies reviewed recommended that attempting to capture comprehensive information and analysing group interactions in mental health research requires the research method to use field notes as a supplementary data source to help validate the FGDs [ 31 , 40 , 41 ]. The use of field notes in addition to FGDs essentially provides greater detail in the accounts of consumers’ subjective experiences. Furthermore, Montgomery and Bailey [ 40 ] suggest that field notes require observational sensitivity, and also require having specific content such as descriptive and interpretive data.
Three studies in this section suggested that in-depth interviews are used to collect data from consumers of mental health services [ 19 , 30 , 34 ]. This approach is particularly important to explore the behaviour, subjective experiences and psychological processes; opinions, and perceptions of mental health services. de Jong and Van Ommeren [ 30 ] recommend that in-depth interviews help to collect data on culturally marked disorders, their personal and interpersonal significance, patient and family explanatory models, individual and family coping styles, symptom symbols and protective mediators. Palinkas [ 19 ] also highlights that the structured narrative form of extended interviewing is the type of in-depth interview used in mental health research. This approach provides participants with the opportunity to describe the experience of living with an illness and seeking services that assist them.
Consideration for data collection
Six studies recommended consideration required in the data collection process [ 31 , 32 , 37 , 41 , 47 , 49 ]. Some studies highlighted that consumers of mental health services might refuse to participate in research due to several factors [ 37 ] like the severity of their illness, stigma and discrimination [ 41 ]. Subsequently, such issues are recommended to be addressed by building confidence and trust between the researcher and consumers [ 31 , 37 ]. This is a significant prerequisite, as it can sensitise and normalise the research process and aims with the participants prior to discussing their personal mental health issues. Similarly, some studies added that the researcher can gain the confidence of service providers who manage consumers of mental health services [ 41 , 47 ], seek ethical approval from the relevant committee(s) [ 41 , 47 ], meet and greet the consumers of mental health services before data collection, and arrange a mutually acceptable venue for the groups and possibly supply transport [ 41 ].
Two studies further suggested that the cultural and social differences of the participants need consideration [ 26 , 31 ]. These factors could influence the perception and interpretation of ethical issues in the research situation.
Additionally, two studies recommended the use of standardised assessment instruments for mental health research that involve quantitative data collection [ 33 , 49 ]. A recent survey suggested that measures to standardise the data collection approach can convert self-completion instruments to interviewer-completion instruments [ 49 ]. The interviewer can then read the items of the instruments to respondents and record their responses. The study further suggested the need to collect demographic and behavioural information about the participant(s).
Preparing for data collection
Eight studies highlighted the procedures involved in preparing for data collection in mental health research [ 25 , 30 , 33 , 34 , 35 , 39 , 41 , 49 ]. These studies suggest that the preparation process involve organising meetings of researchers, colleagues and representatives of the research population. The meeting of researchers generally involves training of interviewers about the overall design, objectives and research questions associated with the study. de Jong and Van Ommeren [ 30 ] recommended that preparation for the use of quantitative data encompasses translating and adapting instruments with the aim of achieving content, semantic, concept, criterion and technical equivalence.
Quality assurance procedures in mental health research
This section describes the quality assurance procedures used in mental health research. Quality assurance is explained according to three sub-themes: 1) seeking informed consent, 2) the procedure for ensuring quality assurance in a quantitative study and 3) the procedure for ensuring quality control in a qualitative study. The sub-themes are explained in the following content.
Seeking informed consent
The papers analysed for the integrative review suggested that the rights of participants to safeguard their integrity must always be respected, and so each potential subject must be adequately informed of the aims, methods, anticipated benefits and potential hazards of the study and any potential discomforts (see Table 3 ). Seven studies highlight that potential participants of mental health research must be consented to the study prior to data collection [ 25 , 26 , 33 , 35 , 37 , 39 , 47 ]. The consent process helps to assure participants of anonymity and confidentiality and further explain the research procedure to them. Baarnhielm and Ekblad [ 26 ] argue that the research should be guided by four basic moral values for medical ethics, autonomy, non-maleficence, beneficence, and justice. In particular, potential consumers of mental health services who may have severe conditions and unable to consent themselves are expected to have their consent signed by a respective family caregiver [ 37 ]. Latvala, Vuokila-Oikkonen [ 37 ] further suggested that researchers are responsible to agree on the criteria to determine the competency of potential participants in mental health research. The criteria are particularly relevant when potential participants have difficulties in understanding information due to their mental illness.
Procedure for ensuring quality control (quantitative)
Several studies highlighted procedures for ensuring quality control in mental health research (see Table 3 ). The quality control measures are used to achieve the highest reliability, validity and timeliness. Some studies demonstrate that ensuring quality control should consider factors such as pre-testing tools [ 25 , 49 ], minimising non-response rates [ 25 , 39 ] and monitoring of data collection processes [ 25 , 33 , 49 ].
Accordingly, two studies suggested that efforts should be made to re-approach participants who initially refuse to participate in the study. For instance, Liu, Huang [ 39 ] recommended that when a consumer of mental health services refuse to participate in a study (due to low self-esteem) when approached for the first time, a different interviewer can re-approach the same participant to see if they are more comfortable to participate after the first invitation. Three studies further recommend that monitoring data quality can be accomplished through “checks across individuals, completion status and checks across variables” [ 25 , 33 , 49 ]. For example, Alonso, Angermeyer [ 25 ] advocate that various checks are used to verify completion of the interview, and consistency across instruments against the standard procedure.
Procedure for ensuring quality control (qualitative)
Four studies highlighted the procedures for ensuring quality control of qualitative data in mental health research [ 19 , 32 , 37 , 46 ]. A further two studies suggested that the quality of qualitative research is governed by the principles of credibility, dependability, transferability, reflexivity, confirmability [ 19 , 32 ]. Some studies explain that the credibility or trustworthiness of qualitative research in mental health is determined by methodological and interpretive rigour of the phenomenon being investigated [ 32 , 37 ]. Consequently, Fossey, Harvey [ 32 ] propose that the methodological rigour for assessing the credibility of qualitative research are congruence, responsiveness or sensitivity to social context, appropriateness (importance and impact), adequacy and transparency. Similarly, interpretive rigour is classified as authenticity, coherence, reciprocity, typicality and permeability of the researcher’s intentions; including engagement and interpretation [ 32 ].
Robinson [ 46 ] explained that transparency (openness and honesty) is achieved if the research report explicitly addresses how the sampling, data collection, analysis, and presentation are met. In particular, efforts to address these methodological issues highlight the extent to which the criteria for quality profoundly interacts with standards for ethics. Similarly, responsiveness, or sensitivity, helps to situate or locate the study within a place, a time and a meaningful group [ 46 ]. The study should also consider the researcher’s background, location and connection to the study setting, particularly in the recruitment process. This is often described as role conflict or research bias.
In the interpretive phenomenon, coherence highlights the ability to select an appropriate sampling procedure that mutually matches the research aims, questions, data collection, analysis, as well as any theoretical concepts or frameworks [ 32 , 46 ]. Similarly, authenticity explains the appropriate representation of participants’ perspectives in the research process and the interpretation of results. Authenticity is maximised by providing evidence that participants are adequately represented in the interpretive process, or provided an opportunity to give feedback on the researcher’s interpretation [ 32 ]. Again, the contribution of the researcher’s perspective to the interpretation enhances permeability. Fossey, Harvey [ 32 ] further suggest that reflexive reporting, which distinguishes the participants’ voices from that of the researcher in the report, enhances the permeability of the researcher’s role and perspective.
One study highlighted the approaches used to ensure validity in qualitative research, which includes saturation, identification of deviant or non-confirmatory cases, member checking and coding by consensus. Saturation involves completeness in the research process, where all relevant data collection, codes and themes required to answer the phenomenon of inquiry are achieved; and no new data emerges [ 19 ]. Similarly, member checking is the process whereby participants or others who share similar characteristics review study findings to elaborate on confirming them [ 19 ]. The coding by consensus involves a collaborative approach to analysing the data. Ensuring regular meetings among coders to discuss procedures for assigning codes to segments of data and resolve differences in coding procedures, and by comparison of codes assigned on selected transcripts to calculate a percentage agreement or kappa measure of interrater reliability, are commonly applied [ 19 ].
Two studies recommend the need to acknowledge the importance of generalisability (transferability). This concept aims to provide sufficient information about the research setting, findings and interpretations for readers to appropriately determine the replicability of the findings from one context, or population to another, otherwise known as reliability in quantitative research [ 19 , 32 ]. Similarly, the researchers should employ reflexivity as a means of identifying and addressing potential biases in data collection and interpretation. Palinkas [ 19 ] suggests that such bias is associated with theoretical orientations; pre-conceived beliefs, assumptions, and demographic characteristics; and familiarity and experience with the methods and phenomenon. Another approach to enhance the rigour of analysis involves peer debriefing and support meetings held among team members which facilitate detailed auditing during data analysis [ 19 ].
The integrative review was conducted to synthesise evidence into recommended methodological considerations when conducting mental health research. The evidence from the review has been discussed according to five major themes: 1) mixed methods study in mental health research; 2) qualitative study in mental health research; 3) sampling in mental health research; 4) data collection in mental health research; and 5) quality assurance procedures in mental health research.
Mixed methods study in mental health research
The evidence suggests that mixed methods approach in mental health are generally categorised according to their function (rationale, objectives or purpose), structure and process [ 18 , 19 , 43 , 48 ]. The mixed methods study can be conducted for the purpose of achieving convergence, complementarity, expansion, development and sampling [ 18 , 19 , 43 ]. Researchers conducting mental health studies should understand the underlying functions or purpose of mixed methods. Similarly, mixed methods in mental health studies can be structured simultaneously (concurrent) and sequential [ 18 , 19 , 42 , 43 , 48 ]. More importantly, the process of combining qualitative and quantitative data can be achieved through merging or converging, connecting and embedding one data set within the other [ 18 , 19 , 42 , 43 , 48 ]. The evidence further recommends that researchers need to understand the stage of integrating the two sets of data and the rationale for doing so. This can inform researchers regarding the best stage and appropriate ways of combining the two components of data to adequately address the research question(s).
The evidence recommended some methodological consideration in the design of mixed methods projects in mental health [ 18 , 19 , 45 ]. These issues include establishing early collaboration, becoming familiar with the topic, sharing information on the topic, negotiating any emerging problems and seeking contributions from team members. The involvement of various expertise could ensure that methodological issues are clearly identified. However, addressing such issues midway, or late through the design can negatively affect the implementation [ 45 ]. Any robust discoveries can rarely be accommodated under the existing design. Therefore, the inclusion of various methodological expertise during inception can lead to a more robust mixed-methods design which maximises the contributions of team members. Whilst fundamental and philosophical differences in qualitative and quantitative methods may not be resolved, some workable solutions can be employed, particularly if challenges are viewed as philosophical rather than personal [ 45 ]. The cultural issues can be alleviated by understanding the concepts, norms and values of the setting, further to respecting and including perspectives of the various stakeholders.
The review findings suggest that qualitative methods are relevant when conducting mental health research. The qualitative methods are mostly used where there has been limited previous research and an absence of theoretical perspectives. The approach is also used to gather initial pilot data. More importantly, the qualitative methods are relevant when we want to understand sensitive issues, especially from consumers of mental health services, where the ‘lived experience is paramount [ 19 , 28 , 44 ]. Qualitative methods can help understand the experiences of consumers in the process of treatment, as well as their therapeutic relationship with mental health professionals. The experiences of consumers from qualitative data are particularly important in developing clinical policy [ 28 ]. The review findings find two paradigms of qualitative methods are used in mental health research. These paradigms are the interpretive and critical approach [ 32 ]. The interpretive qualitative method(s) include phenomenology, ethnography and narrative approaches [ 32 , 36 ]. Conversely, critical qualitative approaches are participatory action research and emancipatory approach. The review findings suggest that these approaches to qualitative methods need critical considerations, particularly when dealing with consumers of mental health services.
The review findings identified several sampling techniques used in mental health research. Quantitative studies, usually employ probability sampling, whilst qualitative studies use non-probability sampling [ 25 , 34 ]. The most common sampling techniques for quantitative studies are multi-stage sampling, which involves systematic, stratified, random sampling and consecutive sampling. In contrast, the predominant sampling approaches for qualitative studies are purposive [ 19 , 28 , 32 , 42 , 46 ], snowballing [ 30 , 32 , 46 ] and theoretical sampling [ 31 , 32 ].
The sampling of consumers of mental health services requires some important considerations. The sampling should consider the appropriateness and adequacy of the sampling approach, diversity and variety of consumers of services, attributes such as social, or cultural experiences, shared concerns related to the study, practical and organisational skills, as well as ethical and sensitivity issues are all relevant [ 31 , 32 , 46 ]. Sampling consumers of mental health services should also consider the homogeneity and heterogeneity of consumers. However, failure to address these considerations can present difficulty in sampling and subsequently result in selection and reporting bias in mental health research.
The evidence recommends several data collection approaches in collecting data in mental health research, including focus group discussion, extended in-depth interviews, observations, field notes, Delphi data collection and quasi-statistical techniques. The focus group discussions appear as an approach widely used to collect data from consumers of mental health services [ 19 , 28 , 30 , 31 , 41 , 44 , 47 ]. The focus group discussion appears to be a significant source of obtaining information. This approach promotes the participation of consumers with severe conditions, particularly at the group level interaction. Mental health researchers are encouraged to use this approach to collect data from consumers, in order to promote group level interaction. Additionally, field notes can be used to supplement information and to more deeply analyse the interactions of consumers of mental health services. Field notes are significant when wanting to gather detailed accounts about the subjective experiences of consumers of mental health services [ 40 ]. Field notes can help researchers to capture the gestures and opinions of consumers of mental health services which cannot be covered in the audio-tape recording. Particularly, the field note is relevant to complement the richness of information collected through focus group discussion from consumers of mental health services.
Furthermore, it was found that in-depth interviews can be used to explore specific mental health issues, particularly culturally marked disorders, their personal and interpersonal significance, patient and family explanatory models, individual and family coping styles, as well as symptom symbols and protective mediators [ 19 , 30 , 34 ]. The in-depth interviews are particularly relevant if the study is interested in the lived experiences of consumers without the contamination of others in a group situation. The in-depth interviews are relevant when consumers of mental health services are uncomfortable in disclosing their confidential information in front of others [ 31 ]. The lived experience in a phenomenological context preferably allows the consumer the opportunity to express themselves anonymously without any tacit coercion created by a group context.
The review findings recommend significant factors requiring consideration when collecting data in mental health research. These considerations include building confidence and trust between the researcher and consumers [ 31 , 37 ], gaining confidence of mental health professionals who manage consumers of mental health services, seeking ethical approval from the relevant committees, meeting consumers of services before data collection as well as arranging a mutually acceptable venue for the groups and providing transport services [ 41 , 47 ]. The evidence confirms that the identification of consumers of mental health services to participate in research can be facilitated by mental health professionals. Similarly, the cultural and social differences of the consumers of mental health services need consideration when collecting data from them [ 26 , 31 ].
Moreover, our review advocates that standardised assessment instruments can be used to collect data from consumers of mental health services, particularly in quantitative data. The self-completion instruments for collecting such information can be converted to interviewer-completion instruments [ 33 , 49 ]. The interviewer can read the questions to consumers of mental health services and record their responses. It is recommended that collecting data from consumers of mental health services requires significant preparation, such as training with co-investigators and representatives from consumers of mental health services [ 25 , 30 , 33 , 34 , 35 , 39 , 49 ]. The training helps interviewers and other investigators to understand the research project, particularly translating and adapting an instrument for the study setting with the aim to achieve content, semantic, concept, criteria and technical equivalence [ 30 ]. The evidence indicates that there is a need to adequately train interviewers when preparing for fieldwork to collect data from consumers of mental health services.
The evidence provides several approaches that can be employed to ensure quality assurance in mental health research involving quantitative methods. The quality assurance approach encompasses seeking informed consent from consumers of mental health services [ 26 , 37 ], pre-testing of tools [ 25 , 49 ], minimising non-response rates and monitoring of the data collection process [ 25 , 33 , 49 ]. The quality assurance process in mental health research primarily aims to achieve the highest reliability, validity and timeliness, to improve the quality of care provided. For instance, the informed consent exposes consumers of mental health services to the aim(s), methods, anticipated benefits and potential hazards and discomforts of participating in the study. Herein, consumers of mental health services who cannot respond to the inform consent process because of the severity of their illness can have it signed by their family caregivers. The implication is that researchers should determine which category of consumers of mental health services need family caregivers involved in the consent process [ 37 ].
The review findings advises that researchers should use pre-testing to evaluate the data collection procedure on a small scale and then to subsequently make any necessary changes [ 25 ]. The pre-testing aims to help the interviewers get acquainted with the procedures and to detect any potential problems [ 49 ]. The researchers can discuss the findings of the pre-testing and then further resolve any challenges that may arise prior to the actual field work being commenced. The non-response rates in mental health research can be minimised by re-approaching consumers of mental health services who initially refuse to participate in the study.
In addition, quality assurance for qualitative data can be ensured by applying the principles of credibility, dependability, transferability, reflexivity, confirmability [ 19 , 32 ]. It was found that the credibility of qualitative research in mental health is achieved through methodological and interpretive rigour [ 32 , 37 ]. The methodological rigour for assessing credibility relates to congruence, responsiveness or sensitivity to a social context, appropriateness, adequacy and transparency. By contrast, ensuring interpretive rigour is achieved through authenticity, coherence, reciprocity, typicality and permeability of researchers’ intentions, engagement and interpretation [ 32 , 46 ].
Strengths and limitations
The evidence has several strengths and limitations that require interpretation and explanation. Firstly, we employed a systematic approach involving five stages of problem identification, literature search, data evaluation, data synthesis and presentation of results [ 21 ]. Similarly, we searched six databases and developed a data extraction form to extract information. The rigorous process employed in this study, for instance, searching databases and data extraction forms, helped to capture comprehensive information on the subject.
The integrative review has several limitations largely related to the search words, language limitations, time period and appraisal of methodological quality of included papers. In particular, the differences in key terms and words concerning methodological issues in the context of mental health research across cultures and organisational contexts may possibly have missed some relevant articles pertaining to the study. Similarly, limiting included studies to only English language articles and those published from January 2000 to July 2018 could have missed useful articles published in other languages and those published prior to 2000. The review did not assess the methodological quality of included papers using a critical appraisal tool, however, the combination of clearly articulated search methods, consultation with the research librarian, and reviewing articles with methodological experts in mental health research helped to address the limitations.
The review identified several methodological issues that need critical attention when conducting mental health research. The evidence confirms that studies that addressed methodological considerations in conducting mental health research largely focuses on qualitative studies in a transcultural setting, in addition to lessons from multi-site surveys in mental health research. Specifically, the methodological issues related to the study design, sampling, data collection processes and quality assurance are critical to the research design chosen for any particular study. The review highlighted that researchers conducting mental health research can establish early collaboration, familiarise themselves with the topic, share information on the topic, negotiate to resolve any emerging problems and seek the contribution of clinical (or researcher) team members on the ground. In addition, the recruitment of consumers of mental health services should consider the appropriateness and adequacy of sampling approaches, diversity and variety of consumers of services, their social or cultural experiences, practical and organisational skills, as well as ethical and sensitivity issues.
The evidence confirms that in an attempt to effectively recruit and collect data from consumers of mental health services, there is the need to build confidence and trust between the researcher and consumers; and to gain the confidence of mental health service providers. Furthermore, seeking ethical approval from the relevant committee, meeting with consumers of services before data collection, arranging a mutually acceptable venue for the groups, and providing transport services, are all further important considerations. The review findings establish that researchers conducting mental health research should consider several quality assurance issues. Issues such as adequate training prior to data collection, seeking informed consent from consumers of mental health services, pre-testing of tools, minimising non-response rates and monitoring of the data collection process. More specifically, quality assurance for qualitative data can be achieved by applying the principles of credibility, dependability, transferability, reflexivity, confirmability.
Based on the findings from this review, it is recommended that mental health research should adequately consider the methodological issues regarding study design, sampling, data collection procedures and quality assurance issues to effectively conduct meaningful research.
Availability of data and materials
Not applicable
Abbreviations
focus group discussions
Joanna Briggs Institute
Preferred Reporting Items for Systematic Reviews and Meta-Analyses
National Ethics Advisory Committee. Ethical guidelines for intervention studies: revised edition. Wellington (New Zealand): Ministry of Health. 2012.
Mann C. Observational research methods. Research design II: cohort, cross sectional, and case-control studies. Emerg Med J. 2003;20(1):54–60.
Article CAS Google Scholar
DiPietro NA. Methods in epidemiology: observational study designs. Pharmacotherapy: The Journal of Human Pharmacology and Drug Therapy. 2010;30(10):973–84.
Article Google Scholar
Hong NQ, Pluyr P, Fabregues S, Bartlett G, Boardman F, Cargo M, et al. Mixed Methods Appraisal Tool (MMAT). Canada.: Intellectual Property Office, Canada; 2018.
Creswell JW, Creswell JD. Research design: qualitative, quantitative, and mixed methods approaches: sage publications; 2017.
Google Scholar
Wisdom J, Creswell JW. Mixed methods: integrating quantitative and qualitative data collection and analysis while studying patient-centered medical home models. Rockville: Agency for Healthcare Research and Quality; 2013.
Bonita R, Beaglehole R, Kjellström T. Basic epidemiology: World Health Organization; 2006.
Centers for Disease Control Prevention [CDC]. Principles of epidemiology in public health practice: an introduction to applied epidemiology and biostatistics. Atlanta, GA: US Dept. of Health and Human Services, Centers for Disease Control and Prevention (CDC), Office of Workforce and Career Development; 2012.
Parab S, Bhalerao S. Study designs. International journal of Ayurveda research. 2010;1(2):128.
Yang W, Zilov A, Soewondo P, Bech OM, Sekkal F, Home PD. Observational studies: going beyond the boundaries of randomized controlled trials. Diabetes Res Clin Pract. 2010;88:S3–9.
Department of Family Medicine (McGill University). Mixed Methods Appraisal Tool (MMAT) – Version 2011 Canada: McGill University; 2011 [Available from: http://mixedmethodsappraisaltoolpublic.pbworks.com/w/file/fetch/84371689/MMAT%202011%20criteria%20and%20tutorial%202011-06-29updated2014.08.21.pdf .
Besen J, Gan DS. A critical evaluation of clinical research study designs. J Investig Dermatol. 2014;134.
Axelrod DA, Hayward R. Nonrandomized interventional study designs (quasi-experimental designs). Clinical research methods for surgeons: Springer; 2006. p. 63–76.
Thiese MS. Observational and interventional study design types; an overview. Biochemia medica: Biochemia medica. 2014;24(2):199–210.
Velengtas P, Mohr P, Messner DA. Making informed decisions: assessing the strengths and weaknesses of study designs and analytic methods for comparative effectiveness research. National Pharmaceutical Council 2012.
Guerrera F, Renaud S, Tabbò F, Filosso PL. How to design a randomized clinical trial: tips and tricks for conduct a successful study in thoracic disease domain. Journal of thoracic disease. 2017;9(8):2692.
Bhide A, Shah PS, Acharya G. A simplified guide to randomized controlled trials. Acta Obstet Gynecol Scand. 2018;97(4):380–7.
Palinkas L, Horwitz SM, Chamberlain P, Hurlburt MS, Landsverk J. Mixed-methods designs in mental health services research: a review. Psychiatr Serv. 2011;62(3):255–63.
Palinkas L. Qualitative and mixed methods in mental health services and implementation research. J Clin Child Adolesc Psychol. 2014;43(6):851–61.
World Health Organization [WHO]. Mental health: a state of well-being 2014 [Available from: http://www.who.int/features/factfiles/mental_health/en/ .
Whittemore R, Knafl K. The integrative review: updated methodology. J Adv Nurs. 2005;52(5):546–53.
Hopia H, Latvala E, Liimatainen L. Reviewing the methodology of an integrative review. Scand J Caring Sci. 2016;30(4):662–9.
Pearson A, White H, Bath-Hextall F, Apostolo J, Salmond S, Kirkpatrick P. Methodology for JBI mixed methods systematic reviews. The Joanna Briggs Institute Reviewers Manual. 2014;1:5–34.
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6(7):e1000097.
Alonso J, Angermeyer MC, Bernert S, Bruffaerts R, Brugha TS, Bryson H, et al. Sampling and methods of the European study of the epidemiology of mental disorders (ESEMeD) project. Acta Psychiatr Scand Suppl. 2004;109(420):8–20.
Baarnhielm S, Ekblad S. Qualitative research, culture and ethics: a case discussion. Transcultural Psychiatry. 2002;39(4):469–83.
Braun V, Clarke V. Using thematic analysis in psychology. Qual Res Psychol. 2006;3(2):77–101.
Brown C, Lloyd K. Qualitative methods in psychiatric research. Adv Psychiatr Treat. 2001;7(5):350–6.
Davidsen AS. Phenomenological approaches in psychology and health sciences. Qual Res Psychol. 2013;10(3):318–39.
de Jong JT, Van Ommeren M. Toward a culture-informed epidemiology: combining qualitative and quantitative research in transcultural contexts. Transcultural Psychiatry. 2002;39(4):422–33.
Ekblad S, Baarnhielm S. Focus group interview research in transcultural psychiatry: reflections on research experiences. Transcultural Psychiatry. 2002;39(4):484–500.
Fossey E, Harvey C, McDermott F, Davidson L. Understanding and evaluating qualitative research. Aust N Z J Psychiatry. 2002;36(6):717–32.
Jacobi F, Wittchen H-U, Holting C, Sommer S, Lieb R, Hofler M, et al. Estimating the prevalence of mental and somatic disorders in the community: aims and methods of the German National Health Interview and examination survey. Int J Methods Psychiatr Res 2002;11(1):1–18.
Koch A, Vogel A, Holzmann M, Pfennig A, Salize HJ, Puschner B, et al. MEMENTA-‘Mental healthcare provision for adults with intellectual disability and a mental disorder’. A cross-sectional epidemiological multisite study assessing prevalence of psychiatric symptomatology, needs for care and quality of healthcare provision for adults with intellectual disability in Germany: a study protocol. BMJ Open. 2014;4(5):e004878.
Korver N, Quee PJ, Boos HB, Simons CJ, de Haan L, Investigators G. Genetic risk and outcome of psychosis (GROUP), a multi site longitudinal cohort study focused on gene–environment interaction: objectives, sample characteristics, recruitment and assessment methods. Int J Methods Psychiatr Res. 2012;21(3):205–21.
Larkin M, Watts S, Clifton E. Giving voice and making sense in interpretative phenomenological analysis. Qual Res Psychol. 2006;3(2):102–20.
Latvala E, Vuokila-Oikkonen P, Janhonen S. Videotaped recording as a method of participant observation in psychiatric nursing research. J Adv Nurs. 2000;31(5):1252–7.
Leese MN, White IR, Schene AH, Koeter MW, Ruggeri M, Gaite L. Reliability in multi-site psychiatric studies. Int J Methods Psychiatr Res. 2001;10(1):29–42.
Liu Z, Huang Y, Lv P, Zhang T, Wang H, Li Q, et al. The China mental health survey: II. Design and field procedures. Soc Psychiatry Psychiatr Epidemiol. 2016;51(11):1547–57.
Montgomery P, Bailey PH. Field notes and theoretical memos in grounded theory. West J Nurs Res. 2007;29(1):65–79.
Owen S. The practical, methodological and ethical dilemmas of conducting focus groups with vulnerable clients. J Adv Nurs. 2001;36(5):652–8.
Palinkas L, Horwitz SM, Green CA, Wisdom JP, Duan N, Hoagwood K. Purposeful sampling for qualitative data collection and analysis in mixed method implementation research. Adm Policy Ment Health Ment Health Serv Res. 2015;42(5):533–44.
Palinkas L, Aarons GA, Horwitz S, Chamberlain P, Hurlburt M, Landsverk J. Mixed method designs in implementation research. Adm Policy Ment Health Ment Health Serv Res. 2011;38(1):44–53.
Razafsha M, Behforuzi H, Azari H, Zhang Z, Wang KK, Kobeissy FH, et al. Qualitative versus quantitative methods in psychiatric research. Methods Mol Biol. 2012;829:49–62.
Robins CS, Ware NC, Dosreis S, Willging CE, Chung JY, Lewis-Fernández R. Dialogues on mixed-methods and mental health services research: anticipating challenges, building solutions. Psychiatr Serv. 2008;59(7):727–31.
Robinson OC. Sampling in interview-based qualitative research: a theoretical and practical guide. Qual Res Psychol. 2014;11(1):25–41.
Schilder K, Tomov T, Mladenova M, Mayeya J, Jenkins R, Gulbinat W, et al. The appropriateness and use of focus group methodology across international mental health communities. International Review of Psychiatry. 2004;16(1–2):24–30.
Schoonenboom J, Johnson RB. How to construct a mixed methods research DesignWie man ein mixed methods-Forschungs-design konstruiert. KZfSS Kölner Zeitschrift für Soziologie und Sozialpsychologie. 2017;69(2):107–31.
Yin H, Phillips MR, Wardenaar KJ, Xu G, Ormel J, Tian H, et al. The Tianjin mental health survey (TJMHS): study rationale, design and methods. Int J Methods Psychiatr Res. 2017;26(3):09.
Download references
Acknowledgements
The authors wish to thank the University of Newcastle Graduate Research and the School of Nursing and Midwifery, for the Doctoral Scholarship offered to the lead author. The authors are also grateful for the support received from Ms. Debbie Booth, the Librarian for supporting the literature search.
Author information
Authors and affiliations.
School of Nursing and Midwifery, The University of Newcastle, Callaghan, Australia
Faculty of Health and Medicine, School Nursing and Midwifery, University of Newcastle, Callaghan, Australia
Anthony Paul O’Brien
Faculty of Business and Economics, Macquarie University, North Ryde, Australia
Rebecca Mitchell
You can also search for this author in PubMed Google Scholar
Contributions
EB, APO’B, and RM conceptualized the study. EB conducted the data extraction, APO’B, and RM, conducted the second review of the extracted data. EB, working closely with APO’B and RM performed the content analysis and drafted the manuscript. EB, APO’B, and RM, reviewed and made inputs into the intellectual content and agreed on its submission for publication. All authors read and approved the final manuscript.
Corresponding author
Correspondence to Eric Badu .
Ethics declarations
Ethics approval and consent to participate, consent for publication, competing interests.
The authors declare that they have no competing interests.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Additional file
Additional file 1:.
Data extraction form. (DOCX 18 kb)
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( http://creativecommons.org/licenses/by/4.0/ ), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( http://creativecommons.org/publicdomain/zero/1.0/ ) applies to the data made available in this article, unless otherwise stated.
Reprints and permissions
About this article
Cite this article.
Badu, E., O’Brien, A.P. & Mitchell, R. An integrative review on methodological considerations in mental health research – design, sampling, data collection procedure and quality assurance. Arch Public Health 77 , 37 (2019). https://doi.org/10.1186/s13690-019-0363-z
Download citation
Received : 13 November 2018
Accepted : 22 July 2019
Published : 10 October 2019
DOI : https://doi.org/10.1186/s13690-019-0363-z
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Mental health
- Methodological approach
- Mixed methods
- Data collection
Archives of Public Health
ISSN: 2049-3258
- General enquiries: [email protected]
- Open access
- Published: 14 January 2022
COVID-19 impact on mental health
- Jingyu Cui 1 ,
- Jingwei Lu 1 ,
- Yijia Weng 1 ,
- Grace Y. Yi 1 , 2 &
- Wenqing He 1
BMC Medical Research Methodology volume 22 , Article number: 15 ( 2022 ) Cite this article
12k Accesses
18 Citations
Metrics details
The coronavirus disease 2019 (COVID-19) pandemic has posed a significant influence on public mental health. Current efforts focus on alleviating the impacts of the disease on public health and the economy, with the psychological effects due to COVID-19 relatively ignored. In this research, we are interested in exploring the quantitative characterization of the pandemic impact on public mental health by studying an online survey dataset of the United States.
The analyses are conducted based on a large scale of online mental health-related survey study in the United States, conducted over 12 consecutive weeks from April 23, 2020 to July 21, 2020. We are interested in examining the risk factors that have a significant impact on mental health as well as in their estimated effects over time. We employ the multiple imputation by chained equations (MICE) method to deal with missing values and take logistic regression with the least absolute shrinkage and selection operator (Lasso) method to identify risk factors for mental health.
Our analysis shows that risk predictors for an individual to experience mental health issues include the pandemic situation of the State where the individual resides, age, gender, race, marital status, health conditions, the number of household members, employment status, the level of confidence of the future food affordability, availability of health insurance, mortgage status, and the information of kids enrolling in school. The effects of most of the predictors seem to change over time though the degree varies for different risk factors. The effects of risk factors, such as States and gender show noticeable change over time, whereas the factor age exhibits seemingly unchanged effects over time.
Conclusions
The analysis results unveil evidence-based findings to identify the groups who are psychologically vulnerable to the COVID-19 pandemic. This study provides helpful evidence for assisting healthcare providers and policymakers to take steps for mitigating the pandemic effects on public mental health, especially in boosting public health care, improving public confidence in future food conditions, and creating more job opportunities.
Trial registration
This article does not report the results of a health care intervention on human participants.
Peer Review reports
Since the outbreak of the COVID-19 pandemic, people's lifestyle has been changed significantly. However, no sufficient resources have been available to attenuate the pandemic effects on mental health and well-being [ 1 ]. Various studies have been conducted to investigate how the COVID-19 pandemic may affect people psychologically. For example, Cao et al. [ 2 ] conducted a survey on college students in China and showed that more than 24% of the students were experiencing anxiety. Spoorthy et al. [ 3 ] investigated the mental health problems faced by healthcare workers during the COVID-19 pandemic.
While those studies provided descriptive results by summarizing the information obtained from the questionnaire, it is unclear how the impact of COVID-19 changes over time; what factors are relevant to describe the impact of the pandemic; and how the severity of the mental health issues is quantitatively associated with the risk factors. In this paper, we examine these questions and aim to provide some quantitative insights. Our explorations are carried out using a large scale online public survey study conducted by the U.S. Census Bureau [ 4 ]. The data include twelve data sets each collected in a 1-week window over 12 consecutive weeks from April 23, 2020 to July 21, 2020. Different data sets contain the measurements from different participants on the same questions. Among the 12 data sets, the smallest one contains 41,996 subjects and the largest one has 132,961 participants. We treat the survey in each week as an independent study. We are interested in assessing how the effects of the associated risk factors may change over time by applying the same method to each of the 12 data sets separately.
The survey includes multiple questions perceived to be relevant to describing the impact of the pandemic on the public. To quantitatively identify the risk factors for impacting the mental health by the pandemic, we engage the penalized logistic regression method, with the least absolute shrinkage and selection operator (Lasso) penalty [ 5 ]. However, a direct application of the Lasso method is not possible due to the presence of missing observations. To handle missing values, we employ the multiple imputation by chained equations (MICE) method (e.g., [ 6 , 7 ]). Further, survey data commonly involve measurement error due to recall bias, the inability of providing precise descriptions of some answers, and reporting errors. It is imperative to address this issue when pre-processing the data. To this end, we combine the levels of those highly related categorical variables to mitigate the measurement error effects.
Original survey data
The data used in this project are from phase 1 of the Household Pulse Survey conducted by the U.S. Census Bureau [ 4 ] from April 23, 2020 to July 21, 2020 for 12 consecutive weeks, giving rise to 12 data sets each for a week. The survey aims to study the pandemic impacts on the households across the United States from social and economic perspectives. The survey contains 50 questions ranging from education, employment, food sufficiency, health, housing, social security benefits, household spending, stimulus payments, to transportation. The participants of the survey come from all the 50 states plus Washington, D.C., United States, aging from 18 to 88. The gender ratio (the ratio of males to females) remains fairly stable ranging between 0.6 and 0.7 over the 12 weeks. Figure S1 in the Supplementary Material shows the curves of the number of cumulative confirmed cases for all the states which are grouped into four categories of the severity of the pandemic, derived from the data from the Centers for Disease Control and Prevention [ 8 ]. Table 1 lists the state members for each category, together with the total number of participants over the 12 weeks and the corresponding percentage for each category. It is seen that the majority (72.5%) of the participants of the survey come from the states with mild pandemic and the least proportion (2.3%) of subjects are from the states with a serious pandemic.
Pre-processing the data to reduce errors
Among the initial 50 questions, nine questions, such as “ Where did you get free groceries or free meals ” and “ How often is the Internet available to children for educational purposes ”, are excluded because they are not perceived as sustainable factors on affecting mental health. Measurement error is typically involved in survey data. Prior to a formal analysis of the data, we implement a pre-processing procedure to mitigate the measurement error effects by combining questions to create new variables, or collapsing levels of variables to form binary variables.
Information on mental health is collected via four questions concerning anxiety , worry , loss of interest , and feeling down . Each question is a four-level Likert item [ 9 ] with values 1, 2, 3 and 4, showing the degree of each aspect for the past 7 days prior to the survey time. In contrast to Twenge and Joiner [ 10 ] who combined the measurements of the first two questions anxiety and worry to indicate the anxiety level and the last two questions loss of interest and feeling down to show the depression level, we define a single binary response to reflect the mental health status of an individual by combing measurements of the four variables. The response variable takes value 1 if the average of the scores of the four variables is greater than 2.5, and 0 otherwise, where the threshold 2.5 is the median value for each question. This binary response gives a synthetic way to indicate the mental health status which is easier thaeach question. This binary response gives a synthetic wayn examining measurements of multiple variables.
Two variables describe the loss of work: Wrkloss indicates whether an individual in the household experiences a loss of employment income since March 13, 2020; Expctloss indicates if the individual expects a member in the household to experience a loss of employment income in the next 4 weeks because of the COVID-19 pandemic. These two variables are combined to form a single indicator which is denoted Wrkloss , with value 1 if at least one of these two events happens. Two ordinal variables, Prifoodsuf and Curfoodsuf , are used to describe the food sufficiency status before the pandemic and at present, respectively. The Foodcon.change variable is constructed by comparing the current and the previous food sufficiency status to form a binary variable, taking 1 if the current food sufficiency status is no worse than the food status before the pandemic, and 0 otherwise. Variable Med.delay.notget is combined from two indicator variables Delay (indicating if medical care is delayed) and Notget (indicating if the medical care is not received), taking value 1 if either medical care is delayed or no medical care is received, and 0 otherwise. Predictor Mort.prob is combined from one binary variable and an ordinal variable, taking 1 if a participant does not pay last month’s rent or mortgage or does not have enough confidence in paying the next rent or mortgage payment on time, and 0 otherwise. In addition, three ordinal variables, Emppay , Healins, and Schoolenroll , are modified by collapsing their levels to form binary categories. Emppay has value 1 if he/she gets paid for the time he/she is not working, and 0 otherwise. Healins has value 1 if the individual is currently covered by the health insurance, and 0 otherwise. Schoolenroll has value 1 if there is a child in the household enrolled in school, and 0 otherwise. Except for the variables discussed above, the remaining variables are kept as in the original form.
The final data include the binary response (indicating the mental health status of an individual) and 25 predictors measuring various aspects of individuals. To be specific, nine predictors show basic information: State , Age , Male , Rhispanic , Race , Educ , MS (marital status), Numper (the number of people in the household), and Numkid (the number of people under 18 in the household); five variables concern the income and employment: Income , Wrkloss , Anywork , Kindwork , and Emppay ; five variables are related to food: Foodcon.change , Freefood , Tspndfood , Tspndprpd , and Foodconf ; three variables pertain to health and insurance: Hlthstatus , Healins , and Med.delay.notget ; one variable, Mort.prob , is for mortgage and housing; and two variables, Schoolenroll and Ttch_Hrs , reflect child education. The variable dictionary for the pre-processed data is shown in Table 2 .
Missing observations
In the data sets, 17 covariates together with the response variable have missing observations. To provide a quick and intuitive sense of the missingness proportions for different variables over the 12 data sets, we combine those data sets by individual variable to form a single pooled data set. Then we calculate the missingness proportion for each variable by dividing the number of missing observations in the variable by the total number of subjects in the pooled data set. We display in Fig. 1 the missingness rates for those 17 risk factors and the response variable (mental health status) for the pooled data. The risk factors having the three highest missingness rates are the variables Ttch_hrs , Schoolenroll and Emppay , and the corresponding missingness rates are 76.7%, 66.9% and 60.5%, respectively. Five variables incur higher than 30% missingness proportions, and the missingness proportion for 12 risk factors is larger than 5%. The missingness proportion for the response variable is about 8.6%.
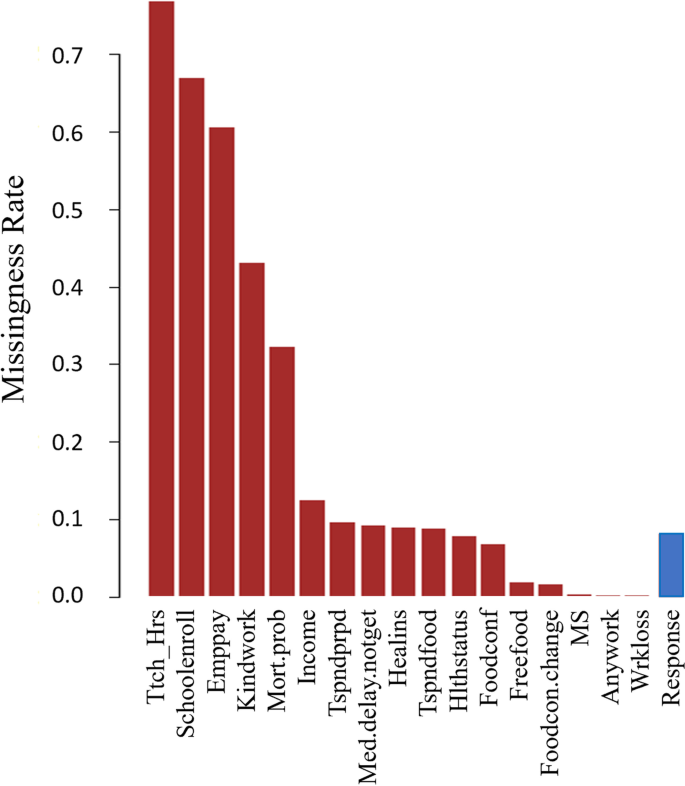
The missingness rates for the 17 risk factors and the response of the pooled data
Missing values present a challenge for data analysis and model fitting. One may perform the so-called complete data analysis by deleting those subjects with missing observations or the so-called available data analysis by using all available data, and then repeating a standard analysis procedure. Such analyses are easy to implement, however, biased results are expected if the missing completely at random (MCAR) mechanism is not true. Here we consider a broader setting where missing data do not necessarily follow the MCAR but follow the missing at random (MAR) mechanism. We employ the MICE method which is developed under the MAR mechanism and applies to various types of variables such as continuous, binary, nominal, and ordinal variables subject to missingness. A detailed discussion on this method was provided by van Buuren et al. [ 11 ].
Here we employ the MICE method to accommodate missing observations that are present in both the predictors and the response. Following the suggestion of Allison [ 12 ], we choose to do five imputations for the data in each week by employing the same algorithm with different random seeds. The implementation is conducted in R (version 3.6.1) with the R package: Multivariate Imputation by Chained Equation (mice). The details on the R code are presented in the code availability in the Declarations section .
To empirically assess the imputation results, we take the data in week 6 as an example and compare the five imputed data sets to the original data by displaying their distribution using the R function density for the continuous variables; the results are reported in Figure S2 in the Supplementary Material . It is seen that the distributions of the 5 imputed data sets for the three continuous variables, Tspndfood , Tspndprpd , and Ttch_hrs , are fairly similar to that of the original data. Further, in Tables S1, S2, and S3 in the Supplementary Material , we report the proportions of different levels for the categorical variables for both the imputed and original data, showing the similarity in the distributions of the imputed data and of the original data.
Model building and inference
We intend to employ logistic regression with the Lasso penalty to analyze the data that contain a binary response and potentially related predictors or covariates. First, we introduce the basic notation and discuss the method in general terms. For i = 1, …, n , let Y i represent the binary response with value 1 indicating that the mental health problem occurs for subject i and 0 otherwise. Let X ij denote the j th covariate for subject i , where j = 1, …, p , and p is the number of predictors. Write X i = ( X i 1 , X i 2 , …, X ip ) T and let π i = P ( Y i = 1| X i ).
Consider the logistic regression model
where β = ( β 1 , …, β p ) T denotes the vector of regression parameters. Consequently, the log-likelihood function for β is given by
To select the predictors associated with the dichotomous response, we employ the Lasso method. The Lasso estimates are the values that maximize the penalized log-likelihood function obtained by adding an L 1 penalty to the expression (2):
where λ is the tuning parameter. The 10-fold cross-validation is employed to obtain a proper value for the tuning parameter and the one-standard-error rule [ 13 ] is applied to pick the most parsimonious model within one standard error of the minimum cross-validation misclassification rate (e.g., [ 14 ]).
Model fitting and variable selection
The Lasso logistic regression is applied to each of the five imputed data sets for each week. The predictors corresponding to the nonzero coefficient estimates are considered the risk factors selected, which may be different across five imputed data sets for each of the 12 weeks. To explore in a full spectrum, we start with two extreme models, called the full model by including the union of all the selected risk factors by the Lasso logistic regression, and the reduced model by including only the common factors selected for all five imputed data sets in any week. The full model includes all the 25 predictors in the original data, and the reduced model contains 11 predictors: Age , Male , MS , Numkid , Wrkloss , Anywork , Foodconf , Hlthstatus , Healins , Med.delay.notget , and Mort.prob . We expect the predictors in the final model to form a set in-between the sets of the predictors for the reduced mode and the full model . Now, the problem is how to find the final model using the reduced and full models . To this end, we carry out the following four steps.
In Step 1, we fit logistic regression with predictors in the full model and in the reduced model , respectively, to each of the five surrogate data sets for each of the 12 weeks.
In Step 2, the estimates and standard errors of the model coefficients for a given week are obtained using the algorithm described by Allison [ 12 ]. To be specific, let M = 5 be the number of surrogate data sets for the original incomplete data. Let β j be the j th component of the model parameter vector β . For k = 1, …, M , let \({\hat{\beta}}_j^{(k)}\) denote the estimate of the model parameter β j obtained from fitting the k th surrogate data set in a week and let \({S}_j^{(k)}\) be its associated standard error. Then the point estimate of β j is given by the average of those estimates of β j derived from the M imputed data sets:
To determine the variability associated with \({\hat{\beta}}_j\) , one needs to incorporate both the within imputation variance, denoted V w , and the between imputation variance, denoted V b . According to Rubin’s rule [ 6 ], the total variance associated with the multiple imputation estimate \({\hat{\beta}}_j\) is given by \(Var\left({\hat{\beta}}_j\right)={V}_w+\left(1+\frac{1}{M}\right){V}_b\) , where \({V}_w=\frac{1}{M}\sum_{k=1}^M{\left\{{S}_j^{(k)}\right\}}^2\) , and the between imputation variance, \({V}_b=\frac{1}{M-1}\sum_{k=1}^M{\left\{{\hat{\beta}}_j^{(k)}-{\hat{\beta}}_j\right\}}^2\) , is inflated by a factor \(\frac{1}{M}\) . As a result, the standard error associated with \({\hat{\beta}}_j\) is given by \(se\left({\hat{\beta}}_j\right)=\sqrt{Var\left({\hat{\beta}}_j\right)}\) , i.e.,
We report in Tables S4 and S5 in the Supplementary Material the estimated results of the covariate effects obtained, respectively, from the full and reduced models for the data in 12 weeks, where the covariates marked with an asterisk are statistically significant with p-values smaller than 0.05 for more than 6 weeks. It is found that in addition to those covariates included in the reduced model, fitting the full model also shows that five additional covariates, State , Rhispanic , Race , Numper , and Schoolenroll, are statistically significant for more than 6 weeks’ data. Table S 5 shows that almost all the covariates in the reduced model are statistically significant, with all the p-values derived from the data in 12 weeks smaller than 0.05.
Consequently, in Step 3, we take the 11 significant risk factors from the reduced model , and the 5 additional partially significant covariates suggested by fitting the full model , State , Rhispanic , Race , Numper , and Schoolenroll, to form the list of risk factors for the final model.
In Step 4, we construct the final model using the model form (1) to include the selected variables in Step 3 as predictors, where dummy variables are used to express categorical variables State , Race , MS , Foodconf , and Hlthstatus with levels more than two, yielding 28 variables in the model. The final model is then given by
where β j is the regression coefficients for j = 0, 1, …, 28, and the subscript i is suppressed in π and the covariates for ease of exposition.
Then, we fit the final logistic model (6) to each of the imputed data sets for each of the 12 weeks; in the same manner as indicated by (4) and (5), we obtain the point estimates of the model parameters and the associated standard errors. To have a visual display, we plot in Fig. 2 the estimates of the coefficients for all the factors in the final model for 12 weeks; to precisely show the estimates, we report in Table 3 the point estimates for the covariate effects obtained from the final model , where we further calculate the average of the 12 estimates for each covariate and report the results in the last column. The associated standard errors and the p-values are deferred to Table S6 in the Supplementary Material . The results suggest that the factors Numper, Healins and Schoolenroll are only significant in some of 12 weeks, while other factors in the final models are significant in all 12 weeks.
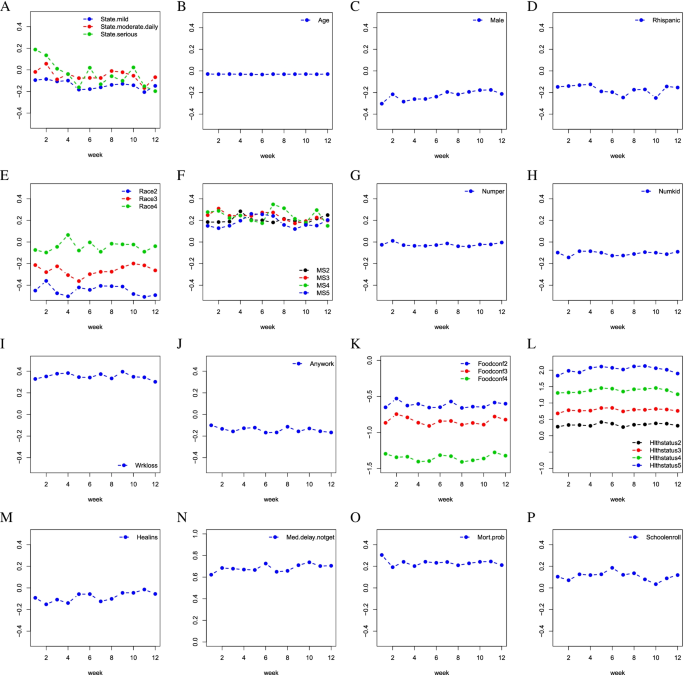
The estimates of the coefficients for all the factors in the final model are displayed against the week number
Figure 2 shows that the absolute values of coefficient estimates for some levels of variables Foodconf and Hlthstatus are greater than 1 (in Fig. 2 K and L). The coefficient estimates of Med.delay.notget over 12 weeks are between 0.5 and 1 (in Fig. 2 N). Other variables have coefficient estimates between -0.5 and 0.5.
To have an overall sense of the estimates of the predictor effects in the final model, we now utilize the averages reported in the last column of Table 3 to estimate the relative change in the odds of having mental issues with one unit increase in a predictor from its baseline while keeping other predictors unchanged, yet leaving the associated variability uncharacterized. Let \({\overline{\hat{\beta}}}_j\) represent the average of those estimates of the covariate effect β j over the 12 weeks for j = 1, …, 28, which is a sensible estimate of β j , because the arithmetic average preserves the consistency if all the estimators obtained for the 12 weeks are consistent for β j . Using \({\overline{\hat{\beta}}}_j\) is advantageous in offering us a single estimate of β j with generally expected smaller variability than those estimates obtained from each of the 12 weeks. If \({\overline{\hat{\beta}}}_j\) is negative, then \(1-{\exp}\left({\overline{\hat{\beta}}}_j\right)\) shows an estimate of the decrease in the odds of having mental issues relative to the baseline; if \({\overline{\hat{\beta}}}_j\) is positive, then \({\exp}\left({\overline{\hat{\beta}}}_j\right)-1\) suggests an estimate of the increase in the odds of having mental issues relative to the baseline.
To be specific, for the variable State with large daily increases of cases as the baseline, people from mild pandemic States exhibit an estimate of 1 − exp (−0.139) ≈ 13% decrease in the odds of having mental issues; people from the States with moderate daily increases show an estimate of 1 − exp (−0.053) ≈ 5.16% degrease in the odds; people from serious pandemic States are generally associated with an estimate of 1 − exp (−0.039) ≈ 3.82% decrease in the odds.
For Age and Gender , their averages of the estimates over the 12 weeks are -0.030 and -0.228, respectively, implying that one unit increase in Age is associated with about an estimate of 1 − exp (−0.030) ≈ 2.96% decrease in the odds of occurrence of mental health problems; and being a male relative to a female is associated with an estimate of 1 − exp (−0.228) ≈ 20.39% decrease in the odds of having mental health issues. Similarly, the 12-week estimated effects of Rhispanic indicate that the origin of Hispanic, Latino or Spanish is associated with a smaller odds of having mental issues than others. The 12-week mean of the coefficient estimates of Rhispanic is -0.172, leading to an estimate of the odds of mental health problem occurrence being reduced by around 1 − exp (−0.172) ≈ 15.80%.
For the variable Race with White as the baseline, the 12-week mean of coefficient estimates for Black (Race2) and Asian (Race3) are -0.446 and -0.262, respectively, yielding an estimate of the odds of occurrence of mental health issues for Black and Asian to be, respectively, 1 − exp (−0.446) ≈ 35.98% and 1 − exp (−0.262) ≈ 23.05% less than White .
For MS (marital status) with now married as the baseline, an estimate of the increase in the odds of having mental issues relative to the baseline, is exp (0.206) − 1≈22.88%, exp (0.236) − 1≈26.62%, exp (0.242) − 1≈27.38%, and exp (0.181) − 1≈19.84%, respectively, for people who are widowed (MS2), divorced (MS3), separated (MS4) , or never married (MS5).
For predictors Numper and Numkid , the averages of the estimates suggest that the increase of the number of people and kids in the household is associated with the decrease of the odds of having mental issues. Specifically, one person increase in the household is associated with an estimate of 1 − exp (−0.024)≈2.37% decrease in odds, and one more kid in the household is associated with an estimate of 1 − exp (−0.106)≈10.06% decrease in the odds.
For the work-related factors Wrkloss and Anywork , the results shown in the last column in Table 3 indicate that experiencing a loss of employment income since March 13, 2020 is associated with an estimate of exp (0.352) − 1≈42.19% increase in the odds of having mental issues, and doing any work during the last 7 days is associated with an estimate of 1 − exp (−0.141)≈13.15% decrease in the odds.
The 12-week results of Foodconf in Table 3 show that, with the not at all confident on the future food affordability as the baseline, an increase in the confidence of food affordability is negatively associated with the odds of having mental issues. On average of 12 weeks, shown in the last column in Table 3 , the more confident in the food affordability, the less the odds of having mental issues. For example, the person who is very confident (Foodconf4) in the food affordability for the next four weeks demonstrates an estimate of 1 − exp (−1.348)≈74.02% decrease in the odds of having mental issues, relative to the person who is not at all confident .
With excellent health conditions as the baseline, the estimates of Hlthstatus in Table 3 say that the worse the self-evaluated health condition, the larger the odds of having mental issues. Considering the worst level of health condition poor (Hlthstatus5) as an example, the average of the estimates over the 12 weeks yields that people in poor health conditions have an estimate of the odds of having mental issues exp (2.021)≈7.55 times higher than people of excellent health conditions. For other health-related predictors, Healins and Med.delay.notget , people who are currently covered by health insurance are associated with an estimate of 1 − exp (−0.083)≈7.96% decrease in the odds of mental issues occurrence, and people who do not get medical care or have delayed medical care are associated with an estimate of exp (0.684) − 1≈98.18% increase in the odds.
For Mort.prob and Schoolenroll , people having rental or mortgage problems are associated with an estimate of exp (0.232) − 1≈26.15% increase in the odds of having mental health problems, and people whose household has kids enrolled in school are associated with an estimate of exp (0.109) − 1≈11.52% increase in the odds of having mental issues.
In summary, the factors in the final model associated with a reduction in the odds of having mental health issues include: States not having large daily increases of cases, older in age, being male, having a Hispanic, Latino or Spanish origin, being non-White, more people or kids in the household, having job during the last 7 days, having confidence in the food affordability in the future, and being covered by insurance. The factors in the final model associated with the increase in the odds of getting mental issues are: not married, experiencing loss of job, poor self-evaluations on health conditions, having problems in getting medical care and mortgage, and having kids enrolled in school.
In this paper we investigate the impact of the COVID-19 pandemic on the public mental health using an online survey data set from the United States. Prior to the analysis, we pre-process the data by combining some levels of certain variables in the hope to ameliorate the effects of the errors that are often induced in survey data, including recall bias, reporting error, uncertainty in providing a precise assessment of the situation, inability to decide a right scale to a question, and inconsistency in the answers to the same question that is phrased differently [ 15 ]. In addition, some variables are quite similar or even identical in nature, thus, combining them can help alleviate unwanted noise. Further, we employ multiple imputation to account for the missingness effects, and use the penalized logistic regression with the Lasso penalty to select important risk factors for mental health.
While this study offers us quantitative evidence how the COVID-19 pandemic can psychologically challenge the public, several limitations need to be pointed out. Firstly, the online survey data were designed to assess the pandemic impact from the social and economic perspectives, and they may not contain enough necessary factors related to mental health issues. In addition, the interaction effects between the predictors are not considered in our analysis, which may restrict the capacity of the model. Secondly, while the choice of M = 5 in our analysis follows the suggestion of Allison [ 12 ], it would be interesting to study how the variability may be incurred by setting different values for M .
Thirdly, though it is easy to see that the data exhibit arbitrary missingness patterns, or the so-called intermittent missing data patterns , it is difficult to tell what exactly the underlying missing data mechanism is, as in many other missing data problems [ 16 ]. Though the multiple imputation method is useful for handling missing data with the MAR mechanism [ 16 ], its performance can be considerably impacted by different proportions of missing values. Efforts of accounting for missingness effects do not always come to be rewarding. In the presence of excessive missing observations, the multiple imputation method, like any other method, can fail to yield sensible results even if the MAR mechanism is true. In such instances, one needs to be cautious to interpret the analysis results and be aware of potentially induced biases due to a high proportion of missing information.
Finally, in the analysis, we define the response variable to be binary by combining the information collected from four questions about mental health. While this approach gives a simple way to indicate the mental health status and is similarly taken by other authors (e.g., [ 10 ]), it is heuristic, as pointed out by a referee. It is thereby interesting to take the original four categorial variables as outcomes and conduct multivariate analysis to examine how those outcomes are associated with the covariates with missingness effects accommodated. Such analyses would be more sophisticated and require extra care to facilitate the association structures among the multiple response variables. Further, the yielded results may be less intuitive to interpret than those derived from using a single response variable.
The analysis results unveil evidence-based findings to identify the groups who are psychologically vulnerable to the COVID-19 pandemic. This study provides helpful evidence to assist healthcare providers and policymakers to take steps for mitigating the pandemic effects on public mental health, especially in boosting public health care, improving public confidence in future food conditions, and creating more job opportunities.
Availability of data and materials
The data sets analyzed here are available in the Bureau of the Census, Household Pulse Survey Public Use File (PUF) repository [ 4 ], https://www.census.gov/programs-surveys/household-pulse-survey/datasets.html .
Abbreviations
Coronavirus disease 2019
multiple imputations by chained equations
least absolute shrinkage and selection operator
Taylor S. The psychology of pandemics: Preparing for the next global outbreak of infectious disease. Cambridge Scholars Publishing; 2019.
Cao W, Fang Z, Hou G, Han M, Xu X, Dong J, et al. The psychological impact of the COVID-19 epidemic on college students in China. Psychiatry Research. 2020;287:112934.
Article CAS Google Scholar
Spoorthy MS, Pratapa SK, Mahant S. Mental health problems faced by healthcare workers due to the COVID-19 pandemic-A review. Asian J Psychiatr. 2020;51:102119.
Article Google Scholar
United States Census Bureau (USCB). Household pulse survey public use file (PUF) [Internet]. Bureau of the Census; 2020. Available from: https://www.census.gov/programs-surveys/household-pulse-survey/datasets.html Accessed Oct 2020.
Tibshirani R. Regression shrinkage and selection via the Lasso. J R Stat Soc Series B Stat Methodol. 1996;58(1):267–88.
Google Scholar
Rubin DB. Multiple imputation for nonresponse in surveys. New York: Wiley; 1987.
Book Google Scholar
Yu LM, Burton A, Rivero-Arias O. Evaluation of software for multiple imputation of semi-continuous data. Stat Methods Med Res. 2007;16(3):243–58.
Center for Disease Control and Prevention (CDC). United States COVID-19 cases and deaths by state over time [Internet]. CDC; 2020. Available from: https://data.cdc.gov/Case-surveillance/United-States-COVID-19-Cases-and-Deaths-by-State-o/9mfq-cb36/data Accessed Oct 2020.
Joshi A, Kale S, Chandel S, Pal DK. Likert scale: explored and explained. Curr J Appl Sci Technol. 2015;7(4):396–403.
Twenge JM, Joiner TE. U.S. Census Bureau-assessed prevalence of anxiety and depressive symptoms in 2019 and during the 2020 COVID-19 pandemic. Depress Anxiety. 2020;37(10):954–6.
Buuren SV, Groothuis-Oudshoorn K. mice: Multivariate imputation by chained equations in R. J Stat Softw. 2011;45:1–67.
Allison PD. Multiple imputation for missing data: a cautionary tale. Sociol Methods Res. 2000;28(3):301–9.
Hastie T, Tibshirani R, Friedman J. The elements of statistical learning: Data mining, inference, and prediction. 2ed ed. New York: Springer Science & Business Media; 2009. 244 p.
Krstajic D, Buturovic LJ, Leahy DE, Thomas S. Cross-validation pitfalls when selecting and assessing regression and classification models. J Cheminform. 2014;6(1):1–15.
Yi GY. Statistical Analysis with Measurement Error or Misclassification: Strategy, Method and Application. New York: Springer; 2017.
Little RJ, Rubin DB. Statistical Analysis with Missing Data. 2nd ed. Hoboken: Wiley; 2002.
Cui J, Lu J, Weng Y. R code for COVID 19 Impact on mental health over time [Internet]. GitHub; 2021 [updated 2021 Sep 9; cited 2021 Sep 9]. Available from: https://github.com/JingyuCui639/R-code-for-COVID-19-Impact-on-Mental-Health-over-Time
Download references
Acknowledgements
The authors thank the reviewers for their helpful comments on the initial submission. The research was partially supported by the grants of the Discovery Grants Program and the Emerging Infectious Disease Modeling Program from the Natural Sciences and Engineering Research Council of Canada. Yi is Canada Research Chair in Data Science (Tier 1). Her research was undertaken, in part, thanks to funding from the Canada Research Chairs program. The grants provide support to JC, JL and YW to conduct the study.
Code availability
All the computation in this study is conducted in R (version 3.6.1) and the R code is posted in GitHub at: https://github.com/JingyuCui639/R-code-for-COVID-19-Impact-on-Mental-Health-over-Time [ 17 ].
The research was partially supported by the grants of the Discovery Grants Program and the Emerging Infectious Disease Modeling Program from the Natural Sciences and Engineering Research Council of Canada. Yi is Canada Research Chair in Data Science (Tier 1). Her research was undertaken, in part, thanks to funding from the Canada Research Chairs program. The grants provide support to JC, JL and YW to conduct the analyses.
Author information
Authors and affiliations.
Department of Statistical and Actuarial Sciences, Western University, London, Ontario, N6A 5B7, Canada
Jingyu Cui, Jingwei Lu, Yijia Weng, Grace Y. Yi & Wenqing He
Department of Computer Science, Western University, London, Ontario, N6A 5B7, Canada
Grace Y. Yi
You can also search for this author in PubMed Google Scholar
Contributions
JC leads the project; YW identifies the data; JC, JL, and YW jointly analyze the data and prepare the initial draft. Professors WH and GYY offer ideas and discussions for the project; GYY writes the manuscript. All authors have read and approved the manuscript.
Corresponding author
Correspondence to Grace Y. Yi .
Ethics declarations
Ethics approval and consent to participate.
Not applicable
Consent for publication
Competing interests.
The authors declare that they have no competing interests.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Additional file 1., rights and permissions.
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/ . The Creative Commons Public Domain Dedication waiver ( http://creativecommons.org/publicdomain/zero/1.0/ ) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
Reprints and permissions
About this article
Cite this article.
Cui, J., Lu, J., Weng, Y. et al. COVID-19 impact on mental health. BMC Med Res Methodol 22 , 15 (2022). https://doi.org/10.1186/s12874-021-01411-w
Download citation
Received : 03 April 2021
Accepted : 20 September 2021
Published : 14 January 2022
DOI : https://doi.org/10.1186/s12874-021-01411-w
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- logistic regression
- mental health
- missing data
- multiple imputation
- survey data
BMC Medical Research Methodology
ISSN: 1471-2288
- General enquiries: [email protected]
Quantitative needs assessment tools for people with mental health problems: a systematic scoping review
- Open access
- Published: 12 March 2024
- Volume 43 , pages 19996–20013, ( 2024 )
Cite this article
You have full access to this open access article

- Irena Makivić ORCID: orcid.org/0000-0003-2748-5522 1 ,
- Anja Kragelj 1 &
- Antonio Lasalvia ORCID: orcid.org/0000-0001-9963-6081 2
1817 Accesses
Explore all metrics
Needs assessment in mental health is a complex and multifaceted process that involves different steps, from assessing mental health needs at the population or individual level to assessing the different needs of individuals or groups of people. This review focuses on quantitative needs assessment tools for people with mental health problems. Our aim was to find all possible tools that can be used to assess different needs within different populations, according to their diverse uses. A comprehensive literature search with the Boolean operators “Mental health” AND “Needs assessment” was conducted in the PubMed and PsychINFO electronic databases. The search was performed with the inclusion of all results without time or other limits. Only papers addressing quantitative studies on needs assessment in people with mental health problems were included. Additional articles were added through a review of previous review articles that focused on a narrower range of such needs and their assessment. Twenty-nine different need-assessment tools specifically designed for people with mental health problems were found. Some tools can only be used by professionals, some by patients, some even by caregivers, or a combination of all three. Within each recognized tool, there are different fields of needs, so they can be used for different purposes within the needs assessment process, according to the final research or clinical aims. The added value of this review is that the retrieved tools can be used for assessment at the individual level, research purposes or evaluation at the outcome level. Therefore, best needs assessment tool can be chosen based on the specific goals or focus of the related needs assessment.
Similar content being viewed by others
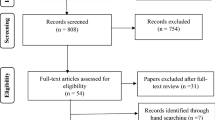
The Conceptualization of Mental Health Service Quality Assessment: Consumer Perspective
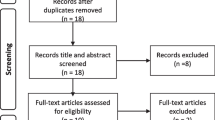
Measurement of perceived needs in humanitarian contexts using the HESPER scale: a scoping study with reflections on the collaboration between researchers and humanitarian actors
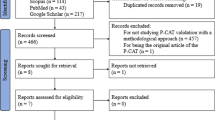
Person-centered care assessment tool with a focus on quality healthcare: a systematic review of psychometric properties
Explore related subjects.
- Artificial Intelligence
Avoid common mistakes on your manuscript.
Mental disorders are the largest contributor to the disease burden in Europe (Wykes et al., 2021 ), and mortality related to such conditions increases the overall economic burden (McGorry & Hamilton, 2016 ). Mental disorders affect various life domains, from physical health to daily living, friends, family situations, and education, and are associated with greater unemployment and economic problems (Wykes et al., 2021 ).
In order to plan and carry out successful mental health care, it is necessary to have a good mental health information system that also includes data about related needs (Wykes et al., 2021 ). When a need is identified, an action can be (re)organized to address it. Such action, based on the needs identified by the affected individuals, professionals or society, results in either satisfaction or dissatisfaction if the needs continue to be present (Endacott, 1997 ). Assessing needs might also be used to assess the adequacy and prioritization of mental health services at the population level (Ashaye et al., 2003 ; Hamid et al., 2009 ) as well as for the evaluation of mental health care (Hamid et al., 2009 ).
When considering mental health, a need represents a gap between what is and what should be (Witkin & Altschuld, 1995 ), and any changes that are made to the system should thus work to reduce this gap. There are various definitions of both “need” and “assessment” (Royse & Drude, 1982 ). Kahn (1969) considered needs from a social perspective to represent what someone requires in a broader bio-psycho-social context to be able to fully and productively participate in a social process (Royse & Drude, 1982 ). Brewin conceptualised needs (Lesage, 2017 ) as assessing what kind of social disability an individual has for professionals to be able to use an adequate model of care. Disability in this context is the result of interactions between people and the environment, and thus a disability can be seen as a lack of appropriate care models in relation to recognized needs. The concept of “need” in mental health care may be defined according to different points of view: a “normative need” is defined by professionals, while a “felt need” is what people with mental health problems experience and ask to be met (Endacott, 1997 ). What patients request and what they really need may differ, as they can only get what is available and provided at the system level, and what is the most beneficial for them in the current situation. Moreover, what they ask for is not always feasible. However, according to Bradshaw, what an individual requests is important and should be considered as felt needs (Endacott, 1997 ). Bearing in mind Maslow’s hierarchy of needs, only a combination of assessments from different points of view can provide a comprehensive needs assessment: needs assessed at the individual level from service users, their family members, caregivers, practitioners, and other professionals (Endacott, 1997 ). Indicators of needs at the individual level include functioning on different levels, symptoms, diagnoses, quality of life and, access to services (Aoun et al., 2004 ). Patient-centredness is vital to ensure the highest quality of care through monitoring performance (Kilbourne et al., 2018 ). Taking into account the patients’ perspective is also important to assess needs correctly, since such an assessment is more than just the professionals’ perception. An assessment of needs, as Thornicroft ( 1991 ) pointed out, provides care in the community with an emphasis on the provider-user relationship as a key component through which effective care is organized (Carter et al., 1995 ). According to Slade ( 1994 ), the concept of a need in mental health has no single correct definition, but it should rather be seen s a “socially-negotiated concept” (Thornicroft & Slade, 2002 ). Additionally, needs have to be assessed through the bio-psycho-social model (Makivić & Klemenc-Ketiš, 2022 ), including not just medical needs but also a wide array of social needs.
Initially, the assessment of needs (Balacki, 1988 ) in the community was seen as an approach using different forms of analysis to gain insights into the use of services, characteristics of people, incidence and prevalence rates and indicators to recognize crucial determinants that lead to the worsening of mental health. The assessment of mental health needs in Western societies began in 1775 with the analysis of public health data contained in the case registers (Royse & Drude, 1982 ). In the mid-1970s, with the beginning of the transition to care for mental health in the community (and the launch of community mental health service organizations), needs assessment was required within the evaluation process to help meet the patients’ needs. Needs assessment also represents a crucial part of mental health planning (Royse & Drude, 1982 ), where different needs must be considered, especially those felt by individuals. At the end of seventies, Kimmel pointed out that this area of needs assessment had no systematic procedures (Royse & Drude, 1982 ). However, several mental health needs assessment tools have been developed over the last thirty years.
The MRC Needs for Care Assessment (NFCAS) (by Brewin, 1987) was the first attempt to introduce a standardized assessment of the needs of the severely mentally ill (Lesage, 2017 ). Subsequently, a reduced version of the instrument applicable to common mental disorders was developed – i.e., the Needs for Care Assessment Schedule-Community version (NFCAS-C) (Bebbington et al., 1996 ). The shortened version of NFCAS was the Cardinal Needs Schedule (CNS), which is used to assess needs to address them with appropriate interventions (Marshall et al., 1995 ). Later the self-administered Perceived Needs for Care Questionnaire (PNCQ) was developed for use at the population level (Meadows et al., 2000 ), while in 1995 the Camberwell Assessment of Need (CAN) (Phelan et al., 1995 ) was published. After this time the focus shifted more to people-centred approaches, and therefore the assessment of needs also moved beyond psychiatric symptomatology to bring in “consumers”, i.e. patients and their caregivers. Other scales have also been used as needs assessment tools, such as the HoNOS scale (Joska & Flisher, 2005 ) which was designed to evaluate the clinical and social outcomes of mental health care.
Needs assessment is not always a clear and straightforward process with one approach and one goal. Therefore, different tools and approaches may be used to assess needs from different perspectives at different levels and with the help of different tools. The problem with using different techniques is that there is a lack of comparability and a consequent danger of not using the needs assessment outcome data as intended (Stewart, 1979 ); thus, it is important to have a good overview of the available tools.
To the best of our knowledge, only six reviews on needs assessment in people with mental health problems have been published to date (Davies et al., 2018 , 2019 ; Dobrzyńska et al., 2008b ; Joska & Flisher, 2005 ; Keulen-de Vos & Schepers, 2016 ; Lasalvia et al., 2000b ). Four additional reviews focused on the general needs or general health needs of people without mental health problems (Asadi-Lari & Gray, 2005 ; Carvacho et al., 2021 ; Lasalvia et al., 2000a ; Ravaghi et al., 2023 ), which was not focus group of our review. Finally, another article was considered inadequate for this study’s purposes, as it was published in Polish (as the one above) and is not a review paper (Dobrzyńska et al., 2008a ). None of the reviews published thus far have focused on the different assessment tools available for assessing the needs of people with different mental disorders. To date, no study has attempted to review all the available published studies on the various needs assessment processes to systematize the topic. The reviews mentioned above deal with only one specific population (patients with first-episode psychosis; forensic patients), or with specific needs (need for mental health services, supportive care needs, or individual needs for care). Thus, this study aimed to review all studies addressing needs assessment tools specifically designed for people with mental health problems, regardless of their diagnoses. The added value of this study is especially because of its wholeness in presenting different tools that can be used on different populations and by different groups. Thus this study may serve as a framework for starting different needs-assessment processes.
Search strategy
A comprehensive literature search using the Boolean operators “Mental health” AND “Needs assessment” was conducted in electronic bibliographic databases PubMed [Needs Assessment (Mesh Terms) AND Mental Health (Mesh Terms); Mental Health (Title/Abstract) AND Needs assessment (Title/Abstract);] and PsychINFO [Needs assessment AND Mental health in keywords; Needs assessment AND Mental health in Title; Needs assessment AND Mental health in Abstract]. Searching was carried out with the inclusion of all results without time or other limits in August 2021. The search strategy was based on the needs from a clinical context as well as some research priorities in the field of mental health. After the first systematic search we collected additional papers with an overview of six review articles (Davies et al., 2018 , 2019 ; Dobrzyńska et al., 2008b ; Joska & Flisher, 2005 ; Keulen-de Vos & Schepers, 2016 ; Lasalvia et al., 2000b ) and their results, and by searching PubMed within all connected articles. This was important since keywords changed over all this broad timeframe.
Inclusion and exclusion criteria
Our research exclusively focused on quantitative studies. We thus excluded all theoretical/conceptual articles, editorials, books, book commentaries or dissertations. Studies assessing the needs of patients with dementia and groups of people with physical and psychological disabilities were also excluded. We did not include papers related to 1) only general health (care), 2) other needs of the general population, 3) screening, prevalence, general diagnostic tools, and 4) tools for assessing caregivers’ needs. All those steps were done comprehensively by two researchers (IM, AK) independently. When there was a disagreement on the inclusion or exclusion of an article, both researchers looked at it again before reaching a consensus. We then manually added all relevant articles that could have been missed during the electronic search. We added articles that were cited within or were related with all the six mentioned reviews, but were not yet retrieved in the first search. These review articles were not included in the final number of all the articles examined in this study with the aim of exploring the different tools used for needs assessment of people with mental health problems. The aim of this process is to first obtain an overview of all the tools available, as this will make it possible to better use them within clinical settings, as well as for research and development purposes in order to plan a system or intervention that addresses the recognized needs (Fig. 1 ).
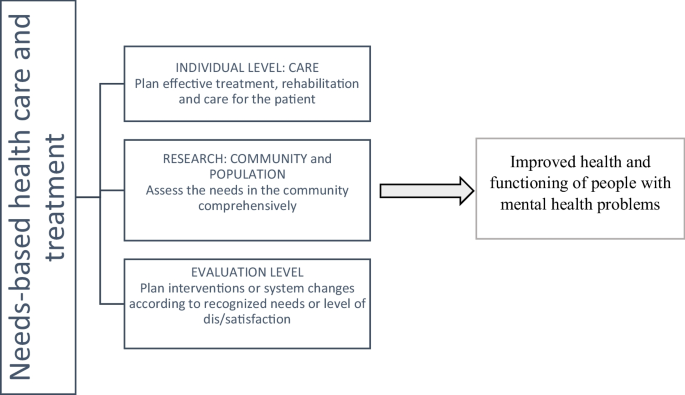
Concept of patient-centred care based on needs
Scoping studies, as Arksey and O'Malley ( 2005 ) mentioned, follow five steps, which we also took into consideration. First (step one) we identified the research question, which was “What are all different needs assessment tools that have been used in the population of people with mental health problems within different studies”. We then identified the relevant studies within recognised databases, as well as manually searching and adding the relevant articles (step two). We selected the appropriate studies (step three) as described within the search strategy process, with all inclusion and exclusion criteria. Finally, we presented the results (step four) in the chart flow in Fig. 2 , and Tables 1 , 2 and 3 , which corresponds to the concept of patient-centred care based on needs (Fig. 1 ). Because our focus was on different tools, we prepared the tables accordingly. There was no other relevant information in the original 242 articles to be presented at this occasion, other than those about the usage of different needs assessment tools, as this was the goal of the scoping review. The presentation of the results is based on the use of all recognized needs assessment tools, since geographical studies have been presented elsewhere (Makivić & Kragelj, 2023 ).
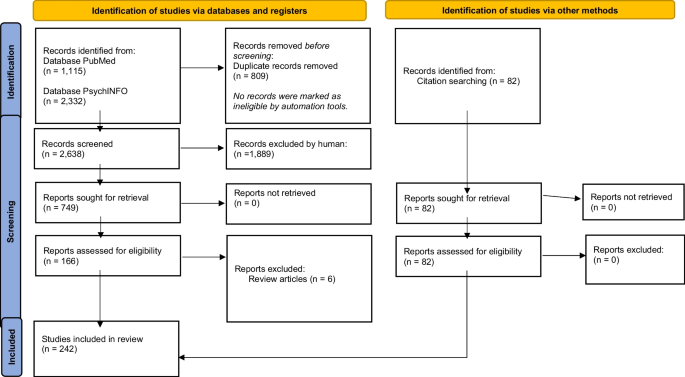
Research process within the databases
The analysis was multi-structured to provide an overview of all the recognized tools and the related time trends, country use and population of the most frequently used assessment methods.
The study selection process is shown in Fig. 2 . PubMed provided 578 records within the Mesh search and 537 within the title/abstract search, with after duplicates were removed this gave 1,090 results. Searching in PsychINFO provided 650 results from a search within the Abstract, 232 within Keywords and 1450 within Title; after combining these and removing duplicates, a total of 1,548 results were obtained.
The first selection was made within the final database (n = 2,638) by reading the abstracts and excluding all studies covering topics not relevant for this review. After this was completed, 166 articles remained. These were reviews and research articles covering the needs assessment of people with mental disorders (MD). After this, we eliminated review articles (n = 6) and used them for additional search to manually add all relevant articles that could have been missed during the electronic search, mainly because of the use of different keywords. Specifically, we added the articles that were cited within or were related to all the six mentioned reviews, but were not found in the first search (n = 82). After this process, a total of 242 articles were included in the final review.
Most studies addressing needs assessment tools retrieved with both electronic and manual searches were published in English (n = 231), although some were published in German (n = 3), Spanish (n = 3), and Italian (n = 2). Only one article each was published in Dutch, French and Turkish. Regarding the geographical distribution, most studies were published from European groups (n = 163), while 43 studies were conducted in America, 22 in Australia or New Zealand, 11 in Asia and only three in Africa. Some of the studies were published in collaboration among researchers from different countries. Regarding the publication period, the first studies on this issue were published in 1978, 52.9% of the studies were published from 2000 to 2012, and 66.1% had been published further by 2016.
Through the search performed in this study we found 29 different needs assessment tools, as shown in Table 1 in alphabetical order. We have made and additional search in order to find original sources and the information about the validation. Original sources for each of the recognized tools are listed in Supplementary information ( SI 1 ). Some tools, additional to those 29, were developed for the purposes of a single research study and its specific aims and the information about the validation were not available (n = 11), and thus we eliminated those tools at this point, although they will later be presented elsewhere in another study.
The retrieved tools and their respective constructs of need are presented in Table 2 . The various needs assessment tools are listed in alphabetical order. The tools are presented with regard to (1) who can answer the scale, (2) who the target population is, and (3) the domains addressed. Table 2 provides information on the various needs assessment tools, listed in alphabetical order. The tools are presented with regard to (1) who can answer the scale, (2) who the target population is, and (3) the domains addressed.
Service needs (Hamid et al., 2009 ) are defined as care requirements for prevention, treatment and rehabilitation. These needs can either be assessed by waiting lists or by only asking a simple question (e.g. “Do you think that you require any professional mental health services?”) along with the screening for mental and physical health problems (Yu et al., 2019 ) or social problems, with the help of the tools listed below. Moreover, there are different bio-psycho-social needs that are related to various mental health, physical health, and quality of life factors, as well as personal interests or abilities and social factors (Keulen-de Vos & Schepers, 2016 ), and these can be measured for different purposes. Social needs can be assessed by tools such as the Social Behavioral Schedule or REHAB Schedules, and therefore the need for rehabilitation can also be assessed (Hamid et al., 2009 ) using the comprehensive tools mentioned in our review.
Most of the needs assessment tools were self-completed by the patients (n = 85), completed by professionals (n = 41), or by combination of both (n = 78). Some tools were also completed by the patients and their caregivers (n = 12) or by the patients, caregivers, and professionals at the same time (n = 12). There were few studies where the researchers completed the needs assessment tool (n = 5). The majority of the tools were developed for assessing needs in an adult population with mental health problems (n = 193), either with severe mental disorders or with some other mental health diagnosis. Seventeen studies focused on an elderly population with mental health problems, and six on children with mental health problems. Some needs assessment tools for specific populations were found, such as tools for assessing the needs of forensic patients with mental health problems (n = 18), homeless people and migrants with a mental health diagnosis (n = 4), and mothers or pregnant women with a severe mental disorder (n = 1). In some studies, there was a combination of all these different populations and even people without a diagnosis, which we assigned to each of the mentioned groups.
In the second Supplementary information ( SI 2 ) there are reported the studies found in the literature search that used recognized needs assessment tools (n = 227). In this presentation some of the studies are not presented, namely those without validated tools (n = 11) as already mentioned and all articles using mentioned three different models (n = 4). In some studies, more tools have been used and in this case the study is counted within each tool in the total number of studies. Among the different needs-assessment tool, the CAN is mentioned as the most frequently used scale and, to the best of our knowledge, it has the highest number of different versions. The tools are presented based on their frequency of recognized use within this scoping review, from the most frequent to the least.
The recognized tools can be used in different contexts. Table 3 , groups the needs assessment tools according to their use at the care, research, and system levels.
This scoping review addressed all the published needs assessment tools specifically designed for use in mental health field. Nevertheless, some of the reviewed tools had also been used on the populations without a mental health diagnosis (Carvacho et al., 2021 ). Overall, we found twenty-nine different tools measuring needs in various mental health populations. The list of authors of the originally developed scales mentioned below are provided in the Supplementary information ( SI 1 ).
The reviewed literature highlights that the majority of needs assessment tools have been developed and used in Europe as the adoption of a community psychiatry model is relatively more widespread in this region than in other world regions; some tools, however, have been also used in America, Australia, and New Zealand.
Some scales had been developed with the aim to simplify or shorten previously published needs assessment tools, such as the Camberwell Assessment of Need (CAN) derived from the MRC Needs for Care Assessment Schedule. Similarly, the Difficulties and Needs Self-Assessment Tool was derived from the CAN, where some items are identical, some are a combination of several items of the CAN and some were added as new ones (on work, public places, family and friendship). Some tools, like the Montreal Assessment of Needs Questionnaire, were also developed from the CAN and had different aims, like enhancing data variability to broaden outcome measures for service planning, or simply because the organization of the related system is different and other tools are more appropriate. On the other hand, some tools are based on the CAN, but have been designed for use on a larger scale at the population level, like the Needs Assessment Scale. While most of the tools are used within health care services, the Resident Assessment Instrument Mental Health is a tool developed to support a seamless approach to person-centred health and social care. Some of the tools can also be used outside of the mental health field – such as the Child and Adolescent Needs and Strengths, which can be used in juvenile justice, intervention applications and child welfare – and the abovementioned CAN and others.
There are slightly different ideas regarding the needs and concepts about measuring needs. Many tools include a combination of needs assessed from different perspectives, such as the Bangor Assessment of Need Profile and the CAN. In some tools, like the Community Placement Questionnaire, it is predicted that various people rate the situation for one patient to eliminate any inaccuracies. On the other hand, some tools presented here, like the Self-Sufficiency Matrix, measure needs indirectly through self-sufficiency. When there is higher self-sufficiency for a certain life domain then there is less need presented for this area. Some tools, like Services Needed, Available, Planned, Offered, are complicated to use, since they include an investigation method with the review of the tool and assessment of the service use after the needs have been recognized. But this can be a good approach for the evaluation of the performance of community mental health centres about meeting the needs of their patients. Although we must bear in mind that such a tool is not directly transferable to every community mental health centre, as this depends on how each system is organized.
Needs can be evaluated according to different points of view, from patients themselves and their caregivers, as well as professionals. Studies show there are different outcomes based on the assessor (Lasalvia et al., 2000a , b , c ; Macpherson et al., 2003 ), and that professionals may see the needs differently to the users. Therefore, it is important not only what the tool is being used, but also who can complete it. Therefore, the most useful tools are the ones that can be used by various different people, so that the needs are assessed (also) from the patients’ standpoints (Larson et al., 2001 ).
Although the CAN is the most widely used tool, the research shows that sometimes there is not a very high agreement between staff and patients about needs, as was also found with the Health of the Nation Outcome Scales (HoNOS), which is the reason why some additional scales, such as the Profile of Community Psychiatry Clients, were developed. There are also some tools, such as the HoNOS, that indirectly measure needs for care, so they can be used as either a clinical or needs assessment tool.
Needs assessment tools are generally used by community psychiatry organizations and are also used to support changes to the organizations of countries’ related systems. The tools have already been used in order to assess the needs within clinical procedures, as well as at higher organizational levels in order to supplement services and direct programming (Royse & Drude, 1982 ). Different tools have good potential to evaluate community mental health services through assessing if patients’ needs have been met. Therefore, this study also aims at answering the question of which tool(s) can be most appropriate regarding different goals.
Within this review, we identified three systematic approaches to needs assessment which encompass different tools. The first is the DISC (Developing Individual Services in the Community) Framework (Smith, 1998 ), which includes the CAN and the Avon Self-Assessment Measure. The second is the Cumulative Needs for Care Monitor (Drukker et al., 2010 ), developed in order to choose the best treatment for each person. This one also uses the CAN and other more clinical tools and outcome measures (such as quality of life). The third is the Colorado Client Assessment Record (Ellis et al., 1984 ), which includes different measures of social functioning, such as the Denver Community of Mental Health Questionnaire, the Community Adjustment Profile, the Fort Logan Evaluation Screen, the Personal Role Skills Scale and the Global Assessment Scale.
This study has several strengths. First, we searched for as many tools and articles as possible. Second, we followed the standard rules of systematic and scoping reviews to present the data in a structured and non-biased manner: we thus searched for information extensively; the search was transparent and reproducible; the data were presented in a structured way. Finally, the scoping review was carried out, since the goal was not to compare and assess the quality of the evidence in the studies, but rather to review of all potential tools that can be used within the process of assessing the needs. Third, this study considered different populations, from severe mental disorders to other mental health problems, including addiction, which produced a strong overview of different tools and versions of the same tool used in other contexts. Fourth, the use of such tools also has a different basis depending on the goals of the system, so it can reflect the organization of care for mental health in a given country. The fifth strength of this work is that in addition to the original 242 articles within the review, we have also included all original sources for development of each of the 29 recognized tools.
This study also has some limitations. First, as the keywords are not same for every study, some studies could have been left out and therefore some tools might have been unrecognized. Second, our needs assessment review focuses on all people with mental health problems, even though the group of those with severe mental illness differs from the group with less severe mental health disorders. Therefore, no conclusion can be made on which tool is better for use in different population groups or disease severities. Third, we only included tools that assess the needs of people with mental health problems, although other tools for the general population could also potentially be useful. Fourth, some tools were developed and validated in only one country, so transferability is questionable or requires additional validation.
Since this scoping review provides insight into the evidence about the existence of different tools for needs assessment, it would also be valuable to conduct additional research on the level of each tool to see if it has already been validated and culturally adapted. To the best of our knowledge, the CAN is the most frequently used tool, and has been translated and adapted into more than 33 different languages (Phelan et al., 1995 ). Some of the tools reviewed in this study use items similar to the CAN, such as the Needs Assessment Scale (de Weert-van Oene et al., 2009 ). Some tools use the same items with a few additional ones, such as the Montreal Assessment of Needs Questionnaire (Tremblay et al., 2014 ), which shows even greater use of the CAN. Thus, the concepts in this latter tool are widely applied.
There are different fields in which certain needs must be addressed to deal with the mental health of the general population or the needs of the population with mental health problems, with the latter being our main focus. This review aimed to develop a tool for needs assessment that can be applied clinically and for research purposes. It is also vital to see what kind of tools can be used to assess needs for the purpose of a formative evaluation process, and the possibility of service development following the identification of actual needs (Makivić et al., 2021 ). Therefore, this article is valuable for a variety of final users, as it can be used by service providers at the level of health or social care, researchers, policymakers and other relevant stakeholders.
Moreover, it is also necessary to assess needs in the field of communication, especially targeting anti-stigma and anti-discrimination campaigns, and to assess the needs of educational systems (Kragelj et al., 2022 ) for the representation of mental health topics (Makivić et al., 2022 ). The use of different tools for assessing needs not only gives us the possibility of identifying such needs, but also establishes the possibility of meeting those needs when these tools are used within bio-psycho-socially oriented primary care or interdisciplinary-oriented mental health care. The assessment of needs at the individual level is important for the effective development of person-centred care plans (Martin et al., 2009 ). Patient-centred psychiatric practice is also needed to increase patient empowerment, which can be done with the help of a needs assessment process.
The review of all the tools for assessing different needs for people with mental health problems presented in this work is new, and therefore fills an important gap in the scientific knowledge of the needs assessment process in the field of mental health.
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
Aoun, S., Pennebaker, D., & Wood, C. (2004). Assessing population need for mental health care: A review of approaches and predictors. Mental Health Services Research, 6 (1), 33–46. https://doi.org/10.1023/b:mhsr.0000011255.10887.59
Article PubMed Google Scholar
Arksey, H., & O’Malley, L. (2005). Scoping studies: Towards a methodological framework. International Journal of Social Research Methodology, 8 (1), 19–32. https://doi.org/10.1080/1364557032000119616
Article Google Scholar
Asadi-Lari, M., & Gray, D. (2005). Health needs assessment tools: Progress and potential. International Journal of Technology Assessment in Health Care, 21 (3), 288–297. https://doi.org/10.1017/s0266462305050385
Ashaye, O. A., Livingston, G., & Orrell, M. W. (2003). Does standardized needs assessment improve the outcome of psychiatric day hospital care for older people? A randomized controlled trial. Aging & Mental Health, 7 (3), 195–199. https://doi.org/10.1080/1360786031000101166
Balacki, M. F. (1988). Assessing mental health needs in the rural community: A critique of assessment approaches. Issues in Mental Health Nursing, 9 (3), 299–315. https://doi.org/10.3109/01612848809140931
Bebbington, P., Brewin, C. R., Marsden, L., & Lesage, A. (1996). Measuring the need for psychiatric treatment in the general population: the community version of the MRC Needs for Care Assessment. Psychological Medicine, 26 (2), 229–236. https://doi.org/10.1017/s0033291700034620
Carter, M. F., Crosby, C., Geerthuis, S., & Startup, M. (1995). A client-centered assessment of need needs assessment. Journal of Mental Health, 4 (4), 383–394. https://doi.org/10.1080/09638239550037433
Carvacho, R., Carrasco, M., Lorca, M. B. F., & Miranda-Castillo, C. (2021). Met and unmet needs of dependent older people according to the Camberwell Assessment of Need for the Elderly (CANE): A scoping review. Revista Espanola De Geriatria y Gerontologia, 56 (4), 225–235. https://doi.org/10.1016/j.regg.2021.02.004
Davies, E. L., Gordon, A. L., Pelentsov, L. J., Hooper, K. J., & Esterman, A. J. (2018). Needs of individuals recovering from a first episode of mental illness: A scoping review. International Journal of Mental Health Nursing, 27 (5), 1326–1343. https://doi.org/10.1111/inm.12518
Davies, E. L., Gordon, A. L., Pelentsov, L. J., & Esterman, A. J. (2019). The supportive care needs of individuals recovering from first episode psychosis: A scoping review. Perspectives in Psychiatric Care, 55 (1), 6–14. https://doi.org/10.1111/ppc.12259
de Weert-van Oene, G. H., Havenaar, J. M., & Schrijvers, A. J. (2009). Self-assessment of need for help in patients undergoing psychiatric treatment. Psychiatry Research, 167 (3), 221–230. https://doi.org/10.1016/j.psychres.2008.02.001
Dobrzyńska, E., Rymaszewska, J., & Kiejna, A. (2008a). CANSAS-Krótka Ocena Potrzeb Camberwell oraz inne narzedzia oceny potrzeb osób z zaburzeniami psychicznymi [CANSAS-Camberwell Assessment of Need Short Appraisal Schedule and other needs of persons with mental disorders assessment tools]. Psychiatria Polska, 42 (4), 525–532.
PubMed Google Scholar
Dobrzyńska, E., Rymaszewska, J., & Kiejna, A. (2008b). Potrzeby osób z zaburzeniami psychicznymi–definicje, przeglad badań [Needs of persons with mental disorders-definitions and literature review]. Psychiatria Polska, 42 (4), 515–524.
Drukker, M., Bak, M., Campo, J.à, Driessen, G., Van Os, J., & Delespaul, P. (2010). The cumulative needs for care monitor: a unique monitoring system in the south of the Netherlands. Social Psychiatry and Psychiatric Epidemiology , 45 (4), 475–485. https://doi.org/10.1007/s00127-009-0088-3
Ellis, R. H., Wilson, N. Z., & Foster, F. M. (1984). Statewide treatment outcome assessment in Colorado: The Colorado Client Assessment Record (CCAR). Community Mental Health Journal, 20 (1), 72–89. https://doi.org/10.1007/BF00754105
Endacott, R. (1997). Clarifying the concept of need: A comparison of two approaches to concept analysis. Journal of Advanced Nursing, 25 (3), 471–476. https://doi.org/10.1046/j.1365-2648.1997.1997025471.x
Hamid, W. A., Lewis-Cole, K., Holloway, F., & Silverman, M. (2009). Older people with enduring mental illness: A needs assessment tool. Psychiatric Bulletin, 33 (3), 91–95. https://doi.org/10.1192/pb.bp.107.017392
Joska, J., & Flisher, A. J. (2005). The assessment of need for mental health services. Social Psychiatry and Psychiatric Epidemiology, 40 (7), 529–539. https://doi.org/10.1007/s00127-005-0920-3
Keulen-de Vos, M., & Schepers, K. (2016). Needs assessment in forensic patients: A review of instrument suites. International Journal of Forensic Mental Health, 15 (3), 283–300. https://doi.org/10.1080/14999013.2016.1152614
Kilbourne, A. M., Beck, K., Spaeth-Rublee, B., Ramanuj, P., O’Brien, R. W., Tomoyasu, N., & Pincus, H. A. (2018). Measuring and improving the quality of mental health care: A global perspective. World Psychiatry: Official Journal of the World Psychiatric Association (WPA), 17 (1), 30–38. https://doi.org/10.1002/wps.20482
Kragelj, A., Pahor, M., Zaletel-Kragelj, L., & Makivic, I. (2022). Learning needs assessment among professional workers in community mental health centres in Slovenia: Study protocol. South Eastern European Journal of Public Health , Special Volume No. 1 . https://doi.org/10.11576/seejph-5478
Larson, A., Frkovic, I., van Kooten-Prasad, M., & Manderson, L. (2001). Mental health needs assessment in Australia’s Culturally Diverse Society. Transcultural Psychiatry, 38 (3), 333–347. https://doi.org/10.1177/136346150103800304
Lasalvia, A., Stefani, B., & Ruggeri, M. (2000a). I bisogni di cura nei pazienti psichiatrici: una revisione sistematica della letteratura. I. Concetti generali e strumenti di valutazione. I bisogni di servizi [Therapeutic needs in psychiatric patients: a systematic review of the literature. I. General concepts and assessment measures. Needs for services]. Epidemiologia e Psichiatria Sociale , 9 (3), 190–213. https://doi.org/10.1017/s1121189x00007879
Lasalvia, A., Stefani, B., & Ruggeri, M. (2000b). I bisogni di cura nei pazienti psichiatrici: una revisione sistematica della letteratura. II. I bisogni di cura individuali [Needs for care in psychiatric patients: a systematic review. II. Needs for care on individual]. Epidemiologia e Psichiatria Sociale , 9 (4), 282–307. https://doi.org/10.1017/s1121189x00008411
Lasalvia, A., Ruggeri, M., Mazzi, M. A., & Dall'Agnola, R. B. (2000). The perception of needs for care in staff and patients in community-based mental health services. The South-Verona Outcome Project 3. Acta Psychiatrica Scandinavica , 102 (5), 366–375. https://doi.org/10.1034/j.1600-0447.2000.102005366.x
Le Grand, D., Kessler, E., & Reeves, B. (1996). The avon mental health measure. Mental Health Review Journal, 1 (4), 31–32. https://doi.org/10.1108/13619322199600042
Lesage, A. (2017). Populational and individual perspective on needs. Epidemiology and Psychiatric Sciences, 26 (6), 609–611. https://doi.org/10.1017/S204579601700049X
Article PubMed PubMed Central Google Scholar
Macpherson, R., Varah, M., Summerfield, L., Foy, C., & Slade, M. (2003). Staff and patient assessments of need in an epidemiologically representative sample of patients with psychosis-staff and patient assessments of need. Social Psychiatry and Psychiatric Epidemiology, 38 (11), 662–667. https://doi.org/10.1007/s00127-003-0669-5
Makivić, I., & Klemenc-Ketiš, Z. (2022). Development and validation of the scale for measuring biopsychosocial approach of family physicians to their patients. Family Medicine and Community Health, 10 (2), e001407. https://doi.org/10.1136/fmch-2021-001407
Makivić, I., & Kragelj, A. (2023). Needs assessment tools at the field of mental health: Countries presentation. V: Conference abstract book: 11th European Conference on Mental Health [S. l. ]: Evipro, Str. Ljubljana, Slovenia, p. 184.
Makivić, I., Švab, V., & Selak, Š. (2021). Mental health needs assessment during the COVID-19 Pandemic: Consensus based on Delphi Study. Frontiers in Public Health, 9 , 732539. https://doi.org/10.3389/fpubh.2021.732539
Makivić, I., Kragelj, A., & Selak, Š. (2022). Educational needs assessment in the field of mental health: Review of the tools. V: 10th European conference on mental health: Conference abstract boo k. Evipro, Str. Lisbon, Portugal, Helsinki, pp. 183–184.
Marshall, M., Hogg, L. I., Gath, D. H., & Lockwood, A. (1995). The cardinal needs schedule-a modified version of the MRC needs for care assessment schedule. Psychological Medicine, 25 (3), 605–617. https://doi.org/10.1017/s0033291700033511
Martin, L., Hirdes, J. P., Morris, J. N., Montague, P., Rabinowitz, T., & Fries, B. E. (2009). Validating the Mental Health Assessment Protocols (MHAPs) in the Resident Assessment Instrument Mental Health (RAI-MH). Journal of Psychiatric and Mental Health Nursing, 16 (7), 646–653. https://doi.org/10.1111/j.1365-2850.2009.01429.x
McGorry, P. D., & Hamilton, M. P. (2016). Stepwise expansion of evidence-based care is needed for mental health reform. The Medical Journal of Australia, 204 (9), 351–353. https://doi.org/10.5694/mja16.00120
Meadows, G., Harvey, C., Fossey, E., & Burgess, P. (2000). Assessing perceived need for mental health care in a community survey: Development of the Perceived Need for Care Questionnaire (PNCQ). Social Psychiatry and Psychiatric Epidemiology, 35 (9), 427–435. https://doi.org/10.1007/s001270050260
Munn, Z., Peters, M. D. J., Stern, C., Tufanaru, C., McArthur, A., & Aromataris, E. (2018). Systematic review or scoping review? Guidance for authors when choosing between a systematic or scoping review approach. BMC Medical Research Methodology, 18 (1), 143. https://doi.org/10.1186/s12874-018-0611-x
Phelan, M., Slade, M., Thornicroft, G., Dunn, G., Holloway, F., Wykes, T., Strathdee, G., Loftus, L., McCrone, P., & Hayward, P. (1995). The Camberwell assessment of need: The validity and reliability of an instrument to assess the needs of people with severe mental illness. The British Journal of Psychiatry: The Journal of Mental Science, 167 (5), 589–595. https://doi.org/10.1192/bjp.167.5.589
Ravaghi, H., Guisset, A. L., Elfeky, S., Nasir, N., Khani, S., Ahmadnezhad, E., & Abdi, Z. (2023). A scoping review of community health needs and assets assessment: Concepts, rationale, tools and uses. BMC Health Services Research, 23 (1), 44. https://doi.org/10.1186/s12913-022-08983-3
Royse, D., & Drude, K. (1982). Mental health needs assessment: Beware of false promises. Community Mental Health Journal, 18 (2), 97–106. https://doi.org/10.1007/BF00754454
Slade M. (1994). Needs assessment. Involvement of staff and users will help to meet needs. The British journal of psychiatry: the journal of mental science, 165 (3), 293–296. https://doi.org/10.1192/bjp.165.3.293
Smith, H. (1998). Needs assessment in mental health services: The DISC framework. Journal of Public Health Medicine, 20 (2), 154–160. https://doi.org/10.1093/oxfordjournals.pubmed.a024736
Stewart, R. (1979). The nature of needs assessment in community mental health. Community Mental Health Journal, 15 , 287–295. https://doi.org/10.1007/BF00778708
Thornicroft, G. (1991). The concept of case management for long-term mental illness. International Review of Psychiatry, 3 (1), 125–132. https://doi.org/10.3109/0954026910906752
Thornicroft, G., & Slade, M. (2002). Comparing needs assessed by staff and by service users: Paternalism or partnership in mental health? Epidemiologia e Psichiatria Sociale, 11 (3), 186–191. https://doi.org/10.1017/s1121189x00005704
Tremblay, J., Bamvita, J. M., Grenier, G., & Fleury, M. J. (2014). Utility of the Montreal assessment of need questionnaire for community mental health planning. The Journal of Nervous and Mental Disease, 202 (9), 677–687. https://doi.org/10.1097/NMD.0000000000000180
Witkin, B. R., & Altschuld, J. W. (1995). Planning and Conducting Needs Assessments: A Practical Guide . Sage Publications. https://doi.org/10.1177/002087289603900316
Wykes, T., Bell, A., Carr, S., Coldham, T., Gilbody, S., Hotopf, M., Johnson, S., Kabir, T., Pinfold, V., Sweeney, A., Jones, P. B., & Creswell, C. (2021). Shared goals for mental health research: what, why and when for the 2020s. Journal of Mental Health (Abingdon, England) , 1–9. Advance online publication. https://doi.org/10.1080/09638237.2021.1898552
Yu, J. Y., Dong, Z. Q., Liu, Y., Liu, Z. H., Chen, L., Wang, J., Huang, M. J., Mo, L. L., Luo, S. X., Wang, Y., Guo, W. J., He, N., Chen, R., & Zhang, L. (2019). Patient-doctor concordance of perceived mental health service needs in Chinese hospitalized patients: a cross-sectional study. Annals of Palliative Medicine , 8 (4), 442–450. https://doi.org/10.21037/apm.2019.08.06
Download references
This work was supported by the Slovenian Research Agency (project No.: Z3-2652).[Display Image Removed]. Project was funded by the Reseach agency. Only IM was paid from this. But the project didn't finance the outcomes and the goal of publishing this work was solely for the research purposes.
Author information
Authors and affiliations.
National Institute of Public Health, Ljubljana, Slovenia
Irena Makivić & Anja Kragelj
Section of Psychiatry, Department of Neuroscience, Biomedicine and Movement Sciences, University of Verona, Verona, Italy
Antonio Lasalvia
You can also search for this author in PubMed Google Scholar
Contributions
Conceptualization: [Irena Makivić]; Methodology: [Irena Makivić]; Formal analysis and investigation: [Irena Makivić], [Anja Kragelj]; Writing—original draft preparation: [Irena Makivić]; Writing—review and editing: [Irena Makivić], [Anja Kragelj], [Antonio Lasalvia]; Funding acquisition: [Irena Makivić]; Resources: [Irena Makivić]; Supervision: [Antonio Lasalvia].

Corresponding author
Correspondence to Irena Makivić .
Ethics declarations
There are no financial or non-financial interests that are directly or indirectly related to the work submitted for publication. All authors have no relevant financial or non-financial interests to disclose.
There was no need to apply for ethical committee or for informed consent, since there were no humans directly involved in this scoping review.
Embargoes on data sharing are permitted.
Additional information
Publisher's note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file1 (PDF 432 KB)
Supplementary file2 (pdf 556 kb), rights and permissions.
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/ .
Reprints and permissions
About this article
Makivić, I., Kragelj, A. & Lasalvia, A. Quantitative needs assessment tools for people with mental health problems: a systematic scoping review. Curr Psychol 43 , 19996–20013 (2024). https://doi.org/10.1007/s12144-024-05817-9
Download citation
Accepted : 27 February 2024
Published : 12 March 2024
Issue Date : June 2024
DOI : https://doi.org/10.1007/s12144-024-05817-9
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Needs assessment
- Mental health
- Patient-centred care
- Find a journal
- Publish with us
- Track your research
- Systematic Review
- Open access
- Published: 18 December 2023
Utilising quantitative methods to study the intersectionality of multiple social disadvantages in women with common mental disorders: a systematic review
- Nadia Alhamd Alghamdi 1 , 2 ,
- Kirsty Dunn 1 , 2 ,
- Deborah Cairns 1 , 2 &
- Craig Melville 1 , 2
International Journal for Equity in Health volume 22 , Article number: 264 ( 2023 ) Cite this article
2033 Accesses
1 Citations
9 Altmetric
Metrics details
Women are at greater risk of common mental disorders. The intersectionality concept provides a framework to examine the effects of multiple social disadvantages on women’s mental health. We conducted a systematic review to collect and analyse information to identify the quantitative methodologies and study designs used in intersectional research to examine women’s mental health and multiple social disadvantages. Included studies used accepted statistical methods to explore the intersectional effects of gender and one or more types of social disadvantage from the PROGRESS-Plus inequity framework: a place of residence, race/ethnicity, occupation, gender/ sex, religion, education, socioeconomic status, social capital (O’Neill et al. J Clin Epidemiol 67:56–64, 2014). The scope of this systematic review was limited to studies that analysed common mental disorders in women and men comparatively. Studies focusing on only one gender were excluded, ensuring a comprehensive comparative analysis of the intersection of social disadvantages in mental health.
Twelve papers were included in the narrative synthesis (Table 1). Eight of the included papers (67%) reported an intersectional effect of gender and one or more additional types of social disadvantage. The multiplicative effect of gender and socioeconomic status on the risk of common mental disorders was the most commonly reported interaction. This systematic review shows that multiplicative and simultaneous interactions of multiple social disadvantage increase the risk of common mental disorders experienced by women. Moreover, it underlines the potential for quantitative research methods to complement qualitative intersectionality research on gender and mental health. The findings of this systematic review highlight the importance of multiple social disadvantage in understanding the increased risk of mental health experienced by women.
Introduction
Encompassing a state of complete physical, mental, and social well-being [ 1 ], women’s health plays an essential role in the health and well-being of modern society. Evidence from existing literature on women’s health suggests that healthier women lead to better-educated and more productive societies, as well as influencing the pace of economic growth and societal development [ 2 ]. Further evidence suggests that women’s health also crucially impacts the health and economic well-being of future generations [ 2 ]. While it is evident that healthy women are a cornerstone of healthy societies, globally, women continue to experience poor health [ 3 ].
A compelling body of evidence has identified social inequalities to have a crucial impact on women’s health and access to health care. These inequalities are based on gender, age, income, race, disability, sexuality, ethnicity, and class, which are considered to shape a woman’s exposure to health risks and access to health services [ 4 , 5 , 6 , 7 ] & World Health Organization [ 8 ]. It is important to acknowledge that these social inequalities rarely impact women’s health in a unilateral way; instead, they experience multiple social disadvantages that substantially impact women’s health.
Health inequality, a global issue, often follows a social gradient where advantaged groups with more resources tend to be healthier [ 9 ]. These inequalities extend to mental health, affecting aspects like socioeconomic status, gender, and gender identity [ 9 ]. Mental disorders are prevalent in women worldwide [ 8 ], with women experiencing a higher rate of internalising disorders such as depression and anxiety than men [ 10 ]. Studies show significant differences in mental health across countries and genders, with worse mental health observed in women, lower socioeconomic groups, and individuals with weak support networks [ 11 ]. Sexuality and ethnicity also impact mental health [ 12 ]. However, the effects of these social determinants on health are intricate and interconnected, extending beyond the simple sum of their individual effects.
The theory of intersectionality is a framework which seeks to understand the interactions between multiple social identities such as race, gender/sex, and class to create unique forms of discrimination, oppression, inequality, and social justice. Originally a Black feminist theory, this approach was the first to propose there was mutuality between factors that could not be understood within the context of research which sought to analyse one factor at a time [ 13 , 14 ]. With regard to population health, the concept of intersectionality has much to offer. Indeed, it was recently recognised as an important framework for public health in providing accuracy in identifying inequalities, developing intervention strategies, and ensuring results of interventions are relevant within specific communities, outcomes that cannot always be sought from methods focusing on the unitary cause [ 13 ].
In qualitative designs within feminist studies, intersectionality provides a vital lens for understanding social phenomena by underlining the interconnected social identities and their affiliated forms of oppression [ 15 ]. From an epistemic perspective, intersectionality provides a more thriving, multifaceted analysis that allows for a subtle understanding of lived experiences, giving a voice to individuals who represent intersecting identities [ 16 ]. Furthermore, it highlights contextual factors such as socio-political systems and cultural norms that influence these experiences [ 16 ]. It allows the researcher to examine and address the layers of inequalities individuals face at the intersections of multiple marginalisation’s [ 14 ].
Despite such concerns about people’s lived reality and personal experience, adopting a quantitative approach to investigate intersectionality has several advantages such as estimating the effect measure of statistical relationship between factors or variables. However, employing this theoretically rich technique in population health research nevertheless has limitations and methodological challenges [ 17 ]. There are concerns, for example, about how quantitative terms used mathematically in a theoretical study can provoke difficulties concerning how to interpret intersectionality effects in research and how quantitative interpretation will reflect on the analysis and measurement of the outcome results [ 13 ]. As such, further investigation is required to determine the most appropriate quantitative approach (es), analytical method(s), and technique(s) for quantitative studies of intersectionality and to determine what would enable the integration of intersectional theory in a way that addresses the inequity about incorporating intersectionality in quantitative research [ 18 ].
This systematic review thus collects and examines evidence to do the following:
Identify the quantitative methods and study designs used in intersectional research to understand women’s mental health and social disadvantage.
Determine whether these techniques help understand women’s mental health and social disadvantage.
Analyse and underline the most significant statistical challenges in quantitative intersectionality studies, highlighting methodological limitations and the strength of using the quantitative methods.
Assess and classify the overall strength and validity of using an intersectionality framework in quantitative research, focusing on its contributions to women’s mental health and social disadvantage.
The systematic review was conducted in adherence with the Preferred Reporting Items for Systematic Reviews and Meta-analysis (PRISMA) guidelines [ 19 ] and the Cochrane Handbook for Systematic Review of Interventions [ 20 ]. No protocol for this review has been published.
Search strategy
A search strategy (see Additional file 1 : Appendix 1) was developed with the help of a research librarian specialist, and the following electronic databases were searched during December 2019 and updated on 30 June 2022: Medline, EMBASE, CINAHL, PsycINFO, and Sociological Abstract. Hand searching for journals was also conducted during the same period, including articles and papers that suit the search terms in printed journals or general web searches to find niche journals that might not cover academic electronic databases such as Journal of Mental Health , Journal of Health and Social Behaviour , Social Science and Medicine and the British Journal of Psychiatry . The search strategy was developed using detailed search terms to capture the essence and key aspects of this systematic review. These aspects include:
Gender and its synonyms;
Social disadvantage and its synonyms;
Intersectionality and its synonyms;
Common mental disorders.
Gender keywords were adopted from the ‘Development of a PubMed-Based Search Tool for Identifying Gender and Gender-Specific Health Literature’ [ 21 ]. Keywords for ‘common mental disorder’ (CMD) were chosen from the study’ Recruitment and Retention Strategies in Mental Health Trials–A Systematic Review’ [ 22 ]. Social disadvantage keywords were developed from the PROGRESS-Plus inequity framework [ 23 ]. In collaboration with my primary academic advisor, we carefully selected keywords to cover the meaning of intersectionality. After this preparation, we searched each eligible paper using specific terms such as ‘intersectionality’, ‘intersectional’ and ‘intersection’ along with terms such as ‘inequal’, ‘social inequal’, ‘marginalise’, ‘multiple inequality’, and ‘inequity’.
It is important in this systematic review to broadly define the concepts of sex and gender when examining potential differences between men and women. Sex refers to the biological characteristics that distinguish males, females and intersex, and these characteristics include hormone variations, reproductive organs, and chromosomes [ 24 , 25 ]. Gender, however, is a psychosocial construct that encompasses societal expectations, roles, relationships, behaviours, attributes, and opportunities considered suitable for men and women [ 24 , 25 ]. Furthermore, gender identity refers to an individual’s understanding and psychological connection to the societal categories and expectations relating to gender, regardless of whether they accept or reject these expectations [ 26 ].
Study selection
The inclusion and exclusion criteria to determine eligible studies are listed below.
Inclusion criteria:
Quantitative Methodologies : Studies employed one of quantitative method: cross-sectional, observational, cohort, and controlled studies. The main focus of the systematic review is to capture the utilisation of intersectionality in quantitative research techniques. Therefore, only quantitative studies will be considered for incorporation into the analysis.
Participants : Studies including both male and female participants were considered eligible. This criterion allows exploring gender-based disparities in mental health outcomes across diverse populations.
Age : Studies has participants aged 18 years and older were included to ensure relevance to adult populations.
Social Disadvantage : Eligible studies examined the relationship between two or more types of social disadvantage, as defined within the PROGRESS-Plus framework (Place of residence, Race/ethnicity, Occupation, Gender/sex, Religion, Education, Socioeconomic status, Social capital).
Analytical Methodologies : Studies that used one of the following analytical strategies used in quantitative intersectionality research [ 17 ], including studies that do not explicitly adopt the intersectionality framework but still examine the influence of multiple social identities and the intersection effect:
Statistical interactions
Moderators in meta-analysis
Multilevel modelling
Moderated mediation
Person-centred methods
Decomposition analysis.
Outcome : The study outcomes focused on common mental disorders as defined by the Mental Health Foundation, including Depression, Generalised Anxiety Disorder (GAD), Social Anxiety Disorder, Panic Disorder, Obsessive-Compulsive Disorder (OCD), Post-Traumatic Stress Disorder (PTSD), and Phobias.
Language : Only studies published in English were included in this review.
Exclusion criteria
Qualitative Studies : Qualitative research was excluded from this systematic review as our focus was on quantitative methodologies.
Conference Abstracts : Conference abstracts were excluded to ensure that the included studies provided sufficient data for a comprehensive analysis.
Lab-based Studies : Laboratory-based studies were excluded due to concerns related to lack of these type of studies on capturing intersectionality and social disadvantages.
Single-gender Studies : Include only males or females are excluded to ensure a comprehensive investigation of social identities and experiences to align with the intersectionality framework. However, it is important to recognise that this decision has limited the number of eligible studies and potentially influenced the results.
Myself (NA) the first author, and the primary supervisor (CM) independently reviewed the titles and abstracts of the identified records. A consensus discussion resolved disagreements about inclusion/exclusion. In the second stage, my supervisor and I independently completed inclusion and exclusion checklists for each full-text paper. The level of agreement was 40%, with a Cohen’s kappa of 0.4, and disagreement was resolved through a consensus discussion.
Data extraction
A data extraction form was designed specifically to identify certain information (i.e., country, sampling period, sample size, age, gender, participant characteristics, type of social disadvantage) using PROGRESS-Plus (a data extraction file was piloted and revised before final use). This review was designed to examine ways of incorporating intersectionality into quantitative methods regarding social disadvantage and mental health. The first author (NA) extracted data from all included studies, with assistive collaboration from the primary supervisor (CM) who also independently extracted data from half of the included articles. A dual review (NA)/(CM) compared extracted data, and disagreements were resolved through consensus discussion.
Quality assessment
The quality of the included articles was assessed with the Standard Quality Assessment Criteria – the most suitable tool for evaluating quantitative and qualitative research papers from various fields [ 27 ]. This assessment includes 14 questions to evaluate the study (e.g., Is the study design evident and appropriate? Is the objective of the study sufficiently described?). Each study has a summary score in the range of 0-1.0, with a higher score representing better quality.
The search strategy generated a total of 5530 potentially relevant articles. Of these, 439 duplicates were identified and removed. Of the remaining 5091 potentially relevant articles, 4972 studies were screened against title and abstract. The resultant 114 papers were assessed for title and abstract review eligibility, and 70 were excluded for not meeting the specified inclusion and exclusion criteria. In sum, 44 articles were considered for full-text eligibility, and 12 were deemed suitable for the narrative synthesis (see the flow diagram in Fig. 1 ).
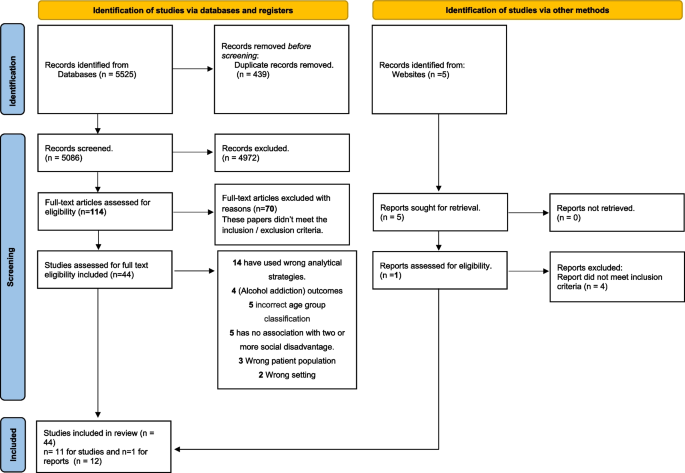
PRISMA flow diagram of the study selection process (2022)
Summary of study characteristics
Of the suitable 12 studies, three were conducted in the United States of America [ 28 , 29 , 30 ], two in Scotland [ 31 , 32 ], one multinational study was conducted in Russia, Poland and Czech Republic [ 33 ] and one study was conducted in each of the following countries: Brazil [ 34 ], Iran [ 35 ], Canada [ 36 ], Sweden [ 37 ], United Kingdom [ 38 ], and Czech Republic [ 39 ].
The population’s race was reported in four studies [ 28 , 30 , 34 , 38 ], with the reported groups being White, Black, Dark, African American, Native American, Asian, Hispanic and other race/ethnicities. Education level was reported in six studies, with this being school level (primary – university) in four studies [ 29 , 33 , 36 , 39 ]. In exploring education, different parameters were used. A single study investigated participant demographics using years of schooling (ranging from less than 4 to more than 12 years) [ 28 ]. In two separate studies, separate types were selected, including specified classifications as Low, Medium, or High [ 30 , 34 ]. Moreover, qualifications were explored, ranging from No qualification to A-level, as employed by Lewis et al. [ 38 ].
Employment status was reported in two studies – by manual or non-manual occupation in one study [ 31 ] and full-time or part-time in the other [ 38 ]. Marital status was reported in seven studies – as single / married /divorced / widowed / never married in three studies [ 28 , 33 , 35 ]; married / cohabitating / formerly married (separated, divorced, or widowed) / never married in two studies [ 34 , 36 ], couple or single in one study [ 29 ], and one-person family units / couples with children / couples without children / single-parent households / respondents living with parents in one study [ 38 ]. Financial status was reported in six studies – as low income / not low income in one study [ 36 ], report of average net wealth in one study [ 28 ], report of financial difficulties and ownership of defined household items in one study [ 33 ], household per capita income in one study [ 34 ], mean household income in one study [ 29 ], and housing tenure and car access in one study [ 38 ].
Type of social disadvantage
Of the twelve overall papers, all reported on gender / gender identity, nine reported on socioeconomic status. Furthermore, six reported on education level, four reported on race / ethnicity, two reported on social cohesion / social ties, one reported on occupation, three reported on age, three reported on social class, and one study reported on marital status (Table 1 ), farther explanation of each study social disadvantages will be appeared in the summary.
Type of common mental disorders
All the studies reported affective disorders as common mental disorders, including depression / depressive symptoms / depressive mood / depressive thoughts, reported by [ 28 , 29 , 30 , 31 , 33 , 34 , 36 , 37 , 39 ], dysthymia [ 30 , 39 ], hypomanic and manic episodes [ 39 ] as common mental disorders. Studies also reported anxiety disorders, including social anxiety disorder by [ 33 , 34 , 36 , 39 ], anxiety/general anxiety disorder [ 31 , 39 ], panic disorder [ 36 , 39 ], obsessive-compulsive disorder [ 39 ], agoraphobia [ 36 , 39 ].
Multiple studies reported personality/behaviour disorders such as neurotic psychiatric disorder [ 38 ], anti-social personality disorder [ 30 ], conduct disorder [ 30 ], and bipolar disorder [ 36 ]. Furthermore, two studies [ 36 , 39 ] reported substance use disorders,1 study reported insomnia [ 32 ],one study reported somatic symptoms and decreased in vital energy [ 34 ], 1 study reported anxiety and alcohol use disorders [ 39 ], one study reported phobias [ 36 ], one study reported psychiatric distress [ 32 ], and 1 study [ 35 ] reported poor mental health as a general description for common mental disorders.
Summary of study design
Twelve papers were accepted for inclusion within the narrative synthesis, of which five studies were cross-sectional studies [ 28 , 34 , 37 , 38 , 39 ], five studies were cohort studies [ 31 , 32 , 33 , 35 , 36 ], one study was a longitudinal study [ 29 ], and one study was a secondary analysis [ 30 ].
Summary of type of data-analytic techniques and statistical methodology
Ten studies used statistical interactions [ 28 , 30 , 31 , 32 , 33 , 34 , 35 , 36 , 38 , 39 ], one study used mediation decomposition analysis [ 37 ], one study used multilevel modelling [ 29 ].
Summary of the social disadvantage and mental health effects in the studies
Socioeconomic status.
Principally, social inequality involves variables that interact with gender, potentially increasing the likelihood of a mental disorder – particularly among women. In this context, 11 out of the 12 studies examined the aspect of socioeconomic status [ 28 , 29 , 31 , 32 , 33 , 34 , 35 , 36 , 37 , 38 , 39 ]. Among these, seven studies demonstrated an interaction between lower socioeconomic status and the presence of a mental disorder, a relationship that becomes more pronounced when women originate from middle or lower-income backgrounds [ 29 , 31 , 33 , 35 , 36 , 37 , 38 ].
Gustafsson et al. [ 37 ] found that mid-income women reported poorer mental health than mid-income men and high-income women. Certain studies have also found statistical interactions with more specific mental disorders. Nicholson et al. [ 33 ] discovered a significant correlation between social inequality and depression in Eastern Europe, linked explicitly to economic circumstances. Their findings showed that women consistently conveyed higher levels of depression than men across all levels of the trajectory variable. This pattern held valid for every country within Eastern Europe. Furthermore, women who experience psychiatric distress and are socioeconomically disadvantaged were additionally more likely to experience chronic insomnia symptoms, with psychiatric distress more likely to recur or still be present 20 years later than that for higher socioeconomic groups. Applying quantitative methods to socioeconomic status, standard of living and neurotic disorders in the context of the United Kingdom, Lewis et al. [ 38 ] found a strong univariate relation between several socioeconomic variables and the prevalence of neurotic disorders in women, and this has also been reflected in usage of clinical facilities. For example, Cairney et al. [ 36 ] found that women were significantly more likely to have pursued any clinical service with respect to mental health (OR 1.4, p < 0.001), and the authors’ predictive CART analysis modelling indicated that low-income women aged 23–46 were most likely to use mental health services. Also, Najafi et al. [ 35 ] found that people with lower socioeconomic status were more likely to have poor mental health, as there was a slightly higher concentration of poor mental health among less-advantaged participants. In a Scottish cohort, Green et al. [ 32 ] identified an association between gender and psychiatric distress, with women in late middle age more likely to develop insomnia symptoms than men. Furthermore, Pabayo et al. [ 29 ] reported a significant cross-level interaction between depression and lower-income women.
Race/ethnicity
The addition of race / ethnicity as an interaction in the aetiology of mental disorders has been identified in the current review. Four studies demonstrated an interaction between race / ethnicity and mental disorder, especially when present in women with lower socioeconomic status [ 28 , 29 , 30 , 34 ]. With a Brazilian cohort, Moraes et al. [ 34 ] identified that common mental disorders are more prevalent in women at lower levels of income, at lower levels of education, and who are Black. In the context of ‘triple jeopardy’ as a minority, Mair [ 28 ] observed that Black women might face increased vulnerability due to increasing age, which intersects with being an older woman. This demographic intersection could potentially lead to compounded challenges. Furthermore, race/ethnicity has been identified as a significant determinant in mental health disparities. Rosenfield’s [ 30 ] study found that Black females in lower social classes experienced more significant mental health disadvantages than white males in higher social positions.
Educational level
Findings on the interaction between educational level and common mental disorders were similar to those on socioeconomic status. Five studies [ 28 , 33 , 34 , 38 , 39 ] reported a high association of no education / low education level with common mental disorders, as opposed to lower rates of common mental disorders in persons with high school and/or university / graduate education.
Age/marital status
Regarding age, only one study shows interaction: Najafi et al. [ 35 ] found that older adults more likely experience common mental health disorders as opposed to younger persons. Moreover, regarding marital status the systematic findings align with the observations of Najafi et al. [ 35 ], who recognised a correlation between poor mental health and marital status among Iranian adults. It is important to note that although the current study’s findings align with the authors results, not all the examined cases offer specific details.
Social class
The interaction between social class and common mental disorders was explored by Green and Benzeval [ 31 ], who found a non-linear decrease in the prevalence of anxiety with age and a non-linear increase in the prevalence of depression with age in people within the manual social class as opposed to those in the non-manual social class. Lewis et al. [ 38 ] found that people of lower social class status – particularly men – were associated with a higher prevalence of neurotic disorders. Lewis et al. [ 38 ] also found a strong correlation between social class and the prevalence of neurotic disorders in people aged 40–54 years.
Place of residence
Only one study has shown interaction between a place of residence and poor mental health. Najafi et al. [ 35 ] discovered that people living in Sistan and Balouchestan provinces in Iran had the largest prevalence of poor mental health. All 12 studies recognised gender/gender identity [ 28 , 29 , 30 , 31 , 32 , 33 , 34 , 35 , 36 , 37 , 38 , 39 ]. However, only eight studies showed strong interactions of gender as a variable with common mental disorders. All these studies found that women and girls were more at risk of experiencing and being diagnosed with common mental health disorders than men and boys,irrespective of other factors such as race/ethnicity, education or socioeconomic status, gender is an extremely predominant and strong factor.
Summary of statistical measurement
In this systematic review, nine of the 12 studies reported statistically significant findings (summarised in this section), offering valuable insights into social disadvantage and mental health intersections. Analysing the social determinants of mental health service using intersectionality theory and a CART analysis [ 36 ], the main effects model (logistic regression) revealed that being female was significantly associated with seeking any service for mental health (OR 1.4 p < 0.001). Gustafsson et al. [ 37 ] found that mid-income women experienced poorer mental health compared with both mid-income men (effect size: 0.42, 95% CI: 0.14–0.71, p < 0.001) and high-income women (effect size: 0.44, 95% CI: 0.13–0.74, p < 0.001). Also, Mair [ 28 ] showed the moderating effect of race and gender on the relationship between social ties and depressive symptoms, with the three-way interaction effects explaining 22.4% of the variation. Moraes et al. [ 34 ] identified a higher prevalence of common mental disorders among females, Blacks with lower education and income levels, and those who are divorced, separated, or widowed, with females having a CMD prevalence of 20.5% compared to 7.4% among males. Nicholson et al. [ 33 ] consistently found higher odds ratios for depressive symptoms in women than men across all trajectory variables in all Eastern European countries, with odds ratios for depressive symptoms being 2.03 (95% CI: 1.75–2.35) for women and 2.10 (95% CI: 1.82–2.43) for men in Russia, 2.31 (95% CI: 2.03–2.62) for women and 2.39 (95% CI: 2.12–2.71) for men in Poland, and 1.64 (95% CI: 1.40–1.94) for women and 1.79 (95% CI: 1.53–2.08) for men in the Czech Republic. Higher-income inequality was associated with an increased risk of depression among women in the fourth quintile (OR 1.37, 95% CI 1.03 to 1.82) and the fifth quintile (OR 1.50, 95% CI 1.14 to 1.96), and women in states with higher-income inequality had a higher risk of developing depression [ 29 ]. Lewis et al. [ 38 ] observed a significantly higher prevalence of neurotic disorder in women with no qualifications than those with higher educational attainment (odds ratio: 1.26, 95% CI: 1.06–1.49). Green and Benzeval [ 31 ] reported a higher prevalence rate of anxiety among females (34.8%), while depression among females was 12.0% in the West of Scotland. Lastly, Najafi et al. [ 35 ] revealed a higher prevalence of poor mental health in women (17.2%) compared with men (13%), indicating a gender difference in the prevalence of mental disorders – that is, to reiterate, a higher rate for women. The reporting of effect measures and statistical results provides a quantitative understanding of variable associations, while the complex interplay among social disadvantage factors and mental health outcomes increases the clarity and comprehensiveness of the systematic review’s findings.
This systematic review has sought to address a crucial gap in quantitative intersectionality by focusing on the methods for incorporating intersectionality into understandings of mental health disorders among women.
An overview finding on quantitative methods of intersectionality and its effects in women mental health studies
The findings from previous studies have observed consistent associations between mental disorders and social disadvantage in women. However, the results of this systematic review highlight that the cause of mental disorders in women is not simply the effect of an independent unitary social disadvantage. Instead, it emerges from complex multiplicative and simultaneous interactions, emphasising the indispensability of intersectionality approaches in comprehending and addressing the dynamic health issues relating to gender [ 17 ].
The term ‘intersectionality’ was initially introduced by Kimberle Crenshaw in 1989 [ 14 ], though the first quantitative intersectionality paper appeared 11 years later in 2001. Bauer et al. [ 40 ] stated that quantitative intersectionality analyses offer to explore the research data and the statistical effect on both micro and macro aspects of health issues, solving complicated multiplicative and compound effects within large datasets [ 40 ]. This quantitative approach to the theory enables policymakers to create strategies for addressing the root causes of health disparities. By illustrating the impact of social disadvantages on mental health disparities in women through statistical techniques involving numbers and percentages, this approach offers a more precise description of intersectionality’s impact.
The concept of intersectionality, implanted in feminist theory and discussed by scholars like Hancock [ 41 ], provides a crucial framework for understanding marginalised women [ 15 ]. While it is predominantly explored through qualitative research, this systematic review used a quantitative perspective on intersectionality to identify useful findings such as those from the quantitative analysis of Moraes et al. [ 34 ], which indicated the complex relationship between lower education and income levels and their impact mental health outcomes. Validating the power of quantitative methodologies offers much to feminist theory in terms of evidencing on the social factors that shape women’s mental health experiences.
This systematic review, as noted, identifies the quantitative methods and study designs used in intersectional research to understand women’s mental health and social disadvantage and assesses whether particular techniques were beneficial for understanding social disadvantage effects on mental health disorders among women. The findings from the study show that the most commonly used statistical methods were statistical interactions, mediation decomposition analysis, and multilevel model. Statistical interactions, a method in intersectional research, focus on how two or more categories interact to create combined effects, these interaction terms allow for examining the joint influences of variables and can be implemented as multiplicative or additive effects to explore how variables interact and shape the outcomes [ 16 ] For example, discrimination against Black women is more than just the sum of racism and sexism; in fact, its multiplicative effects imply the descriptions of discrimination when one factor’s impact depends on another factor’s existence [ 18 ]. Statistical interactions thus allow research to comprehend the multiplicative effects of multiple variables, such as gender, socioeconomic status, and race, on mental health outcomes [ 13 ]. Mediation decomposition analysis allows for the breakdown of the total effect of gender on mental health into direct and indirect effects through socioeconomic status. Because of this approach, the study explored how socioeconomic factors mediate or explain the gender inequality observed in mental health outcomes. Integrating mediation analysis adds depth to understanding how specific social categories contribute to the mental health landscape [ 37 ]. Multilevel modelling captures the complex interactions between social disadvantage factors at both individual and contextual levels, and this offers insights into the interpretations of mental health outcomes across different groups [ 29 ]. This is consistent with the findings of previous reviews that examined the use of quantitative methods to explore the intersectionality of multiple social disadvantages for various outcomes, both with and without a focus on gender [ 40 , 42 ].
The strategic use of quantitative techniques not only facilitated the extraction of data from the studies but also enabled a robust analysis of the multiplicative effects of social disadvantages on women’s mental health [ 40 ]. Employing quantitative methods to analyse intersectionality thus helps to present accurate statistical data, including prevalence and numerical figures, which are significant indications of effective research; statistical data works as compelling evidence that guides the policymaker in terms of practical solutions, such as implementing specific policies for improving women’s economic status, addressing gender inequalities, and promoting mental health outcomes for marginalised women. An ideal example from the systematic review comes from a study by Lewis et al. [ 38 ], which investigated complex socioeconomic indicators on neurotic disorders using statistical interactions. The authors observed a significantly higher prevalence of neurotic disorder in women with no qualifications than those with higher educational attainment (odds ratio: 1.26, 95% CI: 1.06–1.49). The same study also provided other valuable insights: this analysis revealed that 10% of neurotic disorders are linked to living standards. Such insights assist policymakers in designing targeted interventions that address specific socioeconomic inequality and enhance public health to improve mental health outcomes for women as well as men nationwide.
This systematic review facilitates understanding of if and how particular quantitative techniques help identify factors relating to social disadvantage effects on women’s mental health. In the analyses of 12 reviewed studies, nine have shown that the most significant variable contributing to social disadvantages affecting women’s mental health is socioeconomic status [ 28 , 29 , 33 , 34 , 35 , 36 , 37 , 38 , 39 ]. The analysis by Moraes et al. [ 34 ] found a prevalence of 20.5% of common mental disorders in women with lower education levels and occupations with lower socioeconomic status compared to 7.4% among men. Quantitative data on social inequality (e.g., income level, education, and occupation) is linked to a high prevalence of common mental disorders in women. Results help identify these inequalities’ causes and potential solutions [ 13 ]. This finding does not imply homogeneity in the employed methodologies, or the populations studied. The studies included in the systematic review showed heterogeneity in various aspects, such as sample sizes, study designs, measurement tools, and demographic characteristics. The differences in the studies influence how the findings are used in other contexts or populations. Solutions can also be extracted from quantitative results of intersectionality analyses, such as improving marginalised women’s educational opportunities and enhancing their skills as these two endeavours will elevate their financial income and give them independence, which will help improve their mental health.
A synthesis of the systematic review findings reveals a significant and consistent interaction between socioeconomic status, gender, and race/ethnicity that affects common mental disorders. Women from ethnic minorities with lower socioeconomic face compound challenges and experience increased rates of mental disorders. Therefore, incorporating a quantitative intersectional lens will help to investigate the accumulative impact of various social indignities to determine the root causes of mental health disorders among women. Such actions can help policies and programmes tackle gender inequality and effectively promote mental health and well-being among marginalised women.
Strengths and limitations
The studies included in the systematic search have various methodological strengths and weaknesses that might have influenced the outcomes reported. One of the strengths of the systematic review is the heterogeneity of methodologies and population of the included studies, which is important to consider when interpreting the findings. The review highlights consistent trends and associations between social disadvantage and mental health outcomes, and the diversity in sample sizes and study designs, such as cross-sectional, cohort and longitudinal studies, along with the use of various measurement tools to estimate common mental disorders and social disadvantage variables, and indeed the demographic characteristics, including age, race/ethnicity, and socioeconomic status, all offer much to this review (Table 1 ). Specifically, for example, certain variations show diversity in the factors that influence mental health and underline the complexity of intersectionality relations between social disadvantage and mental health outcomes.
Furthermore, the restricted number of studies found reflect the limited quantitative research conducted and the challenges posed through the integration of quantitative methods to look at research problems typically addressed by qualitative methods. However, the limited number of studies found could also be because studies that examined heterogeneity from the perspective of social disadvantage exclusively within the group of women were not included.
Nevertheless, the results of the findings do agree with pre-existing qualitative literature and enhance understanding of the area of women’s mental health. Value has been demonstrated in using a quantitative method application to understand intersectionality within this space and should be encouraged to continue with a focus on homogeneity in quantitative approaches to facilitate qualitative and quantitative synthesis ability within the area in future. Both approaches would provide a powerful data set in order to inform clinical approaches to prevention and treatment.
Our results indicate that self-reported data collection methodology is preferred with such study designs, being used within ten of the 12 studies [ 28 , 31 , 32 , 33 , 34 , 35 , 36 , 37 , 38 , 39 ]. Self-reported data is a common method for gathering information about individuals’ social identities. Self-reported data means that participants in these studies are asked to describe their social identities, such as gender, race, ethnicity, and socioeconomic status. Their interpretations of personal identity influence people’s self-reporting, which can present perceptions bias in reporting the data [ 43 ].
In conclusion, to the best of the researcher’s knowledge this systematic review is the first to collectively analyse the quantitative methods and study designs used in quantitative intersectional research on mental health disorders among mixed-gender populations to determine whether these techniques are practical and effective for quantitative intersectionality research. The 12 observational studies included in this review highlight the use of quantitative intersectionality methods to explore the complex relationships among various social disadvantages and effects on common mental disorders. By representing accurate statistical results, quantitative intersectional research can guide policymakers to improve women’s mental health.
In light of the findings from the systematic review, future research is recommended to explore the intersection of social inequalities’ effects on women’s mental health using the quantitative technique of intersectionality with large-scale data. The accurate statistical results can lead to a better understanding of women’s social identity from an intersectionality perspective and help to address social inequalities and thereby improve women’s mental health.
Availability of data and materials
Not applicable.
World Health Organization. Constitution of the World Health Organization. 1948. Available at: https://www.who.int/about/governance/constitution . Accessed: 4 Oct 2022.
Onarheim KH, Iversen JH, Bloom DE. Economic benefits of investing in women’s health: a systematic review. PLoS One. 2016. https://doi.org/10.1371/journal.pone.0150120 .
Kuhlmann E, Annandale E. The Palgrave handbook of gender and healthcare. London: Macmillan Publishers Limited; 2010.
Book Google Scholar
Braveman P, Gottlieb L. The social determinants of health: It’s time to consider the causes of the causes. Public Health Rep. 2014;129(2):19–31. https://doi.org/10.1177/00333549141291S206 .
Article PubMed PubMed Central Google Scholar
Hsieh N, Ruther M. Sexual minority health and health risk factors: Intersection effects of gender, race, and sexual identity. Am J Prev Med. 2016;50(6):746–55. https://doi.org/10.1016/J.AMEPRE.2015.11.016 .
Trinh MH, et al. Health and healthcare disparities among U.S. Women and men at the intersection of sexual orientation and race/ethnicity: a nationally representative cross-sectional study. BMC Public Health. 2017;17(1):1–11. https://doi.org/10.1186/S12889-017-4937-9/TABLES/4 .
Article Google Scholar
Williams DR. Miles to go before we sleep: racial inequities in health. J Health Soc Behav. 2012;53(3):279–95. https://doi.org/10.1177/0022146512455804 .
World Health Organization. Women and health: today’s evidence tomorrow’s agenda. 2009. Available at: https://apps.who.int/iris/handle/10665/44168 . Accessed: 4 Oct 2022.
Trygg NF, Gustafsson PE, Månsdotter A. Languishing in the crossroad? A scoping review of intersectional inequalities in mental health. Int J Equity Health. 2019;18(1):115. https://doi.org/10.1186/S12939-019-1012-4 .
Rehm J, Shield K D. Global burden of disease and the impact of mental and addictive disorders. 2019. https://doi.org/10.1007/s11920-019-0997-0
Lehtinen V, Sohlman B, Kovess-Masfety V. Level of positive mental health in the European Union: results from the eurobarometer 2002 survey. Clin Pract Epidemiol Ment Health. 2005;1:9. https://doi.org/10.1186/1745-0179-1-9 .
Lehavot K, et al. Race/ethnicity and sexual orientation disparities in mental health, sexism, and social support among women veterans. Psychol Sex Orientat Gend Divers. 2019;6(3):347–58. https://doi.org/10.1037/sgd0000333 .
Bauer GR. Incorporating intersectionality theory into population health research methodology: challenges and the potential to advance health equity. Soc Sci Med. 2014;110:10–7. https://doi.org/10.1016/J.SOCSCIMED.2014.03.022 .
Article PubMed Google Scholar
Crenshaw K. Demarginalizing the intersection of race and gender: a black feminist critique of antidiscrimination doctrine, feminist theory and antiracist politics. University of Chicago Legal Forum. 1989(1). http://chicagounbound.uchicago.edu/uclf . http://chicagounbound.uchicago.edu/uclf/vol1989/iss1/8 .
Collins PH. Intersectionality’s definitional dilemmas. Ann Rev Sociol. 2015;41:1–20.
McCall L. The complexity of intersectionality. Signs J Women Culture Soc. 2005;30(3):1771–800.
Bauer GR, Scheim AI. Methods for analytic inter-categorical intersectionality in quantitative research: discrimination as a mediator of health inequalities. Soc Sci Med. 2019;226(April 2018):236–45. https://doi.org/10.1016/j.socscimed.2018.12.015 .
Else-Quest NM, Hyde JS. Intersectionality in quantitative psychological research II. Methods techniques. Psychol Women Q. 2016;40(3):319–36. https://doi.org/10.1177/0361684316647953 .
Moher, D. et al. PRISMA 2009 Checklist. 2009. Available at: https://prismstatement.org//documents/PRISMA%202009%20checklist.pdf . Accessed: 21 Jul 2022.
Higgins JPT. et al. The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ. 2011;343(7829). https://doi.org/10.1136/BMJ.D5928 .
Song MM, et al. Development of a PubMed based search tool for identifying sex and gender specific health literature. J Womens Health. 2016;25(2):181–7. https://doi.org/10.1089/JWH.2015.5217 .
Liu Y. et al. Recruitment and retention strategies in mental health trials -A systematic review. PLoS One. 2018;13(8). https://doi.org/10.1371/JOURNAL.PONE.0203127 .
O’Neill J, Tabish H, Welch V, Petticrew M, Pottie K, Clarke M, Tugwell P. Applying an equity lens to interventions: using PROGRESS ensures consideration of socially stratifying factors to illuminate inequities in health. J Clin Epidemiol. 2014;67(1):56–64.
Mauvais-Jarvis F, Merz NB, Barnes PJ, Brinton RD, Carrero JJ, DeMeo DL, Suzuki A. Sex and gender: modifiers of health, disease, and medicine. Lancet. 2020;396(10250):565–82.
Springer KW, Stellman JM, Jordan-Young RM. Beyond a catalogue of differences: a theoretical frame and good practice guidelines for researching sex/gender in human health. Soc Sci Med. 2012;74(11):1817–24.
Sherif CW. Needed concepts in the study of gender identity. Psychol Women Q. 1982;6(4):375–98.
Kmet, L.M., Lee, R.C. and Cook, L.S. (2004) Standard quality assessment criteria for evaluating primary research papers from a variety of fields, lberta Heritage Foundation for Medical Research [Preprint]. Available at: http://www.ihe.ca/advanced-search/standard-quality-assessment-criteria-for-evaluating-primary-research-papers-from-a-variety-of-fields . Accessed: 4 Oct 2022.
Mair CA. Social ties and depression: an intersectional examination of black and white community-dwelling older adults. J Appl Gerontol. 2010;29(6):667–96. https://doi.org/10.1177/0733464809350167 .
Pabayo R, Kawachi I, Gilman SE. Income inequality among American states and the incidence of major depression. J Epidemiol Community Health. 2014;68(2):110–5. https://doi.org/10.1136/JECH-2013-203093 .
Rosenfield S. Triple jeopardy? Mental health at the intersection of gender, race, and class. Soc Sci Med. 2012;74(11):1791–801. https://doi.org/10.1016/J.SOCSCIMED.2011.11.010 .
Green MJ, Benzeval M. Ageing, social class and common mental disorders: longitudinal evidence from three cohorts in the West of Scotland. Psychol Med. 2011;41(3):565–74. https://doi.org/10.1017/S0033291710000851 .
Article CAS PubMed Google Scholar
Green MJ, Espie CA, Benzeval M. Social class and gender patterning of insomnia symptoms and psychiatric distress: A 20-year prospective cohort study’. BMC Psychiatry. 2014;14(1):152. https://doi.org/10.1186/1471-244X-14-152 .
Nicholson A, et al. Socio-economic status over the life-course and depressive symptoms in men and women in Eastern Europe. J Affect Disord. 2008;105(1–3):125–36. https://doi.org/10.1016/J.JAD.2007.04.026 .
de Moraes RSM, et al. Social inequalities in the prevalence of common mental disorders in adults: a population-based study in Southern Brazil. Rev Bras Epidemiol. 2017;20(1):43–56. https://doi.org/10.1590/1980-5497201700010004 .
Najafi F, et al. Decomposing socioeconomic inequality in poor mental health among Iranian adult population: results from the PERSIAN cohort study. BMC Psychiatry. 2020;20(1):1–11. https://doi.org/10.1186/S12888-020-02596-Y/TABLES/4 .
Cairney J, et al. Exploring the social determinants of mental health service use using intersectionality theory and CART analysis. J Epidemiol Community Health. 2014;68(2):145–50. https://doi.org/10.1136/JECH-2013-203120 .
Gustafsson PE, Sebastián MS, Mosquera PA. Meddling with middle modalities: a decomposition approach to mental health inequalities between intersectional gender and economic middle groups in northern Sweden. Glob Health Action. 2016;9(1). https://doi.org/10.3402/GHA.V9.32819 .
Lewis G, et al. Socioeconomic status, standard of living, and neurotic disorder. Lancet. 1998;352(9128):605–9. https://doi.org/10.1016/S0140-6736(98)04494-8 .
Kuklová M, et al. Educational inequalities in mental disorders in the Czech Republic: data from CZEch Mental health Study (CZEMS). Soc Psychiatry Psychiatr Epidemiol. 2021;56(5):867–77. https://doi.org/10.1007/S00127-020-01930-9 .
Bauer GR, Churchill SM, Mahendran M, Walwyn C, Lizotte D, Villa-Rueda AA. Intersectionality in quantitative research: a systematic review of its emergence and applications of theory and methods. SSM Popul Health. 2021;14:100798.
Hancock AM. When multiplication doesn’t equal quick addition: Examining intersectionality as a research paradigm. Perspect Polit. 2007;5(1):63–79. https://doi.org/10.1017/S1537592707070065 .
Mena E, Bolte G. Intersectionality-based quantitative health research and sex/gender sensitivity: a scoping review. Int J Equity Health. 2019;18(1):1–11.
Schellings G, Van Hout-Wolters B. Measuring strategy use with self-report instruments: theoretical and empirical considerations. Metacogn Learn. 2011;6:83–90.
Download references
Acknowledgements
The paper’s first author is a PhD student at the University of Glasgow. The Saudi Electronic University of Saudi Arabia is paying for her PhD studies.
Saudi Electronic University.
Kingdom of Saudi Arabia Higher Educational Minis.
Author information
Authors and affiliations.
Institute of Health and Wellbeing, University of Glasgow, Glasgow, UK
Nadia Alhamd Alghamdi, Kirsty Dunn, Deborah Cairns & Craig Melville
School of Health and Wellbeing, College of Medical Veterinary and Life Sciences, University of Glasgow, Glasgow, UK
You can also search for this author in PubMed Google Scholar
Contributions
Utilising quantitative methods to study the intersectionality of multiple social disadvantages in women with common mental disorders: a systematic review. All authors have reviewed and accepted the work also we all agreed to the submission to (the International Journal of Equity and Health). Thanks Nadia Alhamd [email protected].
Corresponding author
Correspondence to Craig Melville .
Ethics declarations
Ethics approval and consent to participate.
Not applicable, this systematic review ethical approval was not required.
Consent for publication
I consent to the publication of this systematic review study.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Additional file 1..
The following MEDLINE search strategy was used and was adapted as appropriate for other databases.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/ . The Creative Commons Public Domain Dedication waiver ( http://creativecommons.org/publicdomain/zero/1.0/ ) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
Reprints and permissions
About this article
Cite this article.
Alghamdi, N.A., Dunn, K., Cairns, D. et al. Utilising quantitative methods to study the intersectionality of multiple social disadvantages in women with common mental disorders: a systematic review. Int J Equity Health 22 , 264 (2023). https://doi.org/10.1186/s12939-023-02061-8
Download citation
Received : 29 November 2022
Accepted : 14 November 2023
Published : 18 December 2023
DOI : https://doi.org/10.1186/s12939-023-02061-8
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Mental health disorder
- Intersectionality
- Social disadvantage
International Journal for Equity in Health
ISSN: 1475-9276
- General enquiries: [email protected]
- Search Menu
Sign in through your institution
- Browse content in Arts and Humanities
- Browse content in Archaeology
- Anglo-Saxon and Medieval Archaeology
- Archaeological Methodology and Techniques
- Archaeology by Region
- Archaeology of Religion
- Archaeology of Trade and Exchange
- Biblical Archaeology
- Contemporary and Public Archaeology
- Environmental Archaeology
- Historical Archaeology
- History and Theory of Archaeology
- Industrial Archaeology
- Landscape Archaeology
- Mortuary Archaeology
- Prehistoric Archaeology
- Underwater Archaeology
- Urban Archaeology
- Zooarchaeology
- Browse content in Architecture
- Architectural Structure and Design
- History of Architecture
- Residential and Domestic Buildings
- Theory of Architecture
- Browse content in Art
- Art Subjects and Themes
- History of Art
- Industrial and Commercial Art
- Theory of Art
- Biographical Studies
- Byzantine Studies
- Browse content in Classical Studies
- Classical History
- Classical Philosophy
- Classical Mythology
- Classical Numismatics
- Classical Literature
- Classical Reception
- Classical Art and Architecture
- Classical Oratory and Rhetoric
- Greek and Roman Epigraphy
- Greek and Roman Law
- Greek and Roman Archaeology
- Greek and Roman Papyrology
- Late Antiquity
- Religion in the Ancient World
- Social History
- Digital Humanities
- Browse content in History
- Colonialism and Imperialism
- Diplomatic History
- Environmental History
- Genealogy, Heraldry, Names, and Honours
- Genocide and Ethnic Cleansing
- Historical Geography
- History by Period
- History of Agriculture
- History of Education
- History of Emotions
- History of Gender and Sexuality
- Industrial History
- Intellectual History
- International History
- Labour History
- Legal and Constitutional History
- Local and Family History
- Maritime History
- Military History
- National Liberation and Post-Colonialism
- Oral History
- Political History
- Public History
- Regional and National History
- Revolutions and Rebellions
- Slavery and Abolition of Slavery
- Social and Cultural History
- Theory, Methods, and Historiography
- Urban History
- World History
- Browse content in Language Teaching and Learning
- Language Learning (Specific Skills)
- Language Teaching Theory and Methods
- Browse content in Linguistics
- Applied Linguistics
- Cognitive Linguistics
- Computational Linguistics
- Forensic Linguistics
- Grammar, Syntax and Morphology
- Historical and Diachronic Linguistics
- History of English
- Language Acquisition
- Language Variation
- Language Families
- Language Evolution
- Language Reference
- Lexicography
- Linguistic Theories
- Linguistic Typology
- Linguistic Anthropology
- Phonetics and Phonology
- Psycholinguistics
- Sociolinguistics
- Translation and Interpretation
- Writing Systems
- Browse content in Literature
- Bibliography
- Children's Literature Studies
- Literary Studies (Asian)
- Literary Studies (European)
- Literary Studies (Eco-criticism)
- Literary Studies (Modernism)
- Literary Studies (Romanticism)
- Literary Studies (American)
- Literary Studies - World
- Literary Studies (1500 to 1800)
- Literary Studies (19th Century)
- Literary Studies (20th Century onwards)
- Literary Studies (African American Literature)
- Literary Studies (British and Irish)
- Literary Studies (Early and Medieval)
- Literary Studies (Fiction, Novelists, and Prose Writers)
- Literary Studies (Gender Studies)
- Literary Studies (Graphic Novels)
- Literary Studies (History of the Book)
- Literary Studies (Plays and Playwrights)
- Literary Studies (Poetry and Poets)
- Literary Studies (Postcolonial Literature)
- Literary Studies (Queer Studies)
- Literary Studies (Science Fiction)
- Literary Studies (Travel Literature)
- Literary Studies (War Literature)
- Literary Studies (Women's Writing)
- Literary Theory and Cultural Studies
- Mythology and Folklore
- Shakespeare Studies and Criticism
- Browse content in Media Studies
- Browse content in Music
- Applied Music
- Dance and Music
- Ethics in Music
- Ethnomusicology
- Gender and Sexuality in Music
- Medicine and Music
- Music Cultures
- Music and Religion
- Music and Culture
- Music and Media
- Music Education and Pedagogy
- Music Theory and Analysis
- Musical Scores, Lyrics, and Libretti
- Musical Structures, Styles, and Techniques
- Musicology and Music History
- Performance Practice and Studies
- Race and Ethnicity in Music
- Sound Studies
- Browse content in Performing Arts
- Browse content in Philosophy
- Aesthetics and Philosophy of Art
- Epistemology
- Feminist Philosophy
- History of Western Philosophy
- Meta-Philosophy
- Metaphysics
- Moral Philosophy
- Non-Western Philosophy
- Philosophy of Science
- Philosophy of Action
- Philosophy of Law
- Philosophy of Religion
- Philosophy of Language
- Philosophy of Mind
- Philosophy of Perception
- Philosophy of Mathematics and Logic
- Practical Ethics
- Social and Political Philosophy
- Browse content in Religion
- Biblical Studies
- Christianity
- East Asian Religions
- History of Religion
- Judaism and Jewish Studies
- Qumran Studies
- Religion and Education
- Religion and Health
- Religion and Politics
- Religion and Science
- Religion and Law
- Religion and Art, Literature, and Music
- Religious Studies
- Browse content in Society and Culture
- Cookery, Food, and Drink
- Cultural Studies
- Customs and Traditions
- Ethical Issues and Debates
- Hobbies, Games, Arts and Crafts
- Natural world, Country Life, and Pets
- Popular Beliefs and Controversial Knowledge
- Sports and Outdoor Recreation
- Technology and Society
- Travel and Holiday
- Visual Culture
- Browse content in Law
- Arbitration
- Browse content in Company and Commercial Law
- Commercial Law
- Company Law
- Browse content in Comparative Law
- Systems of Law
- Competition Law
- Browse content in Constitutional and Administrative Law
- Government Powers
- Judicial Review
- Local Government Law
- Military and Defence Law
- Parliamentary and Legislative Practice
- Construction Law
- Contract Law
- Browse content in Criminal Law
- Criminal Procedure
- Criminal Evidence Law
- Sentencing and Punishment
- Employment and Labour Law
- Environment and Energy Law
- Browse content in Financial Law
- Banking Law
- Insolvency Law
- History of Law
- Human Rights and Immigration
- Intellectual Property Law
- Browse content in International Law
- Private International Law and Conflict of Laws
- Public International Law
- IT and Communications Law
- Jurisprudence and Philosophy of Law
- Law and Politics
- Law and Society
- Browse content in Legal System and Practice
- Courts and Procedure
- Legal Skills and Practice
- Legal System - Costs and Funding
- Primary Sources of Law
- Regulation of Legal Profession
- Medical and Healthcare Law
- Browse content in Policing
- Criminal Investigation and Detection
- Police and Security Services
- Police Procedure and Law
- Police Regional Planning
- Browse content in Property Law
- Personal Property Law
- Restitution
- Study and Revision
- Terrorism and National Security Law
- Browse content in Trusts Law
- Wills and Probate or Succession
- Browse content in Medicine and Health
- Browse content in Allied Health Professions
- Arts Therapies
- Clinical Science
- Dietetics and Nutrition
- Occupational Therapy
- Operating Department Practice
- Physiotherapy
- Radiography
- Speech and Language Therapy
- Browse content in Anaesthetics
- General Anaesthesia
- Browse content in Clinical Medicine
- Acute Medicine
- Cardiovascular Medicine
- Clinical Genetics
- Clinical Pharmacology and Therapeutics
- Dermatology
- Endocrinology and Diabetes
- Gastroenterology
- Genito-urinary Medicine
- Geriatric Medicine
- Infectious Diseases
- Medical Oncology
- Medical Toxicology
- Pain Medicine
- Palliative Medicine
- Rehabilitation Medicine
- Respiratory Medicine and Pulmonology
- Rheumatology
- Sleep Medicine
- Sports and Exercise Medicine
- Clinical Neuroscience
- Community Medical Services
- Critical Care
- Emergency Medicine
- Forensic Medicine
- Haematology
- History of Medicine
- Browse content in Medical Dentistry
- Oral and Maxillofacial Surgery
- Paediatric Dentistry
- Restorative Dentistry and Orthodontics
- Surgical Dentistry
- Medical Ethics
- Browse content in Medical Skills
- Clinical Skills
- Communication Skills
- Nursing Skills
- Surgical Skills
- Medical Statistics and Methodology
- Browse content in Neurology
- Clinical Neurophysiology
- Neuropathology
- Nursing Studies
- Browse content in Obstetrics and Gynaecology
- Gynaecology
- Occupational Medicine
- Ophthalmology
- Otolaryngology (ENT)
- Browse content in Paediatrics
- Neonatology
- Browse content in Pathology
- Chemical Pathology
- Clinical Cytogenetics and Molecular Genetics
- Histopathology
- Medical Microbiology and Virology
- Patient Education and Information
- Browse content in Pharmacology
- Psychopharmacology
- Browse content in Popular Health
- Caring for Others
- Complementary and Alternative Medicine
- Self-help and Personal Development
- Browse content in Preclinical Medicine
- Cell Biology
- Molecular Biology and Genetics
- Reproduction, Growth and Development
- Primary Care
- Professional Development in Medicine
- Browse content in Psychiatry
- Addiction Medicine
- Child and Adolescent Psychiatry
- Forensic Psychiatry
- Learning Disabilities
- Old Age Psychiatry
- Psychotherapy
- Browse content in Public Health and Epidemiology
- Epidemiology
- Public Health
- Browse content in Radiology
- Clinical Radiology
- Interventional Radiology
- Nuclear Medicine
- Radiation Oncology
- Reproductive Medicine
- Browse content in Surgery
- Cardiothoracic Surgery
- Gastro-intestinal and Colorectal Surgery
- General Surgery
- Neurosurgery
- Paediatric Surgery
- Peri-operative Care
- Plastic and Reconstructive Surgery
- Surgical Oncology
- Transplant Surgery
- Trauma and Orthopaedic Surgery
- Vascular Surgery
- Browse content in Science and Mathematics
- Browse content in Biological Sciences
- Aquatic Biology
- Biochemistry
- Bioinformatics and Computational Biology
- Developmental Biology
- Ecology and Conservation
- Evolutionary Biology
- Genetics and Genomics
- Microbiology
- Molecular and Cell Biology
- Natural History
- Plant Sciences and Forestry
- Research Methods in Life Sciences
- Structural Biology
- Systems Biology
- Zoology and Animal Sciences
- Browse content in Chemistry
- Analytical Chemistry
- Computational Chemistry
- Crystallography
- Environmental Chemistry
- Industrial Chemistry
- Inorganic Chemistry
- Materials Chemistry
- Medicinal Chemistry
- Mineralogy and Gems
- Organic Chemistry
- Physical Chemistry
- Polymer Chemistry
- Study and Communication Skills in Chemistry
- Theoretical Chemistry
- Browse content in Computer Science
- Artificial Intelligence
- Computer Architecture and Logic Design
- Game Studies
- Human-Computer Interaction
- Mathematical Theory of Computation
- Programming Languages
- Software Engineering
- Systems Analysis and Design
- Virtual Reality
- Browse content in Computing
- Business Applications
- Computer Security
- Computer Games
- Computer Networking and Communications
- Digital Lifestyle
- Graphical and Digital Media Applications
- Operating Systems
- Browse content in Earth Sciences and Geography
- Atmospheric Sciences
- Environmental Geography
- Geology and the Lithosphere
- Maps and Map-making
- Meteorology and Climatology
- Oceanography and Hydrology
- Palaeontology
- Physical Geography and Topography
- Regional Geography
- Soil Science
- Urban Geography
- Browse content in Engineering and Technology
- Agriculture and Farming
- Biological Engineering
- Civil Engineering, Surveying, and Building
- Electronics and Communications Engineering
- Energy Technology
- Engineering (General)
- Environmental Science, Engineering, and Technology
- History of Engineering and Technology
- Mechanical Engineering and Materials
- Technology of Industrial Chemistry
- Transport Technology and Trades
- Browse content in Environmental Science
- Applied Ecology (Environmental Science)
- Conservation of the Environment (Environmental Science)
- Environmental Sustainability
- Environmentalist Thought and Ideology (Environmental Science)
- Management of Land and Natural Resources (Environmental Science)
- Natural Disasters (Environmental Science)
- Nuclear Issues (Environmental Science)
- Pollution and Threats to the Environment (Environmental Science)
- Social Impact of Environmental Issues (Environmental Science)
- History of Science and Technology
- Browse content in Materials Science
- Ceramics and Glasses
- Composite Materials
- Metals, Alloying, and Corrosion
- Nanotechnology
- Browse content in Mathematics
- Applied Mathematics
- Biomathematics and Statistics
- History of Mathematics
- Mathematical Education
- Mathematical Finance
- Mathematical Analysis
- Numerical and Computational Mathematics
- Probability and Statistics
- Pure Mathematics
- Browse content in Neuroscience
- Cognition and Behavioural Neuroscience
- Development of the Nervous System
- Disorders of the Nervous System
- History of Neuroscience
- Invertebrate Neurobiology
- Molecular and Cellular Systems
- Neuroendocrinology and Autonomic Nervous System
- Neuroscientific Techniques
- Sensory and Motor Systems
- Browse content in Physics
- Astronomy and Astrophysics
- Atomic, Molecular, and Optical Physics
- Biological and Medical Physics
- Classical Mechanics
- Computational Physics
- Condensed Matter Physics
- Electromagnetism, Optics, and Acoustics
- History of Physics
- Mathematical and Statistical Physics
- Measurement Science
- Nuclear Physics
- Particles and Fields
- Plasma Physics
- Quantum Physics
- Relativity and Gravitation
- Semiconductor and Mesoscopic Physics
- Browse content in Psychology
- Affective Sciences
- Clinical Psychology
- Cognitive Neuroscience
- Cognitive Psychology
- Criminal and Forensic Psychology
- Developmental Psychology
- Educational Psychology
- Evolutionary Psychology
- Health Psychology
- History and Systems in Psychology
- Music Psychology
- Neuropsychology
- Organizational Psychology
- Psychological Assessment and Testing
- Psychology of Human-Technology Interaction
- Psychology Professional Development and Training
- Research Methods in Psychology
- Social Psychology
- Browse content in Social Sciences
- Browse content in Anthropology
- Anthropology of Religion
- Human Evolution
- Medical Anthropology
- Physical Anthropology
- Regional Anthropology
- Social and Cultural Anthropology
- Theory and Practice of Anthropology
- Browse content in Business and Management
- Business Strategy
- Business History
- Business Ethics
- Business and Government
- Business and Technology
- Business and the Environment
- Comparative Management
- Corporate Governance
- Corporate Social Responsibility
- Entrepreneurship
- Health Management
- Human Resource Management
- Industrial and Employment Relations
- Industry Studies
- Information and Communication Technologies
- International Business
- Knowledge Management
- Management and Management Techniques
- Operations Management
- Organizational Theory and Behaviour
- Pensions and Pension Management
- Public and Nonprofit Management
- Social Issues in Business and Management
- Strategic Management
- Supply Chain Management
- Browse content in Criminology and Criminal Justice
- Criminal Justice
- Criminology
- Forms of Crime
- International and Comparative Criminology
- Youth Violence and Juvenile Justice
- Development Studies
- Browse content in Economics
- Agricultural, Environmental, and Natural Resource Economics
- Asian Economics
- Behavioural Finance
- Behavioural Economics and Neuroeconomics
- Econometrics and Mathematical Economics
- Economic Systems
- Economic Methodology
- Economic History
- Economic Development and Growth
- Financial Markets
- Financial Institutions and Services
- General Economics and Teaching
- Health, Education, and Welfare
- History of Economic Thought
- International Economics
- Labour and Demographic Economics
- Law and Economics
- Macroeconomics and Monetary Economics
- Microeconomics
- Public Economics
- Urban, Rural, and Regional Economics
- Welfare Economics
- Browse content in Education
- Adult Education and Continuous Learning
- Care and Counselling of Students
- Early Childhood and Elementary Education
- Educational Equipment and Technology
- Educational Strategies and Policy
- Higher and Further Education
- Organization and Management of Education
- Philosophy and Theory of Education
- Schools Studies
- Secondary Education
- Teaching of a Specific Subject
- Teaching of Specific Groups and Special Educational Needs
- Teaching Skills and Techniques
- Browse content in Environment
- Applied Ecology (Social Science)
- Climate Change
- Conservation of the Environment (Social Science)
- Environmentalist Thought and Ideology (Social Science)
- Management of Land and Natural Resources (Social Science)
- Natural Disasters (Environment)
- Pollution and Threats to the Environment (Social Science)
- Social Impact of Environmental Issues (Social Science)
- Sustainability
- Browse content in Human Geography
- Cultural Geography
- Economic Geography
- Political Geography
- Browse content in Interdisciplinary Studies
- Communication Studies
- Museums, Libraries, and Information Sciences
- Browse content in Politics
- African Politics
- Asian Politics
- Chinese Politics
- Comparative Politics
- Conflict Politics
- Elections and Electoral Studies
- Environmental Politics
- Ethnic Politics
- European Union
- Foreign Policy
- Gender and Politics
- Human Rights and Politics
- Indian Politics
- International Relations
- International Organization (Politics)
- Irish Politics
- Latin American Politics
- Middle Eastern Politics
- Political Methodology
- Political Communication
- Political Philosophy
- Political Sociology
- Political Theory
- Political Behaviour
- Political Economy
- Political Institutions
- Politics and Law
- Politics of Development
- Public Administration
- Public Policy
- Qualitative Political Methodology
- Quantitative Political Methodology
- Regional Political Studies
- Russian Politics
- Security Studies
- State and Local Government
- UK Politics
- US Politics
- Browse content in Regional and Area Studies
- African Studies
- Asian Studies
- East Asian Studies
- Japanese Studies
- Latin American Studies
- Middle Eastern Studies
- Native American Studies
- Scottish Studies
- Browse content in Research and Information
- Research Methods
- Browse content in Social Work
- Addictions and Substance Misuse
- Adoption and Fostering
- Care of the Elderly
- Child and Adolescent Social Work
- Couple and Family Social Work
- Direct Practice and Clinical Social Work
- Emergency Services
- Human Behaviour and the Social Environment
- International and Global Issues in Social Work
- Mental and Behavioural Health
- Social Justice and Human Rights
- Social Policy and Advocacy
- Social Work and Crime and Justice
- Social Work Macro Practice
- Social Work Practice Settings
- Social Work Research and Evidence-based Practice
- Welfare and Benefit Systems
- Browse content in Sociology
- Childhood Studies
- Community Development
- Comparative and Historical Sociology
- Disability Studies
- Economic Sociology
- Gender and Sexuality
- Gerontology and Ageing
- Health, Illness, and Medicine
- Marriage and the Family
- Migration Studies
- Occupations, Professions, and Work
- Organizations
- Population and Demography
- Race and Ethnicity
- Social Theory
- Social Movements and Social Change
- Social Research and Statistics
- Social Stratification, Inequality, and Mobility
- Sociology of Religion
- Sociology of Education
- Sport and Leisure
- Urban and Rural Studies
- Browse content in Warfare and Defence
- Defence Strategy, Planning, and Research
- Land Forces and Warfare
- Military Administration
- Military Life and Institutions
- Naval Forces and Warfare
- Other Warfare and Defence Issues
- Peace Studies and Conflict Resolution
- Weapons and Equipment

- < Previous chapter
- Next chapter >
5 An Introduction to Quantitative Methods Especially Relevant for Public Mental Health
- Published: July 2012
- Cite Icon Cite
- Permissions Icon Permissions
This chapter provides a brief introduction to some of the epidemiologic and statistical methods for and challenges to gathering and analyzing the data that underlie the research presented in this volume and in the field of public mental health as a whole. It focuses on some of the data and methodological complexities particularly common in public mental health research. It explores three fundamental types of questions relevant to public mental health: estimating rates of disorders in a population across people, place, and time; examining risk and protective factors associated with particular disorders; and exploring interventions to prevent disorders or to treat them once they emerge.
Personal account
- Sign in with email/username & password
- Get email alerts
- Save searches
- Purchase content
- Activate your purchase/trial code
- Add your ORCID iD
Institutional access
Sign in with a library card.
- Sign in with username/password
- Recommend to your librarian
- Institutional account management
- Get help with access
Access to content on Oxford Academic is often provided through institutional subscriptions and purchases. If you are a member of an institution with an active account, you may be able to access content in one of the following ways:
IP based access
Typically, access is provided across an institutional network to a range of IP addresses. This authentication occurs automatically, and it is not possible to sign out of an IP authenticated account.
Choose this option to get remote access when outside your institution. Shibboleth/Open Athens technology is used to provide single sign-on between your institution’s website and Oxford Academic.
- Click Sign in through your institution.
- Select your institution from the list provided, which will take you to your institution's website to sign in.
- When on the institution site, please use the credentials provided by your institution. Do not use an Oxford Academic personal account.
- Following successful sign in, you will be returned to Oxford Academic.
If your institution is not listed or you cannot sign in to your institution’s website, please contact your librarian or administrator.
Enter your library card number to sign in. If you cannot sign in, please contact your librarian.
Society Members
Society member access to a journal is achieved in one of the following ways:
Sign in through society site
Many societies offer single sign-on between the society website and Oxford Academic. If you see ‘Sign in through society site’ in the sign in pane within a journal:
- Click Sign in through society site.
- When on the society site, please use the credentials provided by that society. Do not use an Oxford Academic personal account.
If you do not have a society account or have forgotten your username or password, please contact your society.
Sign in using a personal account
Some societies use Oxford Academic personal accounts to provide access to their members. See below.
A personal account can be used to get email alerts, save searches, purchase content, and activate subscriptions.
Some societies use Oxford Academic personal accounts to provide access to their members.
Viewing your signed in accounts
Click the account icon in the top right to:
- View your signed in personal account and access account management features.
- View the institutional accounts that are providing access.
Signed in but can't access content
Oxford Academic is home to a wide variety of products. The institutional subscription may not cover the content that you are trying to access. If you believe you should have access to that content, please contact your librarian.
For librarians and administrators, your personal account also provides access to institutional account management. Here you will find options to view and activate subscriptions, manage institutional settings and access options, access usage statistics, and more.
Our books are available by subscription or purchase to libraries and institutions.
| Month: | Total Views: |
|---|---|
| October 2022 | 6 |
| November 2022 | 1 |
| December 2022 | 2 |
| January 2023 | 3 |
| February 2023 | 1 |
| March 2023 | 6 |
| April 2023 | 1 |
| May 2023 | 7 |
| June 2023 | 2 |
| August 2023 | 1 |
| September 2023 | 9 |
| October 2023 | 10 |
| November 2023 | 7 |
| December 2023 | 2 |
| January 2024 | 4 |
| February 2024 | 1 |
| March 2024 | 5 |
| May 2024 | 1 |
| June 2024 | 3 |
| July 2024 | 2 |
| August 2024 | 2 |
| September 2024 | 15 |
- About Oxford Academic
- Publish journals with us
- University press partners
- What we publish
- New features
- Open access
- Rights and permissions
- Accessibility
- Advertising
- Media enquiries
- Oxford University Press
- Oxford Languages
- University of Oxford
Oxford University Press is a department of the University of Oxford. It furthers the University's objective of excellence in research, scholarship, and education by publishing worldwide
- Copyright © 2024 Oxford University Press
- Cookie settings
- Cookie policy
- Privacy policy
- Legal notice
This Feature Is Available To Subscribers Only
Sign In or Create an Account
This PDF is available to Subscribers Only
For full access to this pdf, sign in to an existing account, or purchase an annual subscription.
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
- My Bibliography
- Collections
- Citation manager
Save citation to file
Email citation, add to collections.
- Create a new collection
- Add to an existing collection
Add to My Bibliography
Your saved search, create a file for external citation management software, your rss feed.
- Search in PubMed
- Search in NLM Catalog
- Add to Search
A quantitative assessment of the views of mental health professionals on exercise for people with mental illness: perspectives from a low-resource setting
Affiliations.
- 1 KU Leuven Department of Rehabilitation Sciences, Leuven, Belgium.
- 2 KU Leuven, University Psychiatric Center KU Leuven, Leuven-Kortenberg, Belgium.
- 3 Central Queensland University, School of Health. Medical and Applied Sciences, North Rockhampton, Australia.
- 4 KU Leuven, Centre for Contexual Psychiatry, Leuven, Belgium.
- 5 MRC/UVRI, Uganda Research Unit on AIDS, Entebbe, Uganda.
- 6 Department of Psychiatry, Makerere College of Health Sciences, Kampala, Uganda.
- 7 Senior Wellcome Trust Fellowship, London.
- 8 Butabika National Referral Mental Hospital, Kampala, Uganda.
- 9 Kyambogo University, Kampala, Uganda.
- PMID: 31656502
- PMCID: PMC6794511
- DOI: 10.4314/ahs.v19i2.42
Background: Exercise is nowadays considered as an evidence-based treatment modality in people with mental illness. Nurses and occupational therapists working in low-resourced mental health settings are well-placed to provide exercise advice for people with mental illness.
Objectives: We examined the current exercise prescription practices employed by Ugandan health care professionals when working with people with mental illness, and identified perceived barriers to exercise prescription and exercise participation for people with mental illness.
Methods: In this study, 31 Ugandan health care professionals 20 men; 31.2 ± 7.1 years completed the Exercise in Mental Illness Questionnaire- Health Professionals Version EMIQ-HP.
Results: The vast majority of the respondents 29/31, 94% reported they prescribed exercise at least "occasionally" to people with mental illness. Exercise-prescription parameters used were consistent with those recommended for people with mental illness. Regarding barriers to exercise participation, coping with side effects of psychotropic medication at the individual level and reducing stigma at community level should be prioritized.
Conclusion: A health care reform to enable collaboration with exercise professionals, such as exercise physiologists or physiotherapists, might increase exercise uptake for people with mental illness, thereby improving health outcomes for this vulnerable population.
Keywords: Exercise; physical activity.
© 2019 Vancampfort et al.
PubMed Disclaimer
Similar articles
- A 10-hours workshop improves physical activity prescription for mental illness knowledge and confidence in health care professionals: a nation-wide multicentre study from Uganda. Vancampfort D, Kimbowa S, Ward PB, Onekalit K, Lukwata H, Mugisha J. Vancampfort D, et al. Disabil Rehabil. 2023 Jan;45(1):170-175. doi: 10.1080/09638288.2021.2003448. Epub 2021 Nov 14. Disabil Rehabil. 2023. PMID: 34779314
- Barriers to exercise prescription and participation in people with mental illness: the perspectives of nurses working in mental health. Stanton R, Reaburn P, Happell B. Stanton R, et al. J Psychiatr Ment Health Nurs. 2015 Aug;22(6):440-8. doi: 10.1111/jpm.12205. Epub 2015 Apr 8. J Psychiatr Ment Health Nurs. 2015. PMID: 25855247
- Investigating the exercise-prescription practices of nurses working in inpatient mental health settings. Stanton R, Happell B, Reaburn P. Stanton R, et al. Int J Ment Health Nurs. 2015 Apr;24(2):112-20. doi: 10.1111/inm.12125. Epub 2015 Jan 30. Int J Ment Health Nurs. 2015. PMID: 25639383
- Exercise interventions and patient beliefs for people with hip, knee or hip and knee osteoarthritis: a mixed methods review. Hurley M, Dickson K, Hallett R, Grant R, Hauari H, Walsh N, Stansfield C, Oliver S. Hurley M, et al. Cochrane Database Syst Rev. 2018 Apr 17;4(4):CD010842. doi: 10.1002/14651858.CD010842.pub2. Cochrane Database Syst Rev. 2018. PMID: 29664187 Free PMC article. Review.
- Mental health service user and staff perspectives on tobacco addiction and smoking cessation: A meta-synthesis of published qualitative studies. Malone V, Harrison R, Daker-White G. Malone V, et al. J Psychiatr Ment Health Nurs. 2018 May;25(4):270-282. doi: 10.1111/jpm.12458. Epub 2018 Apr 14. J Psychiatr Ment Health Nurs. 2018. PMID: 29498459 Review.
- South African mental healthcare providers' views about exercise for people with mental illness. Marais BS. Marais BS. S Afr J Psychiatr. 2024 Apr 30;30:2227. doi: 10.4102/sajpsychiatry.v30i0.2227. eCollection 2024. S Afr J Psychiatr. 2024. PMID: 38726326 Free PMC article.
- Advising activity-knowledge, attitudes, beliefs, and behaviors regarding the recommendation of physical activity in clinical psychologists. Petzold MB, Betzler F, Plag J, Ströhle A, Bendau A. Petzold MB, et al. Eur Arch Psychiatry Clin Neurosci. 2024 Sep;274(6):1277-1287. doi: 10.1007/s00406-024-01819-7. Epub 2024 May 7. Eur Arch Psychiatry Clin Neurosci. 2024. PMID: 38714563 Free PMC article.
- Exercise Prescription Practices Among Mental Health Professionals on College Campuses: Testing the Information-Motivation-Behavioral Skills Model. Newsome AM, Kilpatrick M, Dedrick RF. Newsome AM, et al. Int J Behav Med. 2024 Feb 26. doi: 10.1007/s12529-024-10266-6. Online ahead of print. Int J Behav Med. 2024. PMID: 38409484
- Physical Activity and Prevalence of Depression and Antidepressants in the Spanish Population. Galán-Arroyo C, Pereira-Payo D, Rojo-Ramos J, Hernández-Mocholí MA, Merellano-Navarro E, Pérez-Gómez J, Denche-Zamorano Á, Adsuar JC. Galán-Arroyo C, et al. Healthcare (Basel). 2022 Feb 12;10(2):363. doi: 10.3390/healthcare10020363. Healthcare (Basel). 2022. PMID: 35206977 Free PMC article.
- Ecologies of care for serious mental illness in Uganda: A scoping review. Cohen F. Cohen F. Glob Soc Welf. 2021 Dec;8(4):301-315. doi: 10.1007/s40609-020-00193-1. Epub 2020 Oct 5. Glob Soc Welf. 2021. PMID: 34926127 Free PMC article. No abstract available.
- Whiteford HA, Degenhardt L, Rehm J, Baxter AJ, Ferrari AJ, Erskine HE, et al. Global burden of disease attributable to mental and substance use disorders: findings from the Global Burden of Disease Study 2010. The Lancet. 2013;3829904:1575–1586. doi: 10.1016/S0140-67361361611-6. - DOI - PubMed
- Bloom DE, Cafiero E, Jané-Llopis E, Abrahams-Gessel S, Bloom LR, Fathima S, et al. The global economic burden of noncommunicable diseases. Program on the Global Demography of Aging. 2012
- Vancampfort D, Stubbs B, Mitchell AJ, De Hert M, Wampers M, Ward PB, et al. Risk of metabolic syndrome and its components in people with schizophrenia and related psychotic disorders, bipolar disorder and major depressive disorder: a systematic review and meta-analysis. World Psychiatry. 2015;143:339–347. doi: 10.1002/wps.20252. - DOI - PMC - PubMed
- Vancampfort D, Correll CU, Galling B, Probst M, De Hert M, Ward PB, et al. Diabetes mellitus in people with schizophrenia, bipolar disorder and major depressive disorder: a systematic review and large scale meta-analysis. World Psychiatry. 2016;152:166–174. doi: 10.1002/wps.20309. - DOI - PMC - PubMed
- Stubbs B, Mitchell AJ, De Hert M, Correll CU, Soundy A, Stroobants M, et al. The prevalence and moderators of clinical pain in people with schizophrenia: A systematic review and large scale meta-analysis. Schizophrenia Research. 2014;1601:1–8. doi: 10.1016/j.schres.2014.10.017. - DOI - PubMed
- Search in MeSH
Related information
Grants and funding.
- 205069/Z/16/Z/WT_/Wellcome Trust/United Kingdom
LinkOut - more resources
Full text sources.
- Europe PubMed Central
- PubMed Central
- MedlinePlus Health Information
Research Materials
- NCI CPTC Antibody Characterization Program
Miscellaneous
- NCI CPTAC Assay Portal
- Citation Manager
NCBI Literature Resources
MeSH PMC Bookshelf Disclaimer
The PubMed wordmark and PubMed logo are registered trademarks of the U.S. Department of Health and Human Services (HHS). Unauthorized use of these marks is strictly prohibited.
Instant insights, infinite possibilities
55 research questions about mental health
Last updated
11 March 2024
Reviewed by
Brittany Ferri, PhD, OTR/L
Short on time? Get an AI generated summary of this article instead
Research in the mental health space helps fill knowledge gaps and create a fuller picture for patients, healthcare professionals, and policymakers. Over time, these efforts result in better quality care and more accessible treatment options for those who need them.
Use this list of mental health research questions to kickstart your next project or assignment and give yourself the best chance of producing successful and fulfilling research.
- Why does mental health research matter?
Mental health research is an essential area of study. It includes any research that focuses on topics related to people’s mental and emotional well-being.
As a complex health topic that, despite the prevalence of mental health conditions, still has an unending number of unanswered questions, the need for thorough research into causes, triggers, and treatment options is clear.
Research into this heavily stigmatized and often misunderstood topic is needed to find better ways to support people struggling with mental health conditions. Understanding what causes them is another crucial area of study, as it enables individuals, companies, and policymakers to make well-informed choices that can help prevent illnesses like anxiety and depression.
- How to choose a strong mental health research topic
As one of the most important parts of beginning a new research project, picking a topic that is intriguing, unique, and in demand is a great way to get the best results from your efforts.
Mental health is a blanket term with many niches and specific areas to explore. But, no matter which direction you choose, follow the tips below to ensure you pick the right topic.
Prioritize your interests and skills
While a big part of research is exploring a new and exciting topic, this exploration is best done within a topic or niche in which you are interested and experienced.
Research is tough, even at the best of times. To combat fatigue and increase your chances of pushing through to the finish line, we recommend choosing a topic that aligns with your personal interests, training, or skill set.
Consider emerging trends
Topical and current research questions are hot commodities because they offer solutions and insights into culturally and socially relevant problems.
Depending on the scope and level of freedom you have with your upcoming research project, choosing a topic that’s trending in your area of study is one way to get support and funding (if you need it).
Not every study can be based on a cutting-edge topic, but this can be a great way to explore a new space and create baseline research data for future studies.
Assess your resources and timeline
Before choosing a super ambitious and exciting research topic, consider your project restrictions.
You’ll need to think about things like your research timeline, access to resources and funding, and expected project scope when deciding how broad your research topic will be. In most cases, it’s better to start small and focus on a specific area of study.
Broad research projects are expensive and labor and resource-intensive. They can take years or even decades to complete. Before biting off more than you can chew, consider your scope and find a research question that fits within it.
Read up on the latest research
Finally, once you have narrowed in on a specific topic, you need to read up on the latest studies and published research. A thorough research assessment is a great way to gain some background context on your chosen topic and stops you from repeating a study design. Using the existing work as your guide, you can explore more specific and niche questions to provide highly beneficial answers and insights.
- Trending research questions for post-secondary students
As a post-secondary student, finding interesting research questions that fit within the scope of your classes or resources can be challenging. But, with a little bit of effort and pre-planning, you can find unique mental health research topics that will meet your class or project requirements.
Examples of research topics for post-secondary students include the following:
How does school-related stress impact a person’s mental health?
To what extent does burnout impact mental health in medical students?
How does chronic school stress impact a student’s physical health?
How does exam season affect the severity of mental health symptoms?
Is mental health counseling effective for students in an acute mental crisis?
- Research questions about anxiety and depression
Anxiety and depression are two of the most commonly spoken about mental health conditions. You might assume that research about these conditions has already been exhausted or that it’s no longer in demand. That’s not the case at all.
According to a 2022 survey by Centers for Disease Control and Prevention (CDC), 12.5% of American adults struggle with regular feelings of worry, nervousness, and anxiety, and 5% struggle with regular feelings of depression. These percentages amount to millions of lives affected, meaning new research into these conditions is essential.
If either of these topics interests you, here are a few trending research questions you could consider:
Does gender play a role in the early diagnosis of anxiety?
How does untreated anxiety impact quality of life?
What are the most common symptoms of anxiety in working professionals aged 20–29?
To what extent do treatment delays impact quality of life in patients with undiagnosed anxiety?
To what extent does stigma affect the quality of care received by people with anxiety?
Here are some examples of research questions about depression:
Does diet play a role in the severity of depression symptoms?
Can people have a genetic predisposition to developing depression?
How common is depression in work-from-home employees?
Does mood journaling help manage depression symptoms?
What role does exercise play in the management of depression symptoms?
- Research questions about personality disorders
Personality disorders are complex mental health conditions tied to a person’s behaviors, sense of self, and how they interact with the world around them. Without a diagnosis and treatment, people with personality disorders are more likely to develop negative coping strategies during periods of stress and adversity, which can impact their quality of life and relationships.
There’s no shortage of specific research questions in this category. Here are some examples of research questions about personality disorders that you could explore:
What environments are more likely to trigger the development of a personality disorder?
What barriers impact access to care for people with personality disorders?
To what extent does undiagnosed borderline personality disorder impact a person’s ability to build relationships?
How does group therapy impact symptom severity in people with schizotypal personality disorder?
What is the treatment compliance rate of people with paranoid personality disorder?
- Research questions about substance use disorders
“Substance use disorders” is a blanket term for treatable behaviors and patterns within a person’s brain that lead them to become dependent on illicit drugs, alcohol, or prescription medications. It’s one of the most stigmatized mental health categories.
The severity of a person’s symptoms and how they impact their ability to participate in their regular daily life can vary significantly from person to person. But, even in less severe cases, people with a substance use disorder display some level of loss of control due to their need to use the substance they are dependent on.
This is an ever-evolving topic where research is in hot demand. Here are some example research questions:
To what extent do meditation practices help with craving management?
How effective are detox centers in treating acute substance use disorder?
Are there genetic factors that increase a person’s chances of developing a substance use disorder?
How prevalent are substance use disorders in immigrant populations?
To what extent do prescription medications play a role in developing substance use disorders?
- Research questions about mental health treatments
Treatments for mental health, pharmaceutical therapies in particular, are a common topic for research and exploration in this space.
Besides the clinical trials required for a drug to receive FDA approval, studies into the efficacy, risks, and patient experiences are essential to better understand mental health therapies.
These types of studies can easily become large in scope, but it’s possible to conduct small cohort research on mental health therapies that can provide helpful insights into the actual experiences of the people receiving these treatments.
Here are some questions you might consider:
What are the long-term effects of electroconvulsive therapy (ECT) for patients with severe depression?
How common is insomnia as a side effect of oral mental health medications?
What are the most common causes of non-compliance for mental health treatments?
How long does it take for patients to report noticeable changes in symptom severity after starting injectable mental health medications?
What issues are most common when weaning a patient off of an anxiety medication?
- Controversial mental health research questions
If you’re interested in exploring more cutting-edge research topics, you might consider one that’s “controversial.”
Depending on your own personal values, you might not think many of these topics are controversial. In the context of the research environment, this depends on the perspectives of your project lead and the desires of your sponsors. These topics may not align with the preferred subject matter.
That being said, that doesn’t make them any less worth exploring. In many cases, it makes them more worthwhile, as they encourage people to ask questions and think critically.
Here are just a few examples of “controversial” mental health research questions:
To what extent do financial crises impact mental health in young adults?
How have climate concerns impacted anxiety levels in young adults?
To what extent do psychotropic drugs help patients struggling with anxiety and depression?
To what extent does political reform impact the mental health of LGBTQ+ people?
What mental health supports should be available for the families of people who opt for medically assisted dying?
- Research questions about socioeconomic factors & mental health
Socioeconomic factors—like where a person grew up, their annual income, the communities they are exposed to, and the amount, type, and quality of mental health resources they have access to—significantly impact overall health.
This is a complex and multifaceted issue. Choosing a research question that addresses these topics can help researchers, experts, and policymakers provide more equitable and accessible care over time.
Examples of questions that tackle socioeconomic factors and mental health include the following:
How does sliding scale pricing for therapy increase retention rates?
What is the average cost to access acute mental health crisis care in [a specific region]?
To what extent does a person’s environment impact their risk of developing a mental health condition?
How does mental health stigma impact early detection of mental health conditions?
To what extent does discrimination affect the mental health of LGBTQ+ people?
- Research questions about the benefits of therapy
Therapy, whether that’s in groups or one-to-one sessions, is one of the most commonly utilized resources for managing mental health conditions. It can help support long-term healing and the development of coping mechanisms.
Yet, despite its popularity, more research is needed to properly understand its benefits and limitations.
Here are some therapy-based questions you could consider to inspire your own research:
In what instances does group therapy benefit people more than solo sessions?
How effective is cognitive behavioral therapy for patients with severe anxiety?
After how many therapy sessions do people report feeling a better sense of self?
Does including meditation reminders during therapy improve patient outcomes?
To what extent has virtual therapy improved access to mental health resources in rural areas?
- Research questions about mental health trends in teens
Adolescents are a particularly interesting group for mental health research due to the prevalence of early-onset mental health symptoms in this age group.
As a time of self-discovery and change, puberty brings plenty of stress, anxiety, and hardships, all of which can contribute to worsening mental health symptoms.
If you’re looking to learn more about how to support this age group with mental health, here are some examples of questions you could explore:
Does parenting style impact anxiety rates in teens?
How early should teenagers receive mental health treatment?
To what extent does cyberbullying impact adolescent mental health?
What are the most common harmful coping mechanisms explored by teens?
How have smartphones affected teenagers’ self-worth and sense of self?
- Research questions about social media and mental health
Social media platforms like TikTok, Instagram, YouTube, Facebook, and X (formerly Twitter) have significantly impacted day-to-day communication. However, despite their numerous benefits and uses, they have also become a significant source of stress, anxiety, and self-worth issues for those who use them.
These platforms have been around for a while now, but research on their impact is still in its infancy. Are you interested in building knowledge about this ever-changing topic? Here are some examples of social media research questions you could consider:
To what extent does TikTok’s mental health content impact people’s perception of their health?
How much non-professional mental health content is created on social media platforms?
How has social media content increased the likelihood of a teen self-identifying themselves with ADHD or autism?
To what extent do social media photoshopped images impact body image and self-worth?
Has social media access increased feelings of anxiety and dread in young adults?
- Mental health research is incredibly important
As you have seen, there are so many unique mental health research questions worth exploring. Which options are piquing your interest?
Whether you are a university student considering your next paper topic or a professional looking to explore a new area of study, mental health is an exciting and ever-changing area of research to get involved with.
Your research will be valuable, no matter how big or small. As a niche area of healthcare still shrouded in stigma, any insights you gain into new ways to support, treat, or identify mental health triggers and trends are a net positive for millions of people worldwide.
Should you be using a customer insights hub?
Do you want to discover previous research faster?
Do you share your research findings with others?
Do you analyze research data?
Start for free today, add your research, and get to key insights faster
Editor’s picks
Last updated: 18 April 2023
Last updated: 27 February 2023
Last updated: 22 August 2024
Last updated: 5 February 2023
Last updated: 16 April 2023
Last updated: 9 March 2023
Last updated: 30 April 2024
Last updated: 12 December 2023
Last updated: 11 March 2024
Last updated: 4 July 2024
Last updated: 6 March 2024
Last updated: 5 March 2024
Last updated: 13 May 2024
Latest articles
Related topics, .css-je19u9{-webkit-align-items:flex-end;-webkit-box-align:flex-end;-ms-flex-align:flex-end;align-items:flex-end;display:-webkit-box;display:-webkit-flex;display:-ms-flexbox;display:flex;-webkit-flex-direction:row;-ms-flex-direction:row;flex-direction:row;-webkit-box-flex-wrap:wrap;-webkit-flex-wrap:wrap;-ms-flex-wrap:wrap;flex-wrap:wrap;-webkit-box-pack:center;-ms-flex-pack:center;-webkit-justify-content:center;justify-content:center;row-gap:0;text-align:center;max-width:671px;}@media (max-width: 1079px){.css-je19u9{max-width:400px;}.css-je19u9>span{white-space:pre;}}@media (max-width: 799px){.css-je19u9{max-width:400px;}.css-je19u9>span{white-space:pre;}} decide what to .css-1kiodld{max-height:56px;display:-webkit-box;display:-webkit-flex;display:-ms-flexbox;display:flex;-webkit-align-items:center;-webkit-box-align:center;-ms-flex-align:center;align-items:center;}@media (max-width: 1079px){.css-1kiodld{display:none;}} build next, decide what to build next, log in or sign up.
Get started for free

Mental health in ultra-endurance runners: A systematic review
Among ultra-endurance runners (UER), the mental, behavioral, and physical demands of training/competition can result in maladaptive outcomes. Mental health issues are common in athletes and can impact psychology, physical health, and performance.
To synthesize information regarding the incidence/prevalence and factors associated with mental health issues among UER.
Systematic searches were performed in PubMed, SPORTDiscus, Scopus, Cochrane databases, CINAHL, Web of Science, and Medline Ovid using key terms related to UER (e.g., trail running, road running) and psychological issues (e.g., exercise addiction, depression). Inclusion criteria included original articles published in peer-reviewed journals in English, using qualitative or quantitative approaches. We considered papers reporting incidence/prevalence and associated factors with mental health outcomes in UER of both sexes, all ages, and levels of competition (e.g., elite, nonprofessional runners). The Joanna Briggs Institute Analytical Cross-Sectional Studies critical appraisal tool was used for quality assessment.
A total of 282 studies were identified, and 11 studies were included in the final selection. A total of 3670 UER were included in the studies. The prevalence of mental health issues among UER ranged between 32.0% and 62.5% for eating disorders, from 11.5% to 18.2% for exercise addiction, 18.6% for depressive symptoms, and 24.5% for sleep disturbance. Exercise addiction was not related to weekly volume, but a strong relationship with exercise in an unstructured space, age, and body mass index was shown.
Mental health issues among UER are common, especially eating disorders, exercise addiction, sleep disturbances, and depressive symptoms. Further high-quality studies are needed to examine underlying factors and find preventative strategies to protect UER.
Publication
External identifier.
- https://doi.org/10.1007/s40279-023-01890-5
Department or School
- Physical Education and Sports Science
Usage metrics

- Sports science and exercise
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
The PMC website is updating on October 15, 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- Elsevier - PMC COVID-19 Collection

Comparing efficacy of telehealth to in-person mental health care in intensive-treatment-seeking adults
The heightened acuity in anxiety and depressive symptoms catalyzed by the COVID-19 pandemic presents an urgent need for effective, feasible alternatives to in-person mental health treatment. While tele-mental healthcare has been investigated for practicability and accessibility, its efficacy as a successful mode for delivering high-quality, high-intensity treatment remains unclear. This study compares the clinical outcomes of a matched sample of patients in a private, nation-wide behavioral health treatment system who received in-person, intensive psychological treatment prior to the COVID-19 pandemic (N = 1,192) to the outcomes of a distinctive group of patients who received telehealth treatment during the pandemic (N = 1,192). Outcomes are measured with respect to depressive symptoms (Quick Inventory of Depressive Symptomatology-Self-Report; QIDS-SR) and quality of life (Quality of Life Enjoyment and Satisfaction Questionnaire; Q-LES-Q). There were no significant differences in admission score on either assessment comparing in-person and telehealth groups. Patients in the partial hospitalization level of care stayed longer when treatment was remote. Results suggest telehealth as a viable care alternative with no significant differences between in-person and telehealth groups in depressive symptom reduction, and significant increases in self-reported quality of life across both groups. Future research is needed to replicate these findings in other healthcare organizations in other geographical locations and diverse patient populations.
1. Introduction
In response to the coronavirus disease 2019 (COVID-19) pandemic, healthcare organizations around the world adapted to remote behavioral health treatment to meet an increased need for high-quality mental health care. With lockdowns and stay-at-home orders, the pandemic presented an acute need for mental health treatment to be virtually accessible—regardless of patient or provider setting—as well as near-equivalent in quality to what a person would have received had they attended in person. This paper examines the current landscape of remote mental health care as a viable treatment delivery method and uses clinical outcomes data from patients undergoing in-person and telehealth mental health treatment at a large, multistate behavioral health system to illustrate telehealth's comparability to traditional, in-person care.
The US Centers for Disease Control and Prevention (CDC) reported that symptoms of anxiety and depressive disorders among adults “increased considerably” when comparing reports from April through June of 2019 to the same time period in 2020 ( Czeisler et al., 2020 ). In the survey with 5,412 adult respondents, the CDC measured anxiety and depressive symptoms related to the pandemic using the four-item patient health questionnaire (PHQ-4) and COVID-19 trauma-related symptoms using the six-item Impact of Event Scale. Overall, 40.9% of survey respondents reported at least one adverse mental health condition, including symptoms of anxiety disorder or depressive disorder (30.9%), and 26.3% reported symptoms of a trauma- and stressor-related disorder because of the pandemic. Suicidal ideation in the last 30 days was reported by 10.7% of respondents. In 2021, the CDC published results of the Household Pulse Survey, a self-report online survey, which showed that the percentage of adults who reported experiencing symptoms related to depression and anxiety disorders increased from 36.4% to 41.5% between August 2020 and February 2021 ( Vahratian et al., 2021 ). Additionally, respondents who reported unmet mental health needs increased from 9.2% to 11.7% in the same time period. Historically there is evidence that mental health needs increase during a pandemic ( Soklaridis et al., 2020 ). Past outbreaks, such as severe acute respiratory syndrome (SARS) in 2003, directly resulted in heightened anxiety related to the virus ( Cheng and Cheung 2005 ; Chong et al., 2004 ), as well as increased stigmatization and discrimination of minority groups (Ren et al., 2020). Feelings of uncertainty, isolation, and confusion over rapidly changing health guidelines have exacerbated feelings of anxiety and mental distress ( Rajkumar, 2020 ). What sets the COVID-19 pandemic apart is the already widespread use of telecommunication platforms for remote work, learning, and basic healthcare. Although prior studies have investigated the impact of telehealth compared to traditional in-person treatment, there has been limited research into these differences in treatment settings beyond the outpatient level ( Hilty et al., 2013 ). This is a novel offering of the current analysis.
Mental healthcare providers have been exploring remote treatment options for over six decades ( Hilty et al., 2013 ). In this domain, providers use videoconferencing for therapy, evaluations, and medication management. In some cases, clinicians use telehealth to supplement in-person treatment. Previous research has shown that telehealth reduces patient-incurred costs and time associated with travel ( Rabinowitz et al., 2010 ) and improves accessibility of mental healthcare for those living in rural areas ( Manfredi et al., 2005 ; Morland et al., 2010 ; Weiner et al., 2011 ). Some even argue that remote treatment is superior to in-person consultations for some patients ( Pakyurek et al., 2010 ; Storch et al., 2011 ). In the context of public health, others have highlighted telehealth as a way for patients to maintain human connection during social distancing and lockdowns ( Whaibeh et al., 2020 ). Findings are mixed with respect to patient satisfaction of psychiatric telehealth services ( Frueh et al., 2005 ; Jacob et al., 2012 ; Nelson et al., 2003 ; Ruskin et al., 2004 ; Zimmerman et al., 2021a ), yet remote care has been shown to improve access to mental health treatment in some cases, especially for individuals experiencing linguistic or financial obstacles ( Chong and Moreno, 2012 ; Moreno et al., 2012 ; Mucic 2010 ; Ye et al., 2012 ). For example, Mucic (2010) highlights that the availability of bilingual clinicians through remote care can help overcome travel requirements for both patients and providers, as well as lead to higher patient satisfaction. In the case of the pandemic, telehealth treatment may also help minority groups navigate greater exposure risk to COVID-19 by allowing them to remain remote and socially distanced distanced during care ( Price-Haywood et al., 2020 ). Prior to the pandemic, telehealth was largely reported as comparable to in-person treatment in terms of its feasibility in obtaining favorable treatment outcomes in a variety of symptom profiles (De Las Cuevas et al., 2006 ; Lopez et al., 2004 ; Nelson et al., 2003 ; Richardson et al., 2009 ; Rojas et al., 2020 ; Ruskin et al., 2004 ; Shore et al., 2008 ; Urness et al., 2006 ; Yellowlees et al., 2010 ). Zimmerman and colleagues describe how patients in a partial hospitalization program reported significant reduction in symptoms whether they received in-person or telehealth treatment ( Zimmerman et al., 2021b ). However, to date, there are few other complete comparisons of patient outcomes prior to and following the pandemic, specifically as they relate to the efficacy of remote versus in-person treatment (although see Hom et al., 2020 for preliminary data). Further, the efficacy of telehealth as a treatment alternative has not previously been examined in a comparison of partial hospitalization and intensive outpatient programming, namely how level of care and acuity might affect outcomes.
The present study analyzes the clinical outcomes of patients who underwent mental health treatment in this telehealth format during the COVID-19 pandemic and compares their outcomes to patients from the same healthcare system who completed in-person care prior to the pandemic. The research questions were twofold: (1) How did treatment delivery (in-person vs. telehealth) affect patient outcomes across Rogers as a nation-wide provider; and (2) does treatment delivery modulate therapeutic response for patients in different levels of care (PHP or IOP)? Considering some service lines utilize therapies traditionally conducted in-person—for example, exposure therapies or behavioral activation exercises—it was hypothesized that any between-group differences may be due to the difficulty associated with implementing these methods virtually in such a short timeframe. If this is the case, patients who received in-person treatment are expected to show greater symptom reduction than patients who received telehealth treatment. However, consistent with the Zimmerman et al. (2021b) study, if the therapies employed translate as planned to the virtual format, we do not expect significant differences in scores at discharge comparing in-person and telehealth groups.
2.1. Participants and procedure
The Rogers Behavioral Health (Rogers) Institutional Review Board is committed to the ethical principles for the protection of human subjects in research which guide the IRB's deliberations and decision-making, including respect for persons, beneficence, and justice. This study was approved with exempt determination by the Rogers Institutional Review Board (IRB). Because this study contained retrospective data analysis only and no prospective data collection, there was no consent process. Only de-identified data was used for analyses. All adult patients between 18 and 65 were eligible for inclusion. If patients were missing either an admission or discharge score for either of the two measures, they were excluded from analyses.
In March of 2020, following the onset of the COVID-19 pandemic, Rogers converted partial hospitalization (PHP) and intensive outpatient (IOP) treatment programs to telehealth. Prior to the pandemic, telehealth services were occasionally provided on an as-needed basis. The organization-wide transition to telehealth leveraged existing technological solutions for videoconferencing and scheduling sessions. If patients did not have a device to access their therapy sessions, laptops were provided. To ensure high-quality treatment, fidelity checks of treatment delivery were conducted by clinical supervisors and directors of clinical services. As pre-existing in-person treatment was protocolized and manualized, an existing audit process was leveraged to ensure compliance with treatment groups and to identify gaps in telehealth treatment delivery as compared to in-person care. Specific aspects of treatment varied by services line (e.g., OCD PHP versus Depression Recovery PHP), however there was overlap in main treatment functions. Specifically, individual meeting invites were sent to each patient for every treatment element daily. Individual sessions included those with their assigned therapist and with their psychiatrists. Group sessions may have included cognitive behavioral therapy skills or possibly dialectal behavior therapy skills depending on the program the patient was enrolled in. Couples or family sessions were also delivered via telehealth. All treatment manuals and materials were sent electronically for patients to use during telehealth programming. Completed forms were emailed back to treatment team members to review in future sessions. Patients completed self-reported outcome measures in a protocolized fashion, at home, and all scores received from these assessments were integrated into the patient's treatment. Close attention was paid to patient attendance for each treatment element and local police phone numbers and emergency contact information was collected and made accessible for all treatment team members in case someone did not appear for treatment in a timely manner. In addition to emergency contact information, safety protocols were developed to ensure response to safety concerns was timely and consistent.
The research study included in this submission aligns with the IRB-approved protocol. Participants include 2,384 adult patients who completed either PHP or IOP programs at Rogers, 1,192 patients in each of the in-person and telehealth groups. Patients in the telehealth group received treatment between July 2020 and March 2021. The group of patients who received telehealth was matched to an equally sized subsample of 1,192 patients who received in-person care between May 2013 and December 2019. Groups were matched using optimal pairwise matching computed with the MatchIt package in R ( Ho et al., 2011 ), where covariates unrelated to treatment were balanced between in-person and telehealth groups. Covariates that were balanced in this way include age, sex, race, diagnosis, and level of care, ensuring that comparable demographic groups could be compared in addition to having an equal proportion of PHP and IOP patients included in each of the groups. Patients whose sex and/or race were unknown were excluded from the matching process and were not included in the analyzed dataset ( Table 1 ). There were no significant differences with respect to diagnosis across the dataset either comparing in-person to telehealth groups or with level of care ( Table 2 ).
Comparison of age, sex assigned at birth, and race of in-person and telehealth groups.
| Partial Hospitalization (PHP) | ||||
|---|---|---|---|---|
| In-Person = 950 | Telehealth = 950 | Comparison | ||
| Mean ± SD | Mean ± SD | |||
| Age | 31.53 ± 11.81 | 31.69 ± 11.84 | (3798) = −0.41 | = .68 |
| % (n) | % (n) | |||
| Sex | (df = 1, 0.02) | = .88 | ||
| Female | 66.0% (627) | 66.4% (631) | ||
| Male | 34.0% (323) | 33.6% (319) | ||
| Race | (df = 4, 0.08) | = 1 | ||
| Asian | 1.6% (15) | 1.7% (16) | ||
| Black or African American | 2.9% (28) | 2.8% (27) | ||
| Native Hawaiian or Pacific Islander | 0.4% (4) | 0.4% (4) | ||
| White | 93.5% (888) | 93.4% (887) | ||
| Multiple | 1.6% (15) | 1.7% (16) | ||
| Intensive Outpatient (IOP) | ||||
| In-Person = 242 | Telehealth = 242 | Comparison | ||
| Mean ± SD | Mean ± SD | |||
| Age | 34.31 ± 13.29 | 33.88 ± 13.19 | (966) = 0.50 | = .62 |
| % (n) | % (n) | |||
| Sex | (df = 1, 0.32) | = .57 | ||
| Female | 61.6% (149) | 64.5% (156) | ||
| Male | 38.4% (93) | 35.5% (86) | ||
| Race | (df = 4, 1.95) | = .58 | ||
| Asian | 3.7% (9) | 4.5% (11) | ||
| Black or African American | 7.4% (18) | 4.5% (11) | ||
| Native Hawaiian or Pacific Islander | 0.0% (0) | 0.0% (0) | ||
| White | 86.4% (209) | 88.4% (214) | ||
| Multiple | 2.5% (6) | 2.5% (6) | ||
Note. Age is denoted as mean ± standard deviation. Demographic percentages are denoted with counts in parentheses. T-tests were used to test for significant differences when age was the dependent variable. Chi-square tests were used to detect differences in sex and race.
Comparison of diagnosis category across in-person and telehealth groups.
| Partial Hospitalization (PHP) | ||||
|---|---|---|---|---|
| In-Person = 950 | Telehealth = 950 | Comparison | ||
| % (n) | % (n) | |||
| Anxiety | 50.7% (482) | 55.3% (525) | (df = 1, 3.73) | .06 |
| Feeding/eating | 8.9% (85) | 7.9% (75) | (df = 1, 0.55) | .46 |
| Mood | 77.9% (740) | 74.8% (711) | (df = 1, 2.29) | .13 |
| Neurodevelopmental | 11.2% (106) | 12.4% (118) | (df = 1, 0.61) | .43 |
| OCD | 23.9% (227) | 25.2% (239) | (df = 1, 0.34) | .56 |
| Social | 9.5% (90) | 8.7% (83) | (df = 1, 0.23) | .63 |
| Substance abuse/addictions | 20.3% (193) | 22.9% (218) | (df = 1, 1.79) | .18 |
| Trauma | 20.3% (193) | 23.9% (227) | (df = 1, 3.33) | .07 |
| Intensive Outpatient (IOP) | ||||
| In-Person = 242 | Telehealth = 242 | Comparison | ||
| % (n) | % (n) | |||
| Anxiety | 59.5% (144) | 55.4% (134) | (df = 1, 0.68) | .41 |
| Feeding/eating | 2.5% (6) | 5.0% (12) | (df = 1, 1.44) | .23 |
| Mood | 68.6% (166) | 60.7% (147) | (df = 1, 2.93) | .09 |
| Neurodevelopmental | 10.3% (25) | 11.6% (28) | (df = 1, 0.08) | .77 |
| OCD | 22.7% (55) | 18.6% (45) | (df = 1, 1.02) | .31 |
| Social | 9.9% (24) | 8.3% (20) | (df = 1, 0.23) | .64 |
| Substance abuse/addictions | 28.5% (69) | 21.5% (52) | (df = 1, 2.82) | .09 |
| Trauma | 14.0% (34) | 12.8% (31) | (df = 1, 0.07) | .79 |
Note. Data are shown as proportions with counts in parentheses. Chi-square test results and p-values are reported.
Regardless of treatment delivery mode, prior to admitting to treatment, patients' psychological symptoms are assessed over the phone. Licensed psychiatrists and psychologists with expertise in the patient's behavioral health area of concern review the phone screen interviews to determine treatment program appropriateness and to recommend level of care. PHP and IOP are multidisciplinary programs that involve individual, group, and family therapies along with medication management. Patients in PHP attend treatment 6 h per day, five days a week, and patients in IOP complete 3 h of treatment five days a week. After they are admitted, patients work with a psychologist to complete a diagnostic assessment where diagnoses are confirmed using the Diagnostic and Statistical Manual-5th Edition (DSM-5; American Psychological Association, 2013 ). Patient-reported outcome measures (PROMs) are collected from each patient at the beginning of treatment, either weekly or biweekly during treatment, and at the end of treatment. Patients received the same treatment content and frequency of treatment sessions regardless of when they completed treatment. In-person and telehealth providers participated in the same internal training program, ensuring a high level of similarity in treatment received by in-person and telehealth patient groups. Due to staff turnover, some providers were consistent across in-person and telehealth timeframes, whereas others were unique to one timeframe.
Two PROMs were used to index treatment efficacy: the Quick Inventory of Depressive Symptomology-Self Report (QIDS-SR; Rush et al., 2003 ) and the Quality of Life Enjoyment and Satisfaction Questionnaire - Short Form (Q-LES-Q; Schechter et al., 2007 ). Both assessments are administered upon admission, discharge, and either weekly or biweekly across all adult programs, service lines, and levels of treatment at Rogers. The Quick Inventory of Depressive Symptomatology Self-Report (QIDS-SR; Rush et al., 2003 ) is a 16-item self-report measure that asks respondents to indicate on a scale of 0–3 (0 = low, 3 = high) how well each item describes them for the past week. The QIDS-SR assesses nine domains of depression symptomatology: sleep, mood, weight, concentration, guilt, suicidal ideation, interest, fatigue, and psychomotor changes. Responses are summed to provide a single outcome metric, which can range from 0 to 27, where a higher score indicates a more severe level of depression symptomatology. The Quality-of-Life Enjoyment and Satisfaction Questionnaire (Q-LES-Q; Schechter et al., 2007 ) is a 16-item self-report measure that asks respondents to indicate on a scale of 1–5 (“very poor” = 1, “very good” = 5) how satisfied they have been in the past week with aspects of their general health, well-being, and feelings about their life. Total scores are reported as percentages ranging from 0 to 100%, with higher percentages indicating greater enjoyment and satisfaction.
Statistical analyses were performed using R ( R Core Team, 2021 ). To measure differences between in-person and telehealth groups, we conducted 2 × 2 between-subjects analyses of variance (ANOVAs) with treatment modality (in-person, telehealth) and level of care (PHP, IOP) as independent variables. One ANOVA was conducted for each of total QIDS-SR score at admission, score at discharge, and percent change over time between admission and discharge. The same three tests were conducted for Q-LES-Q scores. Planned pairwise comparisons within each significant factor were conducted using t-tests (e.g. PHP compared to IOP). For all analyses, a two-tailed level of significance of 5% was adopted.
There were no significant differences in admission score on either the QIDS-SR ( F (2380) = 1.06, p = .30) or the Q-LES-Q ( t (2380) = 0.26, p = .61) between in-person and telehealth groups ( Table 3 ). For QIDS-SR scores, there was a significant main effect of level of care only at both admission ( F (1, 2380) = 88.00, p < .001) and at discharge ( F (1, 2380) = 48.07, p < .001). Planned pairwise comparisons showed that PHP scores at both time points, on average, were higher than IOP scores, which is clinically expected. The main effect of treatment delivery was trending but not significant at discharge only ( F (1, 2380) = 3.60, p = .06) such that patients who received telehealth treatment had a higher average QIDS discharge score compared to in-person. The interaction between treatment delivery and level of care was not significant.
Comparison of clinical assessment outcomes at admission and discharge for in-person and telehealth groups. Data are shown as mean ± standard deviation with analysis of variance results for the group factor.
| Clinical Assessment | Total Score | In-Person | Telehealth | Cohen's D | (1, 2380) | Post-hoc comparisons | ||
|---|---|---|---|---|---|---|---|---|
| QIDS | ||||||||
| ADMISSION | ||||||||
| Treatment Delivery | 1.06 | .30 | 0.00 | |||||
| In-person | 14.15 ± 5.07 | |||||||
| Telehealth | 14.36 ± 5.27 | |||||||
| Level of Care | 88.00 | <.001*** | 0.04 | (746) = 9.35, < .001*** | ||||
| PHP | 14.54 ± 5.04 | 14.95 ± 5.10 | ||||||
| IOP | 12.60 ± 4.87 | 12.04 ± 5.30 | ||||||
| Treatment Delivery × Level of Care | 3.55 | .06 | 0.00 | |||||
| DISCHARGE | ||||||||
| Treatment Delivery | 3.60 | .06 | 0.00 | |||||
| In-person | 8.42 ± 5.12 | 1.13 | ||||||
| Telehealth | 8.82 ± 5.27 | 1.05 | ||||||
| Level of Care | 48.07 | <.001*** | 0.02 | (798) = 7.28, < .001*** | ||||
| PHP | 8.82 ± 5.14 | 9.15 ± 5.31 | 1.12 | |||||
| IOP | 6.85 ± 4.71 | 7.49 ± 4.91 | 1.04 | |||||
| Treatment Delivery × Level of Care | 0.34 | .56 | 0.00 | |||||
| In-person PHP | 1.12 | |||||||
| In-person IOP | 1.20 | |||||||
| Telehealth PHP | 1.11 | |||||||
| Telehealth IOP | 0.89 | |||||||
| % CHANGE | ||||||||
| Treatment Delivery | 0.01 | .90 | 0.00 | |||||
| In-person | −37.34% (37.38%) | |||||||
| Telehealth | −37.06% (37.47%) | |||||||
| Level of Care | 0.00 | .96 | 0.00 | |||||
| PHP | −36.50% (37.43%) | −37.04% (34.73%) | ||||||
| IOP | −37.34% (37.38%) | −37.06% (37.47%) | ||||||
| Treatment Delivery × Level of Care | 2.67 | .10 | 0.00 | |||||
| Q-LES-Q | ||||||||
| ADMISSION | ||||||||
| Treatment Delivery | 0.26 | .61 | 0.00 | |||||
| In-person | 45.89 ± 16.07 | |||||||
| Telehealth | 46.22 ± 16.33 | |||||||
| Level of Care | 78.00 | <.001*** | 0.03 | (742) = −8.77, < .001*** | ||||
| PHP | 44.64 ± 15.87 | 44.55 ± 15.94 | ||||||
| IOP | 50.78 ± 15.94 | 52.75 ± 16.22 | ||||||
| Treatment Delivery × Level of Care | 1.59 | .21 | 0.00 | |||||
| DISCHARGE | ||||||||
| Treatment Delivery | 0.73 | .39 | 0.00 | |||||
| In-person | 61.05 ± 17.62 | 0.90 | ||||||
| Telehealth | 61.67 ± 17.48 | 0.91 | ||||||
| Level of Care | 39.14 | <.001*** | 0.02 | (780) = −6.46, < .001*** | ||||
| PHP | 59.73 ± 17.47 | 60.73 ± 17.71 | 0.93 | |||||
| IOP | 66.23 ± 17.27 | 65.31 ± 16.07 | 0.86 | |||||
| Treatment Delivery × Level of Care | 1.17 | .28 | 0.00 | |||||
| In-person PHP | 0.90 | |||||||
| In-person IOP | 0.93 | |||||||
| Telehealth PHP | 0.96 | |||||||
| Telehealth IOP | 0.78 | |||||||
| % CHANGE | ||||||||
| Treatment Delivery | 1.62 | .20 | 0.00 | |||||
| In-person | 21.46% (35.94%) | |||||||
| Telehealth | 21.06% (34.81%) | |||||||
| Level of Care | 2.69 | .10 | 0.00 | |||||
| PHP | 20.21% (42.93%) | 21.65% (36.79%) | ||||||
| IOP | 21.46% (35.94%) | 21.06% (34.81%) | ||||||
| Treatment Delivery × Level of Care | 2.33 | .13 | 0.00 | |||||
Note: Significance threshold used is 0.05. F-statistics and partial eta-squared (η2) reflect the ANOVA results at the group level. T-tests reflect significant pairwise comparisons. Cohen's D effect size reflects the change between admission and discharge score and is presented alongside discharge data only.
The same pattern of results seen for QIDS scores was also seen for Q-LES-Q scores, namely only a significant main effect of level of care at both admission ( F (2380) = 78.00, p < .001) and at discharge ( F (2380) = 39.14, p < .001). There was no main effect of treatment delivery or interaction between treatment delivery and level of care. Planned pairwise comparisons showed that Q-LES-Q admission and discharge scores were higher for patients in IOP relative to PHP, which is an expected result given the difference in degree of symptom severity at these different levels of care.
Pairwise Cohen's d effect sizes were calculated, as well as descriptive statistics for the change in QIDS-SR and Q-LES-Q scores from admission to discharge for all. Pairwise comparisons show the degree of change between admission and discharge scores comparing in-person and telehealth groups was not significant at either IOP or PHP levels of care for either QIDS-SR or Q-LES-Q. Effect sizes, overall, were moderate to high at all levels of care for both assessments. Length of stay was not significantly different comparing in-person and telehealth IOP groups ( t (481) = −1.66, p = .10), but it was significantly different comparing PHP groups, such that patients receiving telehealth stayed 2.8 days longer in treatment than patients seen in person ( t (1877) = −6.62, p < .001).
4. Discussion
To demonstrate the efficacy of telehealth treatment relative to in-person treatment, we compared clinical outcomes scores at admission and discharge for adult patients (1,192 in-person and 1,192 telehealth) across PHP and IOP programs. Patients who received PHP telehealth stayed an average of 2.8 days longer in treatment than the PHP in-person group; there was no difference in length of stay in IOP programs. This significant finding of increased length of stay in the PHP telehealth group is consistent with prior work ( Zimmerman et al., 2021b ). There were no significant differences in QIDS or Q-LES-Q discharge scores for either IOP or PHP groups, and there were no significant differences in the degree of change between admission and discharge scores for any group. Effect sizes were moderate to large across treatment modalities and levels of care. These data support remote treatment as a viable alternative to in-person mental health services, specifically as both in-person and remote patients experienced symptom reduction, and both populations reported improvements in quality of life.
There are recognized limitations of this study. Patients were not randomized into in-person and telehealth groups; rather, the external variable of the COVID-19 pandemic forced group membership in our sample. However, there were no between-group differences in QIDS-SR and Q-LES-Q admission scores at either the holistic level or by level of care, which suggests that no one group was more acute than the other at onset of treatment as indexed by these assessments. Further, matching in-person and telehealth groups for pre-treatment covariates—age, sex, race, and level of care—allowed us to examine the dependent variable of interest more closely, namely treatment outcomes, independent of these other factors. Additionally, findings are limited by the lack of a structured clinician-administered diagnostic assessment at admission which would strengthen the diagnoses established. However, licensed psychiatrists with years of experience diagnosing mental health disorders conducted the initial diagnostic assessments, and patient charts would be updated to reflect any changes to diagnoses made later in treatment.
Results have implications for both patients considering remote treatment options as well as organizations looking to implement alternatives to in-person care. Despite the difference in treatment delivery, our large sample size from a system-wide perspective supports telehealth as being as effective as in-person care for intensive-treatment-seeking individuals. For patients living far away from treatment centers or for patients who cannot leave home to attend in-person treatment, these results demonstrate telehealth treatment as a viable alternative to in-person treatment.
Author statement
Nyssa Z. Bulkes, Ph.D.: Methodology, Formal Analysis, Writing – Original Draft.
Kaley Davis, M.S.: Writing – Reviewing & Editing, Project Administration.
Brian Kay, Ph.D.: Resources, Writing – Reviewing & Editing, Conceptualization.
Bradley C. Riemann, Ph.D.: Resources, Writing – Reviewing & Editing, Conceptualization.
Declaration of competing interest
- American Psychiatric Association . American Psychiatric Pub; 2013. Diagnostic and Statistical Manual of Mental Disorders (DSM-5®) [ Google Scholar ]
- Cheng C., Cheung M.W. Psychological responses to outbreak of severe acute respiratory syndrome: a prospective, multiple time‐point study. J. Pers. 2005; 73 (1):261–285. [ PMC free article ] [ PubMed ] [ Google Scholar ]
- Chong J., Moreno F. Feasibility and acceptability of clinic-based telepsychiatry for low-income Hispanic primary care patients. Telemed. e Health. 2012; 18 (4):297–304. [ PubMed ] [ Google Scholar ]
- Chong M.Y., Wang W.C., Hsieh W.C., Lee C.Y., Chiu N.M., Yeh W.C., et al. Psychological impact of severe acute respiratory syndrome on health workers in a tertiary hospital. Br. J. Psychiatr. 2004; 185 (2):127–133. [ PubMed ] [ Google Scholar ]
- Cuevas C.D.L., Arredondo M.T., Cabrera M.F., Sulzenbacher H., Meise U. Randomized clinical trial of telepsychiatry through videoconference versus face-to-face conventional psychiatric treatment. Telemed. e Health. 2006; 12 (3):341–350. [ PubMed ] [ Google Scholar ]
- Czeisler M.É., Lane R.I., Petrosky E., Wiley J.F., Christensen A., Njai R., et al. Mental health, substance use, and suicidal ideation during the COVID-19 pandemic—United States, June 24–30, 2020. MMWR (Morb. Mortal. Wkly. Rep.) 2020; 69 (32):1049. [ PMC free article ] [ PubMed ] [ Google Scholar ]
- Frueh B.C., Henderson S., Myrick H. Telehealth service delivery for persons with alcoholism. J. Telemed. Telecare. 2005; 11 (7):372–375. [ PubMed ] [ Google Scholar ]
- Hilty D.M., Ferrer D.C., Parish M.B., Johnston B., Callahan E.J., Yellowlees P.M. The effectiveness of telemental health: a 2013 review. Telemed. e Health. 2013; 19 (6):444–454. [ PMC free article ] [ PubMed ] [ Google Scholar ]
- Ho D.E., Kosuke I., King G., Stuart E.A. MatchIt: nonparametric preprocessing for parametric causal inference. J. Stat. Software. 2011; 42 (8) [ Google Scholar ]
- Hom M.A., Weiss R.B., Millman Z.B., Christensen K., Lewis E.J., Cho S., et al. Development of a virtual partial hospital program for an acute psychiatric population: lessons learned and future directions for telepsychotherapy. J. Psychother. Integrat. 2020; 30 (2):366. [ Google Scholar ]
- Jacob M.K., Larson J.C., Craighead W.E. Establishing a telepsychiatry consultation practice in rural Georgia for primary care physicians: a feasibility report. Clin. Pediatr. 2012; 51 (11):1041–1047. [ PubMed ] [ Google Scholar ]
- Lopez A.M., Cruz M., Lazarus S., Webster P., Jones E.G., Weinstein R.S. Case report: use of American sign language in telepsychiatry consultation. Telemed. e Health. 2004; 10 (3):389–391. [ PubMed ] [ Google Scholar ]
- Manfredi L., Shupe J., Batki S.L. Rural jail telepsychiatry: a pilot feasibility study. Telemed. e Health. 2005; 11 (5):574–577. [ PubMed ] [ Google Scholar ]
- Moreno F.A., Chong J., Dumbauld J., Humke M., Byreddy S. Use of standard Webcam and Internet equipment for telepsychiatry treatment of depression among underserved Hispanics. Psychiatr. Serv. 2012; 63 (12):1213–1217. [ PubMed ] [ Google Scholar ]
- Morland L.A., Greene C.J., Rosen C.S., Foy D., Reilly P., Shore J., et al. Telemedicine for anger management therapy in a rural population of combat veterans with posttraumatic stress disorder: a randomized noninferiority trial. J. Clin. Psychiatr. 2010; 71 (7):855–863. [ PubMed ] [ Google Scholar ]
- Mucic D. Transcultural telepsychiatry and its impact on patient satisfaction. J. Telemed. Telecare. 2010; 16 (5):237–242. [ PubMed ] [ Google Scholar ]
- Nelson E.L., Barnard M., Cain S. Treating childhood depression over videoconferencing. Telemed. e Health. 2003; 9 (1):49–55. [ PubMed ] [ Google Scholar ]
- Pakyurek M., Yellowlees P., Hilty D. The child and adolescent telepsychiatry consultation: can it be a more effective clinical process for certain patients than conventional practice? Telemed. e Health. 2010; 16 (3):289–292. [ PubMed ] [ Google Scholar ]
- Price-Haywood E.G., Burton J., Fort D., Seoane L. Hospitalization and mortality among black patients and white patients with Covid-19. N. Engl. J. Med. 2020; 382 (26):2534–2543. [ PMC free article ] [ PubMed ] [ Google Scholar ]
- R Core Team . R Foundation for Statistical Computing; Vienna, Austria: 2021. R: A Language and Environment for Statistical Computing. https://www.R-project.org/ [ Google Scholar ]
- Rabinowitz T., Murphy K.M., Amour J.L., Ricci M.A., Caputo M.P., Newhouse P.A. Benefits of a telepsychiatry consultation service for rural nursing home residents. Telemed. e Health. 2010; 16 (1):34–40. [ PubMed ] [ Google Scholar ]
- Rajkumar R.P. COVID-19 and mental health: a review of the existing literature. Asian J. Psychiatr. 2020; 52 :102066. [ PMC free article ] [ PubMed ] [ Google Scholar ]
- Richardson L., McCauley E., Katon W. Collaborative care for adolescent depression: a pilot study. Gen. Hosp. Psychiatr. 2009; 31 (1):36–45. [ PMC free article ] [ PubMed ] [ Google Scholar ]
- Rojas S.M., Carter S.P., McGinn M.M., Reger M.A. A review of telemental health as a modality to deliver suicide-specific interventions for rural populations. Telemed. e Health. 2020; 26 (6):700–709. [ PubMed ] [ Google Scholar ]
- Rush A.J., Trivedi M.H., Ibrahim H.M., Carmody T.J., Arnow B., Klein D.N., Keller M.B. The 16-Item Quick Inventory of Depressive Symptomatology (QIDS), clinician rating (QIDS-C), and self-report (QIDS-SR): a psychometric evaluation in patients with chronic major depression. Biol. Psychiatr. 2003; 54 (5):573–583. [ PubMed ] [ Google Scholar ]
- Ruskin P.E., Silver-Aylaian M., Kling M.A., Reed S.A., Bradham D.D., Hebel J.R., et al. Treatment outcomes in depression: comparison of remote treatment through telepsychiatry to in-person treatment. Am. J. Psychiatr. 2004; 161 (8):1471–1476. [ PubMed ] [ Google Scholar ]
- Schechter D., Endicott J., Nee J. Quality of life of ‘normal’ controls: Association with lifetime history of mental illness. Psychiatr. Res. 2007; 152 (1):45–54. [ PMC free article ] [ PubMed ] [ Google Scholar ]
- Shore J.H., Brooks E., Savin D., Orton H., Grigsby J., Manson S.M. Acceptability of telepsychiatry in American Indians. Telemed. e Health. 2008; 14 (5):461–466. [ PMC free article ] [ PubMed ] [ Google Scholar ]
- Soklaridis S., Lin E., Lalani Y., Rodak T., Sockalingam S. Mental health interventions and supports during COVID-19 and other medical pandemics: a rapid systematic review of the evidence. Gen. Hosp. Psychiatr. 2020; 66 :133–146. [ PMC free article ] [ PubMed ] [ Google Scholar ]
- Storch E.A., Ehrenreich May J., Wood J.J., Jones A.M., De Nadai A.S., Lewin A.B., et al. Multiple informant agreement on the anxiety disorders interview schedule in youth with autism spectrum disorders. J. Child Adolesc. Psychopharmacol. 2012; 22 (4):292–299. [ PMC free article ] [ PubMed ] [ Google Scholar ]
- Urness D., Wass M., Gordon A., Tian E., Bulger T. Client acceptability and quality of life–telepsychiatry compared to in-person consultation. J. Telemed. Telecare. 2006; 12 (5):251–254. [ PubMed ] [ Google Scholar ]
- Vahratian A., Blumberg S.J., Terlizzi E.P., Schiller J.S. Symptoms of anxiety or depressive disorder and use of mental health care among adults during the COVID-19 pandemic—United States, August 2020–February 2021. MMWR (Morb. Mortal. Wkly. Rep.) 2021; 70 (13):490. [ PMC free article ] [ PubMed ] [ Google Scholar ]
- Weiner M.F., Rossetti H.C., Harrah K. Videoconference diagnosis and management of Choctaw Indian dementia patients. Alzheimer's Dementia. 2011; 7 (6):562–566. [ PMC free article ] [ PubMed ] [ Google Scholar ]
- Whaibeh E., Mahmoud H., Naal H. Telemental health in the context of a pandemic: the COVID-19 experience. Curr. Treat. Options Psychiatr. 2020; 7 (2):198–202. [ PMC free article ] [ PubMed ] [ Google Scholar ]
- Ye J., Shim R., Lukaszewski T., Yun K., Kim S.H., Rust G. Telepsychiatry services for Korean immigrants. Telemed. e Health. 2012; 18 (10):797–802. [ PMC free article ] [ PubMed ] [ Google Scholar ]
- Yellowlees P., Shore J., Roberts L. Practice guidelines for videoconferencing-based telemental health–October 2009. Telemed. e Health. 2010; 16 (10):1074–1089. [ PubMed ] [ Google Scholar ]
- Zimmerman M., Benjamin I., Tirpak J.W., D'Avanzato C. Patient satisfaction with partial hospital telehealth treatment during the COVID-19 pandemic: comparison to in-person treatment. Psychiatr. Res. 2021:113966. [ PMC free article ] [ PubMed ] [ Google Scholar ]
- Zimmerman M., Terrill D., D'Avanzato C., Tirpak J.W. Telehealth treatment of patients in an intensive acute care psychiatric setting during the COVID-19 pandemic: comparative safety and effectiveness to in-person treatment. J. Clin. Psychiatr. 2021; 82 (2) 0-0. [ PubMed ] [ Google Scholar ]
- Open access
- Published: 27 September 2024
Assessing the health status of migrants upon arrival in Europe: a systematic review of the adverse impact of migration journeys
- Cristina Canova 1 ,
- Lucia Dansero 2 ,
- Cinzia Destefanis 2 ,
- Clara Benna 1 , 3 &
- Isabella Rosato 1
Globalization and Health volume 20 , Article number: 69 ( 2024 ) Cite this article
Metrics details
Numerous studies have explored the impact of pre- and post-migration factors on the overall health of migrant populations. The objective of this study is to enhance our understanding of additional determinants affecting migrants' health by examining the impact of the migration phase and related journeys in the European context.
We conducted a systematic review of studies published in the MEDLINE, Embase, and Scopus databases from 2003 up to January 5, 2024. We included observational studies reporting information on the health status of migrant populations recorded upon arrival in a country situated in Europe, and on the transit phase, including specific risk factors experienced during the journey or its characteristics. Title and abstract screening were performed using active learning techniques provided by ASReview software. The results of the included studies were presented qualitatively, with a focus on publications that formally assessed the association between the journey and the investigated health outcomes. The systematic review was registered on PROSPERO, CRD42024513421.
Out of 11,370 records screened, we ultimately included 25 studies, all conducted since 2017. Most adopted a cross-sectional design and a quantitative approach, with relatively small sample sizes. The majority of the studies were conducted in Serbia and Italy. Only 14 of them formally assessed the association between different exposures in the transit phase and health outcomes, including mental health, well-being and quality of life, infectious and non-communicable diseases.
Epidemiological research focusing on the transit phase in Europe remains limited, with few available studies facing challenges related to data collection, study design and analysis, thereby limiting the interpretability and generalisability of their results. These findings underscore the need for action, prompting the development of adequate and feasible strategies to conduct additional studies focusing on migrant populations during migration journeys.
Introduction
Driven by various geopolitical, economic and social factors, the dimensions of migration flows in European countries have increased in recent years [ 1 ]. A notable number of migrants, escaping from conflict-ridden nations such as Syria, Afghanistan, and Somalia, have marked the onset of what is commonly referred to as the “European migration crisis” [ 2 , 3 ]. In 2015, more than 65 million people migrated towards Europe, posing an unprecedented challenge for European countries [ 4 ]. According to the World Health Organization (WHO), European regions host approximately 36% of the global international migrant population [ 5 ]. In 2023, almost 293,000 migrants arrived in Europe [ 6 ] through one of the main migratory routes: the Western Mediterranean, Central Mediterranean, and Eastern Mediterranean/Balkan routes [ 7 , 8 , 9 ].
These diverse populations are commonly referred to as "migrants", a term defined by the International Organization for Migration (IOM) to describe all individuals who move across an international border or within a state away from their habitual place of residence, regardless of legal status, whether the movement is voluntary or involuntary, the causes of the movement, or the length of the stay [ 10 ].
The relationship between migration and health is extremely intricate. On the one hand, migrating from a context of conflict and extreme poverty could potentially improve health and social standing; on the other hand, the migration journey itself could constitute a significant health risk [ 11 ]. Migratory status can introduce complexity, leaving migrants and refugees more vulnerable to specific health factors depending on the various stages of their displacement. During migration journeys, migrants can suffer from hunger and thirst, experience extortion and robbery, endure maltreatment, violence, and torture [ 12 ]. In some cases, they also report experiences of arrest and deportation. Several psychological and physical issues can be related to the dangerous experiences of the migration transit phase [ 13 , 14 ].
Various studies have explored the health status and well-being of migrant populations both before and after the completion of their journeys, in their countries of origin and destination in the post-migration phase [ 15 , 16 , 17 ]. However, there is a gap in the understanding of migrants’ health during the migration journey [ 18 ], which may be attributed to challenges in data collection, the lack of organized medical records, and the fragmentation of information collected across different countries during the transit process [ 19 ].
To date, there appears to be no systematic review specifically conducted addressing the health status and associated risks encountered by migrant populations during their transit from their country of origin towards European destinations. This systematic review, therefore, aims to determine the health status and health risks faced by migrants during their journey to Europe. The specific objectives are to gather information on the characteristics of migratory paths and typical routes, to examine the experiences, risk factors and potentially traumatic events that occurred during the migration journey, to identify the health outcomes investigated, and to gather information on study designs and tools utilized, as well as the challenges faced by researchers in describing migration journeys and related outcomes. Additionally, our systematic review will focus on studies that formally assessed the association between experiences during transit and related health outcomes, to gain insight into the impact of these factors on the migrants’ health status recorded upon arrival in transit or destination countries.
Materials and methods
Search strategy and selection criteria.
We conducted a systematic search following the Preferred Reporting Items for Systematic Reviews and Meta-Analyses 2020 (PRISMA) guidelines [ 20 ]. The study protocol was registered on PROSPERO (CRD42024513421). Following the PECO (Population, Exposure, Comparator, Outcome) framework (Table S1), we aimed to identify all available papers providing information on the health status of migrant populations (as defined by IOM) upon recent arrival in a transit or destination country in Europe (from less than 24 months), and on the characteristics or specific risk factors of their migration journey experience.
The search was conducted on January 5, 2024 over the following electronic databases: PubMed, Scopus, EMBASE. We used a comprehensive search string developed based on previous literature on the topic [ 21 , 22 ], which included terms and synonyms related to migrant populations, health outcomes and European countries with spelling variations to ensure the capture of all relevant studies. Keywords referred to the population, exposure and outcome were searched in title/abstract, while keywords related to the setting were searched as free terms (all fields) to identify studies conducted in Europe, considering also the reported affiliations of the studies’ authors. The specific search strategy is listed in the Supplementary material (Table S2).
Studies were considered eligible for the systematic review if they met all the following criteria: a) focused on migrants’ health status upon arrival in a transit or destination country in Europe; b) the arrival in the country occurred less than 24 months prior to the study period (this period of time was selected to ensure that sufficient time was allocated for conducting the studies, recruiting participants in camps, and collecting data); c) provided information on the characteristics of migration journeys (at least one among duration, route and type of travel, transit countries) or on the specific risk factors experienced during the journey (experiences and events potentially harmful for health occurred during the journey, such as torture, sexual, physical and psychological violence); d) were published in English or Italian language; e) were published within the last 20 years. A 20-year time frame was selected to acquire the most up-to-date and reliable data related to migrant populations in Europe, considering the rapid changes in migration routes and policies over the years.
We excluded systematic or scoping reviews, commentaries, editorials, conference abstracts, case reports, and study protocols. Additionally, studies in which the origin of migrants was not specified, studies investigating the health status of migrants only before the start of their journey (in their country of origin), studies investigating the health status of foreign nationals residing in the destination country or individuals who have been in the destination country for more than 24 months, and studies providing information exclusively on subgroups of subjects presenting adverse health conditions, were excluded.
Title and abstract screening was performed using ASReview version 1.3, a software that uses Artificial Intelligence to speed up the title/abstract screening phase [ 23 , 24 ]. ASReview uses active learning to influence the order of articles based on relevance for the inclusion process [ 25 ]. A single reviewer (IR) provided initial training data to ASReview and the classifier created a progressive ranking of the unseen records. The same reviewer then screened the relevant papers; when many articles are excluded in a row, it can be assumed that the articles listed after them can be labelled as irrelevant [ 26 ]. The software developers advise a screen-stop decision after 100–120 consecutively excluded studies. To ensure we would not miss relevant studies we decided on a screening-stop decision after 150 consecutively excluded studies [ 27 , 28 ].
The full-text screening was then independently performed using Covidence software [ 29 ] by three reviewers (CC, CB and IR), considering all the papers included after the initial screening using ASReview. Any discrepancy was resolved through discussion. Once full texts were selected, reference lists were screened to search for potentially relevant studies.
Data analysis
Data extraction was conducted by two different reviewers (IR and CB). For each included study, we extracted detailed information on four different topics: a) characteristics of the study (title, author, publication year, journal, study design, sources, period and language for data collection, who collected data, type of database, informed consent, European country in which the study was conducted); b) characteristics of the population (sample size, number of males/females, mean/median age, inclusion of children, accompanied/unaccompanied status, presence of vulnerability, level of education, occupation, terms used to define the migrant population, country/geographic area of origin, partnering status, legal status and planned steps; c) characteristics of exposure (time since arrival, reason for migration, travel duration, whether migration occurred by sea, air, or land, journey route, specific risk factors during journey, how they were measured, specific tools used, perpetrator of violence); d) characteristics of health outcomes (how they were measured, specific tools used, presence of formally assessed association, how they formally assessed the association).
Due to the heterogeneous characteristics of the included studies in terms of population, outcomes, and study design, it was not possible to conduct a meta-analysis. Results were qualitatively presented using graphical representations, creating geographic maps and heatmaps showing the association between exposures and outcomes investigated in the included studies, and the associations that were formally assessed in the included studies.
A risk of bias assessment was conducted for all included studies that formally investigated the association between exposures and outcomes, using the Joanna Briggs assessment tool for cross-sectional or cohort studies [ 30 ]. Two different reviewers (IR and CB) independently assessed the risk of bias for each item provided in the tool. In cases of disagreement, a third reviewer (CC) intervened to resolve the discrepancies. Following to the Joanna Briggs guidelines, instead of assigning a single overall score to each study, we provided a comprehensive assessment of all items. This approach allowed us to identify domains where studies were either lacking or adequate in terms of bias risk.
After removing duplicates, we identified a total of 11,370 records across the three databases, of which 78.6% were marked as not relevant after employing the ASReview tool. In the full-text screening phase, 442 papers were assessed for eligibility, and ultimately, 25 papers were included in the review (Fig. 1 ).

Study selection
Studies’ characteristics
Table 1 and Table S3 present the general characteristics of the included studies. All studies were published from 2017, with the majority from 2020 ( n = 16, 64.0%). The cross-sectional study design was the most adopted, investigating characteristics of exposures and outcomes of interest simultaneously ( n = 21, 84.0%). Four studies (16.0%) employed a longitudinal design, investigating migrants’ characteristics during the transit phase and after their resettlement in destination countries [ 31 , 32 , 33 , 34 ]. In most cases ( n = 19, 76.0%) researchers collected quantitative information. Only one study was qualitative (4.0%) [ 35 ], while mixed methods research was employed in the remaining five studies (20.0%).
The majority of the studies employed population-based samples, enrolling all individuals residing in camps and dedicated facilities during the study periods, while in other cases ( n = 9, 36.0%) the investigators employed opportunistic samples. One study (4.0%) used secondary data, relying on information from medical records and health documentation [ 36 ]. The target population participated in the studies mainly while hosted in refugee camps/asylum centers ( n = 15, 60.0%), or in facilities where migrants admitted for resettlement in Europe attended mandatory pre-departure educational activities ( n = 4, 16.0%).
We observed that Higher Education Institutes (HEIs) were the most frequently involved organizations ( n = 6, 24.0%) in the implementation of the studies. In other instances, HEIs were responsible for the studies with the support of IOM ( n = 4, 16.0%). Médecins sans Frontierès (MSF) was the non-governmental organization (NGO) most frequently involved (present in four out of six studies carried out by NGOs). Public Health Institutes (such as the Swiss Tropical and Public Health Institute, the Finnish Institute for Health, the National Institute for Health, Migration and Poverty) were responsible for four (16.0%) of the included studies. In four studies (16.0%), multiple organisations were involved and collaborated in the study process.
In the included studies, data were collected over limited time periods, with mean durations of seven months. The data collection period ranged from a minimum of 15 days to a maximum of 26 months. In most instances, data collection was carried out by the study researchers with the assistance of cultural mediators ( n = 7, 28.0%), healthcare workers with mediators ( n = 6, 24.0%), or by researchers or healthcare workers alone ( n = 10, 40.0%). The healthcare workers involved included physicians, nurses, psychologists, and others.
Populations’ characteristics
Table 1 , Table S3 and Table S4 contain information regarding the populations’ characteristics. The sample sizes were relatively small, ranging from 30 to 2484, with a mean of 463 subjects. The distribution of males and females was homogeneous. Overall, 14 studies (56.0%) were conducted on young adults only, while 11 (44.0%) included also accompanied or unaccompanied minors. Among these, three studies (12.0%) were conducted on minors only, comprising a population aged between 6 and 17 years old [ 37 , 38 , 39 ]. Almost all studies defined their population as either refugees or asylum seekers. Although these terms are distinct, they were used interchangeably by study researchers to refer to study participants regardless of their legal status at the time of the research.
Figure 2 presents a comprehensive overview of the study locations and the main countries of origin of the included populations. Most of the studies involved populations originating from Syria ( n = 11, 44.0%). Ten studies (40.0%) included populations from the African continent, especially Western Africa (Gambia, Senegal, Nigeria, Guinea, Mali). In other studies, the main country of origin was Afghanistan ( n = 3, 12.0%), while one study included populations mainly originating from Middle Eastern or North African countries [ 40 ].

Study locations, main countries of origin and migratory routes towards Europe. The black arrow represents four longitudinal studies in which the initial phases were conducted in Lebanon, and follow-up was conducted in Norway
Regarding the location of the studies, the majority were conducted in Italy and Serbia ( n = 7, 28.0% and n = 6, 24.0%, respectively), followed by Norway ( n = 4, 16.0%). The remaining studies were conducted in Greece ( n = 3, 12.0%), France ( n = 2, 8.0%), Switzerland ( n = 1, 4.0%), Bosnia-Herzegovina ( n = 1, 4.0%) and Finland ( n = 1, 4.0%). Not all studies provided information on the migratory routes used by migrants but based on countries/areas of origin of included populations and study locations we can infer two primary paths: the Central Mediterranean route, to reach Italy, France and Switzerland coming from Western, Northern and Eastern Africa, and the Balkan route, with migrants originating mainly from Syria, Afghanistan and Iraq. It is noteworthy that we did not identify any study on migrants travelling via the Western Mediterranean route.
Journey characteristics, specific risk factors experienced during the journey and health outcomes
The migration journey experience was divided into two categories: journey characteristics ( n = 24 studies, 96.0%) and specific risk factors experienced during travel ( n = 21 studies, 84.0%) (Table S3). A total of 19 studies (76.0%) reported information on the time since arrival in the country where the study was conducted, expressed in median/mean number of days/months/years. In the included studies, migrants had been in those countries for a few days to several months, and in some cases, for more than a year. Two studies (8.0%) stated that migrants were newly arrived without providing further details [ 40 , 41 ]. A total of five studies (20.0%) provided detailed information on the reasons behind migration, which was predominantly driven by factors such as war and conflict, the pursuit of international protection, insecurity, political instability and persecution (Table S3). The duration of travel was reported in 19 studies (76.0%), either as the median time of travel duration (and I-III quartile) or using specific categories. In the included studies, the journeys lasted from one to 60 months (see Additional file 2). Only eight studies (32.0%) specified the journey type, indicating whether migration occurred by sea, air, or land. Additionally, data on the presence of a transit country, the number of transit countries, the median duration of stay in transit countries, and the transit countries crossed were obtained from 11 out of 25 studies (44.0%) (Table S3).
Specific risk factors pertaining to the transit phase included, among others, violent events and trauma experiences, potentially traumatic events, and difficulties encountered during the journey. These risk factors were presented in the included studies either by considering the total number of events experienced by the subjects or by providing detailed information regarding the type of events (torture, threats, sexual or physical violence, robbery, incarceration, forced labor and others). While journey characteristics were consistently assessed through specifically developed questions, validated questionnaires were utilized for evaluating the risk factors experienced during travel. These instruments were either specifically designed for journey experiences or adapted from more generic questionnaires on trauma [ 42 ] (Table S3).
Most of the included studies focused on mental health ( n = 15, 60.0%) as the main health outcome of interest, investigating the presence of anxiety and depression disorders, post-traumatic stress disorder (PTSD) and other psychological symptoms. Studies on physical health ( n = 4, 16.0%) examined the presence of non-communicable diseases (NCDs) and infectious diseases. One study was exclusively focused on perceived health, including well-being and perceived quality of life in participants ( n = 1, 4.0%) [ 34 ]. Five studies (20.0%) addressed multiple health outcomes (Fig. 3 a). The following heatmap (Fig. 3 a) describes all potential combinations of exposures and outcomes investigated in the included papers. Exposures were categorised into specific risk factors experienced during the journey and journey characteristics. Health outcomes were classified into mental health, including anxiety, depression, other psychological symptoms and PTSD symptoms, non-communicable diseases, infectious diseases, well-being and quality of life.

Heatmap for combinations of investigated exposures and outcomes ( a ) and associations between investigated exposures and outcomes ( b )
For each cell, we reported the total number of studies providing information for that combination of exposure and outcome. The colour intensity in each cell reflects the number of studies, indicating that the majority of the available literature focused on mental health problems in combination with the total number of traumatic events experienced, the duration of the journey, and the time since arrival in the countries where the studies were conducted. As previously stated, only 14 out of 25 studies (56.0%) formally assessed the associations between exposures and health outcomes [ 31 , 32 , 33 , 34 , 42 , 43 , 44 , 45 , 46 , 47 , 48 , 49 , 50 , 51 ]. The associations evaluated in these studies are presented in the heatmap (Fig. 3 b). Most of these studies focused on the relationship between mental health problems and the total number of traumatic events, showing that increased exposure to various types of traumatic experiences during the journey was associated with higher risks of experiencing anxiety, depression and PTSD [ 31 , 42 , 44 , 51 ]. Furthermore, a higher risk of mental health problems was positively linked to the length of the journey and the time since arrival [ 45 , 46 , 49 , 50 ]. In addition, a few studies also examined the positive association between exposure to sexual and physical violence, the selection of specific journey routes, and the occurrence of infectious diseases [ 43 , 47 ].
With regard to the characteristics evaluated in the risk of bias assessment (Table S5), it was observed that nearly all included studies adequately defined their inclusion criteria and described subjects and study settings. Furthermore, all studies employed valid methodologies for measuring exposure and outcomes, utilising validated questionnaires or surveys specifically developed for the study’s purposes. However, it is noteworthy that while all studies identified possible confounding factors, some of them ( n = 4, 16.0%) did not employ specific strategies to address these confounders in the statistical analysis. This may be attributed to the limited sample sizes available in the included studies.
We conducted a systematic review of published studies investigating the health status of migrant populations upon their arrival in European countries, with a focus on the experiences and risk factors associated with the migration journey. A total of 25 studies met the inclusion criteria, encompassing various study designs, populations, and health outcomes. Of these, only 14 formally assessed the association between transit-related exposures and health outcomes.
In the studies included in the review, mental health disorders and psychological trauma emerged as the predominant health issues investigated among migrants. Several studies have reported high prevalence rates of PTSD, depression, and anxiety among migrant populations, highlighting the urgent need for mental health support upon arrival [ 48 , 49 , 52 ]. The risk of infectious diseases was another key health outcome identified. Studies have highlighted the prevalence of conditions such as tuberculosis, hepatitis, and various parasitic infections, which are exacerbated by poor living conditions and limited access to healthcare during transit [ 37 , 43 ]. Sexually transmitted diseases (STDs) were also reported among the prevalent infectious diseases identified [ 47 ]. Chronic NCDs have been less studied in the included papers although they represent a cause for concern, due to the significant burden they may pose to healthcare systems in receiving countries [ 33 ]. Indeed, the available studies report that migrants are at high risk of NCDs, particularly cardiovascular, musculoskeletal and respiratory diseases, for which they often do not receive adequate treatment [ 31 , 36 ].
The systematic review highlights that migrants in transit may be exposed to various risk factors, encompassing a range of traumatic events, including physical and verbal violence, torture and threats, sexual violence and exploitation, detention, robbery and forced labour. These events can occur in many ways; migrants may experience them personally or witness them [ 53 , 54 ]. Exposure to these risks may also be gender-related, as women and girls may be more likely to experience sexual violence, while men and boys may also endure physical violence, forced labour, and inhuman and degrading treatments [ 55 , 56 , 57 ]. However, sexual violence against migrant boys and men is often underreported due to social and cultural stigma, as well as the belief that men cannot be victims of rape [ 58 ]. The impact of experiencing these traumatic events can be multifaceted, with potential health effects ranging from physical (such as wounds, fractures, and infectious diseases) to mental and psychological (such as anxiety, depression, PTSD, and substance abuse). Researchers have highlighted significant challenges in documenting individual histories, particularly when reporting instances of sexual violence [ 49 ].
Most of the studies in our systematic review related traumatic events to anxiety and depression symptoms, PTSD, and other mental disorders [ 42 , 44 , 45 , 46 , 51 ], with comparatively less research on their effect on physical health [ 47 ]. The prevalence and type of violent and traumatic experiences that occurred during transit and pushbacks may influence both the incidence and severity of mental disorders, which may also become chronic. Indeed, in host countries, many migrants either lack access to mental health services or encounter barriers to obtaining them, facing interruptions in continuous care [ 59 ]. Even if less investigated in the included studies, communicable diseases remain a major health issue for migrating populations. Sexually transmitted diseases are closely linked to sexual violence, which may occur during transit and displacement in dangerous transit countries [ 36 , 47 , 56 ].
The main migration routes to Europe comprise the Western, Central, and Eastern Mediterranean, which include maritime pathways, along with the Balkan route, used predominantly by migrants traveling by land [ 7 ]. The real impact of the Mediterranean routes on migrant populations’ health is difficult to estimate, as the total number of people drowning during the sea crossing is unknown [ 60 ]. Different routes are chosen based on individual sociodemographic variability and journey-related factors, with both elements contributing to shaping dynamic migration trajectories [ 61 ].
A few studies examined the role of the characteristics of the migratory route, the journey duration, transit countries, and countries of origin in impacting health outcomes. These aspects tend to determine the violence and events experienced by migrants during transit; for instance, routes crossing countries with notorious exploitation systems for migrant populations, considerably increase the risk of experiencing physical violence, sexual exploitation, rape, torture, and incarceration, with negative effects on psychological health [ 44 , 56 ]. Regional differences in the types of physical violence experienced are notable, with people transiting through countries in the WHO African and Eastern Mediterranean regions frequently reporting detention and torture, often as a result of political violence or actions by state actors [ 11 ]. Moreover, violence can also be encountered in the receiving country, compounding the trauma experienced during transit. Additionally, the practice of pushbacks, which involve forcibly returning migrants to their country of origin or a third country, significantly worsens health outcomes [ 51 , 62 ].
In some studies, researchers have focused on the link between the length of the journey and migrants’ mental health [ 45 , 46 ]. Results suggest that prolonged stays in refugee camps during the asylum process, as well as dangerous and protracted long journeys, predispose individuals to extreme physical and psychological distress, heightening the risk of depression [ 50 ]. Conversely, shorter stays in transit countries before resettlement were associated with better mental health outcomes over time [ 33 ]. Moreover, chronic conditions could suffer from extreme delays in diagnosis and treatment due to the journey itself and lack of access to healthcare in the receiving countries, while traveling in small clusters of people, with prolonged sharing of time and places, may influence the prevalence of parasitic infestations [ 43 ].
In studies with a longitudinal design, most migration-related stressors were found to be more closely associated with chronic pain and mental health problems after resettlement compared to the transit phase [ 32 , 33 , 34 , 41 ]. Researchers delved into the concept of general well-being and self-reported health for these populations, underlining how mental health outcomes improved in the early post-migration phase [ 33 ] along with the quality of life over time [ 34 ]. These studies provide useful insight into the sequential changes in health among people moving from completely disparate settings, but as reported in the review, their number is limited.
The main strengths of our analysis lie in the comprehensive search string used and in the specific definition of our inclusion and exclusion criteria. Our criteria ensured the retrieval of papers that effectively presented information regarding both exposures and health outcomes related to the transit phase, while excluding a significant number of publications focused solely on the characteristics of the journey or on health upon arrival in destination countries. The limitations of our review are primarily related to the scarcity of available research on the topic and to the heterogeneous characteristics of the included studies, which did not allow us to conduct a meta-analysis of the results.
To our knowledge, various additional health outcomes have not been adequately considered in this research field thus far, including the health of vulnerable populations such as pregnant women and people with disabilities. Conversely, while certain topics, such as the prevalence of NCDs or STDs, have been widely explored in studies conducted on migrant populations upon arrival in destination countries in Europe [ 16 ], there may still be room for an increase in the number of studies reporting also information on the migration journey as possible risk factor. Interestingly, we did not encounter papers that investigated the characteristics of migrants following the Eastern Mediterranean route, while others, especially the Balkan route, were well represented. This finding underscores the presence of gaps in the evaluation of migration trajectories in the European context and suggests the need for further exploration in future research. Filling these gaps could enhance our understanding of the challenges posed by the transit phase.
The results highlighted by this systematic review underscore the importance of prioritizing the unique health needs of these populations [ 63 ], considering the possible role of several different determinants and experiences in influencing individual well-being. In particular, we suggest that future studies should pay greater attention to the potential impact of the transit phase on the health profile of these populations, in conjunction with other factors pertaining to the pre-migration and post-migration phases [ 64 , 65 ].
In their countries of origin, migrants are forcibly exposed to war, conflicts, persecution, poverty, and hunger. Upon arriving in their destination country, migrants can still face barriers in accessing healthcare and utilizing screening services [ 64 ]. Various studies have explored the role of these determinants [ 16 ], yet research on the threats posed during the transit phase remains scarce, fragmented, and only emerged in very recent years. During the migration journey, migrants are exposed to secondary trauma, including physical safety risks, kidnapping, imprisonment, lack of food and water, and difficult living conditions in refugee camps [ 3 ]. These conditions, combined with the absence of structured and organized flows of medical records [ 19 ], make it methodologically difficult to realize and conduct observational studies, thus influencing the amount of information available to researchers.
During travel, as well as in the countries of transit, migrants’ health outcomes will depend on the travel conditions and mode of travel, including the number and type of potentially traumatic experiences. The qualitative results provided by our systematic review highlight the scarcity of studies that offer insight into migrants’ journeys, their characteristics, and the specific risk factors experienced in relation to health outcomes. The number of studies investigating both the journeys’ characteristics and related health outcomes is low, and the number of studies that formally assessed the presence of an association between the experiences of the transit phase and health outcomes is even lower.
Our findings underscore the limitations of our knowledge regarding the determinants of the health of migrant populations, including migration processes among them. The lack of information in our possession regarding the difficulties experienced during migration journeys and related traumatic events limits the discussion on the impact of the transit phase on migrants’ health.
Availability of data and materials
All data generated or analysed during this study are included in this published article and its supplementary information files.
Data availability
No datasets were generated or analysed during the current study.
Abbreviations
World Health Organization
International Organization for Migration
Médecins sans Frontierès
Non-governmental organization
Post-traumatic stress disorder
Non-communicable diseases
Sexually transmitted diseases
GC2_SriLanka_Report_2017_FINAL_22.09.2017_Internet.pdf . [cited 2024 May 20]. Available from: https://www.iom.int/sites/g/files/tmzbdl486/files/our_work/DMM/Migration-Health/GC2_SriLanka_Report_2017_FINAL_22.09.2017_Internet.pdf .
Schilling T, Rauscher S, Menzel C, Reichenauer S, Müller-Schilling M, Schmid S, et al. Migrants and Refugees in Europe: Challenges. Experiences and Contributions Visc Med. 2017;33(4):295–300.
Article PubMed Google Scholar
Das B. Mental Health Trauma Treatment within the Current Mediterranean Refugee Crisis. Int J Adv Couns. 2019;41(4):481–91.
Article Google Scholar
Turakova Z. The Mediterranean Crisis. Diss Theses. 2019; Available from: https://academicworks.cuny.edu/cc_etds_theses/801 .
Statistics on migration to Europe - European Commission. [cited 2024 May 20]. Available from: https://commission.europa.eu/strategy-and-policy/priorities-2019-2024/promoting-our-european-way-life/statistics-migration-europe_en .
DTM_Mixed Migration Flows to Europe_Yearly_2023_0.pdf. [cited 2024 Sep 9]. Available from: https://dtm.iom.int/sites/g/files/tmzbdl1461/files/reports/DTM_Mixed%20Migration%20Flows%20to%20Europe_Yearly_2023_0.pdf .
The World’s Congested Human Migration Routes in 5 Maps | IOM Blog. [cited 2024 May 17]. Available from: https://weblog.iom.int/worlds-congested-human-migration-routes-5-maps .
Idemudia E, Boehnke K. Travelling Routes to Europe. In 2020. p. 33–49.
FCR December 2019–6_published.pdf. [cited 2024 May 17]. Available from: https://dtm.iom.int/sites/g/files/tmzbdl1461/files/reports/FCR%20December%202019-6_published.pdf .
Nations U. United Nations. United Nations; [cited 2024 May 17]. Migrants. Available from: https://www.un.org/en/fight-racism/vulnerable-groups/migrants .
World report on the health of refugees and migrants. [cited 2024 May 15]. Available from: https://www.who.int/publications-detail-redirect/9789240054462 .
Abused and Neglected: UNODC study reveals violence suffered by migrants. [cited 2024 May 15]. Available from: https://www.unodc.org/lpo-brazil/en/frontpage/2022/01/abused-and-neglected-unodc-study-reveals-violence-suffered-by-migrants.html .
Fassin D, Defossez AC. Displaced people’s perilous journeys: border violence as a public health issue. Lancet. 2023;402(10409):1209–11.
Wickramage K, Vearey J, Zwi AB, Robinson C, Knipper M. Migration and health: a global public health research priority. BMC Public Health. 2018;18(1):987.
Article PubMed PubMed Central Google Scholar
Pfarrwaller E, Suris JC. Determinants of health in recently arrived young migrants and refugees: a review of the literature. Ital J Public Health. 2012;9(3). [cited 2024 May 15]. Available from: https://ijphjournal.it/article/view/7529 .
Lebano A, Hamed S, Bradby H, Gil-Salmerón A, Durá-Ferrandis E, Garcés-Ferrer J, et al. Migrants’ and refugees’ health status and healthcare in Europe: a scoping literature review. BMC Public Health. 2020;20(1):1039.
Mesa-Vieira C, Haas AD, Buitrago-Garcia D, Roa-Diaz ZM, Minder B, Gamba M, et al. Mental health of migrants with pre-migration exposure to armed conflict: a systematic review and meta-analysis. Lancet Public Health. 2022;7(5):e469–81.
Bozorgmehr K, Samuilova M, Petrova-Benedict R, Girardi E, Piselli P, Kentikelenis A. Infectious disease health services for refugees and asylum seekers during a time of crisis: A scoping study of six European Union countries. Health Policy Amst Neth. 2019;123(9):882–7.
Chiesa V, Chiarenza A, Mosca D, Rechel B. Health records for migrants and refugees: A systematic review. Health Policy Amst Neth. 2019;123(9):888–900.
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;29(372):n71.
Winters M, Rechel B, de Jong L, Pavlova M. A systematic review on the use of healthcare services by undocumented migrants in Europe. BMC Health Serv Res. 2018;18(1):30.
Cooper B, Behnke NL, Cronk R, Anthonj C, Shackelford BB, Tu R, et al. Environmental health conditions in the transitional stage of forcible displacement: A systematic scoping review. Sci Total Environ. 2021;25(762):143136.
developers AsrL. ASReview LAB Software Documentation. 2023. [cited 2024 Apr 29]; Available from: https://zenodo.org/records/10066693 .
van Dijk SHB, Brusse-Keizer MGJ, Bucsán CC, van der Palen J, Doggen CJM, Lenferink A. Artificial intelligence in systematic reviews: promising when appropriately used. BMJ Open. 2023;13(7):e072254.
van de Schoot R, de Bruin J, Schram R, Zahedi P, de Boer J, Weijdema F, et al. An open source machine learning framework for efficient and transparent systematic reviews. Nat Mach Intell. 2021;3(2):125–33.
Boetje J, van de Schoot R. The SAFE procedure: a practical stopping heuristic for active learning-based screening in systematic reviews and meta-analyses. Syst Rev. 2024;13(1):81.
Westendorp J, Geerse OP, Van Der Lee ML, Schoones JW, Van Vliet MHM, Wit T, et al. Harmful communication behaviors in cancer care: A systematic review of patients and family caregivers perspectives. Psychooncology. 2023;32(12):1827–38.
Penfornis KM, Van Vliet MHM, Meijer E, Gebhardt WA. Mapping the evidence on identity processes and identity-related interventions in the smoking and physical activity domains: a scoping review protocol. BMJ Open. 2022;12(7):e058405.
Covidence systematic review software, Veritas Health Innovation, Melbourne, Australia. Available at www.covidence.org . Covidence.
JBI Critical Appraisal Tools | JBI. [cited 2024 May 15]. Available from: https://jbi.global/critical-appraisal-tools .
Strømme EM, Haj-Younes J, Hasha W, Fadnes LT, Kumar B, Igland J, et al. Health status and use of medication and their association with migration related exposures among Syrian refugees in Lebanon and Norway: a cross-sectional study. BMC Public Health. 2020;20(1):341.
Strømme EM, Igland J, Haj-Younes J, Kumar BN, Fadnes LT, Hasha W, et al. Chronic pain and mental health problems among Syrian refugees: associations, predictors and use of medication over time: a prospective cohort study. BMJ Open. 2021;11(9):e046454.
Strømme EM, Haj-Younes J, Hasha W, Fadnes LT, Kumar B, Igland J, et al. Changes in health among Syrian refugees along their migration trajectories from Lebanon to Norway: a prospective cohort study. Public Health. 2020;186:240–5.
Haj-Younes J, Strømme EM, Igland J, Kumar B, Abildsnes E, Hasha W, et al. Changes in self-rated health and quality of life among Syrian refugees migrating to Norway: a prospective longitudinal study. Int J Equity Health. 2020;19(1):188.
Arsenijević J, Burtscher D, Ponthieu A, Severy N, Contenta A, Moissaing S, et al. ‘I feel like I am less than other people’: Health-related vulnerabilities of male migrants travelling alone on their journey to Europe. Soc Sci Med. 2018;209:86–94.
Bronsino M, Castagneri C, Spinazzola M, Pepe RR, Sacerdote C, Ricceri F. ‘Journey of hope’: a study on sexual gender-based violence reported by asylum-seeking women during their journey to Europe. Epidemiol Prev. 2020;44(5–6 Suppl 1):102–6.
Bergevin A, Husain M, Cruz M, Blanc CL, Dieme A, Girardin ML, et al. Medical check-up of newly arrived unaccompanied minors: A dedicated pediatric consultation service in a hospital. Arch Pediatr. 2021;28(8):689–95.
Article CAS PubMed Google Scholar
Giannopoulou I, Mourloukou L, Efstathiou V, Douzenis A, Ferentinos P. Mental health of unaccompanied refugee minors in Greece living ‘in limbo.’ Psychiatriki. 2022;33(3):219–27.
PubMed Google Scholar
Giordano F, Cipolla A, Ragnoli F, Brajda BF. Transit Migration and Trauma: the Detrimental Effect of Interpersonal Trauma on Syrian Children in Transit in Italy. Psychol Inj Law. 2019;12(1):76–87.
Garoff F, Skogberg N, Klemettilä A, Lilja E, Ahmed Haji Omar A, Snellman O, et al. Mental Health and Traumatization of Newly Arrived Asylum Seeker Adults in Finland: A Population-Based Study. Int J Env Res Public Health. 2021;18(13):7160.
Chernet A, Probst-Hensch N, Sydow V, Paris DH, Labhardt ND. Mental health and resilience among Eritrean refugees at arrival and one-year post-registration in Switzerland: a cohort study. BMC Res Notes. 2021;14(1):281.
Purić D, Vukčević MM. Development and validation of the Stressful Experiences in Transit Questionnaire (SET-Q) and its Short Form (SET-SF). Eur J Psychotraumatol. 2019;10(1):1611091.
FontanelliSulekova L, Ceccarelli G, Pombi M, Esvan R, Lopalco M, Vita S, et al. Occurrence of intestinal parasites among asylum seekers in Italy: A cross-sectional study. Travel Med Infect Dis. 2019;27:46–52.
Guarch-Rubio M, Byrne S, Manzanero AL. Violence and torture against migrants and refugees attempting to reach the European Union through the Western Balkans. Torture. 2020;30(3):67–83.
Jankovic-Rankovic J, Oka RC, Meyer JS, Snodgrass JJ, Eick GN, Gettler LT. Transient refugees’ social support, mental health, and physiological markers: Evidence from Serbian asylum centers. Am J Hum Biol. 2022;34(7):e23747.
Jankovic-Rankovic J, Oka RC, Meyer JS, Gettler LT. Forced migration experiences, mental well-being, and nail cortisol among recently settled refugees in Serbia. Soc Sci Med. 2020;258: 113070.
Prestileo T, Di Marco V, Dino O, Sanfilippo A, Tutone M, Milesi M, et al. Effectiveness of a screening program for HBV, HCV, and HIV infections in African migrants to Sicily. Dig Liver Dis. 2022;54(6):800–4.
Rodolico A, Vaccino N, Riso MC, Concerto C, Aguglia E, Signorelli MS. Prevalence of Post-Traumatic Stress Disorder Among Asylum Seekers in Italy: A Population-Based Survey in Sicily. J Immigr Minor Health. 2020;22(3):634–8.
Ben Farhat J, Blanchet K, JuulBjertrup P, Veizis A, Perrin C, Coulborn RM, et al. Syrian refugees in Greece: experience with violence, mental health status, and access to information during the journey and while in Greece. BMC Med. 2018;16(1):40.
Poole DN, Hedt-Gauthier B, Liao S, Raymond NA, Bärnighausen T. Major depressive disorder prevalence and risk factors among Syrian asylum seekers in Greece. BMC Public Health. 2018;18(1):908.
VukčevićMarković M, Bobić A, Živanović M. The effects of traumatic experiences during transit and pushback on the mental health of refugees, asylum seekers, and migrants. Eur J Psychotraumatology. 2023;14(1):2163064.
Crepet A, Rita F, Reid A, Van den Boogaard W, Deiana P, Quaranta G, et al. Mental health and trauma in asylum seekers landing in Sicily in 2015: a descriptive study of neglected invisible wounds. Confl Health. 2017;11:1.
AnderssonNystedt T, Herder T, Agardh A, Asamoah BO. No evidence, no problem? A critical interpretive synthesis of the vulnerabilities to and experiences of sexual violence among young migrants in Europe. Glob Health Action. 2024;17(1):2340114.
Belanteri RA, Hinderaker SG, Wilkinson E, Episkopou M, Timire C, De Plecker E, et al. Sexual violence against migrants and asylum seekers. The experience of the MSF clinic on Lesvos Island, Greece. PloS One. 2020;15(9):e0239187.
Keygnaert I, Guieu A. What the eye does not see: a critical interpretive synthesis of European Union policies addressing sexual violence in vulnerable migrants. Reprod Health Matters. 2015;23(46):45–55.
Reques L, Aranda-Fernandez E, Rolland C, Grippon A, Fallet N, Reboul C, et al. Episodes of violence suffered by migrants transiting through Libya: a cross-sectional study in “Médecins du Monde’s” reception and healthcare centre in Seine-Saint-Denis, France. Confl Health. 2020;14(1):12.
Article CAS PubMed PubMed Central Google Scholar
Tan SE, Kuschminder K. Migrant experiences of sexual and gender based violence: a critical interpretative synthesis. Glob Health. 2022;18(1):68.
Chynoweth SK, Buscher D, Martin S, Zwi AB. Characteristics and Impacts of Sexual Violence Against Men and Boys in Conflict and Displacement: A Multicountry Exploratory Study. J Interpers Violence. 2022;37(9–10):NP7470–501.
Marchetti F, Preziosi J, Zambri F, Tambascia G, Di Nolfi A, Scardetta P, et al. Health needs and perception of health care quality among Asylum Seekers and Refugees in an Italian local health authority: A qualitative study. Front Public Health. 2023;12(11):1125125.
Cañardo G, Gálvez J, Jiménez J, Serre N, Molina I, Bocanegra C. Health status of rescued people by the NGO Open Arms in response to the refugee crisis in the Mediterranean Sea. Confl Health. 2020;14(1):21.
Pries L, ZulfikarSavci BS. Syrian refugees arriving in Germany: choice of corridor and individual characteristics of forced migrants. Front Sociol. 2023;8:1070065.
Oliveira C, Keygnaert I, Oliveira Martins M do R, Dias S. Assessing reported cases of sexual and gender-based violence, causes and preventive strategies, in European asylum reception facilities. Glob Health. 2018;14(1):48.
Greenaway C, Castelli F. Migration Medicine. Infect Dis Clin North Am. 2019;33(1):265–87.
Riza E, Karnaki P, Gil-Salmerón A, Zota K, Ho M, Petropoulou M, et al. Determinants of Refugee and Migrant Health Status in 10 European Countries: The Mig-HealthCare Project. Int J Environ Res Public Health. 2020;17(17):6353.
Vearey J, Hui C, Wickramage K. Migration and health: Current issues, governance and knowledge gaps. United Nations; 2019 [cited 2024 May 8]. Available from: https://www.un-ilibrary.org/content/books/9789290687894s004-c003 .
Download references
Acknowledgements
Not applicable.
Open access funding provided by Università degli Studi di Padova.
Author information
Authors and affiliations.
Unit of Biostatistics, Epidemiology and Public Health (UBEP), Department of Cardiac, Thoracic, Vascular Sciences and Public Health, University of Padua, Padua, Italy
Cristina Canova, Clara Benna & Isabella Rosato
Centre for Biostatistics, Epidemiology and Public Health (C-BEPH), Department of Clinical and Biological Sciences, University of Turin, Orbassano, Italy
Lucia Dansero & Cinzia Destefanis
Department of Surgery Oncology and Gastroenterology, University of Padua, Padua, Italy
Clara Benna
You can also search for this author in PubMed Google Scholar
Contributions
CC and IR were involved in the coordination of the study. IR, CC, and CB managed the systematic review and screening phases, reviewed papers, and extracted data. CD and LD accessed and verified the data accuracy. All authors contributed to the development of the study methodology, the writing of the first draft, and the review of the manuscript. All authors had full access to all the data in the study, approved the final version of the manuscript, and had final responsibility for the decision to submit it for publication.
Corresponding author
Correspondence to Cristina Canova .
Ethics declarations
Ethics approval and consent to participate, consent for publication, competing interests.
The authors declare no competing interests.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
12992_2024_1075_moesm1_esm.docx.
Additional file 1: Table S1: PECO framework; Table S2: Search strings for included databases; Table S4: Studied populations’ characteristics; Table S5: Risk of bias table for studies that formally investigated the association between exposures and outcomes.
Additional file 2: Table S3: General characteristics of included studies.
Rights and permissions.
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/ .
Reprints and permissions
About this article
Cite this article.
Canova, C., Dansero, L., Destefanis, C. et al. Assessing the health status of migrants upon arrival in Europe: a systematic review of the adverse impact of migration journeys. Global Health 20 , 69 (2024). https://doi.org/10.1186/s12992-024-01075-3
Download citation
Received : 25 June 2024
Accepted : 16 September 2024
Published : 27 September 2024
DOI : https://doi.org/10.1186/s12992-024-01075-3
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Migration journey
- Systematic review
- Traumatic events
- Mental health
Globalization and Health
ISSN: 1744-8603
- General enquiries: [email protected]

IMAGES
COMMENTS
Notably, health equity was assessed in few quantitative measures of mental health policy implementation, which has been reported in previous studies of policy measures (Allen et al. ... Administration and Policy in Mental Health and Mental Health Services Research, 42 (5), 545-573. 10.1007/s10488-014-0551-7 ...
A quantitative report on the anxiety and depression scale based on a collected dataset from various professions on their regular lifestyle, choices, and internet uses phone through simulations and statistical reports. The contributions of this paper for Psychological health analysis in COVID - 19 pandemics summarized below: (1)
In clinical practice, the existing staff including mental health nurses, occupational therapists, psychologists, doctors and psychiatrists, are currently better placed to deliver exercise counseling for people with mental illness.Qualitative 25 and quantitative Stanton et al., 2015 a studies in high income countries suggest that nurses working ...
This research addressed these gaps by comparing SRMH, community belonging and life satisfaction in the 2019 CCHS to Fall 2020 data from the Survey on COVID-19 and Mental Health (SCMH). 22 SRMH, community belonging and life satisfaction are well-established and validated outcomes that are included in PHAC's Positive Mental Health Surveillance ...
Participants were either diagnosed with a mental condition (n = 169) or members of the broader mental health ecosystem (n = 101), including professionals of the health and social sector (n = 52 ...
Purpose Mental health inequalities across social identities/positions during the COVID-19 pandemic have been mostly reported independently from each other or in a limited way (e.g., at the intersection between age and sex or gender). We aim to provide an inclusive socio-demographic mapping of different mental health measures in the population using quantitative methods that are consistent with ...
The review findings identified several sampling techniques used in mental health research. Quantitative studies, usually employ probability sampling, whilst qualitative studies use non-probability sampling [25, 34]. The most common sampling techniques for quantitative studies are multi-stage sampling, which involves systematic, stratified ...
The coronavirus disease 2019 (COVID-19) pandemic has posed a significant influence on public mental health. Current efforts focus on alleviating the impacts of the disease on public health and the economy, with the psychological effects due to COVID-19 relatively ignored. In this research, we are interested in exploring the quantitative characterization of the pandemic impact on public mental ...
ObjectiveTo identify the prevalence of anxiety, depression, and suicidal ideation that would place university students at risk for mental health disorders.To explore the source of stressors and possible interventions that may benefit student mental health in a university setting. Participants: University students (n = 483) who had been learning remotely due to the COVID-19 pandemic.
mental health is addressing time lags in the relationship between exposure and outcome. This is a key aspect to . Panel: A snapshot of methodological trends and issues in the climate change and . mental health quantitative literature identified in our scoping review* • Most literature to date has focused on assessing the risks to mental ...
The quantitative literature on climate change and mental health is growing rapidly. However, the methodological quality of the evidence is heterogeneous, and there is scope for methodological improvement and innovation. The first section of this Personal View provides a snapshot of current methodological trends and issues in the quantitative literature on climate change and mental health ...
Notably, health equity was assessed in few quantitative measures of mental health policy implementation, which has been reported in previous studies of policy measures (Allen et al., ... Administration and Policy in Mental Health and Mental Health Services Research, 38(2), 65-76.
2. Materials and Methods. In order to search for criteria, indicators and methodology for evaluating and improving the quality of mental health services and related qualitative and quantitative indicators, a bibliography was searched in large databases PubMed, Google Scholar, CINAHL, using the keywords "mental", "health", "quality", "indicators", alone or in combinations thereof.
Needs assessment in mental health is a complex and multifaceted process that involves different steps, from assessing mental health needs at the population or individual level to assessing the different needs of individuals or groups of people. This review focuses on quantitative needs assessment tools for people with mental health problems. Our aim was to find all possible tools that can be ...
Women are at greater risk of common mental disorders. The intersectionality concept provides a framework to examine the effects of multiple social disadvantages on women's mental health. We conducted a systematic review to collect and analyse information to identify the quantitative methodologies and study designs used in intersectional research to examine women's mental health and ...
Stuart, Elizabeth A., and others, 'An Introduction to Quantitative Methods Especially Relevant for Public Mental ... the chapter focuses more specifically on some of the data and methodological complexities particularly common in public mental health research. Readers interested in obtaining a more general overview of statistical methods ...
Centre for Mental Health Research, Research School of Population Health, The Australian National University, Canberra, ACT, Australia. ... it has minimal relevance. Quantitative studies might be somewhat limited in their ability to capture this variability, although methods that investigate subgroups are to be encouraged.
Methods: In this study, 31 Ugandan health care professionals 20 men; 31.2 ± 7.1 years completed the Exercise in Mental Illness Questionnaire- Health Professionals Version EMIQ-HP. Results: The vast majority of the respondents 29/31, 94% reported they prescribed exercise at least "occasionally" to people with mental illness. Exercise ...
Centre for Mental Health Research, Research School of Population Health, The Australian National University, Canberra, ACT, Australia Correspondence Phil J. Batterham, Centre for Mental review Health Research, 63 Eggleston Road, The Australian National University,
Introduction. Adolescent mental health and substance use have been areas of substantial concern during the COVID-19 pandemic, 1 as there have been documented increases in major depressive disorder, generalized anxiety, drinking and cannabis use since April 2020. 2, 3 During the pandemic, a substantial proportion of adolescents began using substances primarily in solitude, 3 and it is estimated ...
Mental health and related conditions are a hot-button healthcare topic in 2024. With an estimated one in five Americans living with a mental health condition, ongoing research into the causes, treatment options, and possible triggers has never been more necessary.. Research in the mental health space helps fill knowledge gaps and create a fuller picture for patients, healthcare professionals ...
Mainly, this research will give a guideline that government should focus more on mental health as youths are being open towards mental health issues and if there will come support from the ...
Inclusion criteria included original articles published in peer-reviewed journals in English, using qualitative or quantitative approaches. We considered papers reporting incidence/prevalence and associated factors with mental health outcomes in UER of both sexes, all ages, and levels of competition (e.g., elite, nonprofessional runners).
2.1. Participants and procedure. The Rogers Behavioral Health (Rogers) Institutional Review Board is committed to the ethical principles for the protection of human subjects in research which guide the IRB's deliberations and decision-making, including respect for persons, beneficence, and justice.
Background Numerous studies have explored the impact of pre- and post-migration factors on the overall health of migrant populations. The objective of this study is to enhance our understanding of additional determinants affecting migrants' health by examining the impact of the migration phase and related journeys in the European context. Methods We conducted a systematic review of studies ...